
NEOMYCIN
First draft prepared by
J.E.M. van Koten-Vermeulen and Dr.F.X.R. van Leeuwen
Laboratory of Toxicology
National Institute of Public Health and Environmental Protection
Bilthoven, Netherlands
1. EXPLANATION
The aminoglycosides were evaluated as a group at the twelfth
meeting of the Joint FAO/WHO Expert Committee on Food Additives when
an ADI was not established. Because adequate toxicological and residue
data were not available it was stated that when aminoglycosides are
used they should not be allowed to give rise to detectable residue
levels in human food. (Annex I, reference 17). Since then, data
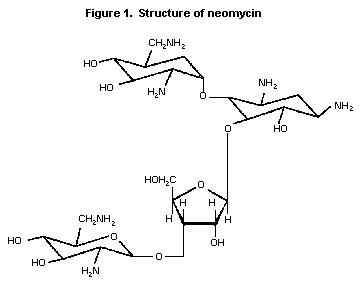
specific for neomycin have become available. The structure of
neomycin is shown in Figure 1.
 2. BIOLOGICAL DATA
2.1 Biochemical aspects
2.1.1 Absorption, distribution and excretion
2.1.1.1 Guinea-pigs
Groups of 4 male guinea-pigs were administered single oral doses
of 5, 10 or 100 mg/kg bw neomycin B sulfate. Serum was collected 1,
2, 3, and 4 hours after treatment. Neomycin concentrations of 1.5 and
0.45 µg/ml were measured at 1 and 2 hours after dosing with 100 mg/kg
bw, respectively. Serum concentrations of neomycin were below
detectable levels (< 0.10 µg/ml) in the low- and mid-dose groups at
all time points, and in the high-dose group at 3 and 4 hours post-
administration (Hall et al., 1983).
2.1.1.2 Chickens
Lohman chickens (14 total, weighing approximately 2 kg each) were
administered a single oral dose of 20 mg neomycin/kg bw. Neomycin
could not be detected in blood samples collected up to 8 hours post-
administration using a microbiological assay (detection limit not
specified) (Atef et al., 1986).
After a single i.v. administration of 20 mg/kg bw neomycin to
five Lohman chickens, the blood concentration curve showed a
biexponential decline with a T´ of about 6 hours for the elimination
phase and an AUC of approximately 196 µg/ml/h. After a single i.m.
administration of 20 mg/kg bw to 14 chickens, the peak blood level
(Cmax) was approximately 17 µg/ml and the mean maximum concentration
was reached 40 minutes after administration. The AUC was approximately
132 µg/ml/h. The bio-availability following i.m. administration was
approximately 70% (Atef et al., 1986).
In 22 Lohman chickens administered neomycin i.m. at 20 mg/kg bw
twice daily for 5 days, plateau levels of neomycin (about 6 µg/ml)
were retained for 1-4 days. Neomycin concentrations were detected in
the spleen for 3 days, in liver and lung for 6 days, and in kidney for
10 days post-injection (Atef et al., 1986).
2.1.1.3 Sheep
Serum and milk concentrations of neomycin were determined in
lactating Awassi ewes (4/group) after a single i.v. (20 mg/kg bw) or
i.m. injection (10 mg/kg bw). Neomycin was assayed micro-biologically
using the cylinder cup method (sensitivity limit 1 µg/ml). After i.v.
administration the T´ was approximately 3 hours and distribution
equilibrium was reached within 20 min. After i.m. administration peak
concentrations were reached after 1 hour. Neomycin was not detectable
in serum 12 hours after treament. A very small fraction of the dose
(0.01%-0.02%) was recovered in milk secreted from normal or irritated
glands (in which the left-side glands of the udder were infused with
150 ml of hypertonic NaCl solution 24 hours before treatment) during
the 12 hours after treatment. Peak milk concentrations of neomycin
following i.v. or i.m. treatment were less than 2 µg/ml (Ziv & Sulman,
1974).
2.1.1.4 Pigs
Two groups (6 pigs/group) of Yorkshire crossed weanling pigs (10
weeks old, weighing 10 to 15 kg) were orally administered 22 mg
neomycin sulfate/kg bw/day for 5 consecutive days. Group 1 consisted
of 3 males and 3 females, while group 2 had 5 males and 1 female. In
addition to the oral neomycin treatment, pigs in the second group
received diets supplemented with sodium sulfate at a rate of 10 g/kg
feed. Serum neomycin concentrations were measured up to 96 hours after
dosing. The mean peak serum concentration (approximately 0.2 µg/ml)
of neomycin was reached in the fourth hour in pigs fed the normal
ration. For pigs receiving the supplemented diets, the mean peak
serum concentration (approximately 0.1 µg/ml) was reached at 8 and 24
hours after dosing (Heath, 1985).
In another study by the same author, a single i.v. dose of 22
mg/kg bw neomycin sulfate was administered to 6 (3/sex) 10-month old
pigs. A peak mean serum level of approximately 30 µg/ml was detected
one hour after dosing, which decreased to 0.01 µg/ml by 72 hours
(Heath, 1985).
A single i.m. dose (22 mg/kg bw) of neomycin sulfate was
administered to 12 female pigs weighing 20 to 50 kg. A peak mean
serum level of approximately 40 µg/ml which was reached one hour after
dosing, decreased to 0.02 µg/ml after 72 hours (Heath, 1985).
2.1.1.5 Cattle
Ten castrated Holstein calves (2 to 6 months of age, weighing 80
to 180 kg) were orally administered 22 mg neomycin sulfate/kg bw/day
for 5 days. Serum concentrations were determined up to 96 hours after
dosing. Mean serum concentrations ranged from 0-0.06 µg/ml during the
1-96-hour dosing period (Heath, 1985).
A single i.v. dose (22 mg/kg bw) of neomycin sulfate was
administered to 10 castrated Holstein calves (2 to 6 months old,
weighing 70 to 170 kg). A peak mean serum concentration of
approximately 19 µg/ml which was detected one hour after dosing,
decreased to 0.03 µg/ml by 72 hours (Heath, 1985).
Four male Holstein calves (3 to 60 days old) were given a single
oral dose of 30 mg 14C-neomycin/kg bw and then killed after 96 hours.
The distribution of 14C in excreta and tissues was determined by mass
spectrophotometric analysis. Most of the radioactivity was recovered
in faeces (85-97%). The radioactivity found in urine decreased with
increasing age of the animal, from 11 to 0.5% of the administered
dose. Radioactivity found in the kidneys, liver and muscle of calves
at 3 days of age represented 55, 1.93 and 0.09 ppm of neomycin
equivalents, respectively. At least 90% of the 14C in the kidneys of
3-day old calves was present as neomycin. Seventy to 88% of the 14C
present in faeces of all calves was also identified as neomycin
(Aschbacher & Feil, 1991, 1994).
Serum and milk concentrations of neomycin were measured in 4
lactating Israeli-Friesian dairy cows following administration of a
single i.m. dose (10 mg/kg bw). Neomycin was assayed micro-
biologically by the cylinder cup method (sensitivity limit 1 µg/ml).
Peak serum concentrations were reached after 1 hour. Neomycin was not
detectable in serum 12 hours after treament. A very small fraction of
the dose (0.016%-0.022%) was recovered in milk secreted from normal or
irritated glands (in which the left-side glands of the udder were
infused with 150 ml of hypertonic NaCl solution 24 hours before
treatment) during the 12 hours after treatment. Peak milk
concentrations of neomycin were less than 2 µg/ml (Ziv & Sulman,
1974).
2.1.1.6 Humans
An oral dose of 1.5 g neomycin/day was administered to a 2- year
old female tuberculosis patient for 15 consecutive days. A nine-month
old male tuberculosis patient received 200 mg neomycin/day orally for
80 days. Both patients were diagnosed with miliary tuberculosis and
tuberculous meningitis. A maximum neomycin serum concentration of
approximately 5.0 µg/ml was achieved in both patients. Cerebrospinal
fluid concentrations of 1.25 and 2.5 µg/ml were measured in the female
and male patient, respectively (Waisbren & Spink, 1950).
Poth et al. (1951) reported serum concentrations ranging from
not detectable to <80 µg/ml in patients treated with oral neomycin
(6 g/day) for 3 days. The majority of the administered dose was
excreted in the faeces unchanged. Only 3% of the dose was recovered
from the urine.
The absorption and excretion of a 2 g oral or rectally
administered dose of neomycin sulfate was studied in 10 normal
subjects (healthy physicians who had no history of renal or liver
disease) and in patients with liver disease, peptic ulcer, regional
enteritis, or active ulcerative colitis. Urinary excretion (0.58%) of
neomycin and serum neomycin concentrations over 48 hours were similar
in all groups and by both routes. The percentage of the neomycin dose
excreted in the faeces following oral or rectal administration was
comparable (approximately 99%) (Breen et al., 1972).
2.1.2 Biotransformation
Aminoglycosides as a class are not metabolized in animals (Bevan
& Thompson, 1983) and are mostly excreted unchanged (Aschbacher &
Feil, 1994; Keen, 1975).
2.1.3 Special studies on binding to macromolecules
Lactating Israeli-Freisian cows (2 animals) and Awassi ewes (4
animals) were given single doses of 20 mg/kg bw neomycin i.m. or i.v.
Resulting serum concentrations ranged from 5-10 µg/ml. Serum protein
binding, determined by equilibrium dialysis and ultrafiltration
methods, was approximately 45-50% and 50-55% for cows and ewes,
respectively (Ziv & Sulman, 1972).
2.2 Toxicological studies
2.2.1 Acute toxicity studies
The results of acute toxicity studies after oral, i.v., s.c. or
i.p. administration of neomycin are summarized in Table 1.
2.2.2 Short-term toxicity studies
2.2.2.1 Cats
Groups of cats (8/sex/group) were orally dosed (gelatin capsule)
with 0, 6, 12 or 25 mg technical neomycin sulfate/kg bw/day for 1
year. The actual administered doses were found by chemical analysis
to be 72% of the intended doses. Clinical signs, auditory and
vestibular examinations, body weight, haematology, serum chemistry,
urinalysis, organ weights, macroscopy and histopathology were
evaluated.
The cause of the death of 7 cats during the study was not
considered to be treatment-related. The RBC counts were significantly
decreased in males at the highest dose at weeks 26 and 52. Blood urea
nitrogen levels were significantly increased in high-dose males at 13,
26 and 52 weeks, but no histopathological evidence of kidney damage
was observed. In the high-dose males at termination, potassium,
chloride and alkaline phosphatase were decreased, and cholesterol
levels were increased. Relative spleen and pancreas weights were
significantly decreased at all dose levels in male cats but without a
dose-related trend. Bone marrow hypoplasia was seen histogically in
the high-dose group (3/6 males and 4/8 females) (Kakuk, 1981).
Table 1. Acute toxicity of neomycin
Species Sex Route Substance Purity LD50 Reference
(mg/kg bw)
Mouse ? oral neomycin sulfate ? approx. Swoap, 1952c,d
2250-2500
Mouse M&F oral neomycin sulfate bulk 900 µg/mg 2250-2298 Swoap, 1952f,g,h
Mouse M&F oral neomycin sulfate (bulk 900-1000 >2500 Swoap, 1952b
powder from resin process) µg/mg
Mouse ? i.v. neomycin sulfate ? 40-158 Vander Brook, 1949;
Swoap, 1949a,b;
1950a,b,c,d,e,i,j,k;
1951a,b; Cale, 1950;
Gray, 1964
Mouse M i.v. neomycin sulfate ? 64.6-107 Brockie, 1951; Cale,
1950; Swoap,
1950f,g,h
Mouse M&F i.v. neomycin sulfate ? >50 Swoap, 1953a
Mouse ? i.v. neomycin A hydrochloride ? 97.6 Swoap, 1949a
Mouse M&F i.v. neomycin in HCH ? 74-115 Swoap, 1952a
Mouse ? i.v. neomycin sulfate bulk 900 µg/mg 110 Swoap, 1952e
Mouse M&F i.v. neomycin sulfate (bulk 910 µg/mg 100 Swoap, 1952b
powder from resin process)
Mouse ? s.c. neomycin sulfate ? 550 Vander Brook, 1949;
Swoap, 1950c,d,e
Table 1 (contd)
Species Sex Route Substance Purity LD50 Reference
(mg/kg bw)
Mouse ? s.c. neomycin sulfate ? 400 Brockie, 1951
Mouse ? s.c. neomycin A ? 470 Vander Brook, 1949
hydrochloride (51)
Mouse ? i.p. neomycin sulfate ? 274 Gray, 1964
Mouse M&F i.p. neomycin sulfate 690 µg/mg 310-457 Feenstra, 1958a;
Swoap, 1957a
Mouse M&F i.p. neomycin B sulfate ? 277-389 Swoap, 1954a,b;
Shealy, 1956
Mouse M&F i.p. neomycin B sulfate 1000 µg/mg 533 Swoap, 1953c
Shealy, 1956
Mouse M&F i.p. neomycin sulfate Po. 690 µg/mg 356 Swoap, 1958
blended USP
Mouse M&F i.p. neomycin sulfate bulk 658 µg/mg 248 Feenstra 1959
2.2.3 Long-term toxicity/carcinogenicity studies
2.2.3.1 Rats
Eight groups of Sprague-Dawley (SD)BR F1a weanling rats (4 groups
of males, 4 groups of females, 54-56/group) were administered neomycin
sulfate via the diet at 0, 6.25, 12.5 or 25 mg/kg bw/day until
terminal sacrifice. The test animals were offspring from the
F0generation that were mated after consuming similar levels of
neomycin in the diet for 11 weeks (see section 2.2.4). After 52 weeks
of treatment 10 rats/sex/group were selected for an interim kill and
evaluation. All male groups were killed after 104 weeks when the
control group survival reached 20%. When survival in female groups
reached 20%, the remaining animals of the group were sacrificed (27 to
30 months). Clinical signs, body weight, food consumption,
haematology, clinical chemistry, urinalysis, ophthalmoscopy, auditory
and vestibular tests, organ weight and histopathology were evaluated
in control and high-dose male and female rats.
To assess the possible effects of neomycin on the vestibular and
auditory functions an additional group (6/rats/sex, weanlings selected
from the control group in the reproduction study) was administered
neomycin sulfate s.c. at 100 mg/kg bw/day. Auditory and vestibular
function tests were scheduled weekly until study termination. When
all rats showed hearing loss (week 14), they were killed. Tissues of
the inner ear were preserved, but histopathological examinations were
not carried out.
Up to week 84, overall survival was about 84% and 92% for males
and females respectively. At the end of the study high mortality was
observed in all groups (33/44, 27/45, 29/46 and 30/45 for males and
33/46, 34/45, 34/44 and 35/45 for females at 0, 6.5, 12.5 and 25 mg/kg
bw/day, respectively). Female body weights were dose-relatedly
increased during the first three weeks of the study. Although not
statistically significant 3/15 rats at 25 mg/kg bw/day showed
hearing loss at the end of the study. No treatment-related effects
were observed in any of the other parameters evaluated. There was no
evidence of carcinogenicity. The NOEL was 12.5 mg/kg bw/day (Kakuk,
1982).
2.2.4 Reproductive toxicity studies
2.2.4.1 Rats
In a 3-generation reproductive toxicity study groups of Sprague-
Dawley (SD)BR rats (40-20/sex/group) were administered neomycin
sulfate via the diet at 0, 6.25, 12.5 or 25 mg/kg bw/day. After 11
weeks F0 generation rats were mated to produce F1a offspring which
were subsequently continued on neomycin sulfate in the life-time
feeding study described in section 2.2.3. F0 animals were bred a
second time to produce F1b offspring for use in the reproduction study
(through F3b litters). Through all generations no treatment-related
effects were observed in any of the parameters evaluated. The NOEL was
25 mg/kg bw/day (Kakuk, 1980).
2.2.5 Special studies on embryotoxicity and teratogenicity
2.2.5.1 Rats
Groups of 20 pregnant Sprague-Dawley (SD)BR rats (F2b females
from the reproductive toxicity study) were maintained on the same dose
regimen of 0, 6.25, 12.5 or 25 mg/kg bw/day (see section 2.2.4). From
gestation days 6-15, doses were increased to 0, 62.5, 125 or 250 mg/kg
bw/day. From gestaton days 16-20, doses were returned to 0, 6.25,
12.5 or 25 mg/kg bw. Dams were killed on day 20 of gestation. No
evidence of maternal toxicity, fetotoxicity or teratogenicity was
observed (Kakuk, 1980).
2.2.6 Special studies on genotoxicity
The results of the available genotoxicity studies on neomycin are
summarized in Table 2.
2.2.7 Special study on nephrotoxicity
2.2.7.1 Mice
Ten mice/group were given s.c. doses of 0, 30, 100, 300, 600 or
1000 mg/kg bw/day neomycin A (neamine), neomycin B or neomycin C for
14 days. None of the mice at the 2 highest doses survived 14 days.
Two mice in the 1000 mg/kg bw/day neamine group died.
Histopathological examination of the kidneys was performed. Based on
lesion indices the degree of nephrotoxicty was established. Neomycin
B and Neomycin C were about equally nephrotoxic. The observed
nephrotoxicity in the neamine groups was about 50% of that observed in
the other neomycin groups (Feenstra, 1954).
2.2.7.2 Guinea-pigs
Guinea-pigs (3/sex/group) were administered 10, 20, or 60 mg
neomycin sulfate/kg bw/day for 3 months (route not specified). One
female was kept as a control. Histopathological evaluation of the
kidney revealed subacute to chronic focal interstitial nephritis
associated with degeneration and necrosis at all doses, with a dose-
related increase in severity (Feenstra, 1950).
Table 2. Results of genotoxicity studies on neomycin
Test system Test object Concentration Results Reference
In vitro
Chromosome human 20, 40 and 80 µg/ml positivea,b Jaju et al., 1986
aberration assay lymphocytes
SCE test human 20, 40 and 80 µg/ml negativeb Jaju et al., 1986
lymphocytes
In vivo
Cytogenetic Mice bone 50 mg/kg bw positiveb,c Manna & Bardhan,
assay marrow 1973
a At doses that significantly inhibit the progression of the cell cycle.
b No positive control group was used.
c Test was not performed to current standards, i.e., results from 12 fixation
times are combined in 6 groups and number and sex of animals not stated.
Mitotic frequency was decreased; therefore, it was concluded that neomycin
reached the bone marrow.
2.2.7.3 Dogs
Six dogs (3/group) were administered 20 or 60 mg neomycin
sulfate/kg bw/day for 88 days (route not specified). All 3 dogs in
the high-dose group died after 14, 16 and 21 days. One low-dose dog
survived. The other 2 died after 21 and 45 days. Urine samples from
all dogs were taken before and after the beginning of treatment and
analyzed for albumin, blood and the presence of casts.
Histopathological examinations of kidneys showed degeneration,
necrosis and focal interstitial nephritis in all 6 dogs (Feenstra,
1950).
Twelve dogs were injected intramuscularly with 24, 48, or 96
mg/kg bw/day neomycin. At the highest dose all dogs died within 1-3
weeks. Blood urea nitrogen was increased and renal function impaired
as shown by decreased phenolsulfonphthalein excretion.
Histopathological evaluation of kidneys revealed renal tubular damage
characterized by marked epithelial necrosis in the proximal convoluted
tubules. Moderate changes in bone marrow and marked congestion of the
liver were also found. Inflammation at injection sites was also
noted. At the mid-dose the severity of effects were described as
intermediate. Dogs exposed to 24 mg/kg bw/day were killed and
examined after 1 month. The severity of renal damage in this group
was described as slight with increased granularity and occasional
desquamation of epithelial cells being most evident (Nelson et al.,
1951).
No kidney damage was observed in dogs (number/sex/group not
stated) orally dosed with 100 mg neomycin/kg bw/day for 6 weeks based
on urinalyses and gross and histopathological examinations of kidneys.
No other abnormalities were observed (Poth et al., 1951).
2.2.8 Special studies on ototoxicity
2.2.8.1 Guinea-pigs
Groups of 3 guinea-pigs were administered i.m. doses of 25, 50,
100, or 150 mg neomycin/kg bw/day for 30 to 60 weeks. Parameters
evaluated included vestibular function, auditory function (Preyer's
reflex) and histolopathological examination of labyrinths and central
nervous systems.
One guinea-pig in the high-dose group died after 22 days on test.
Vestibular function was reported as normal or slightly impaired across
all treatment groups with no dose-response relationship. Preyer's
reflex was abolished in all guinea-pigs receiving 100 and 150 mg/kg
bw/day. Histopathological examinations of animals in which the
Preyer's reflex was abolished revealed marked destruction of hair
cells and sometimes complete destruction of the organ of Corti.
Animals with intact hearing had normal cochleae, cristae, and maculae.
Reversible as well as irreversible degeneration of the ganglion cells
was seen in animals with abolished hearing, while animals with intact
hearing showed no definite pathological changes (Riskaer et al.,
1956) .
Hearing was not affected (determined by audiometry) after the
installation of 3 mg/kg bw neomycin into the middle ear of 18 guinea-
pigs. Six of the test animals had either one or both tympanic
membranes perforated prior to treatment (Riskaer et al., 1956).
Groups of guinea-pigs (50/sex/group) were orally admini-stered
neomycin B sulfate at 0, 1, 5, or 10 mg/kg bw/day for 90 days. Two
positive control groups (20/sex/group) received 10 or 100 mg/kg bw/day
s.c. for 90 and 34 days, respectively. Parameters evaluated included
clinical signs, body weight, auditory function test (Preyer pinna
reflex), gross necropsy, and histopathology (including cochleae to
score the loss of hair cells from the organ of Corti).
At 100 mg/kg bw/day s.c., ototoxic changes in the Preyer pinna
reflex thresholds and cochlear hair cell counts were observed. These
changes were not seen in the low-dose s.c. group nor in any of the
groups after oral administration. The NOEL for orally administered
neomycin in this study was 10 mg/kg bw/day (Brummett et al., 1985).
2.2.8.2 Cats
A clinical neomycin formulation (containing mostly neomycin B
sulfate), neomycin A hydrochloride and neomycin B sulfate were
administered s.c. to groups of cats (number/sex/group not stated) in
daily doses of 80 mg/kg bw/day for 5 or 15 days. The clinical
formulation was also administered in doses of 20, 40, or 100 mg/kg
bw/day s.c. for periods of 90, 60 and 30 days, respectively. Crude
neomycin (about 70% pure) was orally administered at 2 daily doses of
500 mg/kg bw (1 g/animal/day) for 30 days. Vestibular function was
studied by electrical recording of nystagmus evoked by rotating the
animal on a motor-driven turntable. Hearing ability was followed and
the cochlear function was studied electrophysically.
Histopathological examination of the kidneys was performed of all
cats.
Vestibular function was affected only in cats receiving the
highest dose of the clinical formulation (100 mg/kg bw/day) for 30
days. One of these cats showed a gradual loss of nystagmus which was
entirely absent by day 35, 5 days after the last treatment. Depression
of cochlear function was observed in all groups of cats and was most
severe in cats receiving the clinical preparation s.c. Degeneration
of external hair cells in the organ of Corti and internal hair cells
was also observed. A dose-related increase in the severity of damage
to renal tubular epithelium occurred in all cats receiving the
clinical preparation s.c. and in cats orally dosed with crude neomycin
(Hawkins, 1952; Hawkins et al., 1953).
Ototoxicity was studied in 5, 8, 3, and 4 cats who received oral
doses of 0, 6.25, 12.5, or 25 mg neomycin/kg bw/day, respectively, for
1 year. No evidence of auditory or vestibular dysfunction was
observed. In surface preparations of the organ of Corti
(cytocochleograms) ototoxicity was present microscopically as loss of
outer hair cells from the extreme lower portion of the basal turn of
the cochlea. Severe ototoxicity was observed in 3/4 high-dose cats.
Hair cell loss of a lesser degree was also observed in 7/8 and 1/3
cats in the low- and mid-dose groups, respectively (Kakuk, 1981). Due
to serious shortcomings in the histological technique and the absence
of a clear dose-related effect, the Committee considered this study
inadequate for the safety evaluation of neomycin.
2.2.9 Special studies on irritation and sensitization
No significant irritation was observed 24 hours after the
intrapleural administration of single doses of solutions of 1 ml
neomycin sulfate (0-100 mg/ml) to guinea-pigs (3-4/dose) (Swoap,
1951c).
A group of 9 neomycin-sensitive guinea-pigs was evaluated with
the patch test for cross sensitivy to kanamycin, streptomycin,
dihydrostreptomycin and bacitrin. Positive results were obtained for
kanamycin (1/9) and streptomycin (8/9) (Epstein & Wenzel, 1962).
2.2.10 Special studies on microbiological effects
Neomycin is active against most gram-positive and gram-negative
rods, many gram-positive cocci, and such acid-fast pathogens as
Mycobacterium tuberculosis.
Neomycin reacts with 30S ribosomal subunits of procaryotic cells
by electrostatic attraction causing a change in the conformation of
the ribosomal binding protein. This results in mRNA reading errors
and disrupted protein synthesis.
2.2.10.1 In vitro
Minimum Inhibitory Concentration (MIC) values for different
bacterial strains obtained from animal or human isolates are listed in
Tables 3 and 4, respectively.
In a special study, strains of various bacterial genera, mostly
of human origin, were tested for their susceptibility to neomycin
sulfate. MIC values were estimated on two agar types, Wilkens
Chalgren/glucose medium (WCG) and supplemented blood medium (SB) with
2 inoculum densities. Estimations were made under anaerobic and
aerobic conditions (E. coli) by the agar dilution method. The
results are listed in Table 5 (Thurn et al., 1994).
The adsorption of neomycin to dog faeces was calculated as the
difference between the amount of neomycin added to dilute suspension
of dog faeces and the amount of neomycin measured (microbioloigal
assay) in the supernatant after the mixture was incubated and
centrifuged. About 75% adsorption of neomycin was observed. After
acid extraction 47% of the added neomycin was still bound to the
faecal solids (Wagman et al., 1974).
Several concentrations of neomycin were evaluated for adsorption
to human faeces. Faecal samples were obtained from 8 healthy human
volunteers. The binding of neomycin to the faeces was calculated as
the difference between the amount added to a dilute suspension of
faeces and the amount measured (micro-biological assay) in the
supernatant after the mixture was incubated for 1 hour and
centrifuged. Approximately 83-98% faecal binding was observed
(Hazenberg et al., 1983b, 1984).
Neomycin solutions of approximately 0.1-30 mg/ml were mixed with
faecal suspensions prepared from faeces of 8 healthy human volunteers.
Neomycin antimicrobial activity (tested with Enterobacter cloacae)
remaining in the supernatants was measured and used for calculating
the "% inactivation" relative to the amount of added neomycin. The
percentage of added neomycin that was biologically inactivated
decreased with increasing concentrations of neomycin. Nearly 100%
inactivation due to binding occurred when the ratios of neomycin to
faecal weight were < 5 mg neomycin to 1 g wet weight of faeces in an
incubation mixture (Veringa & Van der Waaij, 1984).
2.2.10.2 In vivo
Oral administration of neomycin to 37 healthy mongrel dogs (400
mg/day for 2, 4, or 10 days) and 24 healthy humans (6 g/day for 1 or
3 days) caused a marked reduction or complete elimination of coliform
bacilli from faeces in both species within 24 to 48 hours. In 4/10
dogs receiving a dose of 400 mg/day for 10 days resistant strains of
E. coli appeared on the 5th-6th day of treatment. Resistance was
not observed in E. coli isolates from humans treated with neomycin
in this study (Schweinburg et al., 1952).
Groups of 3-5 human flora associated (HFA) mice (germ-free mice
colonized with bacteria from human faecal suspensions) were
administered 1, 2, 3 or 4 g/l neomycin in their drinking-water.
Faecal samples were cultured on days 0, 1, 3, 5, 7, 14, 21, 28 and 35
of treatment. A control group of HFA mice received no neomycin
treatment. The number of obligate anaerobes, gram negative obligate
anaerobes, E. coli and Enterococci did not change over 35 days
in the 1 g neomycin/l drinking-water group. In the 2 and 3 g
neomycin/l groups, Escherichia coli and Enterococci were
eliminated, and the percentage of gram-negative obligate anaerobes was
increased. The NOAEL in this study is 1 g/l, equal to 125 mg/kg bw/day
(Hazenberg et al., 1983a).
Table 3. Summary of MIC values for different bacterial species obtained from animal isolates
MIC (µg/ml)
Species No. of Mean or Range MIC50 Reference
strains
Staphylococcus aureus 0.5 Moellering, 1983
Escherichia coli 8.0
Klebsiella pneumoniae 2.0
Proteus mirabilis 8.0
Proteus morganii 8.0
Proteus rettgeri 8.0
Proteus vulgaris 4.0
Escherichia coli (calves) 16 Hewett, 1990
Escherichia coli (pigs) 16
Escherichia coli (chickens) 1
Salmonella sp. (calves) 1
Salmonella sp. (pigs) 0.5
Bacteroides nodosus 68 16 - >256 >256 Duran et
al. , 1991
Bacteroides putredinis 36 16 - >256 128
Bacteroides buccae 16 2 - >256 128
Bacteroides sp. 21 8 - >256 >256
Table 3 (contd)
MIC (µg/ml)
Species No. of Mean or Range MIC50 Reference
strains
Fusobacterium necrophorum 10 16 - >256 128
Fusobacterium sp. 19 2 - >256 128
Peptostreptococus sp. 35 <0.06 - >256 64 Piriz et al., 1992
Table 4. Summary of MIC values for different bacterial species obtained from
human isolates
MIC (µg/ml)
Species No. of Mean or range Reference
strains
Escherichia coli 10 0.25 - 12.5 Schweinberg et al.,
1952
Enterococci 5 3.2 - 15
Sphaerophorus necrophorus 7 200 - 1600 Finegold et al.,
1967
Bacteroides fragilis 55 1600 - >25 600
Bacteroides melaninogenicus 20 <100 - 400
Bacteroides oralis 16 <100 - 400
Fusobacterum sp. 22 100 - 3200
Bifidobacterium adolescentis 11 12.5 - 400 Miller & Finegold,
1967
Bifidobacterium bifidum 5 400 - 1600
Bifidobacterium longum 11 200 - 1600
Bifidobacterium sp. 6 200 - 1600
Clostridium novyi Type A 16 32 - 512 Dornbusch et al.,
1975
Clostridium novyi Type B 7 64 - 512
Clostridium bifermentans 9 64 - 512
Clostridium sordellii 6 64 - 512
Clostridium sporogenes 18 32 - 512
Table 4 (contd)
MIC (µg/ml)
Species No. of Mean or range Reference
strains
Propionicum agnes 38 6.25 - 25 Hoeffler & Pulverer,
1976
Escherichia coli 2 16 Hazenberg et al.,
1983b
Escherichia coli 3 1 - 32 Hazenberg et al.,
1984
Table 5. Summary of MIC values under different agar medium and inoculum density conditions
MIC50 (µg/ml)a
Bacterial species/genus Strains Low densityb High densityc
SBd WCGd SBd WCGd
Bacteroides 15e,f >128 >128 >128 >128
Bifidobacterium 12e 16 128
Clostridium 11e, 5f >128 128 >128
Enterococcus 10e, 2f >128 128 >128 >128
Escherichia 13e 16 64
Escherichia - Aerobic 13e >128 >128
Eubacterium - Anaerobic 9e 8 >128
Fusobacterium 5e, 3f 16 32 >128 128
Lactobacillus 15e, 2f >128 32 >128 64
Peptostreptococcus/ 16e, 14f >128 32 >128 128
Peptococcus
a MIC50 values are for the multiple strains included in the assay.
b Low density inocula had cell concentrations of approx. 1 x 108 cells/ml.
c High density inocula had cell concentrations of approx. 1 x 1010 cells/ml.
d SB = Supplemented blood medium; WCG = Wilkins-Chalgren/glucose medium
e Number of tested strains of which MIC values for WCG were used to
calculate the summary values
f Number of tested strains of which MIC values for SB were used to
calculate the summary values
2.2.10.3 Special studies on potential effects on microorganisms used
for industrial food processing
Thirty strains of Propionobacterium sp., used to manufacture
Emmenthal and related cheese varieties, showed no resistance to 30
µg/disc neomycin but at 5 µg/disc moderate sensitivity was observed
(8/30 strains were resistant) (Reddy et al., 1973).
Forty-two strains of mesophilic lactic Streptococci,
Enterococci, Lactobacilli, Leuconostoc, Staphylococci and
other dairy- and food-related microorgansims were tested for their
sensitivity to neomycin at 5 and 30 µg/disc. Elliker's lactic agar
served as the growth medium; incubations temperature and times were
varied according to individual culture growth requirements.
Most of the strains of the starter streptococci (S. lactis,
S.cremoris, S. diacetilactis and S. thermophilus) and Lactobacillus
bulgaricus were sensitive to neomycin. Strains of S. faecalis,
exhibited resistance at 5 and 30 µg/disc (Reinbold & Reddy, 1974).
In another study, 24/29 strains of Lactobacillus bulgaricus
and all 15 tested strains of Streptococcus thermophilus were
resistant to 5 µg/disc neomycin. The tests for resistance were
carried out with commercially available sensitivity disks. At higher
doses of neomycin (30 µg/disc) resistance in 14/15 strains of
S.thermophilus and 10/29 strains of L. bulgaricus was observed
(Sozzi & Smiley, 1980).
The effect of residues of neomycin in milk on bacterial starter
cultures used in the production of fermented milk products was
investigated. Milk samples spiked with either 4 or 40 µg/ml neomycin
were serially diluted with antibiotic-free milk to provide
concentrations ranging from 0.063-4 µg/ml. Actual concentrations
measured with a microbiological cylinder plate assay ranged from
<0.20-3.12 µg/ml (detection limit: 0.20 µg/ml). The starter culture
types included a group of buttermilk/sour cream cultures containing
strains of Lactococcus lactis spp. and spp. cremoris or a
mixture of lactic acid producers and citric acid fermenters, 2 groups
of Italian cheese cultures containing strains of Streptococcus
thermophilus, another group of Italian cheese cultures containing
strains of Lactobacillus helveticus, and a group of yogurt cultures
containing Streptococcus thermophilus and Lactobacillus debruckii
spp. bulgaricus. "Time to clot" ratios greater than 2 indicated
that cultures were adversely affected by the presence of neomycin.
The only cultures adversely affected were the yogurt starter cultures
at a neomycin concentration of 4 µg/ml (equivalent to 3.12 µg/ml). In
this study neomycin concentrations in milk <2 µg/ml (equivalent to
1.42 µg/ml) had no effect on the growth of the bacteria in any of the
starter cultures (Hallberg et al., 1994).
2.3 Observations in humans
2.3.1 Nephrotoxicity
A clinical investigation of 63 patients (34 males and 29 females
ranging in age from nine months to 63 years (22 of them >60 years) on
neomycin therapy was undertaken. Renal toxicity and ototoxicity
toxicity were reported as treatment-related effects in some patients.
Twenty-four out of 32 patients, in whom serial urinalyses were
performed, showed fine granular casts in their urine either during or
just after neomycin therapy (Waisbren & Spink, 1950).
Powell and Hooker (1956) reported several cases of severe tubular
damage found in kidneys at autopsy of patients treated intramuscularly
with neomycin.
Oral administration of decreasing doses of neomycin (9.4- 1.5 g/d
(total 46 g over 11 days) to a patient produced acute renal failure
(Greenberg & Momary, 1965).
2.3.2 Ototoxicity
Ototoxic effects determined by audiograms and vestibular
functional tests were observed in patients treated with neomycin at
doses ranging from 1.5-2 g/day i.m. for up to 9 days. Hearing loss
was reported in 5 patients and loss of vestibular function occurred in
2 patients (Waisbren & Spink, 1950).
Deafness with histopathological inner ear changes were reported
in patients receiving high doses of neomycin orally (18 to 633 g total
dose) for unspecified periods of time (Lindsay et al., 1960;
Halpern & Heller, 1961; Greenberg & Momary, 1965).
Severe deafness occurred in a 1´-year old female, treated for
enteritis for 10 days with a neomycin-containing medication. The
total dose of neomycin was less than 2 g (King, 1962).
Severe deafness was reported in a 75 year-old female patient
receiving colonic and rectal irrigations with a neomycin solution for
2 months. A 5% solution was administered initially, then decreased to
a 1% solution for the majority of the treatment period. The total
neomycin dose administered was estimated at >900 g. The patient had
a hearing deficit but did not require a hearing aid prior to treatment
(Fields, 1964).
2.3.3 Hypersensitivity
From a survey of 675 patients with skin infections treated with
neomycin it was concluded that the sensitizing index for neomycin was
very low (Kile et al., 1952). However, cases of contact dermatitis
from neomycin (e.g., eardrops and eyedrops) were reported as dermal
delayed (tuberculin-type) and not epidermal sensitivity (Epstein,
1956; Calnan & Sarkany, 1958). In 55-75% of patients with neomycin
sensitivity, evidence of atopy (a genetic predisposition to mounting
large immune responses to antigenic stimulation) was established
(Epstein, 1965).
Results of patch tests with 21 antibiotics performed on a large
number of patients sensitive to neomycin showed cross-sensitivity to
bacitracin (80%), framycetin (91%), paromomycin (up to 99%) and
kanamycin (61%) (Pirila & Rouhunkoski, 1962). Cross-sensitization
with neomycin in streptomycin-sensitized patients was also described,
although contradictory results were obtained with respect to the
neomycin sensitivity in streptomycin-sensitive patients
(Sidi et al., 1958; Calnan & Sarkany, 1958).
A patient treated with ear drops containing neomycin (5 mg/ml in
distilled water) developed an acute exacerbation of otitis externa
after previously having shown a highly satisfactory response to the
use of the neomycin ear drops (Baer & Ludwig, 1952).
2.3.4 Special studies on the malabsorption syndrome
Morphologic alterations in the jejunal mucosa of patients,
similar to but less marked than those seen in patients with idiopathic
steatorrhea, were seen in 11/12 biopsy specimens from patients treated
with neomycin (4-12 g/day) for at least 4 days. Eighteen days after
the last dose of neomycin the jejunal morphology was restored
(Jacobson et al., 1960).
During the oral administration of 4-6 g neomycin/day for 6-8 days
plasma carotene concentrations were decreased in 6/8 patients despite
the administration of supplemental carotene (10 000 units/day). In
addition, d-xylose excretion in urine was decreased in 3/4 subjects.
Faecal fat excretion doubled during the treatment period in 1 patient
(Jacobson & Faloon, 1961).
Neomycin sulfate was administered orally (12 g/day for 4 days) as
well as by inlying tube directly into the jejenum and ilieum in 11
subjects. Urine and faeces were evaluated for fat, calcium, sodium,
potassium and nitrogen content. Steatorrhea was produced after oral
administration, but when neomycin was administered more distally, the
faecal fat content progressively diminished. Lowest urinary calcium,
sodium and potassium levels were measured after oral administration.
Faecal sodium, potassium and nitrogen levels were less affected by
this administration route, whereas the faecal calcium content was
greatest after jejunal instillation. The steatorrhea could not be
reversed by the administration of bile salts, sodium bicarbonate or
pancreatic enzymes (Gordon et al., 1968).
Three healthy male volunteers were orally administered 8 g
neomycin sulfate/day for 7 days. Lactose malabsorption was induced
after 3 days of treatment. Biopsy specimens from the small bowel
taken after 7 days of treatment showed slight villous blunting of the
mucosa and depressed disaccharidase activity. The lamina propria was
infiltrated with plasma cells and eosinophils. Enzyme levels and
histology of the mucosa and lamina propria of the small bowel returned
to normal 10 to 14 days after the treatment was stopped. No
treatment-related effects on stool lactic acids were observed (Cain
et al., 1968).
2.3.5 Special studies on microbiological effects
In a study with 37 hospitalized patients with various types of
intestinal lesions, the effect of oral neomycin treatment on bacteria
from the intestinal tract was determined. Treatment regimes of
neomycin administered prior to surgery (duration not stated) were as
follows: 1.5 g 4 times/day; 2 g 3 times/day; or 1 g every hour for
four doses the first day, then 1.5 g 4 times/day. After the
administration of neomycin the only clinical observations were
occasional nausea and vomiting. In stool specimens from patients
treated with 1.5 g 4 times/day (30 mg/kg bw/day) most of the aerobic
bacteria ( E. coli, A. aerogenes, S. faecalis, Proteus and
Pseudomonas) disappeared within 1´-4´ days, whereas anaerobic
organisms ( Bacteroides and Clostridium) remained. No resistant
strains of Mycrococcus pyopgenes were found. Similar results were
seen in patients receiving 2 g 3 times/day. In the group receiving 1
g hourly for four doses followed by 1.5 g 4 times/day, aerobic
bacteria were removed from the intestinal tract within two to three
days, while anaerobes ( Bacteroides and Clostridium) persisted
(Deering & Needham, 1953).
The intestinal flora of 14 patients hospitalized for non-
gastrointestinal diseases was studied before and after the use of
neomycin. Four patients received 4 g neomycin orally for 7 days and 10
patients were given 2 g neomycin for 6 days. The bacterial populations
of faecal specimens collected before, during and after neomycin
treatment were enumerated. A decrease in all bacterial species was
noted. Most affected were Enterococci, followed by E.coli,
lactose non-fermenters, Lactobacilli, Clostridia and Proteus
sp. Yeast and Klebsiellae were increased (Daikos et al., 1968).
Seven healthy adult volunteers received 1 g neomycin orally 3
times a day for 5 days (equivalent to 50 mg/kg bw/day). Fresh stool
samples were collected before, during and after treatment, and
bacterial counts recorded. Neomycin treatment did not affect
Bacteroides or Clostridia counts. E. coli counts were
significantly reduced in 2/7 volunteers (Arabi et al., 1979).
3. COMMENTS
The Committee considered data on pharmacokinetics, acute
toxicity, short-term and long-term toxicity, reproductive and
developmental toxicity, genotoxicity and carcinogenicity, effects in
humans and effects on antimicrobial activity. An evaluation report,
as requested for veterinary drugs with a long history of use (Annex 1,
reference 104) was also provided.
Neomycin is poorly absorbed after oral administration, whereas
after parenteral administration it is readily bioavailable. In
calves, oral absorption was estimated at 1-11%, depending on age. In
humans, up to 3% of an oral dose was recovered in urine, indicating
low absorption. Of the neomycin present in blood, 45-55% was bound to
plasma proteins in cows and ewes and the remainder was present in
nonionized form and may cross tissue barriers. After oral
administration the compound is mainly excreted unchanged in the
faeces. After parenteral administration neomycin is mainly excreted in
the urine.
Single doses of neomycin were slightly toxic to mice after oral
administration (LD50 = 2250 mg/kg bw), but single i.v. doses in mice
were highly toxic (LD50 <100 mg/kg bw).
Nephrotoxic effects were observed in mice after repeated s.c.
administration of 30-300 mg neomycin/kg bw/day, in guinea-pigs after
repeated s.c. doses of 10-60 mg neomycin sulfate/kg bw/day, and in
dogs after repeated i.m. doses of 24-96 mg neomycin/kg bw/day. No
kidney damage was observed in dogs receiving 100 mg/kg bw/day orally
for 6 weeks. Ototoxicity was observed after parenteral administration
of neomycin ranging from 25 to 150 mg/kg bw/day in guinea-pigs, and
20 to 80 mg/kg bw/day in cats. No ototoxic effects were observed in
guinea-pigs following oral administration of up to 10 mg neomycin
sulfate/kg bw/day for 90 days. In cats orally administered 6.25, 12.5
or 25 mg of neomycin/kg bw/day for one year, auditory function was not
affected, but upon histopathological examination changes in the organ
of Corti were reported at all dose levels.
The Committee concluded that, although ototoxicity was observed
in the one-year study in cats at the lowest dose tested (6.25 mg/kg
bw/day), this study was inadequate for the safety evaluation of
neomycin because of serious shortcomings in the histological technique
and the absence of a clear dose-related effect. It, however, accepted
the NOEL of 10 mg neomycin sulfate/kg bw/day, equivalent to 6 mg
neomycin/kg bw/day, for ototoxicity from the study in guinea-pigs.
Only a limited number of mutagenicity studies were available,
which had been poorly performed. The available in vitro
genotoxicity tests indicated that neomycin causes chromosomal
aberrations.
The tumour incidence was not increased in a two-year toxicity and
carcinogenicity study with rats orally administered neomycin up to a
dose level of 25 mg/kg bw/day. In the high-dose males only a slight
but statistically non-significant impairment of hearing was observed.
Because the Committee regarded the observed impairment of hearing as
treatment-related, the NOEL was 12.5 mg/kg bw/day.
In a multi-generation reproductive toxicity study in rats in
which neomycin was administered orally, no effects on reproductive
parameters were observed up to a dose of 25 mg/kg bw/day, which was
the highest dose administered. A teratogenicity study with an
unconventional protocol was conducted with F2b female rats from the
reproductive toxicity study. Neomycin was administered in the feed at
0, 6.25, 12.5 or 25 mg/kg bw/day from days 0-6 and 16-20 of gestation.
Dose levels were raised to 62.5, 125 or 250 mg/kg bw/day from days 6-
15 of gestation. No malformations, feto-toxicity or maternal toxicity
were observed.
Skin reactions due to hypersensitivity have been observed in
humans after the therapeutic use of neomycin. Nephrotoxic effects and
ototoxicity have been observed in humans after oral therapeutic use of
neomycin.
From several in vitro microbiological studies with different
bacteria, mostly isolated from humans, an MIC50 of 64 µg/ml was
derived for the most relevant sensitive bacterial organisms
( Escherichia coli and Lactobacillus spp.) under conditions of
high inoculum density. In human-flora-associated mice the NOEL for
antibacterial activity was 125 mg/kg bw/day. Studies on the effect of
neomycin on human gut flora in patients revealed effects at oral doses
>30 mg/kg bw/day.
Applying the formula developed at the thirty-eighth meeting of
the Committee (Annex 1, reference 97) an ADI based on anti-microbial
activity could be calculated as follows:
Concentration without effect daily faecal
of ADI on human gut flora (µg/ml)a x bolus (g)
Upper limit =
of ADI fraction of oral x safety x Weight of human (60kg)
dose availableb factorc
64 x 150
=
1 x 1 x 60
= 160 µg/kg bw
a The MIC50 value of 64 µg/ml was measured in the most relevant
sensitive species under conditions of high inoculum density. No
adjustment was deemed necessary.
b A conservative estimate of 100% availability to human gut flora
was selected. Experimental data were inadequate to correct for
inactivation of neomycin as a result of binding to gut contents.
c A substantial amount of data covering a variety of organisms,
including anaerobes isolated from the human gut, were available.
Also in view of the applied conservative factor for the availability
of neomycin to the gut flora a safety factor of 1 was adopted.
In reviewing the available toxicological and antimicrobial data
the Committee concluded that the toxicological data provided the most
appropriate endpoint for the evaluation of neomycin.
Only a limited set of genotoxicity tests was available, with gene
mutation studies in eukaryotic cells being absent. The available
information indicates that neomycin causes chromosomal aberrations.
However, the Committee noted that the long-term study in rats did not
provide evidence for a carcinogenic potential of neomycin.
The Committee established a temporary ADI of 0-30 µg/kg bw based
on the NOEL of 6 mg/kg bw/day for ototoxicity in the guinea-pig and a
safety factor of 200. The ADI was made temporary in view of the
deficiencies in the genotoxicity data.
5. REFERENCES
ARABI, Y., DIMOCK, F., BURDON, D.W., WILLIAMS, J.A. & KEIGHLEY, M.R.R.
(1979). Influence of neomycin and metronidazole on colonic microflora
of volunteers. J. Antimicrobial. Chemother., 5: 531-537.
ASCHBACHER, P.W. & FEIL, V.J. (1991). Fate of oral 14C Neomycin in
calves. USDA, ARS, Biosciences Research Laboratory, Farbo, ND.
J. Animal Science, 69(1): 733.
ASCHBACHER, P.W. & FEIL, V.J. (1994). Neomycin metabolism in calves.
J. Animal Science, 72: 683-689.
ATEF, M., EL-GENDI, A.Y.I., EL-SAYED, M.G.A. & A.M.M.AMER (1986).
Certain physico-pharmacologic properties of neomycin in chickens.
Arch. Geflügelk, 50(4): 132-135.
BAER, R.L. & LUDWIG, J.S. (1952). Allergic eczematous sensitization to
neomycin. Annals of Allergy, March-April: 136-137.
BEVAN, J.A. & THOMPSON, J.H. (1983). Introduction to principles of
drug action. Essentials of pharmacology, 3rd Ed. Harper and Row,
Philadelphia.
BREEN, K.J., BRYANT, R.E. LEVINSON, J.D. & SCHENKER, S. (1972).
Neomycin studies in man. Studies of oral and enema administration and
effect of intestinal ulceration. Ann. Intern. Med., 76: 211-218.
BROCKIE, P.H. (1951). Acute toxicity test with neomycin sulphate dated
2-22-1951. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
BRUMMETT, R.E., HALL, A.D. & RUSSELL, K.B. (1985). Ninety-day oral
neomycin sulfate (U-4,567) Ototoxicity study in the guinea-pig.
Technical report No. 7263/85/068 dated 23 october 1985. Submitted to
WHO by The Upjohn Company, Kalamazoo, MI, USA.
CAIN, C.D., REINER, E.B. & PATTERSON, M. (1968). Effects of neomycin
on disaccharidase activity of the small bowel. Arch. Intern Med.,
122: 311-314.
CALE , R.J. (1950). Memo dated 1950, subject : Toxicity neomycin
sulfate. Ssubmitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
CALNAN,C.D. & SARKANY, I. (1958). Contact dermatitis from neomycin.
Brit. J. Dermatol., 70: 435-445.
DAIKOS, G.K., KONTOMICHALOU, P. BILALIS, D. & PIMENDOU. L. (1968).
Intestinal flora ecology after oral use of antibiotics. Chemotherapy,
13: 146 - 160.
DEERING, W.H. & NEEDHAM, G.M. (1953). Effects of oral administration
of neomycin on the intestinal bacterial flora of man. Staff meeetings
of the Mayo Clinic, September 9, 502-507. Submitted to WHO by The
Upjohn Company, Kalamazoo, MI, USA.
DORNBUSCH, K., NORD, C.E. & DAHLBECK, A. (1975). Antibiotic
susceptibility of clostridium dpecies isolated from human infections.
Scand. J. Infect. Dis., 7: 127-134.
DURAN, S.P., VALERA, R.G., MANZANO, J.V. & MACHOTA, V. (1991).
Comparative in vitro susceptibility of Bacteroides and
Fusobacterium isolated from footrot in sheep to 28 antimicrobial
agents. J. Vet. Pharmacol. Therap., 14: 185-192.
EPSTEIN, S. (1956). Contact dermatitis from neomycin due to dermal
delayed (tuberculin-type) sensitivity. Dermatologica, 113(4): 191-
201.
EPSTEIN, S. (1965). Neomycin sensitivity and atopy. Dermatology,
130: 280-286.
EPSTEIN, S. & WENTZEL, F.J. (1962). Cross-sensitivity to various
"Mycins" Neomycin, Kanamycin, Streptomycin and Bacitracin: an
experimental study. Arch. Dermatol., 86: 183-194.
FEENSTRA, E.S. (1950). Interoffice memorandum of pathology report -
Chronic toxicity (s Mo.) of Neomycin sulfate #9084-10 in guinea-pigs
and dogs, dated 22 August 1950. Submitted to WHO by The Upjohn
Company, Kalamazoo, MI, USA.
FEENSTRA, E.S. (1954). Interoffice memorandum: Comparative
nephrotoxicity of neamine, neomycin B and neomycin C, Preliminary
report dated 22 September 1954. Submitted to WHO by The Upjohn
Company, Kalamazoo, MI, USA.
FEENSTRA, E.S. (1958). Unpublished technical acute toxicity i.p.
neomycin sulphate. dated 8 July 1958. Submitted to WHO by The Upjohn
Company, Kalamazoo, MI, USA.
FEENSTRA, E.S. (1959). Unpublished technical acute toxicity i.p.
neomycin sulphate. dated 19 January 1959. Submitted to WHO by The
Upjohn Company, Kalamazoo, MI, USA.
FIELDS, R.L. (1964). Neomycin ototoxicity. Arch. Otolaryngol., 79:
67-70. FINEGOLD, S.M., HARADA, N.E. & MILLER, L.G. (1967). Antibiotic
susceptibility Patterns as aids in classification and characterization
of gram-negative anaerobic bacilli. J. Bacteriol., 94(5): 443-350.
GORDON, S.J., HARO, E.N., PERS, I.C. & FALOON, W.W. (1968). Studies of
malabsorption and calcium excretion induced by neomycin sulfate.
Effect of intestinal site, bile salt and pancreatic enzymes. JAMA,
204: 129-134.
GRAY, J.E. (1964). Interoffice memorandum to E.S. Feenstra d.d. 6-5-
1964 LD50 neomycin sulfate submitted to WHO by The Upjohn Company,
Kalamazoo, MI, USA.
GREENBERG, L.H. & MOMARY, H. (1965). Audiotoxicity and nephrotoxicity
due to orally administered neomycin. JAMA, 194: 827-828.
HALL, A.D., SKINNER, P.J. & BARBIERS, A.R. (1983). A preliminary study
of the absorption of neomycin sulfate following oral administration to
guinea-pigs. Unpublished technical report No. 756-9610=83-001 dated
18-1-1983 from The Upjohn Company, Agricultural Research and
development laboratories, Kalamazoo Michigan , USA. Submitted to WHO
by The Upjohn Company, Kalamazoo, MI, USA.
HALLBERG, J.W., CHESTER, S.T., DAME, K.J., HORNISCH, R.E., TRAVIS,
M.A. & CORNELL, C.P. (1994). Effect of neomycin in milk on the
performance of cheese and yoghurt starter cultures. Unpublished
technical report No. 802-9690-94-001 dated 16 September 1994 from The
Upjohn Company, Agricultural Division. Submitted to WHO by The Upjohn
Company, Kalamazoo, MI, USA.
HALPERN, E.B. & HELLER, M.F. (1961). Ototoxicity of orally
administered neomycin. Arch. Otolaryngol., 73: 675-677.
HAWKINS, J.E. (1952). The ototoxicity of the neomycins. Trans. 11th
Conf. Chemother. of Tuberculosis, p. 189-191. Submitted to WHO by The
Upjohn Company, Kalamazoo, MI, USA.
HAWKINS, J.E., RAHWAY, N.J. & LURIE, M.H. (1953). The ototoxicity of
dihydrostreptomycin and neomycin in the cat. Ann. Otol. Rhin.
Laryngol., 62: 1128-1148.
HAZENBERG, M.P., VAN DE BOOM, M. BAKKER, M. & VAN DE MERWE, J.P.
(1983a). Effect of antibiotics on the human intestinal flora in mice.
Antonie van Leeuwenhoek, 49: 97-109.
HAZENBERG, M.P., VAN DE BOOM, M. BAKKER, M. & VAN DE MERWE, J.P.
(1983b). Binding to faeces and influence on human anaerobes of
antimicrobial aganets used for selective decontimination. Antonie van
Leeuwenhoek, 49: 111-117.
HAZENBERG, M.P., PENNOCK-SCHRODER, A.M., VAN DEN BOOM, M. & VAN DE
MERWE, J.P. (1984). Binding to and antibacterial effect ampicillin,
neomycin and polymyxin B on human faeces. J. Hyg.Camb., 93: 27-34.
HEATH, G.E. (1985). The pharmacokinetics of neomycin in the serum of
calves and young cross-bred swine. Thesus, University of Minnisota.
Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
HEWETT, G.R. (1990). Determination of the minimum Inhibitory
Concentration (MIC) of neomycin sulphate versus Salmonellae Species
and Escherichia coli isolated from calves, pigs and chicks.
Unpublished technical report No. 004-AHTR-9542-90-007 dated 3 May,
1990 from Agricultural Research and Development Laboratories, The
Upjohn Company U.K. Submitted to WHO by The Upjohn Company, Kalamazoo,
MI, USA.
HOEFFLER, E.H.L.K. & PULVERE, G. (1976). Antimicrobial susceptibility
of Propionibacterium acnes and related microbiological species.
Antimicrob. Ag. Chemother., 10(3): 387-394.
JACOBSON, E.D., PRIOR, J.T. & SYRACUSE, N.Y. (1960). Malabsorptive
syndrome induced by neomycin: morphological alterations in the jejunal
mucosa. J. Lab. Clin. Med., 56(2): 245-250.
JACOBSON, E.D. & FALOON, W.W. (1961). Malabsorptive efefcts of
neomycin in commonly used doses. JAMA, 175(3): 187-190.
JAJU, M., JAJU, M. & AHUJA, Y.R. (1986). Cytogenetic effect of
neomycin on human lymphocytes in vitro. Ind. J. Exp. Biol., 24:
595-598.
KAKUK, T.J. (1980). Neomycin sulfate: three-generation rat
reproductive teratology study. Technical report No. 756-9610-80-002
dated 30 November 1980, Agricultural Research and Development
Laboratories, The Upjohn Company. Submitted to WHO by The Upjohn
Company, Kalamazoo, MI, USA.
KAKUK, T.J. (1981). Neomycin sulfate: one-year tolerance study in the
domestic cat. Tecnical report No. 756-9610-81-001 dated 19 October
1981, Agricultural Research and Development Laboratories, The Upjohn
Company. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
KAKUK, T.J. (1982). Neomycin sulfate: lifetime feeding study in the
rat (Study #T-702)/Technical report No. 756-9610-82-001 dated 14
September 1982, Agricultural Research and Development Laboratories,
The Upjohn Company. Submitted to WHO by The Upjohn Company, Kalamazoo,
MI, USA.
KEEN, P. (1975). Some aspects of the pharmacology of antibiotics in
the cat and dog. J. Small Anim. Pract., 16: 767-773.
KILE, R.L., ROCKWELL, E.M. & SCHWARTZ, J. (1952). Use of neomycin in
dermatology. JAMA, 148(5): 339- 343.
KING, J.T. (1962). Severe deafness in an infant following oral
administration of neomycin. J. Med. Assoc. Georgia, 51: 530-531.
KUBINSKI, H., GUTZKE, G.E. & KUBINSKI, Z.O. (1981). DNA-cell-binding
(DCB) assay for suscpected carcinogens and mutagens. Mutat. Res.,
89: 95-136.
LINDSAY, J.R., PROCTOR, L.R. & WORK, W.P. (1960). Histopathological
inner ear changes in deafness due to neomycin in a human.
Laryngoscope, 70: 382-392.
MANNA, G.K. & BARDHAN, S. (1973). Effects of two antobiotics on the
chromosomes and mitotic frequency in the bone marrow cells of mice.
Chromosomes Today, 4: 277-282.
MILLER, L.G. & FINEGOLD, S.M. (1967). Antibacterial sensitivity of
Bifidobacterium (Lactobacillus bifidus). J. Bacteriol., 93(1): 125-
130.
MOELLERING, R.C. (1983). In vitro antibacterial activity of the
aminoglycoside antiobiotics. Rev. Infect. Dis., 5(2): S212-S231.
NELSON, A.A., RADOWSKI, J.L. & HAGAN, E.C. (1951). Renal and other
lesions in dogs and rats from intramuscular injection of neomycin.
Fed. Proc. 10(1): 366-367.
PIRILA, V., & ROUHUNKOSKI, S. (1962). The pattern of cross-sensitivity
to neomycin. Dermatologica, 125: 273-278.
PIRIZ, S., CUENCA, R. VALLE, J. & VADILLO, S. (1992). Susceptibilities
of anaerobic bacteris isolated from animals with ovine foot rot to 28
antimicrobial agents. Antimicrob. Ag. Chemother., 36(1): 198-201.
POTH, E.J., MARTIN, R.G., FROMM, S.M., WISE, R.I. & HSANG, C.M.
(1951). A critical analysis of neomycin as an intestinal antiseptic.
Tex. Rep. Biol. Med., 9: 631.
POWELL, L.W. & HOOKER, J.W. (1956). Neomycin nephropathy. JAMA,
160: 557-560.
REINBOLD, G.W. and REDDY, M.S. (1974). Sensitivity or resistance dairy
starter and associated microorganisms to selected antibiotics.
J. Milk Food Technol., 37(10): 517-521.
REDDY, M.S., REINBOLD, G.W. & WILLIAMS, F.D. (1973). Inhibition of
propionibacteria by antibiotic and antimicrobial agents. J. Milk Food
Technol., 36(11): 564-569.
RISKAER, N., CHRISTENSEN, E. PETERSEN & WEIDMAN, H. (1956). The
otoxicity of neomycin. Experimental investigations. Acta
Otolaryngol., 46: 137-152.
SCHWEINBURG, F.B., JACOB, S. & RUTENBURG, A.M. (1952). Effect of oral
Neomycin on normal intestinal flora of dogs and man. Proc. Soc. Expr.
Biol. & Med., 335-338.
SHEALY, Y.F. (1956). Technical unpublished report TUC No. U-4567 of
the acute toxicity of neomycin sulphate dated 6 July 1956. Submitted
to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SIDI, E., HINCKY. M. & LONGUEVILLE, R. (1958). Cross-sensitization
between neomycin and streptomycin. J. Invest. Dermatol., 30: 225-
231.
SOZZI, T. & SMILEY, M.B. (1980). Antibiotic resistance of Yogurt
starter cultures Streptoccus thermophilus and Lactobacillus
bulgaricus. Appl. Environm. Microbiol., 40(5): 862-865.
SWOAP, O.F. (1949a). Memo dated 12-2-1949, subject: Toxicity studies
on neomycin. Submitted to WHO by The Upjohn Company, Kalamazoo, MI,
USA.
SWOAP, O.F. (1949b). Memo dated 12-19-1949, subject: Toxicity studies
on neomycin SO4. Submitted to WHO by The Upjohn Company, Kalamazoo,
MI, USA.
SWOAP, O.F. (1950a). Memo on subject: Toxicity studies on SO4.
Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1950b). Memo dated 3-24-1950, subject: Toxicity: neomycin
SO4. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1950c). Memo dated 4-6-1950, subject: Toxicity: Neomycin
sulfate. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1950d). Memo dated 4-6-1950, subject: Toxicity: neomycin
sulfate. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1950e). Memo dated 6-16-1950, subject: Toxicity: neomycin
sulfate. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1950f). Memo dated 11-16-1950, subject: Toxicity:
neomycin SO4. Submitted to WHO by The Upjohn Company, Kalamazoo, MI,
USA.
SWOAP, O.F. (1950g). Memo dated 12-1-1950, subject: Neomycin toxicity
testing. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1950h). Memo dated 12-4-1950, subject: Toxicity: neomycin
SO4. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1950i). Memo dated 12-8-1950, subject: Toxicity: neomycin
SO4. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1950j). Memo dated 12-21-1950, subject: Toxicity:
neomycin SO4. Submitted to WHO by The Upjohn Company, Kalamazoo, MI,
USA.
SWOAP, O.F. (1950k). Memo dated 12-21-1950, subject: Toxicity:
neomycin SO4. Submitted to WHO by The Upjohn Company, Kalamazoo, MI,
USA.
SWOAP, O.F. (1951a). Memo dated 1-17-1951, subject: Toxicity: neomycin
SO4. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1951b). Toxicology report dated 5-8-1951 on neomycin
sulfate. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1951c). Toxicology report dated 7-2-51 on neomycin
sulfate. Submitted to WHO by the Upjohn Company, Kalamazoo, MI; USA.
SWOAP, O.F. (1952a). Toxicology report dated 5-13-1952 on neomycin
(lot 91-cat-6). Submitted to WHO by The Upjohn Company, Kalamazoo, MI,
USA.
SWOAP, O.F. (1952b). Toxicology report dated 7-3-1952 compound: Bulk
powder neomycin sulfate ( from resin process). Submitted to WHO by The
Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1952c). Toxicology report neomycin sulphate dated 6-10-
1952. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1952d). Toxicology report neomycin sulphate dated 6-10-
1952a. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1952e). Toxicology report Bulk powder neomycin sulphate
(from resin process) dated 7-3-1952. Submitted to WHO by The Upjohn
Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1952f). Toxicology report I: Bulk powder neomycin
sulphate (from resin process) dated 25 september 1952. Submitted to
WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1952g). Toxicology report II: Bulk powder neomycin
sulphate (from resin process) dated 25 september 1952. Submitted to
WHO by The Upjohn Company, Kalamazoo, MI 49001.
SWOAP, O.F. (1952h). Toxicology report III: Bulk powder neomycin
sulphate (from resin process) dated 25 september 1952 submitted to WHO
by The Upjohn Company, Kalamazoo, MI 49001.
SWOAP, O.F. (1953a). Toxicology report neomycin sulphate dated 12-2-
1953 submitted to WHO by The Upjohn Company, Kalamazoo, MI 49001.
SWOAP, O.F. (1953b). Interoffice memorandum dated 2-18-1953 subject:
meomycin B Submitted to WHO by The Upjohn Company, Kalamazoo, MI
49001.
SWOAP, O.F. (1954a). Memo acute toxicity no 983 Neomycin sulfate B
dated 24 September 1954, submitted to WHO by The Upjohn Company,
Kalamazoo, MI 49001.
SWOAP, O.F. (1954b). Interoffice memorandum - parallel toxicity tests
on neomycin B sulfate samples (U-4567) dated 30 September 1954,
submitted to WHO by The Upjohn Company, Kalamazoo, MI 49001.
SWOAP, O.F. (1957a). Memo - acute toxicity neomycin sulphate dated 1
November 1957, submitted to WHO by The Upjohn Company, Kalamazoo, MI,
USA.
SWOAP, O.F. (1958). Memo - acute toxicity neomycin sulphate Po.
Blended USP. 21 march 1958. Submitted to WHO by The Upjohn Company,
Kalamazoo, MI, USA.
THURN, K.K., BAKER, K.D., GREENING, R.C. & KOTARSKI, S.F. (1994).
Minimum inhibitory concentrations of neomycin sulfate against
bacterial species frequently isolated from the human gastrointestinal
tract. Unpublished technical report No. 802-7928-94-001 from The
Upjohn Company, Upjohn Laboratories, Kalamazoo, MI USA 49001.
Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
VAN DER BROOK, M.J. (1949). Memo dated 6-15-1949 about toxicity on
neomycin. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
VERINGA, E.M. & VAN DER WAAIJ, D. (1984). Biological inactivation by
faeces of antimicrobial drugs applicable in selective decontamination
of the digestive tract. J. Antimicrob. Chemother., 14: 605-612.
WAGMAN, G.H., BAILEY, J.V. & WEINSTEIN, M.J. (1974). Binding of
aminoglycosides to feces. Antimicrob. Ag. Chemother., 6(4): 415-
417.
WAISBREN, B.A. & SPINK, W.W. (1950). A clinical appraisal of neomycin.
Ann. Int. Med., 33: 1099-1119.
ZIV, G. & SULMAN, F.G. (1972). Binding of antibiotics to bovine and
ovine serum. Antimicrob. Ag. Chemother., 2(3): 206-213.
ZIV, G. & SULMAN, F.G. (1974). Distribution of aminoglycoside
antibiotics in blood and milk. Res. Vet. Sci., 17: 68-74.
2. BIOLOGICAL DATA
2.1 Biochemical aspects
2.1.1 Absorption, distribution and excretion
2.1.1.1 Guinea-pigs
Groups of 4 male guinea-pigs were administered single oral doses
of 5, 10 or 100 mg/kg bw neomycin B sulfate. Serum was collected 1,
2, 3, and 4 hours after treatment. Neomycin concentrations of 1.5 and
0.45 µg/ml were measured at 1 and 2 hours after dosing with 100 mg/kg
bw, respectively. Serum concentrations of neomycin were below
detectable levels (< 0.10 µg/ml) in the low- and mid-dose groups at
all time points, and in the high-dose group at 3 and 4 hours post-
administration (Hall et al., 1983).
2.1.1.2 Chickens
Lohman chickens (14 total, weighing approximately 2 kg each) were
administered a single oral dose of 20 mg neomycin/kg bw. Neomycin
could not be detected in blood samples collected up to 8 hours post-
administration using a microbiological assay (detection limit not
specified) (Atef et al., 1986).
After a single i.v. administration of 20 mg/kg bw neomycin to
five Lohman chickens, the blood concentration curve showed a
biexponential decline with a T´ of about 6 hours for the elimination
phase and an AUC of approximately 196 µg/ml/h. After a single i.m.
administration of 20 mg/kg bw to 14 chickens, the peak blood level
(Cmax) was approximately 17 µg/ml and the mean maximum concentration
was reached 40 minutes after administration. The AUC was approximately
132 µg/ml/h. The bio-availability following i.m. administration was
approximately 70% (Atef et al., 1986).
In 22 Lohman chickens administered neomycin i.m. at 20 mg/kg bw
twice daily for 5 days, plateau levels of neomycin (about 6 µg/ml)
were retained for 1-4 days. Neomycin concentrations were detected in
the spleen for 3 days, in liver and lung for 6 days, and in kidney for
10 days post-injection (Atef et al., 1986).
2.1.1.3 Sheep
Serum and milk concentrations of neomycin were determined in
lactating Awassi ewes (4/group) after a single i.v. (20 mg/kg bw) or
i.m. injection (10 mg/kg bw). Neomycin was assayed micro-biologically
using the cylinder cup method (sensitivity limit 1 µg/ml). After i.v.
administration the T´ was approximately 3 hours and distribution
equilibrium was reached within 20 min. After i.m. administration peak
concentrations were reached after 1 hour. Neomycin was not detectable
in serum 12 hours after treament. A very small fraction of the dose
(0.01%-0.02%) was recovered in milk secreted from normal or irritated
glands (in which the left-side glands of the udder were infused with
150 ml of hypertonic NaCl solution 24 hours before treatment) during
the 12 hours after treatment. Peak milk concentrations of neomycin
following i.v. or i.m. treatment were less than 2 µg/ml (Ziv & Sulman,
1974).
2.1.1.4 Pigs
Two groups (6 pigs/group) of Yorkshire crossed weanling pigs (10
weeks old, weighing 10 to 15 kg) were orally administered 22 mg
neomycin sulfate/kg bw/day for 5 consecutive days. Group 1 consisted
of 3 males and 3 females, while group 2 had 5 males and 1 female. In
addition to the oral neomycin treatment, pigs in the second group
received diets supplemented with sodium sulfate at a rate of 10 g/kg
feed. Serum neomycin concentrations were measured up to 96 hours after
dosing. The mean peak serum concentration (approximately 0.2 µg/ml)
of neomycin was reached in the fourth hour in pigs fed the normal
ration. For pigs receiving the supplemented diets, the mean peak
serum concentration (approximately 0.1 µg/ml) was reached at 8 and 24
hours after dosing (Heath, 1985).
In another study by the same author, a single i.v. dose of 22
mg/kg bw neomycin sulfate was administered to 6 (3/sex) 10-month old
pigs. A peak mean serum level of approximately 30 µg/ml was detected
one hour after dosing, which decreased to 0.01 µg/ml by 72 hours
(Heath, 1985).
A single i.m. dose (22 mg/kg bw) of neomycin sulfate was
administered to 12 female pigs weighing 20 to 50 kg. A peak mean
serum level of approximately 40 µg/ml which was reached one hour after
dosing, decreased to 0.02 µg/ml after 72 hours (Heath, 1985).
2.1.1.5 Cattle
Ten castrated Holstein calves (2 to 6 months of age, weighing 80
to 180 kg) were orally administered 22 mg neomycin sulfate/kg bw/day
for 5 days. Serum concentrations were determined up to 96 hours after
dosing. Mean serum concentrations ranged from 0-0.06 µg/ml during the
1-96-hour dosing period (Heath, 1985).
A single i.v. dose (22 mg/kg bw) of neomycin sulfate was
administered to 10 castrated Holstein calves (2 to 6 months old,
weighing 70 to 170 kg). A peak mean serum concentration of
approximately 19 µg/ml which was detected one hour after dosing,
decreased to 0.03 µg/ml by 72 hours (Heath, 1985).
Four male Holstein calves (3 to 60 days old) were given a single
oral dose of 30 mg 14C-neomycin/kg bw and then killed after 96 hours.
The distribution of 14C in excreta and tissues was determined by mass
spectrophotometric analysis. Most of the radioactivity was recovered
in faeces (85-97%). The radioactivity found in urine decreased with
increasing age of the animal, from 11 to 0.5% of the administered
dose. Radioactivity found in the kidneys, liver and muscle of calves
at 3 days of age represented 55, 1.93 and 0.09 ppm of neomycin
equivalents, respectively. At least 90% of the 14C in the kidneys of
3-day old calves was present as neomycin. Seventy to 88% of the 14C
present in faeces of all calves was also identified as neomycin
(Aschbacher & Feil, 1991, 1994).
Serum and milk concentrations of neomycin were measured in 4
lactating Israeli-Friesian dairy cows following administration of a
single i.m. dose (10 mg/kg bw). Neomycin was assayed micro-
biologically by the cylinder cup method (sensitivity limit 1 µg/ml).
Peak serum concentrations were reached after 1 hour. Neomycin was not
detectable in serum 12 hours after treament. A very small fraction of
the dose (0.016%-0.022%) was recovered in milk secreted from normal or
irritated glands (in which the left-side glands of the udder were
infused with 150 ml of hypertonic NaCl solution 24 hours before
treatment) during the 12 hours after treatment. Peak milk
concentrations of neomycin were less than 2 µg/ml (Ziv & Sulman,
1974).
2.1.1.6 Humans
An oral dose of 1.5 g neomycin/day was administered to a 2- year
old female tuberculosis patient for 15 consecutive days. A nine-month
old male tuberculosis patient received 200 mg neomycin/day orally for
80 days. Both patients were diagnosed with miliary tuberculosis and
tuberculous meningitis. A maximum neomycin serum concentration of
approximately 5.0 µg/ml was achieved in both patients. Cerebrospinal
fluid concentrations of 1.25 and 2.5 µg/ml were measured in the female
and male patient, respectively (Waisbren & Spink, 1950).
Poth et al. (1951) reported serum concentrations ranging from
not detectable to <80 µg/ml in patients treated with oral neomycin
(6 g/day) for 3 days. The majority of the administered dose was
excreted in the faeces unchanged. Only 3% of the dose was recovered
from the urine.
The absorption and excretion of a 2 g oral or rectally
administered dose of neomycin sulfate was studied in 10 normal
subjects (healthy physicians who had no history of renal or liver
disease) and in patients with liver disease, peptic ulcer, regional
enteritis, or active ulcerative colitis. Urinary excretion (0.58%) of
neomycin and serum neomycin concentrations over 48 hours were similar
in all groups and by both routes. The percentage of the neomycin dose
excreted in the faeces following oral or rectal administration was
comparable (approximately 99%) (Breen et al., 1972).
2.1.2 Biotransformation
Aminoglycosides as a class are not metabolized in animals (Bevan
& Thompson, 1983) and are mostly excreted unchanged (Aschbacher &
Feil, 1994; Keen, 1975).
2.1.3 Special studies on binding to macromolecules
Lactating Israeli-Freisian cows (2 animals) and Awassi ewes (4
animals) were given single doses of 20 mg/kg bw neomycin i.m. or i.v.
Resulting serum concentrations ranged from 5-10 µg/ml. Serum protein
binding, determined by equilibrium dialysis and ultrafiltration
methods, was approximately 45-50% and 50-55% for cows and ewes,
respectively (Ziv & Sulman, 1972).
2.2 Toxicological studies
2.2.1 Acute toxicity studies
The results of acute toxicity studies after oral, i.v., s.c. or
i.p. administration of neomycin are summarized in Table 1.
2.2.2 Short-term toxicity studies
2.2.2.1 Cats
Groups of cats (8/sex/group) were orally dosed (gelatin capsule)
with 0, 6, 12 or 25 mg technical neomycin sulfate/kg bw/day for 1
year. The actual administered doses were found by chemical analysis
to be 72% of the intended doses. Clinical signs, auditory and
vestibular examinations, body weight, haematology, serum chemistry,
urinalysis, organ weights, macroscopy and histopathology were
evaluated.
The cause of the death of 7 cats during the study was not
considered to be treatment-related. The RBC counts were significantly
decreased in males at the highest dose at weeks 26 and 52. Blood urea
nitrogen levels were significantly increased in high-dose males at 13,
26 and 52 weeks, but no histopathological evidence of kidney damage
was observed. In the high-dose males at termination, potassium,
chloride and alkaline phosphatase were decreased, and cholesterol
levels were increased. Relative spleen and pancreas weights were
significantly decreased at all dose levels in male cats but without a
dose-related trend. Bone marrow hypoplasia was seen histogically in
the high-dose group (3/6 males and 4/8 females) (Kakuk, 1981).
Table 1. Acute toxicity of neomycin
Species Sex Route Substance Purity LD50 Reference
(mg/kg bw)
Mouse ? oral neomycin sulfate ? approx. Swoap, 1952c,d
2250-2500
Mouse M&F oral neomycin sulfate bulk 900 µg/mg 2250-2298 Swoap, 1952f,g,h
Mouse M&F oral neomycin sulfate (bulk 900-1000 >2500 Swoap, 1952b
powder from resin process) µg/mg
Mouse ? i.v. neomycin sulfate ? 40-158 Vander Brook, 1949;
Swoap, 1949a,b;
1950a,b,c,d,e,i,j,k;
1951a,b; Cale, 1950;
Gray, 1964
Mouse M i.v. neomycin sulfate ? 64.6-107 Brockie, 1951; Cale,
1950; Swoap,
1950f,g,h
Mouse M&F i.v. neomycin sulfate ? >50 Swoap, 1953a
Mouse ? i.v. neomycin A hydrochloride ? 97.6 Swoap, 1949a
Mouse M&F i.v. neomycin in HCH ? 74-115 Swoap, 1952a
Mouse ? i.v. neomycin sulfate bulk 900 µg/mg 110 Swoap, 1952e
Mouse M&F i.v. neomycin sulfate (bulk 910 µg/mg 100 Swoap, 1952b
powder from resin process)
Mouse ? s.c. neomycin sulfate ? 550 Vander Brook, 1949;
Swoap, 1950c,d,e
Table 1 (contd)
Species Sex Route Substance Purity LD50 Reference
(mg/kg bw)
Mouse ? s.c. neomycin sulfate ? 400 Brockie, 1951
Mouse ? s.c. neomycin A ? 470 Vander Brook, 1949
hydrochloride (51)
Mouse ? i.p. neomycin sulfate ? 274 Gray, 1964
Mouse M&F i.p. neomycin sulfate 690 µg/mg 310-457 Feenstra, 1958a;
Swoap, 1957a
Mouse M&F i.p. neomycin B sulfate ? 277-389 Swoap, 1954a,b;
Shealy, 1956
Mouse M&F i.p. neomycin B sulfate 1000 µg/mg 533 Swoap, 1953c
Shealy, 1956
Mouse M&F i.p. neomycin sulfate Po. 690 µg/mg 356 Swoap, 1958
blended USP
Mouse M&F i.p. neomycin sulfate bulk 658 µg/mg 248 Feenstra 1959
2.2.3 Long-term toxicity/carcinogenicity studies
2.2.3.1 Rats
Eight groups of Sprague-Dawley (SD)BR F1a weanling rats (4 groups
of males, 4 groups of females, 54-56/group) were administered neomycin
sulfate via the diet at 0, 6.25, 12.5 or 25 mg/kg bw/day until
terminal sacrifice. The test animals were offspring from the
F0generation that were mated after consuming similar levels of
neomycin in the diet for 11 weeks (see section 2.2.4). After 52 weeks
of treatment 10 rats/sex/group were selected for an interim kill and
evaluation. All male groups were killed after 104 weeks when the
control group survival reached 20%. When survival in female groups
reached 20%, the remaining animals of the group were sacrificed (27 to
30 months). Clinical signs, body weight, food consumption,
haematology, clinical chemistry, urinalysis, ophthalmoscopy, auditory
and vestibular tests, organ weight and histopathology were evaluated
in control and high-dose male and female rats.
To assess the possible effects of neomycin on the vestibular and
auditory functions an additional group (6/rats/sex, weanlings selected
from the control group in the reproduction study) was administered
neomycin sulfate s.c. at 100 mg/kg bw/day. Auditory and vestibular
function tests were scheduled weekly until study termination. When
all rats showed hearing loss (week 14), they were killed. Tissues of
the inner ear were preserved, but histopathological examinations were
not carried out.
Up to week 84, overall survival was about 84% and 92% for males
and females respectively. At the end of the study high mortality was
observed in all groups (33/44, 27/45, 29/46 and 30/45 for males and
33/46, 34/45, 34/44 and 35/45 for females at 0, 6.5, 12.5 and 25 mg/kg
bw/day, respectively). Female body weights were dose-relatedly
increased during the first three weeks of the study. Although not
statistically significant 3/15 rats at 25 mg/kg bw/day showed
hearing loss at the end of the study. No treatment-related effects
were observed in any of the other parameters evaluated. There was no
evidence of carcinogenicity. The NOEL was 12.5 mg/kg bw/day (Kakuk,
1982).
2.2.4 Reproductive toxicity studies
2.2.4.1 Rats
In a 3-generation reproductive toxicity study groups of Sprague-
Dawley (SD)BR rats (40-20/sex/group) were administered neomycin
sulfate via the diet at 0, 6.25, 12.5 or 25 mg/kg bw/day. After 11
weeks F0 generation rats were mated to produce F1a offspring which
were subsequently continued on neomycin sulfate in the life-time
feeding study described in section 2.2.3. F0 animals were bred a
second time to produce F1b offspring for use in the reproduction study
(through F3b litters). Through all generations no treatment-related
effects were observed in any of the parameters evaluated. The NOEL was
25 mg/kg bw/day (Kakuk, 1980).
2.2.5 Special studies on embryotoxicity and teratogenicity
2.2.5.1 Rats
Groups of 20 pregnant Sprague-Dawley (SD)BR rats (F2b females
from the reproductive toxicity study) were maintained on the same dose
regimen of 0, 6.25, 12.5 or 25 mg/kg bw/day (see section 2.2.4). From
gestation days 6-15, doses were increased to 0, 62.5, 125 or 250 mg/kg
bw/day. From gestaton days 16-20, doses were returned to 0, 6.25,
12.5 or 25 mg/kg bw. Dams were killed on day 20 of gestation. No
evidence of maternal toxicity, fetotoxicity or teratogenicity was
observed (Kakuk, 1980).
2.2.6 Special studies on genotoxicity
The results of the available genotoxicity studies on neomycin are
summarized in Table 2.
2.2.7 Special study on nephrotoxicity
2.2.7.1 Mice
Ten mice/group were given s.c. doses of 0, 30, 100, 300, 600 or
1000 mg/kg bw/day neomycin A (neamine), neomycin B or neomycin C for
14 days. None of the mice at the 2 highest doses survived 14 days.
Two mice in the 1000 mg/kg bw/day neamine group died.
Histopathological examination of the kidneys was performed. Based on
lesion indices the degree of nephrotoxicty was established. Neomycin
B and Neomycin C were about equally nephrotoxic. The observed
nephrotoxicity in the neamine groups was about 50% of that observed in
the other neomycin groups (Feenstra, 1954).
2.2.7.2 Guinea-pigs
Guinea-pigs (3/sex/group) were administered 10, 20, or 60 mg
neomycin sulfate/kg bw/day for 3 months (route not specified). One
female was kept as a control. Histopathological evaluation of the
kidney revealed subacute to chronic focal interstitial nephritis
associated with degeneration and necrosis at all doses, with a dose-
related increase in severity (Feenstra, 1950).
Table 2. Results of genotoxicity studies on neomycin
Test system Test object Concentration Results Reference
In vitro
Chromosome human 20, 40 and 80 µg/ml positivea,b Jaju et al., 1986
aberration assay lymphocytes
SCE test human 20, 40 and 80 µg/ml negativeb Jaju et al., 1986
lymphocytes
In vivo
Cytogenetic Mice bone 50 mg/kg bw positiveb,c Manna & Bardhan,
assay marrow 1973
a At doses that significantly inhibit the progression of the cell cycle.
b No positive control group was used.
c Test was not performed to current standards, i.e., results from 12 fixation
times are combined in 6 groups and number and sex of animals not stated.
Mitotic frequency was decreased; therefore, it was concluded that neomycin
reached the bone marrow.
2.2.7.3 Dogs
Six dogs (3/group) were administered 20 or 60 mg neomycin
sulfate/kg bw/day for 88 days (route not specified). All 3 dogs in
the high-dose group died after 14, 16 and 21 days. One low-dose dog
survived. The other 2 died after 21 and 45 days. Urine samples from
all dogs were taken before and after the beginning of treatment and
analyzed for albumin, blood and the presence of casts.
Histopathological examinations of kidneys showed degeneration,
necrosis and focal interstitial nephritis in all 6 dogs (Feenstra,
1950).
Twelve dogs were injected intramuscularly with 24, 48, or 96
mg/kg bw/day neomycin. At the highest dose all dogs died within 1-3
weeks. Blood urea nitrogen was increased and renal function impaired
as shown by decreased phenolsulfonphthalein excretion.
Histopathological evaluation of kidneys revealed renal tubular damage
characterized by marked epithelial necrosis in the proximal convoluted
tubules. Moderate changes in bone marrow and marked congestion of the
liver were also found. Inflammation at injection sites was also
noted. At the mid-dose the severity of effects were described as
intermediate. Dogs exposed to 24 mg/kg bw/day were killed and
examined after 1 month. The severity of renal damage in this group
was described as slight with increased granularity and occasional
desquamation of epithelial cells being most evident (Nelson et al.,
1951).
No kidney damage was observed in dogs (number/sex/group not
stated) orally dosed with 100 mg neomycin/kg bw/day for 6 weeks based
on urinalyses and gross and histopathological examinations of kidneys.
No other abnormalities were observed (Poth et al., 1951).
2.2.8 Special studies on ototoxicity
2.2.8.1 Guinea-pigs
Groups of 3 guinea-pigs were administered i.m. doses of 25, 50,
100, or 150 mg neomycin/kg bw/day for 30 to 60 weeks. Parameters
evaluated included vestibular function, auditory function (Preyer's
reflex) and histolopathological examination of labyrinths and central
nervous systems.
One guinea-pig in the high-dose group died after 22 days on test.
Vestibular function was reported as normal or slightly impaired across
all treatment groups with no dose-response relationship. Preyer's
reflex was abolished in all guinea-pigs receiving 100 and 150 mg/kg
bw/day. Histopathological examinations of animals in which the
Preyer's reflex was abolished revealed marked destruction of hair
cells and sometimes complete destruction of the organ of Corti.
Animals with intact hearing had normal cochleae, cristae, and maculae.
Reversible as well as irreversible degeneration of the ganglion cells
was seen in animals with abolished hearing, while animals with intact
hearing showed no definite pathological changes (Riskaer et al.,
1956) .
Hearing was not affected (determined by audiometry) after the
installation of 3 mg/kg bw neomycin into the middle ear of 18 guinea-
pigs. Six of the test animals had either one or both tympanic
membranes perforated prior to treatment (Riskaer et al., 1956).
Groups of guinea-pigs (50/sex/group) were orally admini-stered
neomycin B sulfate at 0, 1, 5, or 10 mg/kg bw/day for 90 days. Two
positive control groups (20/sex/group) received 10 or 100 mg/kg bw/day
s.c. for 90 and 34 days, respectively. Parameters evaluated included
clinical signs, body weight, auditory function test (Preyer pinna
reflex), gross necropsy, and histopathology (including cochleae to
score the loss of hair cells from the organ of Corti).
At 100 mg/kg bw/day s.c., ototoxic changes in the Preyer pinna
reflex thresholds and cochlear hair cell counts were observed. These
changes were not seen in the low-dose s.c. group nor in any of the
groups after oral administration. The NOEL for orally administered
neomycin in this study was 10 mg/kg bw/day (Brummett et al., 1985).
2.2.8.2 Cats
A clinical neomycin formulation (containing mostly neomycin B
sulfate), neomycin A hydrochloride and neomycin B sulfate were
administered s.c. to groups of cats (number/sex/group not stated) in
daily doses of 80 mg/kg bw/day for 5 or 15 days. The clinical
formulation was also administered in doses of 20, 40, or 100 mg/kg
bw/day s.c. for periods of 90, 60 and 30 days, respectively. Crude
neomycin (about 70% pure) was orally administered at 2 daily doses of
500 mg/kg bw (1 g/animal/day) for 30 days. Vestibular function was
studied by electrical recording of nystagmus evoked by rotating the
animal on a motor-driven turntable. Hearing ability was followed and
the cochlear function was studied electrophysically.
Histopathological examination of the kidneys was performed of all
cats.
Vestibular function was affected only in cats receiving the
highest dose of the clinical formulation (100 mg/kg bw/day) for 30
days. One of these cats showed a gradual loss of nystagmus which was
entirely absent by day 35, 5 days after the last treatment. Depression
of cochlear function was observed in all groups of cats and was most
severe in cats receiving the clinical preparation s.c. Degeneration
of external hair cells in the organ of Corti and internal hair cells
was also observed. A dose-related increase in the severity of damage
to renal tubular epithelium occurred in all cats receiving the
clinical preparation s.c. and in cats orally dosed with crude neomycin
(Hawkins, 1952; Hawkins et al., 1953).
Ototoxicity was studied in 5, 8, 3, and 4 cats who received oral
doses of 0, 6.25, 12.5, or 25 mg neomycin/kg bw/day, respectively, for
1 year. No evidence of auditory or vestibular dysfunction was
observed. In surface preparations of the organ of Corti
(cytocochleograms) ototoxicity was present microscopically as loss of
outer hair cells from the extreme lower portion of the basal turn of
the cochlea. Severe ototoxicity was observed in 3/4 high-dose cats.
Hair cell loss of a lesser degree was also observed in 7/8 and 1/3
cats in the low- and mid-dose groups, respectively (Kakuk, 1981). Due
to serious shortcomings in the histological technique and the absence
of a clear dose-related effect, the Committee considered this study
inadequate for the safety evaluation of neomycin.
2.2.9 Special studies on irritation and sensitization
No significant irritation was observed 24 hours after the
intrapleural administration of single doses of solutions of 1 ml
neomycin sulfate (0-100 mg/ml) to guinea-pigs (3-4/dose) (Swoap,
1951c).
A group of 9 neomycin-sensitive guinea-pigs was evaluated with
the patch test for cross sensitivy to kanamycin, streptomycin,
dihydrostreptomycin and bacitrin. Positive results were obtained for
kanamycin (1/9) and streptomycin (8/9) (Epstein & Wenzel, 1962).
2.2.10 Special studies on microbiological effects
Neomycin is active against most gram-positive and gram-negative
rods, many gram-positive cocci, and such acid-fast pathogens as
Mycobacterium tuberculosis.
Neomycin reacts with 30S ribosomal subunits of procaryotic cells
by electrostatic attraction causing a change in the conformation of
the ribosomal binding protein. This results in mRNA reading errors
and disrupted protein synthesis.
2.2.10.1 In vitro
Minimum Inhibitory Concentration (MIC) values for different
bacterial strains obtained from animal or human isolates are listed in
Tables 3 and 4, respectively.
In a special study, strains of various bacterial genera, mostly
of human origin, were tested for their susceptibility to neomycin
sulfate. MIC values were estimated on two agar types, Wilkens
Chalgren/glucose medium (WCG) and supplemented blood medium (SB) with
2 inoculum densities. Estimations were made under anaerobic and
aerobic conditions (E. coli) by the agar dilution method. The
results are listed in Table 5 (Thurn et al., 1994).
The adsorption of neomycin to dog faeces was calculated as the
difference between the amount of neomycin added to dilute suspension
of dog faeces and the amount of neomycin measured (microbioloigal
assay) in the supernatant after the mixture was incubated and
centrifuged. About 75% adsorption of neomycin was observed. After
acid extraction 47% of the added neomycin was still bound to the
faecal solids (Wagman et al., 1974).
Several concentrations of neomycin were evaluated for adsorption
to human faeces. Faecal samples were obtained from 8 healthy human
volunteers. The binding of neomycin to the faeces was calculated as
the difference between the amount added to a dilute suspension of
faeces and the amount measured (micro-biological assay) in the
supernatant after the mixture was incubated for 1 hour and
centrifuged. Approximately 83-98% faecal binding was observed
(Hazenberg et al., 1983b, 1984).
Neomycin solutions of approximately 0.1-30 mg/ml were mixed with
faecal suspensions prepared from faeces of 8 healthy human volunteers.
Neomycin antimicrobial activity (tested with Enterobacter cloacae)
remaining in the supernatants was measured and used for calculating
the "% inactivation" relative to the amount of added neomycin. The
percentage of added neomycin that was biologically inactivated
decreased with increasing concentrations of neomycin. Nearly 100%
inactivation due to binding occurred when the ratios of neomycin to
faecal weight were < 5 mg neomycin to 1 g wet weight of faeces in an
incubation mixture (Veringa & Van der Waaij, 1984).
2.2.10.2 In vivo
Oral administration of neomycin to 37 healthy mongrel dogs (400
mg/day for 2, 4, or 10 days) and 24 healthy humans (6 g/day for 1 or
3 days) caused a marked reduction or complete elimination of coliform
bacilli from faeces in both species within 24 to 48 hours. In 4/10
dogs receiving a dose of 400 mg/day for 10 days resistant strains of
E. coli appeared on the 5th-6th day of treatment. Resistance was
not observed in E. coli isolates from humans treated with neomycin
in this study (Schweinburg et al., 1952).
Groups of 3-5 human flora associated (HFA) mice (germ-free mice
colonized with bacteria from human faecal suspensions) were
administered 1, 2, 3 or 4 g/l neomycin in their drinking-water.
Faecal samples were cultured on days 0, 1, 3, 5, 7, 14, 21, 28 and 35
of treatment. A control group of HFA mice received no neomycin
treatment. The number of obligate anaerobes, gram negative obligate
anaerobes, E. coli and Enterococci did not change over 35 days
in the 1 g neomycin/l drinking-water group. In the 2 and 3 g
neomycin/l groups, Escherichia coli and Enterococci were
eliminated, and the percentage of gram-negative obligate anaerobes was
increased. The NOAEL in this study is 1 g/l, equal to 125 mg/kg bw/day
(Hazenberg et al., 1983a).
Table 3. Summary of MIC values for different bacterial species obtained from animal isolates
MIC (µg/ml)
Species No. of Mean or Range MIC50 Reference
strains
Staphylococcus aureus 0.5 Moellering, 1983
Escherichia coli 8.0
Klebsiella pneumoniae 2.0
Proteus mirabilis 8.0
Proteus morganii 8.0
Proteus rettgeri 8.0
Proteus vulgaris 4.0
Escherichia coli (calves) 16 Hewett, 1990
Escherichia coli (pigs) 16
Escherichia coli (chickens) 1
Salmonella sp. (calves) 1
Salmonella sp. (pigs) 0.5
Bacteroides nodosus 68 16 - >256 >256 Duran et
al. , 1991
Bacteroides putredinis 36 16 - >256 128
Bacteroides buccae 16 2 - >256 128
Bacteroides sp. 21 8 - >256 >256
Table 3 (contd)
MIC (µg/ml)
Species No. of Mean or Range MIC50 Reference
strains
Fusobacterium necrophorum 10 16 - >256 128
Fusobacterium sp. 19 2 - >256 128
Peptostreptococus sp. 35 <0.06 - >256 64 Piriz et al., 1992
Table 4. Summary of MIC values for different bacterial species obtained from
human isolates
MIC (µg/ml)
Species No. of Mean or range Reference
strains
Escherichia coli 10 0.25 - 12.5 Schweinberg et al.,
1952
Enterococci 5 3.2 - 15
Sphaerophorus necrophorus 7 200 - 1600 Finegold et al.,
1967
Bacteroides fragilis 55 1600 - >25 600
Bacteroides melaninogenicus 20 <100 - 400
Bacteroides oralis 16 <100 - 400
Fusobacterum sp. 22 100 - 3200
Bifidobacterium adolescentis 11 12.5 - 400 Miller & Finegold,
1967
Bifidobacterium bifidum 5 400 - 1600
Bifidobacterium longum 11 200 - 1600
Bifidobacterium sp. 6 200 - 1600
Clostridium novyi Type A 16 32 - 512 Dornbusch et al.,
1975
Clostridium novyi Type B 7 64 - 512
Clostridium bifermentans 9 64 - 512
Clostridium sordellii 6 64 - 512
Clostridium sporogenes 18 32 - 512
Table 4 (contd)
MIC (µg/ml)
Species No. of Mean or range Reference
strains
Propionicum agnes 38 6.25 - 25 Hoeffler & Pulverer,
1976
Escherichia coli 2 16 Hazenberg et al.,
1983b
Escherichia coli 3 1 - 32 Hazenberg et al.,
1984
Table 5. Summary of MIC values under different agar medium and inoculum density conditions
MIC50 (µg/ml)a
Bacterial species/genus Strains Low densityb High densityc
SBd WCGd SBd WCGd
Bacteroides 15e,f >128 >128 >128 >128
Bifidobacterium 12e 16 128
Clostridium 11e, 5f >128 128 >128
Enterococcus 10e, 2f >128 128 >128 >128
Escherichia 13e 16 64
Escherichia - Aerobic 13e >128 >128
Eubacterium - Anaerobic 9e 8 >128
Fusobacterium 5e, 3f 16 32 >128 128
Lactobacillus 15e, 2f >128 32 >128 64
Peptostreptococcus/ 16e, 14f >128 32 >128 128
Peptococcus
a MIC50 values are for the multiple strains included in the assay.
b Low density inocula had cell concentrations of approx. 1 x 108 cells/ml.
c High density inocula had cell concentrations of approx. 1 x 1010 cells/ml.
d SB = Supplemented blood medium; WCG = Wilkins-Chalgren/glucose medium
e Number of tested strains of which MIC values for WCG were used to
calculate the summary values
f Number of tested strains of which MIC values for SB were used to
calculate the summary values
2.2.10.3 Special studies on potential effects on microorganisms used
for industrial food processing
Thirty strains of Propionobacterium sp., used to manufacture
Emmenthal and related cheese varieties, showed no resistance to 30
µg/disc neomycin but at 5 µg/disc moderate sensitivity was observed
(8/30 strains were resistant) (Reddy et al., 1973).
Forty-two strains of mesophilic lactic Streptococci,
Enterococci, Lactobacilli, Leuconostoc, Staphylococci and
other dairy- and food-related microorgansims were tested for their
sensitivity to neomycin at 5 and 30 µg/disc. Elliker's lactic agar
served as the growth medium; incubations temperature and times were
varied according to individual culture growth requirements.
Most of the strains of the starter streptococci (S. lactis,
S.cremoris, S. diacetilactis and S. thermophilus) and Lactobacillus
bulgaricus were sensitive to neomycin. Strains of S. faecalis,
exhibited resistance at 5 and 30 µg/disc (Reinbold & Reddy, 1974).
In another study, 24/29 strains of Lactobacillus bulgaricus
and all 15 tested strains of Streptococcus thermophilus were
resistant to 5 µg/disc neomycin. The tests for resistance were
carried out with commercially available sensitivity disks. At higher
doses of neomycin (30 µg/disc) resistance in 14/15 strains of
S.thermophilus and 10/29 strains of L. bulgaricus was observed
(Sozzi & Smiley, 1980).
The effect of residues of neomycin in milk on bacterial starter
cultures used in the production of fermented milk products was
investigated. Milk samples spiked with either 4 or 40 µg/ml neomycin
were serially diluted with antibiotic-free milk to provide
concentrations ranging from 0.063-4 µg/ml. Actual concentrations
measured with a microbiological cylinder plate assay ranged from
<0.20-3.12 µg/ml (detection limit: 0.20 µg/ml). The starter culture
types included a group of buttermilk/sour cream cultures containing
strains of Lactococcus lactis spp. and spp. cremoris or a
mixture of lactic acid producers and citric acid fermenters, 2 groups
of Italian cheese cultures containing strains of Streptococcus
thermophilus, another group of Italian cheese cultures containing
strains of Lactobacillus helveticus, and a group of yogurt cultures
containing Streptococcus thermophilus and Lactobacillus debruckii
spp. bulgaricus. "Time to clot" ratios greater than 2 indicated
that cultures were adversely affected by the presence of neomycin.
The only cultures adversely affected were the yogurt starter cultures
at a neomycin concentration of 4 µg/ml (equivalent to 3.12 µg/ml). In
this study neomycin concentrations in milk <2 µg/ml (equivalent to
1.42 µg/ml) had no effect on the growth of the bacteria in any of the
starter cultures (Hallberg et al., 1994).
2.3 Observations in humans
2.3.1 Nephrotoxicity
A clinical investigation of 63 patients (34 males and 29 females
ranging in age from nine months to 63 years (22 of them >60 years) on
neomycin therapy was undertaken. Renal toxicity and ototoxicity
toxicity were reported as treatment-related effects in some patients.
Twenty-four out of 32 patients, in whom serial urinalyses were
performed, showed fine granular casts in their urine either during or
just after neomycin therapy (Waisbren & Spink, 1950).
Powell and Hooker (1956) reported several cases of severe tubular
damage found in kidneys at autopsy of patients treated intramuscularly
with neomycin.
Oral administration of decreasing doses of neomycin (9.4- 1.5 g/d
(total 46 g over 11 days) to a patient produced acute renal failure
(Greenberg & Momary, 1965).
2.3.2 Ototoxicity
Ototoxic effects determined by audiograms and vestibular
functional tests were observed in patients treated with neomycin at
doses ranging from 1.5-2 g/day i.m. for up to 9 days. Hearing loss
was reported in 5 patients and loss of vestibular function occurred in
2 patients (Waisbren & Spink, 1950).
Deafness with histopathological inner ear changes were reported
in patients receiving high doses of neomycin orally (18 to 633 g total
dose) for unspecified periods of time (Lindsay et al., 1960;
Halpern & Heller, 1961; Greenberg & Momary, 1965).
Severe deafness occurred in a 1´-year old female, treated for
enteritis for 10 days with a neomycin-containing medication. The
total dose of neomycin was less than 2 g (King, 1962).
Severe deafness was reported in a 75 year-old female patient
receiving colonic and rectal irrigations with a neomycin solution for
2 months. A 5% solution was administered initially, then decreased to
a 1% solution for the majority of the treatment period. The total
neomycin dose administered was estimated at >900 g. The patient had
a hearing deficit but did not require a hearing aid prior to treatment
(Fields, 1964).
2.3.3 Hypersensitivity
From a survey of 675 patients with skin infections treated with
neomycin it was concluded that the sensitizing index for neomycin was
very low (Kile et al., 1952). However, cases of contact dermatitis
from neomycin (e.g., eardrops and eyedrops) were reported as dermal
delayed (tuberculin-type) and not epidermal sensitivity (Epstein,
1956; Calnan & Sarkany, 1958). In 55-75% of patients with neomycin
sensitivity, evidence of atopy (a genetic predisposition to mounting
large immune responses to antigenic stimulation) was established
(Epstein, 1965).
Results of patch tests with 21 antibiotics performed on a large
number of patients sensitive to neomycin showed cross-sensitivity to
bacitracin (80%), framycetin (91%), paromomycin (up to 99%) and
kanamycin (61%) (Pirila & Rouhunkoski, 1962). Cross-sensitization
with neomycin in streptomycin-sensitized patients was also described,
although contradictory results were obtained with respect to the
neomycin sensitivity in streptomycin-sensitive patients
(Sidi et al., 1958; Calnan & Sarkany, 1958).
A patient treated with ear drops containing neomycin (5 mg/ml in
distilled water) developed an acute exacerbation of otitis externa
after previously having shown a highly satisfactory response to the
use of the neomycin ear drops (Baer & Ludwig, 1952).
2.3.4 Special studies on the malabsorption syndrome
Morphologic alterations in the jejunal mucosa of patients,
similar to but less marked than those seen in patients with idiopathic
steatorrhea, were seen in 11/12 biopsy specimens from patients treated
with neomycin (4-12 g/day) for at least 4 days. Eighteen days after
the last dose of neomycin the jejunal morphology was restored
(Jacobson et al., 1960).
During the oral administration of 4-6 g neomycin/day for 6-8 days
plasma carotene concentrations were decreased in 6/8 patients despite
the administration of supplemental carotene (10 000 units/day). In
addition, d-xylose excretion in urine was decreased in 3/4 subjects.
Faecal fat excretion doubled during the treatment period in 1 patient
(Jacobson & Faloon, 1961).
Neomycin sulfate was administered orally (12 g/day for 4 days) as
well as by inlying tube directly into the jejenum and ilieum in 11
subjects. Urine and faeces were evaluated for fat, calcium, sodium,
potassium and nitrogen content. Steatorrhea was produced after oral
administration, but when neomycin was administered more distally, the
faecal fat content progressively diminished. Lowest urinary calcium,
sodium and potassium levels were measured after oral administration.
Faecal sodium, potassium and nitrogen levels were less affected by
this administration route, whereas the faecal calcium content was
greatest after jejunal instillation. The steatorrhea could not be
reversed by the administration of bile salts, sodium bicarbonate or
pancreatic enzymes (Gordon et al., 1968).
Three healthy male volunteers were orally administered 8 g
neomycin sulfate/day for 7 days. Lactose malabsorption was induced
after 3 days of treatment. Biopsy specimens from the small bowel
taken after 7 days of treatment showed slight villous blunting of the
mucosa and depressed disaccharidase activity. The lamina propria was
infiltrated with plasma cells and eosinophils. Enzyme levels and
histology of the mucosa and lamina propria of the small bowel returned
to normal 10 to 14 days after the treatment was stopped. No
treatment-related effects on stool lactic acids were observed (Cain
et al., 1968).
2.3.5 Special studies on microbiological effects
In a study with 37 hospitalized patients with various types of
intestinal lesions, the effect of oral neomycin treatment on bacteria
from the intestinal tract was determined. Treatment regimes of
neomycin administered prior to surgery (duration not stated) were as
follows: 1.5 g 4 times/day; 2 g 3 times/day; or 1 g every hour for
four doses the first day, then 1.5 g 4 times/day. After the
administration of neomycin the only clinical observations were
occasional nausea and vomiting. In stool specimens from patients
treated with 1.5 g 4 times/day (30 mg/kg bw/day) most of the aerobic
bacteria ( E. coli, A. aerogenes, S. faecalis, Proteus and
Pseudomonas) disappeared within 1´-4´ days, whereas anaerobic
organisms ( Bacteroides and Clostridium) remained. No resistant
strains of Mycrococcus pyopgenes were found. Similar results were
seen in patients receiving 2 g 3 times/day. In the group receiving 1
g hourly for four doses followed by 1.5 g 4 times/day, aerobic
bacteria were removed from the intestinal tract within two to three
days, while anaerobes ( Bacteroides and Clostridium) persisted
(Deering & Needham, 1953).
The intestinal flora of 14 patients hospitalized for non-
gastrointestinal diseases was studied before and after the use of
neomycin. Four patients received 4 g neomycin orally for 7 days and 10
patients were given 2 g neomycin for 6 days. The bacterial populations
of faecal specimens collected before, during and after neomycin
treatment were enumerated. A decrease in all bacterial species was
noted. Most affected were Enterococci, followed by E.coli,
lactose non-fermenters, Lactobacilli, Clostridia and Proteus
sp. Yeast and Klebsiellae were increased (Daikos et al., 1968).
Seven healthy adult volunteers received 1 g neomycin orally 3
times a day for 5 days (equivalent to 50 mg/kg bw/day). Fresh stool
samples were collected before, during and after treatment, and
bacterial counts recorded. Neomycin treatment did not affect
Bacteroides or Clostridia counts. E. coli counts were
significantly reduced in 2/7 volunteers (Arabi et al., 1979).
3. COMMENTS
The Committee considered data on pharmacokinetics, acute
toxicity, short-term and long-term toxicity, reproductive and
developmental toxicity, genotoxicity and carcinogenicity, effects in
humans and effects on antimicrobial activity. An evaluation report,
as requested for veterinary drugs with a long history of use (Annex 1,
reference 104) was also provided.
Neomycin is poorly absorbed after oral administration, whereas
after parenteral administration it is readily bioavailable. In
calves, oral absorption was estimated at 1-11%, depending on age. In
humans, up to 3% of an oral dose was recovered in urine, indicating
low absorption. Of the neomycin present in blood, 45-55% was bound to
plasma proteins in cows and ewes and the remainder was present in
nonionized form and may cross tissue barriers. After oral
administration the compound is mainly excreted unchanged in the
faeces. After parenteral administration neomycin is mainly excreted in
the urine.
Single doses of neomycin were slightly toxic to mice after oral
administration (LD50 = 2250 mg/kg bw), but single i.v. doses in mice
were highly toxic (LD50 <100 mg/kg bw).
Nephrotoxic effects were observed in mice after repeated s.c.
administration of 30-300 mg neomycin/kg bw/day, in guinea-pigs after
repeated s.c. doses of 10-60 mg neomycin sulfate/kg bw/day, and in
dogs after repeated i.m. doses of 24-96 mg neomycin/kg bw/day. No
kidney damage was observed in dogs receiving 100 mg/kg bw/day orally
for 6 weeks. Ototoxicity was observed after parenteral administration
of neomycin ranging from 25 to 150 mg/kg bw/day in guinea-pigs, and
20 to 80 mg/kg bw/day in cats. No ototoxic effects were observed in
guinea-pigs following oral administration of up to 10 mg neomycin
sulfate/kg bw/day for 90 days. In cats orally administered 6.25, 12.5
or 25 mg of neomycin/kg bw/day for one year, auditory function was not
affected, but upon histopathological examination changes in the organ
of Corti were reported at all dose levels.
The Committee concluded that, although ototoxicity was observed
in the one-year study in cats at the lowest dose tested (6.25 mg/kg
bw/day), this study was inadequate for the safety evaluation of
neomycin because of serious shortcomings in the histological technique
and the absence of a clear dose-related effect. It, however, accepted
the NOEL of 10 mg neomycin sulfate/kg bw/day, equivalent to 6 mg
neomycin/kg bw/day, for ototoxicity from the study in guinea-pigs.
Only a limited number of mutagenicity studies were available,
which had been poorly performed. The available in vitro
genotoxicity tests indicated that neomycin causes chromosomal
aberrations.
The tumour incidence was not increased in a two-year toxicity and
carcinogenicity study with rats orally administered neomycin up to a
dose level of 25 mg/kg bw/day. In the high-dose males only a slight
but statistically non-significant impairment of hearing was observed.
Because the Committee regarded the observed impairment of hearing as
treatment-related, the NOEL was 12.5 mg/kg bw/day.
In a multi-generation reproductive toxicity study in rats in
which neomycin was administered orally, no effects on reproductive
parameters were observed up to a dose of 25 mg/kg bw/day, which was
the highest dose administered. A teratogenicity study with an
unconventional protocol was conducted with F2b female rats from the
reproductive toxicity study. Neomycin was administered in the feed at
0, 6.25, 12.5 or 25 mg/kg bw/day from days 0-6 and 16-20 of gestation.
Dose levels were raised to 62.5, 125 or 250 mg/kg bw/day from days 6-
15 of gestation. No malformations, feto-toxicity or maternal toxicity
were observed.
Skin reactions due to hypersensitivity have been observed in
humans after the therapeutic use of neomycin. Nephrotoxic effects and
ototoxicity have been observed in humans after oral therapeutic use of
neomycin.
From several in vitro microbiological studies with different
bacteria, mostly isolated from humans, an MIC50 of 64 µg/ml was
derived for the most relevant sensitive bacterial organisms
( Escherichia coli and Lactobacillus spp.) under conditions of
high inoculum density. In human-flora-associated mice the NOEL for
antibacterial activity was 125 mg/kg bw/day. Studies on the effect of
neomycin on human gut flora in patients revealed effects at oral doses
>30 mg/kg bw/day.
Applying the formula developed at the thirty-eighth meeting of
the Committee (Annex 1, reference 97) an ADI based on anti-microbial
activity could be calculated as follows:
Concentration without effect daily faecal
of ADI on human gut flora (µg/ml)a x bolus (g)
Upper limit =
of ADI fraction of oral x safety x Weight of human (60kg)
dose availableb factorc
64 x 150
=
1 x 1 x 60
= 160 µg/kg bw
a The MIC50 value of 64 µg/ml was measured in the most relevant
sensitive species under conditions of high inoculum density. No
adjustment was deemed necessary.
b A conservative estimate of 100% availability to human gut flora
was selected. Experimental data were inadequate to correct for
inactivation of neomycin as a result of binding to gut contents.
c A substantial amount of data covering a variety of organisms,
including anaerobes isolated from the human gut, were available.
Also in view of the applied conservative factor for the availability
of neomycin to the gut flora a safety factor of 1 was adopted.
In reviewing the available toxicological and antimicrobial data
the Committee concluded that the toxicological data provided the most
appropriate endpoint for the evaluation of neomycin.
Only a limited set of genotoxicity tests was available, with gene
mutation studies in eukaryotic cells being absent. The available
information indicates that neomycin causes chromosomal aberrations.
However, the Committee noted that the long-term study in rats did not
provide evidence for a carcinogenic potential of neomycin.
The Committee established a temporary ADI of 0-30 µg/kg bw based
on the NOEL of 6 mg/kg bw/day for ototoxicity in the guinea-pig and a
safety factor of 200. The ADI was made temporary in view of the
deficiencies in the genotoxicity data.
5. REFERENCES
ARABI, Y., DIMOCK, F., BURDON, D.W., WILLIAMS, J.A. & KEIGHLEY, M.R.R.
(1979). Influence of neomycin and metronidazole on colonic microflora
of volunteers. J. Antimicrobial. Chemother., 5: 531-537.
ASCHBACHER, P.W. & FEIL, V.J. (1991). Fate of oral 14C Neomycin in
calves. USDA, ARS, Biosciences Research Laboratory, Farbo, ND.
J. Animal Science, 69(1): 733.
ASCHBACHER, P.W. & FEIL, V.J. (1994). Neomycin metabolism in calves.
J. Animal Science, 72: 683-689.
ATEF, M., EL-GENDI, A.Y.I., EL-SAYED, M.G.A. & A.M.M.AMER (1986).
Certain physico-pharmacologic properties of neomycin in chickens.
Arch. Geflügelk, 50(4): 132-135.
BAER, R.L. & LUDWIG, J.S. (1952). Allergic eczematous sensitization to
neomycin. Annals of Allergy, March-April: 136-137.
BEVAN, J.A. & THOMPSON, J.H. (1983). Introduction to principles of
drug action. Essentials of pharmacology, 3rd Ed. Harper and Row,
Philadelphia.
BREEN, K.J., BRYANT, R.E. LEVINSON, J.D. & SCHENKER, S. (1972).
Neomycin studies in man. Studies of oral and enema administration and
effect of intestinal ulceration. Ann. Intern. Med., 76: 211-218.
BROCKIE, P.H. (1951). Acute toxicity test with neomycin sulphate dated
2-22-1951. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
BRUMMETT, R.E., HALL, A.D. & RUSSELL, K.B. (1985). Ninety-day oral
neomycin sulfate (U-4,567) Ototoxicity study in the guinea-pig.
Technical report No. 7263/85/068 dated 23 october 1985. Submitted to
WHO by The Upjohn Company, Kalamazoo, MI, USA.
CAIN, C.D., REINER, E.B. & PATTERSON, M. (1968). Effects of neomycin
on disaccharidase activity of the small bowel. Arch. Intern Med.,
122: 311-314.
CALE , R.J. (1950). Memo dated 1950, subject : Toxicity neomycin
sulfate. Ssubmitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
CALNAN,C.D. & SARKANY, I. (1958). Contact dermatitis from neomycin.
Brit. J. Dermatol., 70: 435-445.
DAIKOS, G.K., KONTOMICHALOU, P. BILALIS, D. & PIMENDOU. L. (1968).
Intestinal flora ecology after oral use of antibiotics. Chemotherapy,
13: 146 - 160.
DEERING, W.H. & NEEDHAM, G.M. (1953). Effects of oral administration
of neomycin on the intestinal bacterial flora of man. Staff meeetings
of the Mayo Clinic, September 9, 502-507. Submitted to WHO by The
Upjohn Company, Kalamazoo, MI, USA.
DORNBUSCH, K., NORD, C.E. & DAHLBECK, A. (1975). Antibiotic
susceptibility of clostridium dpecies isolated from human infections.
Scand. J. Infect. Dis., 7: 127-134.
DURAN, S.P., VALERA, R.G., MANZANO, J.V. & MACHOTA, V. (1991).
Comparative in vitro susceptibility of Bacteroides and
Fusobacterium isolated from footrot in sheep to 28 antimicrobial
agents. J. Vet. Pharmacol. Therap., 14: 185-192.
EPSTEIN, S. (1956). Contact dermatitis from neomycin due to dermal
delayed (tuberculin-type) sensitivity. Dermatologica, 113(4): 191-
201.
EPSTEIN, S. (1965). Neomycin sensitivity and atopy. Dermatology,
130: 280-286.
EPSTEIN, S. & WENTZEL, F.J. (1962). Cross-sensitivity to various
"Mycins" Neomycin, Kanamycin, Streptomycin and Bacitracin: an
experimental study. Arch. Dermatol., 86: 183-194.
FEENSTRA, E.S. (1950). Interoffice memorandum of pathology report -
Chronic toxicity (s Mo.) of Neomycin sulfate #9084-10 in guinea-pigs
and dogs, dated 22 August 1950. Submitted to WHO by The Upjohn
Company, Kalamazoo, MI, USA.
FEENSTRA, E.S. (1954). Interoffice memorandum: Comparative
nephrotoxicity of neamine, neomycin B and neomycin C, Preliminary
report dated 22 September 1954. Submitted to WHO by The Upjohn
Company, Kalamazoo, MI, USA.
FEENSTRA, E.S. (1958). Unpublished technical acute toxicity i.p.
neomycin sulphate. dated 8 July 1958. Submitted to WHO by The Upjohn
Company, Kalamazoo, MI, USA.
FEENSTRA, E.S. (1959). Unpublished technical acute toxicity i.p.
neomycin sulphate. dated 19 January 1959. Submitted to WHO by The
Upjohn Company, Kalamazoo, MI, USA.
FIELDS, R.L. (1964). Neomycin ototoxicity. Arch. Otolaryngol., 79:
67-70. FINEGOLD, S.M., HARADA, N.E. & MILLER, L.G. (1967). Antibiotic
susceptibility Patterns as aids in classification and characterization
of gram-negative anaerobic bacilli. J. Bacteriol., 94(5): 443-350.
GORDON, S.J., HARO, E.N., PERS, I.C. & FALOON, W.W. (1968). Studies of
malabsorption and calcium excretion induced by neomycin sulfate.
Effect of intestinal site, bile salt and pancreatic enzymes. JAMA,
204: 129-134.
GRAY, J.E. (1964). Interoffice memorandum to E.S. Feenstra d.d. 6-5-
1964 LD50 neomycin sulfate submitted to WHO by The Upjohn Company,
Kalamazoo, MI, USA.
GREENBERG, L.H. & MOMARY, H. (1965). Audiotoxicity and nephrotoxicity
due to orally administered neomycin. JAMA, 194: 827-828.
HALL, A.D., SKINNER, P.J. & BARBIERS, A.R. (1983). A preliminary study
of the absorption of neomycin sulfate following oral administration to
guinea-pigs. Unpublished technical report No. 756-9610=83-001 dated
18-1-1983 from The Upjohn Company, Agricultural Research and
development laboratories, Kalamazoo Michigan , USA. Submitted to WHO
by The Upjohn Company, Kalamazoo, MI, USA.
HALLBERG, J.W., CHESTER, S.T., DAME, K.J., HORNISCH, R.E., TRAVIS,
M.A. & CORNELL, C.P. (1994). Effect of neomycin in milk on the
performance of cheese and yoghurt starter cultures. Unpublished
technical report No. 802-9690-94-001 dated 16 September 1994 from The
Upjohn Company, Agricultural Division. Submitted to WHO by The Upjohn
Company, Kalamazoo, MI, USA.
HALPERN, E.B. & HELLER, M.F. (1961). Ototoxicity of orally
administered neomycin. Arch. Otolaryngol., 73: 675-677.
HAWKINS, J.E. (1952). The ototoxicity of the neomycins. Trans. 11th
Conf. Chemother. of Tuberculosis, p. 189-191. Submitted to WHO by The
Upjohn Company, Kalamazoo, MI, USA.
HAWKINS, J.E., RAHWAY, N.J. & LURIE, M.H. (1953). The ototoxicity of
dihydrostreptomycin and neomycin in the cat. Ann. Otol. Rhin.
Laryngol., 62: 1128-1148.
HAZENBERG, M.P., VAN DE BOOM, M. BAKKER, M. & VAN DE MERWE, J.P.
(1983a). Effect of antibiotics on the human intestinal flora in mice.
Antonie van Leeuwenhoek, 49: 97-109.
HAZENBERG, M.P., VAN DE BOOM, M. BAKKER, M. & VAN DE MERWE, J.P.
(1983b). Binding to faeces and influence on human anaerobes of
antimicrobial aganets used for selective decontimination. Antonie van
Leeuwenhoek, 49: 111-117.
HAZENBERG, M.P., PENNOCK-SCHRODER, A.M., VAN DEN BOOM, M. & VAN DE
MERWE, J.P. (1984). Binding to and antibacterial effect ampicillin,
neomycin and polymyxin B on human faeces. J. Hyg.Camb., 93: 27-34.
HEATH, G.E. (1985). The pharmacokinetics of neomycin in the serum of
calves and young cross-bred swine. Thesus, University of Minnisota.
Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
HEWETT, G.R. (1990). Determination of the minimum Inhibitory
Concentration (MIC) of neomycin sulphate versus Salmonellae Species
and Escherichia coli isolated from calves, pigs and chicks.
Unpublished technical report No. 004-AHTR-9542-90-007 dated 3 May,
1990 from Agricultural Research and Development Laboratories, The
Upjohn Company U.K. Submitted to WHO by The Upjohn Company, Kalamazoo,
MI, USA.
HOEFFLER, E.H.L.K. & PULVERE, G. (1976). Antimicrobial susceptibility
of Propionibacterium acnes and related microbiological species.
Antimicrob. Ag. Chemother., 10(3): 387-394.
JACOBSON, E.D., PRIOR, J.T. & SYRACUSE, N.Y. (1960). Malabsorptive
syndrome induced by neomycin: morphological alterations in the jejunal
mucosa. J. Lab. Clin. Med., 56(2): 245-250.
JACOBSON, E.D. & FALOON, W.W. (1961). Malabsorptive efefcts of
neomycin in commonly used doses. JAMA, 175(3): 187-190.
JAJU, M., JAJU, M. & AHUJA, Y.R. (1986). Cytogenetic effect of
neomycin on human lymphocytes in vitro. Ind. J. Exp. Biol., 24:
595-598.
KAKUK, T.J. (1980). Neomycin sulfate: three-generation rat
reproductive teratology study. Technical report No. 756-9610-80-002
dated 30 November 1980, Agricultural Research and Development
Laboratories, The Upjohn Company. Submitted to WHO by The Upjohn
Company, Kalamazoo, MI, USA.
KAKUK, T.J. (1981). Neomycin sulfate: one-year tolerance study in the
domestic cat. Tecnical report No. 756-9610-81-001 dated 19 October
1981, Agricultural Research and Development Laboratories, The Upjohn
Company. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
KAKUK, T.J. (1982). Neomycin sulfate: lifetime feeding study in the
rat (Study #T-702)/Technical report No. 756-9610-82-001 dated 14
September 1982, Agricultural Research and Development Laboratories,
The Upjohn Company. Submitted to WHO by The Upjohn Company, Kalamazoo,
MI, USA.
KEEN, P. (1975). Some aspects of the pharmacology of antibiotics in
the cat and dog. J. Small Anim. Pract., 16: 767-773.
KILE, R.L., ROCKWELL, E.M. & SCHWARTZ, J. (1952). Use of neomycin in
dermatology. JAMA, 148(5): 339- 343.
KING, J.T. (1962). Severe deafness in an infant following oral
administration of neomycin. J. Med. Assoc. Georgia, 51: 530-531.
KUBINSKI, H., GUTZKE, G.E. & KUBINSKI, Z.O. (1981). DNA-cell-binding
(DCB) assay for suscpected carcinogens and mutagens. Mutat. Res.,
89: 95-136.
LINDSAY, J.R., PROCTOR, L.R. & WORK, W.P. (1960). Histopathological
inner ear changes in deafness due to neomycin in a human.
Laryngoscope, 70: 382-392.
MANNA, G.K. & BARDHAN, S. (1973). Effects of two antobiotics on the
chromosomes and mitotic frequency in the bone marrow cells of mice.
Chromosomes Today, 4: 277-282.
MILLER, L.G. & FINEGOLD, S.M. (1967). Antibacterial sensitivity of
Bifidobacterium (Lactobacillus bifidus). J. Bacteriol., 93(1): 125-
130.
MOELLERING, R.C. (1983). In vitro antibacterial activity of the
aminoglycoside antiobiotics. Rev. Infect. Dis., 5(2): S212-S231.
NELSON, A.A., RADOWSKI, J.L. & HAGAN, E.C. (1951). Renal and other
lesions in dogs and rats from intramuscular injection of neomycin.
Fed. Proc. 10(1): 366-367.
PIRILA, V., & ROUHUNKOSKI, S. (1962). The pattern of cross-sensitivity
to neomycin. Dermatologica, 125: 273-278.
PIRIZ, S., CUENCA, R. VALLE, J. & VADILLO, S. (1992). Susceptibilities
of anaerobic bacteris isolated from animals with ovine foot rot to 28
antimicrobial agents. Antimicrob. Ag. Chemother., 36(1): 198-201.
POTH, E.J., MARTIN, R.G., FROMM, S.M., WISE, R.I. & HSANG, C.M.
(1951). A critical analysis of neomycin as an intestinal antiseptic.
Tex. Rep. Biol. Med., 9: 631.
POWELL, L.W. & HOOKER, J.W. (1956). Neomycin nephropathy. JAMA,
160: 557-560.
REINBOLD, G.W. and REDDY, M.S. (1974). Sensitivity or resistance dairy
starter and associated microorganisms to selected antibiotics.
J. Milk Food Technol., 37(10): 517-521.
REDDY, M.S., REINBOLD, G.W. & WILLIAMS, F.D. (1973). Inhibition of
propionibacteria by antibiotic and antimicrobial agents. J. Milk Food
Technol., 36(11): 564-569.
RISKAER, N., CHRISTENSEN, E. PETERSEN & WEIDMAN, H. (1956). The
otoxicity of neomycin. Experimental investigations. Acta
Otolaryngol., 46: 137-152.
SCHWEINBURG, F.B., JACOB, S. & RUTENBURG, A.M. (1952). Effect of oral
Neomycin on normal intestinal flora of dogs and man. Proc. Soc. Expr.
Biol. & Med., 335-338.
SHEALY, Y.F. (1956). Technical unpublished report TUC No. U-4567 of
the acute toxicity of neomycin sulphate dated 6 July 1956. Submitted
to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SIDI, E., HINCKY. M. & LONGUEVILLE, R. (1958). Cross-sensitization
between neomycin and streptomycin. J. Invest. Dermatol., 30: 225-
231.
SOZZI, T. & SMILEY, M.B. (1980). Antibiotic resistance of Yogurt
starter cultures Streptoccus thermophilus and Lactobacillus
bulgaricus. Appl. Environm. Microbiol., 40(5): 862-865.
SWOAP, O.F. (1949a). Memo dated 12-2-1949, subject: Toxicity studies
on neomycin. Submitted to WHO by The Upjohn Company, Kalamazoo, MI,
USA.
SWOAP, O.F. (1949b). Memo dated 12-19-1949, subject: Toxicity studies
on neomycin SO4. Submitted to WHO by The Upjohn Company, Kalamazoo,
MI, USA.
SWOAP, O.F. (1950a). Memo on subject: Toxicity studies on SO4.
Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1950b). Memo dated 3-24-1950, subject: Toxicity: neomycin
SO4. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1950c). Memo dated 4-6-1950, subject: Toxicity: Neomycin
sulfate. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1950d). Memo dated 4-6-1950, subject: Toxicity: neomycin
sulfate. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1950e). Memo dated 6-16-1950, subject: Toxicity: neomycin
sulfate. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1950f). Memo dated 11-16-1950, subject: Toxicity:
neomycin SO4. Submitted to WHO by The Upjohn Company, Kalamazoo, MI,
USA.
SWOAP, O.F. (1950g). Memo dated 12-1-1950, subject: Neomycin toxicity
testing. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1950h). Memo dated 12-4-1950, subject: Toxicity: neomycin
SO4. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1950i). Memo dated 12-8-1950, subject: Toxicity: neomycin
SO4. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1950j). Memo dated 12-21-1950, subject: Toxicity:
neomycin SO4. Submitted to WHO by The Upjohn Company, Kalamazoo, MI,
USA.
SWOAP, O.F. (1950k). Memo dated 12-21-1950, subject: Toxicity:
neomycin SO4. Submitted to WHO by The Upjohn Company, Kalamazoo, MI,
USA.
SWOAP, O.F. (1951a). Memo dated 1-17-1951, subject: Toxicity: neomycin
SO4. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1951b). Toxicology report dated 5-8-1951 on neomycin
sulfate. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1951c). Toxicology report dated 7-2-51 on neomycin
sulfate. Submitted to WHO by the Upjohn Company, Kalamazoo, MI; USA.
SWOAP, O.F. (1952a). Toxicology report dated 5-13-1952 on neomycin
(lot 91-cat-6). Submitted to WHO by The Upjohn Company, Kalamazoo, MI,
USA.
SWOAP, O.F. (1952b). Toxicology report dated 7-3-1952 compound: Bulk
powder neomycin sulfate ( from resin process). Submitted to WHO by The
Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1952c). Toxicology report neomycin sulphate dated 6-10-
1952. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1952d). Toxicology report neomycin sulphate dated 6-10-
1952a. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1952e). Toxicology report Bulk powder neomycin sulphate
(from resin process) dated 7-3-1952. Submitted to WHO by The Upjohn
Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1952f). Toxicology report I: Bulk powder neomycin
sulphate (from resin process) dated 25 september 1952. Submitted to
WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1952g). Toxicology report II: Bulk powder neomycin
sulphate (from resin process) dated 25 september 1952. Submitted to
WHO by The Upjohn Company, Kalamazoo, MI 49001.
SWOAP, O.F. (1952h). Toxicology report III: Bulk powder neomycin
sulphate (from resin process) dated 25 september 1952 submitted to WHO
by The Upjohn Company, Kalamazoo, MI 49001.
SWOAP, O.F. (1953a). Toxicology report neomycin sulphate dated 12-2-
1953 submitted to WHO by The Upjohn Company, Kalamazoo, MI 49001.
SWOAP, O.F. (1953b). Interoffice memorandum dated 2-18-1953 subject:
meomycin B Submitted to WHO by The Upjohn Company, Kalamazoo, MI
49001.
SWOAP, O.F. (1954a). Memo acute toxicity no 983 Neomycin sulfate B
dated 24 September 1954, submitted to WHO by The Upjohn Company,
Kalamazoo, MI 49001.
SWOAP, O.F. (1954b). Interoffice memorandum - parallel toxicity tests
on neomycin B sulfate samples (U-4567) dated 30 September 1954,
submitted to WHO by The Upjohn Company, Kalamazoo, MI 49001.
SWOAP, O.F. (1957a). Memo - acute toxicity neomycin sulphate dated 1
November 1957, submitted to WHO by The Upjohn Company, Kalamazoo, MI,
USA.
SWOAP, O.F. (1958). Memo - acute toxicity neomycin sulphate Po.
Blended USP. 21 march 1958. Submitted to WHO by The Upjohn Company,
Kalamazoo, MI, USA.
THURN, K.K., BAKER, K.D., GREENING, R.C. & KOTARSKI, S.F. (1994).
Minimum inhibitory concentrations of neomycin sulfate against
bacterial species frequently isolated from the human gastrointestinal
tract. Unpublished technical report No. 802-7928-94-001 from The
Upjohn Company, Upjohn Laboratories, Kalamazoo, MI USA 49001.
Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
VAN DER BROOK, M.J. (1949). Memo dated 6-15-1949 about toxicity on
neomycin. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
VERINGA, E.M. & VAN DER WAAIJ, D. (1984). Biological inactivation by
faeces of antimicrobial drugs applicable in selective decontamination
of the digestive tract. J. Antimicrob. Chemother., 14: 605-612.
WAGMAN, G.H., BAILEY, J.V. & WEINSTEIN, M.J. (1974). Binding of
aminoglycosides to feces. Antimicrob. Ag. Chemother., 6(4): 415-
417.
WAISBREN, B.A. & SPINK, W.W. (1950). A clinical appraisal of neomycin.
Ann. Int. Med., 33: 1099-1119.
ZIV, G. & SULMAN, F.G. (1972). Binding of antibiotics to bovine and
ovine serum. Antimicrob. Ag. Chemother., 2(3): 206-213.
ZIV, G. & SULMAN, F.G. (1974). Distribution of aminoglycoside
antibiotics in blood and milk. Res. Vet. Sci., 17: 68-74.
 2. BIOLOGICAL DATA
2.1 Biochemical aspects
2.1.1 Absorption, distribution and excretion
2.1.1.1 Guinea-pigs
Groups of 4 male guinea-pigs were administered single oral doses
of 5, 10 or 100 mg/kg bw neomycin B sulfate. Serum was collected 1,
2, 3, and 4 hours after treatment. Neomycin concentrations of 1.5 and
0.45 µg/ml were measured at 1 and 2 hours after dosing with 100 mg/kg
bw, respectively. Serum concentrations of neomycin were below
detectable levels (< 0.10 µg/ml) in the low- and mid-dose groups at
all time points, and in the high-dose group at 3 and 4 hours post-
administration (Hall et al., 1983).
2.1.1.2 Chickens
Lohman chickens (14 total, weighing approximately 2 kg each) were
administered a single oral dose of 20 mg neomycin/kg bw. Neomycin
could not be detected in blood samples collected up to 8 hours post-
administration using a microbiological assay (detection limit not
specified) (Atef et al., 1986).
After a single i.v. administration of 20 mg/kg bw neomycin to
five Lohman chickens, the blood concentration curve showed a
biexponential decline with a T´ of about 6 hours for the elimination
phase and an AUC of approximately 196 µg/ml/h. After a single i.m.
administration of 20 mg/kg bw to 14 chickens, the peak blood level
(Cmax) was approximately 17 µg/ml and the mean maximum concentration
was reached 40 minutes after administration. The AUC was approximately
132 µg/ml/h. The bio-availability following i.m. administration was
approximately 70% (Atef et al., 1986).
In 22 Lohman chickens administered neomycin i.m. at 20 mg/kg bw
twice daily for 5 days, plateau levels of neomycin (about 6 µg/ml)
were retained for 1-4 days. Neomycin concentrations were detected in
the spleen for 3 days, in liver and lung for 6 days, and in kidney for
10 days post-injection (Atef et al., 1986).
2.1.1.3 Sheep
Serum and milk concentrations of neomycin were determined in
lactating Awassi ewes (4/group) after a single i.v. (20 mg/kg bw) or
i.m. injection (10 mg/kg bw). Neomycin was assayed micro-biologically
using the cylinder cup method (sensitivity limit 1 µg/ml). After i.v.
administration the T´ was approximately 3 hours and distribution
equilibrium was reached within 20 min. After i.m. administration peak
concentrations were reached after 1 hour. Neomycin was not detectable
in serum 12 hours after treament. A very small fraction of the dose
(0.01%-0.02%) was recovered in milk secreted from normal or irritated
glands (in which the left-side glands of the udder were infused with
150 ml of hypertonic NaCl solution 24 hours before treatment) during
the 12 hours after treatment. Peak milk concentrations of neomycin
following i.v. or i.m. treatment were less than 2 µg/ml (Ziv & Sulman,
1974).
2.1.1.4 Pigs
Two groups (6 pigs/group) of Yorkshire crossed weanling pigs (10
weeks old, weighing 10 to 15 kg) were orally administered 22 mg
neomycin sulfate/kg bw/day for 5 consecutive days. Group 1 consisted
of 3 males and 3 females, while group 2 had 5 males and 1 female. In
addition to the oral neomycin treatment, pigs in the second group
received diets supplemented with sodium sulfate at a rate of 10 g/kg
feed. Serum neomycin concentrations were measured up to 96 hours after
dosing. The mean peak serum concentration (approximately 0.2 µg/ml)
of neomycin was reached in the fourth hour in pigs fed the normal
ration. For pigs receiving the supplemented diets, the mean peak
serum concentration (approximately 0.1 µg/ml) was reached at 8 and 24
hours after dosing (Heath, 1985).
In another study by the same author, a single i.v. dose of 22
mg/kg bw neomycin sulfate was administered to 6 (3/sex) 10-month old
pigs. A peak mean serum level of approximately 30 µg/ml was detected
one hour after dosing, which decreased to 0.01 µg/ml by 72 hours
(Heath, 1985).
A single i.m. dose (22 mg/kg bw) of neomycin sulfate was
administered to 12 female pigs weighing 20 to 50 kg. A peak mean
serum level of approximately 40 µg/ml which was reached one hour after
dosing, decreased to 0.02 µg/ml after 72 hours (Heath, 1985).
2.1.1.5 Cattle
Ten castrated Holstein calves (2 to 6 months of age, weighing 80
to 180 kg) were orally administered 22 mg neomycin sulfate/kg bw/day
for 5 days. Serum concentrations were determined up to 96 hours after
dosing. Mean serum concentrations ranged from 0-0.06 µg/ml during the
1-96-hour dosing period (Heath, 1985).
A single i.v. dose (22 mg/kg bw) of neomycin sulfate was
administered to 10 castrated Holstein calves (2 to 6 months old,
weighing 70 to 170 kg). A peak mean serum concentration of
approximately 19 µg/ml which was detected one hour after dosing,
decreased to 0.03 µg/ml by 72 hours (Heath, 1985).
Four male Holstein calves (3 to 60 days old) were given a single
oral dose of 30 mg 14C-neomycin/kg bw and then killed after 96 hours.
The distribution of 14C in excreta and tissues was determined by mass
spectrophotometric analysis. Most of the radioactivity was recovered
in faeces (85-97%). The radioactivity found in urine decreased with
increasing age of the animal, from 11 to 0.5% of the administered
dose. Radioactivity found in the kidneys, liver and muscle of calves
at 3 days of age represented 55, 1.93 and 0.09 ppm of neomycin
equivalents, respectively. At least 90% of the 14C in the kidneys of
3-day old calves was present as neomycin. Seventy to 88% of the 14C
present in faeces of all calves was also identified as neomycin
(Aschbacher & Feil, 1991, 1994).
Serum and milk concentrations of neomycin were measured in 4
lactating Israeli-Friesian dairy cows following administration of a
single i.m. dose (10 mg/kg bw). Neomycin was assayed micro-
biologically by the cylinder cup method (sensitivity limit 1 µg/ml).
Peak serum concentrations were reached after 1 hour. Neomycin was not
detectable in serum 12 hours after treament. A very small fraction of
the dose (0.016%-0.022%) was recovered in milk secreted from normal or
irritated glands (in which the left-side glands of the udder were
infused with 150 ml of hypertonic NaCl solution 24 hours before
treatment) during the 12 hours after treatment. Peak milk
concentrations of neomycin were less than 2 µg/ml (Ziv & Sulman,
1974).
2.1.1.6 Humans
An oral dose of 1.5 g neomycin/day was administered to a 2- year
old female tuberculosis patient for 15 consecutive days. A nine-month
old male tuberculosis patient received 200 mg neomycin/day orally for
80 days. Both patients were diagnosed with miliary tuberculosis and
tuberculous meningitis. A maximum neomycin serum concentration of
approximately 5.0 µg/ml was achieved in both patients. Cerebrospinal
fluid concentrations of 1.25 and 2.5 µg/ml were measured in the female
and male patient, respectively (Waisbren & Spink, 1950).
Poth et al. (1951) reported serum concentrations ranging from
not detectable to <80 µg/ml in patients treated with oral neomycin
(6 g/day) for 3 days. The majority of the administered dose was
excreted in the faeces unchanged. Only 3% of the dose was recovered
from the urine.
The absorption and excretion of a 2 g oral or rectally
administered dose of neomycin sulfate was studied in 10 normal
subjects (healthy physicians who had no history of renal or liver
disease) and in patients with liver disease, peptic ulcer, regional
enteritis, or active ulcerative colitis. Urinary excretion (0.58%) of
neomycin and serum neomycin concentrations over 48 hours were similar
in all groups and by both routes. The percentage of the neomycin dose
excreted in the faeces following oral or rectal administration was
comparable (approximately 99%) (Breen et al., 1972).
2.1.2 Biotransformation
Aminoglycosides as a class are not metabolized in animals (Bevan
& Thompson, 1983) and are mostly excreted unchanged (Aschbacher &
Feil, 1994; Keen, 1975).
2.1.3 Special studies on binding to macromolecules
Lactating Israeli-Freisian cows (2 animals) and Awassi ewes (4
animals) were given single doses of 20 mg/kg bw neomycin i.m. or i.v.
Resulting serum concentrations ranged from 5-10 µg/ml. Serum protein
binding, determined by equilibrium dialysis and ultrafiltration
methods, was approximately 45-50% and 50-55% for cows and ewes,
respectively (Ziv & Sulman, 1972).
2.2 Toxicological studies
2.2.1 Acute toxicity studies
The results of acute toxicity studies after oral, i.v., s.c. or
i.p. administration of neomycin are summarized in Table 1.
2.2.2 Short-term toxicity studies
2.2.2.1 Cats
Groups of cats (8/sex/group) were orally dosed (gelatin capsule)
with 0, 6, 12 or 25 mg technical neomycin sulfate/kg bw/day for 1
year. The actual administered doses were found by chemical analysis
to be 72% of the intended doses. Clinical signs, auditory and
vestibular examinations, body weight, haematology, serum chemistry,
urinalysis, organ weights, macroscopy and histopathology were
evaluated.
The cause of the death of 7 cats during the study was not
considered to be treatment-related. The RBC counts were significantly
decreased in males at the highest dose at weeks 26 and 52. Blood urea
nitrogen levels were significantly increased in high-dose males at 13,
26 and 52 weeks, but no histopathological evidence of kidney damage
was observed. In the high-dose males at termination, potassium,
chloride and alkaline phosphatase were decreased, and cholesterol
levels were increased. Relative spleen and pancreas weights were
significantly decreased at all dose levels in male cats but without a
dose-related trend. Bone marrow hypoplasia was seen histogically in
the high-dose group (3/6 males and 4/8 females) (Kakuk, 1981).
Table 1. Acute toxicity of neomycin
Species Sex Route Substance Purity LD50 Reference
(mg/kg bw)
Mouse ? oral neomycin sulfate ? approx. Swoap, 1952c,d
2250-2500
Mouse M&F oral neomycin sulfate bulk 900 µg/mg 2250-2298 Swoap, 1952f,g,h
Mouse M&F oral neomycin sulfate (bulk 900-1000 >2500 Swoap, 1952b
powder from resin process) µg/mg
Mouse ? i.v. neomycin sulfate ? 40-158 Vander Brook, 1949;
Swoap, 1949a,b;
1950a,b,c,d,e,i,j,k;
1951a,b; Cale, 1950;
Gray, 1964
Mouse M i.v. neomycin sulfate ? 64.6-107 Brockie, 1951; Cale,
1950; Swoap,
1950f,g,h
Mouse M&F i.v. neomycin sulfate ? >50 Swoap, 1953a
Mouse ? i.v. neomycin A hydrochloride ? 97.6 Swoap, 1949a
Mouse M&F i.v. neomycin in HCH ? 74-115 Swoap, 1952a
Mouse ? i.v. neomycin sulfate bulk 900 µg/mg 110 Swoap, 1952e
Mouse M&F i.v. neomycin sulfate (bulk 910 µg/mg 100 Swoap, 1952b
powder from resin process)
Mouse ? s.c. neomycin sulfate ? 550 Vander Brook, 1949;
Swoap, 1950c,d,e
Table 1 (contd)
Species Sex Route Substance Purity LD50 Reference
(mg/kg bw)
Mouse ? s.c. neomycin sulfate ? 400 Brockie, 1951
Mouse ? s.c. neomycin A ? 470 Vander Brook, 1949
hydrochloride (51)
Mouse ? i.p. neomycin sulfate ? 274 Gray, 1964
Mouse M&F i.p. neomycin sulfate 690 µg/mg 310-457 Feenstra, 1958a;
Swoap, 1957a
Mouse M&F i.p. neomycin B sulfate ? 277-389 Swoap, 1954a,b;
Shealy, 1956
Mouse M&F i.p. neomycin B sulfate 1000 µg/mg 533 Swoap, 1953c
Shealy, 1956
Mouse M&F i.p. neomycin sulfate Po. 690 µg/mg 356 Swoap, 1958
blended USP
Mouse M&F i.p. neomycin sulfate bulk 658 µg/mg 248 Feenstra 1959
2.2.3 Long-term toxicity/carcinogenicity studies
2.2.3.1 Rats
Eight groups of Sprague-Dawley (SD)BR F1a weanling rats (4 groups
of males, 4 groups of females, 54-56/group) were administered neomycin
sulfate via the diet at 0, 6.25, 12.5 or 25 mg/kg bw/day until
terminal sacrifice. The test animals were offspring from the
F0generation that were mated after consuming similar levels of
neomycin in the diet for 11 weeks (see section 2.2.4). After 52 weeks
of treatment 10 rats/sex/group were selected for an interim kill and
evaluation. All male groups were killed after 104 weeks when the
control group survival reached 20%. When survival in female groups
reached 20%, the remaining animals of the group were sacrificed (27 to
30 months). Clinical signs, body weight, food consumption,
haematology, clinical chemistry, urinalysis, ophthalmoscopy, auditory
and vestibular tests, organ weight and histopathology were evaluated
in control and high-dose male and female rats.
To assess the possible effects of neomycin on the vestibular and
auditory functions an additional group (6/rats/sex, weanlings selected
from the control group in the reproduction study) was administered
neomycin sulfate s.c. at 100 mg/kg bw/day. Auditory and vestibular
function tests were scheduled weekly until study termination. When
all rats showed hearing loss (week 14), they were killed. Tissues of
the inner ear were preserved, but histopathological examinations were
not carried out.
Up to week 84, overall survival was about 84% and 92% for males
and females respectively. At the end of the study high mortality was
observed in all groups (33/44, 27/45, 29/46 and 30/45 for males and
33/46, 34/45, 34/44 and 35/45 for females at 0, 6.5, 12.5 and 25 mg/kg
bw/day, respectively). Female body weights were dose-relatedly
increased during the first three weeks of the study. Although not
statistically significant 3/15 rats at 25 mg/kg bw/day showed
hearing loss at the end of the study. No treatment-related effects
were observed in any of the other parameters evaluated. There was no
evidence of carcinogenicity. The NOEL was 12.5 mg/kg bw/day (Kakuk,
1982).
2.2.4 Reproductive toxicity studies
2.2.4.1 Rats
In a 3-generation reproductive toxicity study groups of Sprague-
Dawley (SD)BR rats (40-20/sex/group) were administered neomycin
sulfate via the diet at 0, 6.25, 12.5 or 25 mg/kg bw/day. After 11
weeks F0 generation rats were mated to produce F1a offspring which
were subsequently continued on neomycin sulfate in the life-time
feeding study described in section 2.2.3. F0 animals were bred a
second time to produce F1b offspring for use in the reproduction study
(through F3b litters). Through all generations no treatment-related
effects were observed in any of the parameters evaluated. The NOEL was
25 mg/kg bw/day (Kakuk, 1980).
2.2.5 Special studies on embryotoxicity and teratogenicity
2.2.5.1 Rats
Groups of 20 pregnant Sprague-Dawley (SD)BR rats (F2b females
from the reproductive toxicity study) were maintained on the same dose
regimen of 0, 6.25, 12.5 or 25 mg/kg bw/day (see section 2.2.4). From
gestation days 6-15, doses were increased to 0, 62.5, 125 or 250 mg/kg
bw/day. From gestaton days 16-20, doses were returned to 0, 6.25,
12.5 or 25 mg/kg bw. Dams were killed on day 20 of gestation. No
evidence of maternal toxicity, fetotoxicity or teratogenicity was
observed (Kakuk, 1980).
2.2.6 Special studies on genotoxicity
The results of the available genotoxicity studies on neomycin are
summarized in Table 2.
2.2.7 Special study on nephrotoxicity
2.2.7.1 Mice
Ten mice/group were given s.c. doses of 0, 30, 100, 300, 600 or
1000 mg/kg bw/day neomycin A (neamine), neomycin B or neomycin C for
14 days. None of the mice at the 2 highest doses survived 14 days.
Two mice in the 1000 mg/kg bw/day neamine group died.
Histopathological examination of the kidneys was performed. Based on
lesion indices the degree of nephrotoxicty was established. Neomycin
B and Neomycin C were about equally nephrotoxic. The observed
nephrotoxicity in the neamine groups was about 50% of that observed in
the other neomycin groups (Feenstra, 1954).
2.2.7.2 Guinea-pigs
Guinea-pigs (3/sex/group) were administered 10, 20, or 60 mg
neomycin sulfate/kg bw/day for 3 months (route not specified). One
female was kept as a control. Histopathological evaluation of the
kidney revealed subacute to chronic focal interstitial nephritis
associated with degeneration and necrosis at all doses, with a dose-
related increase in severity (Feenstra, 1950).
Table 2. Results of genotoxicity studies on neomycin
Test system Test object Concentration Results Reference
In vitro
Chromosome human 20, 40 and 80 µg/ml positivea,b Jaju et al., 1986
aberration assay lymphocytes
SCE test human 20, 40 and 80 µg/ml negativeb Jaju et al., 1986
lymphocytes
In vivo
Cytogenetic Mice bone 50 mg/kg bw positiveb,c Manna & Bardhan,
assay marrow 1973
a At doses that significantly inhibit the progression of the cell cycle.
b No positive control group was used.
c Test was not performed to current standards, i.e., results from 12 fixation
times are combined in 6 groups and number and sex of animals not stated.
Mitotic frequency was decreased; therefore, it was concluded that neomycin
reached the bone marrow.
2.2.7.3 Dogs
Six dogs (3/group) were administered 20 or 60 mg neomycin
sulfate/kg bw/day for 88 days (route not specified). All 3 dogs in
the high-dose group died after 14, 16 and 21 days. One low-dose dog
survived. The other 2 died after 21 and 45 days. Urine samples from
all dogs were taken before and after the beginning of treatment and
analyzed for albumin, blood and the presence of casts.
Histopathological examinations of kidneys showed degeneration,
necrosis and focal interstitial nephritis in all 6 dogs (Feenstra,
1950).
Twelve dogs were injected intramuscularly with 24, 48, or 96
mg/kg bw/day neomycin. At the highest dose all dogs died within 1-3
weeks. Blood urea nitrogen was increased and renal function impaired
as shown by decreased phenolsulfonphthalein excretion.
Histopathological evaluation of kidneys revealed renal tubular damage
characterized by marked epithelial necrosis in the proximal convoluted
tubules. Moderate changes in bone marrow and marked congestion of the
liver were also found. Inflammation at injection sites was also
noted. At the mid-dose the severity of effects were described as
intermediate. Dogs exposed to 24 mg/kg bw/day were killed and
examined after 1 month. The severity of renal damage in this group
was described as slight with increased granularity and occasional
desquamation of epithelial cells being most evident (Nelson et al.,
1951).
No kidney damage was observed in dogs (number/sex/group not
stated) orally dosed with 100 mg neomycin/kg bw/day for 6 weeks based
on urinalyses and gross and histopathological examinations of kidneys.
No other abnormalities were observed (Poth et al., 1951).
2.2.8 Special studies on ototoxicity
2.2.8.1 Guinea-pigs
Groups of 3 guinea-pigs were administered i.m. doses of 25, 50,
100, or 150 mg neomycin/kg bw/day for 30 to 60 weeks. Parameters
evaluated included vestibular function, auditory function (Preyer's
reflex) and histolopathological examination of labyrinths and central
nervous systems.
One guinea-pig in the high-dose group died after 22 days on test.
Vestibular function was reported as normal or slightly impaired across
all treatment groups with no dose-response relationship. Preyer's
reflex was abolished in all guinea-pigs receiving 100 and 150 mg/kg
bw/day. Histopathological examinations of animals in which the
Preyer's reflex was abolished revealed marked destruction of hair
cells and sometimes complete destruction of the organ of Corti.
Animals with intact hearing had normal cochleae, cristae, and maculae.
Reversible as well as irreversible degeneration of the ganglion cells
was seen in animals with abolished hearing, while animals with intact
hearing showed no definite pathological changes (Riskaer et al.,
1956) .
Hearing was not affected (determined by audiometry) after the
installation of 3 mg/kg bw neomycin into the middle ear of 18 guinea-
pigs. Six of the test animals had either one or both tympanic
membranes perforated prior to treatment (Riskaer et al., 1956).
Groups of guinea-pigs (50/sex/group) were orally admini-stered
neomycin B sulfate at 0, 1, 5, or 10 mg/kg bw/day for 90 days. Two
positive control groups (20/sex/group) received 10 or 100 mg/kg bw/day
s.c. for 90 and 34 days, respectively. Parameters evaluated included
clinical signs, body weight, auditory function test (Preyer pinna
reflex), gross necropsy, and histopathology (including cochleae to
score the loss of hair cells from the organ of Corti).
At 100 mg/kg bw/day s.c., ototoxic changes in the Preyer pinna
reflex thresholds and cochlear hair cell counts were observed. These
changes were not seen in the low-dose s.c. group nor in any of the
groups after oral administration. The NOEL for orally administered
neomycin in this study was 10 mg/kg bw/day (Brummett et al., 1985).
2.2.8.2 Cats
A clinical neomycin formulation (containing mostly neomycin B
sulfate), neomycin A hydrochloride and neomycin B sulfate were
administered s.c. to groups of cats (number/sex/group not stated) in
daily doses of 80 mg/kg bw/day for 5 or 15 days. The clinical
formulation was also administered in doses of 20, 40, or 100 mg/kg
bw/day s.c. for periods of 90, 60 and 30 days, respectively. Crude
neomycin (about 70% pure) was orally administered at 2 daily doses of
500 mg/kg bw (1 g/animal/day) for 30 days. Vestibular function was
studied by electrical recording of nystagmus evoked by rotating the
animal on a motor-driven turntable. Hearing ability was followed and
the cochlear function was studied electrophysically.
Histopathological examination of the kidneys was performed of all
cats.
Vestibular function was affected only in cats receiving the
highest dose of the clinical formulation (100 mg/kg bw/day) for 30
days. One of these cats showed a gradual loss of nystagmus which was
entirely absent by day 35, 5 days after the last treatment. Depression
of cochlear function was observed in all groups of cats and was most
severe in cats receiving the clinical preparation s.c. Degeneration
of external hair cells in the organ of Corti and internal hair cells
was also observed. A dose-related increase in the severity of damage
to renal tubular epithelium occurred in all cats receiving the
clinical preparation s.c. and in cats orally dosed with crude neomycin
(Hawkins, 1952; Hawkins et al., 1953).
Ototoxicity was studied in 5, 8, 3, and 4 cats who received oral
doses of 0, 6.25, 12.5, or 25 mg neomycin/kg bw/day, respectively, for
1 year. No evidence of auditory or vestibular dysfunction was
observed. In surface preparations of the organ of Corti
(cytocochleograms) ototoxicity was present microscopically as loss of
outer hair cells from the extreme lower portion of the basal turn of
the cochlea. Severe ototoxicity was observed in 3/4 high-dose cats.
Hair cell loss of a lesser degree was also observed in 7/8 and 1/3
cats in the low- and mid-dose groups, respectively (Kakuk, 1981). Due
to serious shortcomings in the histological technique and the absence
of a clear dose-related effect, the Committee considered this study
inadequate for the safety evaluation of neomycin.
2.2.9 Special studies on irritation and sensitization
No significant irritation was observed 24 hours after the
intrapleural administration of single doses of solutions of 1 ml
neomycin sulfate (0-100 mg/ml) to guinea-pigs (3-4/dose) (Swoap,
1951c).
A group of 9 neomycin-sensitive guinea-pigs was evaluated with
the patch test for cross sensitivy to kanamycin, streptomycin,
dihydrostreptomycin and bacitrin. Positive results were obtained for
kanamycin (1/9) and streptomycin (8/9) (Epstein & Wenzel, 1962).
2.2.10 Special studies on microbiological effects
Neomycin is active against most gram-positive and gram-negative
rods, many gram-positive cocci, and such acid-fast pathogens as
Mycobacterium tuberculosis.
Neomycin reacts with 30S ribosomal subunits of procaryotic cells
by electrostatic attraction causing a change in the conformation of
the ribosomal binding protein. This results in mRNA reading errors
and disrupted protein synthesis.
2.2.10.1 In vitro
Minimum Inhibitory Concentration (MIC) values for different
bacterial strains obtained from animal or human isolates are listed in
Tables 3 and 4, respectively.
In a special study, strains of various bacterial genera, mostly
of human origin, were tested for their susceptibility to neomycin
sulfate. MIC values were estimated on two agar types, Wilkens
Chalgren/glucose medium (WCG) and supplemented blood medium (SB) with
2 inoculum densities. Estimations were made under anaerobic and
aerobic conditions (E. coli) by the agar dilution method. The
results are listed in Table 5 (Thurn et al., 1994).
The adsorption of neomycin to dog faeces was calculated as the
difference between the amount of neomycin added to dilute suspension
of dog faeces and the amount of neomycin measured (microbioloigal
assay) in the supernatant after the mixture was incubated and
centrifuged. About 75% adsorption of neomycin was observed. After
acid extraction 47% of the added neomycin was still bound to the
faecal solids (Wagman et al., 1974).
Several concentrations of neomycin were evaluated for adsorption
to human faeces. Faecal samples were obtained from 8 healthy human
volunteers. The binding of neomycin to the faeces was calculated as
the difference between the amount added to a dilute suspension of
faeces and the amount measured (micro-biological assay) in the
supernatant after the mixture was incubated for 1 hour and
centrifuged. Approximately 83-98% faecal binding was observed
(Hazenberg et al., 1983b, 1984).
Neomycin solutions of approximately 0.1-30 mg/ml were mixed with
faecal suspensions prepared from faeces of 8 healthy human volunteers.
Neomycin antimicrobial activity (tested with Enterobacter cloacae)
remaining in the supernatants was measured and used for calculating
the "% inactivation" relative to the amount of added neomycin. The
percentage of added neomycin that was biologically inactivated
decreased with increasing concentrations of neomycin. Nearly 100%
inactivation due to binding occurred when the ratios of neomycin to
faecal weight were < 5 mg neomycin to 1 g wet weight of faeces in an
incubation mixture (Veringa & Van der Waaij, 1984).
2.2.10.2 In vivo
Oral administration of neomycin to 37 healthy mongrel dogs (400
mg/day for 2, 4, or 10 days) and 24 healthy humans (6 g/day for 1 or
3 days) caused a marked reduction or complete elimination of coliform
bacilli from faeces in both species within 24 to 48 hours. In 4/10
dogs receiving a dose of 400 mg/day for 10 days resistant strains of
E. coli appeared on the 5th-6th day of treatment. Resistance was
not observed in E. coli isolates from humans treated with neomycin
in this study (Schweinburg et al., 1952).
Groups of 3-5 human flora associated (HFA) mice (germ-free mice
colonized with bacteria from human faecal suspensions) were
administered 1, 2, 3 or 4 g/l neomycin in their drinking-water.
Faecal samples were cultured on days 0, 1, 3, 5, 7, 14, 21, 28 and 35
of treatment. A control group of HFA mice received no neomycin
treatment. The number of obligate anaerobes, gram negative obligate
anaerobes, E. coli and Enterococci did not change over 35 days
in the 1 g neomycin/l drinking-water group. In the 2 and 3 g
neomycin/l groups, Escherichia coli and Enterococci were
eliminated, and the percentage of gram-negative obligate anaerobes was
increased. The NOAEL in this study is 1 g/l, equal to 125 mg/kg bw/day
(Hazenberg et al., 1983a).
Table 3. Summary of MIC values for different bacterial species obtained from animal isolates
MIC (µg/ml)
Species No. of Mean or Range MIC50 Reference
strains
Staphylococcus aureus 0.5 Moellering, 1983
Escherichia coli 8.0
Klebsiella pneumoniae 2.0
Proteus mirabilis 8.0
Proteus morganii 8.0
Proteus rettgeri 8.0
Proteus vulgaris 4.0
Escherichia coli (calves) 16 Hewett, 1990
Escherichia coli (pigs) 16
Escherichia coli (chickens) 1
Salmonella sp. (calves) 1
Salmonella sp. (pigs) 0.5
Bacteroides nodosus 68 16 - >256 >256 Duran et
al. , 1991
Bacteroides putredinis 36 16 - >256 128
Bacteroides buccae 16 2 - >256 128
Bacteroides sp. 21 8 - >256 >256
Table 3 (contd)
MIC (µg/ml)
Species No. of Mean or Range MIC50 Reference
strains
Fusobacterium necrophorum 10 16 - >256 128
Fusobacterium sp. 19 2 - >256 128
Peptostreptococus sp. 35 <0.06 - >256 64 Piriz et al., 1992
Table 4. Summary of MIC values for different bacterial species obtained from
human isolates
MIC (µg/ml)
Species No. of Mean or range Reference
strains
Escherichia coli 10 0.25 - 12.5 Schweinberg et al.,
1952
Enterococci 5 3.2 - 15
Sphaerophorus necrophorus 7 200 - 1600 Finegold et al.,
1967
Bacteroides fragilis 55 1600 - >25 600
Bacteroides melaninogenicus 20 <100 - 400
Bacteroides oralis 16 <100 - 400
Fusobacterum sp. 22 100 - 3200
Bifidobacterium adolescentis 11 12.5 - 400 Miller & Finegold,
1967
Bifidobacterium bifidum 5 400 - 1600
Bifidobacterium longum 11 200 - 1600
Bifidobacterium sp. 6 200 - 1600
Clostridium novyi Type A 16 32 - 512 Dornbusch et al.,
1975
Clostridium novyi Type B 7 64 - 512
Clostridium bifermentans 9 64 - 512
Clostridium sordellii 6 64 - 512
Clostridium sporogenes 18 32 - 512
Table 4 (contd)
MIC (µg/ml)
Species No. of Mean or range Reference
strains
Propionicum agnes 38 6.25 - 25 Hoeffler & Pulverer,
1976
Escherichia coli 2 16 Hazenberg et al.,
1983b
Escherichia coli 3 1 - 32 Hazenberg et al.,
1984
Table 5. Summary of MIC values under different agar medium and inoculum density conditions
MIC50 (µg/ml)a
Bacterial species/genus Strains Low densityb High densityc
SBd WCGd SBd WCGd
Bacteroides 15e,f >128 >128 >128 >128
Bifidobacterium 12e 16 128
Clostridium 11e, 5f >128 128 >128
Enterococcus 10e, 2f >128 128 >128 >128
Escherichia 13e 16 64
Escherichia - Aerobic 13e >128 >128
Eubacterium - Anaerobic 9e 8 >128
Fusobacterium 5e, 3f 16 32 >128 128
Lactobacillus 15e, 2f >128 32 >128 64
Peptostreptococcus/ 16e, 14f >128 32 >128 128
Peptococcus
a MIC50 values are for the multiple strains included in the assay.
b Low density inocula had cell concentrations of approx. 1 x 108 cells/ml.
c High density inocula had cell concentrations of approx. 1 x 1010 cells/ml.
d SB = Supplemented blood medium; WCG = Wilkins-Chalgren/glucose medium
e Number of tested strains of which MIC values for WCG were used to
calculate the summary values
f Number of tested strains of which MIC values for SB were used to
calculate the summary values
2.2.10.3 Special studies on potential effects on microorganisms used
for industrial food processing
Thirty strains of Propionobacterium sp., used to manufacture
Emmenthal and related cheese varieties, showed no resistance to 30
µg/disc neomycin but at 5 µg/disc moderate sensitivity was observed
(8/30 strains were resistant) (Reddy et al., 1973).
Forty-two strains of mesophilic lactic Streptococci,
Enterococci, Lactobacilli, Leuconostoc, Staphylococci and
other dairy- and food-related microorgansims were tested for their
sensitivity to neomycin at 5 and 30 µg/disc. Elliker's lactic agar
served as the growth medium; incubations temperature and times were
varied according to individual culture growth requirements.
Most of the strains of the starter streptococci (S. lactis,
S.cremoris, S. diacetilactis and S. thermophilus) and Lactobacillus
bulgaricus were sensitive to neomycin. Strains of S. faecalis,
exhibited resistance at 5 and 30 µg/disc (Reinbold & Reddy, 1974).
In another study, 24/29 strains of Lactobacillus bulgaricus
and all 15 tested strains of Streptococcus thermophilus were
resistant to 5 µg/disc neomycin. The tests for resistance were
carried out with commercially available sensitivity disks. At higher
doses of neomycin (30 µg/disc) resistance in 14/15 strains of
S.thermophilus and 10/29 strains of L. bulgaricus was observed
(Sozzi & Smiley, 1980).
The effect of residues of neomycin in milk on bacterial starter
cultures used in the production of fermented milk products was
investigated. Milk samples spiked with either 4 or 40 µg/ml neomycin
were serially diluted with antibiotic-free milk to provide
concentrations ranging from 0.063-4 µg/ml. Actual concentrations
measured with a microbiological cylinder plate assay ranged from
<0.20-3.12 µg/ml (detection limit: 0.20 µg/ml). The starter culture
types included a group of buttermilk/sour cream cultures containing
strains of Lactococcus lactis spp. and spp. cremoris or a
mixture of lactic acid producers and citric acid fermenters, 2 groups
of Italian cheese cultures containing strains of Streptococcus
thermophilus, another group of Italian cheese cultures containing
strains of Lactobacillus helveticus, and a group of yogurt cultures
containing Streptococcus thermophilus and Lactobacillus debruckii
spp. bulgaricus. "Time to clot" ratios greater than 2 indicated
that cultures were adversely affected by the presence of neomycin.
The only cultures adversely affected were the yogurt starter cultures
at a neomycin concentration of 4 µg/ml (equivalent to 3.12 µg/ml). In
this study neomycin concentrations in milk <2 µg/ml (equivalent to
1.42 µg/ml) had no effect on the growth of the bacteria in any of the
starter cultures (Hallberg et al., 1994).
2.3 Observations in humans
2.3.1 Nephrotoxicity
A clinical investigation of 63 patients (34 males and 29 females
ranging in age from nine months to 63 years (22 of them >60 years) on
neomycin therapy was undertaken. Renal toxicity and ototoxicity
toxicity were reported as treatment-related effects in some patients.
Twenty-four out of 32 patients, in whom serial urinalyses were
performed, showed fine granular casts in their urine either during or
just after neomycin therapy (Waisbren & Spink, 1950).
Powell and Hooker (1956) reported several cases of severe tubular
damage found in kidneys at autopsy of patients treated intramuscularly
with neomycin.
Oral administration of decreasing doses of neomycin (9.4- 1.5 g/d
(total 46 g over 11 days) to a patient produced acute renal failure
(Greenberg & Momary, 1965).
2.3.2 Ototoxicity
Ototoxic effects determined by audiograms and vestibular
functional tests were observed in patients treated with neomycin at
doses ranging from 1.5-2 g/day i.m. for up to 9 days. Hearing loss
was reported in 5 patients and loss of vestibular function occurred in
2 patients (Waisbren & Spink, 1950).
Deafness with histopathological inner ear changes were reported
in patients receiving high doses of neomycin orally (18 to 633 g total
dose) for unspecified periods of time (Lindsay et al., 1960;
Halpern & Heller, 1961; Greenberg & Momary, 1965).
Severe deafness occurred in a 1´-year old female, treated for
enteritis for 10 days with a neomycin-containing medication. The
total dose of neomycin was less than 2 g (King, 1962).
Severe deafness was reported in a 75 year-old female patient
receiving colonic and rectal irrigations with a neomycin solution for
2 months. A 5% solution was administered initially, then decreased to
a 1% solution for the majority of the treatment period. The total
neomycin dose administered was estimated at >900 g. The patient had
a hearing deficit but did not require a hearing aid prior to treatment
(Fields, 1964).
2.3.3 Hypersensitivity
From a survey of 675 patients with skin infections treated with
neomycin it was concluded that the sensitizing index for neomycin was
very low (Kile et al., 1952). However, cases of contact dermatitis
from neomycin (e.g., eardrops and eyedrops) were reported as dermal
delayed (tuberculin-type) and not epidermal sensitivity (Epstein,
1956; Calnan & Sarkany, 1958). In 55-75% of patients with neomycin
sensitivity, evidence of atopy (a genetic predisposition to mounting
large immune responses to antigenic stimulation) was established
(Epstein, 1965).
Results of patch tests with 21 antibiotics performed on a large
number of patients sensitive to neomycin showed cross-sensitivity to
bacitracin (80%), framycetin (91%), paromomycin (up to 99%) and
kanamycin (61%) (Pirila & Rouhunkoski, 1962). Cross-sensitization
with neomycin in streptomycin-sensitized patients was also described,
although contradictory results were obtained with respect to the
neomycin sensitivity in streptomycin-sensitive patients
(Sidi et al., 1958; Calnan & Sarkany, 1958).
A patient treated with ear drops containing neomycin (5 mg/ml in
distilled water) developed an acute exacerbation of otitis externa
after previously having shown a highly satisfactory response to the
use of the neomycin ear drops (Baer & Ludwig, 1952).
2.3.4 Special studies on the malabsorption syndrome
Morphologic alterations in the jejunal mucosa of patients,
similar to but less marked than those seen in patients with idiopathic
steatorrhea, were seen in 11/12 biopsy specimens from patients treated
with neomycin (4-12 g/day) for at least 4 days. Eighteen days after
the last dose of neomycin the jejunal morphology was restored
(Jacobson et al., 1960).
During the oral administration of 4-6 g neomycin/day for 6-8 days
plasma carotene concentrations were decreased in 6/8 patients despite
the administration of supplemental carotene (10 000 units/day). In
addition, d-xylose excretion in urine was decreased in 3/4 subjects.
Faecal fat excretion doubled during the treatment period in 1 patient
(Jacobson & Faloon, 1961).
Neomycin sulfate was administered orally (12 g/day for 4 days) as
well as by inlying tube directly into the jejenum and ilieum in 11
subjects. Urine and faeces were evaluated for fat, calcium, sodium,
potassium and nitrogen content. Steatorrhea was produced after oral
administration, but when neomycin was administered more distally, the
faecal fat content progressively diminished. Lowest urinary calcium,
sodium and potassium levels were measured after oral administration.
Faecal sodium, potassium and nitrogen levels were less affected by
this administration route, whereas the faecal calcium content was
greatest after jejunal instillation. The steatorrhea could not be
reversed by the administration of bile salts, sodium bicarbonate or
pancreatic enzymes (Gordon et al., 1968).
Three healthy male volunteers were orally administered 8 g
neomycin sulfate/day for 7 days. Lactose malabsorption was induced
after 3 days of treatment. Biopsy specimens from the small bowel
taken after 7 days of treatment showed slight villous blunting of the
mucosa and depressed disaccharidase activity. The lamina propria was
infiltrated with plasma cells and eosinophils. Enzyme levels and
histology of the mucosa and lamina propria of the small bowel returned
to normal 10 to 14 days after the treatment was stopped. No
treatment-related effects on stool lactic acids were observed (Cain
et al., 1968).
2.3.5 Special studies on microbiological effects
In a study with 37 hospitalized patients with various types of
intestinal lesions, the effect of oral neomycin treatment on bacteria
from the intestinal tract was determined. Treatment regimes of
neomycin administered prior to surgery (duration not stated) were as
follows: 1.5 g 4 times/day; 2 g 3 times/day; or 1 g every hour for
four doses the first day, then 1.5 g 4 times/day. After the
administration of neomycin the only clinical observations were
occasional nausea and vomiting. In stool specimens from patients
treated with 1.5 g 4 times/day (30 mg/kg bw/day) most of the aerobic
bacteria ( E. coli, A. aerogenes, S. faecalis, Proteus and
Pseudomonas) disappeared within 1´-4´ days, whereas anaerobic
organisms ( Bacteroides and Clostridium) remained. No resistant
strains of Mycrococcus pyopgenes were found. Similar results were
seen in patients receiving 2 g 3 times/day. In the group receiving 1
g hourly for four doses followed by 1.5 g 4 times/day, aerobic
bacteria were removed from the intestinal tract within two to three
days, while anaerobes ( Bacteroides and Clostridium) persisted
(Deering & Needham, 1953).
The intestinal flora of 14 patients hospitalized for non-
gastrointestinal diseases was studied before and after the use of
neomycin. Four patients received 4 g neomycin orally for 7 days and 10
patients were given 2 g neomycin for 6 days. The bacterial populations
of faecal specimens collected before, during and after neomycin
treatment were enumerated. A decrease in all bacterial species was
noted. Most affected were Enterococci, followed by E.coli,
lactose non-fermenters, Lactobacilli, Clostridia and Proteus
sp. Yeast and Klebsiellae were increased (Daikos et al., 1968).
Seven healthy adult volunteers received 1 g neomycin orally 3
times a day for 5 days (equivalent to 50 mg/kg bw/day). Fresh stool
samples were collected before, during and after treatment, and
bacterial counts recorded. Neomycin treatment did not affect
Bacteroides or Clostridia counts. E. coli counts were
significantly reduced in 2/7 volunteers (Arabi et al., 1979).
3. COMMENTS
The Committee considered data on pharmacokinetics, acute
toxicity, short-term and long-term toxicity, reproductive and
developmental toxicity, genotoxicity and carcinogenicity, effects in
humans and effects on antimicrobial activity. An evaluation report,
as requested for veterinary drugs with a long history of use (Annex 1,
reference 104) was also provided.
Neomycin is poorly absorbed after oral administration, whereas
after parenteral administration it is readily bioavailable. In
calves, oral absorption was estimated at 1-11%, depending on age. In
humans, up to 3% of an oral dose was recovered in urine, indicating
low absorption. Of the neomycin present in blood, 45-55% was bound to
plasma proteins in cows and ewes and the remainder was present in
nonionized form and may cross tissue barriers. After oral
administration the compound is mainly excreted unchanged in the
faeces. After parenteral administration neomycin is mainly excreted in
the urine.
Single doses of neomycin were slightly toxic to mice after oral
administration (LD50 = 2250 mg/kg bw), but single i.v. doses in mice
were highly toxic (LD50 <100 mg/kg bw).
Nephrotoxic effects were observed in mice after repeated s.c.
administration of 30-300 mg neomycin/kg bw/day, in guinea-pigs after
repeated s.c. doses of 10-60 mg neomycin sulfate/kg bw/day, and in
dogs after repeated i.m. doses of 24-96 mg neomycin/kg bw/day. No
kidney damage was observed in dogs receiving 100 mg/kg bw/day orally
for 6 weeks. Ototoxicity was observed after parenteral administration
of neomycin ranging from 25 to 150 mg/kg bw/day in guinea-pigs, and
20 to 80 mg/kg bw/day in cats. No ototoxic effects were observed in
guinea-pigs following oral administration of up to 10 mg neomycin
sulfate/kg bw/day for 90 days. In cats orally administered 6.25, 12.5
or 25 mg of neomycin/kg bw/day for one year, auditory function was not
affected, but upon histopathological examination changes in the organ
of Corti were reported at all dose levels.
The Committee concluded that, although ototoxicity was observed
in the one-year study in cats at the lowest dose tested (6.25 mg/kg
bw/day), this study was inadequate for the safety evaluation of
neomycin because of serious shortcomings in the histological technique
and the absence of a clear dose-related effect. It, however, accepted
the NOEL of 10 mg neomycin sulfate/kg bw/day, equivalent to 6 mg
neomycin/kg bw/day, for ototoxicity from the study in guinea-pigs.
Only a limited number of mutagenicity studies were available,
which had been poorly performed. The available in vitro
genotoxicity tests indicated that neomycin causes chromosomal
aberrations.
The tumour incidence was not increased in a two-year toxicity and
carcinogenicity study with rats orally administered neomycin up to a
dose level of 25 mg/kg bw/day. In the high-dose males only a slight
but statistically non-significant impairment of hearing was observed.
Because the Committee regarded the observed impairment of hearing as
treatment-related, the NOEL was 12.5 mg/kg bw/day.
In a multi-generation reproductive toxicity study in rats in
which neomycin was administered orally, no effects on reproductive
parameters were observed up to a dose of 25 mg/kg bw/day, which was
the highest dose administered. A teratogenicity study with an
unconventional protocol was conducted with F2b female rats from the
reproductive toxicity study. Neomycin was administered in the feed at
0, 6.25, 12.5 or 25 mg/kg bw/day from days 0-6 and 16-20 of gestation.
Dose levels were raised to 62.5, 125 or 250 mg/kg bw/day from days 6-
15 of gestation. No malformations, feto-toxicity or maternal toxicity
were observed.
Skin reactions due to hypersensitivity have been observed in
humans after the therapeutic use of neomycin. Nephrotoxic effects and
ototoxicity have been observed in humans after oral therapeutic use of
neomycin.
From several in vitro microbiological studies with different
bacteria, mostly isolated from humans, an MIC50 of 64 µg/ml was
derived for the most relevant sensitive bacterial organisms
( Escherichia coli and Lactobacillus spp.) under conditions of
high inoculum density. In human-flora-associated mice the NOEL for
antibacterial activity was 125 mg/kg bw/day. Studies on the effect of
neomycin on human gut flora in patients revealed effects at oral doses
>30 mg/kg bw/day.
Applying the formula developed at the thirty-eighth meeting of
the Committee (Annex 1, reference 97) an ADI based on anti-microbial
activity could be calculated as follows:
Concentration without effect daily faecal
of ADI on human gut flora (µg/ml)a x bolus (g)
Upper limit =
of ADI fraction of oral x safety x Weight of human (60kg)
dose availableb factorc
64 x 150
=
1 x 1 x 60
= 160 µg/kg bw
a The MIC50 value of 64 µg/ml was measured in the most relevant
sensitive species under conditions of high inoculum density. No
adjustment was deemed necessary.
b A conservative estimate of 100% availability to human gut flora
was selected. Experimental data were inadequate to correct for
inactivation of neomycin as a result of binding to gut contents.
c A substantial amount of data covering a variety of organisms,
including anaerobes isolated from the human gut, were available.
Also in view of the applied conservative factor for the availability
of neomycin to the gut flora a safety factor of 1 was adopted.
In reviewing the available toxicological and antimicrobial data
the Committee concluded that the toxicological data provided the most
appropriate endpoint for the evaluation of neomycin.
Only a limited set of genotoxicity tests was available, with gene
mutation studies in eukaryotic cells being absent. The available
information indicates that neomycin causes chromosomal aberrations.
However, the Committee noted that the long-term study in rats did not
provide evidence for a carcinogenic potential of neomycin.
The Committee established a temporary ADI of 0-30 µg/kg bw based
on the NOEL of 6 mg/kg bw/day for ototoxicity in the guinea-pig and a
safety factor of 200. The ADI was made temporary in view of the
deficiencies in the genotoxicity data.
5. REFERENCES
ARABI, Y., DIMOCK, F., BURDON, D.W., WILLIAMS, J.A. & KEIGHLEY, M.R.R.
(1979). Influence of neomycin and metronidazole on colonic microflora
of volunteers. J. Antimicrobial. Chemother., 5: 531-537.
ASCHBACHER, P.W. & FEIL, V.J. (1991). Fate of oral 14C Neomycin in
calves. USDA, ARS, Biosciences Research Laboratory, Farbo, ND.
J. Animal Science, 69(1): 733.
ASCHBACHER, P.W. & FEIL, V.J. (1994). Neomycin metabolism in calves.
J. Animal Science, 72: 683-689.
ATEF, M., EL-GENDI, A.Y.I., EL-SAYED, M.G.A. & A.M.M.AMER (1986).
Certain physico-pharmacologic properties of neomycin in chickens.
Arch. Geflügelk, 50(4): 132-135.
BAER, R.L. & LUDWIG, J.S. (1952). Allergic eczematous sensitization to
neomycin. Annals of Allergy, March-April: 136-137.
BEVAN, J.A. & THOMPSON, J.H. (1983). Introduction to principles of
drug action. Essentials of pharmacology, 3rd Ed. Harper and Row,
Philadelphia.
BREEN, K.J., BRYANT, R.E. LEVINSON, J.D. & SCHENKER, S. (1972).
Neomycin studies in man. Studies of oral and enema administration and
effect of intestinal ulceration. Ann. Intern. Med., 76: 211-218.
BROCKIE, P.H. (1951). Acute toxicity test with neomycin sulphate dated
2-22-1951. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
BRUMMETT, R.E., HALL, A.D. & RUSSELL, K.B. (1985). Ninety-day oral
neomycin sulfate (U-4,567) Ototoxicity study in the guinea-pig.
Technical report No. 7263/85/068 dated 23 october 1985. Submitted to
WHO by The Upjohn Company, Kalamazoo, MI, USA.
CAIN, C.D., REINER, E.B. & PATTERSON, M. (1968). Effects of neomycin
on disaccharidase activity of the small bowel. Arch. Intern Med.,
122: 311-314.
CALE , R.J. (1950). Memo dated 1950, subject : Toxicity neomycin
sulfate. Ssubmitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
CALNAN,C.D. & SARKANY, I. (1958). Contact dermatitis from neomycin.
Brit. J. Dermatol., 70: 435-445.
DAIKOS, G.K., KONTOMICHALOU, P. BILALIS, D. & PIMENDOU. L. (1968).
Intestinal flora ecology after oral use of antibiotics. Chemotherapy,
13: 146 - 160.
DEERING, W.H. & NEEDHAM, G.M. (1953). Effects of oral administration
of neomycin on the intestinal bacterial flora of man. Staff meeetings
of the Mayo Clinic, September 9, 502-507. Submitted to WHO by The
Upjohn Company, Kalamazoo, MI, USA.
DORNBUSCH, K., NORD, C.E. & DAHLBECK, A. (1975). Antibiotic
susceptibility of clostridium dpecies isolated from human infections.
Scand. J. Infect. Dis., 7: 127-134.
DURAN, S.P., VALERA, R.G., MANZANO, J.V. & MACHOTA, V. (1991).
Comparative in vitro susceptibility of Bacteroides and
Fusobacterium isolated from footrot in sheep to 28 antimicrobial
agents. J. Vet. Pharmacol. Therap., 14: 185-192.
EPSTEIN, S. (1956). Contact dermatitis from neomycin due to dermal
delayed (tuberculin-type) sensitivity. Dermatologica, 113(4): 191-
201.
EPSTEIN, S. (1965). Neomycin sensitivity and atopy. Dermatology,
130: 280-286.
EPSTEIN, S. & WENTZEL, F.J. (1962). Cross-sensitivity to various
"Mycins" Neomycin, Kanamycin, Streptomycin and Bacitracin: an
experimental study. Arch. Dermatol., 86: 183-194.
FEENSTRA, E.S. (1950). Interoffice memorandum of pathology report -
Chronic toxicity (s Mo.) of Neomycin sulfate #9084-10 in guinea-pigs
and dogs, dated 22 August 1950. Submitted to WHO by The Upjohn
Company, Kalamazoo, MI, USA.
FEENSTRA, E.S. (1954). Interoffice memorandum: Comparative
nephrotoxicity of neamine, neomycin B and neomycin C, Preliminary
report dated 22 September 1954. Submitted to WHO by The Upjohn
Company, Kalamazoo, MI, USA.
FEENSTRA, E.S. (1958). Unpublished technical acute toxicity i.p.
neomycin sulphate. dated 8 July 1958. Submitted to WHO by The Upjohn
Company, Kalamazoo, MI, USA.
FEENSTRA, E.S. (1959). Unpublished technical acute toxicity i.p.
neomycin sulphate. dated 19 January 1959. Submitted to WHO by The
Upjohn Company, Kalamazoo, MI, USA.
FIELDS, R.L. (1964). Neomycin ototoxicity. Arch. Otolaryngol., 79:
67-70. FINEGOLD, S.M., HARADA, N.E. & MILLER, L.G. (1967). Antibiotic
susceptibility Patterns as aids in classification and characterization
of gram-negative anaerobic bacilli. J. Bacteriol., 94(5): 443-350.
GORDON, S.J., HARO, E.N., PERS, I.C. & FALOON, W.W. (1968). Studies of
malabsorption and calcium excretion induced by neomycin sulfate.
Effect of intestinal site, bile salt and pancreatic enzymes. JAMA,
204: 129-134.
GRAY, J.E. (1964). Interoffice memorandum to E.S. Feenstra d.d. 6-5-
1964 LD50 neomycin sulfate submitted to WHO by The Upjohn Company,
Kalamazoo, MI, USA.
GREENBERG, L.H. & MOMARY, H. (1965). Audiotoxicity and nephrotoxicity
due to orally administered neomycin. JAMA, 194: 827-828.
HALL, A.D., SKINNER, P.J. & BARBIERS, A.R. (1983). A preliminary study
of the absorption of neomycin sulfate following oral administration to
guinea-pigs. Unpublished technical report No. 756-9610=83-001 dated
18-1-1983 from The Upjohn Company, Agricultural Research and
development laboratories, Kalamazoo Michigan , USA. Submitted to WHO
by The Upjohn Company, Kalamazoo, MI, USA.
HALLBERG, J.W., CHESTER, S.T., DAME, K.J., HORNISCH, R.E., TRAVIS,
M.A. & CORNELL, C.P. (1994). Effect of neomycin in milk on the
performance of cheese and yoghurt starter cultures. Unpublished
technical report No. 802-9690-94-001 dated 16 September 1994 from The
Upjohn Company, Agricultural Division. Submitted to WHO by The Upjohn
Company, Kalamazoo, MI, USA.
HALPERN, E.B. & HELLER, M.F. (1961). Ototoxicity of orally
administered neomycin. Arch. Otolaryngol., 73: 675-677.
HAWKINS, J.E. (1952). The ototoxicity of the neomycins. Trans. 11th
Conf. Chemother. of Tuberculosis, p. 189-191. Submitted to WHO by The
Upjohn Company, Kalamazoo, MI, USA.
HAWKINS, J.E., RAHWAY, N.J. & LURIE, M.H. (1953). The ototoxicity of
dihydrostreptomycin and neomycin in the cat. Ann. Otol. Rhin.
Laryngol., 62: 1128-1148.
HAZENBERG, M.P., VAN DE BOOM, M. BAKKER, M. & VAN DE MERWE, J.P.
(1983a). Effect of antibiotics on the human intestinal flora in mice.
Antonie van Leeuwenhoek, 49: 97-109.
HAZENBERG, M.P., VAN DE BOOM, M. BAKKER, M. & VAN DE MERWE, J.P.
(1983b). Binding to faeces and influence on human anaerobes of
antimicrobial aganets used for selective decontimination. Antonie van
Leeuwenhoek, 49: 111-117.
HAZENBERG, M.P., PENNOCK-SCHRODER, A.M., VAN DEN BOOM, M. & VAN DE
MERWE, J.P. (1984). Binding to and antibacterial effect ampicillin,
neomycin and polymyxin B on human faeces. J. Hyg.Camb., 93: 27-34.
HEATH, G.E. (1985). The pharmacokinetics of neomycin in the serum of
calves and young cross-bred swine. Thesus, University of Minnisota.
Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
HEWETT, G.R. (1990). Determination of the minimum Inhibitory
Concentration (MIC) of neomycin sulphate versus Salmonellae Species
and Escherichia coli isolated from calves, pigs and chicks.
Unpublished technical report No. 004-AHTR-9542-90-007 dated 3 May,
1990 from Agricultural Research and Development Laboratories, The
Upjohn Company U.K. Submitted to WHO by The Upjohn Company, Kalamazoo,
MI, USA.
HOEFFLER, E.H.L.K. & PULVERE, G. (1976). Antimicrobial susceptibility
of Propionibacterium acnes and related microbiological species.
Antimicrob. Ag. Chemother., 10(3): 387-394.
JACOBSON, E.D., PRIOR, J.T. & SYRACUSE, N.Y. (1960). Malabsorptive
syndrome induced by neomycin: morphological alterations in the jejunal
mucosa. J. Lab. Clin. Med., 56(2): 245-250.
JACOBSON, E.D. & FALOON, W.W. (1961). Malabsorptive efefcts of
neomycin in commonly used doses. JAMA, 175(3): 187-190.
JAJU, M., JAJU, M. & AHUJA, Y.R. (1986). Cytogenetic effect of
neomycin on human lymphocytes in vitro. Ind. J. Exp. Biol., 24:
595-598.
KAKUK, T.J. (1980). Neomycin sulfate: three-generation rat
reproductive teratology study. Technical report No. 756-9610-80-002
dated 30 November 1980, Agricultural Research and Development
Laboratories, The Upjohn Company. Submitted to WHO by The Upjohn
Company, Kalamazoo, MI, USA.
KAKUK, T.J. (1981). Neomycin sulfate: one-year tolerance study in the
domestic cat. Tecnical report No. 756-9610-81-001 dated 19 October
1981, Agricultural Research and Development Laboratories, The Upjohn
Company. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
KAKUK, T.J. (1982). Neomycin sulfate: lifetime feeding study in the
rat (Study #T-702)/Technical report No. 756-9610-82-001 dated 14
September 1982, Agricultural Research and Development Laboratories,
The Upjohn Company. Submitted to WHO by The Upjohn Company, Kalamazoo,
MI, USA.
KEEN, P. (1975). Some aspects of the pharmacology of antibiotics in
the cat and dog. J. Small Anim. Pract., 16: 767-773.
KILE, R.L., ROCKWELL, E.M. & SCHWARTZ, J. (1952). Use of neomycin in
dermatology. JAMA, 148(5): 339- 343.
KING, J.T. (1962). Severe deafness in an infant following oral
administration of neomycin. J. Med. Assoc. Georgia, 51: 530-531.
KUBINSKI, H., GUTZKE, G.E. & KUBINSKI, Z.O. (1981). DNA-cell-binding
(DCB) assay for suscpected carcinogens and mutagens. Mutat. Res.,
89: 95-136.
LINDSAY, J.R., PROCTOR, L.R. & WORK, W.P. (1960). Histopathological
inner ear changes in deafness due to neomycin in a human.
Laryngoscope, 70: 382-392.
MANNA, G.K. & BARDHAN, S. (1973). Effects of two antobiotics on the
chromosomes and mitotic frequency in the bone marrow cells of mice.
Chromosomes Today, 4: 277-282.
MILLER, L.G. & FINEGOLD, S.M. (1967). Antibacterial sensitivity of
Bifidobacterium (Lactobacillus bifidus). J. Bacteriol., 93(1): 125-
130.
MOELLERING, R.C. (1983). In vitro antibacterial activity of the
aminoglycoside antiobiotics. Rev. Infect. Dis., 5(2): S212-S231.
NELSON, A.A., RADOWSKI, J.L. & HAGAN, E.C. (1951). Renal and other
lesions in dogs and rats from intramuscular injection of neomycin.
Fed. Proc. 10(1): 366-367.
PIRILA, V., & ROUHUNKOSKI, S. (1962). The pattern of cross-sensitivity
to neomycin. Dermatologica, 125: 273-278.
PIRIZ, S., CUENCA, R. VALLE, J. & VADILLO, S. (1992). Susceptibilities
of anaerobic bacteris isolated from animals with ovine foot rot to 28
antimicrobial agents. Antimicrob. Ag. Chemother., 36(1): 198-201.
POTH, E.J., MARTIN, R.G., FROMM, S.M., WISE, R.I. & HSANG, C.M.
(1951). A critical analysis of neomycin as an intestinal antiseptic.
Tex. Rep. Biol. Med., 9: 631.
POWELL, L.W. & HOOKER, J.W. (1956). Neomycin nephropathy. JAMA,
160: 557-560.
REINBOLD, G.W. and REDDY, M.S. (1974). Sensitivity or resistance dairy
starter and associated microorganisms to selected antibiotics.
J. Milk Food Technol., 37(10): 517-521.
REDDY, M.S., REINBOLD, G.W. & WILLIAMS, F.D. (1973). Inhibition of
propionibacteria by antibiotic and antimicrobial agents. J. Milk Food
Technol., 36(11): 564-569.
RISKAER, N., CHRISTENSEN, E. PETERSEN & WEIDMAN, H. (1956). The
otoxicity of neomycin. Experimental investigations. Acta
Otolaryngol., 46: 137-152.
SCHWEINBURG, F.B., JACOB, S. & RUTENBURG, A.M. (1952). Effect of oral
Neomycin on normal intestinal flora of dogs and man. Proc. Soc. Expr.
Biol. & Med., 335-338.
SHEALY, Y.F. (1956). Technical unpublished report TUC No. U-4567 of
the acute toxicity of neomycin sulphate dated 6 July 1956. Submitted
to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SIDI, E., HINCKY. M. & LONGUEVILLE, R. (1958). Cross-sensitization
between neomycin and streptomycin. J. Invest. Dermatol., 30: 225-
231.
SOZZI, T. & SMILEY, M.B. (1980). Antibiotic resistance of Yogurt
starter cultures Streptoccus thermophilus and Lactobacillus
bulgaricus. Appl. Environm. Microbiol., 40(5): 862-865.
SWOAP, O.F. (1949a). Memo dated 12-2-1949, subject: Toxicity studies
on neomycin. Submitted to WHO by The Upjohn Company, Kalamazoo, MI,
USA.
SWOAP, O.F. (1949b). Memo dated 12-19-1949, subject: Toxicity studies
on neomycin SO4. Submitted to WHO by The Upjohn Company, Kalamazoo,
MI, USA.
SWOAP, O.F. (1950a). Memo on subject: Toxicity studies on SO4.
Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1950b). Memo dated 3-24-1950, subject: Toxicity: neomycin
SO4. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1950c). Memo dated 4-6-1950, subject: Toxicity: Neomycin
sulfate. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1950d). Memo dated 4-6-1950, subject: Toxicity: neomycin
sulfate. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1950e). Memo dated 6-16-1950, subject: Toxicity: neomycin
sulfate. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1950f). Memo dated 11-16-1950, subject: Toxicity:
neomycin SO4. Submitted to WHO by The Upjohn Company, Kalamazoo, MI,
USA.
SWOAP, O.F. (1950g). Memo dated 12-1-1950, subject: Neomycin toxicity
testing. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1950h). Memo dated 12-4-1950, subject: Toxicity: neomycin
SO4. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1950i). Memo dated 12-8-1950, subject: Toxicity: neomycin
SO4. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1950j). Memo dated 12-21-1950, subject: Toxicity:
neomycin SO4. Submitted to WHO by The Upjohn Company, Kalamazoo, MI,
USA.
SWOAP, O.F. (1950k). Memo dated 12-21-1950, subject: Toxicity:
neomycin SO4. Submitted to WHO by The Upjohn Company, Kalamazoo, MI,
USA.
SWOAP, O.F. (1951a). Memo dated 1-17-1951, subject: Toxicity: neomycin
SO4. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1951b). Toxicology report dated 5-8-1951 on neomycin
sulfate. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1951c). Toxicology report dated 7-2-51 on neomycin
sulfate. Submitted to WHO by the Upjohn Company, Kalamazoo, MI; USA.
SWOAP, O.F. (1952a). Toxicology report dated 5-13-1952 on neomycin
(lot 91-cat-6). Submitted to WHO by The Upjohn Company, Kalamazoo, MI,
USA.
SWOAP, O.F. (1952b). Toxicology report dated 7-3-1952 compound: Bulk
powder neomycin sulfate ( from resin process). Submitted to WHO by The
Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1952c). Toxicology report neomycin sulphate dated 6-10-
1952. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1952d). Toxicology report neomycin sulphate dated 6-10-
1952a. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1952e). Toxicology report Bulk powder neomycin sulphate
(from resin process) dated 7-3-1952. Submitted to WHO by The Upjohn
Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1952f). Toxicology report I: Bulk powder neomycin
sulphate (from resin process) dated 25 september 1952. Submitted to
WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1952g). Toxicology report II: Bulk powder neomycin
sulphate (from resin process) dated 25 september 1952. Submitted to
WHO by The Upjohn Company, Kalamazoo, MI 49001.
SWOAP, O.F. (1952h). Toxicology report III: Bulk powder neomycin
sulphate (from resin process) dated 25 september 1952 submitted to WHO
by The Upjohn Company, Kalamazoo, MI 49001.
SWOAP, O.F. (1953a). Toxicology report neomycin sulphate dated 12-2-
1953 submitted to WHO by The Upjohn Company, Kalamazoo, MI 49001.
SWOAP, O.F. (1953b). Interoffice memorandum dated 2-18-1953 subject:
meomycin B Submitted to WHO by The Upjohn Company, Kalamazoo, MI
49001.
SWOAP, O.F. (1954a). Memo acute toxicity no 983 Neomycin sulfate B
dated 24 September 1954, submitted to WHO by The Upjohn Company,
Kalamazoo, MI 49001.
SWOAP, O.F. (1954b). Interoffice memorandum - parallel toxicity tests
on neomycin B sulfate samples (U-4567) dated 30 September 1954,
submitted to WHO by The Upjohn Company, Kalamazoo, MI 49001.
SWOAP, O.F. (1957a). Memo - acute toxicity neomycin sulphate dated 1
November 1957, submitted to WHO by The Upjohn Company, Kalamazoo, MI,
USA.
SWOAP, O.F. (1958). Memo - acute toxicity neomycin sulphate Po.
Blended USP. 21 march 1958. Submitted to WHO by The Upjohn Company,
Kalamazoo, MI, USA.
THURN, K.K., BAKER, K.D., GREENING, R.C. & KOTARSKI, S.F. (1994).
Minimum inhibitory concentrations of neomycin sulfate against
bacterial species frequently isolated from the human gastrointestinal
tract. Unpublished technical report No. 802-7928-94-001 from The
Upjohn Company, Upjohn Laboratories, Kalamazoo, MI USA 49001.
Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
VAN DER BROOK, M.J. (1949). Memo dated 6-15-1949 about toxicity on
neomycin. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
VERINGA, E.M. & VAN DER WAAIJ, D. (1984). Biological inactivation by
faeces of antimicrobial drugs applicable in selective decontamination
of the digestive tract. J. Antimicrob. Chemother., 14: 605-612.
WAGMAN, G.H., BAILEY, J.V. & WEINSTEIN, M.J. (1974). Binding of
aminoglycosides to feces. Antimicrob. Ag. Chemother., 6(4): 415-
417.
WAISBREN, B.A. & SPINK, W.W. (1950). A clinical appraisal of neomycin.
Ann. Int. Med., 33: 1099-1119.
ZIV, G. & SULMAN, F.G. (1972). Binding of antibiotics to bovine and
ovine serum. Antimicrob. Ag. Chemother., 2(3): 206-213.
ZIV, G. & SULMAN, F.G. (1974). Distribution of aminoglycoside
antibiotics in blood and milk. Res. Vet. Sci., 17: 68-74.
2. BIOLOGICAL DATA
2.1 Biochemical aspects
2.1.1 Absorption, distribution and excretion
2.1.1.1 Guinea-pigs
Groups of 4 male guinea-pigs were administered single oral doses
of 5, 10 or 100 mg/kg bw neomycin B sulfate. Serum was collected 1,
2, 3, and 4 hours after treatment. Neomycin concentrations of 1.5 and
0.45 µg/ml were measured at 1 and 2 hours after dosing with 100 mg/kg
bw, respectively. Serum concentrations of neomycin were below
detectable levels (< 0.10 µg/ml) in the low- and mid-dose groups at
all time points, and in the high-dose group at 3 and 4 hours post-
administration (Hall et al., 1983).
2.1.1.2 Chickens
Lohman chickens (14 total, weighing approximately 2 kg each) were
administered a single oral dose of 20 mg neomycin/kg bw. Neomycin
could not be detected in blood samples collected up to 8 hours post-
administration using a microbiological assay (detection limit not
specified) (Atef et al., 1986).
After a single i.v. administration of 20 mg/kg bw neomycin to
five Lohman chickens, the blood concentration curve showed a
biexponential decline with a T´ of about 6 hours for the elimination
phase and an AUC of approximately 196 µg/ml/h. After a single i.m.
administration of 20 mg/kg bw to 14 chickens, the peak blood level
(Cmax) was approximately 17 µg/ml and the mean maximum concentration
was reached 40 minutes after administration. The AUC was approximately
132 µg/ml/h. The bio-availability following i.m. administration was
approximately 70% (Atef et al., 1986).
In 22 Lohman chickens administered neomycin i.m. at 20 mg/kg bw
twice daily for 5 days, plateau levels of neomycin (about 6 µg/ml)
were retained for 1-4 days. Neomycin concentrations were detected in
the spleen for 3 days, in liver and lung for 6 days, and in kidney for
10 days post-injection (Atef et al., 1986).
2.1.1.3 Sheep
Serum and milk concentrations of neomycin were determined in
lactating Awassi ewes (4/group) after a single i.v. (20 mg/kg bw) or
i.m. injection (10 mg/kg bw). Neomycin was assayed micro-biologically
using the cylinder cup method (sensitivity limit 1 µg/ml). After i.v.
administration the T´ was approximately 3 hours and distribution
equilibrium was reached within 20 min. After i.m. administration peak
concentrations were reached after 1 hour. Neomycin was not detectable
in serum 12 hours after treament. A very small fraction of the dose
(0.01%-0.02%) was recovered in milk secreted from normal or irritated
glands (in which the left-side glands of the udder were infused with
150 ml of hypertonic NaCl solution 24 hours before treatment) during
the 12 hours after treatment. Peak milk concentrations of neomycin
following i.v. or i.m. treatment were less than 2 µg/ml (Ziv & Sulman,
1974).
2.1.1.4 Pigs
Two groups (6 pigs/group) of Yorkshire crossed weanling pigs (10
weeks old, weighing 10 to 15 kg) were orally administered 22 mg
neomycin sulfate/kg bw/day for 5 consecutive days. Group 1 consisted
of 3 males and 3 females, while group 2 had 5 males and 1 female. In
addition to the oral neomycin treatment, pigs in the second group
received diets supplemented with sodium sulfate at a rate of 10 g/kg
feed. Serum neomycin concentrations were measured up to 96 hours after
dosing. The mean peak serum concentration (approximately 0.2 µg/ml)
of neomycin was reached in the fourth hour in pigs fed the normal
ration. For pigs receiving the supplemented diets, the mean peak
serum concentration (approximately 0.1 µg/ml) was reached at 8 and 24
hours after dosing (Heath, 1985).
In another study by the same author, a single i.v. dose of 22
mg/kg bw neomycin sulfate was administered to 6 (3/sex) 10-month old
pigs. A peak mean serum level of approximately 30 µg/ml was detected
one hour after dosing, which decreased to 0.01 µg/ml by 72 hours
(Heath, 1985).
A single i.m. dose (22 mg/kg bw) of neomycin sulfate was
administered to 12 female pigs weighing 20 to 50 kg. A peak mean
serum level of approximately 40 µg/ml which was reached one hour after
dosing, decreased to 0.02 µg/ml after 72 hours (Heath, 1985).
2.1.1.5 Cattle
Ten castrated Holstein calves (2 to 6 months of age, weighing 80
to 180 kg) were orally administered 22 mg neomycin sulfate/kg bw/day
for 5 days. Serum concentrations were determined up to 96 hours after
dosing. Mean serum concentrations ranged from 0-0.06 µg/ml during the
1-96-hour dosing period (Heath, 1985).
A single i.v. dose (22 mg/kg bw) of neomycin sulfate was
administered to 10 castrated Holstein calves (2 to 6 months old,
weighing 70 to 170 kg). A peak mean serum concentration of
approximately 19 µg/ml which was detected one hour after dosing,
decreased to 0.03 µg/ml by 72 hours (Heath, 1985).
Four male Holstein calves (3 to 60 days old) were given a single
oral dose of 30 mg 14C-neomycin/kg bw and then killed after 96 hours.
The distribution of 14C in excreta and tissues was determined by mass
spectrophotometric analysis. Most of the radioactivity was recovered
in faeces (85-97%). The radioactivity found in urine decreased with
increasing age of the animal, from 11 to 0.5% of the administered
dose. Radioactivity found in the kidneys, liver and muscle of calves
at 3 days of age represented 55, 1.93 and 0.09 ppm of neomycin
equivalents, respectively. At least 90% of the 14C in the kidneys of
3-day old calves was present as neomycin. Seventy to 88% of the 14C
present in faeces of all calves was also identified as neomycin
(Aschbacher & Feil, 1991, 1994).
Serum and milk concentrations of neomycin were measured in 4
lactating Israeli-Friesian dairy cows following administration of a
single i.m. dose (10 mg/kg bw). Neomycin was assayed micro-
biologically by the cylinder cup method (sensitivity limit 1 µg/ml).
Peak serum concentrations were reached after 1 hour. Neomycin was not
detectable in serum 12 hours after treament. A very small fraction of
the dose (0.016%-0.022%) was recovered in milk secreted from normal or
irritated glands (in which the left-side glands of the udder were
infused with 150 ml of hypertonic NaCl solution 24 hours before
treatment) during the 12 hours after treatment. Peak milk
concentrations of neomycin were less than 2 µg/ml (Ziv & Sulman,
1974).
2.1.1.6 Humans
An oral dose of 1.5 g neomycin/day was administered to a 2- year
old female tuberculosis patient for 15 consecutive days. A nine-month
old male tuberculosis patient received 200 mg neomycin/day orally for
80 days. Both patients were diagnosed with miliary tuberculosis and
tuberculous meningitis. A maximum neomycin serum concentration of
approximately 5.0 µg/ml was achieved in both patients. Cerebrospinal
fluid concentrations of 1.25 and 2.5 µg/ml were measured in the female
and male patient, respectively (Waisbren & Spink, 1950).
Poth et al. (1951) reported serum concentrations ranging from
not detectable to <80 µg/ml in patients treated with oral neomycin
(6 g/day) for 3 days. The majority of the administered dose was
excreted in the faeces unchanged. Only 3% of the dose was recovered
from the urine.
The absorption and excretion of a 2 g oral or rectally
administered dose of neomycin sulfate was studied in 10 normal
subjects (healthy physicians who had no history of renal or liver
disease) and in patients with liver disease, peptic ulcer, regional
enteritis, or active ulcerative colitis. Urinary excretion (0.58%) of
neomycin and serum neomycin concentrations over 48 hours were similar
in all groups and by both routes. The percentage of the neomycin dose
excreted in the faeces following oral or rectal administration was
comparable (approximately 99%) (Breen et al., 1972).
2.1.2 Biotransformation
Aminoglycosides as a class are not metabolized in animals (Bevan
& Thompson, 1983) and are mostly excreted unchanged (Aschbacher &
Feil, 1994; Keen, 1975).
2.1.3 Special studies on binding to macromolecules
Lactating Israeli-Freisian cows (2 animals) and Awassi ewes (4
animals) were given single doses of 20 mg/kg bw neomycin i.m. or i.v.
Resulting serum concentrations ranged from 5-10 µg/ml. Serum protein
binding, determined by equilibrium dialysis and ultrafiltration
methods, was approximately 45-50% and 50-55% for cows and ewes,
respectively (Ziv & Sulman, 1972).
2.2 Toxicological studies
2.2.1 Acute toxicity studies
The results of acute toxicity studies after oral, i.v., s.c. or
i.p. administration of neomycin are summarized in Table 1.
2.2.2 Short-term toxicity studies
2.2.2.1 Cats
Groups of cats (8/sex/group) were orally dosed (gelatin capsule)
with 0, 6, 12 or 25 mg technical neomycin sulfate/kg bw/day for 1
year. The actual administered doses were found by chemical analysis
to be 72% of the intended doses. Clinical signs, auditory and
vestibular examinations, body weight, haematology, serum chemistry,
urinalysis, organ weights, macroscopy and histopathology were
evaluated.
The cause of the death of 7 cats during the study was not
considered to be treatment-related. The RBC counts were significantly
decreased in males at the highest dose at weeks 26 and 52. Blood urea
nitrogen levels were significantly increased in high-dose males at 13,
26 and 52 weeks, but no histopathological evidence of kidney damage
was observed. In the high-dose males at termination, potassium,
chloride and alkaline phosphatase were decreased, and cholesterol
levels were increased. Relative spleen and pancreas weights were
significantly decreased at all dose levels in male cats but without a
dose-related trend. Bone marrow hypoplasia was seen histogically in
the high-dose group (3/6 males and 4/8 females) (Kakuk, 1981).
Table 1. Acute toxicity of neomycin
Species Sex Route Substance Purity LD50 Reference
(mg/kg bw)
Mouse ? oral neomycin sulfate ? approx. Swoap, 1952c,d
2250-2500
Mouse M&F oral neomycin sulfate bulk 900 µg/mg 2250-2298 Swoap, 1952f,g,h
Mouse M&F oral neomycin sulfate (bulk 900-1000 >2500 Swoap, 1952b
powder from resin process) µg/mg
Mouse ? i.v. neomycin sulfate ? 40-158 Vander Brook, 1949;
Swoap, 1949a,b;
1950a,b,c,d,e,i,j,k;
1951a,b; Cale, 1950;
Gray, 1964
Mouse M i.v. neomycin sulfate ? 64.6-107 Brockie, 1951; Cale,
1950; Swoap,
1950f,g,h
Mouse M&F i.v. neomycin sulfate ? >50 Swoap, 1953a
Mouse ? i.v. neomycin A hydrochloride ? 97.6 Swoap, 1949a
Mouse M&F i.v. neomycin in HCH ? 74-115 Swoap, 1952a
Mouse ? i.v. neomycin sulfate bulk 900 µg/mg 110 Swoap, 1952e
Mouse M&F i.v. neomycin sulfate (bulk 910 µg/mg 100 Swoap, 1952b
powder from resin process)
Mouse ? s.c. neomycin sulfate ? 550 Vander Brook, 1949;
Swoap, 1950c,d,e
Table 1 (contd)
Species Sex Route Substance Purity LD50 Reference
(mg/kg bw)
Mouse ? s.c. neomycin sulfate ? 400 Brockie, 1951
Mouse ? s.c. neomycin A ? 470 Vander Brook, 1949
hydrochloride (51)
Mouse ? i.p. neomycin sulfate ? 274 Gray, 1964
Mouse M&F i.p. neomycin sulfate 690 µg/mg 310-457 Feenstra, 1958a;
Swoap, 1957a
Mouse M&F i.p. neomycin B sulfate ? 277-389 Swoap, 1954a,b;
Shealy, 1956
Mouse M&F i.p. neomycin B sulfate 1000 µg/mg 533 Swoap, 1953c
Shealy, 1956
Mouse M&F i.p. neomycin sulfate Po. 690 µg/mg 356 Swoap, 1958
blended USP
Mouse M&F i.p. neomycin sulfate bulk 658 µg/mg 248 Feenstra 1959
2.2.3 Long-term toxicity/carcinogenicity studies
2.2.3.1 Rats
Eight groups of Sprague-Dawley (SD)BR F1a weanling rats (4 groups
of males, 4 groups of females, 54-56/group) were administered neomycin
sulfate via the diet at 0, 6.25, 12.5 or 25 mg/kg bw/day until
terminal sacrifice. The test animals were offspring from the
F0generation that were mated after consuming similar levels of
neomycin in the diet for 11 weeks (see section 2.2.4). After 52 weeks
of treatment 10 rats/sex/group were selected for an interim kill and
evaluation. All male groups were killed after 104 weeks when the
control group survival reached 20%. When survival in female groups
reached 20%, the remaining animals of the group were sacrificed (27 to
30 months). Clinical signs, body weight, food consumption,
haematology, clinical chemistry, urinalysis, ophthalmoscopy, auditory
and vestibular tests, organ weight and histopathology were evaluated
in control and high-dose male and female rats.
To assess the possible effects of neomycin on the vestibular and
auditory functions an additional group (6/rats/sex, weanlings selected
from the control group in the reproduction study) was administered
neomycin sulfate s.c. at 100 mg/kg bw/day. Auditory and vestibular
function tests were scheduled weekly until study termination. When
all rats showed hearing loss (week 14), they were killed. Tissues of
the inner ear were preserved, but histopathological examinations were
not carried out.
Up to week 84, overall survival was about 84% and 92% for males
and females respectively. At the end of the study high mortality was
observed in all groups (33/44, 27/45, 29/46 and 30/45 for males and
33/46, 34/45, 34/44 and 35/45 for females at 0, 6.5, 12.5 and 25 mg/kg
bw/day, respectively). Female body weights were dose-relatedly
increased during the first three weeks of the study. Although not
statistically significant 3/15 rats at 25 mg/kg bw/day showed
hearing loss at the end of the study. No treatment-related effects
were observed in any of the other parameters evaluated. There was no
evidence of carcinogenicity. The NOEL was 12.5 mg/kg bw/day (Kakuk,
1982).
2.2.4 Reproductive toxicity studies
2.2.4.1 Rats
In a 3-generation reproductive toxicity study groups of Sprague-
Dawley (SD)BR rats (40-20/sex/group) were administered neomycin
sulfate via the diet at 0, 6.25, 12.5 or 25 mg/kg bw/day. After 11
weeks F0 generation rats were mated to produce F1a offspring which
were subsequently continued on neomycin sulfate in the life-time
feeding study described in section 2.2.3. F0 animals were bred a
second time to produce F1b offspring for use in the reproduction study
(through F3b litters). Through all generations no treatment-related
effects were observed in any of the parameters evaluated. The NOEL was
25 mg/kg bw/day (Kakuk, 1980).
2.2.5 Special studies on embryotoxicity and teratogenicity
2.2.5.1 Rats
Groups of 20 pregnant Sprague-Dawley (SD)BR rats (F2b females
from the reproductive toxicity study) were maintained on the same dose
regimen of 0, 6.25, 12.5 or 25 mg/kg bw/day (see section 2.2.4). From
gestation days 6-15, doses were increased to 0, 62.5, 125 or 250 mg/kg
bw/day. From gestaton days 16-20, doses were returned to 0, 6.25,
12.5 or 25 mg/kg bw. Dams were killed on day 20 of gestation. No
evidence of maternal toxicity, fetotoxicity or teratogenicity was
observed (Kakuk, 1980).
2.2.6 Special studies on genotoxicity
The results of the available genotoxicity studies on neomycin are
summarized in Table 2.
2.2.7 Special study on nephrotoxicity
2.2.7.1 Mice
Ten mice/group were given s.c. doses of 0, 30, 100, 300, 600 or
1000 mg/kg bw/day neomycin A (neamine), neomycin B or neomycin C for
14 days. None of the mice at the 2 highest doses survived 14 days.
Two mice in the 1000 mg/kg bw/day neamine group died.
Histopathological examination of the kidneys was performed. Based on
lesion indices the degree of nephrotoxicty was established. Neomycin
B and Neomycin C were about equally nephrotoxic. The observed
nephrotoxicity in the neamine groups was about 50% of that observed in
the other neomycin groups (Feenstra, 1954).
2.2.7.2 Guinea-pigs
Guinea-pigs (3/sex/group) were administered 10, 20, or 60 mg
neomycin sulfate/kg bw/day for 3 months (route not specified). One
female was kept as a control. Histopathological evaluation of the
kidney revealed subacute to chronic focal interstitial nephritis
associated with degeneration and necrosis at all doses, with a dose-
related increase in severity (Feenstra, 1950).
Table 2. Results of genotoxicity studies on neomycin
Test system Test object Concentration Results Reference
In vitro
Chromosome human 20, 40 and 80 µg/ml positivea,b Jaju et al., 1986
aberration assay lymphocytes
SCE test human 20, 40 and 80 µg/ml negativeb Jaju et al., 1986
lymphocytes
In vivo
Cytogenetic Mice bone 50 mg/kg bw positiveb,c Manna & Bardhan,
assay marrow 1973
a At doses that significantly inhibit the progression of the cell cycle.
b No positive control group was used.
c Test was not performed to current standards, i.e., results from 12 fixation
times are combined in 6 groups and number and sex of animals not stated.
Mitotic frequency was decreased; therefore, it was concluded that neomycin
reached the bone marrow.
2.2.7.3 Dogs
Six dogs (3/group) were administered 20 or 60 mg neomycin
sulfate/kg bw/day for 88 days (route not specified). All 3 dogs in
the high-dose group died after 14, 16 and 21 days. One low-dose dog
survived. The other 2 died after 21 and 45 days. Urine samples from
all dogs were taken before and after the beginning of treatment and
analyzed for albumin, blood and the presence of casts.
Histopathological examinations of kidneys showed degeneration,
necrosis and focal interstitial nephritis in all 6 dogs (Feenstra,
1950).
Twelve dogs were injected intramuscularly with 24, 48, or 96
mg/kg bw/day neomycin. At the highest dose all dogs died within 1-3
weeks. Blood urea nitrogen was increased and renal function impaired
as shown by decreased phenolsulfonphthalein excretion.
Histopathological evaluation of kidneys revealed renal tubular damage
characterized by marked epithelial necrosis in the proximal convoluted
tubules. Moderate changes in bone marrow and marked congestion of the
liver were also found. Inflammation at injection sites was also
noted. At the mid-dose the severity of effects were described as
intermediate. Dogs exposed to 24 mg/kg bw/day were killed and
examined after 1 month. The severity of renal damage in this group
was described as slight with increased granularity and occasional
desquamation of epithelial cells being most evident (Nelson et al.,
1951).
No kidney damage was observed in dogs (number/sex/group not
stated) orally dosed with 100 mg neomycin/kg bw/day for 6 weeks based
on urinalyses and gross and histopathological examinations of kidneys.
No other abnormalities were observed (Poth et al., 1951).
2.2.8 Special studies on ototoxicity
2.2.8.1 Guinea-pigs
Groups of 3 guinea-pigs were administered i.m. doses of 25, 50,
100, or 150 mg neomycin/kg bw/day for 30 to 60 weeks. Parameters
evaluated included vestibular function, auditory function (Preyer's
reflex) and histolopathological examination of labyrinths and central
nervous systems.
One guinea-pig in the high-dose group died after 22 days on test.
Vestibular function was reported as normal or slightly impaired across
all treatment groups with no dose-response relationship. Preyer's
reflex was abolished in all guinea-pigs receiving 100 and 150 mg/kg
bw/day. Histopathological examinations of animals in which the
Preyer's reflex was abolished revealed marked destruction of hair
cells and sometimes complete destruction of the organ of Corti.
Animals with intact hearing had normal cochleae, cristae, and maculae.
Reversible as well as irreversible degeneration of the ganglion cells
was seen in animals with abolished hearing, while animals with intact
hearing showed no definite pathological changes (Riskaer et al.,
1956) .
Hearing was not affected (determined by audiometry) after the
installation of 3 mg/kg bw neomycin into the middle ear of 18 guinea-
pigs. Six of the test animals had either one or both tympanic
membranes perforated prior to treatment (Riskaer et al., 1956).
Groups of guinea-pigs (50/sex/group) were orally admini-stered
neomycin B sulfate at 0, 1, 5, or 10 mg/kg bw/day for 90 days. Two
positive control groups (20/sex/group) received 10 or 100 mg/kg bw/day
s.c. for 90 and 34 days, respectively. Parameters evaluated included
clinical signs, body weight, auditory function test (Preyer pinna
reflex), gross necropsy, and histopathology (including cochleae to
score the loss of hair cells from the organ of Corti).
At 100 mg/kg bw/day s.c., ototoxic changes in the Preyer pinna
reflex thresholds and cochlear hair cell counts were observed. These
changes were not seen in the low-dose s.c. group nor in any of the
groups after oral administration. The NOEL for orally administered
neomycin in this study was 10 mg/kg bw/day (Brummett et al., 1985).
2.2.8.2 Cats
A clinical neomycin formulation (containing mostly neomycin B
sulfate), neomycin A hydrochloride and neomycin B sulfate were
administered s.c. to groups of cats (number/sex/group not stated) in
daily doses of 80 mg/kg bw/day for 5 or 15 days. The clinical
formulation was also administered in doses of 20, 40, or 100 mg/kg
bw/day s.c. for periods of 90, 60 and 30 days, respectively. Crude
neomycin (about 70% pure) was orally administered at 2 daily doses of
500 mg/kg bw (1 g/animal/day) for 30 days. Vestibular function was
studied by electrical recording of nystagmus evoked by rotating the
animal on a motor-driven turntable. Hearing ability was followed and
the cochlear function was studied electrophysically.
Histopathological examination of the kidneys was performed of all
cats.
Vestibular function was affected only in cats receiving the
highest dose of the clinical formulation (100 mg/kg bw/day) for 30
days. One of these cats showed a gradual loss of nystagmus which was
entirely absent by day 35, 5 days after the last treatment. Depression
of cochlear function was observed in all groups of cats and was most
severe in cats receiving the clinical preparation s.c. Degeneration
of external hair cells in the organ of Corti and internal hair cells
was also observed. A dose-related increase in the severity of damage
to renal tubular epithelium occurred in all cats receiving the
clinical preparation s.c. and in cats orally dosed with crude neomycin
(Hawkins, 1952; Hawkins et al., 1953).
Ototoxicity was studied in 5, 8, 3, and 4 cats who received oral
doses of 0, 6.25, 12.5, or 25 mg neomycin/kg bw/day, respectively, for
1 year. No evidence of auditory or vestibular dysfunction was
observed. In surface preparations of the organ of Corti
(cytocochleograms) ototoxicity was present microscopically as loss of
outer hair cells from the extreme lower portion of the basal turn of
the cochlea. Severe ototoxicity was observed in 3/4 high-dose cats.
Hair cell loss of a lesser degree was also observed in 7/8 and 1/3
cats in the low- and mid-dose groups, respectively (Kakuk, 1981). Due
to serious shortcomings in the histological technique and the absence
of a clear dose-related effect, the Committee considered this study
inadequate for the safety evaluation of neomycin.
2.2.9 Special studies on irritation and sensitization
No significant irritation was observed 24 hours after the
intrapleural administration of single doses of solutions of 1 ml
neomycin sulfate (0-100 mg/ml) to guinea-pigs (3-4/dose) (Swoap,
1951c).
A group of 9 neomycin-sensitive guinea-pigs was evaluated with
the patch test for cross sensitivy to kanamycin, streptomycin,
dihydrostreptomycin and bacitrin. Positive results were obtained for
kanamycin (1/9) and streptomycin (8/9) (Epstein & Wenzel, 1962).
2.2.10 Special studies on microbiological effects
Neomycin is active against most gram-positive and gram-negative
rods, many gram-positive cocci, and such acid-fast pathogens as
Mycobacterium tuberculosis.
Neomycin reacts with 30S ribosomal subunits of procaryotic cells
by electrostatic attraction causing a change in the conformation of
the ribosomal binding protein. This results in mRNA reading errors
and disrupted protein synthesis.
2.2.10.1 In vitro
Minimum Inhibitory Concentration (MIC) values for different
bacterial strains obtained from animal or human isolates are listed in
Tables 3 and 4, respectively.
In a special study, strains of various bacterial genera, mostly
of human origin, were tested for their susceptibility to neomycin
sulfate. MIC values were estimated on two agar types, Wilkens
Chalgren/glucose medium (WCG) and supplemented blood medium (SB) with
2 inoculum densities. Estimations were made under anaerobic and
aerobic conditions (E. coli) by the agar dilution method. The
results are listed in Table 5 (Thurn et al., 1994).
The adsorption of neomycin to dog faeces was calculated as the
difference between the amount of neomycin added to dilute suspension
of dog faeces and the amount of neomycin measured (microbioloigal
assay) in the supernatant after the mixture was incubated and
centrifuged. About 75% adsorption of neomycin was observed. After
acid extraction 47% of the added neomycin was still bound to the
faecal solids (Wagman et al., 1974).
Several concentrations of neomycin were evaluated for adsorption
to human faeces. Faecal samples were obtained from 8 healthy human
volunteers. The binding of neomycin to the faeces was calculated as
the difference between the amount added to a dilute suspension of
faeces and the amount measured (micro-biological assay) in the
supernatant after the mixture was incubated for 1 hour and
centrifuged. Approximately 83-98% faecal binding was observed
(Hazenberg et al., 1983b, 1984).
Neomycin solutions of approximately 0.1-30 mg/ml were mixed with
faecal suspensions prepared from faeces of 8 healthy human volunteers.
Neomycin antimicrobial activity (tested with Enterobacter cloacae)
remaining in the supernatants was measured and used for calculating
the "% inactivation" relative to the amount of added neomycin. The
percentage of added neomycin that was biologically inactivated
decreased with increasing concentrations of neomycin. Nearly 100%
inactivation due to binding occurred when the ratios of neomycin to
faecal weight were < 5 mg neomycin to 1 g wet weight of faeces in an
incubation mixture (Veringa & Van der Waaij, 1984).
2.2.10.2 In vivo
Oral administration of neomycin to 37 healthy mongrel dogs (400
mg/day for 2, 4, or 10 days) and 24 healthy humans (6 g/day for 1 or
3 days) caused a marked reduction or complete elimination of coliform
bacilli from faeces in both species within 24 to 48 hours. In 4/10
dogs receiving a dose of 400 mg/day for 10 days resistant strains of
E. coli appeared on the 5th-6th day of treatment. Resistance was
not observed in E. coli isolates from humans treated with neomycin
in this study (Schweinburg et al., 1952).
Groups of 3-5 human flora associated (HFA) mice (germ-free mice
colonized with bacteria from human faecal suspensions) were
administered 1, 2, 3 or 4 g/l neomycin in their drinking-water.
Faecal samples were cultured on days 0, 1, 3, 5, 7, 14, 21, 28 and 35
of treatment. A control group of HFA mice received no neomycin
treatment. The number of obligate anaerobes, gram negative obligate
anaerobes, E. coli and Enterococci did not change over 35 days
in the 1 g neomycin/l drinking-water group. In the 2 and 3 g
neomycin/l groups, Escherichia coli and Enterococci were
eliminated, and the percentage of gram-negative obligate anaerobes was
increased. The NOAEL in this study is 1 g/l, equal to 125 mg/kg bw/day
(Hazenberg et al., 1983a).
Table 3. Summary of MIC values for different bacterial species obtained from animal isolates
MIC (µg/ml)
Species No. of Mean or Range MIC50 Reference
strains
Staphylococcus aureus 0.5 Moellering, 1983
Escherichia coli 8.0
Klebsiella pneumoniae 2.0
Proteus mirabilis 8.0
Proteus morganii 8.0
Proteus rettgeri 8.0
Proteus vulgaris 4.0
Escherichia coli (calves) 16 Hewett, 1990
Escherichia coli (pigs) 16
Escherichia coli (chickens) 1
Salmonella sp. (calves) 1
Salmonella sp. (pigs) 0.5
Bacteroides nodosus 68 16 - >256 >256 Duran et
al. , 1991
Bacteroides putredinis 36 16 - >256 128
Bacteroides buccae 16 2 - >256 128
Bacteroides sp. 21 8 - >256 >256
Table 3 (contd)
MIC (µg/ml)
Species No. of Mean or Range MIC50 Reference
strains
Fusobacterium necrophorum 10 16 - >256 128
Fusobacterium sp. 19 2 - >256 128
Peptostreptococus sp. 35 <0.06 - >256 64 Piriz et al., 1992
Table 4. Summary of MIC values for different bacterial species obtained from
human isolates
MIC (µg/ml)
Species No. of Mean or range Reference
strains
Escherichia coli 10 0.25 - 12.5 Schweinberg et al.,
1952
Enterococci 5 3.2 - 15
Sphaerophorus necrophorus 7 200 - 1600 Finegold et al.,
1967
Bacteroides fragilis 55 1600 - >25 600
Bacteroides melaninogenicus 20 <100 - 400
Bacteroides oralis 16 <100 - 400
Fusobacterum sp. 22 100 - 3200
Bifidobacterium adolescentis 11 12.5 - 400 Miller & Finegold,
1967
Bifidobacterium bifidum 5 400 - 1600
Bifidobacterium longum 11 200 - 1600
Bifidobacterium sp. 6 200 - 1600
Clostridium novyi Type A 16 32 - 512 Dornbusch et al.,
1975
Clostridium novyi Type B 7 64 - 512
Clostridium bifermentans 9 64 - 512
Clostridium sordellii 6 64 - 512
Clostridium sporogenes 18 32 - 512
Table 4 (contd)
MIC (µg/ml)
Species No. of Mean or range Reference
strains
Propionicum agnes 38 6.25 - 25 Hoeffler & Pulverer,
1976
Escherichia coli 2 16 Hazenberg et al.,
1983b
Escherichia coli 3 1 - 32 Hazenberg et al.,
1984
Table 5. Summary of MIC values under different agar medium and inoculum density conditions
MIC50 (µg/ml)a
Bacterial species/genus Strains Low densityb High densityc
SBd WCGd SBd WCGd
Bacteroides 15e,f >128 >128 >128 >128
Bifidobacterium 12e 16 128
Clostridium 11e, 5f >128 128 >128
Enterococcus 10e, 2f >128 128 >128 >128
Escherichia 13e 16 64
Escherichia - Aerobic 13e >128 >128
Eubacterium - Anaerobic 9e 8 >128
Fusobacterium 5e, 3f 16 32 >128 128
Lactobacillus 15e, 2f >128 32 >128 64
Peptostreptococcus/ 16e, 14f >128 32 >128 128
Peptococcus
a MIC50 values are for the multiple strains included in the assay.
b Low density inocula had cell concentrations of approx. 1 x 108 cells/ml.
c High density inocula had cell concentrations of approx. 1 x 1010 cells/ml.
d SB = Supplemented blood medium; WCG = Wilkins-Chalgren/glucose medium
e Number of tested strains of which MIC values for WCG were used to
calculate the summary values
f Number of tested strains of which MIC values for SB were used to
calculate the summary values
2.2.10.3 Special studies on potential effects on microorganisms used
for industrial food processing
Thirty strains of Propionobacterium sp., used to manufacture
Emmenthal and related cheese varieties, showed no resistance to 30
µg/disc neomycin but at 5 µg/disc moderate sensitivity was observed
(8/30 strains were resistant) (Reddy et al., 1973).
Forty-two strains of mesophilic lactic Streptococci,
Enterococci, Lactobacilli, Leuconostoc, Staphylococci and
other dairy- and food-related microorgansims were tested for their
sensitivity to neomycin at 5 and 30 µg/disc. Elliker's lactic agar
served as the growth medium; incubations temperature and times were
varied according to individual culture growth requirements.
Most of the strains of the starter streptococci (S. lactis,
S.cremoris, S. diacetilactis and S. thermophilus) and Lactobacillus
bulgaricus were sensitive to neomycin. Strains of S. faecalis,
exhibited resistance at 5 and 30 µg/disc (Reinbold & Reddy, 1974).
In another study, 24/29 strains of Lactobacillus bulgaricus
and all 15 tested strains of Streptococcus thermophilus were
resistant to 5 µg/disc neomycin. The tests for resistance were
carried out with commercially available sensitivity disks. At higher
doses of neomycin (30 µg/disc) resistance in 14/15 strains of
S.thermophilus and 10/29 strains of L. bulgaricus was observed
(Sozzi & Smiley, 1980).
The effect of residues of neomycin in milk on bacterial starter
cultures used in the production of fermented milk products was
investigated. Milk samples spiked with either 4 or 40 µg/ml neomycin
were serially diluted with antibiotic-free milk to provide
concentrations ranging from 0.063-4 µg/ml. Actual concentrations
measured with a microbiological cylinder plate assay ranged from
<0.20-3.12 µg/ml (detection limit: 0.20 µg/ml). The starter culture
types included a group of buttermilk/sour cream cultures containing
strains of Lactococcus lactis spp. and spp. cremoris or a
mixture of lactic acid producers and citric acid fermenters, 2 groups
of Italian cheese cultures containing strains of Streptococcus
thermophilus, another group of Italian cheese cultures containing
strains of Lactobacillus helveticus, and a group of yogurt cultures
containing Streptococcus thermophilus and Lactobacillus debruckii
spp. bulgaricus. "Time to clot" ratios greater than 2 indicated
that cultures were adversely affected by the presence of neomycin.
The only cultures adversely affected were the yogurt starter cultures
at a neomycin concentration of 4 µg/ml (equivalent to 3.12 µg/ml). In
this study neomycin concentrations in milk <2 µg/ml (equivalent to
1.42 µg/ml) had no effect on the growth of the bacteria in any of the
starter cultures (Hallberg et al., 1994).
2.3 Observations in humans
2.3.1 Nephrotoxicity
A clinical investigation of 63 patients (34 males and 29 females
ranging in age from nine months to 63 years (22 of them >60 years) on
neomycin therapy was undertaken. Renal toxicity and ototoxicity
toxicity were reported as treatment-related effects in some patients.
Twenty-four out of 32 patients, in whom serial urinalyses were
performed, showed fine granular casts in their urine either during or
just after neomycin therapy (Waisbren & Spink, 1950).
Powell and Hooker (1956) reported several cases of severe tubular
damage found in kidneys at autopsy of patients treated intramuscularly
with neomycin.
Oral administration of decreasing doses of neomycin (9.4- 1.5 g/d
(total 46 g over 11 days) to a patient produced acute renal failure
(Greenberg & Momary, 1965).
2.3.2 Ototoxicity
Ototoxic effects determined by audiograms and vestibular
functional tests were observed in patients treated with neomycin at
doses ranging from 1.5-2 g/day i.m. for up to 9 days. Hearing loss
was reported in 5 patients and loss of vestibular function occurred in
2 patients (Waisbren & Spink, 1950).
Deafness with histopathological inner ear changes were reported
in patients receiving high doses of neomycin orally (18 to 633 g total
dose) for unspecified periods of time (Lindsay et al., 1960;
Halpern & Heller, 1961; Greenberg & Momary, 1965).
Severe deafness occurred in a 1´-year old female, treated for
enteritis for 10 days with a neomycin-containing medication. The
total dose of neomycin was less than 2 g (King, 1962).
Severe deafness was reported in a 75 year-old female patient
receiving colonic and rectal irrigations with a neomycin solution for
2 months. A 5% solution was administered initially, then decreased to
a 1% solution for the majority of the treatment period. The total
neomycin dose administered was estimated at >900 g. The patient had
a hearing deficit but did not require a hearing aid prior to treatment
(Fields, 1964).
2.3.3 Hypersensitivity
From a survey of 675 patients with skin infections treated with
neomycin it was concluded that the sensitizing index for neomycin was
very low (Kile et al., 1952). However, cases of contact dermatitis
from neomycin (e.g., eardrops and eyedrops) were reported as dermal
delayed (tuberculin-type) and not epidermal sensitivity (Epstein,
1956; Calnan & Sarkany, 1958). In 55-75% of patients with neomycin
sensitivity, evidence of atopy (a genetic predisposition to mounting
large immune responses to antigenic stimulation) was established
(Epstein, 1965).
Results of patch tests with 21 antibiotics performed on a large
number of patients sensitive to neomycin showed cross-sensitivity to
bacitracin (80%), framycetin (91%), paromomycin (up to 99%) and
kanamycin (61%) (Pirila & Rouhunkoski, 1962). Cross-sensitization
with neomycin in streptomycin-sensitized patients was also described,
although contradictory results were obtained with respect to the
neomycin sensitivity in streptomycin-sensitive patients
(Sidi et al., 1958; Calnan & Sarkany, 1958).
A patient treated with ear drops containing neomycin (5 mg/ml in
distilled water) developed an acute exacerbation of otitis externa
after previously having shown a highly satisfactory response to the
use of the neomycin ear drops (Baer & Ludwig, 1952).
2.3.4 Special studies on the malabsorption syndrome
Morphologic alterations in the jejunal mucosa of patients,
similar to but less marked than those seen in patients with idiopathic
steatorrhea, were seen in 11/12 biopsy specimens from patients treated
with neomycin (4-12 g/day) for at least 4 days. Eighteen days after
the last dose of neomycin the jejunal morphology was restored
(Jacobson et al., 1960).
During the oral administration of 4-6 g neomycin/day for 6-8 days
plasma carotene concentrations were decreased in 6/8 patients despite
the administration of supplemental carotene (10 000 units/day). In
addition, d-xylose excretion in urine was decreased in 3/4 subjects.
Faecal fat excretion doubled during the treatment period in 1 patient
(Jacobson & Faloon, 1961).
Neomycin sulfate was administered orally (12 g/day for 4 days) as
well as by inlying tube directly into the jejenum and ilieum in 11
subjects. Urine and faeces were evaluated for fat, calcium, sodium,
potassium and nitrogen content. Steatorrhea was produced after oral
administration, but when neomycin was administered more distally, the
faecal fat content progressively diminished. Lowest urinary calcium,
sodium and potassium levels were measured after oral administration.
Faecal sodium, potassium and nitrogen levels were less affected by
this administration route, whereas the faecal calcium content was
greatest after jejunal instillation. The steatorrhea could not be
reversed by the administration of bile salts, sodium bicarbonate or
pancreatic enzymes (Gordon et al., 1968).
Three healthy male volunteers were orally administered 8 g
neomycin sulfate/day for 7 days. Lactose malabsorption was induced
after 3 days of treatment. Biopsy specimens from the small bowel
taken after 7 days of treatment showed slight villous blunting of the
mucosa and depressed disaccharidase activity. The lamina propria was
infiltrated with plasma cells and eosinophils. Enzyme levels and
histology of the mucosa and lamina propria of the small bowel returned
to normal 10 to 14 days after the treatment was stopped. No
treatment-related effects on stool lactic acids were observed (Cain
et al., 1968).
2.3.5 Special studies on microbiological effects
In a study with 37 hospitalized patients with various types of
intestinal lesions, the effect of oral neomycin treatment on bacteria
from the intestinal tract was determined. Treatment regimes of
neomycin administered prior to surgery (duration not stated) were as
follows: 1.5 g 4 times/day; 2 g 3 times/day; or 1 g every hour for
four doses the first day, then 1.5 g 4 times/day. After the
administration of neomycin the only clinical observations were
occasional nausea and vomiting. In stool specimens from patients
treated with 1.5 g 4 times/day (30 mg/kg bw/day) most of the aerobic
bacteria ( E. coli, A. aerogenes, S. faecalis, Proteus and
Pseudomonas) disappeared within 1´-4´ days, whereas anaerobic
organisms ( Bacteroides and Clostridium) remained. No resistant
strains of Mycrococcus pyopgenes were found. Similar results were
seen in patients receiving 2 g 3 times/day. In the group receiving 1
g hourly for four doses followed by 1.5 g 4 times/day, aerobic
bacteria were removed from the intestinal tract within two to three
days, while anaerobes ( Bacteroides and Clostridium) persisted
(Deering & Needham, 1953).
The intestinal flora of 14 patients hospitalized for non-
gastrointestinal diseases was studied before and after the use of
neomycin. Four patients received 4 g neomycin orally for 7 days and 10
patients were given 2 g neomycin for 6 days. The bacterial populations
of faecal specimens collected before, during and after neomycin
treatment were enumerated. A decrease in all bacterial species was
noted. Most affected were Enterococci, followed by E.coli,
lactose non-fermenters, Lactobacilli, Clostridia and Proteus
sp. Yeast and Klebsiellae were increased (Daikos et al., 1968).
Seven healthy adult volunteers received 1 g neomycin orally 3
times a day for 5 days (equivalent to 50 mg/kg bw/day). Fresh stool
samples were collected before, during and after treatment, and
bacterial counts recorded. Neomycin treatment did not affect
Bacteroides or Clostridia counts. E. coli counts were
significantly reduced in 2/7 volunteers (Arabi et al., 1979).
3. COMMENTS
The Committee considered data on pharmacokinetics, acute
toxicity, short-term and long-term toxicity, reproductive and
developmental toxicity, genotoxicity and carcinogenicity, effects in
humans and effects on antimicrobial activity. An evaluation report,
as requested for veterinary drugs with a long history of use (Annex 1,
reference 104) was also provided.
Neomycin is poorly absorbed after oral administration, whereas
after parenteral administration it is readily bioavailable. In
calves, oral absorption was estimated at 1-11%, depending on age. In
humans, up to 3% of an oral dose was recovered in urine, indicating
low absorption. Of the neomycin present in blood, 45-55% was bound to
plasma proteins in cows and ewes and the remainder was present in
nonionized form and may cross tissue barriers. After oral
administration the compound is mainly excreted unchanged in the
faeces. After parenteral administration neomycin is mainly excreted in
the urine.
Single doses of neomycin were slightly toxic to mice after oral
administration (LD50 = 2250 mg/kg bw), but single i.v. doses in mice
were highly toxic (LD50 <100 mg/kg bw).
Nephrotoxic effects were observed in mice after repeated s.c.
administration of 30-300 mg neomycin/kg bw/day, in guinea-pigs after
repeated s.c. doses of 10-60 mg neomycin sulfate/kg bw/day, and in
dogs after repeated i.m. doses of 24-96 mg neomycin/kg bw/day. No
kidney damage was observed in dogs receiving 100 mg/kg bw/day orally
for 6 weeks. Ototoxicity was observed after parenteral administration
of neomycin ranging from 25 to 150 mg/kg bw/day in guinea-pigs, and
20 to 80 mg/kg bw/day in cats. No ototoxic effects were observed in
guinea-pigs following oral administration of up to 10 mg neomycin
sulfate/kg bw/day for 90 days. In cats orally administered 6.25, 12.5
or 25 mg of neomycin/kg bw/day for one year, auditory function was not
affected, but upon histopathological examination changes in the organ
of Corti were reported at all dose levels.
The Committee concluded that, although ototoxicity was observed
in the one-year study in cats at the lowest dose tested (6.25 mg/kg
bw/day), this study was inadequate for the safety evaluation of
neomycin because of serious shortcomings in the histological technique
and the absence of a clear dose-related effect. It, however, accepted
the NOEL of 10 mg neomycin sulfate/kg bw/day, equivalent to 6 mg
neomycin/kg bw/day, for ototoxicity from the study in guinea-pigs.
Only a limited number of mutagenicity studies were available,
which had been poorly performed. The available in vitro
genotoxicity tests indicated that neomycin causes chromosomal
aberrations.
The tumour incidence was not increased in a two-year toxicity and
carcinogenicity study with rats orally administered neomycin up to a
dose level of 25 mg/kg bw/day. In the high-dose males only a slight
but statistically non-significant impairment of hearing was observed.
Because the Committee regarded the observed impairment of hearing as
treatment-related, the NOEL was 12.5 mg/kg bw/day.
In a multi-generation reproductive toxicity study in rats in
which neomycin was administered orally, no effects on reproductive
parameters were observed up to a dose of 25 mg/kg bw/day, which was
the highest dose administered. A teratogenicity study with an
unconventional protocol was conducted with F2b female rats from the
reproductive toxicity study. Neomycin was administered in the feed at
0, 6.25, 12.5 or 25 mg/kg bw/day from days 0-6 and 16-20 of gestation.
Dose levels were raised to 62.5, 125 or 250 mg/kg bw/day from days 6-
15 of gestation. No malformations, feto-toxicity or maternal toxicity
were observed.
Skin reactions due to hypersensitivity have been observed in
humans after the therapeutic use of neomycin. Nephrotoxic effects and
ototoxicity have been observed in humans after oral therapeutic use of
neomycin.
From several in vitro microbiological studies with different
bacteria, mostly isolated from humans, an MIC50 of 64 µg/ml was
derived for the most relevant sensitive bacterial organisms
( Escherichia coli and Lactobacillus spp.) under conditions of
high inoculum density. In human-flora-associated mice the NOEL for
antibacterial activity was 125 mg/kg bw/day. Studies on the effect of
neomycin on human gut flora in patients revealed effects at oral doses
>30 mg/kg bw/day.
Applying the formula developed at the thirty-eighth meeting of
the Committee (Annex 1, reference 97) an ADI based on anti-microbial
activity could be calculated as follows:
Concentration without effect daily faecal
of ADI on human gut flora (µg/ml)a x bolus (g)
Upper limit =
of ADI fraction of oral x safety x Weight of human (60kg)
dose availableb factorc
64 x 150
=
1 x 1 x 60
= 160 µg/kg bw
a The MIC50 value of 64 µg/ml was measured in the most relevant
sensitive species under conditions of high inoculum density. No
adjustment was deemed necessary.
b A conservative estimate of 100% availability to human gut flora
was selected. Experimental data were inadequate to correct for
inactivation of neomycin as a result of binding to gut contents.
c A substantial amount of data covering a variety of organisms,
including anaerobes isolated from the human gut, were available.
Also in view of the applied conservative factor for the availability
of neomycin to the gut flora a safety factor of 1 was adopted.
In reviewing the available toxicological and antimicrobial data
the Committee concluded that the toxicological data provided the most
appropriate endpoint for the evaluation of neomycin.
Only a limited set of genotoxicity tests was available, with gene
mutation studies in eukaryotic cells being absent. The available
information indicates that neomycin causes chromosomal aberrations.
However, the Committee noted that the long-term study in rats did not
provide evidence for a carcinogenic potential of neomycin.
The Committee established a temporary ADI of 0-30 µg/kg bw based
on the NOEL of 6 mg/kg bw/day for ototoxicity in the guinea-pig and a
safety factor of 200. The ADI was made temporary in view of the
deficiencies in the genotoxicity data.
5. REFERENCES
ARABI, Y., DIMOCK, F., BURDON, D.W., WILLIAMS, J.A. & KEIGHLEY, M.R.R.
(1979). Influence of neomycin and metronidazole on colonic microflora
of volunteers. J. Antimicrobial. Chemother., 5: 531-537.
ASCHBACHER, P.W. & FEIL, V.J. (1991). Fate of oral 14C Neomycin in
calves. USDA, ARS, Biosciences Research Laboratory, Farbo, ND.
J. Animal Science, 69(1): 733.
ASCHBACHER, P.W. & FEIL, V.J. (1994). Neomycin metabolism in calves.
J. Animal Science, 72: 683-689.
ATEF, M., EL-GENDI, A.Y.I., EL-SAYED, M.G.A. & A.M.M.AMER (1986).
Certain physico-pharmacologic properties of neomycin in chickens.
Arch. Geflügelk, 50(4): 132-135.
BAER, R.L. & LUDWIG, J.S. (1952). Allergic eczematous sensitization to
neomycin. Annals of Allergy, March-April: 136-137.
BEVAN, J.A. & THOMPSON, J.H. (1983). Introduction to principles of
drug action. Essentials of pharmacology, 3rd Ed. Harper and Row,
Philadelphia.
BREEN, K.J., BRYANT, R.E. LEVINSON, J.D. & SCHENKER, S. (1972).
Neomycin studies in man. Studies of oral and enema administration and
effect of intestinal ulceration. Ann. Intern. Med., 76: 211-218.
BROCKIE, P.H. (1951). Acute toxicity test with neomycin sulphate dated
2-22-1951. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
BRUMMETT, R.E., HALL, A.D. & RUSSELL, K.B. (1985). Ninety-day oral
neomycin sulfate (U-4,567) Ototoxicity study in the guinea-pig.
Technical report No. 7263/85/068 dated 23 october 1985. Submitted to
WHO by The Upjohn Company, Kalamazoo, MI, USA.
CAIN, C.D., REINER, E.B. & PATTERSON, M. (1968). Effects of neomycin
on disaccharidase activity of the small bowel. Arch. Intern Med.,
122: 311-314.
CALE , R.J. (1950). Memo dated 1950, subject : Toxicity neomycin
sulfate. Ssubmitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
CALNAN,C.D. & SARKANY, I. (1958). Contact dermatitis from neomycin.
Brit. J. Dermatol., 70: 435-445.
DAIKOS, G.K., KONTOMICHALOU, P. BILALIS, D. & PIMENDOU. L. (1968).
Intestinal flora ecology after oral use of antibiotics. Chemotherapy,
13: 146 - 160.
DEERING, W.H. & NEEDHAM, G.M. (1953). Effects of oral administration
of neomycin on the intestinal bacterial flora of man. Staff meeetings
of the Mayo Clinic, September 9, 502-507. Submitted to WHO by The
Upjohn Company, Kalamazoo, MI, USA.
DORNBUSCH, K., NORD, C.E. & DAHLBECK, A. (1975). Antibiotic
susceptibility of clostridium dpecies isolated from human infections.
Scand. J. Infect. Dis., 7: 127-134.
DURAN, S.P., VALERA, R.G., MANZANO, J.V. & MACHOTA, V. (1991).
Comparative in vitro susceptibility of Bacteroides and
Fusobacterium isolated from footrot in sheep to 28 antimicrobial
agents. J. Vet. Pharmacol. Therap., 14: 185-192.
EPSTEIN, S. (1956). Contact dermatitis from neomycin due to dermal
delayed (tuberculin-type) sensitivity. Dermatologica, 113(4): 191-
201.
EPSTEIN, S. (1965). Neomycin sensitivity and atopy. Dermatology,
130: 280-286.
EPSTEIN, S. & WENTZEL, F.J. (1962). Cross-sensitivity to various
"Mycins" Neomycin, Kanamycin, Streptomycin and Bacitracin: an
experimental study. Arch. Dermatol., 86: 183-194.
FEENSTRA, E.S. (1950). Interoffice memorandum of pathology report -
Chronic toxicity (s Mo.) of Neomycin sulfate #9084-10 in guinea-pigs
and dogs, dated 22 August 1950. Submitted to WHO by The Upjohn
Company, Kalamazoo, MI, USA.
FEENSTRA, E.S. (1954). Interoffice memorandum: Comparative
nephrotoxicity of neamine, neomycin B and neomycin C, Preliminary
report dated 22 September 1954. Submitted to WHO by The Upjohn
Company, Kalamazoo, MI, USA.
FEENSTRA, E.S. (1958). Unpublished technical acute toxicity i.p.
neomycin sulphate. dated 8 July 1958. Submitted to WHO by The Upjohn
Company, Kalamazoo, MI, USA.
FEENSTRA, E.S. (1959). Unpublished technical acute toxicity i.p.
neomycin sulphate. dated 19 January 1959. Submitted to WHO by The
Upjohn Company, Kalamazoo, MI, USA.
FIELDS, R.L. (1964). Neomycin ototoxicity. Arch. Otolaryngol., 79:
67-70. FINEGOLD, S.M., HARADA, N.E. & MILLER, L.G. (1967). Antibiotic
susceptibility Patterns as aids in classification and characterization
of gram-negative anaerobic bacilli. J. Bacteriol., 94(5): 443-350.
GORDON, S.J., HARO, E.N., PERS, I.C. & FALOON, W.W. (1968). Studies of
malabsorption and calcium excretion induced by neomycin sulfate.
Effect of intestinal site, bile salt and pancreatic enzymes. JAMA,
204: 129-134.
GRAY, J.E. (1964). Interoffice memorandum to E.S. Feenstra d.d. 6-5-
1964 LD50 neomycin sulfate submitted to WHO by The Upjohn Company,
Kalamazoo, MI, USA.
GREENBERG, L.H. & MOMARY, H. (1965). Audiotoxicity and nephrotoxicity
due to orally administered neomycin. JAMA, 194: 827-828.
HALL, A.D., SKINNER, P.J. & BARBIERS, A.R. (1983). A preliminary study
of the absorption of neomycin sulfate following oral administration to
guinea-pigs. Unpublished technical report No. 756-9610=83-001 dated
18-1-1983 from The Upjohn Company, Agricultural Research and
development laboratories, Kalamazoo Michigan , USA. Submitted to WHO
by The Upjohn Company, Kalamazoo, MI, USA.
HALLBERG, J.W., CHESTER, S.T., DAME, K.J., HORNISCH, R.E., TRAVIS,
M.A. & CORNELL, C.P. (1994). Effect of neomycin in milk on the
performance of cheese and yoghurt starter cultures. Unpublished
technical report No. 802-9690-94-001 dated 16 September 1994 from The
Upjohn Company, Agricultural Division. Submitted to WHO by The Upjohn
Company, Kalamazoo, MI, USA.
HALPERN, E.B. & HELLER, M.F. (1961). Ototoxicity of orally
administered neomycin. Arch. Otolaryngol., 73: 675-677.
HAWKINS, J.E. (1952). The ototoxicity of the neomycins. Trans. 11th
Conf. Chemother. of Tuberculosis, p. 189-191. Submitted to WHO by The
Upjohn Company, Kalamazoo, MI, USA.
HAWKINS, J.E., RAHWAY, N.J. & LURIE, M.H. (1953). The ototoxicity of
dihydrostreptomycin and neomycin in the cat. Ann. Otol. Rhin.
Laryngol., 62: 1128-1148.
HAZENBERG, M.P., VAN DE BOOM, M. BAKKER, M. & VAN DE MERWE, J.P.
(1983a). Effect of antibiotics on the human intestinal flora in mice.
Antonie van Leeuwenhoek, 49: 97-109.
HAZENBERG, M.P., VAN DE BOOM, M. BAKKER, M. & VAN DE MERWE, J.P.
(1983b). Binding to faeces and influence on human anaerobes of
antimicrobial aganets used for selective decontimination. Antonie van
Leeuwenhoek, 49: 111-117.
HAZENBERG, M.P., PENNOCK-SCHRODER, A.M., VAN DEN BOOM, M. & VAN DE
MERWE, J.P. (1984). Binding to and antibacterial effect ampicillin,
neomycin and polymyxin B on human faeces. J. Hyg.Camb., 93: 27-34.
HEATH, G.E. (1985). The pharmacokinetics of neomycin in the serum of
calves and young cross-bred swine. Thesus, University of Minnisota.
Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
HEWETT, G.R. (1990). Determination of the minimum Inhibitory
Concentration (MIC) of neomycin sulphate versus Salmonellae Species
and Escherichia coli isolated from calves, pigs and chicks.
Unpublished technical report No. 004-AHTR-9542-90-007 dated 3 May,
1990 from Agricultural Research and Development Laboratories, The
Upjohn Company U.K. Submitted to WHO by The Upjohn Company, Kalamazoo,
MI, USA.
HOEFFLER, E.H.L.K. & PULVERE, G. (1976). Antimicrobial susceptibility
of Propionibacterium acnes and related microbiological species.
Antimicrob. Ag. Chemother., 10(3): 387-394.
JACOBSON, E.D., PRIOR, J.T. & SYRACUSE, N.Y. (1960). Malabsorptive
syndrome induced by neomycin: morphological alterations in the jejunal
mucosa. J. Lab. Clin. Med., 56(2): 245-250.
JACOBSON, E.D. & FALOON, W.W. (1961). Malabsorptive efefcts of
neomycin in commonly used doses. JAMA, 175(3): 187-190.
JAJU, M., JAJU, M. & AHUJA, Y.R. (1986). Cytogenetic effect of
neomycin on human lymphocytes in vitro. Ind. J. Exp. Biol., 24:
595-598.
KAKUK, T.J. (1980). Neomycin sulfate: three-generation rat
reproductive teratology study. Technical report No. 756-9610-80-002
dated 30 November 1980, Agricultural Research and Development
Laboratories, The Upjohn Company. Submitted to WHO by The Upjohn
Company, Kalamazoo, MI, USA.
KAKUK, T.J. (1981). Neomycin sulfate: one-year tolerance study in the
domestic cat. Tecnical report No. 756-9610-81-001 dated 19 October
1981, Agricultural Research and Development Laboratories, The Upjohn
Company. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
KAKUK, T.J. (1982). Neomycin sulfate: lifetime feeding study in the
rat (Study #T-702)/Technical report No. 756-9610-82-001 dated 14
September 1982, Agricultural Research and Development Laboratories,
The Upjohn Company. Submitted to WHO by The Upjohn Company, Kalamazoo,
MI, USA.
KEEN, P. (1975). Some aspects of the pharmacology of antibiotics in
the cat and dog. J. Small Anim. Pract., 16: 767-773.
KILE, R.L., ROCKWELL, E.M. & SCHWARTZ, J. (1952). Use of neomycin in
dermatology. JAMA, 148(5): 339- 343.
KING, J.T. (1962). Severe deafness in an infant following oral
administration of neomycin. J. Med. Assoc. Georgia, 51: 530-531.
KUBINSKI, H., GUTZKE, G.E. & KUBINSKI, Z.O. (1981). DNA-cell-binding
(DCB) assay for suscpected carcinogens and mutagens. Mutat. Res.,
89: 95-136.
LINDSAY, J.R., PROCTOR, L.R. & WORK, W.P. (1960). Histopathological
inner ear changes in deafness due to neomycin in a human.
Laryngoscope, 70: 382-392.
MANNA, G.K. & BARDHAN, S. (1973). Effects of two antobiotics on the
chromosomes and mitotic frequency in the bone marrow cells of mice.
Chromosomes Today, 4: 277-282.
MILLER, L.G. & FINEGOLD, S.M. (1967). Antibacterial sensitivity of
Bifidobacterium (Lactobacillus bifidus). J. Bacteriol., 93(1): 125-
130.
MOELLERING, R.C. (1983). In vitro antibacterial activity of the
aminoglycoside antiobiotics. Rev. Infect. Dis., 5(2): S212-S231.
NELSON, A.A., RADOWSKI, J.L. & HAGAN, E.C. (1951). Renal and other
lesions in dogs and rats from intramuscular injection of neomycin.
Fed. Proc. 10(1): 366-367.
PIRILA, V., & ROUHUNKOSKI, S. (1962). The pattern of cross-sensitivity
to neomycin. Dermatologica, 125: 273-278.
PIRIZ, S., CUENCA, R. VALLE, J. & VADILLO, S. (1992). Susceptibilities
of anaerobic bacteris isolated from animals with ovine foot rot to 28
antimicrobial agents. Antimicrob. Ag. Chemother., 36(1): 198-201.
POTH, E.J., MARTIN, R.G., FROMM, S.M., WISE, R.I. & HSANG, C.M.
(1951). A critical analysis of neomycin as an intestinal antiseptic.
Tex. Rep. Biol. Med., 9: 631.
POWELL, L.W. & HOOKER, J.W. (1956). Neomycin nephropathy. JAMA,
160: 557-560.
REINBOLD, G.W. and REDDY, M.S. (1974). Sensitivity or resistance dairy
starter and associated microorganisms to selected antibiotics.
J. Milk Food Technol., 37(10): 517-521.
REDDY, M.S., REINBOLD, G.W. & WILLIAMS, F.D. (1973). Inhibition of
propionibacteria by antibiotic and antimicrobial agents. J. Milk Food
Technol., 36(11): 564-569.
RISKAER, N., CHRISTENSEN, E. PETERSEN & WEIDMAN, H. (1956). The
otoxicity of neomycin. Experimental investigations. Acta
Otolaryngol., 46: 137-152.
SCHWEINBURG, F.B., JACOB, S. & RUTENBURG, A.M. (1952). Effect of oral
Neomycin on normal intestinal flora of dogs and man. Proc. Soc. Expr.
Biol. & Med., 335-338.
SHEALY, Y.F. (1956). Technical unpublished report TUC No. U-4567 of
the acute toxicity of neomycin sulphate dated 6 July 1956. Submitted
to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SIDI, E., HINCKY. M. & LONGUEVILLE, R. (1958). Cross-sensitization
between neomycin and streptomycin. J. Invest. Dermatol., 30: 225-
231.
SOZZI, T. & SMILEY, M.B. (1980). Antibiotic resistance of Yogurt
starter cultures Streptoccus thermophilus and Lactobacillus
bulgaricus. Appl. Environm. Microbiol., 40(5): 862-865.
SWOAP, O.F. (1949a). Memo dated 12-2-1949, subject: Toxicity studies
on neomycin. Submitted to WHO by The Upjohn Company, Kalamazoo, MI,
USA.
SWOAP, O.F. (1949b). Memo dated 12-19-1949, subject: Toxicity studies
on neomycin SO4. Submitted to WHO by The Upjohn Company, Kalamazoo,
MI, USA.
SWOAP, O.F. (1950a). Memo on subject: Toxicity studies on SO4.
Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1950b). Memo dated 3-24-1950, subject: Toxicity: neomycin
SO4. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1950c). Memo dated 4-6-1950, subject: Toxicity: Neomycin
sulfate. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1950d). Memo dated 4-6-1950, subject: Toxicity: neomycin
sulfate. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1950e). Memo dated 6-16-1950, subject: Toxicity: neomycin
sulfate. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1950f). Memo dated 11-16-1950, subject: Toxicity:
neomycin SO4. Submitted to WHO by The Upjohn Company, Kalamazoo, MI,
USA.
SWOAP, O.F. (1950g). Memo dated 12-1-1950, subject: Neomycin toxicity
testing. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1950h). Memo dated 12-4-1950, subject: Toxicity: neomycin
SO4. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1950i). Memo dated 12-8-1950, subject: Toxicity: neomycin
SO4. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1950j). Memo dated 12-21-1950, subject: Toxicity:
neomycin SO4. Submitted to WHO by The Upjohn Company, Kalamazoo, MI,
USA.
SWOAP, O.F. (1950k). Memo dated 12-21-1950, subject: Toxicity:
neomycin SO4. Submitted to WHO by The Upjohn Company, Kalamazoo, MI,
USA.
SWOAP, O.F. (1951a). Memo dated 1-17-1951, subject: Toxicity: neomycin
SO4. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1951b). Toxicology report dated 5-8-1951 on neomycin
sulfate. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1951c). Toxicology report dated 7-2-51 on neomycin
sulfate. Submitted to WHO by the Upjohn Company, Kalamazoo, MI; USA.
SWOAP, O.F. (1952a). Toxicology report dated 5-13-1952 on neomycin
(lot 91-cat-6). Submitted to WHO by The Upjohn Company, Kalamazoo, MI,
USA.
SWOAP, O.F. (1952b). Toxicology report dated 7-3-1952 compound: Bulk
powder neomycin sulfate ( from resin process). Submitted to WHO by The
Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1952c). Toxicology report neomycin sulphate dated 6-10-
1952. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1952d). Toxicology report neomycin sulphate dated 6-10-
1952a. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1952e). Toxicology report Bulk powder neomycin sulphate
(from resin process) dated 7-3-1952. Submitted to WHO by The Upjohn
Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1952f). Toxicology report I: Bulk powder neomycin
sulphate (from resin process) dated 25 september 1952. Submitted to
WHO by The Upjohn Company, Kalamazoo, MI, USA.
SWOAP, O.F. (1952g). Toxicology report II: Bulk powder neomycin
sulphate (from resin process) dated 25 september 1952. Submitted to
WHO by The Upjohn Company, Kalamazoo, MI 49001.
SWOAP, O.F. (1952h). Toxicology report III: Bulk powder neomycin
sulphate (from resin process) dated 25 september 1952 submitted to WHO
by The Upjohn Company, Kalamazoo, MI 49001.
SWOAP, O.F. (1953a). Toxicology report neomycin sulphate dated 12-2-
1953 submitted to WHO by The Upjohn Company, Kalamazoo, MI 49001.
SWOAP, O.F. (1953b). Interoffice memorandum dated 2-18-1953 subject:
meomycin B Submitted to WHO by The Upjohn Company, Kalamazoo, MI
49001.
SWOAP, O.F. (1954a). Memo acute toxicity no 983 Neomycin sulfate B
dated 24 September 1954, submitted to WHO by The Upjohn Company,
Kalamazoo, MI 49001.
SWOAP, O.F. (1954b). Interoffice memorandum - parallel toxicity tests
on neomycin B sulfate samples (U-4567) dated 30 September 1954,
submitted to WHO by The Upjohn Company, Kalamazoo, MI 49001.
SWOAP, O.F. (1957a). Memo - acute toxicity neomycin sulphate dated 1
November 1957, submitted to WHO by The Upjohn Company, Kalamazoo, MI,
USA.
SWOAP, O.F. (1958). Memo - acute toxicity neomycin sulphate Po.
Blended USP. 21 march 1958. Submitted to WHO by The Upjohn Company,
Kalamazoo, MI, USA.
THURN, K.K., BAKER, K.D., GREENING, R.C. & KOTARSKI, S.F. (1994).
Minimum inhibitory concentrations of neomycin sulfate against
bacterial species frequently isolated from the human gastrointestinal
tract. Unpublished technical report No. 802-7928-94-001 from The
Upjohn Company, Upjohn Laboratories, Kalamazoo, MI USA 49001.
Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
VAN DER BROOK, M.J. (1949). Memo dated 6-15-1949 about toxicity on
neomycin. Submitted to WHO by The Upjohn Company, Kalamazoo, MI, USA.
VERINGA, E.M. & VAN DER WAAIJ, D. (1984). Biological inactivation by
faeces of antimicrobial drugs applicable in selective decontamination
of the digestive tract. J. Antimicrob. Chemother., 14: 605-612.
WAGMAN, G.H., BAILEY, J.V. & WEINSTEIN, M.J. (1974). Binding of
aminoglycosides to feces. Antimicrob. Ag. Chemother., 6(4): 415-
417.
WAISBREN, B.A. & SPINK, W.W. (1950). A clinical appraisal of neomycin.
Ann. Int. Med., 33: 1099-1119.
ZIV, G. & SULMAN, F.G. (1972). Binding of antibiotics to bovine and
ovine serum. Antimicrob. Ag. Chemother., 2(3): 206-213.
ZIV, G. & SULMAN, F.G. (1974). Distribution of aminoglycoside
antibiotics in blood and milk. Res. Vet. Sci., 17: 68-74.
