
INTERNATIONAL PROGRAMME ON CHEMICAL SAFETY
ENVIRONMENT HEALTH CRITERIA 23
LASERS AND OPTICAL RADIATION
This report contains the collective views of an international group of
experts and does not necessarily represent the decisions or the stated
policy of the United Nations Environment Programme, the International
Labour Organisation, or the World Health Organization.
Published under the joint sponsorship of
the United Nations Environment Programme,
the International Labour Organisation,
and the International Radiation Protection Association
World Health Orgnization
Geneva, 1982
ISBN 92 4 154083 4
The World Health Organization welcomes requests for permission
to reproduce or translate its publications, in part or in full.
Applications and enquiries should be addressed to the Office of
Publications, World Health Organization, Geneva, Switzerland, which
will be glad to provide the latest information on any changes made
to the text, plans for new editions, and reprints and translations
already available.
(c) World Health Organization 1982
Publications of the World Health Organization enjoy copyright
protection in accordance with the provisions of Protocol 2 of the
Universal Copyright Convention. All rights reserved.
The designations employed and the presentation of the material
in this publication do not imply the expression of any opinion
whatsoever on the part of the Secretariat of the World Health
Organization concerning the legal status of any country, territory,
city or area or of its authorities, or concerning the delimitation
of its frontiers or boundaries.
The mention of specific companies or of certain manufacturers'
products does not imply that they are endorsed or recommended by the
World Health Organization in preference to others of a similar
nature that are not mentioned. Errors and omissions excepted, the
names of proprietary products are distinguished by initial capital
letters.
CONTENTS
ENVIRONMENTAL HEALTH CRITERIA FOR LASERS AND OPTICAL RADIATION
1. SUMMARY AND RECOMMENDATIONS FOR FURTHER STUDIES
1.1. Summary
1.1.1. Scope
1.1.2. Optical radiation exposure
1.1.3. Present health and safety standards
1.2. Recommendations for further studies
2. DEFINITIONS OF OPTICAL RADIATION
2.1. The electromagnetic spectrum
2.2. Interaction of electromagnetic radiation with matter
2.2.1. Interaction at an interface
2.2.1.1 Reflection
2.2.1.2 Refraction
2.2.2. Interaction with a medium
2.2.2.1 Transmission
2.2.2.2 Attenuation
2.2.3. Interference, diffraction and scattering effects
2.2.3.1 Interference and diffraction
2.2.3.2 Scattering
3. SOURCES OF RADIATION
3.1. Molecular and atomic transitions
4. LASERS
4.1. The laser medium
4.2. The pumping system
4.3. The resonant optical cavity
4.4. Types of lasers
4.4.1. Active media
4.4.2. Temporal modes of operation
4.5. Spatial (TEM) modes
4.6. Beam characteristics
4.6.1. Beam diameter
4.6.2. Beam divergence
4.6.3. Beam irradiance versus range for a circular beam
4.6.4. Hot spots
4.6.5. Coherence
5. RADIOMETRIC CONCEPTS
5.1. Radiometric and photometric terminology
5.2. Extended sources versus point sources
5.3. Inverse square law
6. RADIOMETRIC AND PHOTOMETRIC MEASUREMENT
6.1. Introduction
6.2. Measurement instrumentation
6.2.1. Thermal detectors
6.2.2. Quantum detectors
6.2.3. Detectors to resolve short pulses
6.2.4. Safety meters
6.2.5. Spectroradiometers
6.3. Biological weighting of spectroradiometric data
7. BIOLOGICAL EFFECTS
7.1. Thermal injury
7.2. Photochemical injury
7.3. Threshold of injury
7.3.1. Means of determining thresholds of injury
8. EFFECTS OF OPTICAL RADIATION ON THE EYE
8.1. Anatomy and physiology of the human eye
8.1.1. The cornea
8.1.2. The lens
8.1.3. The retina and choroid
8.2. Spectral properties of the eye
8.3. Injury to the anterior portion of the eye
8.3.1. Effects on the cornea
8.3.2. UVR lenticular effects
8.3.3. Infrared cataract
8.4. Retinal injury
8.4.1. Determining the retinal exposure
8.4.1.1 Pupil size
8.4.1.2 Spectral transmission of the ocular
media and spectral absorption by the
retina and choroid
8.4.1.3 Optical image quality
8.4.1.4 Small images
8.4.1.5 Retinal pigment epithelium (RPE)
absorption
8.4.2. Chorioretinal thermal injury
8.4.3. Location of retinal burns
8.5. Photochemical retinal injury
8.5.1. Very long-term exposure
8.6. Flash blindness
8.7. Discomfort glare
8.8. Flashing lights
9. THE SKIN
9.1. Anatomy
9.2. Body heat regulation
9.3. Optical properties
9.4. Penetration depth and reflection
9.4.1. Injury to the skin
9.4.2. The sensation of warmth and heat flow
9.4.3. Thermal injury threshold for the skin
9.4.4. Delayed effects
9.4.5. Ambient environment and heat stress
9.4.6. UVR effects on the skin
9.4.7. Photosensitization
9.4.8. Photoallergy
10. LASER SAFETY STANDARDS: RATIONALE AND CURRENT STANDARDS
10.1. Introduction
10.2. Laser hazard classification
11. EXPOSURE LIMITS
11.1. Rationale
11.2. Assessment of the "safety factor"
11.3. Environmental considerations
11.4. Limiting apertures
11.4.1. The 1-mm aperture
11.4.2. The 11-mm aperture
11.4.3. The 7-mm aperture
11.4.4. The 80-mm aperture
11.5. Spectral dependence of exposure limits
11.6. Repetitively pulsed laser exposure
11.7. Restriction for special applications (Class 3a)
11.8. Present standards of exposure
11.8.1. Laser standards
11.8.1.1 Exposure limits
11.8.1.2 Repetitively pulsed lasers
11.8.1.3 Extended source laser exposure
11.8.1.4 Restrictions on ELs
11.8.2. Standards for non-laser sources
11.8.2.1 Introduction
11.8.2.2 UVR criteria
11.8.2.3 Retinal health criteria
11.8.2.4 Retinal thermal risk evaluation
11.8.2.5 Retinal blue-light risk evaluation
11.8.2.6 IR-A risk analysis
11.8.3. Infrared standards
12. RISK EVALUATION
12.1. Laser hazard classification
12.2. Environmental considerations including
reflection and the probability of exposure
12.2.1. Reflections
12.2.2. Retroreflection
12.2.3. Optically aided viewing
13. ACCIDENTAL INJURIES
14. CONTROL MEASURES
15. HAZARDS OF LAMP SOURCES AND PROJECTION SYSTEMS
16. PROJECTION OPTICS
17. SAFETY GUIDELINES FOR HIGH-INTENSITY SOURCES
18. WELDING ARCS
19. EYE AND SKIN PROTECTION
19.1. Laser safety eyewear
19.2. Welders' filters
19.3. Eye protection for furnace radiation
19.4. Eye protection filters for solar radiation
19.5. Skin-protecting agents for UVR (Sunscreens)
19.6. Protective garments
20. MEDICAL SURVEILLANCE (RATIONALE)
21. FORMAL TEACHING FOR LASER WORKERS
REFERENCES
GLOSSARY
WHO/IRPA TASK GROUP ON ENVIRONMENTAL HEALTH CRITERIA FOR LASERS
Members
Dr B. Bosnjakovica, Ministry of Health and Environment,
Rijswijk, Netherlands
Dr L. Court, Commissariat à l'Energie Atomique, Département
de Protection, Fontenay-aux-Roses, France
Dr P. Czerskia, Bureau of Radiological Health, Food and
Drug Administration, Rockville, MD, USA
Dr M. Fabera, The Finsen Laboratory, Finsen
Institute, Copenhagen, Denmark (Chairman)
Dr M. Garavaglia, Centre of Optical Investigations CIOp,
La Plata, Argentina
Dr F. Hillenkamp, Institute of Biophysics, Frankfurt
University, Frankfurt am Main, Federal Republic of Germany
Dr H. Jammeta, Département de Protection, Commissariat à
l'Energie Atomique, Fontenay-aux-Roses, France
Mr R. Landry, Bureau of Radiological Health, Food and Drug
Administration, Rockville, MD, USA
Dr J. van der Leun, State University of Utrecht, Institute
of Dermatology, Utrecht, Netherlands
Dr J. Marshalla, Department of Visual Science, Institute of
Ophthalmology, London, United Kingdom (Co-Rapporteur)
Dr Z. Naprstek, Department of Surgery, Institute for
Clinical and Experimental Medicine, Research Department of
Surgery, Prague, Czechoslovakia (Vice-Chairman)
Dr Qin Jianan, Department of Biophysics, Second Shanghai
Medical School, Shanghai, China
Dr M. Repacholia, Radiation Protection Bureau, Environmental
Health Centre, Health and Welfare Canada, Ottawa, Ontario, Canada
Dr Y. Skorapad, Institute of Medical Radiology of the
Academy of Medical Sciences of the USSR, Moscow - Obninsk, USSR
Mr D. Slineya, Laser Microwave Division, US Army Environmental Hygiene
Agency, Aberdeen Proving Ground, MD, USA (Co-Rapporteur)
Dr B. Tengroth, Department of Ophthalmology; Director,
Karolinska Hospital (FACK), Stockholm, Sweden
---------------------------------------------------------------------------
a From IRPA/International NIR-Committee
Members (contd.)
Professor A. Tsyb, Institute of Medical Radiology of the
Academy of Medical Sciences of the USSR, Moscow - Obninsk, USSR
Observers
Dr S. Charschan, Western Electric Engineering Research
Laboratory, Princeton, NJ, USA
Secretariat
Dr E. Komarov, Environmental Hazards and Food Protection,
World Health Organization, Geneva, Switzerland
(Secretary)
IRPA Secretariat
Mrs A. Duchêne, Commissariat à l'Energie Atomique,
Département de Protection, Fontenay-aux Roses, France
NOTE TO READERS OF THE CRITERIA DOCUMENTS
While every effort has been made to present information in the
criteria documents as accurately as possible without unduly
delaying their publication, mistakes might have occurred and are
likely to occur in the future. In the interest of all users of the
environmental health criteria documents, readers are kindly
requested to communicate any errors found to the Division of
Environmental Health, World Health Organization, Geneva,
Switzerland, in order that they may be included in corrigenda which
will appear in subsequent volumes.
In addition, experts in any particular field dealt with in the
criteria documents are kindly requested to make available to the
WHO Secretariat any important published information that may have
inadvertently been omitted and which may change the evaluation of
health risks from exposure to the environmental agent under
examination, so that the information may be considered in the event
of updating and re-evaluation of the conclusions in the criteria
documents.
* * *
A detailed data profile and a legal file can be obtained from
the International Register of Potentially Toxic Chemicals, Palais
des Nations, 1211 Geneva 10, Switzerland (Telephone no., 988400 -
985850)
ENVIRONMENTAL HEALTH CRITERIA FOR LASERS AND OPTICAL RADIATION
Further to the recommendations of the Stockholm United Nations
Conference on the Human Environment in 1972, and in response to a
number of World Health Assembly resolutions (WHA23.60, WHA24.47,
WHA25.58, WHA26.68) and the recommendation of the Governing Council
of the United Nations Environment Programme, (UNEP/GC/10,
3 July 1973), a programme on the integrated assessment of the
health effects of environmental pollution was initiated in 1973.
The programme, known as the WHO Environmental Health Criteria
Programme, has been implemented with the support of the Environment
Fund of the United Nations Environment Programme.
A joint WHO/IRPA Task Group on Environmental Health Criteria
for Lasers and Optical Radiation met in Paris from 1-5 June 1982.
Dr E.I. Komarov, Division of Environmental Health, WHO, opened the
meeting on behalf of the Director-General, and Dr H. Jammet,
Chairman of IRPA/INIRC made some introductory comments. The Task
Group reviewed and revised the draft criteria document, made an
evaluation of the health risks of exposure to lasers and optical
radiation, and considered rationales for the development of
exposure limits.
In November 1971, the WHO Regional Office for Europe convened a
Working Group meeting in The Hague which recommended, inter alia,
that protection of man from laser radiation hazards should be
considered a priority activity in the field of non-ionizing
radiation protection. To implement these recommendations, the
Regional Office has prepared a publication on "Nonionizing
radiation protection", which includes a chapter on laser radiation
(Suess, ed., 1982). In October 1974, the Regional Office convened
a Working Group in Dublin, hosted by the Government of Ireland, to
discuss laser radiation hazards. This provided one of the first
opportunities for the exchange of information on the biological
effects of laser radiation and threshold data, at an international
level.
The International Radiation Protection Association (IRPA)
became responsible for NIR activities in 1974 by forming a Working
Group on Non-Ionizing Radiation which became the International Non-
Ionizing Radiation Committee (IRPA/INIRC) at the IRPA meeting in
Paris in 1977 (IRPA, 1977). Dr M. Faber, Dr J. Marshall,
Mr D. Sliney (members of IRPA/INIRC) and Dr L. Court, all acting as
WHO temporary advisers, prepared the draft criteria document on
lasers and optical radiation during 1980-81, and revised it after
receiving comments from the national focal points for the
Environmental Health Criteria Programme and individual experts. Dr
Marshall and Mr Sliney were responsible for the final scientific
editing. The Secretariat gratefully acknowledges the work of these
experts without whose help the document could not have been
completed.
The document is based primarily on original publications listed
in the reference section. Additional information was obtained from
a number of general reviews, monographs, and proceedings of
symposia including: Urbach, ed. (1969), Goldman & Rockwell (1971),
Wolbarsht (1971, 1974, 1977), Sliney & Freasier (1973), Fitzpatrick
(1974), Magnus (1976), Rubin (1977), Parrish et al. (1978), Lerman
(1980a), Pratesi & Sacchi, ed. (1980), Sliney & Wolbarsht (1980),
Williams & Baker, ed. (1980), Goldman, ed. (1981), and Goldman et
al. (1982). Radiometric terms, units, and spectral band
designations used in this criteria document are in accordance with
the SI recommendations (Lowe, 1975) and those recommended by the
Commission Internationale de l'Eclairage (CIE, 1970).
Modern advances in science and technology have changed man's
environment, introducing new factors which, besides their intended
beneficial uses, may also have untoward side effects. Both the
general public and health authorities are aware of the dangers of
pollution by chemicals, ionizing radiation, and noise, and of the
need to take appropriate steps for effective control. The rapid
growth of electro-optics and laser technology and the increasing
use of electro-optical devices and lasers, including optical
scanning equipment, high-intensity lamps, welding arcs, and UV
photo-curing equipment, alignment lasers, and medical lasers have
increased the possibility of human exposure to optical radiation
and, at the same time, concern about health effects.
This document provides information on the physical aspects of
electromagnetic radiation in the optical spectrum, within the
wavelength range of 100 nm - 1 mm. Optical radiation includes
ultraviolet radiation (UVR) from approximately 100 nm to 400 nm,
light (visible radiation) from approximately 400 nm to 760 nm, and
infrared radiation from approximately 760 nm to 1 mm. Each of
these spectral regions can be arbitrarily divided into subregions.
Lasers are capable of producing optical radiation in all three
major divisions of the optical spectrum. A brief survey of lasers
and other man-made sources of optical radiation is presented. It
is known that optical radiation interacts with biological systems
and a summary of knowledge on biological effects and health aspects
has been included in this document. In a few countries, concern
about occupational and public health aspects has led to the
development of radiation protection guides and the establishment of
exposure limits for laser radiation and UVR. Several countries are
considering the introduction of recommendations or legislation
concerned with protection against untoward effects from non-
ionizing radiation in the optical spectrum. In others, efforts are
being made to revise and update existing standards. It is hoped
that this criteria document may provide useful information for the
development, at a national level, of protection measures against
non-ionizing radiation.
Details of the WHO Environmental Criteria Programme, including
definitions of some of the terms used in the documents, may be
found in the general introduction to the Environmental Health
Criteria Programme, published together with the environmental
health criteria document on mercury ( Environmental Health Criteria
I - Mercury, Geneva, World Health Organization, 1976), now available
as a reprint.
1. SUMMARY AND RECOMMENDATIONS FOR FURTHER STUDIES
1.1. Summary
1.1.1. Scope
The potential hazards of optical radiation from wave-lengths
between 100 nm and 1 mm, i.e., ultraviolet radiation (UVR), visible
light, and infrared radiation (IR) are considered in this document,
and known adverse health effects, standards, and control measures
are reviewed. Emphasis is placed on the health risks of laser
radiation, but those of other sources are also covered. The health
effects of UVR are discussed only briefly, as UVR has already been
considered in depth in the WHO Environmental Health Criteria 14
(1979). Risks to the general population are considered as well as
those of occupational exposure.
The clinical treatment of different disorders or non-medical
problems, such as cosmetic surgery, where risk versus benefit must
be addressed, is outside the scope of the document. However, it
should be emphasized that the doses used in such exposures are
entirely the responsibility of the persons authorized to give such
treatment.
Although a certain amount of light is necessary for human
health, this document does not attempt to determine a lower
exposure limit or whether certain wavelengths are more necessary
than others.
1.1.2. Optical radiation exposure
Despite the great increase in the use of man-made optical
sources, the sun remains the principal source of optical radiation
exposure for man. Though the development of the laser in 1960
aroused great interest in the potential hazards of optical
radiation, many other artificial sources pose similar hazards. It
is often more difficult to evaluate the risks of non-laser sources
since, typically, they emit over a broad band of wavelengths. When
broad-band sources emit in all parts of the optical spectrum, each
of the potential hazards must be considered separately, as well as
collectively.
Beneficial effects of sunlight and UVR for man have been
reported in the literature and are treated in the WHO Environmental
Health Criteria 14, Ultraviolet Radiation. The reported beneficial
effects of medical and environmental exposure are important to
public health, but a careful benefit versus risk analysis must be
carried out.
Because optical radiations are not very penetrating, the eye
and the skin are the organs of concern. The main acute effects are
photokeratitis and thermal and photochemical retinal injury for the
eye, and erythema and burns for the skin. Delayed effects include
cataractogenesis and possible retinal degeneration for the eye, and
accelerated aging and cancer for the skin.
The biological effects of all optical radiation can be divided
into three major categories: thermal (including thermo-
mechanical), photochemical, and direct electric field effects. At
threshold levels, the predominant mechanism depends on maximal
exposure rates, total exposure, and on wavelength regimes. The
thermal effects are characteristic of the IR region extending into
the visible. The photochemical effects are mainly characteristic
of the ultraviolet region, but also occur in the visible. Acoustic
and other anomalous effects depend on acute thermal impulses of
nanoseconds (ns) duration, which may induce acoustic or mechanical
transients, damaging the tissue. For sub-ns exposures, direct
electric field (non-linear) interactions with biological molecules
appear to play a major role in the mechanism of injury.
Sources of optical radiation exposure may be categorized as:
(a) sunlight (natural illumination);
(b) lamps;
(c) lasers;
(d) other incandescent (warm-body) sources.
In industry, in addition to lasers, there are continuous
optical radiation sources, such as compact arc lamps (as in solar
simulators), quartz-iodide-tungsten lamps, gas and vapour discharge
tubes, electric welding units, and pulsed optical sources such as
flash lamps used in laser research and photolysis, exploding wires,
and super-radiant light. Common lasers and their applications are
listed in Table 1 and some sources of optical radiation exposure
and potentially exposed populations in Table 2. In most
applications, maintenance and evaluation workers may be exposed.
The general population may also be exposed on occasion, and it is
the responsibility of the operator to minimize this exposure.
Until the advent of the laser, the principal hazard recognized
in the use of optical sources was the potential for injury of the
skin and eye from exposure to UVR at wavelengths of less than 320
nm. The spectral band of less than 320 nm is often called the
"actinic ultraviolet" and consists principally of the 2 bands known
as UV-B and UV-C. The high attenuation afforded by many optical
materials, such as glass in the spectral range 100 - 300 nm,
generally resulted in the empirical safety approach in which
optical sources were enclosed in glass, plastic, or similar
materials to absorb this actinic radiation. If injurious effects
were noted, the thickness of the material enclosing the source or
the filter protecting the eye was increased.
The widespread use of sources that emit high levels of UV-C/B
in industry has been the cause of many corneal injuries. The UVR-
rich industrial sources circumvent the natural defences of the body
by allowing direct exposure of the cornea at normal angles of
incidence, unshielded by the brow or eyelids. In many cases, the
hazards of these UVR-rich sources are greater as they are
incorporated into optical systems, the elements of which are
selected for either high transmission or high reflection in the
UVR. Welding is a prime example of potentially hazardous
industrial exposure. The presence of possible photosensitizers
makes the use of UVR in the chemical industry for the manufacture
of photosetting plastics potentially much more dangerous.
Until recently, it was felt that chorioretinal injury would not
result from exposure to visible light in industrial operations.
Indeed, this is still largely true, since the normal aversion
response to high brightness light sources (the blink reflex and
movement of the head and eyes away from the source) provides
adequate protection against most bright visual sources. However,
the recent increased use of high intensity, high radiance optical
radiation sources with output characteristics that differ
significantly from those seen in the past may present a serious
potential for chorioretinal injury. The recent findings of
photochemically-induced retinal injury, following long-term
exposures, reinforce this conclusion.
Since organic macromolecules absorbing the radiant energy would
have broad spectral absorption bands, the monochromatic nature of
laser radiation would not be expected to create any different
effects from those of radiation emitted by conventional sources;
this conclusion is strongly supported by experimental evidence.
The coherence of laser radiation is also considered not to affect
the hazard potential for thermal or photochemical chorioretinal
injury. Though a speckle pattern resulting from the interference
effects of laser light at the retina does exist, the very fine
gradations in retinal irradiance resulting from this effect
(Considine, 1966; Fried, 1981) would certainly be lost, as soon as
the pulse duration was greater than a few microseconds (µs). Both
thermal conduction and ocular tremor would smooth out the
distribution of light and localized temperature elevations
resulting from the 1-10 µm gradations of the speckle pattern and
these non-uniformities would be blurred. Chorioretinal injury from
either a laser or a non-laser source should not differ, therefore,
if image size (retinal irradiance distribution), exposure duration,
and wavelength are the same.
1.1.3. Present health and safety standards
Because of widespread concern regarding laser hazards,
substantial progress has been made towards the development of both
product performance standards and human (both occupational and
general population) exposure limits. Separate environmental
quality standards are unnecessary. Several national standards have
been promulgated and substantial progress has been made towards
international agreement in these areas, since there appear to be
only minor differences between the most recent national standards.
The laser exposure limits are complex functions of wavelength,
exposure duration, and viewing conditions and cannot be summarized,
without the use of complex tables. Based on present knowledge,
most of these extensive sets of laser standards appear adequate for
the protection of the health of those potentially exposed. Several
areas of concern still exist regarding exposure limits for
ultrashort pulse, repetitive pulse, long-term, and multiwavelength
exposures.
Table 1. Common laser devices and applications
----------------------------------------------------------------------
Type Wavelength(s) Applications
----------------------------------------------------------------------
argon (Ar) 458-515 nm instrumentation;
+ 350 nm holography;
retinal photocoagulation;
entertainment
----------------------------------------------------------------------
carbon dioxide (CO2) 10.6 µm material processing;
optical radar/ranging;
instrumentation;
surgery techniques
----------------------------------------------------------------------
dye(s) variable 350 nm instrumentation
1 µm
----------------------------------------------------------------------
excimer lasers 180-250 nm laser pumping;
spectroscopy
----------------------------------------------------------------------
gallium arsenide (GaAs) 850-950 nm instrumentation ranging;
intrusion detection;
communications;
toys
----------------------------------------------------------------------
helium cadmium (HeCd) 325, 442 nm alignment;
surveying
----------------------------------------------------------------------
helium neon (HeNe) 632.8 nm alignment;
surveying;
holography;
ranging;
intrusion detection;
communications;
entertainment
----------------------------------------------------------------------
neodymium glass 1.06 µm material processing;
(Nd-glass) instrumentation;
neodymium yttrium- optical radar/ranging;
aluminium garnet (Nd-YAG) surgery
----------------------------------------------------------------------
ruby 694.3 nm material processing;
holography;
photocoagulation;
ranging
----------------------------------------------------------------------
Table 2. Some examples of optical radiation exposure
---------------------------------------------------------------------------
Sources Principal wave- Potential Potentially exposed
length bands effects populations
of concern
---------------------------------------------------------------------------
sunlight ultraviolet (UV), skin cancer; outdoor workers
visible cataract; (e.g., farmers,
near-infrared sunburn; construction
accelerated workers); sun-
skin aging; bathers; general
solar retinitis population
---------------------------------------------------------------------------
arc lamps UV, visible, photokeratitis; printing plant
(Xe, Xe-Hg, near-infrared erythema; camera operators;
Hg) skin cancer; optical laboratory
retinal injury workers;
entertainers
---------------------------------------------------------------------------
germicidal actinic, far UV erythema; hospital workers;
(low-pressure photokeratitis; workers in sterile
Hg) skin cancer laboratories
---------------------------------------------------------------------------
medium- UV-A and blue retinal injury street lamp
pressure light replacement
Hg-HID lamps personnel; gymnasium
(broken actinic UVA photokeratitis; users; general
envelope) erythema population
---------------------------------------------------------------------------
carbon arcs UV, blue light photokeratitis; certain laboratory
erythema workers; search light
operators
---------------------------------------------------------------------------
He-Ne lasers visible retinal injury construction workers;
(0.5-5.0 mW) users of alignment
lasers; some members
of general population
---------------------------------------------------------------------------
argon laser visible retinal injury, observers and operators
1-20 W localized skin- of laser light shows;
burns laboratory workers;
medical personnel
---------------------------------------------------------------------------
metal halide near UV, visible cataract; printing plant
UV-A lamps photosensitive maintenance workers;
skin reactions; integrated circuit
retinal injury manufacturing workers
---------------------------------------------------------------------------
sunlamps ultraviolet, photokeratitis; suntan-parlour
blue light erythema, customers; home users
accelerated
skin aging;
skin cancer
---------------------------------------------------------------------------
Table 2. (contd.)
---------------------------------------------------------------------------
Sources Principal wave- Potential Potentially exposed
length bands effects populations
of concern
---------------------------------------------------------------------------
welding arcs ultraviolet photokeratitis; welders' helpers;
and blue light erythema; welders
UV cataract;
retinal injury
---------------------------------------------------------------------------
ruby or visible retinal injury scientific
neodynium near-infrared investigators;
laser military personnel
rangefinders
---------------------------------------------------------------------------
industrial infrared radiant heat steel mill workers;
infrared stress; foundry workers;
sources infrared workers using
cataract infrared drying
equipment
---------------------------------------------------------------------------
Health and safety standards for lamps and other non-laser
sources are almost non-existent. Some exposure limits have been
proposed for ultraviolet, visible, and near-infrared radiation, but
these are quite tentative. The spectrum of the source must be
measured and weighted against several action spectra for risk
analysis - a complex process. Progress has been made, in several
countries, towards product performance safety standards for
specific lamp products such as high intensity discharge (HID)
lamps, sunlamps, and germicidal lamps.
1.2. Recommendations for Further Studies
The following comments cannot hope to be comprehensive in an
area of such rapidly expanding technology and whilst many of the
listed problems may be currently of importance or under
investigation in various research laboratories, others hitherto
unsuspected may assume paramount importance. Current problems are
discussed in the same order as the list of contents of this
criteria document, beginning after the background information
sections 1 - 5; the order does not assert priority ratings.
(a) Radiometric and photometric measurement
Further development of simplified, inexpensive laser or broad-
band survey instruments is desirable for monitoring the health
risks of optical radiation.
(b) The eye
The transmission characteristics of the ocular media are based
on averaged data from relatively few eyes. The variations with
age, in transmission and absorption in individual ocular
components, have not been clearly defined. Present understanding of
the effects of UVR on the cornea and the lens is poor, particularly
of the role, if any, of UV-A in the exacerbation of cataracts.
Further studies, especially in the field of epidemiology, are
needed to establish the possible involvement of short-wavelength
optical radiation in accelerating senile degenerative conditions in
the retina. The special problems of the aphakic (lens-less) eyes
or eyes with intraocular lens implants require attention in
relation to the increased retinal exposure to UVA and short-
wavelength visible radiation, particularly in the elderly. Some
further work is required concerning the spectral dependence of both
retinal damage and changes induced in the vitreous between 750 and
950 nm. It would also be of benefit to obtain a better
understanding of the role of the choroid in both the absorption of
optical radiation and production of damage and its involvement in
the healing process. In conclusion, further studies must be
undertaken on the quantification of the upper limits of flash
blindness and persistent after-image production and the lower
limits for oedema and irreversible damage.
(c) The skin
The optical properties of the skin require further study on the
relationship between penetration depth and absorptivity and
wavelength, skin pigmentation, and the angle of incident radiation.
Epidemiological studies should be undertaken to further clarify the
involvement and wavelength dependence of chronic exposure to
optical radiation in the induction of skin cancers. Such studies
should be encouraged in areas where direct comparison can be made
between negroid indigenous and Caucasian immigrant populations in
tropical and sub-tropical countries. Work is also required on the
possible additive or synergistic effects of different wavebands,
for example UVB, and UVB plus UVA. Finally a better understanding
is required of the additional protective factors that must be
applied to counteract the effects of specific photosensitizers
(WHO, 1979).
(d) Exposure limits (ELs)
To date, the exposure limits and various recommended standards
have been based mainly on empirical studies of acute effects on
animals and extrapolation of limited epidemiological information.
While these figures represent the best current knowledge, it should
be emphasized that standards should be sufficiently flexible to
enable the rapid incorporation of new data. Information is lacking
in many fields, especially with regard to the long-term health
risks associated with the adoption of present standards.
Further information on chronic effects is required and should
be obtained from multicentre epidemiological studies. Such studies
could be either retrospective or prospective but should clearly
isolate ethnic, environmental, sociological, and age-related
variations within participating populations. The systemic effects
of optical radiation have not been adequately studied. These
investigations should also take into account the effects of
progressively increasing exposure to artificial sources in industry
and the home. Active liaison is required between architects,
illumination engineers, and health physicists to establish exposure
limits and recommended lighting levels in relation to a variety of
visual tasks.
The large number of variable parameters associated with
repetitively pulsed exposures means that present ELs have been
established in relation to a limited number of research studies.
Further studies are needed and should include the problems of
repeated exposures to a single system and repeated exposures to
several sources within a relatively short period, i.e., a working
day.
The difficulties involved in measurement of ultra-short,
(sub-ns) pulses have resulted in few bioeffect studies being
undertaken and thus a large degree of extrapolation in establishing
ELs. More work is required and a better understanding is needed of
the bioeffects related to non-linear optical effects.
(e) Evaluation and control measures
In many countries, more than one executive office has some
responsibiities for regulating optical radiation exposure and
optical sources. Lack of clearly defined division of
responsibilities between different agencies has created confusion
for manufacturers and users of lasers and lamp sources. National
agencies should make every effort to work towards uniform and
compatible standards. Clear-cut criteria are needed to define
conditions under which lasers can be used in public places.
Current efforts to achieve international harmonization of laser
classification and control of health risks should be encouraged and
extended.
Radiation product performance and user standards should be
developed for lamps and lighting systems.
(f) Laser accidents
With the exception of a few published cases, medical and
biophysical details relating to laser accidents are difficult to
obtain. It would be helpful if individual countries established
national accident-reporting protocols together with a central
referral agency, in order to provide statistical evaluation of
problems in safety procedures.
(g) Eye protection
The investigation of new types of eye protection filters should
be undertaken and further attempts should be made to standardize
existing filters on an international basis (e.g., welding filters,
laser safety goggles).
(h) Medical surveillance and epidemiological studies
Occupational medical surveillance of workers may be necessary
in certain cases; of great importance is the need for
epidemiological studies on workers exposed for long periods to UVR
and visible radiation. A study of central visual function and
colour vision in comparison with an age-matched control group would
be very informative. An epidemiological study of workers exposed
over long periods to infrared radiation is also needed.
(i) Education
Since control measures for unenclosed lasers rely largely on
the laser operator, training programmes must be instituted for such
individuals. Education of the general population is also required
both to allay unwarranted fears of accidental laser exposure and to
give some background information against which elective optical
radiation exposures (medical and paramedical, e.g., cosmetic) may
be assessed.
2. DEFINITIONS OF OPTICAL RADIATION
2.1. The Electromagnetic Spectrum
Electromagnetic radiation consists of oscillating electric and
magnetic fields. Radio frequency (including microwave), infrared,
visible (lighta), ultraviolet, X, and gamma radiation are all
electromagnetic radiation and are propagated in both free space and
matter. Collectively, this electromagnetic radiation forms the
electromagnetic spectrum, when arranged according to frequency or
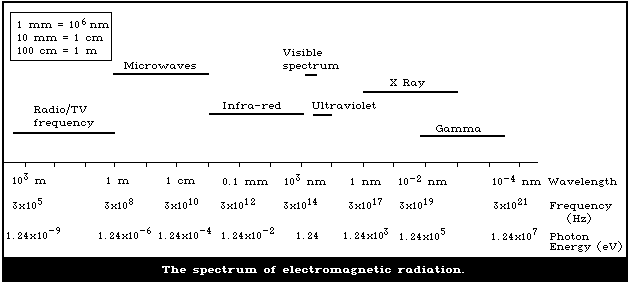
wavelength. A chart of the spectrum is shown in Fig. 1.
 Equation 1 can be modified for electromagnetic radiation by
giving the velocity of the radiation the value of the velocity of
light, usually written as c. In a vacuum:
co = lambda nu Equation (1)
The velocity rhoo has been set as 299792458 m/s or about 3 x 108
m/s = 3 x 1010 cm/s.
The ratio of the velocity of light co in a vacuum to the
velocity c in a medium is termed the refractive index n of that
medium (n = co/c). Equation 1 can also be expressed as
lambda = c/nu, or nu = c/lambda Equation (2)
-------------------------------------------------------------------
a Light by definition is visible radiation; hence, it is incorrect
(but commmon) to speak of "ultraviolet light" or "infrared
light".
The inverse relationship between frequency and wavelength is
clearly evident in Fig. 1. If n is constant at all points within
the medium, then the medium is called optically homogeneous; if n
is independent of direction, the medium is termed isotropic. If n
is considered independent of the amplitude or intensity of the
optical field, the interaction with the medium is termed "linear";
if not, it is "non-linear".
As the frequency increases from microwave radiation through the
optical radiations to gamma radiation, the wavelength becomes
shorter and shorter. The electromagnetic radiations have a
characteristic energy associated with each photon and the photon
energy increases with an increase in frequency. Reference to one
region or another as the "gamma-radiation region" or the "microwave
region" is arbitrary and no internationally accepted set of terms
exist for specifying all of the spectral regions.
The spectral bands represent wavelength intervals within which
a common state of the art and technology exists in sources,
detectors, or in modes of interaction with matter. The upper and
lower limits of the entire electromagnetic spectrum have not been
defined at present. The units used to describe energy, wavelength,
and frequency often differ between spectral regions, as a matter of
convention.
Ultraviolet, visible (light), and infrared radiation,
collectively known as optical radiation are described in terms of
wavelength. Sometimes, the spectral region of wavelengths shorter
than approximately 100 nm is termed ionizing radiation, and
wavelengths longer than 100 nm are placed in the non-ionizing
radiation spectrum. These terms are useful for those who wish to
distinguish between the biological effects of different types of
radiation, but divisions between adjacent spectral bands vary
according to different disciplines. For the physicist, the optical
spectrum generally consists of 5 decades of wavelengths between
10 nm and 1 mm. On the other hand, photobiologists and health
specialists, who are not concerned about vacuum ultraviolet
radiation, begin at approximately 180 - 200 nm (which is the
approximate long-wave edge of the vacuum ultraviolet) and go to
far-infrared radiation at 1 mm. The Commission Internationale de
l'Eclairage (CIE) Committee on Photobiology has provided spectral
band designations that are quite convenient in discussing
biological effects. Three common schemes of dividing the optical
spectrum are given in Table 3 (CIE, 1970).
2.2. Interaction of Electromagnetic Radiation with Matter
Electromagnetic radiation interacting with matter is absorbed,
transmitted, reflected, scattered, and diffracted. In most
instances, one of these effects dominates, almost to the exclusion
of others. However, all effects are always present to some extent.
For instance, if a beam of light passes through a sheet of
transparent glass, at least 4% of the incident light is reflected
from each surface. On the other hand, only a very small percentage
(less than 1%) is usually absorbed within the clear glass, even
when marked refraction or bending of the light takes place.
Similar effects occur in all spectral regions including the
radiofrequency and gamma-radiation bands.
2.2.1. Interaction at an interface
2.2.1.1. Reflection
Reflection takes place at an interface. There are two basic
types of reflections that are of interest, i.e., specular (mirror-
like) and diffuse. Specular reflection is sometimes referred to as
regular reflection. With specular reflection from a mirror or
other very smooth surface, light obeys the law of reflection, which
states that the angle of reflection equals the angle of incidence.
Table 3. Several schemes for dividing the optical spectrum
-----------------------------------------------------------------------
Physical No. 1 Physical No. 2 Photobiological (CIE)a
-----------------------------------------------------------------------
extreme UVR vacuum or extreme UVR UV-C
(1-10 nm to 100 nm) (1-10 nm to 180 nm) (100 nm to 280 nm)
far UVR middle UVR UV-Bb
(200 nm to 300 nm) (180 nm to 300 nm) (280 nm to 315 nm)
near UVR near UVR UV-Ab
(300 nm to 400 nm) (300 nm to 400 nm) (315 nm to 380-400 nm)
light light light
(380 nm to 760 nm) (400 nm to 700 nm) (380-400 nm to 760-780 nm)
near IR near IR IR-A
(760 nm to 4000 nm) (700 nm to 1200 nm) (760-780 nm to 1400 nm)
middle IR middle IR IR-B
(4 µm to 14 µm) (1.2 µm to 7 µm) (1.4 µm to 3 µm)
far IR far IR IR-C
(14 µm to 100 µm) (7 µm to 1 mm) (3 µm to 1 mm)
submillimetre
(100 µm to 1 mm)
-----------------------------------------------------------------------
a Based on the recommendation of the Committee on photobiology of the
Commission Internationale de l'Eclairage (CIE, 1970). The scheme
was originally proposed by W.W. Coblentz of the US National Bureau
of Standards in the 1930s.
b The dividing line between UV-B and UV-A is often taken as 320 nm,
but may be taken as 315 nm. For the purposes of this document,
315 nm is used unless otherwise stated.
Specular reflection can occur, when the size of surface
irregularities or roughness is less than the wavelength of the
incident radiation. This description of specular reflection is
important to keep in mind. Diffuse reflection occurs, when the
surface irregularities are randomly oriented and are much greater
than the wavelength of the incident radiation; for example, when
light is reflected from chalk or a rough granite surface. Perfect
diffuse reflection obeys Lambert's Law, i.e., the Cosine Law of
Reflection. A useful formula in radiometry is:
E = phi rho x cos theta/pi r12 Equation (3)
where E is the irradiance reflected from the surface at angle theta
relative to the surface's normal, phi, the optical beam power upon
the surface, rho, the diffuse reflection coefficient of the surface
for the wavelength, r1 the distance from the beam spot on the
diffuse target to the detector, and phi equals 3.14159.
It is important to remember that diffuse and specular
reflections are strongly dependent on wavelength. A given surface
may produce a reflection that is specular at one wavelength but may
or may not be specular at a different wavelength.
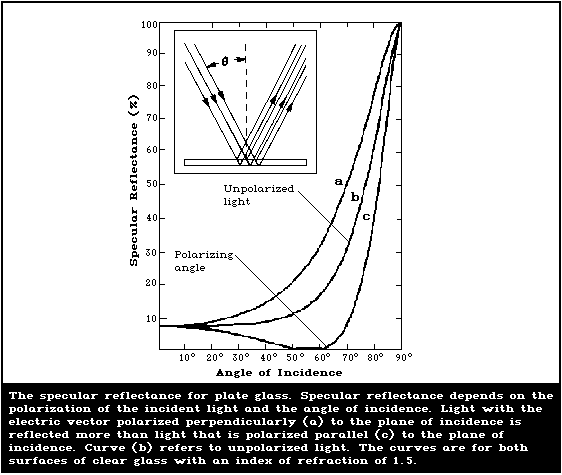
The fraction of incident radiation specularly reflected from
the surface of a transparent medium depends on the index of
refraction, the polarization of the incident beam, and the angle of
incidence. This is illustrated for glass in Fig 2.
Equation 1 can be modified for electromagnetic radiation by
giving the velocity of the radiation the value of the velocity of
light, usually written as c. In a vacuum:
co = lambda nu Equation (1)
The velocity rhoo has been set as 299792458 m/s or about 3 x 108
m/s = 3 x 1010 cm/s.
The ratio of the velocity of light co in a vacuum to the
velocity c in a medium is termed the refractive index n of that
medium (n = co/c). Equation 1 can also be expressed as
lambda = c/nu, or nu = c/lambda Equation (2)
-------------------------------------------------------------------
a Light by definition is visible radiation; hence, it is incorrect
(but commmon) to speak of "ultraviolet light" or "infrared
light".
The inverse relationship between frequency and wavelength is
clearly evident in Fig. 1. If n is constant at all points within
the medium, then the medium is called optically homogeneous; if n
is independent of direction, the medium is termed isotropic. If n
is considered independent of the amplitude or intensity of the
optical field, the interaction with the medium is termed "linear";
if not, it is "non-linear".
As the frequency increases from microwave radiation through the
optical radiations to gamma radiation, the wavelength becomes
shorter and shorter. The electromagnetic radiations have a
characteristic energy associated with each photon and the photon
energy increases with an increase in frequency. Reference to one
region or another as the "gamma-radiation region" or the "microwave
region" is arbitrary and no internationally accepted set of terms
exist for specifying all of the spectral regions.
The spectral bands represent wavelength intervals within which
a common state of the art and technology exists in sources,
detectors, or in modes of interaction with matter. The upper and
lower limits of the entire electromagnetic spectrum have not been
defined at present. The units used to describe energy, wavelength,
and frequency often differ between spectral regions, as a matter of
convention.
Ultraviolet, visible (light), and infrared radiation,
collectively known as optical radiation are described in terms of
wavelength. Sometimes, the spectral region of wavelengths shorter
than approximately 100 nm is termed ionizing radiation, and
wavelengths longer than 100 nm are placed in the non-ionizing
radiation spectrum. These terms are useful for those who wish to
distinguish between the biological effects of different types of
radiation, but divisions between adjacent spectral bands vary
according to different disciplines. For the physicist, the optical
spectrum generally consists of 5 decades of wavelengths between
10 nm and 1 mm. On the other hand, photobiologists and health
specialists, who are not concerned about vacuum ultraviolet
radiation, begin at approximately 180 - 200 nm (which is the
approximate long-wave edge of the vacuum ultraviolet) and go to
far-infrared radiation at 1 mm. The Commission Internationale de
l'Eclairage (CIE) Committee on Photobiology has provided spectral
band designations that are quite convenient in discussing
biological effects. Three common schemes of dividing the optical
spectrum are given in Table 3 (CIE, 1970).
2.2. Interaction of Electromagnetic Radiation with Matter
Electromagnetic radiation interacting with matter is absorbed,
transmitted, reflected, scattered, and diffracted. In most
instances, one of these effects dominates, almost to the exclusion
of others. However, all effects are always present to some extent.
For instance, if a beam of light passes through a sheet of
transparent glass, at least 4% of the incident light is reflected
from each surface. On the other hand, only a very small percentage
(less than 1%) is usually absorbed within the clear glass, even
when marked refraction or bending of the light takes place.
Similar effects occur in all spectral regions including the
radiofrequency and gamma-radiation bands.
2.2.1. Interaction at an interface
2.2.1.1. Reflection
Reflection takes place at an interface. There are two basic
types of reflections that are of interest, i.e., specular (mirror-
like) and diffuse. Specular reflection is sometimes referred to as
regular reflection. With specular reflection from a mirror or
other very smooth surface, light obeys the law of reflection, which
states that the angle of reflection equals the angle of incidence.
Table 3. Several schemes for dividing the optical spectrum
-----------------------------------------------------------------------
Physical No. 1 Physical No. 2 Photobiological (CIE)a
-----------------------------------------------------------------------
extreme UVR vacuum or extreme UVR UV-C
(1-10 nm to 100 nm) (1-10 nm to 180 nm) (100 nm to 280 nm)
far UVR middle UVR UV-Bb
(200 nm to 300 nm) (180 nm to 300 nm) (280 nm to 315 nm)
near UVR near UVR UV-Ab
(300 nm to 400 nm) (300 nm to 400 nm) (315 nm to 380-400 nm)
light light light
(380 nm to 760 nm) (400 nm to 700 nm) (380-400 nm to 760-780 nm)
near IR near IR IR-A
(760 nm to 4000 nm) (700 nm to 1200 nm) (760-780 nm to 1400 nm)
middle IR middle IR IR-B
(4 µm to 14 µm) (1.2 µm to 7 µm) (1.4 µm to 3 µm)
far IR far IR IR-C
(14 µm to 100 µm) (7 µm to 1 mm) (3 µm to 1 mm)
submillimetre
(100 µm to 1 mm)
-----------------------------------------------------------------------
a Based on the recommendation of the Committee on photobiology of the
Commission Internationale de l'Eclairage (CIE, 1970). The scheme
was originally proposed by W.W. Coblentz of the US National Bureau
of Standards in the 1930s.
b The dividing line between UV-B and UV-A is often taken as 320 nm,
but may be taken as 315 nm. For the purposes of this document,
315 nm is used unless otherwise stated.
Specular reflection can occur, when the size of surface
irregularities or roughness is less than the wavelength of the
incident radiation. This description of specular reflection is
important to keep in mind. Diffuse reflection occurs, when the
surface irregularities are randomly oriented and are much greater
than the wavelength of the incident radiation; for example, when
light is reflected from chalk or a rough granite surface. Perfect
diffuse reflection obeys Lambert's Law, i.e., the Cosine Law of
Reflection. A useful formula in radiometry is:
E = phi rho x cos theta/pi r12 Equation (3)
where E is the irradiance reflected from the surface at angle theta
relative to the surface's normal, phi, the optical beam power upon
the surface, rho, the diffuse reflection coefficient of the surface
for the wavelength, r1 the distance from the beam spot on the
diffuse target to the detector, and phi equals 3.14159.
It is important to remember that diffuse and specular
reflections are strongly dependent on wavelength. A given surface
may produce a reflection that is specular at one wavelength but may
or may not be specular at a different wavelength.
The fraction of incident radiation specularly reflected from
the surface of a transparent medium depends on the index of
refraction, the polarization of the incident beam, and the angle of
incidence. This is illustrated for glass in Fig 2.
 2.2.1.2. Refraction
Refraction also takes place at an interface. Refraction
occurs, whenever a beam of light passes from one transmitting
medium to another having a different refractive index (n). For
example, refraction is the bending of light at air-water and air-
glass interfaces. The law of refraction, which is also known as
Snell's Law, states that the angle of incidence (theta1) and the
angle of refraction (theta2) are related by the equation:
sin thetal/sin theta2 = n2/n1 Equation (4)
where n1 and n2 are the indices of refraction of the first medium and
the second medium respectively.
Lenses and prisms are optical components that depend
principally on the phenomenon of refraction. The variation in the
index of refraction with wavelength is termed dispersion. Thus a
simple prism bends blue light and red light differently for the
same angle of incidence, the two angles of refraction differ, and
blue light can be separated from red light. In lenses, this effect
is called chromatic aberration. It can be reduced by choosing a
glass with very little dispersion or by combining two lenses that
have complementary dispersion characteristics.
2.2.2. Interaction with a medium
2.2.2.1. Transmission
The nature of transmitted light that emerges from a medium
depends on the phenomena of absorption and scattering and also on
the reflection of some of the light at the interfaces between
media. The transmittance of a medium is usually represented by tau
and specified at a certain wavelength and for a certain path length
at normal incidence. The transmittance of most materials varies
markedly across the optical spectrum.
2.2.2.2. Attenuation
The absorption and transmission of a beam of optical radiation
in any homogenous, isotropic medium is expressed in terms of the
following equation:
phi = phioe-(alpha+rho)x=phioe-µx Equation (5)
where phi is the radiant power (radiant flux) leaving the medium,
phio the initial radiant power in the beam entering the absorbing
medium, x the thickness of the medium (path length of the beam),
alpha the absorption coefficient, rho the scattering coefficient,
and µ (Greek "mu") the attenuation coefficient of the absorbing
medium.
In the Exponential Law of Absorption (Beer's Law), the constant
alpha is the absorption coefficient. The law shows that the
radiant power diminishes exponentially with distance during
transmission through a uniformly absorbing medium. For a
scattering medium, the same approach may be applied with the
absorption coefficient alpha being replaced by a scattering
coefficient sigma. The attenuation coefficient varies with
wavelength as does the scattering coefficient sigma. Equation 5 is
only an approximation for weak scattering. It can be rewritten to
the base 10 instead of to the base e of natural logarithms and the
constants µ, rho, and alpha will then be different. "Attenuation
depth" and "absorption depth" are useful terms to describe
attenuation and absorption in tissue. The most popular convention
is to define this depth as the distance into the tissue at which
the incident irradiance is reduced to 1/e (37%) of its initial
value. Another convention sets the value at 1/10.
Absorption in all substances is strongly dependent on the
wavelength of the incident radiation. Atoms or molecules become
excited when they absorb a quantum of radiant energy. Following
absorption, this energy may be released in a variety of ways. When
the energy is released as more photons of radiant energy, it is
known as luminescence.
At very high irradiances, non-linear effects can occur as a
result of the direct interaction of the high electric-field
intensities with matter. Saturable absorption and enhanced
absorption are examples that alter the absorption coefficient.
2.2.3. Interference, diffraction, and scattering effects
2.2.3.1. Interference and diffraction
When considering interference and diffraction effects, it is
convenient to use the wave description of light. The bending or
spreading of waves after passing an edge or passing through a small
aperture is a wave phenomenon termed diffraction. The diffraction
effects result from the constructive and destructive interference
of adjacent waves. When the size of the barrier is comparable or
smaller in size than the incident wavelength, the wave is bent
around the barrier considerably. Thus, particles diffract light
most dramatically, when they are approximately the size of the
wavelength of the incident radiation. In this case, the sum of the
diffraction effects is known as scattering.
In the treatment of plane waves impinging on an aperture such
as a circular aperture, Huygens principle may be employed. Each
point within the area of the aperture is regarded as a source of
wavelets to explain the interference effects that produce a
diffraction pattern on a screen some distance away.
2.2.3.2. Scattering
Small particles, the size of which approaches that of a
wavelength of light, scatter light, as do atoms, and molecules. If
the particles are much smaller than the wavelength of light (e.g.,
gas molecules), Rayleigh scattering takes place. For Rayleigh
scattering, the fraction of scattered radiation from a beam is
inversely proportional to the fourth power of the wavelength of the
radiation. That is to say, that this type of scattering increases
dramatically for shorter wavelengths. Rayleigh scattered, non-
polarized light goes in all directions and becomes polarized to
some extent. If light is scattered by particles the size of the
order of the wavelength of light or greater, this strong wavelength
preference is not seen in the scattered light. The type of large-
particle scattering is termed Mie scattering. Unlike Rayleigh
scattering, Mie scattering is strongly directional. Normally, the
forward component of Mie scattered radiation is much greater than
the backscatter.
The scattering of a beam of light passing through a homogeneous
medium can be expressed in terms of the exponential function
(Equation 5).
3. SOURCES OF RADIATION
Sources of optical radiation can be grouped according to the
type of emitting material, the type of apparatus, or the manner in
which the radiation originates.
Incandescent bodies are probably the most common sources of
optical radiation. When the temperature of a body is elevated,
more photons are emitted. If the temperature of the body is
approximately that of the human body (37 °C or 310 K), most of the
emitted photons have wavelengths in the far infrared, in the
vicinity of 10 µm. If a material body is heated to incandescence,
e.g., to 2000 K, the material may be described as "red hot". The
higher the temperature, the greater the percentage of high energy
photons released. But, in all cases, a wide range of photon
energies is associated with the emitted incandescent radiation. A
theoretically perfect incandescent source has a characteristic
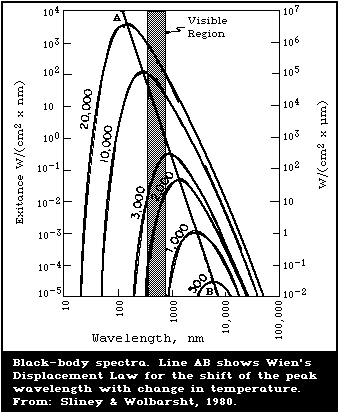
"black-body" spectrum. Fig. 3 shows the black-body spectra for
several different temperatures. In practice, no material actually
emits a perfect black-body spectrum, but some materials such as
solid tungsten or molten metals approach this distribution.
2.2.1.2. Refraction
Refraction also takes place at an interface. Refraction
occurs, whenever a beam of light passes from one transmitting
medium to another having a different refractive index (n). For
example, refraction is the bending of light at air-water and air-
glass interfaces. The law of refraction, which is also known as
Snell's Law, states that the angle of incidence (theta1) and the
angle of refraction (theta2) are related by the equation:
sin thetal/sin theta2 = n2/n1 Equation (4)
where n1 and n2 are the indices of refraction of the first medium and
the second medium respectively.
Lenses and prisms are optical components that depend
principally on the phenomenon of refraction. The variation in the
index of refraction with wavelength is termed dispersion. Thus a
simple prism bends blue light and red light differently for the
same angle of incidence, the two angles of refraction differ, and
blue light can be separated from red light. In lenses, this effect
is called chromatic aberration. It can be reduced by choosing a
glass with very little dispersion or by combining two lenses that
have complementary dispersion characteristics.
2.2.2. Interaction with a medium
2.2.2.1. Transmission
The nature of transmitted light that emerges from a medium
depends on the phenomena of absorption and scattering and also on
the reflection of some of the light at the interfaces between
media. The transmittance of a medium is usually represented by tau
and specified at a certain wavelength and for a certain path length
at normal incidence. The transmittance of most materials varies
markedly across the optical spectrum.
2.2.2.2. Attenuation
The absorption and transmission of a beam of optical radiation
in any homogenous, isotropic medium is expressed in terms of the
following equation:
phi = phioe-(alpha+rho)x=phioe-µx Equation (5)
where phi is the radiant power (radiant flux) leaving the medium,
phio the initial radiant power in the beam entering the absorbing
medium, x the thickness of the medium (path length of the beam),
alpha the absorption coefficient, rho the scattering coefficient,
and µ (Greek "mu") the attenuation coefficient of the absorbing
medium.
In the Exponential Law of Absorption (Beer's Law), the constant
alpha is the absorption coefficient. The law shows that the
radiant power diminishes exponentially with distance during
transmission through a uniformly absorbing medium. For a
scattering medium, the same approach may be applied with the
absorption coefficient alpha being replaced by a scattering
coefficient sigma. The attenuation coefficient varies with
wavelength as does the scattering coefficient sigma. Equation 5 is
only an approximation for weak scattering. It can be rewritten to
the base 10 instead of to the base e of natural logarithms and the
constants µ, rho, and alpha will then be different. "Attenuation
depth" and "absorption depth" are useful terms to describe
attenuation and absorption in tissue. The most popular convention
is to define this depth as the distance into the tissue at which
the incident irradiance is reduced to 1/e (37%) of its initial
value. Another convention sets the value at 1/10.
Absorption in all substances is strongly dependent on the
wavelength of the incident radiation. Atoms or molecules become
excited when they absorb a quantum of radiant energy. Following
absorption, this energy may be released in a variety of ways. When
the energy is released as more photons of radiant energy, it is
known as luminescence.
At very high irradiances, non-linear effects can occur as a
result of the direct interaction of the high electric-field
intensities with matter. Saturable absorption and enhanced
absorption are examples that alter the absorption coefficient.
2.2.3. Interference, diffraction, and scattering effects
2.2.3.1. Interference and diffraction
When considering interference and diffraction effects, it is
convenient to use the wave description of light. The bending or
spreading of waves after passing an edge or passing through a small
aperture is a wave phenomenon termed diffraction. The diffraction
effects result from the constructive and destructive interference
of adjacent waves. When the size of the barrier is comparable or
smaller in size than the incident wavelength, the wave is bent
around the barrier considerably. Thus, particles diffract light
most dramatically, when they are approximately the size of the
wavelength of the incident radiation. In this case, the sum of the
diffraction effects is known as scattering.
In the treatment of plane waves impinging on an aperture such
as a circular aperture, Huygens principle may be employed. Each
point within the area of the aperture is regarded as a source of
wavelets to explain the interference effects that produce a
diffraction pattern on a screen some distance away.
2.2.3.2. Scattering
Small particles, the size of which approaches that of a
wavelength of light, scatter light, as do atoms, and molecules. If
the particles are much smaller than the wavelength of light (e.g.,
gas molecules), Rayleigh scattering takes place. For Rayleigh
scattering, the fraction of scattered radiation from a beam is
inversely proportional to the fourth power of the wavelength of the
radiation. That is to say, that this type of scattering increases
dramatically for shorter wavelengths. Rayleigh scattered, non-
polarized light goes in all directions and becomes polarized to
some extent. If light is scattered by particles the size of the
order of the wavelength of light or greater, this strong wavelength
preference is not seen in the scattered light. The type of large-
particle scattering is termed Mie scattering. Unlike Rayleigh
scattering, Mie scattering is strongly directional. Normally, the
forward component of Mie scattered radiation is much greater than
the backscatter.
The scattering of a beam of light passing through a homogeneous
medium can be expressed in terms of the exponential function
(Equation 5).
3. SOURCES OF RADIATION
Sources of optical radiation can be grouped according to the
type of emitting material, the type of apparatus, or the manner in
which the radiation originates.
Incandescent bodies are probably the most common sources of
optical radiation. When the temperature of a body is elevated,
more photons are emitted. If the temperature of the body is
approximately that of the human body (37 °C or 310 K), most of the
emitted photons have wavelengths in the far infrared, in the
vicinity of 10 µm. If a material body is heated to incandescence,
e.g., to 2000 K, the material may be described as "red hot". The
higher the temperature, the greater the percentage of high energy
photons released. But, in all cases, a wide range of photon
energies is associated with the emitted incandescent radiation. A
theoretically perfect incandescent source has a characteristic
"black-body" spectrum. Fig. 3 shows the black-body spectra for
several different temperatures. In practice, no material actually
emits a perfect black-body spectrum, but some materials such as
solid tungsten or molten metals approach this distribution.
 The ratio of the theoretically possible spectral emittance to
the actual emittance of a grey body is the emissivity. For
instance, the emissivity of tungsten throughout the visible is
approximately 0.4.
A useful relation for black-body sources is the Stefan-
Boltzmann Law, which states that the radiant exitance W integrated
over all wavelengths of a black body is proportional to the fourth
power of the absolute temperature of the body, i.e.:
W = sigmaT4
3.1. Molecular and Atomic Transitions
Other sources of light such as carbon arcs, gas-filled arc
lamps, or gas discharge lamps, depart widely from black-body
characteristics, i.e., vary greatly with the wavelength in the
visible region. In these cases, a stream of electrons flowing
through a gas induces an emission of photons, characteristic of
that particular gas. If gas has a low pressure and the current is
not great, a line spectrum is emitted. Line spectra are the result
of atomic transition. As the gas pressure and the current density
increase, the gas temperature increases and a continuous spectrum
appears. At high current densities and gas pressures, this type of
emission (a continuum) predominates.
The energy Qq of a single photon, emitted because of an atomic
transition, is determined by the frequency of the emitted radiation
as defined by the condition:
Qq = xi1 - xi2 = h nu Equation (6)
where xi1 and xi2 are energies corresponding to the initial and
final energy states, h is the Plank constant (6.625 x 10-34J x s),
and nu is the frequency of radiation (in Hz).
Energy transitions in molecular systems can result in a
radiation emission according to rules similar to those that apply
to atomic systems. The energies (0.001-0.1 eV) of molecular
vibrational or rotational transitions are, typically, less than
those characteristic of electron transitions in atoms or molecules
(1-100 eV). In addition to the electron "orbital" potential and
kinetic energies, part of the energy of molecular systems is
associated with rotational and vibrational modes. Emissions of
this type occur in the infrared and microwave regions of the
electromagnetic spectrum. Heat is the vibrational energy of
molecular systems.
4. LASERS
All lasers have three basic components: (a) a laser (active)
medium; (b) an energy source (pumping system); and (c) a resonant
optical cavity. Lenses, mirrors, shutters, saturable absorbers,
and other accessories may be added to the system to obtain greater
power, shorter pulses, or special beam shapes, but only the three
basic components (a, b, and c) are necessary for laser action.
4.1. The Laser Medium
Laser action depends on the ability of the laser (active)
medium to undergo population inversion (i.e., more atoms or
molecules in the excited state than in the lower state). Once
population inversion occurs, an avalanche of photons can be
generated by stimulated emission. Initial, spontaneously emitted
photons stimulate other excited atoms to emit photons of the same
energy in phase with one another. This process is Light
Amplification by Stimulated Emission of Radiation, with the
acronym, LASER.
Fig. 4 shows a simplified 3-level energy diagram for a laser
material. This is just one of the many possible systems of energy
levels. Though laser action is possible with only 3 energy levels,
most such actions involve 4 or more levels.
The ratio of the theoretically possible spectral emittance to
the actual emittance of a grey body is the emissivity. For
instance, the emissivity of tungsten throughout the visible is
approximately 0.4.
A useful relation for black-body sources is the Stefan-
Boltzmann Law, which states that the radiant exitance W integrated
over all wavelengths of a black body is proportional to the fourth
power of the absolute temperature of the body, i.e.:
W = sigmaT4
3.1. Molecular and Atomic Transitions
Other sources of light such as carbon arcs, gas-filled arc
lamps, or gas discharge lamps, depart widely from black-body
characteristics, i.e., vary greatly with the wavelength in the
visible region. In these cases, a stream of electrons flowing
through a gas induces an emission of photons, characteristic of
that particular gas. If gas has a low pressure and the current is
not great, a line spectrum is emitted. Line spectra are the result
of atomic transition. As the gas pressure and the current density
increase, the gas temperature increases and a continuous spectrum
appears. At high current densities and gas pressures, this type of
emission (a continuum) predominates.
The energy Qq of a single photon, emitted because of an atomic
transition, is determined by the frequency of the emitted radiation
as defined by the condition:
Qq = xi1 - xi2 = h nu Equation (6)
where xi1 and xi2 are energies corresponding to the initial and
final energy states, h is the Plank constant (6.625 x 10-34J x s),
and nu is the frequency of radiation (in Hz).
Energy transitions in molecular systems can result in a
radiation emission according to rules similar to those that apply
to atomic systems. The energies (0.001-0.1 eV) of molecular
vibrational or rotational transitions are, typically, less than
those characteristic of electron transitions in atoms or molecules
(1-100 eV). In addition to the electron "orbital" potential and
kinetic energies, part of the energy of molecular systems is
associated with rotational and vibrational modes. Emissions of
this type occur in the infrared and microwave regions of the
electromagnetic spectrum. Heat is the vibrational energy of
molecular systems.
4. LASERS
All lasers have three basic components: (a) a laser (active)
medium; (b) an energy source (pumping system); and (c) a resonant
optical cavity. Lenses, mirrors, shutters, saturable absorbers,
and other accessories may be added to the system to obtain greater
power, shorter pulses, or special beam shapes, but only the three
basic components (a, b, and c) are necessary for laser action.
4.1. The Laser Medium
Laser action depends on the ability of the laser (active)
medium to undergo population inversion (i.e., more atoms or
molecules in the excited state than in the lower state). Once
population inversion occurs, an avalanche of photons can be
generated by stimulated emission. Initial, spontaneously emitted
photons stimulate other excited atoms to emit photons of the same
energy in phase with one another. This process is Light
Amplification by Stimulated Emission of Radiation, with the
acronym, LASER.
Fig. 4 shows a simplified 3-level energy diagram for a laser
material. This is just one of the many possible systems of energy
levels. Though laser action is possible with only 3 energy levels,
most such actions involve 4 or more levels.
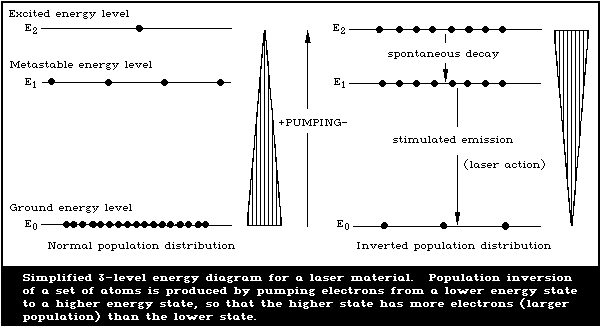 4.2. The Pumping System
Pumping systems are necessary to raise electrons to a higher
energy level in lasers. These systems pump energy into the laser
material, increasing the number of atoms or molecules trapped in
the metastable energy level, until a population inversion exists
large enough to make laser action possible (Fig. 4). Several
different pumping systems are available including optical, electron
collision, and chemical reaction.
In optical pumping, a strong source of light is used, such as a
xenon flashtube or another laser (e.g., an argon or nitrogen
laser), generally of a shorter wavelength than that emitted by the
medium.
Electron collision pumping is accomplished by passing an
electric current through a laser medium, usually a gas (e.g.,
helium-neon laser) or a semiconductor junction (e.g., gallium-
arsenide laser), or by accelerating electrons in an electron gun to
impact on the laser material, as in some semiconductor or gas
lasers.
Chemical pumping is based on energy released in the making and
breaking of chemical bonds. For example, some hydrogen fluoride
(HF) or deuterium fluoride (DF) lasers are pumped in this manner.
4.3. The Resonant Optical Cavity
A resonant optical cavity is formed by placing a mirror at each
end of the laser medium so that a beam of UVR, light, or IR
radiation may be reflected from one mirror to the other. Lasers
are constructed in this way so that the beam passes through the
laser medium one or more times and the number of emitted photons is
amplified at each passage. One of the mirrors is only partially
reflecting and permits part of the beam to be transmitted out of
the cavity at each reflection (Fig. 5). The alignment, curvature,
and separation distance of the mirrors determine the shape (mode
structure) of the emitted laser beam.
4.2. The Pumping System
Pumping systems are necessary to raise electrons to a higher
energy level in lasers. These systems pump energy into the laser
material, increasing the number of atoms or molecules trapped in
the metastable energy level, until a population inversion exists
large enough to make laser action possible (Fig. 4). Several
different pumping systems are available including optical, electron
collision, and chemical reaction.
In optical pumping, a strong source of light is used, such as a
xenon flashtube or another laser (e.g., an argon or nitrogen
laser), generally of a shorter wavelength than that emitted by the
medium.
Electron collision pumping is accomplished by passing an
electric current through a laser medium, usually a gas (e.g.,
helium-neon laser) or a semiconductor junction (e.g., gallium-
arsenide laser), or by accelerating electrons in an electron gun to
impact on the laser material, as in some semiconductor or gas
lasers.
Chemical pumping is based on energy released in the making and
breaking of chemical bonds. For example, some hydrogen fluoride
(HF) or deuterium fluoride (DF) lasers are pumped in this manner.
4.3. The Resonant Optical Cavity
A resonant optical cavity is formed by placing a mirror at each
end of the laser medium so that a beam of UVR, light, or IR
radiation may be reflected from one mirror to the other. Lasers
are constructed in this way so that the beam passes through the
laser medium one or more times and the number of emitted photons is
amplified at each passage. One of the mirrors is only partially
reflecting and permits part of the beam to be transmitted out of
the cavity at each reflection (Fig. 5). The alignment, curvature,
and separation distance of the mirrors determine the shape (mode
structure) of the emitted laser beam.
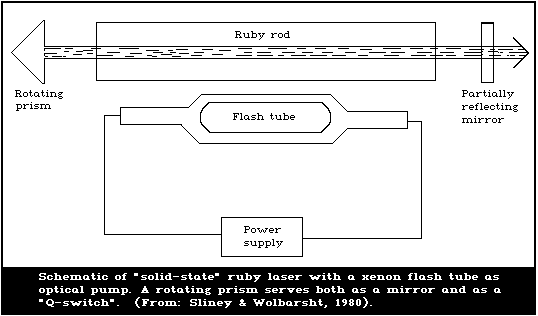 4.4. Types of Lasers
Lasers can be categorized in a variety of ways, e.g., according
to the active medium or temporal mode of operation.
4.4.1. Active media
Lasers are often designated according to the type of laser
medium, as follows:
(a) Solid-state lasers: a glass or crystalline medium
into which active atoms are introduced;
(b) Gas lasers: a medium of pure gas or a mixture of
gases; this category also includes metal vapour
lasers;
(c) Semi-conductor lasers: a medium of n-type and p-type
semiconducting element material;
(d) Liquid lasers: a liquid medium containing an active
material, such as an organic dye, in solution or
suspension.
Optical pumping (both coherent and incoherent) is usually used
in the production of solid-state and liquid lasers while collision
pumping is usually employed to produce gas lasers. However,
chemical-reaction pumping is also used for some types of liquid
and gas lasers. Semiconductor lasers may be optically pumped by an
electric current, another laser beam, or electron-collision from an
electron beam. Table 4 provides an abbreviated list of
commercially available laser wavelengths.
4.4.2. Temporal modes of operation
Some lasers operate continuously, and are termed continuous
wave (cw). In this type of operation, the peak power is equal to
the average power output; that is, the beam irradiance is constant
with time. Many lasers that appear to be cw may actually have a
temporal structure that can only be resolved with very
sophisticated systems of measurement.
The different temporal modes of operation of a laser are
distinguished by the rate at which energy is delivered. In
general, lasers operating in the normal pulse (or "long pulse")
temporal mode have pulse durations of a few tens of µs to a few ms
(Descomps, 1981).
Pulsed lasers can be operated to produce repetitive pulses.
The pulse repetition frequency of a laser is the number of pulses
that a particular laser produces per unit time duration. Lasers
are now available with pulse repetition frequencies as high as
several million pulses per s (MHz).
Table 4. Common lasers
-------------------------------------------------------------------
CIE band Wavelength (nm) Medium Typical operation
-------------------------------------------------------------------
Excimer UVC + B XeCl, XeFl, etc. pulsed
UV-A 325 He-Cd cw
UV-A 337 Nitrogen pulse train
UV-A 350 Argon cw
-------------------------------------------------------------------
Light 441.6 He-Cd cw
Light 458, 488, 514.5 Argon cw
Light 458, 568, 647 Krypton cw
Light 530 or 532 Nd frequency-doubled pulsed
Light 632.8 He-Ne cw
Light 694.3 Ruby pulsed/Q-pulsed
Light 560-640 Rhodamine 6G dye cw/pulsed
-------------------------------------------------------------------
IR-A 850 GaAlAs pulse train
IR-A 905 GaAs pulse train
IR-A 1060 Nd: glass pulsed/Q-pulsed
IR-A 1064 Nd: YAG cw/pulsed/Q-pulsed
-------------------------------------------------------------------
IR-C 5000 CO cw/pulsed
IR-C 10 600 CO2 cw/pulsed
-------------------------------------------------------------------
The resonant quality of the optical cavity of a laser can be
altered by rotating one mirror or by placing a shutter between the
mirrors. The shutter may be active (e.g., pockels cell) or passive
(a saturable absorber). This enables the beam to be turned on and
off rapidly and normally creates pulses with a duration of a few ns
to a few µs. This operation is normally called Q-switching (or
Q-spoiling or giant pulsing) (Fig. 6). The "Q" refers to the
resonant quality of the optical cavity. A Q-switched laser usually
emits less energy than the same laser emitting normal pulses, but
the energy is emitted in a much shorter period of time. Thus,
Q-switched lasers are capable of delivering very high peak powers
of several megawatts or even gigawatts. Fig. 6 shows a variety of
oscilloscope traces including a normal pulse and a Q-switched
pulse.
When the phases of a number of oscillating modes in a laser
resonator are forced to maintain a fixed relation to one another
through a non-linear absorber placed in the resonator, the laser
output observed is a train of regularly spaced ultra-short pulses.
This is termed a mode-locked laser. In a train of pulses, each
pulse has a duration of a few picoseconds (ps) to a few ns. A
mode-locked laser can deliver higher peak powers than the same
laser when Q-switched (Dautray & Watteau, 1980). Fig. 6 also shows
a mode-locked pulse train from a pulsed Nd-YAG laser.
4.4. Types of Lasers
Lasers can be categorized in a variety of ways, e.g., according
to the active medium or temporal mode of operation.
4.4.1. Active media
Lasers are often designated according to the type of laser
medium, as follows:
(a) Solid-state lasers: a glass or crystalline medium
into which active atoms are introduced;
(b) Gas lasers: a medium of pure gas or a mixture of
gases; this category also includes metal vapour
lasers;
(c) Semi-conductor lasers: a medium of n-type and p-type
semiconducting element material;
(d) Liquid lasers: a liquid medium containing an active
material, such as an organic dye, in solution or
suspension.
Optical pumping (both coherent and incoherent) is usually used
in the production of solid-state and liquid lasers while collision
pumping is usually employed to produce gas lasers. However,
chemical-reaction pumping is also used for some types of liquid
and gas lasers. Semiconductor lasers may be optically pumped by an
electric current, another laser beam, or electron-collision from an
electron beam. Table 4 provides an abbreviated list of
commercially available laser wavelengths.
4.4.2. Temporal modes of operation
Some lasers operate continuously, and are termed continuous
wave (cw). In this type of operation, the peak power is equal to
the average power output; that is, the beam irradiance is constant
with time. Many lasers that appear to be cw may actually have a
temporal structure that can only be resolved with very
sophisticated systems of measurement.
The different temporal modes of operation of a laser are
distinguished by the rate at which energy is delivered. In
general, lasers operating in the normal pulse (or "long pulse")
temporal mode have pulse durations of a few tens of µs to a few ms
(Descomps, 1981).
Pulsed lasers can be operated to produce repetitive pulses.
The pulse repetition frequency of a laser is the number of pulses
that a particular laser produces per unit time duration. Lasers
are now available with pulse repetition frequencies as high as
several million pulses per s (MHz).
Table 4. Common lasers
-------------------------------------------------------------------
CIE band Wavelength (nm) Medium Typical operation
-------------------------------------------------------------------
Excimer UVC + B XeCl, XeFl, etc. pulsed
UV-A 325 He-Cd cw
UV-A 337 Nitrogen pulse train
UV-A 350 Argon cw
-------------------------------------------------------------------
Light 441.6 He-Cd cw
Light 458, 488, 514.5 Argon cw
Light 458, 568, 647 Krypton cw
Light 530 or 532 Nd frequency-doubled pulsed
Light 632.8 He-Ne cw
Light 694.3 Ruby pulsed/Q-pulsed
Light 560-640 Rhodamine 6G dye cw/pulsed
-------------------------------------------------------------------
IR-A 850 GaAlAs pulse train
IR-A 905 GaAs pulse train
IR-A 1060 Nd: glass pulsed/Q-pulsed
IR-A 1064 Nd: YAG cw/pulsed/Q-pulsed
-------------------------------------------------------------------
IR-C 5000 CO cw/pulsed
IR-C 10 600 CO2 cw/pulsed
-------------------------------------------------------------------
The resonant quality of the optical cavity of a laser can be
altered by rotating one mirror or by placing a shutter between the
mirrors. The shutter may be active (e.g., pockels cell) or passive
(a saturable absorber). This enables the beam to be turned on and
off rapidly and normally creates pulses with a duration of a few ns
to a few µs. This operation is normally called Q-switching (or
Q-spoiling or giant pulsing) (Fig. 6). The "Q" refers to the
resonant quality of the optical cavity. A Q-switched laser usually
emits less energy than the same laser emitting normal pulses, but
the energy is emitted in a much shorter period of time. Thus,
Q-switched lasers are capable of delivering very high peak powers
of several megawatts or even gigawatts. Fig. 6 shows a variety of
oscilloscope traces including a normal pulse and a Q-switched
pulse.
When the phases of a number of oscillating modes in a laser
resonator are forced to maintain a fixed relation to one another
through a non-linear absorber placed in the resonator, the laser
output observed is a train of regularly spaced ultra-short pulses.
This is termed a mode-locked laser. In a train of pulses, each
pulse has a duration of a few picoseconds (ps) to a few ns. A
mode-locked laser can deliver higher peak powers than the same
laser when Q-switched (Dautray & Watteau, 1980). Fig. 6 also shows
a mode-locked pulse train from a pulsed Nd-YAG laser.
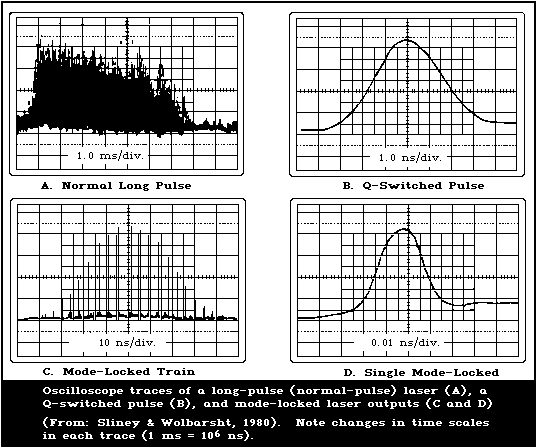 4.5. Spatial (TEM) Modes
A cross-sectional wave pattern is characteristic of all laser
beam geometries (transverse electromagnetic wave or TEM). These
wave patterns across the beam are identified with TEM mode
notation. Fig. 7 illustrates how some of the more common modes
would appear in cross section. The TEM01 mode is similar to the
TEM10 mode rotated through 90°.
4.5. Spatial (TEM) Modes
A cross-sectional wave pattern is characteristic of all laser
beam geometries (transverse electromagnetic wave or TEM). These
wave patterns across the beam are identified with TEM mode
notation. Fig. 7 illustrates how some of the more common modes
would appear in cross section. The TEM01 mode is similar to the
TEM10 mode rotated through 90°.
 Longitudinal (or axial) modes do not influence the emergent
beam profile, but influence the degree of coherency of the spatial
and the temporal frequency spectrum and are, therefore, of no great
significance in the consideration of biological effects (unless
they are intentionally or accidentally mode-locked to produce ps
pulses).
4.6. Beam Characteristics
4.6.1. Beam diameter
The beam diameter of a laser operating in the TEM00 mode has
been variously defined as the circle where the irradiance or
radiant exposure is 1/2, 1/e, 1/e2, or 1/10 of the maximum (Fig. 8).
In almost all discussions in the health and safety literature, the
edge of the beam is defined as 1/e or 0.37 of the maximum, whereas
the beam diameter is almost always defined at 1/e2 points in the
laser industry.
Longitudinal (or axial) modes do not influence the emergent
beam profile, but influence the degree of coherency of the spatial
and the temporal frequency spectrum and are, therefore, of no great
significance in the consideration of biological effects (unless
they are intentionally or accidentally mode-locked to produce ps
pulses).
4.6. Beam Characteristics
4.6.1. Beam diameter
The beam diameter of a laser operating in the TEM00 mode has
been variously defined as the circle where the irradiance or
radiant exposure is 1/2, 1/e, 1/e2, or 1/10 of the maximum (Fig. 8).
In almost all discussions in the health and safety literature, the
edge of the beam is defined as 1/e or 0.37 of the maximum, whereas
the beam diameter is almost always defined at 1/e2 points in the
laser industry.
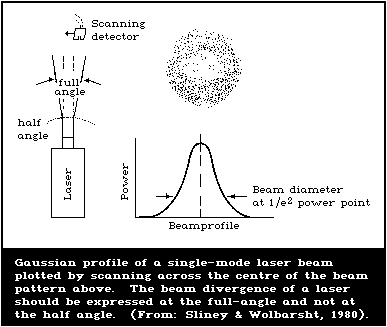 4.6.2. Beam divergence
The wave nature of light prevents lasers from producing
perfectly collimated beams. However, the divergence or beam
spreading is much smaller than that of a searchlight or other
conventional sources of optical radiation.
4.6.3. Beam irradiance versus range for a circular beam
To define potential exposure conditions, it is necessary to
characterize the beam emitted from a laser. The beam's
characteristics may be required near the output of the laser or at
some considerable distance from the laser, after it has been
collimated or focused. The optical radiation emitted by most
lasers is confined to a rather narrow beam that slowly diverges or
fans out as the beam propagates. The beam diameter DL increases
from an initial diameter a at the laser exit port as a result of
the divergence phi:
DL = a + r phi Equation (7)
where r is the range (distance from the laser).
With the beam diameter defined as a function of distance from
the laser, it is a simple matter to derive a formula to estimate
the beam irradiance or radiant exposure at any distance r. The
beam irradiance E (in W/m2 or W/cm2) would be the total power phi
in the beam (in watts) divided by the area of the cross section of
the beam (usually expressed in m2 or cm2). For health risk
assessment, a defining aperture of irradiance measurement is
normally specified (e.g., 7-mm circular aperture).
The effect of atmospheric attenuation may become a major factor
in evaluating the irradiance or radiant exposure at distances
greater than a few kilometres. This attenuation is the result of
three effects: (a) Mie (or large particle) scattering; (b)
Rayleigh (or molecular) scattering; and (c) absorption by gas
molecules. Rayleigh scattering is the most wavelength dependent;
shorter wavelengths are predominantly scattered. The atmospheric
attenuation may best be expressed by an exponential function. The
attenuation of optical radiation could be described by a term (eµr)
where µ is termed the attenuation coefficient of the medium. It is
the sum of scattering coefficients and absorption coefficients of
the medium through which the laser beam propagates. One equation
that is a close approximation for calculating the axial beam
irradiance is:
E = 1.27 phi e-µr/(a + r phi)2 Equation (8)
and a corresponding equation for radiant exposure H from a pulsed
laser of output energy Q is:
H = 1.27 Qe-µr/(a + r phi)2 Equation (9)
These equations can be adjusted for other beam profiles using
simple geometry. The emergent beam diameter term, a, may be
dropped at distances where a << rphi. Equations 7, 8, and 9 are
close approximations to rigorous formulations of Gaussian optics.
4.6.4. Hot spots
Hot spots are defined as areas of the beam, where the localized
beam irradiance is much greater than the average across the beam.
As the irradiance of hot spots may be many times higher than the
average beam irradiance, they are of considerable concern in
relation to health. There are several sources of hot spots:
inhomogeneities in the laser cavity or areas of the active medium,
where more energy is emitted than in other areas; imperfections in
the mirrors and lenses of the laser system; and changes caused by
atmospheric conditions. Atmospheric inhomogeneities along the beam
path produce lenticular effects (scintillation) that are
responsible for atmospheric hot spots. Fog, rain, snow, dust,
smoke, or haze absorb and/or scatter the laser beam but do not
cause hot spots. Such scattering reduces the severity of hot
spots.
4.6.5. Coherence
Two types of coherence are characteristic of laser light:
spatial and temporal. The term spatial coherence indicates that
the optical radiation is spatially in phase, i.e., electromagnetic
waves at different points in space oscillate in synchronism. Laser
speckle is a consequence of spatial coherence. Temporal coherence
indicates that the radiation is strictly monochromatic (of one
wavelength). No light source is either totally coherent or totally
incoherent; the differences between individual lasers and, for that
matter, non-laser sources are merely a matter of degree. The term
"coherence length" is used to describe the degree of spatial
coherence.
5. RADIOMETRIC CONCEPTS
5.1. Radiometric and Photometric Terminology
Two systems of quantities and units are used to describe
optical radiation. One is a physical system called the radiometric
system. The other, the photometric system, attempts to describe
the optical radiation in terms of its ability to elicit the
sensation of light by the eye. Table 5 gives the most commonly
used quantities and the preferred units for each system. There are
generally analogous units in each of the 2 systems. The table is
arranged to illustrate these similarities. Though the radiometric
system of units may be used across the entire spectrum, the
photometric system is limited to describe light (i.e.,
electromagnetic radiation that is visible) from approximately
380 - 400 nm to 760 - 780 nm.
It is important to remember that some terms refer only to
extended sources (e.g., radiance) and other terms (e.g., radiant
intensity) refer only to "point" sources.
5.2. Extended Sources Versus Point Sources
Lasers are often treated as "point" sources, whereas most
conventional light sources are considered to be extended sources,
at least at close distances. An extended source is one that
appears to have some angular extent as seen by the viewer. The
moon is an extended source; a star is a "point" source. Apart from
lasers, a light source can be considered a point source only at a
great distance, or if a pinhole diaphragm is placed in front of the
light source. All other light sources are considered to be
extended sources.
5.3. Inverse Square Law
The inverse square law for calculating the irradiance or
radiant exposure at a distance from a source applies only to a
point source. For example, the ratio of irradiance E1, at one
distance r1 to E2 at another distance r2 is:
El = r22 Equation (10)
E2 r12
For practical purposes, extended sources can be considered as
"point" sources at a distance many times greater than the source
dimension. Both r1 and r2 should be at least as great as 10 source
diameters for a diffuse lambertian source. This also applies to
equation 3. The irradiance E at a distance r from a point source
is:
E = I/r2 Equation (11)
This equation applies to collimated extended sources (e.g.,
searchlights) or lasers, only at considerable distances from the
source.
Table 5. Useful CIE radiometric and photometric quantitities and unitsa,b
-------------------------------------------------------------------------------------
RADIOMETRIC
-------------------------------------------------------------------------------------
Term Symbol Defining equation Quantity SI units &
applicablec abbreviations
-------------------------------------------------------------------------------------
Radiant energy Qe S, R joule (J)
-------------------------------------------------------------------------------------
Radiant energy dQe F joule per cubic
density We We = dV metre (J/m3)
-------------------------------------------------------------------------------------
Radiant power dQe S, R watt (W)
(radiant flux) phieP phie = dt
-------------------------------------------------------------------------------------
Radiant d phie S watt per square
exitance Me Me = dA metre (W/m2)
= /Le x cos x d omega
-------------------------------------------------------------------------------------
Irradiance or d phie R watt per square
flux density Ee Ee = dA metre (W/m2)
(dose rate in
photobiology)
-------------------------------------------------------------------------------------
Radiant d phie S watt per
intensity Ie Ie = d omega steradian
(W/sr1)
-------------------------------------------------------------------------------------
Radiance d d2phie S, F, R watt per
------------------------ steradian and
Le 1e = d omega x dA x cos theta per square metre
(W/sr/m2)
--------------------------------------------------------------------------------------
Radiant dQe R joule per square
exposure He He = dA metre (J/m2)
(dose in
photobiology)
--------------------------------------------------------------------------------------
Radiant P S unitless
efficiencye etae etae = Pi
(of a source)
--------------------------------------------------------------------------------------
Optical De De = -log10taue R unitless
--------------------------------------------------------------------------------------
Table 5. (contd.)
------------------------------------------------------------------------------------
PHOTOMETRIC
------------------------------------------------------------------------------------
Term Symbol Defining equation SI abbreviations
& units
------------------------------------------------------------------------------------
Quantity of Qnu Qnu = /phinudt lumen-second
light (lm x s)
------------------------------------------------------------------------------------
Luminous dQnu lumen-second per
energy density Wnu Wnu = dV cubic metre
(lm x s/m3)
------------------------------------------------------------------------------------
Luminous flux phinu d phie lumen (lm)
-----------------------
phinu = 680 / d lamdaV(lamda)d lamda
------------------------------------------------------------------------------------
Luminous d phinu lumen per square
exitance Mnu Mnu = dA metre (lm/m2)
= /Inu x cos phi x d omega
------------------------------------------------------------------------------------
Illuminance d phinu lumen per square
(luminous Enu Enu = dA metre (lm/m2)
density)
------------------------------------------------------------------------------------
Luminous d phinu lumen per
intensity Inu Inu = dr steradian (lm x sr)
(candlepower) or candela (cd)
------------------------------------------------------------------------------------
Luminance d Lnu d2phie candela per square
------------------- metre (cd/m2)
Lnu = dr x dA x cos theta
------------------------------------------------------------------------------------
Light exposure dQnu lux-second
Hnu Hnu = dA (lx x s)
= /Enudt
------------------------------------------------------------------------------------
Luminous phinu lumen per watt
efficacy (of K K = phie (lm/W)
radiation)
------------------------------------------------------------------------------------
Luminous K K unitless
efficiency V(*) V(*) = / Km = 680
(of a broad
band radiation)
------------------------------------------------------------------------------------
Luminous phinu lumen per watt
efficacye etanu etanu = Pi (lm/W)
------------------------------------------------------------------------------------
Table 5. (contd.)
------------------------------------------------------------------------------------
PHOTOMETRIC
------------------------------------------------------------------------------------
Term Symbol Defining equation SI abbreviations
& units
------------------------------------------------------------------------------------
Optical unitless
densityf Dnu Dnu = -log10taunu
------------------------------------------------------------------------------------
Retinal Troland (td) =
illuminance Et Et = Lnu x Sp luminance of 1 cd/
(in trolands) m2 times pupil
area in mm2
------------------------------------------------------------------------------------
a The quantities may be altered to refer to narrow spectral bands, in which case
the term is preceded by the word spectral, and the unit is then per unit of
wavelength and the symbol has a subscript lambda. For example, spectral
irradiance Hlambda has units of W/(m2 x m) or more often, W/(cm2 x nm).
b While the metre is the preferred unit of length, the centimetre is still the
most commonly used unit of length for many of the above terms and the nm or µm
are most commonly used to express wavelength.
c Some radiometric quantities refer only to the source, field, or receiver. This
noted in this column.
d At the source, dM ; at a receptor, dE
L = d omega x cos theta L = d omega x cos theta
e Pi is electrical input power in watts.
f tau is the transmission; Dnu is also abbreviated as O.D.
6. RADIOMETRIC AND PHOTOMETRIC MEASUREMENT
6.1. Introduction
Reliable radiometric techniques and instruments are available
that make it possible to analyse risks for the skin and eye from
exposure to lasers and other sources of optical radiation.
However, the cost of accurate equipment remains relatively high
compared with that of survey equipment now available to evaluate
many other environmental risks. Radiometric formulae and
manufacturers' specifications of lasers will often be an adequate
substitute for measurement.
There are many types of measurements for defining conditions or
characterizing a source's output. The types of measurements
considered in this section fall under the broad term of
"radiometric". For characterizing a conventional light source,
radiance is generally the most useful. For laser output
measurements, radiant power and radiant energy are by far the most
important. Irradiance and radiant exposure are of greater
importance in defining hazardous exposure conditions from all
optical sources.
In any discussion of the measurement of laser radiation for
purposes of evaluating health risks, it is important first to
clarify the conditions and requirements for such measurements.
Industrial and environmental health specialists and health
physicists usually rely heavily on instruments to detect or
estimate a chemical or physical agent that their own human senses
cannot detect. The presence of a laser beam can generally be
detected by the human eye or through the use of an image converter,
thus raising the question "Why should the laser beam be measured?".
It soon becomes evident that, in most cases, even routine
monitoring of either a work area or an individual by
instrumentation is a hopeless task. A more logical approach to
risk assessment is to develop a means of analysing the potential
risk of a laser, based on the laser's output parameters.
As a general rule, present standards require only measurement
of the laser-output characteristics for laser risk classification.
Routine monitoring is seldom considered necessary and all
measurements are normally performed only once, by (or for) the
manufacturer of the laser equipment. Periodic measurements may be
considered worthwhile for certain lasers that are near the
borderline between two classes in the hazard classification and
field measurements of outdoor laser propagation paths have often
been found useful. Unlike most noxious agents, a high-powered
laser beam is almost always hazardous for a considerable distance
and its hazard generally exceeds exposure limits by orders of
magnitude. Diagnostics of the beam profile and measurement of beam
divergence have been discussed.
The evaluation of more conventional broad-band sources is more
complex, since spectral characteristics and source size must be
considered. To evaluate a broad-band optical source, it is
normally necessary to determine the spectral distribution of
optical radiation emitted from the source at the point or points of
human access. The spectral distribution of the accessible
emission, which is of interest for a lighting system, may differ
from that actually being emitted by the lamp alone because of
apertures or filtration by any optical elements in the light path.
Secondly, the size, or projected size, of the source must be
characterized in the retinal hazard spectral region. Thirdly, it
may be necessary to determine the variation of irradiance and
radiance with distance. The necessary measurements are normally
complex. The spectrum of an arc lamp, a gas discharge lamp, or a
fluorescent lamp consists of both line structure and a continuum.
Significant errors can be introduced in the representation of the
spectrum and in the weighting of the spectrum against a biological-
or a safety-action spectrum, if the fraction of energy in each line
is not properly added to the continuum.
6.2. Measurement Instrumentation
The radiometric instruments of interest in this discussion
generally consist of detectors that produce a voltage, a current, a
resistance change, or an electronic charge, one of which is
measured by a sensitive electronic meter. The type of read-out
meter for the radiometric instrument is not normally of great
concern and seldom determines the selection of the instrument.
There are both advantages and disadvantages associated with each
type of detector and each has certain characteristics that may be
useful for measuring a specific level of optical radiation in a
wavelength range of interest. No single detector is best for
measuring all wavelengths and radiant powers of optical radiation.
A very sensitive detector can be readily damaged or its response
distorted by a high-powered laser beam, whereas a detector designed
to measure very high-powered laser radiation is normally
insensitive to low-power radiation. Narrow-band detectors have the
advantage of being insensitive to extraneous radiation, though
their usefulness is limited to measurement of lasers operating in
that particular spectral band.
In many countries, national physical standards laboratories
exist, which offer calibration services for some radiometric
instruments. Examples are: Laboratoire National d'Essais (France);
National Physical Laboratory (United Kingdom); Assistance Committee
for Measures and Standards (USSR); National Bureau of Standards
(USA); and Physikalisch-Technische Bundesanstalt (Federal Republic
of Germany).
6.2.1. Thermal detectors
Thermal detectors are mainly used for measuring the output
power or energy of lasers and total irradiances from broad-band
optical sources, in particular infrared sources. Some of these
detectors are particularly useful for absolute measurements.
Thermopiles, bolometers, disc calorimeters, and pyroelectric
detectors are characterized by a relatively flat response as a
function of wavelength. The spectral response of these detectors
is dictated by the "black" absorbers that are normally used to coat
the detector's metal or crystalline substrate. As optical energy
falls on the detector, the temperature increases. The temperature
rise in the substrate is then converted into an electrical voltage
or current. Because of the thermal mass of the metal, the time
required to heat or cool the detector element limits the response
time of the instrument. The absorber in a disc calorimeter may be
a black painted disc or a glass volume absorber (James, ed. 1976).
In recent years, the response time of thermopiles has been
shortened by using thin-film techniques. Low powers (typically
0.01 - 100 mW) can be measured and the response time reduced.
Pyroelectric detectors measure the rate of temperature change in a
crystalline material rather than the final temperature elevation in
a metal. Radiometric calorimeters can be used to measure cw
radiation over the power range from 1 mW to over 1 kW, depending on
the detector and wavelength. Pulsed radiant energy can be measured
over the range from 10 mJ to 10 kJ.
The detector may be covered by a window, which limits spectral
response. Quartz windows are necessary for UVR, but there is
probably no window material that is universally flat from 200 to
20 000 nm.
6.2.2. Quantum detectors
Quantum detectors operate normally at room temperature and
offer by far the most sensitive means of measuring optical
radiation, therefore, their principle use is in spectroradiometers
and detectors required for the measurement of lower powers and
irradiances or for temporal resolution of pulses. The spectral
sensitivity of photoemissive detectors depends on the photocathode
material used in vacuum photodiodes or photomultiplier tubes, or
in the characteristics of (doped) silicon. All detectors that
operate by means of the photoelectric effect have a characteristic
cutoff wavelength. At wavelengths greater than this cutoff,
photons are largely ineffective in producing photoelectrons and the
resulting photocurrent.
Because of the strong spectral dependence of the photodiode,
these instruments are often not direct reading and the meter
reading may have to be multiplied by one of several calibration
factors.
Simple silicon-detector instruments can be quite useful, when
the natural spectral response of silicon (approx 200 - 1100 nm) is
changed by an appropriate input filter to yield a flat spectral
response from 450 to 950 nm (Marshall, 1980).
6.2.3. Detectors to resolve short pulses
A variety of techniques have been developed to resolve the
temporal behaviour of short laser pulses. An ultrafast
oscilloscope with a solid-state silicon detector or biplanar vacuum
photodiode is most often used to display the pulse shape of a
Q-switched (1.0 - 100 ns) pulse. For temporal domains of less than
1 ns, streak cameras and some non-linear optical techniques are
used to resolve the structure of a train of mode-locked laser
pulses.
The techniques used in photometry and radiometry are far too
numerous and complex to detail here (see for example: Grum &
Becherer, ed. 1979; Le Bodo, 1976; or Sliney & Wolbarsht, 1980).
Differences in measured values for the same source from each of two
different laboratories may arise through a problem of "geometry" or
incorrect allowance for extraneous light.
6.2.4. Safety meters
At present, inexpensive, portable radiometric measuring
instruments that have been designed specifically for the risk
analysis of a great variety of lasers, are not available. Indeed,
it is unlikely that such instruments will be made in the future,
because of the great variation in exposure criteria for different
wavelengths and different exposure durations. The same holds true
for non-laser optical source survey instruments. However, some
relatively expensive, microprocessor-based instruments have been
developed to cover a wide range of measurements. Simple
instruments are possible for the purpose of measuring one type of
laser or optical source.
Because of the great interest in photometry, there are many
satisfactory photometers that measure both luminance and
illuminance and follow the CIE photopic function Vlambda quite
well. This is not always the case for the other weighting
functions. Direct reading UVR instruments are a case in point.
The principal difficulty in developing a suitable UVR instrument is
the rejection of unwanted wavelengths. It is difficult to measure
only the UV-B and UV-C radiation with sufficient sensitivity, while
still rejecting all of the UV-A and visible light.
6.2.5. Spectroradiometers
As well as broad-band measurements, it is often necessary to
measure the spectrum of a conventional source. A grating or prism
monochromator is used to resolve the spectrum.
An important part of measuring the spectral distribution of a
broad-band lamp source or an arc process is the specification of
the desired bandwidth, and the intervals at which data will be
recorded. One of the most useful approaches is to scan through a
spectrum and record the detector output in analogue fashion on an
X-Y recorder, rather than to record digitized data.
An X-Y recorder can indicate the bandwidth of the monochromator
and may quite often indicate the regions of the spectrum in which
problems may arise from stray light or extraneous signals.
The required bandwidth and sampling interval are determined by
comparing the so-called "slit function" of the monochromator system
with the need for sufficient spectral resolution to make possible
accurate weighting against action spectra used in risk analysis.
Two common difficulties are encountered in obtaining an
accurate radiometric description of a broad-band, extended source.
The first problem is to achieve adequate rejection of unwanted
wavelengths from the passband of the monochromator (e.g., rejecting
"stray light"). The second is the proper definition of the actual
or effective source size of an arc or a discharge lamp. Several
other special problem areas (such as background isolation,
wavelength calibration, and the proper separation of line and
continuous values) are also encountered in specific situations.
6.3. Biological Weighting of Spectroradiometric Data
Many of the calculations that are useful in risk analyses
require weighting of the measured spectrum against a biological
action spectrum. There are several, including the erythemal and
the photokeratitic action spectra, the photopic response V lambda
of the eye, and the retinal photochemical injury action spectrum B
lambda (Ham, et al., 1976; ACGIH, 1981; Sliney & Wolbarsht, 1980)
(Fig. 9).
4.6.2. Beam divergence
The wave nature of light prevents lasers from producing
perfectly collimated beams. However, the divergence or beam
spreading is much smaller than that of a searchlight or other
conventional sources of optical radiation.
4.6.3. Beam irradiance versus range for a circular beam
To define potential exposure conditions, it is necessary to
characterize the beam emitted from a laser. The beam's
characteristics may be required near the output of the laser or at
some considerable distance from the laser, after it has been
collimated or focused. The optical radiation emitted by most
lasers is confined to a rather narrow beam that slowly diverges or
fans out as the beam propagates. The beam diameter DL increases
from an initial diameter a at the laser exit port as a result of
the divergence phi:
DL = a + r phi Equation (7)
where r is the range (distance from the laser).
With the beam diameter defined as a function of distance from
the laser, it is a simple matter to derive a formula to estimate
the beam irradiance or radiant exposure at any distance r. The
beam irradiance E (in W/m2 or W/cm2) would be the total power phi
in the beam (in watts) divided by the area of the cross section of
the beam (usually expressed in m2 or cm2). For health risk
assessment, a defining aperture of irradiance measurement is
normally specified (e.g., 7-mm circular aperture).
The effect of atmospheric attenuation may become a major factor
in evaluating the irradiance or radiant exposure at distances
greater than a few kilometres. This attenuation is the result of
three effects: (a) Mie (or large particle) scattering; (b)
Rayleigh (or molecular) scattering; and (c) absorption by gas
molecules. Rayleigh scattering is the most wavelength dependent;
shorter wavelengths are predominantly scattered. The atmospheric
attenuation may best be expressed by an exponential function. The
attenuation of optical radiation could be described by a term (eµr)
where µ is termed the attenuation coefficient of the medium. It is
the sum of scattering coefficients and absorption coefficients of
the medium through which the laser beam propagates. One equation
that is a close approximation for calculating the axial beam
irradiance is:
E = 1.27 phi e-µr/(a + r phi)2 Equation (8)
and a corresponding equation for radiant exposure H from a pulsed
laser of output energy Q is:
H = 1.27 Qe-µr/(a + r phi)2 Equation (9)
These equations can be adjusted for other beam profiles using
simple geometry. The emergent beam diameter term, a, may be
dropped at distances where a << rphi. Equations 7, 8, and 9 are
close approximations to rigorous formulations of Gaussian optics.
4.6.4. Hot spots
Hot spots are defined as areas of the beam, where the localized
beam irradiance is much greater than the average across the beam.
As the irradiance of hot spots may be many times higher than the
average beam irradiance, they are of considerable concern in
relation to health. There are several sources of hot spots:
inhomogeneities in the laser cavity or areas of the active medium,
where more energy is emitted than in other areas; imperfections in
the mirrors and lenses of the laser system; and changes caused by
atmospheric conditions. Atmospheric inhomogeneities along the beam
path produce lenticular effects (scintillation) that are
responsible for atmospheric hot spots. Fog, rain, snow, dust,
smoke, or haze absorb and/or scatter the laser beam but do not
cause hot spots. Such scattering reduces the severity of hot
spots.
4.6.5. Coherence
Two types of coherence are characteristic of laser light:
spatial and temporal. The term spatial coherence indicates that
the optical radiation is spatially in phase, i.e., electromagnetic
waves at different points in space oscillate in synchronism. Laser
speckle is a consequence of spatial coherence. Temporal coherence
indicates that the radiation is strictly monochromatic (of one
wavelength). No light source is either totally coherent or totally
incoherent; the differences between individual lasers and, for that
matter, non-laser sources are merely a matter of degree. The term
"coherence length" is used to describe the degree of spatial
coherence.
5. RADIOMETRIC CONCEPTS
5.1. Radiometric and Photometric Terminology
Two systems of quantities and units are used to describe
optical radiation. One is a physical system called the radiometric
system. The other, the photometric system, attempts to describe
the optical radiation in terms of its ability to elicit the
sensation of light by the eye. Table 5 gives the most commonly
used quantities and the preferred units for each system. There are
generally analogous units in each of the 2 systems. The table is
arranged to illustrate these similarities. Though the radiometric
system of units may be used across the entire spectrum, the
photometric system is limited to describe light (i.e.,
electromagnetic radiation that is visible) from approximately
380 - 400 nm to 760 - 780 nm.
It is important to remember that some terms refer only to
extended sources (e.g., radiance) and other terms (e.g., radiant
intensity) refer only to "point" sources.
5.2. Extended Sources Versus Point Sources
Lasers are often treated as "point" sources, whereas most
conventional light sources are considered to be extended sources,
at least at close distances. An extended source is one that
appears to have some angular extent as seen by the viewer. The
moon is an extended source; a star is a "point" source. Apart from
lasers, a light source can be considered a point source only at a
great distance, or if a pinhole diaphragm is placed in front of the
light source. All other light sources are considered to be
extended sources.
5.3. Inverse Square Law
The inverse square law for calculating the irradiance or
radiant exposure at a distance from a source applies only to a
point source. For example, the ratio of irradiance E1, at one
distance r1 to E2 at another distance r2 is:
El = r22 Equation (10)
E2 r12
For practical purposes, extended sources can be considered as
"point" sources at a distance many times greater than the source
dimension. Both r1 and r2 should be at least as great as 10 source
diameters for a diffuse lambertian source. This also applies to
equation 3. The irradiance E at a distance r from a point source
is:
E = I/r2 Equation (11)
This equation applies to collimated extended sources (e.g.,
searchlights) or lasers, only at considerable distances from the
source.
Table 5. Useful CIE radiometric and photometric quantitities and unitsa,b
-------------------------------------------------------------------------------------
RADIOMETRIC
-------------------------------------------------------------------------------------
Term Symbol Defining equation Quantity SI units &
applicablec abbreviations
-------------------------------------------------------------------------------------
Radiant energy Qe S, R joule (J)
-------------------------------------------------------------------------------------
Radiant energy dQe F joule per cubic
density We We = dV metre (J/m3)
-------------------------------------------------------------------------------------
Radiant power dQe S, R watt (W)
(radiant flux) phieP phie = dt
-------------------------------------------------------------------------------------
Radiant d phie S watt per square
exitance Me Me = dA metre (W/m2)
= /Le x cos x d omega
-------------------------------------------------------------------------------------
Irradiance or d phie R watt per square
flux density Ee Ee = dA metre (W/m2)
(dose rate in
photobiology)
-------------------------------------------------------------------------------------
Radiant d phie S watt per
intensity Ie Ie = d omega steradian
(W/sr1)
-------------------------------------------------------------------------------------
Radiance d d2phie S, F, R watt per
------------------------ steradian and
Le 1e = d omega x dA x cos theta per square metre
(W/sr/m2)
--------------------------------------------------------------------------------------
Radiant dQe R joule per square
exposure He He = dA metre (J/m2)
(dose in
photobiology)
--------------------------------------------------------------------------------------
Radiant P S unitless
efficiencye etae etae = Pi
(of a source)
--------------------------------------------------------------------------------------
Optical De De = -log10taue R unitless
--------------------------------------------------------------------------------------
Table 5. (contd.)
------------------------------------------------------------------------------------
PHOTOMETRIC
------------------------------------------------------------------------------------
Term Symbol Defining equation SI abbreviations
& units
------------------------------------------------------------------------------------
Quantity of Qnu Qnu = /phinudt lumen-second
light (lm x s)
------------------------------------------------------------------------------------
Luminous dQnu lumen-second per
energy density Wnu Wnu = dV cubic metre
(lm x s/m3)
------------------------------------------------------------------------------------
Luminous flux phinu d phie lumen (lm)
-----------------------
phinu = 680 / d lamdaV(lamda)d lamda
------------------------------------------------------------------------------------
Luminous d phinu lumen per square
exitance Mnu Mnu = dA metre (lm/m2)
= /Inu x cos phi x d omega
------------------------------------------------------------------------------------
Illuminance d phinu lumen per square
(luminous Enu Enu = dA metre (lm/m2)
density)
------------------------------------------------------------------------------------
Luminous d phinu lumen per
intensity Inu Inu = dr steradian (lm x sr)
(candlepower) or candela (cd)
------------------------------------------------------------------------------------
Luminance d Lnu d2phie candela per square
------------------- metre (cd/m2)
Lnu = dr x dA x cos theta
------------------------------------------------------------------------------------
Light exposure dQnu lux-second
Hnu Hnu = dA (lx x s)
= /Enudt
------------------------------------------------------------------------------------
Luminous phinu lumen per watt
efficacy (of K K = phie (lm/W)
radiation)
------------------------------------------------------------------------------------
Luminous K K unitless
efficiency V(*) V(*) = / Km = 680
(of a broad
band radiation)
------------------------------------------------------------------------------------
Luminous phinu lumen per watt
efficacye etanu etanu = Pi (lm/W)
------------------------------------------------------------------------------------
Table 5. (contd.)
------------------------------------------------------------------------------------
PHOTOMETRIC
------------------------------------------------------------------------------------
Term Symbol Defining equation SI abbreviations
& units
------------------------------------------------------------------------------------
Optical unitless
densityf Dnu Dnu = -log10taunu
------------------------------------------------------------------------------------
Retinal Troland (td) =
illuminance Et Et = Lnu x Sp luminance of 1 cd/
(in trolands) m2 times pupil
area in mm2
------------------------------------------------------------------------------------
a The quantities may be altered to refer to narrow spectral bands, in which case
the term is preceded by the word spectral, and the unit is then per unit of
wavelength and the symbol has a subscript lambda. For example, spectral
irradiance Hlambda has units of W/(m2 x m) or more often, W/(cm2 x nm).
b While the metre is the preferred unit of length, the centimetre is still the
most commonly used unit of length for many of the above terms and the nm or µm
are most commonly used to express wavelength.
c Some radiometric quantities refer only to the source, field, or receiver. This
noted in this column.
d At the source, dM ; at a receptor, dE
L = d omega x cos theta L = d omega x cos theta
e Pi is electrical input power in watts.
f tau is the transmission; Dnu is also abbreviated as O.D.
6. RADIOMETRIC AND PHOTOMETRIC MEASUREMENT
6.1. Introduction
Reliable radiometric techniques and instruments are available
that make it possible to analyse risks for the skin and eye from
exposure to lasers and other sources of optical radiation.
However, the cost of accurate equipment remains relatively high
compared with that of survey equipment now available to evaluate
many other environmental risks. Radiometric formulae and
manufacturers' specifications of lasers will often be an adequate
substitute for measurement.
There are many types of measurements for defining conditions or
characterizing a source's output. The types of measurements
considered in this section fall under the broad term of
"radiometric". For characterizing a conventional light source,
radiance is generally the most useful. For laser output
measurements, radiant power and radiant energy are by far the most
important. Irradiance and radiant exposure are of greater
importance in defining hazardous exposure conditions from all
optical sources.
In any discussion of the measurement of laser radiation for
purposes of evaluating health risks, it is important first to
clarify the conditions and requirements for such measurements.
Industrial and environmental health specialists and health
physicists usually rely heavily on instruments to detect or
estimate a chemical or physical agent that their own human senses
cannot detect. The presence of a laser beam can generally be
detected by the human eye or through the use of an image converter,
thus raising the question "Why should the laser beam be measured?".
It soon becomes evident that, in most cases, even routine
monitoring of either a work area or an individual by
instrumentation is a hopeless task. A more logical approach to
risk assessment is to develop a means of analysing the potential
risk of a laser, based on the laser's output parameters.
As a general rule, present standards require only measurement
of the laser-output characteristics for laser risk classification.
Routine monitoring is seldom considered necessary and all
measurements are normally performed only once, by (or for) the
manufacturer of the laser equipment. Periodic measurements may be
considered worthwhile for certain lasers that are near the
borderline between two classes in the hazard classification and
field measurements of outdoor laser propagation paths have often
been found useful. Unlike most noxious agents, a high-powered
laser beam is almost always hazardous for a considerable distance
and its hazard generally exceeds exposure limits by orders of
magnitude. Diagnostics of the beam profile and measurement of beam
divergence have been discussed.
The evaluation of more conventional broad-band sources is more
complex, since spectral characteristics and source size must be
considered. To evaluate a broad-band optical source, it is
normally necessary to determine the spectral distribution of
optical radiation emitted from the source at the point or points of
human access. The spectral distribution of the accessible
emission, which is of interest for a lighting system, may differ
from that actually being emitted by the lamp alone because of
apertures or filtration by any optical elements in the light path.
Secondly, the size, or projected size, of the source must be
characterized in the retinal hazard spectral region. Thirdly, it
may be necessary to determine the variation of irradiance and
radiance with distance. The necessary measurements are normally
complex. The spectrum of an arc lamp, a gas discharge lamp, or a
fluorescent lamp consists of both line structure and a continuum.
Significant errors can be introduced in the representation of the
spectrum and in the weighting of the spectrum against a biological-
or a safety-action spectrum, if the fraction of energy in each line
is not properly added to the continuum.
6.2. Measurement Instrumentation
The radiometric instruments of interest in this discussion
generally consist of detectors that produce a voltage, a current, a
resistance change, or an electronic charge, one of which is
measured by a sensitive electronic meter. The type of read-out
meter for the radiometric instrument is not normally of great
concern and seldom determines the selection of the instrument.
There are both advantages and disadvantages associated with each
type of detector and each has certain characteristics that may be
useful for measuring a specific level of optical radiation in a
wavelength range of interest. No single detector is best for
measuring all wavelengths and radiant powers of optical radiation.
A very sensitive detector can be readily damaged or its response
distorted by a high-powered laser beam, whereas a detector designed
to measure very high-powered laser radiation is normally
insensitive to low-power radiation. Narrow-band detectors have the
advantage of being insensitive to extraneous radiation, though
their usefulness is limited to measurement of lasers operating in
that particular spectral band.
In many countries, national physical standards laboratories
exist, which offer calibration services for some radiometric
instruments. Examples are: Laboratoire National d'Essais (France);
National Physical Laboratory (United Kingdom); Assistance Committee
for Measures and Standards (USSR); National Bureau of Standards
(USA); and Physikalisch-Technische Bundesanstalt (Federal Republic
of Germany).
6.2.1. Thermal detectors
Thermal detectors are mainly used for measuring the output
power or energy of lasers and total irradiances from broad-band
optical sources, in particular infrared sources. Some of these
detectors are particularly useful for absolute measurements.
Thermopiles, bolometers, disc calorimeters, and pyroelectric
detectors are characterized by a relatively flat response as a
function of wavelength. The spectral response of these detectors
is dictated by the "black" absorbers that are normally used to coat
the detector's metal or crystalline substrate. As optical energy
falls on the detector, the temperature increases. The temperature
rise in the substrate is then converted into an electrical voltage
or current. Because of the thermal mass of the metal, the time
required to heat or cool the detector element limits the response
time of the instrument. The absorber in a disc calorimeter may be
a black painted disc or a glass volume absorber (James, ed. 1976).
In recent years, the response time of thermopiles has been
shortened by using thin-film techniques. Low powers (typically
0.01 - 100 mW) can be measured and the response time reduced.
Pyroelectric detectors measure the rate of temperature change in a
crystalline material rather than the final temperature elevation in
a metal. Radiometric calorimeters can be used to measure cw
radiation over the power range from 1 mW to over 1 kW, depending on
the detector and wavelength. Pulsed radiant energy can be measured
over the range from 10 mJ to 10 kJ.
The detector may be covered by a window, which limits spectral
response. Quartz windows are necessary for UVR, but there is
probably no window material that is universally flat from 200 to
20 000 nm.
6.2.2. Quantum detectors
Quantum detectors operate normally at room temperature and
offer by far the most sensitive means of measuring optical
radiation, therefore, their principle use is in spectroradiometers
and detectors required for the measurement of lower powers and
irradiances or for temporal resolution of pulses. The spectral
sensitivity of photoemissive detectors depends on the photocathode
material used in vacuum photodiodes or photomultiplier tubes, or
in the characteristics of (doped) silicon. All detectors that
operate by means of the photoelectric effect have a characteristic
cutoff wavelength. At wavelengths greater than this cutoff,
photons are largely ineffective in producing photoelectrons and the
resulting photocurrent.
Because of the strong spectral dependence of the photodiode,
these instruments are often not direct reading and the meter
reading may have to be multiplied by one of several calibration
factors.
Simple silicon-detector instruments can be quite useful, when
the natural spectral response of silicon (approx 200 - 1100 nm) is
changed by an appropriate input filter to yield a flat spectral
response from 450 to 950 nm (Marshall, 1980).
6.2.3. Detectors to resolve short pulses
A variety of techniques have been developed to resolve the
temporal behaviour of short laser pulses. An ultrafast
oscilloscope with a solid-state silicon detector or biplanar vacuum
photodiode is most often used to display the pulse shape of a
Q-switched (1.0 - 100 ns) pulse. For temporal domains of less than
1 ns, streak cameras and some non-linear optical techniques are
used to resolve the structure of a train of mode-locked laser
pulses.
The techniques used in photometry and radiometry are far too
numerous and complex to detail here (see for example: Grum &
Becherer, ed. 1979; Le Bodo, 1976; or Sliney & Wolbarsht, 1980).
Differences in measured values for the same source from each of two
different laboratories may arise through a problem of "geometry" or
incorrect allowance for extraneous light.
6.2.4. Safety meters
At present, inexpensive, portable radiometric measuring
instruments that have been designed specifically for the risk
analysis of a great variety of lasers, are not available. Indeed,
it is unlikely that such instruments will be made in the future,
because of the great variation in exposure criteria for different
wavelengths and different exposure durations. The same holds true
for non-laser optical source survey instruments. However, some
relatively expensive, microprocessor-based instruments have been
developed to cover a wide range of measurements. Simple
instruments are possible for the purpose of measuring one type of
laser or optical source.
Because of the great interest in photometry, there are many
satisfactory photometers that measure both luminance and
illuminance and follow the CIE photopic function Vlambda quite
well. This is not always the case for the other weighting
functions. Direct reading UVR instruments are a case in point.
The principal difficulty in developing a suitable UVR instrument is
the rejection of unwanted wavelengths. It is difficult to measure
only the UV-B and UV-C radiation with sufficient sensitivity, while
still rejecting all of the UV-A and visible light.
6.2.5. Spectroradiometers
As well as broad-band measurements, it is often necessary to
measure the spectrum of a conventional source. A grating or prism
monochromator is used to resolve the spectrum.
An important part of measuring the spectral distribution of a
broad-band lamp source or an arc process is the specification of
the desired bandwidth, and the intervals at which data will be
recorded. One of the most useful approaches is to scan through a
spectrum and record the detector output in analogue fashion on an
X-Y recorder, rather than to record digitized data.
An X-Y recorder can indicate the bandwidth of the monochromator
and may quite often indicate the regions of the spectrum in which
problems may arise from stray light or extraneous signals.
The required bandwidth and sampling interval are determined by
comparing the so-called "slit function" of the monochromator system
with the need for sufficient spectral resolution to make possible
accurate weighting against action spectra used in risk analysis.
Two common difficulties are encountered in obtaining an
accurate radiometric description of a broad-band, extended source.
The first problem is to achieve adequate rejection of unwanted
wavelengths from the passband of the monochromator (e.g., rejecting
"stray light"). The second is the proper definition of the actual
or effective source size of an arc or a discharge lamp. Several
other special problem areas (such as background isolation,
wavelength calibration, and the proper separation of line and
continuous values) are also encountered in specific situations.
6.3. Biological Weighting of Spectroradiometric Data
Many of the calculations that are useful in risk analyses
require weighting of the measured spectrum against a biological
action spectrum. There are several, including the erythemal and
the photokeratitic action spectra, the photopic response V lambda
of the eye, and the retinal photochemical injury action spectrum B
lambda (Ham, et al., 1976; ACGIH, 1981; Sliney & Wolbarsht, 1980)
(Fig. 9).
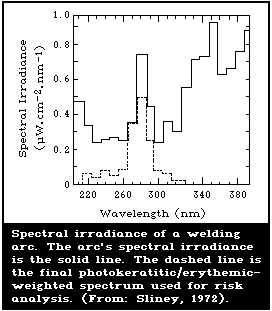 7. BIOLOGICAL EFFECTS
For biological effects to take place, some of the incident
radiation must be absorbed. This is known as Draper's Law (Smith,
1977).
The primary effects can be related to two general mechanisms,
thermal and photochemical injury. In some special instances (as
with ps pulses), non-linear effects related to the direct electric
field of photons may be important. The observable biological
effects are the result of secondary events. Under certain
circumstances, these effects can be changed in size and direction.
A number of these modifying factors are treated in the text such as
pigmentation, increased body temperature, and photosensitizing
substances.
7.1. Thermal Injury
Thermal injury mechanisms all require that sufficient radiant
energy is absorbed in a tissue, sufficiently fast, to create a
substantial increase above normal tissue temperature (typically
10 - 25 °C for short periods of a min or less). There is no
dependence on photon energy, though energy must be absorbed. Heat
conduction away from an irradiated area is of great importance.
Thus, the presence of blood vessels and the size of the irradiated
volume, as well as spectral absorption, influence the threshold of
injury (Marshall, 1970).
For every short exposure, changes of state may occur so rapidly
that micro-explosions (Hanson & Fine, 1968) or thermo-mechanical
effects may become important (Vos, 1966a; Ham et al., 1970).
7.2. Photochemical Injury
Significant adverse effects have now been shown to result
initially from a photochemical reaction rather than through a
thermal damage mechanism. A photochemical reaction takes place
when single photons have sufficient quantum energy to convert
individual molecules to one or more different chemical molecules.
A photochemical injury mechanism is demonstrated, when a
reciprocity relation between irradiance (dose-rate) and exposure
duration exists. That is, a constant radiant exposure (dose) is
required to elicit the response over a wide variation of exposure
durations, up to durations at which biological repair comes into
play. An additional characteristic of any photochemical reaction
is a rather steep drop-off of the action spectrum in the long
wavelength end. The yield of the photochemical reaction products
is propotional to the photon flux and each photon must have the
amount of energy required for the reaction. At the long-wavelength
end of the induced response (action spectrum), the energy of a
single photon coupled with available thermal energy is generally
insufficient to induce an effect.
Most photochemical effects of radiation are still not
understood in detail. The relative spectral effectiveness of
radiation in eliciting any particular biological effect is referred
to by photobiologists as an "action spectrum". The steep slopes of
many ultraviolet action spectra demonstrate the importance of not
routinely extrapolating biological data concerning injury occurring
at one wavelength to another wavelength, and of not assuming that
any smooth curve does not have fine structures.
There are some instances where both photochemical and thermal
effects contribute to the final biological effect. In general,
they will enhance one another.
7.3. Threshold of Injury
All thermal injury has a macroscopically apparent threshold.
Individual photons in the long-wavelength range do not have
sufficient energy, normally, to cause more than temporary
biological change at the molecular level. Acute pathological
changes can only be demonstrated, when a sufficient thermal photon
flux exists to cause temperature rises so rapid that normal heat
dissipation and molecular repair are overwhelmed. In the case of
photochemical injury, individual photons may alter or damage an
individual molecule. However, it has been shown that many critical
biomolecules have repair mechanisms to correct such damage (Smith,
1978). For very high photon flux densities the repair processes
may be overwhelmed and macroscopic damage will be apparent.
Occupational exposure limits can thus be set for any type of
radiation in which the reciprocal relation of progressively lower
power levels and longer exposure duration seems to show a marked
deviation from linearity (non-reciprocity). At this irradiance
level, any increases in the exposure duration may not be followed
by pathological changes in the exposed tissues. This would not be
accepted as a true threshold of injury by some investigators, since
it could always be argued that a repair mechanism could fail.
Thus, it must be admitted that there may be some finite, albeit
extremely slight, risk of injury or delayed effects in a small
population (Sliney & Wolbarsht, 1980).
7.3.1. Means of determining thresholds of injury
There are several different criteria that have been used in
studying potential injury in tissue (Beatrice & Velez, 1978).
Examples are:
(a) direct observation of irradiated tissue at low
magnification
(i) without special techniques
(ii) with special visualization techniques such as
fundoscopy or fluorescein angiography (eye)
(Borland et al., 1978);
(b) histology
(i) light microscopy
(ii) electron microscopy (EM)
(iii) histochemical studies;
(c) biochemical studies;
(d) electrophysiological tests (e.g., the eye) (Court et al.,
1978);
(e) functional studies;
(f) epidemiological studies (i.e., skin cancer).
In setting exposure limits, all of these studies must be taken
into account. In studies of skin reaction to optical radiation,
the first criteria of direct observation of erythema mainly has
been used, though histological and histochemical techniques have
been used in a few studies. The threshold criteria just listed
will be discussed briefly, as they apply to studies of injury from
optical radiation.
8. EFFECTS OF OPTICAL RADIATION ON THE EYE
The attendant hazards of optical radiation vary greatly
depending on the type of the source and its application. Generally,
the effects of laser radiation are not different from the effects
of optical radiation from a conventional source with the same
wavelength, exposure duration, and given irradiance.
The effects of optical radiation on the eye vary significantly
with wavelength. For this reason, the subject will be discussed in
three sections. First, the effects of UVR, which are generally
photochemical, on the lens and cornea will be considered. The main
discussion will relate to the retinal hazard region (the visible
and IR-A) where the eye is particularly vulnerable to injury,
because of its imaging characteristics. Finally, IR effects on the
anterior structures of the eye will be discussed.
There are many end points that can be used in establishing
injury. Damage to the retina of the eye from visible radiation can
appear as an altered light reflex or a white patch on the retina,
visible during ophthalmoscopic examination. This criterion has
been used in most injury studies. The end point could also be any
histologically-defined injury seen with the light microscope; or,
it could be consistently observed ultrastructural changes only
visible with an electron microscope (transmission or scanning EM).
Histochemical techniques can also serve to document an end point
for injury. There is also the detection of functional alterations
in sensory (behavioural) responses of task-oriented animal
subjects, e.g., visual acuity, colour vision, dark adaptation.
Often, these functional changes can also be detected by
electrophysiological recordings of altered neural function within
the visual system. A problem arises, when different investigators
define the "threshold" for any one of these end points in different
ways. The most meaningful thresholds for health criteria are those
related to a persistent functional decrement.
8.1. Anatomy and Physiology of the Human Eye
In the human eye, light passes through the various ocular
structures (Fig. 10) to fall on the retina, where it triggers a
photochemical process that evokes the neural impulses that lead to
vision. The light first passes through the structures in the
anterior portion of the eye - the cornea, the aqueous humor in the
anterior chamber, the pupil (and sometimes the iris), the somewhat
pliable crystalline lens, then into the posterior part, the
vitreous humor and the numerous layers of the retina. Only the
three structures of the eye that are critical in relation to the
subject of optical radiation hazards will be discussed, i.e., the
cornea, the lens, and the retina.
8.1.1. The cornea
The cornea and the conjuctiva of the eye are exposed directly
to the environmental elements. These structures are protected from
drying by the tear film, which is 6 - 10 µ in thickness.
7. BIOLOGICAL EFFECTS
For biological effects to take place, some of the incident
radiation must be absorbed. This is known as Draper's Law (Smith,
1977).
The primary effects can be related to two general mechanisms,
thermal and photochemical injury. In some special instances (as
with ps pulses), non-linear effects related to the direct electric
field of photons may be important. The observable biological
effects are the result of secondary events. Under certain
circumstances, these effects can be changed in size and direction.
A number of these modifying factors are treated in the text such as
pigmentation, increased body temperature, and photosensitizing
substances.
7.1. Thermal Injury
Thermal injury mechanisms all require that sufficient radiant
energy is absorbed in a tissue, sufficiently fast, to create a
substantial increase above normal tissue temperature (typically
10 - 25 °C for short periods of a min or less). There is no
dependence on photon energy, though energy must be absorbed. Heat
conduction away from an irradiated area is of great importance.
Thus, the presence of blood vessels and the size of the irradiated
volume, as well as spectral absorption, influence the threshold of
injury (Marshall, 1970).
For every short exposure, changes of state may occur so rapidly
that micro-explosions (Hanson & Fine, 1968) or thermo-mechanical
effects may become important (Vos, 1966a; Ham et al., 1970).
7.2. Photochemical Injury
Significant adverse effects have now been shown to result
initially from a photochemical reaction rather than through a
thermal damage mechanism. A photochemical reaction takes place
when single photons have sufficient quantum energy to convert
individual molecules to one or more different chemical molecules.
A photochemical injury mechanism is demonstrated, when a
reciprocity relation between irradiance (dose-rate) and exposure
duration exists. That is, a constant radiant exposure (dose) is
required to elicit the response over a wide variation of exposure
durations, up to durations at which biological repair comes into
play. An additional characteristic of any photochemical reaction
is a rather steep drop-off of the action spectrum in the long
wavelength end. The yield of the photochemical reaction products
is propotional to the photon flux and each photon must have the
amount of energy required for the reaction. At the long-wavelength
end of the induced response (action spectrum), the energy of a
single photon coupled with available thermal energy is generally
insufficient to induce an effect.
Most photochemical effects of radiation are still not
understood in detail. The relative spectral effectiveness of
radiation in eliciting any particular biological effect is referred
to by photobiologists as an "action spectrum". The steep slopes of
many ultraviolet action spectra demonstrate the importance of not
routinely extrapolating biological data concerning injury occurring
at one wavelength to another wavelength, and of not assuming that
any smooth curve does not have fine structures.
There are some instances where both photochemical and thermal
effects contribute to the final biological effect. In general,
they will enhance one another.
7.3. Threshold of Injury
All thermal injury has a macroscopically apparent threshold.
Individual photons in the long-wavelength range do not have
sufficient energy, normally, to cause more than temporary
biological change at the molecular level. Acute pathological
changes can only be demonstrated, when a sufficient thermal photon
flux exists to cause temperature rises so rapid that normal heat
dissipation and molecular repair are overwhelmed. In the case of
photochemical injury, individual photons may alter or damage an
individual molecule. However, it has been shown that many critical
biomolecules have repair mechanisms to correct such damage (Smith,
1978). For very high photon flux densities the repair processes
may be overwhelmed and macroscopic damage will be apparent.
Occupational exposure limits can thus be set for any type of
radiation in which the reciprocal relation of progressively lower
power levels and longer exposure duration seems to show a marked
deviation from linearity (non-reciprocity). At this irradiance
level, any increases in the exposure duration may not be followed
by pathological changes in the exposed tissues. This would not be
accepted as a true threshold of injury by some investigators, since
it could always be argued that a repair mechanism could fail.
Thus, it must be admitted that there may be some finite, albeit
extremely slight, risk of injury or delayed effects in a small
population (Sliney & Wolbarsht, 1980).
7.3.1. Means of determining thresholds of injury
There are several different criteria that have been used in
studying potential injury in tissue (Beatrice & Velez, 1978).
Examples are:
(a) direct observation of irradiated tissue at low
magnification
(i) without special techniques
(ii) with special visualization techniques such as
fundoscopy or fluorescein angiography (eye)
(Borland et al., 1978);
(b) histology
(i) light microscopy
(ii) electron microscopy (EM)
(iii) histochemical studies;
(c) biochemical studies;
(d) electrophysiological tests (e.g., the eye) (Court et al.,
1978);
(e) functional studies;
(f) epidemiological studies (i.e., skin cancer).
In setting exposure limits, all of these studies must be taken
into account. In studies of skin reaction to optical radiation,
the first criteria of direct observation of erythema mainly has
been used, though histological and histochemical techniques have
been used in a few studies. The threshold criteria just listed
will be discussed briefly, as they apply to studies of injury from
optical radiation.
8. EFFECTS OF OPTICAL RADIATION ON THE EYE
The attendant hazards of optical radiation vary greatly
depending on the type of the source and its application. Generally,
the effects of laser radiation are not different from the effects
of optical radiation from a conventional source with the same
wavelength, exposure duration, and given irradiance.
The effects of optical radiation on the eye vary significantly
with wavelength. For this reason, the subject will be discussed in
three sections. First, the effects of UVR, which are generally
photochemical, on the lens and cornea will be considered. The main
discussion will relate to the retinal hazard region (the visible
and IR-A) where the eye is particularly vulnerable to injury,
because of its imaging characteristics. Finally, IR effects on the
anterior structures of the eye will be discussed.
There are many end points that can be used in establishing
injury. Damage to the retina of the eye from visible radiation can
appear as an altered light reflex or a white patch on the retina,
visible during ophthalmoscopic examination. This criterion has
been used in most injury studies. The end point could also be any
histologically-defined injury seen with the light microscope; or,
it could be consistently observed ultrastructural changes only
visible with an electron microscope (transmission or scanning EM).
Histochemical techniques can also serve to document an end point
for injury. There is also the detection of functional alterations
in sensory (behavioural) responses of task-oriented animal
subjects, e.g., visual acuity, colour vision, dark adaptation.
Often, these functional changes can also be detected by
electrophysiological recordings of altered neural function within
the visual system. A problem arises, when different investigators
define the "threshold" for any one of these end points in different
ways. The most meaningful thresholds for health criteria are those
related to a persistent functional decrement.
8.1. Anatomy and Physiology of the Human Eye
In the human eye, light passes through the various ocular
structures (Fig. 10) to fall on the retina, where it triggers a
photochemical process that evokes the neural impulses that lead to
vision. The light first passes through the structures in the
anterior portion of the eye - the cornea, the aqueous humor in the
anterior chamber, the pupil (and sometimes the iris), the somewhat
pliable crystalline lens, then into the posterior part, the
vitreous humor and the numerous layers of the retina. Only the
three structures of the eye that are critical in relation to the
subject of optical radiation hazards will be discussed, i.e., the
cornea, the lens, and the retina.
8.1.1. The cornea
The cornea and the conjuctiva of the eye are exposed directly
to the environmental elements. These structures are protected from
drying by the tear film, which is 6 - 10 µ in thickness.
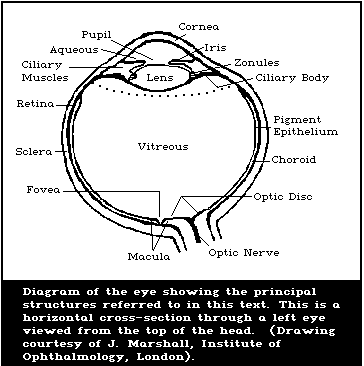 The cornea and conjuctiva are tissues rich in sensory receptors
and nerve endings serving as triggers of protective reflexes for
mechanical and thermal agents.
As the epithelial cells must survive a harsh environment, they
have a very short life span of approximately 2 - 5 days. If the
cell death rate increases (as in photokerititis) and replacement is
not in step with the loss, small erosions will develop that elicit
a pain sensation.
The corneal stroma is built in a very regular fashion, which
accounts for its transparency. If this regularity is distorted,
i.e., by an oedema, the cornea will be less transparent or even
opaque. A disturbance of the epithelium, or, more important still,
of the inner cell layer of the cornea (the endothelium) will result
in an oedema. Any scar formation will also alter the regular
construction and hence will result in an opaque cornea. Thus
serious visual handicap will be the result of irreversible corneal
damage.
8.1.2. The lens
The lens is a tissue built up from cells that progressively
deform to produce the lens fibres. These are arranged in an onion-
like way and are covered with an elastic capsule. The capsule is
attached through fine ligaments to the cilary muscle which alters
the shape of the lens.
As new cells are formed, older cells become fibres and are
progressively displaced towards the centre of the lens. The more
superficial fibres form the cortex while the central fibres
constitute the nucleus.
The lens fibres are transparent, ribbon-like cells, each of
which runs completely around from the front of the lens to the
back. Injury to any single fibre will, in time, extend throughout
the entire fibre cell and will be more apparent in the thicker
posterior part of the lens (posterior subcapsular cataract).
The lens, like the cornea, is not optically homogeneous but it
is transparent in the visible range of the spectrum. However,
increasing absorption of short-wavelength light occurs with age
(Wolbarsht et al., 1977). The transparancy is the result of a
precise relation of the various minute, optically well ordered,
constituents. A disturbance of the cell elements or the fibre will
result in the hydration of the fibre. Damage to the lens disturbs
this relation resulting in increased light scattering. The lens
becomes milky (a cataract).
8.1.3. The retina and choroid
The retina is divided into two major components - a pigmented
monolayer - the retinal pigmented epithelium (RPE) and a
multilayered lamina of neural cells called the neural retina. The
light-sensitive cells are adjacent to the RPE. There are two types
of photoreceptor cells: rods and cones, named according to the
shape of the distal (away from the synaptic end) extension of the
photoreceptor cells. Light entering the eye must first pass
through all of the neural retina before striking the receptor
cells. In the retina, there are probably 120 million rods
approximately 60 µm long and 2 µm in diameter and 6 million cones
approximately 50 µm long and 3 - 5 µm in diameter. These receptor
cells are interconnected by other specialized cells. Rods are
mainly concerned with vision at low light levels and are
predominant in the periphery of the retina. Cones are responsible
for colour vision and high acuity visual tasks. They are most
concentrated in a specialized central region of the retina, the
fovea. The fovea is responsible for central vision used for
reading. The anatomical aspects of the retinal pigment epithelium
(RPE) and adjacent layers are of particular importance in a study
of retinal injury from light sources. The outer segments of the
rods and cones (the light-sensitive section of the cell) are
immediately anterior to the RPE.
There are very small protrusions (microvilli) of the RPE that
extend upward around the outer segments (Fig. 11). As the cones do
not extend as near to the RPE as the rods, the microvilli extend
out further to the cone outer segments. It is known that the RPE
plays a critical role in the retinal metabolism and photochemistry,
hence proper functioning of the REP is essential for normal vision.
The outer segments of both rods and cones contain a stack of coin-
like membranes on which their visual pigments are oriented. These
discs are in a continuous state of flux. In rods, 10 - 30 new
discs are made each day, while a similar number are phagocytized by
the RPE cells (Fig. 11); the rate of shedding is greatest in the
early morning. The life span of a disc is two weeks. The cone
lamellar membranes do not form complete discs and do not appear to
shed in the same manner as in the rods. The renewal activity of
the cones is slower than that of the rods and it occurs at night.
Bruch's membrane separates the RPE from the blood supply in the
capillary layer of the choriocapillaries which is the innermost
layer of the choroid, and is where the smallest vessels are found.
The choroid is an extremely vascular spongy tissue with many
pigmented cells scattered throughout it. The thickness is
variable; the average is about 250 µm. The blood vessels
progressively increase in size towards the scleral surface. It has
been suggested by Ernest & Potts (1971) that the primary function
of the blood in the choroid is to keep the eye warm and at a
uniform temperature. Because of this extreme vascularity, heat
from laser exposures introduced in this region under steady-state
conditions will do little to elevate the temperature unless high
power levels are used.
The cornea and conjuctiva are tissues rich in sensory receptors
and nerve endings serving as triggers of protective reflexes for
mechanical and thermal agents.
As the epithelial cells must survive a harsh environment, they
have a very short life span of approximately 2 - 5 days. If the
cell death rate increases (as in photokerititis) and replacement is
not in step with the loss, small erosions will develop that elicit
a pain sensation.
The corneal stroma is built in a very regular fashion, which
accounts for its transparency. If this regularity is distorted,
i.e., by an oedema, the cornea will be less transparent or even
opaque. A disturbance of the epithelium, or, more important still,
of the inner cell layer of the cornea (the endothelium) will result
in an oedema. Any scar formation will also alter the regular
construction and hence will result in an opaque cornea. Thus
serious visual handicap will be the result of irreversible corneal
damage.
8.1.2. The lens
The lens is a tissue built up from cells that progressively
deform to produce the lens fibres. These are arranged in an onion-
like way and are covered with an elastic capsule. The capsule is
attached through fine ligaments to the cilary muscle which alters
the shape of the lens.
As new cells are formed, older cells become fibres and are
progressively displaced towards the centre of the lens. The more
superficial fibres form the cortex while the central fibres
constitute the nucleus.
The lens fibres are transparent, ribbon-like cells, each of
which runs completely around from the front of the lens to the
back. Injury to any single fibre will, in time, extend throughout
the entire fibre cell and will be more apparent in the thicker
posterior part of the lens (posterior subcapsular cataract).
The lens, like the cornea, is not optically homogeneous but it
is transparent in the visible range of the spectrum. However,
increasing absorption of short-wavelength light occurs with age
(Wolbarsht et al., 1977). The transparancy is the result of a
precise relation of the various minute, optically well ordered,
constituents. A disturbance of the cell elements or the fibre will
result in the hydration of the fibre. Damage to the lens disturbs
this relation resulting in increased light scattering. The lens
becomes milky (a cataract).
8.1.3. The retina and choroid
The retina is divided into two major components - a pigmented
monolayer - the retinal pigmented epithelium (RPE) and a
multilayered lamina of neural cells called the neural retina. The
light-sensitive cells are adjacent to the RPE. There are two types
of photoreceptor cells: rods and cones, named according to the
shape of the distal (away from the synaptic end) extension of the
photoreceptor cells. Light entering the eye must first pass
through all of the neural retina before striking the receptor
cells. In the retina, there are probably 120 million rods
approximately 60 µm long and 2 µm in diameter and 6 million cones
approximately 50 µm long and 3 - 5 µm in diameter. These receptor
cells are interconnected by other specialized cells. Rods are
mainly concerned with vision at low light levels and are
predominant in the periphery of the retina. Cones are responsible
for colour vision and high acuity visual tasks. They are most
concentrated in a specialized central region of the retina, the
fovea. The fovea is responsible for central vision used for
reading. The anatomical aspects of the retinal pigment epithelium
(RPE) and adjacent layers are of particular importance in a study
of retinal injury from light sources. The outer segments of the
rods and cones (the light-sensitive section of the cell) are
immediately anterior to the RPE.
There are very small protrusions (microvilli) of the RPE that
extend upward around the outer segments (Fig. 11). As the cones do
not extend as near to the RPE as the rods, the microvilli extend
out further to the cone outer segments. It is known that the RPE
plays a critical role in the retinal metabolism and photochemistry,
hence proper functioning of the REP is essential for normal vision.
The outer segments of both rods and cones contain a stack of coin-
like membranes on which their visual pigments are oriented. These
discs are in a continuous state of flux. In rods, 10 - 30 new
discs are made each day, while a similar number are phagocytized by
the RPE cells (Fig. 11); the rate of shedding is greatest in the
early morning. The life span of a disc is two weeks. The cone
lamellar membranes do not form complete discs and do not appear to
shed in the same manner as in the rods. The renewal activity of
the cones is slower than that of the rods and it occurs at night.
Bruch's membrane separates the RPE from the blood supply in the
capillary layer of the choriocapillaries which is the innermost
layer of the choroid, and is where the smallest vessels are found.
The choroid is an extremely vascular spongy tissue with many
pigmented cells scattered throughout it. The thickness is
variable; the average is about 250 µm. The blood vessels
progressively increase in size towards the scleral surface. It has
been suggested by Ernest & Potts (1971) that the primary function
of the blood in the choroid is to keep the eye warm and at a
uniform temperature. Because of this extreme vascularity, heat
from laser exposures introduced in this region under steady-state
conditions will do little to elevate the temperature unless high
power levels are used.
 8.2. Spectral Properties of the Eye
To understand the biological effects of different optical
spectral bands on different ocular structures, it is first
necessary to consider the relative spectral absorption of the
different ocular media. Fig. 12 shows the spectral absorption for
each of the media.
Essentially all incident optical radiation at very short
wavelengths in the ultraviolet and long wavelengths in the infrared
is absorbed in the cornea. Clearly an ocular structure cannot be
damaged unless optical radiation is absorbed. In some instances,
particularly in the UV region, less than 1% of the total incident
radiation absorbed in a structure can be significant, if the
radiation contains critically effective wavelengths.
8.2. Spectral Properties of the Eye
To understand the biological effects of different optical
spectral bands on different ocular structures, it is first
necessary to consider the relative spectral absorption of the
different ocular media. Fig. 12 shows the spectral absorption for
each of the media.
Essentially all incident optical radiation at very short
wavelengths in the ultraviolet and long wavelengths in the infrared
is absorbed in the cornea. Clearly an ocular structure cannot be
damaged unless optical radiation is absorbed. In some instances,
particularly in the UV region, less than 1% of the total incident
radiation absorbed in a structure can be significant, if the
radiation contains critically effective wavelengths.
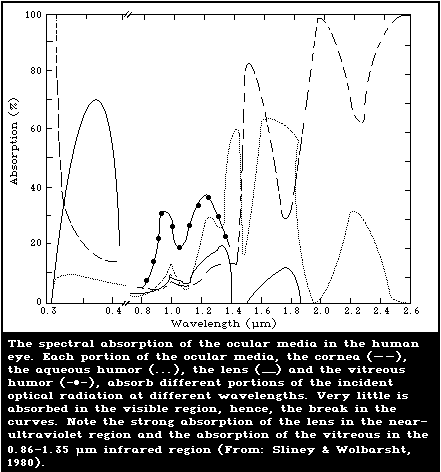 8.3. Injury to the Anterior Portion of the Eye
The anterior structures of the eye are the cornea, conjunctiva,
aqueous humor, iris, and lens. The cornea, aqueous humor, and lens
are part of the optical pathway and, as such, must be transparent
to light. Loss of transparency is serious. Because of the rapid
turnover of corneal epithelial cells, damage limited to this outer
layer can be expected to be temporary. Indeed, injury to this
tissue by exposure to UV-B and UV-C, as occurs in a particular
keratoconjuntivitis, the ultraviolet photokeratitis or
photoophthalmia (known also as "arc eye", or "welder's flash"),
seldom lasts more than one or two days. Unless deeper tissues of
the cornea are also affected, surface epithelium injuries are
rarely permanent.
Near-ultraviolet and near-infrared radiation (UV-A, IR-A, and
possibly IR-B) are strongly absorbed in the lens of the eye.
Damage to this structure is of great concern in that the lens has a
very slow turnover of cells. A one-day exposure may result in
effects that will not become evident for many years. This is
probably the case of glass-blower's or steel puddler's cataract and
in cataracts caused by ionizing radiation. Long-term exposure may
also result in delayed effects (Tengroth et al., 1980).
8.3.1. Effects on the cornea
UV-B and UV-C radiation are absorbed in the cornea and
conjunctiva and sufficiently high doses will cause kerato-
conjunctivitis. The initial effect of UVR exposure is damage to,
or destruction of, the epithelial cells. Under normal conditions,
the corneal epithelial layer is completely replaced in a matter of
a day or so. After exposure, there is a latent period, generally
shorter than 12 h, which varies inversely with the exposure dose.
Healing of the corneal and conjuctival epithelium takes 1 - 2 days.
In severe exposures, damage to Bowman's membrane and the stroma may
occur and is commonly followed by scar formation (usually of a
milky appearance) and sometimes by invasion of the entire cornea by
blood vessels. Some limited recovery of moderate damage may occur
in months or years.
The action spectrum and threshold dose for ultraviolet
keratoconjunctivitis (Fig. 13) have been generally agreed on by
several groups of investigators.
8.3. Injury to the Anterior Portion of the Eye
The anterior structures of the eye are the cornea, conjunctiva,
aqueous humor, iris, and lens. The cornea, aqueous humor, and lens
are part of the optical pathway and, as such, must be transparent
to light. Loss of transparency is serious. Because of the rapid
turnover of corneal epithelial cells, damage limited to this outer
layer can be expected to be temporary. Indeed, injury to this
tissue by exposure to UV-B and UV-C, as occurs in a particular
keratoconjuntivitis, the ultraviolet photokeratitis or
photoophthalmia (known also as "arc eye", or "welder's flash"),
seldom lasts more than one or two days. Unless deeper tissues of
the cornea are also affected, surface epithelium injuries are
rarely permanent.
Near-ultraviolet and near-infrared radiation (UV-A, IR-A, and
possibly IR-B) are strongly absorbed in the lens of the eye.
Damage to this structure is of great concern in that the lens has a
very slow turnover of cells. A one-day exposure may result in
effects that will not become evident for many years. This is
probably the case of glass-blower's or steel puddler's cataract and
in cataracts caused by ionizing radiation. Long-term exposure may
also result in delayed effects (Tengroth et al., 1980).
8.3.1. Effects on the cornea
UV-B and UV-C radiation are absorbed in the cornea and
conjunctiva and sufficiently high doses will cause kerato-
conjunctivitis. The initial effect of UVR exposure is damage to,
or destruction of, the epithelial cells. Under normal conditions,
the corneal epithelial layer is completely replaced in a matter of
a day or so. After exposure, there is a latent period, generally
shorter than 12 h, which varies inversely with the exposure dose.
Healing of the corneal and conjuctival epithelium takes 1 - 2 days.
In severe exposures, damage to Bowman's membrane and the stroma may
occur and is commonly followed by scar formation (usually of a
milky appearance) and sometimes by invasion of the entire cornea by
blood vessels. Some limited recovery of moderate damage may occur
in months or years.
The action spectrum and threshold dose for ultraviolet
keratoconjunctivitis (Fig. 13) have been generally agreed on by
several groups of investigators.
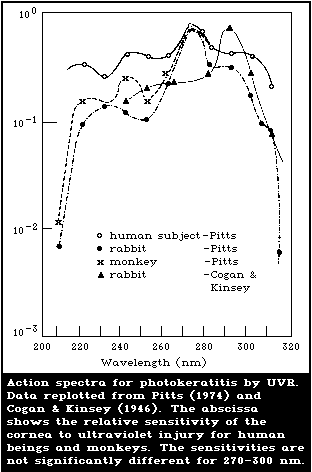 The reciprocity or irradiance and exposure duration probably
hold for time periods similar to those for ultraviolet erythema
(reddening) of the skin. Specifically, it matters little whether
radiant exposure of the cornea occurs in 1 µs or in 2 h. The
product of the irradiance and the duration of exposure required for
the same effect is a constant for periods up to several h.
The cornea is quite transparent in the IR-A. In the IR-B,
there are some fairly narrow water absorption bands at 1430 nm and
1959 nm. Above 2000 nm, absorption is very high, making the cornea
very susceptible to far-infrared radiation. Thus, as might be
expected, the threshold for damage corresponds to the absorption
bands. Radiation in the IR-C band can induce a burn on the cornea
similar to that on the skin.
The nerve endings of the cornea are quite sensitive to all
temperature elevations and an elevation of 10 °C causes a pain
response. With full-face exposure, a temperature rise can be felt
before corneal pain appears.
Infrared lasers such as CO2 lasers (10.69 µm), HF, and DF
lasers (2.7 - 4.0 µm) or CO lasers (5 µm), having cw output
irradiances of the order of 10 W/cm2 or more can produce corneal
lesions by delivering at least 0.5 - 10 J/cm2, before the blink
reflex is operative (Fig. 14).
The reciprocity or irradiance and exposure duration probably
hold for time periods similar to those for ultraviolet erythema
(reddening) of the skin. Specifically, it matters little whether
radiant exposure of the cornea occurs in 1 µs or in 2 h. The
product of the irradiance and the duration of exposure required for
the same effect is a constant for periods up to several h.
The cornea is quite transparent in the IR-A. In the IR-B,
there are some fairly narrow water absorption bands at 1430 nm and
1959 nm. Above 2000 nm, absorption is very high, making the cornea
very susceptible to far-infrared radiation. Thus, as might be
expected, the threshold for damage corresponds to the absorption
bands. Radiation in the IR-C band can induce a burn on the cornea
similar to that on the skin.
The nerve endings of the cornea are quite sensitive to all
temperature elevations and an elevation of 10 °C causes a pain
response. With full-face exposure, a temperature rise can be felt
before corneal pain appears.
Infrared lasers such as CO2 lasers (10.69 µm), HF, and DF
lasers (2.7 - 4.0 µm) or CO lasers (5 µm), having cw output
irradiances of the order of 10 W/cm2 or more can produce corneal
lesions by delivering at least 0.5 - 10 J/cm2, before the blink
reflex is operative (Fig. 14).
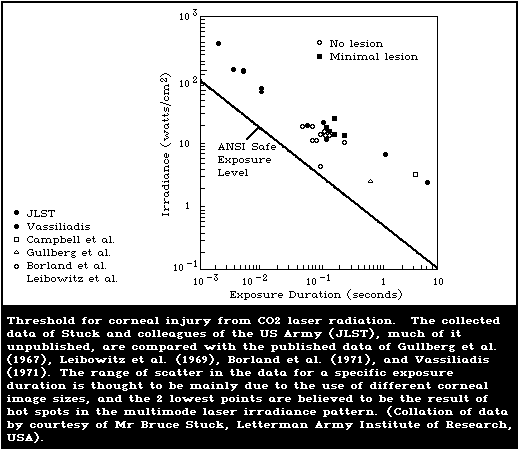 8.3.2. UVR lenticular effects
The lens has much the same sensitivity to UVR as the cornea.
With exposure to UV-A, there is substantial transmission in the
cornea and high absorption in the lens (Fig. 12).
Acute exposures of the order of 105 to 3 x 106 J/m2 (10 to
300 J/cm2) to radiation in the 320 - 400 nm region cause corneal
opacities, but only exposure to radiation in the UV-B region
appears to be strongly effective in causing lenticular opacities
under acute exposure conditions (Pitts et al., 1977; Zuchlich &
Kurtin, 1977) (Fig. 15). The lenticular opacity may only last for
a few days at low exposures.
8.3.2. UVR lenticular effects
The lens has much the same sensitivity to UVR as the cornea.
With exposure to UV-A, there is substantial transmission in the
cornea and high absorption in the lens (Fig. 12).
Acute exposures of the order of 105 to 3 x 106 J/m2 (10 to
300 J/cm2) to radiation in the 320 - 400 nm region cause corneal
opacities, but only exposure to radiation in the UV-B region
appears to be strongly effective in causing lenticular opacities
under acute exposure conditions (Pitts et al., 1977; Zuchlich &
Kurtin, 1977) (Fig. 15). The lenticular opacity may only last for
a few days at low exposures.
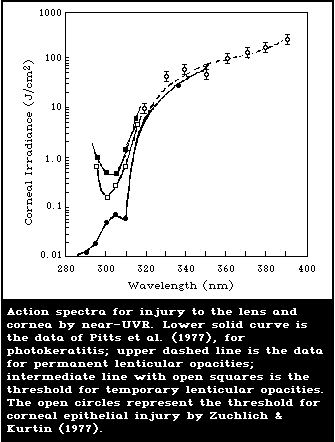 On the other hand, since long-term exposure to UVR at ambient
outdoor levels may be associated with a reduction in the ability of
the lens to transmit short-wavelength light (Lerman, 1980b) and
with senile cataracts (Weale, 1982), the effects of UVR on the lens
may be cummulative. In addition, there is experimental evidence
that UV-A radiation can induce photosensitized oxidation of the
ocular lens (Zigler & Goosey, 1981).
8.3.3. Infrared cataract
As explained earlier, the ocular media absorb an increasing
amount of the radiant energy incident upon the cornea for
increasing wavelengths in the near infrared (IR-A). For infrared
wavelengths greater than 1400 nm (IR-B and IR-C), the cornea and
aqueous absorb essentially all of the incident radiation, and,
beyond 1900 nm, the cornea is considered to be the sole absorber
(Fig. 12). This absorbed energy may be conducted to interior
structures of the eyes elevating the temperature of the lens, as
well as that of the cornea itself. Heating of the iris by
absorption of visible and near-infrared radiation is considered to
play a role in the development of opacities in the lens, at least
for short exposure times (Goldmann, 1933). Hence, it would be
expected that the spectral absorption and reflectance of the iris
would determine the action spectrum for this effect, for such
exposure times. However, radiation of the lens alone, at lower
levels for longer exposures induces cataracts in the part of the
lens not covered by the iris (Vogt, 1919; Wolbarsht, 1978b). Most
IR-B and IR-C lasers cause damage only to the cornea (Andeev et
al., 1978; Stuck et al., 1981).
8.4. Retinal Injury
The retina is particularly vulnerable to visible and near-
infrared radiation, a spectral domain known as the retinal hazard
region. In most real situations, the refractive power of the
cornea and lens leads to a dramatic increase in irradiance between
the cornea and the retina. When an object is viewed directly, the
light forms an image on the fovea, the centre of the macula, which,
in man, is approximately 0.25 mm in diameter. The typical result
of a retinal injury is a blind spot (i.e., a scotoma) within the
irradiated area. A peripheral scotoma, unless very large, may go
unnoticed. However, if the scotoma results from a lesion located
in the fovea, severe visual handicap results. A central scotoma
could result from looking directly at a hazardous source. The size
of the scotoma depends on the irradiance relative to threshold, the
angular extent of the source, and the extent of accommodation.
Laser lesions of the retina resulting from exposures to light
cause many alterations in structure that can only be seen
histologically (Marshall, 1973). Fig. 16 shows two typical lesions
in the macula of a human being.
The subjective loss of vision associated with laser-induced
retinal injury may be immediate or may develop progressively over a
period of hours or days (Gabel & Birngruber, 1981). The extent to
which visual function recovers depends on the size of the initial
injury and the types of retinal cells involved, as well as the
presence and extent of retinal haemorrhages and their subsequent
degree of resorption (Boldry, et al., 1981). Retinal neurons do
not undergo cell division so repair by cell replacement does not
occur. In small lesions, recovery may result from either growth of
new parts of damaged cells such as photoreceptor outer segments, or
by migration of viable cells into the damaged site. Severe damage
is irreversible and visual loss is permanent.
On the other hand, since long-term exposure to UVR at ambient
outdoor levels may be associated with a reduction in the ability of
the lens to transmit short-wavelength light (Lerman, 1980b) and
with senile cataracts (Weale, 1982), the effects of UVR on the lens
may be cummulative. In addition, there is experimental evidence
that UV-A radiation can induce photosensitized oxidation of the
ocular lens (Zigler & Goosey, 1981).
8.3.3. Infrared cataract
As explained earlier, the ocular media absorb an increasing
amount of the radiant energy incident upon the cornea for
increasing wavelengths in the near infrared (IR-A). For infrared
wavelengths greater than 1400 nm (IR-B and IR-C), the cornea and
aqueous absorb essentially all of the incident radiation, and,
beyond 1900 nm, the cornea is considered to be the sole absorber
(Fig. 12). This absorbed energy may be conducted to interior
structures of the eyes elevating the temperature of the lens, as
well as that of the cornea itself. Heating of the iris by
absorption of visible and near-infrared radiation is considered to
play a role in the development of opacities in the lens, at least
for short exposure times (Goldmann, 1933). Hence, it would be
expected that the spectral absorption and reflectance of the iris
would determine the action spectrum for this effect, for such
exposure times. However, radiation of the lens alone, at lower
levels for longer exposures induces cataracts in the part of the
lens not covered by the iris (Vogt, 1919; Wolbarsht, 1978b). Most
IR-B and IR-C lasers cause damage only to the cornea (Andeev et
al., 1978; Stuck et al., 1981).
8.4. Retinal Injury
The retina is particularly vulnerable to visible and near-
infrared radiation, a spectral domain known as the retinal hazard
region. In most real situations, the refractive power of the
cornea and lens leads to a dramatic increase in irradiance between
the cornea and the retina. When an object is viewed directly, the
light forms an image on the fovea, the centre of the macula, which,
in man, is approximately 0.25 mm in diameter. The typical result
of a retinal injury is a blind spot (i.e., a scotoma) within the
irradiated area. A peripheral scotoma, unless very large, may go
unnoticed. However, if the scotoma results from a lesion located
in the fovea, severe visual handicap results. A central scotoma
could result from looking directly at a hazardous source. The size
of the scotoma depends on the irradiance relative to threshold, the
angular extent of the source, and the extent of accommodation.
Laser lesions of the retina resulting from exposures to light
cause many alterations in structure that can only be seen
histologically (Marshall, 1973). Fig. 16 shows two typical lesions
in the macula of a human being.
The subjective loss of vision associated with laser-induced
retinal injury may be immediate or may develop progressively over a
period of hours or days (Gabel & Birngruber, 1981). The extent to
which visual function recovers depends on the size of the initial
injury and the types of retinal cells involved, as well as the
presence and extent of retinal haemorrhages and their subsequent
degree of resorption (Boldry, et al., 1981). Retinal neurons do
not undergo cell division so repair by cell replacement does not
occur. In small lesions, recovery may result from either growth of
new parts of damaged cells such as photoreceptor outer segments, or
by migration of viable cells into the damaged site. Severe damage
is irreversible and visual loss is permanent.
 Only an extremely small fraction of UVR incident on the cornea
reaches the retina. Nevertheless, the fraction of a percent of
UV-A that reaches the retina can have adverse effects, as has been
demonstrated by Zuchlich & Taboada (1978). Retinal lesions were
seen following exposure to a He-Cd laser at 325 nm. Because of the
strong scattering of UV-A in the ocular media, it is difficult to
estimate the retinal exposure. Young rhesus monkeys were used,
hence, the transmission of the ocular media was still relatively
high (perhaps 1%), whereas, in adult human beings this transmission
is much less.
Aphakics (persons with the lens removed) are special exceptions
to this rule and would be expected to be extremely susceptible to
UV-A injury of the retina, particularly as their corrective lenses
will usually transmit UV-A radiation very well.
8.4.1. Determining the retinal exposure
The optical properties of the eye play an important role in
determining retinal injury. Such factors as the image quality,
pupil size, spectral absorption, and scattering by the cornea,
aqueous, lens, and vitreous, as well as the spectral reflectance of
the fundus and absorption and scattering in the various retinal
layers, must be known for a definitive description of retinal
exposure. These factors will be considered separately.
8.4.1.1. Pupil size
The limiting aperture of the eye determines the amount of
radiant energy entering the eye, and thus reaching the retina. It
is therefore proportional to the area of the pupil. For the
normal, dark-adapted eye, pupil sizes range from approximately 7 to
8 mm; for outdoor daylight, the normal pupil constricts to
approximately 1.6 - 2.0 mm. The ratio of areas between a 2-mm and
an 8-mm pupil is: 1:16; hence, a 2-mm pupil permits the entry of
one-sixteenth of the light admitted by a 8-mm pupil. The angle
subtended by the source also plays a role; thus a light source of a
given size and luminance causes a different pupil size, depending
on the viewing distance (i.e., the image area on the retina), and
the luminance of the surrounding field.
The pupilomotor reflex will constrict the pupil on exposure to
a bright light source within a period of the order of 20 ms
(Davson, ed., 1962). Some medications and drugs will create an
abnormal pupil size. Therefore, in a large population, the pupil
size may vary greatly under the same environmental exposure
conditions.
8.4.1.2. Spectral transmission of the ocular media and spectral
absorption by the retina and choroid
The transmission of the ocular media between 300 nm and 1400 nm
has been studied by several investigators and results vary
(Geeraets & Berry, 1968; Gabel et al., 1976). Fig. 17 shows a
representative spectral transmission of the human ocular media.
Only an extremely small fraction of UVR incident on the cornea
reaches the retina. Nevertheless, the fraction of a percent of
UV-A that reaches the retina can have adverse effects, as has been
demonstrated by Zuchlich & Taboada (1978). Retinal lesions were
seen following exposure to a He-Cd laser at 325 nm. Because of the
strong scattering of UV-A in the ocular media, it is difficult to
estimate the retinal exposure. Young rhesus monkeys were used,
hence, the transmission of the ocular media was still relatively
high (perhaps 1%), whereas, in adult human beings this transmission
is much less.
Aphakics (persons with the lens removed) are special exceptions
to this rule and would be expected to be extremely susceptible to
UV-A injury of the retina, particularly as their corrective lenses
will usually transmit UV-A radiation very well.
8.4.1. Determining the retinal exposure
The optical properties of the eye play an important role in
determining retinal injury. Such factors as the image quality,
pupil size, spectral absorption, and scattering by the cornea,
aqueous, lens, and vitreous, as well as the spectral reflectance of
the fundus and absorption and scattering in the various retinal
layers, must be known for a definitive description of retinal
exposure. These factors will be considered separately.
8.4.1.1. Pupil size
The limiting aperture of the eye determines the amount of
radiant energy entering the eye, and thus reaching the retina. It
is therefore proportional to the area of the pupil. For the
normal, dark-adapted eye, pupil sizes range from approximately 7 to
8 mm; for outdoor daylight, the normal pupil constricts to
approximately 1.6 - 2.0 mm. The ratio of areas between a 2-mm and
an 8-mm pupil is: 1:16; hence, a 2-mm pupil permits the entry of
one-sixteenth of the light admitted by a 8-mm pupil. The angle
subtended by the source also plays a role; thus a light source of a
given size and luminance causes a different pupil size, depending
on the viewing distance (i.e., the image area on the retina), and
the luminance of the surrounding field.
The pupilomotor reflex will constrict the pupil on exposure to
a bright light source within a period of the order of 20 ms
(Davson, ed., 1962). Some medications and drugs will create an
abnormal pupil size. Therefore, in a large population, the pupil
size may vary greatly under the same environmental exposure
conditions.
8.4.1.2. Spectral transmission of the ocular media and spectral
absorption by the retina and choroid
The transmission of the ocular media between 300 nm and 1400 nm
has been studied by several investigators and results vary
(Geeraets & Berry, 1968; Gabel et al., 1976). Fig. 17 shows a
representative spectral transmission of the human ocular media.
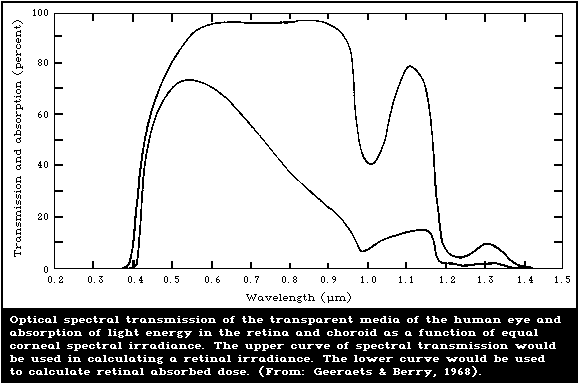 There is considerable individual variability in these spectral
quantities and this must be remembered when using the data in an
accurate calculation. The other factor that must not be forgotten
is the shift of the short-wavelength cutoff at 390 - 410 nm with
age. The lens transmits less UV-A and blue light with increasing
age as it yellows. With the above factors taken into account, it
is possible to multiply the spectral absorption data of the retina
and choroid by the spectral transmission data for the ocular media
to arrive at an estimate of the absorbed spectral exposure dose in
the retina and choroid, relative to the spectral radiant exposure
at the cornea. This spectral effectiveness curve for retinal
thermal injury is applicable, at least, to exposure durations of
less than approximately 10 s (Fig. 17).
8.4.1.3. Optical image quality
The retinal image size can be calculated for most extended
sources by geometrical optics. As shown in Fig. 18, the angle
subtended by an extended source defines the image size. The
effective focal length of the relaxed normal eye fe is approx.
1.7 cm. With fe known, the retinal image size dr can be
calculated, if the viewing distance r and the dimension of the
light source DL are known:
dr = DLfe/r Equation (12)
From this, the quantitative relation can be obtained of retinal
irradiance Er to source radiance L (or retinal illuminance to
source luminance) for small angles:
Er = (pi x dp2 L x tau)/4fe2
= 0.27 dp2 x L x tau(for dp in cm) Equation (13)
where dp is the pupillary diameter and tau is the spectral
transmission of the ocular media.
From equation 13, it is possible to define a permissible
radiance (luminance) from a permissible retinal irradiance for any
source of known radiance or luminance, without taking into account
the viewing angle or viewing distance.
Each source point has a corresponding image point, hence, the
retinal irradiance in an incremental area of the image is related
to the radiance of a corresponding incremental area of the source
(Hartman & Kleman, 1980).
8.4.1.4. Small images
Equation 13 breaks down for very small images (or for very
small hot spots in an image), where the source or source element in
question subtends an angle of less than 10 minutes-of-arc (i.e.,
image size is less than 50 µm).
There is considerable individual variability in these spectral
quantities and this must be remembered when using the data in an
accurate calculation. The other factor that must not be forgotten
is the shift of the short-wavelength cutoff at 390 - 410 nm with
age. The lens transmits less UV-A and blue light with increasing
age as it yellows. With the above factors taken into account, it
is possible to multiply the spectral absorption data of the retina
and choroid by the spectral transmission data for the ocular media
to arrive at an estimate of the absorbed spectral exposure dose in
the retina and choroid, relative to the spectral radiant exposure
at the cornea. This spectral effectiveness curve for retinal
thermal injury is applicable, at least, to exposure durations of
less than approximately 10 s (Fig. 17).
8.4.1.3. Optical image quality
The retinal image size can be calculated for most extended
sources by geometrical optics. As shown in Fig. 18, the angle
subtended by an extended source defines the image size. The
effective focal length of the relaxed normal eye fe is approx.
1.7 cm. With fe known, the retinal image size dr can be
calculated, if the viewing distance r and the dimension of the
light source DL are known:
dr = DLfe/r Equation (12)
From this, the quantitative relation can be obtained of retinal
irradiance Er to source radiance L (or retinal illuminance to
source luminance) for small angles:
Er = (pi x dp2 L x tau)/4fe2
= 0.27 dp2 x L x tau(for dp in cm) Equation (13)
where dp is the pupillary diameter and tau is the spectral
transmission of the ocular media.
From equation 13, it is possible to define a permissible
radiance (luminance) from a permissible retinal irradiance for any
source of known radiance or luminance, without taking into account
the viewing angle or viewing distance.
Each source point has a corresponding image point, hence, the
retinal irradiance in an incremental area of the image is related
to the radiance of a corresponding incremental area of the source
(Hartman & Kleman, 1980).
8.4.1.4. Small images
Equation 13 breaks down for very small images (or for very
small hot spots in an image), where the source or source element in
question subtends an angle of less than 10 minutes-of-arc (i.e.,
image size is less than 50 µm).
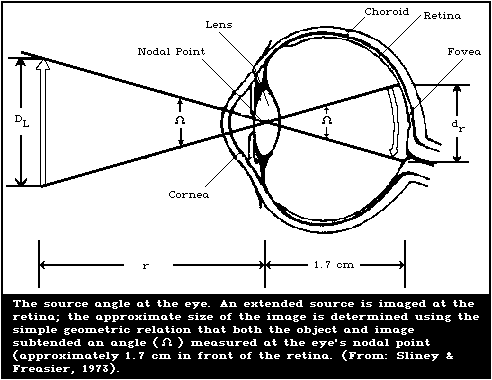 The diffraction theory can be applied to estimate the minimal
retinal image size for viewing a point source such as a laser.
However, scattering in the ocular media and corneal aberations
limits this image diameter to approximately 10 - 20 µm (Sliney,
1971).
It would be expected that, in the case of small-sized images,
the retinal hazard would increase in proportion to the area of the
pupil. Therefore, night-time viewing of a point source would be
expected to be far more dangerous than day-time viewing; however,
this is not the case, since the image blur increases with larger
pupil sizes. It is worthwhile noting that the increase in
irradiance from cornea to retina, when the relaxed eye views a
point source, is about 105 (100 000 times) (Sliney & Freasier,
1973). Almost any directly viewed laser can appear as a point
source.
8.4.1.5. Retinal pigment epithelium (RPE) absorption
As previously indicated, visible and near-infrared radiation is
transmitted through the ocular media and is absorbed principally in
the retina. The radiation passes through the neural layers of the
retina before reaching the RPE and choroid. The visual pigments in
the rods and cones absorb only a small fraction of light to
initiate the visual response, perhaps only 5% of the total energy
entering the eye. The RPE absorbs a substantial fraction of the
light (about 50% in the green) and is optically the most absorbent
layer. As the absorption takes place in a highly concentrated
layer of melanin granules approximately 3 - 6 µm thick, the greatest
temperature rise occurs in this layer (Bergquist et al., 1978;
Birngruber, 1978). The actual size, shape, distribution, and
physical characteristics of individual melanin granules become
quite important for a thermal model adequate to describe the
behaviour of this layer, during very short pulse exposures
(Wolbarsht, et al., 1980). The granules may be heated to
incandescence during Q-switched exposures, and this incandescence
can be seen, if viewed during a 1064-nm (neodymium-YAG) laser
experiment (Mueller & Ham, 1980, private communication).
8.4.2. Chorioretinal thermal injury
The retinal injury mechanism is considered to be largely
thermal for accidental exposures from arc lamps, cw lasers, or
optically aided viewing of the sun, for durations of the order of
1 ms to ~10 s. Since injury appears to result principally from
protein denaturation and enzyme inactivation, the variation in
retinal temperature during and following the insult must be
considered (Beatrice & Velez, 1975). Several efforts to develop
mathematical models for light absorption, heat flow, and the rate-
process injury mechanisms within the complex structure of the
retina have been moderately successful, over periods of exposure
lasting from 1 ms to 10 s (Vos, 1966a; Mainster et al., 1970;
Allen, 1980).
The tissue surrounding the absorption site can much more
readily conduct away the absorbed heat for images, 10 - 50 µm in
diameter, than it can for large images of the order of 1000 µm
(1 mm). Indeed, retinal injury thresholds for the same time range
of 0.1 - 10 s are very closely related to image size, as would be
expected from calculations of heat flow in the retina. For
example, exposure to irradiances of 10-100 kW/m2 (i.e., 1-10 W/cm2)
results in a minimal retinal injury threshold for a 1000-µm image,
whereas an irradiance of 10 MW/m2 (1 kW/cm2) is required to produce
the same type of threshold lesion in a 20-µm image (Ham et al.,
1970).
For short-pulse durations, the reason for the spot-size
dependence of the threshold is not clear (Frisch et al., 1971).
The expectation, when exposure durations are of the order of 1 ms,
is that injury will take place before there is significant heat
flow. Indeed, the variation of threshold with pulse duration
itself is also rather puzzling, especially the increase in
threshold for 20-ns, Q-switched pulses over those of 1-µs duration
(Hansen & Fine, 1968; Harlen, 1978; Anderson, 1980b). Obviously,
the Q-switched pulse energy is being dissipated in some mechanism
such as a mechanical displacement of tissue (an acoustic
transient), which does not contribute to the normal thermal injury
process that determines the minimum threshold.
In studies conducted by Beatrice & Lund (1979) with image
distributions that were non-circular, such as line images on the
retina, circular lesions were produced after long-term exposures.
This would be predicted by thermal injury and heat flow
calculations. Very short, Q-switched exposures with similar line
image distributions produced lesions that were very elongated, as,
again, would be predicted by a simple thermal model or injury. It
might be thought that the contribution of acoustic transients from
such a short exposure would have been to enlarge the lesion.
Photoacoustic effects should certainly make a considerable
contribution; but whether the acoustic transient adds to, or
subtracts from the injury mechanism is not yet clear.
For short-term exposures (< 1 µs) resulting from Q-switched
lasers, exploding wires, super-radiant light, and mode-locked
lasers, the exposure thresholds of injury are lowest. Although it
is believed that, for a Q-switched exposure, the injury mechanism
is largely thermal, the effect of acoustic transients due to rapid
heating and thermal expansion in the immediate vicinity of the
absorption site (individual melanin granules) may play a role. For
still shorter durations of exposure, direct electric field effects,
Raman and Brillouin scattering, and multiphoton absorption could
play a role in the damage mechanism (Greisemann & Marti, 1978;
Rockerolles, 1978).
8.4.3. Location of retinal burns
As previously explained, the different regions of the retina
play different roles in vision. Thus, the significance of
functional loss of all or part of any one of these regions, because
of retinal injury, varies. The loss of foveal vision seriously
reduces visual performance. Limited peripheral loss could be
unnoticed, subjectively (Kaufman, 1970; Holzinger et al., 1978).
8.5. Photochemical Retinal Injury
8.5.1. Very long-term exposure
The human retina is normally subjected to irradiances below
1 W/m2 (10-4 W/cm2), as shown in Fig. 19, except for occasional
momentary exposure to the sun, welding arcs, and similar bright
sources. The retinal images resulting from viewing such sources
are often quite small (for example 0.15 mm for the sun) and the
duration of exposure is normally limited to the duration of the
blink reflex (0.15 - 0.2 s). Natural aversion to bright light
usually limits further retinal exposures above 10-4 W/cm2. Until
recently, few studies of adverse retinal effects existed for the
irradiance range of 10-4-1 W/cm2. Studies in this range have
generally centred on flash blindness effects following light
exposures lasting up to 1 s.
Exposure of large areas of the retina to moderately high
luminance light of the order of 105 cd/m2 (~100 µW/cm2, i.e.,
1 W/m2 at the retina) for durations of one to several hours has
been investigated in experimental animals. Generally, the light
sources employed in these studies were fluorescent lamps. A
thermally-enhanced photochemical mechanism of injury or a
phototoxic effect appears to be most likely (Kuwabara, 1970; Noell
& Albrecht, 1971). More recently, similar fluorescent light
exposure of rhesus monkeys with dilated pupils showed that this
effect was not limited to nocturnal animals but could conceivably
be related to very lengthy direct-viewing by man (Sykes, et al.,
1981). Collectively, the results of these studies suggest that
abnormally high environmental levels of retinal illumination cause
retinal degeneration for any species. This is particularly marked
in albinos (LaVail, 1980). The effects are most dramatic when the
normal, diurnal cycle of light and dark is eliminated by constant
illumination (Williams & Baker, 1980). The levels and durations of
these retinal exposures exceed those encountered during normal
human behaviour. Only rarely have investigators reported that
continual exposure to high luminance levels in the natural
environment (or work environment) has elicited significant
functional changes in the human retina (Livingston, 1932; Smith,
1944; Peckham & Harley, 1951; Medvedovskaja, 1970; Roger, 1973).
The diffraction theory can be applied to estimate the minimal
retinal image size for viewing a point source such as a laser.
However, scattering in the ocular media and corneal aberations
limits this image diameter to approximately 10 - 20 µm (Sliney,
1971).
It would be expected that, in the case of small-sized images,
the retinal hazard would increase in proportion to the area of the
pupil. Therefore, night-time viewing of a point source would be
expected to be far more dangerous than day-time viewing; however,
this is not the case, since the image blur increases with larger
pupil sizes. It is worthwhile noting that the increase in
irradiance from cornea to retina, when the relaxed eye views a
point source, is about 105 (100 000 times) (Sliney & Freasier,
1973). Almost any directly viewed laser can appear as a point
source.
8.4.1.5. Retinal pigment epithelium (RPE) absorption
As previously indicated, visible and near-infrared radiation is
transmitted through the ocular media and is absorbed principally in
the retina. The radiation passes through the neural layers of the
retina before reaching the RPE and choroid. The visual pigments in
the rods and cones absorb only a small fraction of light to
initiate the visual response, perhaps only 5% of the total energy
entering the eye. The RPE absorbs a substantial fraction of the
light (about 50% in the green) and is optically the most absorbent
layer. As the absorption takes place in a highly concentrated
layer of melanin granules approximately 3 - 6 µm thick, the greatest
temperature rise occurs in this layer (Bergquist et al., 1978;
Birngruber, 1978). The actual size, shape, distribution, and
physical characteristics of individual melanin granules become
quite important for a thermal model adequate to describe the
behaviour of this layer, during very short pulse exposures
(Wolbarsht, et al., 1980). The granules may be heated to
incandescence during Q-switched exposures, and this incandescence
can be seen, if viewed during a 1064-nm (neodymium-YAG) laser
experiment (Mueller & Ham, 1980, private communication).
8.4.2. Chorioretinal thermal injury
The retinal injury mechanism is considered to be largely
thermal for accidental exposures from arc lamps, cw lasers, or
optically aided viewing of the sun, for durations of the order of
1 ms to ~10 s. Since injury appears to result principally from
protein denaturation and enzyme inactivation, the variation in
retinal temperature during and following the insult must be
considered (Beatrice & Velez, 1975). Several efforts to develop
mathematical models for light absorption, heat flow, and the rate-
process injury mechanisms within the complex structure of the
retina have been moderately successful, over periods of exposure
lasting from 1 ms to 10 s (Vos, 1966a; Mainster et al., 1970;
Allen, 1980).
The tissue surrounding the absorption site can much more
readily conduct away the absorbed heat for images, 10 - 50 µm in
diameter, than it can for large images of the order of 1000 µm
(1 mm). Indeed, retinal injury thresholds for the same time range
of 0.1 - 10 s are very closely related to image size, as would be
expected from calculations of heat flow in the retina. For
example, exposure to irradiances of 10-100 kW/m2 (i.e., 1-10 W/cm2)
results in a minimal retinal injury threshold for a 1000-µm image,
whereas an irradiance of 10 MW/m2 (1 kW/cm2) is required to produce
the same type of threshold lesion in a 20-µm image (Ham et al.,
1970).
For short-pulse durations, the reason for the spot-size
dependence of the threshold is not clear (Frisch et al., 1971).
The expectation, when exposure durations are of the order of 1 ms,
is that injury will take place before there is significant heat
flow. Indeed, the variation of threshold with pulse duration
itself is also rather puzzling, especially the increase in
threshold for 20-ns, Q-switched pulses over those of 1-µs duration
(Hansen & Fine, 1968; Harlen, 1978; Anderson, 1980b). Obviously,
the Q-switched pulse energy is being dissipated in some mechanism
such as a mechanical displacement of tissue (an acoustic
transient), which does not contribute to the normal thermal injury
process that determines the minimum threshold.
In studies conducted by Beatrice & Lund (1979) with image
distributions that were non-circular, such as line images on the
retina, circular lesions were produced after long-term exposures.
This would be predicted by thermal injury and heat flow
calculations. Very short, Q-switched exposures with similar line
image distributions produced lesions that were very elongated, as,
again, would be predicted by a simple thermal model or injury. It
might be thought that the contribution of acoustic transients from
such a short exposure would have been to enlarge the lesion.
Photoacoustic effects should certainly make a considerable
contribution; but whether the acoustic transient adds to, or
subtracts from the injury mechanism is not yet clear.
For short-term exposures (< 1 µs) resulting from Q-switched
lasers, exploding wires, super-radiant light, and mode-locked
lasers, the exposure thresholds of injury are lowest. Although it
is believed that, for a Q-switched exposure, the injury mechanism
is largely thermal, the effect of acoustic transients due to rapid
heating and thermal expansion in the immediate vicinity of the
absorption site (individual melanin granules) may play a role. For
still shorter durations of exposure, direct electric field effects,
Raman and Brillouin scattering, and multiphoton absorption could
play a role in the damage mechanism (Greisemann & Marti, 1978;
Rockerolles, 1978).
8.4.3. Location of retinal burns
As previously explained, the different regions of the retina
play different roles in vision. Thus, the significance of
functional loss of all or part of any one of these regions, because
of retinal injury, varies. The loss of foveal vision seriously
reduces visual performance. Limited peripheral loss could be
unnoticed, subjectively (Kaufman, 1970; Holzinger et al., 1978).
8.5. Photochemical Retinal Injury
8.5.1. Very long-term exposure
The human retina is normally subjected to irradiances below
1 W/m2 (10-4 W/cm2), as shown in Fig. 19, except for occasional
momentary exposure to the sun, welding arcs, and similar bright
sources. The retinal images resulting from viewing such sources
are often quite small (for example 0.15 mm for the sun) and the
duration of exposure is normally limited to the duration of the
blink reflex (0.15 - 0.2 s). Natural aversion to bright light
usually limits further retinal exposures above 10-4 W/cm2. Until
recently, few studies of adverse retinal effects existed for the
irradiance range of 10-4-1 W/cm2. Studies in this range have
generally centred on flash blindness effects following light
exposures lasting up to 1 s.
Exposure of large areas of the retina to moderately high
luminance light of the order of 105 cd/m2 (~100 µW/cm2, i.e.,
1 W/m2 at the retina) for durations of one to several hours has
been investigated in experimental animals. Generally, the light
sources employed in these studies were fluorescent lamps. A
thermally-enhanced photochemical mechanism of injury or a
phototoxic effect appears to be most likely (Kuwabara, 1970; Noell
& Albrecht, 1971). More recently, similar fluorescent light
exposure of rhesus monkeys with dilated pupils showed that this
effect was not limited to nocturnal animals but could conceivably
be related to very lengthy direct-viewing by man (Sykes, et al.,
1981). Collectively, the results of these studies suggest that
abnormally high environmental levels of retinal illumination cause
retinal degeneration for any species. This is particularly marked
in albinos (LaVail, 1980). The effects are most dramatic when the
normal, diurnal cycle of light and dark is eliminated by constant
illumination (Williams & Baker, 1980). The levels and durations of
these retinal exposures exceed those encountered during normal
human behaviour. Only rarely have investigators reported that
continual exposure to high luminance levels in the natural
environment (or work environment) has elicited significant
functional changes in the human retina (Livingston, 1932; Smith,
1944; Peckham & Harley, 1951; Medvedovskaja, 1970; Roger, 1973).
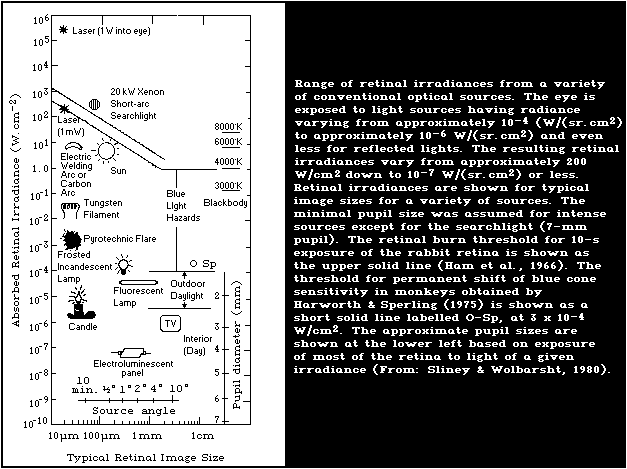 It has been shown that short-wavelength exposures are most
effective in inducing photochemical retinal injury (Ham et al.,
1976, 1978; Lawwill et al., 1977). The adverse effect is normally
centralized in the pigment layer and adjacent outer receptor layer.
Other retinal layers may be affected, but this generally follows
changes in the RPE. The effect appears first where pigment is
located.
Results of studies of photochemical retinal injury in
experimental rhesus monkeys (Ham et al., 1978; Moon et al., 1978)
agree with clinical experience reviewed by Sliney (1978) concerning
the development of eclipse-burn photoretinitis after staring at the
sun. Until recently, it was generally accepted that solar retinal
injury was permanent; however Hatfield (1970) and Penner & McNair
(1966) reported significant numbers of patients who recovered
within 30 days.
Repeated exposure of large retinal areas in trained monkeys to
incoherent light at retinal irradiances just above those
experienced in a bright natural outdoor environment, showed a
permanent decrease in functional sensitivity to blue light
(Harwerth & Sperling, 1975). Exposure of the monkeys to narrow
bands of wavelengths from the green to the red elicited a similar,
but not lasting, reaction. These types of studies, repeated by
Zwick & Beatrice (1978), showed more dramatic changes with coherent
light having a speckle pattern. Prolonged erythropsia (red vision)
in aphakics has also been reported following exposure to large-
area, high-luminance sources with large amounts of ultraviolet such
as snow fields.
Follow-up studies conducted during the 1940s showed the effects
on vision of the prolonged exposure of beach lifeguards to bright
outdoor environments. Temporary reductions in sensitivity for both
daylight and night vision lasting for periods of several days were
reported (Peckham & Harley, 1951).
There is growing concern among some investigators, who have
studied the adverse retinal effects of intense light sources, that
life-long exposure to light plays a role in retinal aging
(Marshall, 1978). Certain age-degenerative retinal effects may be
light-initiated. This opinion is prompted by the strong similarity
between histological and ultrastructural changes in aged retinae
and those in retinae exposed to intense light sources including
disorganization of the outer receptors; depigmentation of the RPE,
and a decrease in the total number of receptors. Clearly,
considerably more research will be required before this opinion can
be confirmed.
8.6. Flash Blindness
Flash blindness is a normal physiological process, being a
transitory loss of visual function. This phenomenon is a function
of the preadaptive state of the subject, the nature of the visual
task (i.e., task luminance, position in the visual field, and
acuity), and the luminance of the stimulating source. The
mechanism is complex and not fully understood, as it involves both
biochemical and neural processes. The recovery time is a measure
of the degree of flash blindness.
Flash blindness has been intensively investigated, both in
predicting functional loss that might be expected from a given
exposure and in the design of protective devices. The response
times of present-day protective devices range from a few ms down to
several µs. Even within this long delay, great difficulty has been
encountered in producing a device that can attenuate the luminance
of the source by a factor of more than 1000.
In dealing with the data on flash blindness and attempting to
relate it to retinal mechanisms, it is well to keep in mind the
ideas originally expressed by Brown (1973), who showed that
recovery from flash blindness did not involve a single, simple
mechanism. It involves both dark adaptation and neurophysiological
effects not usually seen in studies of dark adaption.
8.7. Discomfort Glare
If a very bright light source is suddenly switched on after the
eye has adapted to a luminance much lower than that of the source,
the viewer experiences discomfort, blinks, and tends to turn the
head or eyes. This effect is much more dramatic when the ambient
luminance is low. Out-of-doors, in full daylight, the luminance of
a large extended source required to elicit this phenomenon is of
the order of 100 000 cd/m2 (10 cd/cm2 or 29 000 foot-lamberts);
however, the luminance of this source must be far greater to elicit
a response, if the source subtends an angle of less than about 4.5
mrad (0.25 degree).
8.8. Flashing Lights
Classical studies of vision suggest that a strobe operating at
10 Hz can appear subjectively brighter than a cw source of the same
peak brightness, due to the Bartley Effect for flashing light
sources. Similarly, the brightness of a single pulse appears
brighter than it really is; this phenomenon is termed the Broca-
Sulzer Effect (Cornsweet, 1966).
Strobe light sources produce little annoyance during daylight
hours. However, at night, if a strobe illuminates an area that
would otherwise be dark, at a frequency of 5 - 10 Hz, the static
objects illuminated by the strobe appear to float around, because
of loss of a fixation point during off-periods of the light.
The medical literature suggests that epileptic seizures in
susceptible individuals represent the only well-documented health
hazard from exposure to low-frequency intermittent light. The most
sensitive frequency range is from 8 to l6 Hz. Various estimates
indicate that approximately 1.0% of the epileptic population, which
itself constitutes less than 1.0% of the general population, will
experience these "flicker-induced" seizures.
9. THE SKIN
9.1. Anatomy
The skin is normally of less interest than the eye as far as
optical radiation hazards are concerned. However, under certain
conditions, it may be more vulnerable than the eye, which can be
protected by the blink reflex or by eye protectors.
The outermost layer, the stratum corneum or horny layer,
consists of flattened, epidermal cells. They originate in the
germinative layer (a single cell layer of collumnar germinative
basal cells) at the bottom of the epidermis, grow, and are
gradually pushed outward until they die and are flattened to form a
protective layer over the living cells.
The stratum corneum is approximately 10 - 20 µm thick over most
parts of the body, except the soles of the feet and the palms of
the hand, where it is much thicker (500 - 600 µm).
The epidermis is relatively uniform in thickness throughout the
body (50 - 150 µm) and can be separated into a number of layers
with the growing cells in the lowest level toward the basal
membrane.
Melanocytes, specialized cells that produce melanin pigment
granules, are located in the basal layer of the epidermis. The
melanocytes send out dendritic processes that interdigitate within
the keratinocytes. Melanosomes (the pigment granules) are then
transferred into the keratinocytes. The pigment is thus
distributed throughout the epidermis and stratum corneum by
migration of the keratinocytes.
The dermis, or corium, is thicker than the epidermis, and
consists largely of connective tissue which gives the skin its
elasticity and supportive strength. The sweat glands extend into
the corium.
9.2. Body Heat Regulation
The skin plays a major role in the thermoregulatory system of
the human body. At incident irradiances less than those that cause
thermal skin burns, the body can be subjected to heat stress.
Several physical means are employed by the skin for cooling
(conductive, convective, and radiative cooling).
The sweat glands produce sweat, which permits evaporative
cooling as well as conductive cooling. The reflectance of human
skin in the far infrared is very low with a correspondingly high
emissivity for wavelengths in the 8 - 13 µm infrared region. The
high emissivity at these wavelengths permits highly efficient
radiative cooling of the skin at body temperature.
Comparison of the reflectance spectrum of the human skin with
the solar emission spectrum shows a striking similarity. The skin
reflects largely in the visible part and near-infrared parts of the
spectrum, where solar radiation is greatest, and absorbs heavily in
the ultraviolet and far infrared, where there is very little solar
radiation. Any good radiator of infrared energy (a black body)
must have very high absorption, hence very low total reflection.
The skin does indeed have low reflectance in the far infrared, and
seems well adapted to the natural environment. The skin both
reflects direct solar radiation and reradiates internally generated
infrared radiation with the greatest possible efficiency. However,
the human body is less capable of reflecting the infrared radiation
from man-made sources such as fire, or more specifically from
molten steel in a steel mill (Hardy, 1968; Sliney & Freasier, 1973;
Stolwijk, 1980).
9.3. Optical Properties
The stratum corneum strongly absorbs actinic UVR, which causes
sunburn. This layer also strongly absorbs far-infrared radiation.
Melanin granules are small (1 µm diameter) and not only protect the
dermis by absorption of UVR, but also by scattering optical
radiation. Melanin scatters rather than absorbs radiation in the
near-infrared region. For this and other reasons, near-infrared
radiation penetrates deeply into the tissue. Since the index of
refraction of the stratum corneum is about 1.5, the Fresnel
reflective component is somewhat similar to that of glass (Fig. 2).
Optical radiation incident on the skin at grazing angles of
incidence is hardly absorbed at all. The relative effectiveness of
optical radiation in penetrating the epidermis (and dermis) varies
approximately as the cosine of the angle of incidence. Since light
penetrates the outermost layers of the skin, undergoes multiple
scattering, and some light is scattered back out of the skin, the
skin has an appearance that cannot easily be duplicated by a non-
translucent surface (Anderson & Parrish, 1981).
9.4. Penetration Depth and Reflection
Studies of the effects of pulsed visible and IR laser radiation
on pig skin, performed in the 1960s, provided single-wavelength
thresholds for injury for very short-term exposures of the order of
1 ms and 20 ns. For such short durations of exposure, the
influence of heat flow from the absorbing site is not a major
factor. For this reason, these studies aptly showed that the
threshold of injury depended on the reflectance of the skin and the
depth of penetration of the optical radiation into the skin (Fig.
20).
The reflectance of the skin also plays a role in determining
how much radiation can effectively be absorbed. The skin's
spectral reflectance varies with pigmentation and is significant
only in the visible and near-infrared spectrum. The skin's
reflectance at wavelengths of less than 310 nm and above 2.5 µm is
less than 5%.
It has been shown that short-wavelength exposures are most
effective in inducing photochemical retinal injury (Ham et al.,
1976, 1978; Lawwill et al., 1977). The adverse effect is normally
centralized in the pigment layer and adjacent outer receptor layer.
Other retinal layers may be affected, but this generally follows
changes in the RPE. The effect appears first where pigment is
located.
Results of studies of photochemical retinal injury in
experimental rhesus monkeys (Ham et al., 1978; Moon et al., 1978)
agree with clinical experience reviewed by Sliney (1978) concerning
the development of eclipse-burn photoretinitis after staring at the
sun. Until recently, it was generally accepted that solar retinal
injury was permanent; however Hatfield (1970) and Penner & McNair
(1966) reported significant numbers of patients who recovered
within 30 days.
Repeated exposure of large retinal areas in trained monkeys to
incoherent light at retinal irradiances just above those
experienced in a bright natural outdoor environment, showed a
permanent decrease in functional sensitivity to blue light
(Harwerth & Sperling, 1975). Exposure of the monkeys to narrow
bands of wavelengths from the green to the red elicited a similar,
but not lasting, reaction. These types of studies, repeated by
Zwick & Beatrice (1978), showed more dramatic changes with coherent
light having a speckle pattern. Prolonged erythropsia (red vision)
in aphakics has also been reported following exposure to large-
area, high-luminance sources with large amounts of ultraviolet such
as snow fields.
Follow-up studies conducted during the 1940s showed the effects
on vision of the prolonged exposure of beach lifeguards to bright
outdoor environments. Temporary reductions in sensitivity for both
daylight and night vision lasting for periods of several days were
reported (Peckham & Harley, 1951).
There is growing concern among some investigators, who have
studied the adverse retinal effects of intense light sources, that
life-long exposure to light plays a role in retinal aging
(Marshall, 1978). Certain age-degenerative retinal effects may be
light-initiated. This opinion is prompted by the strong similarity
between histological and ultrastructural changes in aged retinae
and those in retinae exposed to intense light sources including
disorganization of the outer receptors; depigmentation of the RPE,
and a decrease in the total number of receptors. Clearly,
considerably more research will be required before this opinion can
be confirmed.
8.6. Flash Blindness
Flash blindness is a normal physiological process, being a
transitory loss of visual function. This phenomenon is a function
of the preadaptive state of the subject, the nature of the visual
task (i.e., task luminance, position in the visual field, and
acuity), and the luminance of the stimulating source. The
mechanism is complex and not fully understood, as it involves both
biochemical and neural processes. The recovery time is a measure
of the degree of flash blindness.
Flash blindness has been intensively investigated, both in
predicting functional loss that might be expected from a given
exposure and in the design of protective devices. The response
times of present-day protective devices range from a few ms down to
several µs. Even within this long delay, great difficulty has been
encountered in producing a device that can attenuate the luminance
of the source by a factor of more than 1000.
In dealing with the data on flash blindness and attempting to
relate it to retinal mechanisms, it is well to keep in mind the
ideas originally expressed by Brown (1973), who showed that
recovery from flash blindness did not involve a single, simple
mechanism. It involves both dark adaptation and neurophysiological
effects not usually seen in studies of dark adaption.
8.7. Discomfort Glare
If a very bright light source is suddenly switched on after the
eye has adapted to a luminance much lower than that of the source,
the viewer experiences discomfort, blinks, and tends to turn the
head or eyes. This effect is much more dramatic when the ambient
luminance is low. Out-of-doors, in full daylight, the luminance of
a large extended source required to elicit this phenomenon is of
the order of 100 000 cd/m2 (10 cd/cm2 or 29 000 foot-lamberts);
however, the luminance of this source must be far greater to elicit
a response, if the source subtends an angle of less than about 4.5
mrad (0.25 degree).
8.8. Flashing Lights
Classical studies of vision suggest that a strobe operating at
10 Hz can appear subjectively brighter than a cw source of the same
peak brightness, due to the Bartley Effect for flashing light
sources. Similarly, the brightness of a single pulse appears
brighter than it really is; this phenomenon is termed the Broca-
Sulzer Effect (Cornsweet, 1966).
Strobe light sources produce little annoyance during daylight
hours. However, at night, if a strobe illuminates an area that
would otherwise be dark, at a frequency of 5 - 10 Hz, the static
objects illuminated by the strobe appear to float around, because
of loss of a fixation point during off-periods of the light.
The medical literature suggests that epileptic seizures in
susceptible individuals represent the only well-documented health
hazard from exposure to low-frequency intermittent light. The most
sensitive frequency range is from 8 to l6 Hz. Various estimates
indicate that approximately 1.0% of the epileptic population, which
itself constitutes less than 1.0% of the general population, will
experience these "flicker-induced" seizures.
9. THE SKIN
9.1. Anatomy
The skin is normally of less interest than the eye as far as
optical radiation hazards are concerned. However, under certain
conditions, it may be more vulnerable than the eye, which can be
protected by the blink reflex or by eye protectors.
The outermost layer, the stratum corneum or horny layer,
consists of flattened, epidermal cells. They originate in the
germinative layer (a single cell layer of collumnar germinative
basal cells) at the bottom of the epidermis, grow, and are
gradually pushed outward until they die and are flattened to form a
protective layer over the living cells.
The stratum corneum is approximately 10 - 20 µm thick over most
parts of the body, except the soles of the feet and the palms of
the hand, where it is much thicker (500 - 600 µm).
The epidermis is relatively uniform in thickness throughout the
body (50 - 150 µm) and can be separated into a number of layers
with the growing cells in the lowest level toward the basal
membrane.
Melanocytes, specialized cells that produce melanin pigment
granules, are located in the basal layer of the epidermis. The
melanocytes send out dendritic processes that interdigitate within
the keratinocytes. Melanosomes (the pigment granules) are then
transferred into the keratinocytes. The pigment is thus
distributed throughout the epidermis and stratum corneum by
migration of the keratinocytes.
The dermis, or corium, is thicker than the epidermis, and
consists largely of connective tissue which gives the skin its
elasticity and supportive strength. The sweat glands extend into
the corium.
9.2. Body Heat Regulation
The skin plays a major role in the thermoregulatory system of
the human body. At incident irradiances less than those that cause
thermal skin burns, the body can be subjected to heat stress.
Several physical means are employed by the skin for cooling
(conductive, convective, and radiative cooling).
The sweat glands produce sweat, which permits evaporative
cooling as well as conductive cooling. The reflectance of human
skin in the far infrared is very low with a correspondingly high
emissivity for wavelengths in the 8 - 13 µm infrared region. The
high emissivity at these wavelengths permits highly efficient
radiative cooling of the skin at body temperature.
Comparison of the reflectance spectrum of the human skin with
the solar emission spectrum shows a striking similarity. The skin
reflects largely in the visible part and near-infrared parts of the
spectrum, where solar radiation is greatest, and absorbs heavily in
the ultraviolet and far infrared, where there is very little solar
radiation. Any good radiator of infrared energy (a black body)
must have very high absorption, hence very low total reflection.
The skin does indeed have low reflectance in the far infrared, and
seems well adapted to the natural environment. The skin both
reflects direct solar radiation and reradiates internally generated
infrared radiation with the greatest possible efficiency. However,
the human body is less capable of reflecting the infrared radiation
from man-made sources such as fire, or more specifically from
molten steel in a steel mill (Hardy, 1968; Sliney & Freasier, 1973;
Stolwijk, 1980).
9.3. Optical Properties
The stratum corneum strongly absorbs actinic UVR, which causes
sunburn. This layer also strongly absorbs far-infrared radiation.
Melanin granules are small (1 µm diameter) and not only protect the
dermis by absorption of UVR, but also by scattering optical
radiation. Melanin scatters rather than absorbs radiation in the
near-infrared region. For this and other reasons, near-infrared
radiation penetrates deeply into the tissue. Since the index of
refraction of the stratum corneum is about 1.5, the Fresnel
reflective component is somewhat similar to that of glass (Fig. 2).
Optical radiation incident on the skin at grazing angles of
incidence is hardly absorbed at all. The relative effectiveness of
optical radiation in penetrating the epidermis (and dermis) varies
approximately as the cosine of the angle of incidence. Since light
penetrates the outermost layers of the skin, undergoes multiple
scattering, and some light is scattered back out of the skin, the
skin has an appearance that cannot easily be duplicated by a non-
translucent surface (Anderson & Parrish, 1981).
9.4. Penetration Depth and Reflection
Studies of the effects of pulsed visible and IR laser radiation
on pig skin, performed in the 1960s, provided single-wavelength
thresholds for injury for very short-term exposures of the order of
1 ms and 20 ns. For such short durations of exposure, the
influence of heat flow from the absorbing site is not a major
factor. For this reason, these studies aptly showed that the
threshold of injury depended on the reflectance of the skin and the
depth of penetration of the optical radiation into the skin (Fig.
20).
The reflectance of the skin also plays a role in determining
how much radiation can effectively be absorbed. The skin's
spectral reflectance varies with pigmentation and is significant
only in the visible and near-infrared spectrum. The skin's
reflectance at wavelengths of less than 310 nm and above 2.5 µm is
less than 5%.
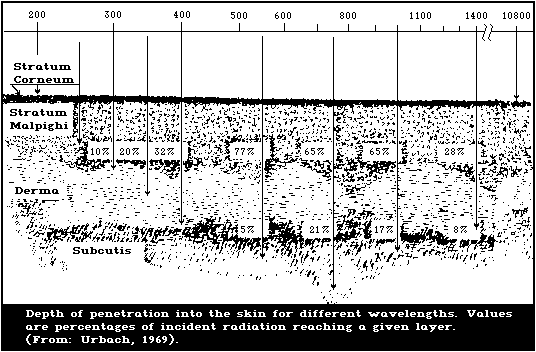 It must be remembered that small amounts of optical radiation
penetrate deeply into the body, where it may react with
photosensitive cells. This may give rise to physiological
reactions of great importance, such as circadian rhythms and annual
rhythms. Artificial constant irradiation may suppress the
circadian rhythms, giving rise to health problems.
9.4.1. Injury to the skin
Laser radiation injury to the skin is normally considered less
important than injury to the eye, despite the fact that injury
thresholds for the skin and eye are comparable, except in the
retinal hazard region (400 - 1400 nm). In the IR-C and UV-C
spectral regions, where optical radiation is not focused on the
retina, skin injury thresholds are approximately the same as
corneal injury thresholds. The probability of exposure is greater
for the skin than for the eye, because of the skin's greater
surface area, and yet injury to the eye is still considered to be
of greater significance. For a comparable area of tissue
destruction, the functional losses associated with the eye are more
debilitating than with the skin. Threshold injuries resulting from
the short-term (i.e., less than 10 s) exposure of the skin to far-
infrared (IR-C) and UV-C radiation are also very superficial and
may only involve changes to the outer dead layer - the "horny
layer" - of the skin cells. A temporary injury to the skin may be
painful, if sufficiently severe, but eventually it will heal, often
without any sign of the injury. Burns (thermal injuries) to larger
areas of skin are far more serious, as they may lead to serious
loss of body fluids, toxaemia, and systematic infections.
Thermal injury of the skin has been the subject of many studies
in this century. Hardy et al. (1956) found that severe pain could
always be induced in human skin tissue, when the tissue temperature
was elevated to 45 °C. This temperature also corresponds to an
injury threshold, if the exposure to optical radiation lasts for
many seconds.
Skin injury resulting from momentary but very intense exposures
to optical radiation are generally termed "flash burns". Flash
burns of the skin following exposure to optical radiation in
industry are rare. Most conventional sources such as open-arc
processes and industrial furnaces do not create significant
irradiances in work areas where skin injury could occur
sufficiently fast to preclude a natural protective reaction to the
intense heat. The flash burns that do occur are more often the
result of conductive heating of the skin by exceedingly hot gases
or steam. Though the eye is protected from most flash burns, the
eye lid may be injured with resulting complications in vision. The
threshold depends on the area of irradiated tissue. Heat
conduction in tissue is far more efficient for small than for
larger irradiated areas (e.g., 1 mm2) and exposure to higher levels
of irradiance would be possible before injury occurred. With
extensive irradiation, injury would occur at a far lower level of
irradiance. Hazardous exposure of large areas of skin is unlikely
to be encountered in the normal work environment, as the heat alone
from a source that could produce heat stress due to elevation of
deep body temperature, would require protective measures at lower
irradiance levels.
The threshold of injury obviously depends also on the duration
of exposure. The previously mentioned thresholds are for just one
exposure duration of 0.5 s. For exposures lasting less than 0.5 s
the irradiance required for an injury would significantly increase
as the duration of exposure decreased.
Studies of the process of thermal injury in skin show that the
longer the length of exposure, the lower the temperature required
to coagulate proteins and destroy tissue by elevated temperature.
Fig. 21 shows this time dependence of threshold for white-light,
arc-source burns (upper curve), and for far infrared laser
radiation (lower curve). The explanation for these threshold
differences lies in the fact that thermal injury depends on energy
absorbed per unit volume (or mass) to produce a critical
temperature elevation. Skin reflectance and penetration greatly
influence this absorption. Skin disorders are common and may
change the reaction of the skin to irradiation. Some disorders may
be aggravated while, in others, healing may be enhanced by optical
radiation.
It must be remembered that small amounts of optical radiation
penetrate deeply into the body, where it may react with
photosensitive cells. This may give rise to physiological
reactions of great importance, such as circadian rhythms and annual
rhythms. Artificial constant irradiation may suppress the
circadian rhythms, giving rise to health problems.
9.4.1. Injury to the skin
Laser radiation injury to the skin is normally considered less
important than injury to the eye, despite the fact that injury
thresholds for the skin and eye are comparable, except in the
retinal hazard region (400 - 1400 nm). In the IR-C and UV-C
spectral regions, where optical radiation is not focused on the
retina, skin injury thresholds are approximately the same as
corneal injury thresholds. The probability of exposure is greater
for the skin than for the eye, because of the skin's greater
surface area, and yet injury to the eye is still considered to be
of greater significance. For a comparable area of tissue
destruction, the functional losses associated with the eye are more
debilitating than with the skin. Threshold injuries resulting from
the short-term (i.e., less than 10 s) exposure of the skin to far-
infrared (IR-C) and UV-C radiation are also very superficial and
may only involve changes to the outer dead layer - the "horny
layer" - of the skin cells. A temporary injury to the skin may be
painful, if sufficiently severe, but eventually it will heal, often
without any sign of the injury. Burns (thermal injuries) to larger
areas of skin are far more serious, as they may lead to serious
loss of body fluids, toxaemia, and systematic infections.
Thermal injury of the skin has been the subject of many studies
in this century. Hardy et al. (1956) found that severe pain could
always be induced in human skin tissue, when the tissue temperature
was elevated to 45 °C. This temperature also corresponds to an
injury threshold, if the exposure to optical radiation lasts for
many seconds.
Skin injury resulting from momentary but very intense exposures
to optical radiation are generally termed "flash burns". Flash
burns of the skin following exposure to optical radiation in
industry are rare. Most conventional sources such as open-arc
processes and industrial furnaces do not create significant
irradiances in work areas where skin injury could occur
sufficiently fast to preclude a natural protective reaction to the
intense heat. The flash burns that do occur are more often the
result of conductive heating of the skin by exceedingly hot gases
or steam. Though the eye is protected from most flash burns, the
eye lid may be injured with resulting complications in vision. The
threshold depends on the area of irradiated tissue. Heat
conduction in tissue is far more efficient for small than for
larger irradiated areas (e.g., 1 mm2) and exposure to higher levels
of irradiance would be possible before injury occurred. With
extensive irradiation, injury would occur at a far lower level of
irradiance. Hazardous exposure of large areas of skin is unlikely
to be encountered in the normal work environment, as the heat alone
from a source that could produce heat stress due to elevation of
deep body temperature, would require protective measures at lower
irradiance levels.
The threshold of injury obviously depends also on the duration
of exposure. The previously mentioned thresholds are for just one
exposure duration of 0.5 s. For exposures lasting less than 0.5 s
the irradiance required for an injury would significantly increase
as the duration of exposure decreased.
Studies of the process of thermal injury in skin show that the
longer the length of exposure, the lower the temperature required
to coagulate proteins and destroy tissue by elevated temperature.
Fig. 21 shows this time dependence of threshold for white-light,
arc-source burns (upper curve), and for far infrared laser
radiation (lower curve). The explanation for these threshold
differences lies in the fact that thermal injury depends on energy
absorbed per unit volume (or mass) to produce a critical
temperature elevation. Skin reflectance and penetration greatly
influence this absorption. Skin disorders are common and may
change the reaction of the skin to irradiation. Some disorders may
be aggravated while, in others, healing may be enhanced by optical
radiation.
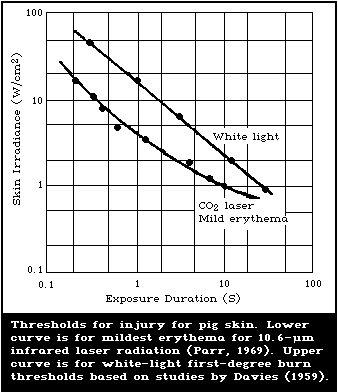 9.4.2. The sensation of warmth and heat flow
The sensation of warmth, resulting from the absorption of
radiant energy, normally provides adequate warning for avoiding
action to prevent thermal injury of the skin from almost all
sources except the nuclear fireball and some high-powered, far-
infrared lasers. The spot size dependence of this sensation is
illustrated by irradiating human skin with a beam of CO2-laser
radiation at 10.6 µm. An irradiance of 0.1 W/cm2 produces a
definite sensation of warmth for beam diameters larger than 1 cm.
On the other hand, one-tenth this level (0.01 W/cm2) can readily be
sensed, if the whole body or a larger portion of the body is
exposed. The dependence on the size of the irradiated area results
from conduction of heat away from the absorbing area, thus limitng
surface temperature rise, the sensation of heat being a function
of temperature rise. As noted previously, the skin temperature
elevation required to elicit persistent pain (as well as thermal
injury after several s) is approximately 45 °C (Hardy et al., 1956;
Hardy, 1968).
9.4.3. Thermal injury threshold for the skin
Fig. 22 presents data reported by Rockwell & Goldman (1974),
which illustrate that for some wavelengths, the threshold depends
on skin pigmentation. In the far-infrared, however, all tissue
absorbs heavily, not just melanin pigment granules.
9.4.2. The sensation of warmth and heat flow
The sensation of warmth, resulting from the absorption of
radiant energy, normally provides adequate warning for avoiding
action to prevent thermal injury of the skin from almost all
sources except the nuclear fireball and some high-powered, far-
infrared lasers. The spot size dependence of this sensation is
illustrated by irradiating human skin with a beam of CO2-laser
radiation at 10.6 µm. An irradiance of 0.1 W/cm2 produces a
definite sensation of warmth for beam diameters larger than 1 cm.
On the other hand, one-tenth this level (0.01 W/cm2) can readily be
sensed, if the whole body or a larger portion of the body is
exposed. The dependence on the size of the irradiated area results
from conduction of heat away from the absorbing area, thus limitng
surface temperature rise, the sensation of heat being a function
of temperature rise. As noted previously, the skin temperature
elevation required to elicit persistent pain (as well as thermal
injury after several s) is approximately 45 °C (Hardy et al., 1956;
Hardy, 1968).
9.4.3. Thermal injury threshold for the skin
Fig. 22 presents data reported by Rockwell & Goldman (1974),
which illustrate that for some wavelengths, the threshold depends
on skin pigmentation. In the far-infrared, however, all tissue
absorbs heavily, not just melanin pigment granules.
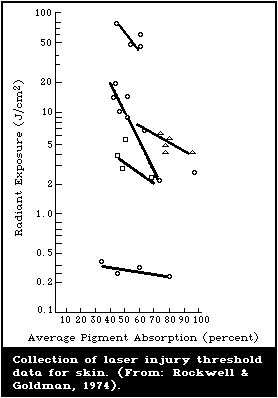 9.4.4. Delayed effects
The possibility of adverse effects from repeated or long-term
laser irradiation of the skin is normally discounted, if scarring
does not occur (Goldman et al., 1971). Only UVR has been shown to
cause long-term, delayed effects. These effects are accelerated
skin aging and skin cancer. It is difficult to quantitatively
evaluate the role of UVR in the induction of skin cancer. For
solar radiation, the high-risk wavelengths are around 310 nm. Some
attempts to calculate the dose-effect relationship have now been
made (de Gruijl & van der Leun, 1980). At present, laser safety
standards for exposure of the skin do attempt to take into account
all of these adverse effects.
9.4.5. Ambient environment and heat stress
The temperature of the ambient environment can play a role in
adding to or subtracting from, the temperature rise through
continuous exposure of the skin to optical radiation, particularly
if full-profile exposure is possible. Though full-profile exposure
to laser radiation is uncommon, it is not impossible. Just as
full-profile exposure to far-infrared radiation from furnaces can
cause heat stress, so also can exposure to far-infrared laser
radiation. Radiant absorption is, however, only one factor in
defining heat stress (WHO Scientific Group ..., 1969; Stolwijk,
1980). Increased body temperature due to fever or other causes
generally lowers the irradiance threshold of the effects of optical
radiation.
Man in his natural environment is already exposed to
significant optical radiation out-of-doors. The sun's irradiance
on a clear day may vary from 0.5 to 1.1 kW/m2 (50 to 110 mW/cm2) at
midday. The human body is well designed to reflect direct solar
radiation. In the far-infrared region of the spectrum, the skin's
low reflectance and high emissivity make it possible for the body
to both radiate and strongly absorb 10-µm radiation. The ambient
radiant exitance of surrounding structures and the ground may vary
from 10 to 400 W/m2 (1 to 40 mW/cm2).
9.4.6. UVR effects on the skin
UVR gives rise to acute and delayed visible effects. The acute
effects are erythema (skin reddening), thickening of the stratum
corneum and pigmentation through melanogenesis (Van der Leun,
1965). The delayed effects are accelerated skin aging and
carcinogenesis (Urbach, 1980).
Threshold levels for the acute effects from UV-A are generally
of the order of 1000 times greater than those of UV-B or UV-C. The
effects depend, to a large extent, on skin pigmentation at the time
of exposure. These subjects have been dealt with in detail in the
WHO Environmental Health Criteria document on ultraviolet radiation
(WHO, 1980).
9.4.7. Photosensitization
Light-induced damage to the skin in the presence of certain
chemicals (photosensitizers) may be considered phototoxic if an
allergic mechanism is not ivolved. It can occur in any type of
skin exposed to UVR of the proper wavelength and looks like a
normal erythema. In some cases the reaction may be delayed, but in
general it will appear immediately after exposure. A number of
systemic photosensitizers have been identified and examples are
given in Table 6.
9.4.8. Photoallergy
Photoallergy is an acquired altered capacity of the skin to
react to light (and UVR) alone or in the presence of a
photosensitizer. This subject has been treated in detail in WHO
(1979).
Table 6. Systemic photosensitizers: Chemicals that induce
photosensitivitya
-------------------------------------------------------------------
Uses Name
-------------------------------------------------------------------
Antibacterial nalidixic acid
Anticonvulsant carbamazepine
Antimycotic griseofulvin
-------------------------------------------------------------------
Table 6. (contd.)
-------------------------------------------------------------------
Uses Name
-------------------------------------------------------------------
Artificial sweeteners cyclamates, calcium
cyclamate sodium
cyclohexylsulfamate
Broad spectrum antibiotic antibiotics
Chemotherapeutic, antibacterial sulfonamides
Diuretics, antihypertensive chlorthiazides
Hypoglycaemic or antidiabetic drugs sulfonylurea
In vitiligo for sun tolerance furocoumarins
and increased pigment formation
Laxative triacetyldiphenolisatin
Oral contraceptives estrogens and progesterones
Tranquillizer, nematode infestation phenothiazines
control urinary antiseptic,
antihistamine
Tranquilizer, psychotropic chlordiazepoxide
-------------------------------------------------------------------
a Adapted from: Fitzpatrick et al. (1974).
10. LASER SAFETY STANDARDS: RATIONALE AND CURRENT STANDARDS
10.1. Introduction
Laser safety standards may take several forms. The standard
may be simply a list of guidelines concerning laser operation or
equipment design with no mention of exposure limits or a list of
personnel exposure limits (ELs) or product emission limits. Today,
most safety standards incorporate all of these aspects, to some
extent. This section explains the scientific and philosophical
problems encountered in the development of today's standards. The
distinction between occupational exposure standards and equipment
performance standards will also be discussed.
Exposure limits may be applied in three general categories of
standards, i.e., occupational safety and health standards,
environmental quality standards and equipment performance
standards. ELs for laser radiation for general population and
occupational exposure were developed in many countries during the
late 1960s and throughout the 1970s. A general consensus for many
of these limits can be found in the 1982 draft international
standard of the International Electrotechnical Commission (IEC, in
preparation).
10.2. Laser Hazard Classification
It was recognized during the early development of laser safety
standards that some form of risk classification was necessary.
This resulted from many complaints from research scientists in the
1960s that they were being needlessly constrained in their use of
small He-Ne lasers by safety specialists, who were attempting to
apply guidelines originally drafted for high-power ruby and
neodymium lasers.
Most recent laser safety standards therefore include a hazard
classification scheme to simplify risk evaluation on which to base
control measures (Harlen, 1978).
The safety procedures necessary for any laser operation vary
according to three aspects: (a) the laser hazard classification;
(b) the environment in which the laser is to used, and (c) the
people operating or within the vicinity of the laser beam. Hazard
classification schemes differ only slightly, depending on which
standard is being followed; and a brief explanation of the most
commonly used hazard classification system follows.
Class 1 lasers are the lowest powered lasers. This group is
normally limited to certain gallium-arsenide lasers or enclosed
lasers. These lasers are not considered hazardous, even if the
output laser beam can be collected by 80-mm collecting optics and
concentrated into the pupil of the eye. An infrared or ultraviolet
laser is Class 1 if the radiation concentrated on the skin or eye
will not cause injury within the maximum exposure duration possible
during one day of laser operation. Most lasers are not Class 1,
however, when they are incorporated into consumer or office machine
equipment, the resulting system may become Class 1. If a Class 1
system contains a more dangerous laser, the access panel to it must
be interlocked or contain a warning to alert the user of the
hazardous laser radiation that may be encountered, when the panel
is removed.
Class 2 lasers, often termed "low-power" or "low-risk" laser
systems, are those that are only hazardous if the viewer overcomes
the natural aversion response to bright light and stares
continuously into the source - an unlikely event. This could just
as readily occur by forcing oneself to stare at the sun for more
than a minute or to stare into a film projector source for several
minutes. This hazard, though rare, is as real as eclipse
blindness, hence Class 2 lasers should have a caution label affixed
to indicate that purposeful staring into the laser should be
avoided. Since the aversion response only occurs for light, the
Class 2 category is limited to the visible spectrum from 400 to
700 nm.
Class 3 "moderate-risk" or "medium-power" laser systems are
those that can cause eye injury within the natural aversion
response time, i.e., during the blink reflex (0.25 s). Class 3
lasers do not cause serious skin injury or hazardous diffuse
reflections under normal use. However, these must have danger
labels and the safety precautions required are often considerable.
Class 4 laser systems are the highest powered lasers and
present the greatest potential for injury or combustion of
flammable materials. They may also cause diffuse reflections that
are hazardous to view or induce serious skin injury from direct
exposure. More restrictive control measures and additional
warnings are necessary (Clevet & Mayer, 1980).
Fig. 23 summarizes the most typical classification
scheme. Some standards further refine the above
classification scheme to include special subclasses referred
to as Class 2a, Class 3a, and Class 4a. Relaxed restrictions
may apply to these subclasses.
9.4.4. Delayed effects
The possibility of adverse effects from repeated or long-term
laser irradiation of the skin is normally discounted, if scarring
does not occur (Goldman et al., 1971). Only UVR has been shown to
cause long-term, delayed effects. These effects are accelerated
skin aging and skin cancer. It is difficult to quantitatively
evaluate the role of UVR in the induction of skin cancer. For
solar radiation, the high-risk wavelengths are around 310 nm. Some
attempts to calculate the dose-effect relationship have now been
made (de Gruijl & van der Leun, 1980). At present, laser safety
standards for exposure of the skin do attempt to take into account
all of these adverse effects.
9.4.5. Ambient environment and heat stress
The temperature of the ambient environment can play a role in
adding to or subtracting from, the temperature rise through
continuous exposure of the skin to optical radiation, particularly
if full-profile exposure is possible. Though full-profile exposure
to laser radiation is uncommon, it is not impossible. Just as
full-profile exposure to far-infrared radiation from furnaces can
cause heat stress, so also can exposure to far-infrared laser
radiation. Radiant absorption is, however, only one factor in
defining heat stress (WHO Scientific Group ..., 1969; Stolwijk,
1980). Increased body temperature due to fever or other causes
generally lowers the irradiance threshold of the effects of optical
radiation.
Man in his natural environment is already exposed to
significant optical radiation out-of-doors. The sun's irradiance
on a clear day may vary from 0.5 to 1.1 kW/m2 (50 to 110 mW/cm2) at
midday. The human body is well designed to reflect direct solar
radiation. In the far-infrared region of the spectrum, the skin's
low reflectance and high emissivity make it possible for the body
to both radiate and strongly absorb 10-µm radiation. The ambient
radiant exitance of surrounding structures and the ground may vary
from 10 to 400 W/m2 (1 to 40 mW/cm2).
9.4.6. UVR effects on the skin
UVR gives rise to acute and delayed visible effects. The acute
effects are erythema (skin reddening), thickening of the stratum
corneum and pigmentation through melanogenesis (Van der Leun,
1965). The delayed effects are accelerated skin aging and
carcinogenesis (Urbach, 1980).
Threshold levels for the acute effects from UV-A are generally
of the order of 1000 times greater than those of UV-B or UV-C. The
effects depend, to a large extent, on skin pigmentation at the time
of exposure. These subjects have been dealt with in detail in the
WHO Environmental Health Criteria document on ultraviolet radiation
(WHO, 1980).
9.4.7. Photosensitization
Light-induced damage to the skin in the presence of certain
chemicals (photosensitizers) may be considered phototoxic if an
allergic mechanism is not ivolved. It can occur in any type of
skin exposed to UVR of the proper wavelength and looks like a
normal erythema. In some cases the reaction may be delayed, but in
general it will appear immediately after exposure. A number of
systemic photosensitizers have been identified and examples are
given in Table 6.
9.4.8. Photoallergy
Photoallergy is an acquired altered capacity of the skin to
react to light (and UVR) alone or in the presence of a
photosensitizer. This subject has been treated in detail in WHO
(1979).
Table 6. Systemic photosensitizers: Chemicals that induce
photosensitivitya
-------------------------------------------------------------------
Uses Name
-------------------------------------------------------------------
Antibacterial nalidixic acid
Anticonvulsant carbamazepine
Antimycotic griseofulvin
-------------------------------------------------------------------
Table 6. (contd.)
-------------------------------------------------------------------
Uses Name
-------------------------------------------------------------------
Artificial sweeteners cyclamates, calcium
cyclamate sodium
cyclohexylsulfamate
Broad spectrum antibiotic antibiotics
Chemotherapeutic, antibacterial sulfonamides
Diuretics, antihypertensive chlorthiazides
Hypoglycaemic or antidiabetic drugs sulfonylurea
In vitiligo for sun tolerance furocoumarins
and increased pigment formation
Laxative triacetyldiphenolisatin
Oral contraceptives estrogens and progesterones
Tranquillizer, nematode infestation phenothiazines
control urinary antiseptic,
antihistamine
Tranquilizer, psychotropic chlordiazepoxide
-------------------------------------------------------------------
a Adapted from: Fitzpatrick et al. (1974).
10. LASER SAFETY STANDARDS: RATIONALE AND CURRENT STANDARDS
10.1. Introduction
Laser safety standards may take several forms. The standard
may be simply a list of guidelines concerning laser operation or
equipment design with no mention of exposure limits or a list of
personnel exposure limits (ELs) or product emission limits. Today,
most safety standards incorporate all of these aspects, to some
extent. This section explains the scientific and philosophical
problems encountered in the development of today's standards. The
distinction between occupational exposure standards and equipment
performance standards will also be discussed.
Exposure limits may be applied in three general categories of
standards, i.e., occupational safety and health standards,
environmental quality standards and equipment performance
standards. ELs for laser radiation for general population and
occupational exposure were developed in many countries during the
late 1960s and throughout the 1970s. A general consensus for many
of these limits can be found in the 1982 draft international
standard of the International Electrotechnical Commission (IEC, in
preparation).
10.2. Laser Hazard Classification
It was recognized during the early development of laser safety
standards that some form of risk classification was necessary.
This resulted from many complaints from research scientists in the
1960s that they were being needlessly constrained in their use of
small He-Ne lasers by safety specialists, who were attempting to
apply guidelines originally drafted for high-power ruby and
neodymium lasers.
Most recent laser safety standards therefore include a hazard
classification scheme to simplify risk evaluation on which to base
control measures (Harlen, 1978).
The safety procedures necessary for any laser operation vary
according to three aspects: (a) the laser hazard classification;
(b) the environment in which the laser is to used, and (c) the
people operating or within the vicinity of the laser beam. Hazard
classification schemes differ only slightly, depending on which
standard is being followed; and a brief explanation of the most
commonly used hazard classification system follows.
Class 1 lasers are the lowest powered lasers. This group is
normally limited to certain gallium-arsenide lasers or enclosed
lasers. These lasers are not considered hazardous, even if the
output laser beam can be collected by 80-mm collecting optics and
concentrated into the pupil of the eye. An infrared or ultraviolet
laser is Class 1 if the radiation concentrated on the skin or eye
will not cause injury within the maximum exposure duration possible
during one day of laser operation. Most lasers are not Class 1,
however, when they are incorporated into consumer or office machine
equipment, the resulting system may become Class 1. If a Class 1
system contains a more dangerous laser, the access panel to it must
be interlocked or contain a warning to alert the user of the
hazardous laser radiation that may be encountered, when the panel
is removed.
Class 2 lasers, often termed "low-power" or "low-risk" laser
systems, are those that are only hazardous if the viewer overcomes
the natural aversion response to bright light and stares
continuously into the source - an unlikely event. This could just
as readily occur by forcing oneself to stare at the sun for more
than a minute or to stare into a film projector source for several
minutes. This hazard, though rare, is as real as eclipse
blindness, hence Class 2 lasers should have a caution label affixed
to indicate that purposeful staring into the laser should be
avoided. Since the aversion response only occurs for light, the
Class 2 category is limited to the visible spectrum from 400 to
700 nm.
Class 3 "moderate-risk" or "medium-power" laser systems are
those that can cause eye injury within the natural aversion
response time, i.e., during the blink reflex (0.25 s). Class 3
lasers do not cause serious skin injury or hazardous diffuse
reflections under normal use. However, these must have danger
labels and the safety precautions required are often considerable.
Class 4 laser systems are the highest powered lasers and
present the greatest potential for injury or combustion of
flammable materials. They may also cause diffuse reflections that
are hazardous to view or induce serious skin injury from direct
exposure. More restrictive control measures and additional
warnings are necessary (Clevet & Mayer, 1980).
Fig. 23 summarizes the most typical classification
scheme. Some standards further refine the above
classification scheme to include special subclasses referred
to as Class 2a, Class 3a, and Class 4a. Relaxed restrictions
may apply to these subclasses.
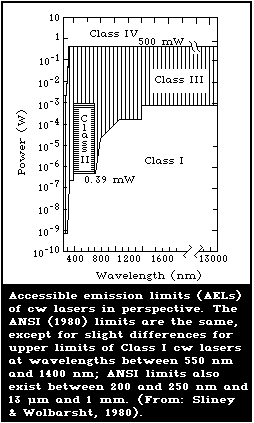 11. EXPOSURE LIMITS
11.1. Rationale
Exposure limits for lasers and optical radiation cover a wide
range of wavelengths and exposure conditions, and biological
effects may apply to both the eye and skin. For this reason, no
single rationale can apply to all of the specific ELs. It is first
important to distinguish between acute and chronic (or delayed)
effects. For acute effects, thresholds exist and statistical
(probit analysis) techniques can indicate this threshold with a
degree of uncertainty. The method of assessing the acute effect
may not always be the most sensitive, but is often chosen for
reasons of simplicity and repeatability. However, this approach is
feasible only because the relationship between this assessment
threshold and the onset of irreversible damage is known from more
rigorous studies using the most sensitive techniques for damage
assessment. While a threshold for most chronic effects can be
expected on theoretical grounds, this threshold can best be
estimated from careful evaluation of epidemiological data. ELs are
set by considering both types of effects and the degree of
uncertainty in thresholds.
Scientists working in the field of ionizing radiation are used
to the problems of cumulative doses and total lifetime exposure.
In describing the adverse biological effects of optical radiation
at wavelengths greater than 320 nm, few scientists would argue that
a linear hypothesis applies with total integration of the lifetime
exposure.
Optical radiation is usually absorbed in a thin layer of tissue
and its effects are thermal in nature, except for the ultraviolet
and visible photochemical processes. For both of these acute
effects, there is a definite threshold; that is, an exposure level
exists below which no adverse change will occur and no real risk
exists. Of course, the threshold can vary with the individual and
with environmental conditions. However, if the safety level is set
well below these variations, then the exposure conditions are not
hazardous.
To establish a rationale for developing exposure limits from
the biological data requires careful analysis of the spread of the
empirical data. These include the variables influencing potential
for injury in exposed individuals, the increase in severity of
injury for suprathreshold exposure doses, and the degree of repair
of injury.
The accuracy of available measuring instruments and the desire
for simplicity in expressing the limits have also influenced the
exposure limits. It is difficult to inter-relate all these
factors; however, most specialists agree on the final limits, even
though they may have derived them in different ways.
Separate high risk occupational limits - in contrast to
exposure limits for the general population - have not been
developed. Unlike ionizing radiation, there has been little debate
as to whether a threshold of injury actually exists. However,
there can be a debate concerning the exact "threshold values" for
specific wavelengths and exposure durations. UV-B and UV-C laser
radiation could, in theory, have delayed effects with no real
threshold, but has nevertheless been treated like longer wavelength
laser radiation. Long-term effects of low-level exposure have been
indicted as a possible contributing agents in senile degenerative
processes in the retina (Marshall, 1978; Young, 1981). If true, a
simple threshold for these effects probably does not exist.
11.2. Assessment of the "Safety Factor"
It is very difficult to decide on the margin that should be
introduced, to account for individual variation in experimental
error, in deriving the ELs. This margin is sometimes loosely
termed the safety factor; however, this is not correct. The
threshold of injury is actually the result of considering the
probit analysis of many data points.
The most reliable statistical method for describing any
biological threshold is probit analysis. One point on the curve,
the 50% damage probability, is often assigned a special
significance. This point is known as the ED50 and is the exposure
dose required, for example, to produce an ophthalmoscopically
visible (or an otherwise measurable) lesion in 50% of the exposures
in a group of animals or in a single animal, where several
exposures have taken place. The ED50 point has in the past been
termed a threshold point by some investigators, though clearly the
use of the term threshold in describing a 50% probability of injury
seems rather inappropriate. In toxicological studies of the
effects of chemicals on biological systems, the term threshold has
often been used to define a 10% probability of a biological
response.
Probit analysis is a powerful tool in determining safety
information but was not originally applied, e.g., to retinal damage
from laser exposure. In the early studies on retinal damage, the
experimental design was usually such as to facilitate calculations
of only the ED50 point.
When the data are plotted on probit paper, a line results that
can easily be extrapolated to the clinical damage probability.
Indeed, studies should be designed to give the slope with maximum
precision. For this, two points at low and high probability, e.g.,
the 20% and 80% probability points are more important than the ED50
point. Once this information is available together with the
criterion for injury and the accepted degree of safety, it is
possible to determine the exposure limit. Present-day laser ELs
are typically a factor of 5 - 20 below an ED50 for observable acute
injury, this ratio varying as a result of functional-loss,
histological, and suprathreshold-severity studies.
11.3. Environmental Considerations
Though laboratory studies of the adverse effects of optical
radiation provide the basic insight into thresholds, locations, and
mechanisms of tissue injury, it is difficult to extrapolate these
findings to protection standards. Of special importance, is the
separation of acute temporary effects from those leading to delayed
permanent detrimental effects.
In this regard, it will also be necessary to take the actual
exposure conditions of man into consideration - both from natural
environmental sources or from artificial sources. It must be
remembered, for instance, that terrestrial solar radiation changes,
both in total irradiance and in spectral distribution, throughout
the day. Furthermore, the direction of illumination is of great
importance because of the reflection from the cornea, as seen in
Fig. 24.
11. EXPOSURE LIMITS
11.1. Rationale
Exposure limits for lasers and optical radiation cover a wide
range of wavelengths and exposure conditions, and biological
effects may apply to both the eye and skin. For this reason, no
single rationale can apply to all of the specific ELs. It is first
important to distinguish between acute and chronic (or delayed)
effects. For acute effects, thresholds exist and statistical
(probit analysis) techniques can indicate this threshold with a
degree of uncertainty. The method of assessing the acute effect
may not always be the most sensitive, but is often chosen for
reasons of simplicity and repeatability. However, this approach is
feasible only because the relationship between this assessment
threshold and the onset of irreversible damage is known from more
rigorous studies using the most sensitive techniques for damage
assessment. While a threshold for most chronic effects can be
expected on theoretical grounds, this threshold can best be
estimated from careful evaluation of epidemiological data. ELs are
set by considering both types of effects and the degree of
uncertainty in thresholds.
Scientists working in the field of ionizing radiation are used
to the problems of cumulative doses and total lifetime exposure.
In describing the adverse biological effects of optical radiation
at wavelengths greater than 320 nm, few scientists would argue that
a linear hypothesis applies with total integration of the lifetime
exposure.
Optical radiation is usually absorbed in a thin layer of tissue
and its effects are thermal in nature, except for the ultraviolet
and visible photochemical processes. For both of these acute
effects, there is a definite threshold; that is, an exposure level
exists below which no adverse change will occur and no real risk
exists. Of course, the threshold can vary with the individual and
with environmental conditions. However, if the safety level is set
well below these variations, then the exposure conditions are not
hazardous.
To establish a rationale for developing exposure limits from
the biological data requires careful analysis of the spread of the
empirical data. These include the variables influencing potential
for injury in exposed individuals, the increase in severity of
injury for suprathreshold exposure doses, and the degree of repair
of injury.
The accuracy of available measuring instruments and the desire
for simplicity in expressing the limits have also influenced the
exposure limits. It is difficult to inter-relate all these
factors; however, most specialists agree on the final limits, even
though they may have derived them in different ways.
Separate high risk occupational limits - in contrast to
exposure limits for the general population - have not been
developed. Unlike ionizing radiation, there has been little debate
as to whether a threshold of injury actually exists. However,
there can be a debate concerning the exact "threshold values" for
specific wavelengths and exposure durations. UV-B and UV-C laser
radiation could, in theory, have delayed effects with no real
threshold, but has nevertheless been treated like longer wavelength
laser radiation. Long-term effects of low-level exposure have been
indicted as a possible contributing agents in senile degenerative
processes in the retina (Marshall, 1978; Young, 1981). If true, a
simple threshold for these effects probably does not exist.
11.2. Assessment of the "Safety Factor"
It is very difficult to decide on the margin that should be
introduced, to account for individual variation in experimental
error, in deriving the ELs. This margin is sometimes loosely
termed the safety factor; however, this is not correct. The
threshold of injury is actually the result of considering the
probit analysis of many data points.
The most reliable statistical method for describing any
biological threshold is probit analysis. One point on the curve,
the 50% damage probability, is often assigned a special
significance. This point is known as the ED50 and is the exposure
dose required, for example, to produce an ophthalmoscopically
visible (or an otherwise measurable) lesion in 50% of the exposures
in a group of animals or in a single animal, where several
exposures have taken place. The ED50 point has in the past been
termed a threshold point by some investigators, though clearly the
use of the term threshold in describing a 50% probability of injury
seems rather inappropriate. In toxicological studies of the
effects of chemicals on biological systems, the term threshold has
often been used to define a 10% probability of a biological
response.
Probit analysis is a powerful tool in determining safety
information but was not originally applied, e.g., to retinal damage
from laser exposure. In the early studies on retinal damage, the
experimental design was usually such as to facilitate calculations
of only the ED50 point.
When the data are plotted on probit paper, a line results that
can easily be extrapolated to the clinical damage probability.
Indeed, studies should be designed to give the slope with maximum
precision. For this, two points at low and high probability, e.g.,
the 20% and 80% probability points are more important than the ED50
point. Once this information is available together with the
criterion for injury and the accepted degree of safety, it is
possible to determine the exposure limit. Present-day laser ELs
are typically a factor of 5 - 20 below an ED50 for observable acute
injury, this ratio varying as a result of functional-loss,
histological, and suprathreshold-severity studies.
11.3. Environmental Considerations
Though laboratory studies of the adverse effects of optical
radiation provide the basic insight into thresholds, locations, and
mechanisms of tissue injury, it is difficult to extrapolate these
findings to protection standards. Of special importance, is the
separation of acute temporary effects from those leading to delayed
permanent detrimental effects.
In this regard, it will also be necessary to take the actual
exposure conditions of man into consideration - both from natural
environmental sources or from artificial sources. It must be
remembered, for instance, that terrestrial solar radiation changes,
both in total irradiance and in spectral distribution, throughout
the day. Furthermore, the direction of illumination is of great
importance because of the reflection from the cornea, as seen in
Fig. 24.
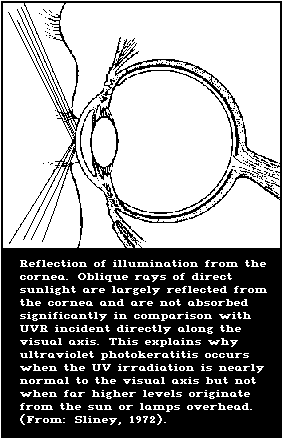 11.4. Limiting Apertures
One difficulty in developing ELs is the specification of the
limiting aperture over which the values must be either measured or
calculated. For the skin, where no self-focusing effect takes
place, the smallest feasible aperture is most desirable.
Unfortunately, the smaller the aperture, the higher the sensitivity
required for the measuring instrument and the greater the
inaccuracy that will result from calibration problems associated
with diffraction and other optical effects. Since various
biological effects are influenced differently by the size of an
incident beam, the limiting aperture varies for different
conditions.
11.4.1. The 1-mm aperture
A 1-mm aperture has been typically considered the smallest
practical aperture size for specifying ELs. Under continuous
exposure conditions, heat flow and scattering within the layers of
the skin tend to eliminate any adverse effects from hot spots
smaller than 1 mm in diameter.
11.4.2. The 11-mm aperture
Wavelengths greater than 0.1 mm present a further difficulty.
At these far-infrared, submillimetre wavelengths, a 1-mm aperture
creates significant diffraction effects and calibration becomes a
problem. Hot spots predicted by physical optics are larger than at
shorter wavelengths. For these reasons, a 1-cm square, or 11-mm
diameter (1 cm2) circular aperture has typically been chosen as the
limiting aperture for wavelengths between 0.1 mm and 1 mm.
11.4.3. The 7-mm aperture
For ocular ELs in the "retinal hazard region", from
approximately 400 nm to 1400 nm, the averaging (sampling) aperture
is determined by the pupil of the eye. A pupil size of 7-mm has
been decided as typical, though not without a great deal of debate.
11.4.4. The 80-mm aperture
A still larger measuring aperture of 80 mm is conventionally
used for power and energy measurements to account for intrabeam
viewing conditions with optical telescopes or binoculars.
11.5. Spectral Dependence of Exposure Limits
Eye and skin injury thresholds vary considerably with
wavelength. To establish the spectral dependence of ELs, it is
generally accepted that the biological data can only be followed
approximately. The ELs have been adjusted for variation in
wavelength, but do not precisely follow the empirical biological
data. Fig. 25 shows an example of theoretical variation of
susceptibility modified to provide a spectral correction factor,
useful for calculating the EL.
Fig. 25 provides the reciprocal of the product of the relative
spectral transmission of the ocular media with the retinal
absorption (Fig. 17). This indicates the relative effectiveness of
different wavelengths for causing retinal thermal injury. However,
this curve still does not show the relative spectral hazard to the
lens of the eye in the near infrared. Also plotted in this graph
is the spectral modification factor used for pulsed retinal
exposure limits in the American National Standards Institute
standard (ANSI, 1980). This modification factor is used for other
limits for protection against thermal injury. Because of variation
of threshold with image size and variation of image size with
wavelength, a further increase in the ratio between IR-A and
visible ELs is given in the ANSI Z-136.1 standard for IR-A
wavelengths between 1050 nm and 1400 nm, but only for durations of
exposure of less than 0.05 ms.
11.4. Limiting Apertures
One difficulty in developing ELs is the specification of the
limiting aperture over which the values must be either measured or
calculated. For the skin, where no self-focusing effect takes
place, the smallest feasible aperture is most desirable.
Unfortunately, the smaller the aperture, the higher the sensitivity
required for the measuring instrument and the greater the
inaccuracy that will result from calibration problems associated
with diffraction and other optical effects. Since various
biological effects are influenced differently by the size of an
incident beam, the limiting aperture varies for different
conditions.
11.4.1. The 1-mm aperture
A 1-mm aperture has been typically considered the smallest
practical aperture size for specifying ELs. Under continuous
exposure conditions, heat flow and scattering within the layers of
the skin tend to eliminate any adverse effects from hot spots
smaller than 1 mm in diameter.
11.4.2. The 11-mm aperture
Wavelengths greater than 0.1 mm present a further difficulty.
At these far-infrared, submillimetre wavelengths, a 1-mm aperture
creates significant diffraction effects and calibration becomes a
problem. Hot spots predicted by physical optics are larger than at
shorter wavelengths. For these reasons, a 1-cm square, or 11-mm
diameter (1 cm2) circular aperture has typically been chosen as the
limiting aperture for wavelengths between 0.1 mm and 1 mm.
11.4.3. The 7-mm aperture
For ocular ELs in the "retinal hazard region", from
approximately 400 nm to 1400 nm, the averaging (sampling) aperture
is determined by the pupil of the eye. A pupil size of 7-mm has
been decided as typical, though not without a great deal of debate.
11.4.4. The 80-mm aperture
A still larger measuring aperture of 80 mm is conventionally
used for power and energy measurements to account for intrabeam
viewing conditions with optical telescopes or binoculars.
11.5. Spectral Dependence of Exposure Limits
Eye and skin injury thresholds vary considerably with
wavelength. To establish the spectral dependence of ELs, it is
generally accepted that the biological data can only be followed
approximately. The ELs have been adjusted for variation in
wavelength, but do not precisely follow the empirical biological
data. Fig. 25 shows an example of theoretical variation of
susceptibility modified to provide a spectral correction factor,
useful for calculating the EL.
Fig. 25 provides the reciprocal of the product of the relative
spectral transmission of the ocular media with the retinal
absorption (Fig. 17). This indicates the relative effectiveness of
different wavelengths for causing retinal thermal injury. However,
this curve still does not show the relative spectral hazard to the
lens of the eye in the near infrared. Also plotted in this graph
is the spectral modification factor used for pulsed retinal
exposure limits in the American National Standards Institute
standard (ANSI, 1980). This modification factor is used for other
limits for protection against thermal injury. Because of variation
of threshold with image size and variation of image size with
wavelength, a further increase in the ratio between IR-A and
visible ELs is given in the ANSI Z-136.1 standard for IR-A
wavelengths between 1050 nm and 1400 nm, but only for durations of
exposure of less than 0.05 ms.
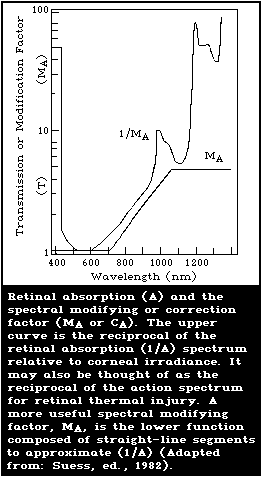 11.6. Repetitively Pulsed Laser Exposure
The values in the present standards for repetitive ocular
exposure have been based on limited data and developed from purely
empirical extrapolations. The cumulative effect of repetitive
pulses was considered to be a function of the duration of the
individual pulse in a pulse train. For short pulses (duration less
than 10 µs), the EL for a single pulse was multiplied by a
correction factor to provide a reduced exposure on a per-pulse
basis. This value was then compared with the EL values for the
total energy and for a total exposure of the duration of the entire
train of exposures, to determine which limit would apply. For a
train of pulses, where the individual pulse duration exceeded 10
ms, a criterion based on total on-time Tt of the train of pulses
was applied to each individual pulse. This resulted in a reduced
EL for each pulse. However, all of these approaches were based
largely on studies in which the eye of the rhesus monkey was
exposed to single pulses of "minimal image size".
More recent studies (Greiss et al., 1980) suggest that the
pulse thresholds add as a function of N-¨ for small image sizes,
but not for large image sizes. The letter N refers to the number
of pulses in the train.
11.7. Restrictions for Special Applications (Class 3a)
The low risk of Class 2 lasers differs little from the lack of
risk of Class 1 lasers, in practice. Class 2 lasers emit a power
of 0.4 µW - 1 mW, a light level difficult to stare into because of
the aversion response. The risk increases significantly, when the
eye is unable to protect itself, as occurs when a visible laser
beam irradiance exceeds 2.5 mW/cm2 (i.e., a total of 1 mW entering
the 7-mm pupil of the eye by either unaided or optically-aided
viewing). The laser classification denotes risk, when the laser is
viewed under worse-case conditions. In practice, if worst-case
conditions are seldom experienced, further relaxations can be
applied for certain limited applications. An example of this is
the 5 mW limit applied to the total power for surveying/ alignment
of lasers. This recognizes that "moderate-risk" (Class 3) lasers
are sometimes needed in this application but that the benefit in
this application outweighs the moderate risk of the 1-5 mW visible
laser group (US DHEW, 1979).
11.8. Present Standards of Exposure
11.8.1. Laser standards
A number of national and international standards have been
promulgated that show only minor differences, some of which may be
partly resolved, when future editions of the American National
Standards Institute (ANSI), British Standards Institute (BSI),
GOST, and the International Electrotechnical Commission (IEC)
appear.
Tables 7-11 present the most recent set of occupational ELs,
those promulgated by the ANSI Z-136.1 Standard (ANSI, 1980) and the
threshold limit values (TLVs) of the American Conference of
Governmental Industrial Hygienists (ACGIH, 1981), those given in
the draft International Electrotechnical Commission standard (IEC,
in preparation), and the values mentioned as "best available" in
Suess, ed. (1982).
11.8.1.1. Exposure limits
The tables and figures presented in this section are from the
ACGIH booklet Threshold limit values for chemical substances and
physical agents in the workroom environment with intended changes
for 1981 (ACGIH, 1981). For this criteria document, the term
"exposure limit" is used.
While the concept of an EL (or TLV) is that neither the general
population nor workers should be intentionally exposed above the
limit, accidental over-exposure may not always result in injury.
It is helpful to quote the TLV preamble given by ACGIH: "The
threshold limit values are for exposure to laser radiation under
conditions to which nearly all workers may be exposed without
adverse effects. The values should be used as guides in the
control of exposures and should not be regarded as fine lines
between safe and dangerous levels. They are based on the best
available information from experimental studies".
11.8.1.2. Repetitively pulsed lasers
Since the additive effects of multiple pulses are not fully
understood, caution must be used in the evaluation of such
exposures. The exposure limits for irradiance or radiant exposure
in multiple pulse trains have the following limitations:
(a) The exposure from any single pulse in the train is limited to
the exposure limit for a single comparable pulse;
(b) The average irradiance for a group of pulses is limited to the
EL (as given in Tables 7, 8, and 9) of a single pulse of the
same duration as the entire pulse group;
(c) When the instantaneous Pulse Repetition Frequency (PRF) of any
pulses within a train exceeds 1, the EL, applicable to each
pulse, is reduced by a factor (Cp), as shown in Fig. 26 for
pulse durations of less than 10-5 s. For pulses of greater
duration, the EL of a pulse in the train is found by dividing
the EL of a longer pulse of duration Nt by N, where N is the
number of pulses in the train, t is the duration of a single
pulse in the train, and the EL of Nt is the exposure limit of
one pulse having a duration equal to Nt s. The "pulse"
duration Nt is known as the TOTP (total on time pulse), Tt in
the ANSI standard. For a short group of N pulses, the reduced
EL will not be less than the single pulse EL divided by N.
Repeated exposures at repetition rates of less than 1 Hz should
be considered additive over a 24-h period.
11.6. Repetitively Pulsed Laser Exposure
The values in the present standards for repetitive ocular
exposure have been based on limited data and developed from purely
empirical extrapolations. The cumulative effect of repetitive
pulses was considered to be a function of the duration of the
individual pulse in a pulse train. For short pulses (duration less
than 10 µs), the EL for a single pulse was multiplied by a
correction factor to provide a reduced exposure on a per-pulse
basis. This value was then compared with the EL values for the
total energy and for a total exposure of the duration of the entire
train of exposures, to determine which limit would apply. For a
train of pulses, where the individual pulse duration exceeded 10
ms, a criterion based on total on-time Tt of the train of pulses
was applied to each individual pulse. This resulted in a reduced
EL for each pulse. However, all of these approaches were based
largely on studies in which the eye of the rhesus monkey was
exposed to single pulses of "minimal image size".
More recent studies (Greiss et al., 1980) suggest that the
pulse thresholds add as a function of N-¨ for small image sizes,
but not for large image sizes. The letter N refers to the number
of pulses in the train.
11.7. Restrictions for Special Applications (Class 3a)
The low risk of Class 2 lasers differs little from the lack of
risk of Class 1 lasers, in practice. Class 2 lasers emit a power
of 0.4 µW - 1 mW, a light level difficult to stare into because of
the aversion response. The risk increases significantly, when the
eye is unable to protect itself, as occurs when a visible laser
beam irradiance exceeds 2.5 mW/cm2 (i.e., a total of 1 mW entering
the 7-mm pupil of the eye by either unaided or optically-aided
viewing). The laser classification denotes risk, when the laser is
viewed under worse-case conditions. In practice, if worst-case
conditions are seldom experienced, further relaxations can be
applied for certain limited applications. An example of this is
the 5 mW limit applied to the total power for surveying/ alignment
of lasers. This recognizes that "moderate-risk" (Class 3) lasers
are sometimes needed in this application but that the benefit in
this application outweighs the moderate risk of the 1-5 mW visible
laser group (US DHEW, 1979).
11.8. Present Standards of Exposure
11.8.1. Laser standards
A number of national and international standards have been
promulgated that show only minor differences, some of which may be
partly resolved, when future editions of the American National
Standards Institute (ANSI), British Standards Institute (BSI),
GOST, and the International Electrotechnical Commission (IEC)
appear.
Tables 7-11 present the most recent set of occupational ELs,
those promulgated by the ANSI Z-136.1 Standard (ANSI, 1980) and the
threshold limit values (TLVs) of the American Conference of
Governmental Industrial Hygienists (ACGIH, 1981), those given in
the draft International Electrotechnical Commission standard (IEC,
in preparation), and the values mentioned as "best available" in
Suess, ed. (1982).
11.8.1.1. Exposure limits
The tables and figures presented in this section are from the
ACGIH booklet Threshold limit values for chemical substances and
physical agents in the workroom environment with intended changes
for 1981 (ACGIH, 1981). For this criteria document, the term
"exposure limit" is used.
While the concept of an EL (or TLV) is that neither the general
population nor workers should be intentionally exposed above the
limit, accidental over-exposure may not always result in injury.
It is helpful to quote the TLV preamble given by ACGIH: "The
threshold limit values are for exposure to laser radiation under
conditions to which nearly all workers may be exposed without
adverse effects. The values should be used as guides in the
control of exposures and should not be regarded as fine lines
between safe and dangerous levels. They are based on the best
available information from experimental studies".
11.8.1.2. Repetitively pulsed lasers
Since the additive effects of multiple pulses are not fully
understood, caution must be used in the evaluation of such
exposures. The exposure limits for irradiance or radiant exposure
in multiple pulse trains have the following limitations:
(a) The exposure from any single pulse in the train is limited to
the exposure limit for a single comparable pulse;
(b) The average irradiance for a group of pulses is limited to the
EL (as given in Tables 7, 8, and 9) of a single pulse of the
same duration as the entire pulse group;
(c) When the instantaneous Pulse Repetition Frequency (PRF) of any
pulses within a train exceeds 1, the EL, applicable to each
pulse, is reduced by a factor (Cp), as shown in Fig. 26 for
pulse durations of less than 10-5 s. For pulses of greater
duration, the EL of a pulse in the train is found by dividing
the EL of a longer pulse of duration Nt by N, where N is the
number of pulses in the train, t is the duration of a single
pulse in the train, and the EL of Nt is the exposure limit of
one pulse having a duration equal to Nt s. The "pulse"
duration Nt is known as the TOTP (total on time pulse), Tt in
the ANSI standard. For a short group of N pulses, the reduced
EL will not be less than the single pulse EL divided by N.
Repeated exposures at repetition rates of less than 1 Hz should
be considered additive over a 24-h period.
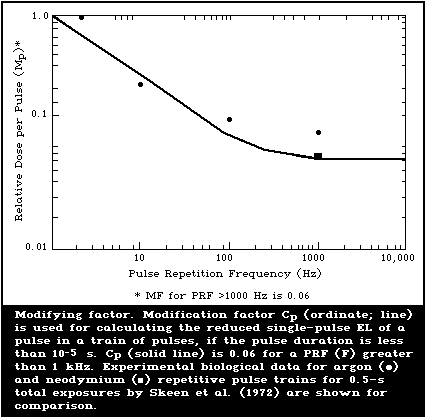 Table 7. Exposure limits for direct ocular exposures (intrabeam viewing)
from a laser beam
-------------------------------------------------------------------------
Spectral Wavelength Exposure time (t) Exposure limits
region seconds (s)
-------------------------------------------------------------------------
UVC 200 nm to 280 nm 10-9 to 3 x 104 3 mJ/cm2
UVB 280 nm to 302 nm 10-9 to 3 x 104 3 mJ/cm2
303 nm 10-9 to 3 x 104 4 mJ/cm2
304 nm 10-9 to 3 x 104 6 mJ/cm2
305 nm 10-9 to 3 x 104 10 mJ/cm2
306 nm 10-9 to 3 x 104 16 mJ/cm2 )
307 nm 10-9 to 3 x 104 25 mJ/cm2 )
308 nm 10-9 to 3 x 104 40 mJ/cm2 ) not to
309 nm 10-9 to 3 x 104 63 mJ/cm2 ) exceed
310 nm 10-9 to 3 x 104 100 mJ/cm2) 0.56t¨
311 nm 10-9 to 3 x 104 160 mJ/cm2) J/cm2
312 nm 10-9 to 3 x 104 250 mJ/cm2)
313 nm 10-9 to 3 x 104 400 mJ/cm2)
314 nm 10-9 to 3 x 104 630 mJ/cm2)
315 nm 10-9 to 3 x 104 1.0 J/cm2)
315 nm to 400 nm 10-9 to 10 0.56t1/4 J/cm2
UVA 315 nm to 400 nm 10 to 103 1.0 J/cm2
315 nm to 400 nm 103 to 3 x 104 1.0 mW/cm2
-------------------------------------------------------------------------
Table 7 (contd.)
-------------------------------------------------------------------------
Spectral Wavelength Exposure time (t) Exposure limits
region seconds (s)
-------------------------------------------------------------------------
Light 400 nm to 700 nm 10-9 to 1.8 x 10-5 5 x 10-7J/cm2
400 nm to 700 nm 1.8 x 10-5 to 10 1.8(t/4 ´t) mJ/cm2
400 nm to 549 nm 10 to 104 10 mJ/cm2
500 nm to 700 nm 10 to T1 1.8(t/4 ´t) mJ/cm2
550 nm to 700 nm T1 to 104 10CB mJ/cm2
400 nm to 700 nm 104 to 3 x 104 CB µW/cm2
IR-A 700 nm to 1049 nm 10-9 to 1.8 x 10-5 5 CA x 10-7 J/cm2
700 nm to 1049 nm 1.8 x 10-5 to 103 1.8CA(t/4 ´/t) mJ/cm2
1050 nm to 1400 nm 10-9 to 5 x 10-4 5 x 10-6 J/cm2
1050 nm to 1400 nm 5 x 10-4 to 103 9(t/4 ´/t) mJ/cm2
700 nm to 1400 nm 103 to 3 x 104 320 CA µW/cm2
IR-B & C 1.4 µm to 103 µm 10-9 to 10-7 10-2 J/cm2
1.4 µm to 103 µm 10-7 to 10 0.56 4 ´/t) J/cm2
1.4 µm to 103 µm 10 to 3 x 104 0.1 W/cm2
-------------------------------------------------------------------------
The formula for Correction Factor CA (Fig. 25) is
CA = 1 for wavelength (lambda) of 400 nm - 700 nm;
CA = 10(0.002[lambda-700 nm]) for 700 nm < lambda < 1050 nm; and
CA = 5 for 1050 < lambda < 1400 nm.
CB = 1 for lambda = 400 - 550 nm;
CB = 10(0.015[lambda-550]) for lambda = 550 - 700 nm.
T1 = 10 s for g = 400 - 550 nm; T1 = 10 x 10(0.02[lambda-550]) for
lambda = 550 - 700 nm.
For lambda = 1.5 to 1.6 xi m increase EL by 100 for periods of less
than 1 µs.
Table 8. Exposure limits for viewing a diffuse reflection of a
laser beam or an extended source laser
-------------------------------------------------------------------------
Spectral Exposure limits Wave-length Exposure time (t) (s)
region
-------------------------------------------------------------------------
UV 200 nm to 400 nm 10-9 to 3 x 104 Same as Table 7
Light 400 nm to 700 nm 10-9 to 10 10 3 ´t J/(cm2 x sr)
400 nm to 549 nm 10 to 104 21 J/(cm2 x sr)
550 nm to 700 nm 10 to T1 3.83 (t/ 4 ´t) J/(cm2 x sr)
550 nm to 700 nm T1 to 104 21/CB J/(cm2 x sr)
400 nm to 700 nm 104 to 3 x 104 2.1/CB x 10-3 W/(cm2 x sr)
IR-A 700 nm to 1400 nm 10-9 to 10 10CA 3 ´t J/(cm2 x sr)
700 nm to 1400 nm 10 to 103 3.83CA(t/4 ´t)J/(cm2 x sr)
700 nm to 1400 nm 103 to 3 x 104 0.64CA W/(cm2 x sr)
IR-B & C 1.4 µm to 1 mm 10-9 to 3 x 104 Same as Table 7
-------------------------------------------------------------------------
CA, CB, and T1 are the same as in footnote to Table 7.
Table 9. Exposure limits for skin exposure from a laser beam
---------------------------------------------------------------
Spectral Wave-length Exposure time Exposure limits
region (t) (s)
---------------------------------------------------------------
UV 200 nm to 400 nm 10-9 to 3x104 Same as Table 7
Light & 400 nm to 1400 nm 10-9 to 10-7 2CA x 10-2 J/cm2
IR-A 400 nm to 1400 nm 10-7 to 10 1.1CA 4´t J/cm2
IR-B & C 1.4 µm to 1 mm 10-9 to 3 x 104 Same as Table 6
---------------------------------------------------------------
CA = 1.0 for lambda = 400 - 700 nm; see Fig. 25 for value at
greater wavelengths.
NOTE: To aid in the determination of ELs for exposure
durations requiring calculations of fractional powers,
Fig. 25 may be used.
Table 10. Additivity of effects on eye and skin from different spectral regionsa
---------------------------------------------------------------------------------
UV-C and UV-B UV-A Visible and IR-A IR-B and IR-C
Spectral region 200-315 nm 315-400 nm 400-1400 nm 1400-106 nm
---------------------------------------------------------------------------------
UV-C and UV-B eye
200-314 nm skin
UV-A eye eye
315 nm skin skin skin
Visible and IR-A eye
400-1400 nm skin skin skin
IR-B and IR-C eye eye
1400-106 nm skin skin skin
---------------------------------------------------------------------------------
a Some synergism is expected when 2 spectral bands illuminate the same tissue
simultaneously. Exact formulae to treat these additive effects have not been
developed for most standards.
Table 11. Selected values of the minimum angle of an extended
source that may be used for applying extended source ELs
--------------------------------
Exposure duration Angle alpha
(s) (mrad)
--------------------------------
10-9 8.0a
10-8 5.4a
10-7 3.7a
10-6 2.5a
10-5 1.7a
10-4 2.2
10-3 3.6
10-2 5.7
10-1 9.2
--------------------------------
Table 11 (contd.)
--------------------------------
Exposure duration Angle alpha
(s) (mrad)
--------------------------------
1.0 15
10 24
102 24
103 24
104 24
--------------------------------
a For exposure durations of less
than 0.05 ms alphamin is less
for lambda = 1050 to 1400 nm.
11.8.1.3. Extended source laser exposure
The ELs for "extended sources" apply to sources that subtend an
angle greater than alphamin (Table 11), which varies with exposure
duration (t). This angle is not the beam divergence of the source.
Limits expressed as either radiance or integrated radiance may be
averaged over an angle as great as alphamin or sampled over a
source area as small as 1 mm in diameter.
Table 8 should be used to calculate the EL (as a brightness)
for an extended source such as a holographic display or a screen
illuminated by a static or scanning laser beam. The values in
Table 8 apply to viewing a diffuse reflection from a laser beam,
where a truly extensive retinal image occurs. Some laser devices
are intentionally designed as diffuse sources (e.g., beacons) to
radiate monochromatic optical power and still remain Class 1. The
extended source ELs of Table 8 apply to the direct output of the
laser system if the source is diffuse. As a further example, a
low-quality semiconductor diode laser or a semiconductor laser
diode array may be "extended". In this case, the average radiance
of the diode array might be applied against the extended source EL.
It must be emphasized that, in almost all instances, a laser source
is still a "point source" within definitions used by the standards.
To aid in determining when extended-source ELs are applicable,
the concept of alphamin was invented. The value of alphamin is a
linear angle expressed in mrads and is the minimum viewing angle at
which extended-source ELs apply. For viewing distances beyond the
location where the source angle subtends an angle less than
alphamin, the source is considered from a safety standpoint to be a
"point source" and the intrabeam viewing criteria of Table 7 apply.
Because the extended source ELs and the point source ELs do not
vary in exactly the same way as a function of pulse duration (or
exposure duration) (t), this limiting angle alphamin varies with
exposure duration (Table 11). Indeed alphamin is nothing more than:
alphamin = (4/pi) (EL [point source]/EL [extended source])´ Equation (14)
11.8.1.4. Restriction on ELs
The ELs were developed for conditions of occupational exposure
and the underlying assumption is that nearly all workers may be
exposed to the levels without adverse effects. However, some
photosensitive individuals may experience adverse effects at lower
levels for wavelengths of less than 500 nm.
11.8.2. Standards for non-laser sources
11.8.2.1. Introduction
The most commonly occurring hazardous effects from arcs and
high-intensity lamps are ultraviolet erythema and photokeratitis.
Retinal injury from such sources is seldom recognized though it is
not unheard of. Considering that much was known about optical
radiation hazards prior to the development of the laser, it seems
somewhat surprising that ELs and safety standards for lamps and
arcs did not exist prior to laser safety standards. Standards were
developed empirically for eye protective filters for welders, but
were not based on ELs.
Bright sources emitting cw light elicit a normal aversion or
pain response that serves to protect the eye and skin from injury.
Visual comfort has often been used as an approximate hazard index.
Eye protection baffles and other controls have been provided on
this basis. The determination of shade number for welding goggles
is one example. The present standards for welding goggle
specifications were simply based on a comfort index for viewing the
arc. Since UVR and infrared radiation were considered to be of no
value in viewing welding arcs, they were deliberately filtered out.
UV and IR filtration factors exceeding those for light were
specified as the best that could be achieved with readily available
glass materials.
Quantitative guidance is often sought with regard to both eye
and skin safety in relation to new sources of radiation. Though
several safety limits for optical radiation have been proposed in
the literature within recent years, it is only for the ultraviolet
spectral region that there have been any widely accepted limits,
but even these have provoked controversy.
ELs applicable to broad-band sources such as open-arc
processes, arc lamps, incandescent lamps, and gas discharge lamps
may differ considerably from laser ELs for two main reasons. The
first is that the source normally emits in a broad spectral band.
Therefore, effects due to narrow wavelength absorption or
coherence, which are potentially of concern with laser exposure,
are not likely to have a substantial impact on the hazards from a
broad-band source. All of the composite optical spectral bands for
conventional sources must be evaluated separately. For instance,
ultraviolet hazard criteria differ completely from light hazard
criteria.
The second major difference between laser and non-laser health
criteria results from the fact that most hazardous laser exposures
result from viewing a point source, whereas hazardous lamps and
arcs are usually extended sources. In the development of a new
lamp, any unwanted ultraviolet radiation should be filtered out by
the choice of an appropriately thick glass envelope, based on
computation, and assessments of both acute and chronic risks and
actual UVR measurements. In the past, manufacturers have watched
for acute effects in people exposed to prototype lamps.
The radiance from a conventional source is generally physically
limited compared with that of a laser source. The exposure of an
individual from a lamp source is seldom likely to exceed that under
normal operating conditions. Laser output powers can change
enormously with slight changes in the laser cavity.
11.8.2.2. UVR Criteria
As previously noted, the health hazards associated with UV-B + C
exposure of the eye and skin are often considered separately from
those associated with UV-A.
In the development of health criteria for industrial UVR
exposure, the prime consideration must be ELs that would prevent
unwanted acute and chronic effects. At the same time, simplicity
of measurement and application are important. If a single
instrument having a spectral response weighted against the envelope
action spectrum for UV-B and UV-C injury were developed, then a
direct measurement could be made of the UVR risk. Without a
spectrally integrating instrument, the spectral irradiance from the
source of interest can be measured at the point of greatest concern
(normally the nearest point of access). This spectral irradiance
Elambda is then weighted by the ACGIH envelope action curve Slambda
(Fig. 27, Table 12 and 13) for wavelengths of less than 320 nm.
Table 7. Exposure limits for direct ocular exposures (intrabeam viewing)
from a laser beam
-------------------------------------------------------------------------
Spectral Wavelength Exposure time (t) Exposure limits
region seconds (s)
-------------------------------------------------------------------------
UVC 200 nm to 280 nm 10-9 to 3 x 104 3 mJ/cm2
UVB 280 nm to 302 nm 10-9 to 3 x 104 3 mJ/cm2
303 nm 10-9 to 3 x 104 4 mJ/cm2
304 nm 10-9 to 3 x 104 6 mJ/cm2
305 nm 10-9 to 3 x 104 10 mJ/cm2
306 nm 10-9 to 3 x 104 16 mJ/cm2 )
307 nm 10-9 to 3 x 104 25 mJ/cm2 )
308 nm 10-9 to 3 x 104 40 mJ/cm2 ) not to
309 nm 10-9 to 3 x 104 63 mJ/cm2 ) exceed
310 nm 10-9 to 3 x 104 100 mJ/cm2) 0.56t¨
311 nm 10-9 to 3 x 104 160 mJ/cm2) J/cm2
312 nm 10-9 to 3 x 104 250 mJ/cm2)
313 nm 10-9 to 3 x 104 400 mJ/cm2)
314 nm 10-9 to 3 x 104 630 mJ/cm2)
315 nm 10-9 to 3 x 104 1.0 J/cm2)
315 nm to 400 nm 10-9 to 10 0.56t1/4 J/cm2
UVA 315 nm to 400 nm 10 to 103 1.0 J/cm2
315 nm to 400 nm 103 to 3 x 104 1.0 mW/cm2
-------------------------------------------------------------------------
Table 7 (contd.)
-------------------------------------------------------------------------
Spectral Wavelength Exposure time (t) Exposure limits
region seconds (s)
-------------------------------------------------------------------------
Light 400 nm to 700 nm 10-9 to 1.8 x 10-5 5 x 10-7J/cm2
400 nm to 700 nm 1.8 x 10-5 to 10 1.8(t/4 ´t) mJ/cm2
400 nm to 549 nm 10 to 104 10 mJ/cm2
500 nm to 700 nm 10 to T1 1.8(t/4 ´t) mJ/cm2
550 nm to 700 nm T1 to 104 10CB mJ/cm2
400 nm to 700 nm 104 to 3 x 104 CB µW/cm2
IR-A 700 nm to 1049 nm 10-9 to 1.8 x 10-5 5 CA x 10-7 J/cm2
700 nm to 1049 nm 1.8 x 10-5 to 103 1.8CA(t/4 ´/t) mJ/cm2
1050 nm to 1400 nm 10-9 to 5 x 10-4 5 x 10-6 J/cm2
1050 nm to 1400 nm 5 x 10-4 to 103 9(t/4 ´/t) mJ/cm2
700 nm to 1400 nm 103 to 3 x 104 320 CA µW/cm2
IR-B & C 1.4 µm to 103 µm 10-9 to 10-7 10-2 J/cm2
1.4 µm to 103 µm 10-7 to 10 0.56 4 ´/t) J/cm2
1.4 µm to 103 µm 10 to 3 x 104 0.1 W/cm2
-------------------------------------------------------------------------
The formula for Correction Factor CA (Fig. 25) is
CA = 1 for wavelength (lambda) of 400 nm - 700 nm;
CA = 10(0.002[lambda-700 nm]) for 700 nm < lambda < 1050 nm; and
CA = 5 for 1050 < lambda < 1400 nm.
CB = 1 for lambda = 400 - 550 nm;
CB = 10(0.015[lambda-550]) for lambda = 550 - 700 nm.
T1 = 10 s for g = 400 - 550 nm; T1 = 10 x 10(0.02[lambda-550]) for
lambda = 550 - 700 nm.
For lambda = 1.5 to 1.6 xi m increase EL by 100 for periods of less
than 1 µs.
Table 8. Exposure limits for viewing a diffuse reflection of a
laser beam or an extended source laser
-------------------------------------------------------------------------
Spectral Exposure limits Wave-length Exposure time (t) (s)
region
-------------------------------------------------------------------------
UV 200 nm to 400 nm 10-9 to 3 x 104 Same as Table 7
Light 400 nm to 700 nm 10-9 to 10 10 3 ´t J/(cm2 x sr)
400 nm to 549 nm 10 to 104 21 J/(cm2 x sr)
550 nm to 700 nm 10 to T1 3.83 (t/ 4 ´t) J/(cm2 x sr)
550 nm to 700 nm T1 to 104 21/CB J/(cm2 x sr)
400 nm to 700 nm 104 to 3 x 104 2.1/CB x 10-3 W/(cm2 x sr)
IR-A 700 nm to 1400 nm 10-9 to 10 10CA 3 ´t J/(cm2 x sr)
700 nm to 1400 nm 10 to 103 3.83CA(t/4 ´t)J/(cm2 x sr)
700 nm to 1400 nm 103 to 3 x 104 0.64CA W/(cm2 x sr)
IR-B & C 1.4 µm to 1 mm 10-9 to 3 x 104 Same as Table 7
-------------------------------------------------------------------------
CA, CB, and T1 are the same as in footnote to Table 7.
Table 9. Exposure limits for skin exposure from a laser beam
---------------------------------------------------------------
Spectral Wave-length Exposure time Exposure limits
region (t) (s)
---------------------------------------------------------------
UV 200 nm to 400 nm 10-9 to 3x104 Same as Table 7
Light & 400 nm to 1400 nm 10-9 to 10-7 2CA x 10-2 J/cm2
IR-A 400 nm to 1400 nm 10-7 to 10 1.1CA 4´t J/cm2
IR-B & C 1.4 µm to 1 mm 10-9 to 3 x 104 Same as Table 6
---------------------------------------------------------------
CA = 1.0 for lambda = 400 - 700 nm; see Fig. 25 for value at
greater wavelengths.
NOTE: To aid in the determination of ELs for exposure
durations requiring calculations of fractional powers,
Fig. 25 may be used.
Table 10. Additivity of effects on eye and skin from different spectral regionsa
---------------------------------------------------------------------------------
UV-C and UV-B UV-A Visible and IR-A IR-B and IR-C
Spectral region 200-315 nm 315-400 nm 400-1400 nm 1400-106 nm
---------------------------------------------------------------------------------
UV-C and UV-B eye
200-314 nm skin
UV-A eye eye
315 nm skin skin skin
Visible and IR-A eye
400-1400 nm skin skin skin
IR-B and IR-C eye eye
1400-106 nm skin skin skin
---------------------------------------------------------------------------------
a Some synergism is expected when 2 spectral bands illuminate the same tissue
simultaneously. Exact formulae to treat these additive effects have not been
developed for most standards.
Table 11. Selected values of the minimum angle of an extended
source that may be used for applying extended source ELs
--------------------------------
Exposure duration Angle alpha
(s) (mrad)
--------------------------------
10-9 8.0a
10-8 5.4a
10-7 3.7a
10-6 2.5a
10-5 1.7a
10-4 2.2
10-3 3.6
10-2 5.7
10-1 9.2
--------------------------------
Table 11 (contd.)
--------------------------------
Exposure duration Angle alpha
(s) (mrad)
--------------------------------
1.0 15
10 24
102 24
103 24
104 24
--------------------------------
a For exposure durations of less
than 0.05 ms alphamin is less
for lambda = 1050 to 1400 nm.
11.8.1.3. Extended source laser exposure
The ELs for "extended sources" apply to sources that subtend an
angle greater than alphamin (Table 11), which varies with exposure
duration (t). This angle is not the beam divergence of the source.
Limits expressed as either radiance or integrated radiance may be
averaged over an angle as great as alphamin or sampled over a
source area as small as 1 mm in diameter.
Table 8 should be used to calculate the EL (as a brightness)
for an extended source such as a holographic display or a screen
illuminated by a static or scanning laser beam. The values in
Table 8 apply to viewing a diffuse reflection from a laser beam,
where a truly extensive retinal image occurs. Some laser devices
are intentionally designed as diffuse sources (e.g., beacons) to
radiate monochromatic optical power and still remain Class 1. The
extended source ELs of Table 8 apply to the direct output of the
laser system if the source is diffuse. As a further example, a
low-quality semiconductor diode laser or a semiconductor laser
diode array may be "extended". In this case, the average radiance
of the diode array might be applied against the extended source EL.
It must be emphasized that, in almost all instances, a laser source
is still a "point source" within definitions used by the standards.
To aid in determining when extended-source ELs are applicable,
the concept of alphamin was invented. The value of alphamin is a
linear angle expressed in mrads and is the minimum viewing angle at
which extended-source ELs apply. For viewing distances beyond the
location where the source angle subtends an angle less than
alphamin, the source is considered from a safety standpoint to be a
"point source" and the intrabeam viewing criteria of Table 7 apply.
Because the extended source ELs and the point source ELs do not
vary in exactly the same way as a function of pulse duration (or
exposure duration) (t), this limiting angle alphamin varies with
exposure duration (Table 11). Indeed alphamin is nothing more than:
alphamin = (4/pi) (EL [point source]/EL [extended source])´ Equation (14)
11.8.1.4. Restriction on ELs
The ELs were developed for conditions of occupational exposure
and the underlying assumption is that nearly all workers may be
exposed to the levels without adverse effects. However, some
photosensitive individuals may experience adverse effects at lower
levels for wavelengths of less than 500 nm.
11.8.2. Standards for non-laser sources
11.8.2.1. Introduction
The most commonly occurring hazardous effects from arcs and
high-intensity lamps are ultraviolet erythema and photokeratitis.
Retinal injury from such sources is seldom recognized though it is
not unheard of. Considering that much was known about optical
radiation hazards prior to the development of the laser, it seems
somewhat surprising that ELs and safety standards for lamps and
arcs did not exist prior to laser safety standards. Standards were
developed empirically for eye protective filters for welders, but
were not based on ELs.
Bright sources emitting cw light elicit a normal aversion or
pain response that serves to protect the eye and skin from injury.
Visual comfort has often been used as an approximate hazard index.
Eye protection baffles and other controls have been provided on
this basis. The determination of shade number for welding goggles
is one example. The present standards for welding goggle
specifications were simply based on a comfort index for viewing the
arc. Since UVR and infrared radiation were considered to be of no
value in viewing welding arcs, they were deliberately filtered out.
UV and IR filtration factors exceeding those for light were
specified as the best that could be achieved with readily available
glass materials.
Quantitative guidance is often sought with regard to both eye
and skin safety in relation to new sources of radiation. Though
several safety limits for optical radiation have been proposed in
the literature within recent years, it is only for the ultraviolet
spectral region that there have been any widely accepted limits,
but even these have provoked controversy.
ELs applicable to broad-band sources such as open-arc
processes, arc lamps, incandescent lamps, and gas discharge lamps
may differ considerably from laser ELs for two main reasons. The
first is that the source normally emits in a broad spectral band.
Therefore, effects due to narrow wavelength absorption or
coherence, which are potentially of concern with laser exposure,
are not likely to have a substantial impact on the hazards from a
broad-band source. All of the composite optical spectral bands for
conventional sources must be evaluated separately. For instance,
ultraviolet hazard criteria differ completely from light hazard
criteria.
The second major difference between laser and non-laser health
criteria results from the fact that most hazardous laser exposures
result from viewing a point source, whereas hazardous lamps and
arcs are usually extended sources. In the development of a new
lamp, any unwanted ultraviolet radiation should be filtered out by
the choice of an appropriately thick glass envelope, based on
computation, and assessments of both acute and chronic risks and
actual UVR measurements. In the past, manufacturers have watched
for acute effects in people exposed to prototype lamps.
The radiance from a conventional source is generally physically
limited compared with that of a laser source. The exposure of an
individual from a lamp source is seldom likely to exceed that under
normal operating conditions. Laser output powers can change
enormously with slight changes in the laser cavity.
11.8.2.2. UVR Criteria
As previously noted, the health hazards associated with UV-B + C
exposure of the eye and skin are often considered separately from
those associated with UV-A.
In the development of health criteria for industrial UVR
exposure, the prime consideration must be ELs that would prevent
unwanted acute and chronic effects. At the same time, simplicity
of measurement and application are important. If a single
instrument having a spectral response weighted against the envelope
action spectrum for UV-B and UV-C injury were developed, then a
direct measurement could be made of the UVR risk. Without a
spectrally integrating instrument, the spectral irradiance from the
source of interest can be measured at the point of greatest concern
(normally the nearest point of access). This spectral irradiance
Elambda is then weighted by the ACGIH envelope action curve Slambda
(Fig. 27, Table 12 and 13) for wavelengths of less than 320 nm.
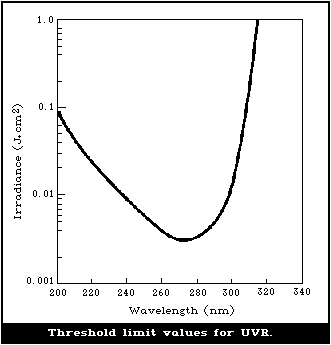 Table 12. Relative spectral
effectiveness for selected wavelengths
--------------------------------------
Relative
spectral
Wavelength Elambda effectiveness
(nm) (mJ/cm2) Slambda
--------------------------------------
200 100 0.03
210 40 0.075
220 25 0.12
230 16 0.19
240 10 0.30
250 7.0 0.43
254 6.0 0.5
260 4.6 0.65
270 3.0 1.0
280 3.4 0.88
290 4.7 0.64
300 10 0.30
305 50 0.06
310 200 0.015
315 1000 0.003
--------------------------------------
Table 13. ACGIH ultraviolet exposure limits
--------------------------------------------
Duration of exposure Effective irradiance,
per day Eeff (µW/cm2)
--------------------------------------------
8 h 0.1
4 h 0.2
2 h 0.4
1 h 0.8
30 min 1.7
15 min 3.3
10 min 5
5 min 10
1 min 50
30 s 100
10 s 300
1 s 3000
0.5 s 6000
0.1 s 30 000
--------------------------------------------
All the preceding ELs for ultraviolet energy apply to sources
that subtend an angle less than 80°. Sources that subtend a
greater angle need to be measured only over an angle of 80°.
ACGIH recommended values: The threshold limit values for
occupational exposure to UVR incident on skin or eye, where
irradiance values are known and exposure time is controlled, are as
follows:
1. For the near ultraviolet spectral region (320-400 nm),
total irradiance incident on the unprotected skin or eye
should not exceed 1 mW/cm2 for periods greater than 103 s
(approximately 16 min) and for exposure times less than
103 s should not exceed one J/cm2.
2. For the actinic ultraviolet spectral region (200-315 nm),
radiant exposure incident on the unprotected skin or eye
should not exceed the values given in Table 10, within an
8-h period.
3. To determine the effective irradiance of a broad-band
source weighted against the peak of the spectral
effectiveness curve (270 nm), the following weighting
formula should be used:
Eeff = SIGMA Elambda Slambda delta lambda where:
Eeff = effective irradiance relative to a monochromatic
source at 270 nm in W/cm2 (J/s/cm2)
Elambda = spectral irradiance in W/cm2/nm
Slambda = relative spectral effectiveness (unitless)
delta lambda = band width (nm)
4. Permissible exposure time in seconds for exposure to
actinic ultraviolet radiation incident on the unprotected
skin or eye may be computed by dividing 0.003 J/cm2 by
Eeff in W/cm2. The exposure time may also be determined
using Table 13, which provides exposure times
corresponding to effective irradiances in µW/cm2.
Conditioned (tanned) individuals can tolerate skin exposure in
excess of the TLV without erythemal effects. However, such
conditioning may not protect persons against skin cancer.
For the UV-A, ACGIH considered it reasonable to propose a
guideline for ocular exposure so low that no conceivable thermal or
photochemical injury mechanisms were likely to be demonstrated. To
prevent thermal injury, it was assumed that, for exposure durations
of less than 100 s, the eye should be protected against exposures
above 10 kJ/m2 (1 J/cm2). Because of the lack of adverse effects
reported in individuals working with ultraviolet "black light"
sources at levels of 1 mW/cm2 (or above), it was presumed that a
level of 1 mW/cm2, the approximate level of exposure of the eye to
UVA-A in outdoor reflected sunlight, would be a reasonable upper
limit for exposures lasting 1000 s or more. The skin exposure limit
could presumably be increased by a factor of 5 for the longer
exposure durations. To avoid thermal effects at very short
exposure durations, the total UVR corneal irradiance was also
limited to 1 W/cm2. It is now known that photochemical effects
occur in both the eye and skin and that total daily doses of 20 -
100 J/cm2 cause acute corneal opacities (Pitts et al., 1977;
Zuchlich & Kurtin, 1977) and skin erythema from the UV-A (Parrish
et al., 1978). Hence, these UV-A criteria must be applied with
great caution for conditions of very long (exceeding 4 h) exposure.
11.8.2.3. Retinal health criteria
Laser protection standards incorporate several simplifications
that depend on the single-wavelength and point-source
characteristics of the laser. These standards may provide a too
conservative estimate of the real risk, if laser criteria are
applied to broad-band sources. No official standards exist for the
retinal risk evaluation of a broad-band source. Tentative
guidelines exist from ACGIH. To use these guidelines, both a blue-
light hazard function B lambda and a retinal thermal injury
function R lambda must be used. The source spectrum may be weighted
to indicate comparative levels of risk from the two types of
retinal injury mechanisms. Using equation 13 (section 8.4.1.3), in
which the retinal irradiance Er is directly proportional to the
radiance L of the source, the square of the pupil diameter dp, and
the transmission t of the ocular media. The retinal spectral
irradiance distribution can be calculated from the spectral
radiance distribution Llambda and knowledge of the spectral
transmission of the ocular media taulambda. In the absence of a
radiance standard, this approach can be used to calculate retinal
levels directly and to compare them directly with thresholds of
injury (Sliney & Freasier, 1973). However, the present approach is
to establish ELs for the spectrally weighted radiances. These
safety weighting functions are given in Table 14. Spectral factors
weighted against the spectral radiance are then applied as shown in
sections 11.8.2.4 and 11.8.2.5.
Table 14. Spectral weighting functions for assessing
retinal risks from broad-band optical sourcesa
-------------------------------------------------------
Blue-light Thermal
Wavelength hazard function hazard function
(nm) Blambda Rlambda
-------------------------------------------------------
400 0.10 1.0
405 0.20 2.0
410 0.40 4.0
415 0.80 8.0
420 0.90 9.0
425 0.95 9.5
430 0.98 9.8
435 1.0 10
440 1.0 10
445 0.97 9.7
450 0.94 9.4
455 0.90 9.0
460 0.80 8.0
465 0.70 7.0
470 0.62 6.2
475 0.55 5.5
-------------------------------------------------------
Table 14 (contd.)
-------------------------------------------------------
Blue-light Thermal
Wavelength hazard function hazard function
(nm) Blambda Rlambda
-------------------------------------------------------
480 0.45 4.5
485 0.40 4.0
490 0.22 2.2
495 0.16 1.6
500-600 10[(450-lambda)/50] 1.0
600-700 0.001 1.0
700-1049 0.001 10[(700-lambda)/500]
1050-1400 0.001 0.2
-------------------------------------------------------
a From: ACGIH (1981).
11.8.2.4. Retinal thermal risk evaluation
To protect against thermal retinal injury from short-term
exposures, the spectral radiance of the lamp weighted against the
function Rlambda (Table 14) should not exceed:
1400
SIGMA Llambda Rlambda delta lambda L(Haz) = ´ t/(alpha t) W/(cm2 x sr)
400 Equation (15)
where Llambda is given in W/(cm2 x sr), t is the viewing duration
(or pulse duration if the lamp is pulse limited) which is limited
to 1 ms - 10 s, and alpha is the angular subtense of the source in
radians. The angle alpha should be limited to approximately 0.1
radian. If the lamp is oblong, alpha refers to the longest
dimension (1) that can be viewed. For instance, at a viewing
distance (r) of 500 cm from a tubular lamp 50 cm long, the viewing
angle alpha is 1/r or 0.1 rad. Spectral radiance (Llambda)
measurements must be made at frequent wavelength intervals (delta
lambda) to preclude serious error. The delta lambda should be less
than 5 nm in the UV and blue end of the visible spectrum.
11.8.2.5. Retinal blue-light risk evaluation
To protect against retinal injury from blue-light exposure, the
integrated spectral radiance of the lamp weighted with the blue-
light hazard function (Blambda of Table 14) should not exceed 100
J/cm2 x sr for a duration of less that 104 or exceed 10 mW/(cm2 x
sr) for t > 104 s:
1400
SIGMA Llambda x t x Blambda x delta lambda < 100 J/(cm2 x sr) for t < 104 s
400 Equation (16)
or
1400
SIGMA Llambda x Blambda x delta lambda < 10 W/(cm2 x sr) for t > 104 s
400 Equation (17)
and for a point source (alpha < 11 mrad)
1400
SIGMA Elambda x t x Blambda x delta lambda < H(Haz) = 10 mJ/cm2 for t < 104 s
400 Equation (18)
or
1400
SIGMA Elambda x Blambda x delta lambda < E(Haz) = 1 µW/cm2 for t > 104 s
400 Equation (19)
These levels assume a constricted pupil, as would occur with
fixed viewing of any type of extended source with a radiance
approaching the EL. For a spectrally weighted source radiance (L)
that exceeds 10 mW/(cm2 x sr) in the blue-light spectral region,
the permissible exposure duration tmax in s is simply:
1400
tmax = 100 J/(cm2 x sr) / SIGMA Llambda x Blambda x delta lambda for t < 104 s
400 Equation (20)
The extended-source limits are greater than the 198. ELs for a
440-nm laser radiation source given by either ANSI or ACGIH, which
assume a 7-mm pupil rather than the 3-mm used for the broad-band
source analysis.
11.8.2.6. IR-A risk analysis
The proposed ACGIH EL also limited the IR-A and IR-B infrared
radiation beyond 770 nm to 10 mW/cm2 to avoid possible
cataractogenesis (the appearance of which may be delayed). For an
infrared heat lamp or other source that lacks a strong visual
stimulus, the radiance for wavelengths between 700 and 1400 nm for
long-term viewing should be limited to:
1400
SIGMA Llambda x delta lambda < L(Haz) = [0.6/alpha] W/(cm2 x sr)
700 Equation (21)
This limit is also based on a 7-mm pupil diameter.
NOTE: Equations 16 to 21 are empirical and are not, strictly
speaking, dimensionally correct. To make these formulae
correct, a dimensional correction factor must be inserted
into each formula. It is, therefore, important to use only
the units specified.
11.8.3. Infrared standards
There are no established non-laser, infrared (IR) health
standards. However, the laser ELs can be applied for broad-band
sources, if, in addition, the whole-body irradiation is evaluated.
Even irradiances as low as 100 W/m2 (10 mW/cm2) can place an
uncomfortable thermal load on the human body, especially when the
irradiation is not confined to one side of the body and this
radiant heat load occurs along with high ambient air temperatures.
In contrast, the IR laser EL for periods exceeding 10 s is 1 kW/m2
(100 mW/cm2), assuming that the total irradiated area of the skin
or the eye will be small. For laser exposure the irradiated area
is generally small, but this is not so likely when the body is
exposed to optical radiation from non-laser sources; and heat
stress must be evaluated.
The determination of the wet-bulb-globe-temperature (WBGT)
index requires a combination of a dry-bulb temperature with a wet-
bulb (WB) temperature (which involves humidity, air movement, etc.)
and a black-globe (BG) temperature (which includes the radiant
(predominantly infrared) contribution). These three temperatures
are weighted differently in two equations used for evaluating heat
stress - one for outdoor workers exposed to sunlight, another for
indoor workers exposed to infrared sources. The nature of the
skin's reflectance is such that much of the visible and IR-A are
reflected, whereas IR-B and IR-C are almost totally absorbed. The
spectral reflectance of most clothing is somewhat similar to that
of skin in the infrared. Obviously the second formula would be
used in any IR risk evaluation. The ACGIH formula for indoor heat
stress is:
WBGT = 0.7 WB + 0.3 GT Equation (22)
A heat-stress condition exists when this WBGT value exceeds 25 -
30 °C depending on work load.
A major problem in any infrared safety standard concerned with
wavelengths beyond 1.4 µm is ambient IR-C. The black-body radiant
exitance at 273 K (0 °C) is 32 mW/cm2; at 300 K (27.2 °C), it is 46
mW/cm2. A whole-body irradiance of 20 - 50 mW/cm2 from radiant
warmers on a cold (0 °C) winter day is comfortable; but the same
irradiance on a hot summer day could bring on heat stress.
Therefore any IR safety standard should distinguish between all the
IR bands, and IR-C limits would have to vary with ambient
conditions.
12. RISK EVALUATION
There are three broad areas of concern for any potentially
hazardous optical source: (a) the potential of the source for
causing personal injury; (b) the environment in which the laser or
optical source is used; and (c) the individuals who operate and
those who are potentially at risk from exposure to the emitted
optical radiation. For both lasers and lamp systems, it is
possible to develop a hazard classification scheme that would
greatly assist the health and safety professional in evaluating the
risk from an optical source in a particular environment (Anderson,
1980a).
It is important to understand that the laser classification
system was developed to aid the user in establishing a safety
programme for a particular laser device to relieve the user and
also the health and safety professional of the burden of detailed
and often complex measurements or calculations. The unique risks
and control measures applicable to specific environments depend on
the personnel potentially exposed and vary with each laser
application. However, fortunately, many of the protection measures
depend entirely, or to a great extent, on the laser hazard
classification.
Since the control measures required for Class 1 and Class 2
laser systems are minimal or nonexistent for the user, it is the
applications of Class 3 and Class 4 lasers that require careful
study of the risks, and the development of detailed control
measures. There are several protective methods, which can apply to
a Class 3 or a Class 4 laser product. The total enclosure of the
source is certainly the most desirable control measure. However,
since total enclosure with proper interlocks would result in a
Class 1 laser product, there is normally a reason why a laser
system was not originally designed as a Class 1 device. There are
a few instances where a specific enclosure must be developed for
each application. Where the enclosure approach is feasible, this
solution is strongly recommended.
Where the laser beam is operated without being enclosed -
either indoors or out-of-doors - the laser safety officer (a health
or safety professional or other special trained individual) has
great need of reference material and technical data. These data
include the reflective properties of materials found in the
environment, attenuating properties of filters, windows, or other
enclosures, and a working knowledge of several aspects of optical
systems.
Several system-safety items should be considered for
incorporation in laser system design, including:
beam attenuators;
interlocks;
manual switches;
the enclosure;
emission indicators;
accidental laser firing;
beam diffusers;
multiple wavelengths;
mode locking;
beam hotspots.
12.1. Laser Hazard Classification
For the classification of a laser, the following variables
concerned with output should be known: (a) the wavelength or
wavelength range; (b) the classification duration (i.e., in the
ANSI standard: how long is it possible for a person to be exposed
to an applicable EL); (c) average power output (for cw or
repetitively-pulsed lasers); and (d) total energy per pulse (or
peak power, pulse duration, PRF, and emergent beam radiant
exposures) for all pulsed lasers. The laser source radiance or
integrated radiance and the maximum viewing angular subtense is
required, if the source is an extended laser source and is
operating in the retinal hazard region (400 - 1400 nm).
If the laser is modified, after manufacture, in a way that
could affect the hazard classification, then the user or the
individual performing the modification should reclassify the
modified system.
12.2. Environmental Considerations including Reflection and the
Probability of Exposure
Environmental considerations probably play a greater role in
determining the control measures for Class 3 and Class 4 laser
systems, and these can only be evaluated by the user. These
environmental considerations include the possibility of reflections
(Gorodetski et al., 1968).
12.2.1. Reflections
The three general types of reflection that may be encountered
in many environments are shown in Fig. 28. Diffuse reflections
normally greatly reduce the hazards of the primary beam, though,
for Class 4 visible and near-infrared lasers, hazardous diffuse
reflections are likely (Komorova et al., 1978). The dividing line
between Class 3 and Class 4 visible and IR-A lasers is defined by
diffusely reflective hazard conditions. Reflections from flat
mirrors produce substantial risks of hazardous exposure at
considerable distances from the reflector as can be seen in
Fig. 28. Where random orientation of the reflectors can occur, the
potentialy hazardous area can be quite large. Curved surface
specular reflections,on the other hand, are normally hazardous only
at relatively short distances of the order of magnitude of the
radius of curvature from the reflector surface. Though specular
surfaces are of greatest concern in open laboratory situations,
they are not unheard of in the outdoor use of lasers and in medical
applications.
Table 12. Relative spectral
effectiveness for selected wavelengths
--------------------------------------
Relative
spectral
Wavelength Elambda effectiveness
(nm) (mJ/cm2) Slambda
--------------------------------------
200 100 0.03
210 40 0.075
220 25 0.12
230 16 0.19
240 10 0.30
250 7.0 0.43
254 6.0 0.5
260 4.6 0.65
270 3.0 1.0
280 3.4 0.88
290 4.7 0.64
300 10 0.30
305 50 0.06
310 200 0.015
315 1000 0.003
--------------------------------------
Table 13. ACGIH ultraviolet exposure limits
--------------------------------------------
Duration of exposure Effective irradiance,
per day Eeff (µW/cm2)
--------------------------------------------
8 h 0.1
4 h 0.2
2 h 0.4
1 h 0.8
30 min 1.7
15 min 3.3
10 min 5
5 min 10
1 min 50
30 s 100
10 s 300
1 s 3000
0.5 s 6000
0.1 s 30 000
--------------------------------------------
All the preceding ELs for ultraviolet energy apply to sources
that subtend an angle less than 80°. Sources that subtend a
greater angle need to be measured only over an angle of 80°.
ACGIH recommended values: The threshold limit values for
occupational exposure to UVR incident on skin or eye, where
irradiance values are known and exposure time is controlled, are as
follows:
1. For the near ultraviolet spectral region (320-400 nm),
total irradiance incident on the unprotected skin or eye
should not exceed 1 mW/cm2 for periods greater than 103 s
(approximately 16 min) and for exposure times less than
103 s should not exceed one J/cm2.
2. For the actinic ultraviolet spectral region (200-315 nm),
radiant exposure incident on the unprotected skin or eye
should not exceed the values given in Table 10, within an
8-h period.
3. To determine the effective irradiance of a broad-band
source weighted against the peak of the spectral
effectiveness curve (270 nm), the following weighting
formula should be used:
Eeff = SIGMA Elambda Slambda delta lambda where:
Eeff = effective irradiance relative to a monochromatic
source at 270 nm in W/cm2 (J/s/cm2)
Elambda = spectral irradiance in W/cm2/nm
Slambda = relative spectral effectiveness (unitless)
delta lambda = band width (nm)
4. Permissible exposure time in seconds for exposure to
actinic ultraviolet radiation incident on the unprotected
skin or eye may be computed by dividing 0.003 J/cm2 by
Eeff in W/cm2. The exposure time may also be determined
using Table 13, which provides exposure times
corresponding to effective irradiances in µW/cm2.
Conditioned (tanned) individuals can tolerate skin exposure in
excess of the TLV without erythemal effects. However, such
conditioning may not protect persons against skin cancer.
For the UV-A, ACGIH considered it reasonable to propose a
guideline for ocular exposure so low that no conceivable thermal or
photochemical injury mechanisms were likely to be demonstrated. To
prevent thermal injury, it was assumed that, for exposure durations
of less than 100 s, the eye should be protected against exposures
above 10 kJ/m2 (1 J/cm2). Because of the lack of adverse effects
reported in individuals working with ultraviolet "black light"
sources at levels of 1 mW/cm2 (or above), it was presumed that a
level of 1 mW/cm2, the approximate level of exposure of the eye to
UVA-A in outdoor reflected sunlight, would be a reasonable upper
limit for exposures lasting 1000 s or more. The skin exposure limit
could presumably be increased by a factor of 5 for the longer
exposure durations. To avoid thermal effects at very short
exposure durations, the total UVR corneal irradiance was also
limited to 1 W/cm2. It is now known that photochemical effects
occur in both the eye and skin and that total daily doses of 20 -
100 J/cm2 cause acute corneal opacities (Pitts et al., 1977;
Zuchlich & Kurtin, 1977) and skin erythema from the UV-A (Parrish
et al., 1978). Hence, these UV-A criteria must be applied with
great caution for conditions of very long (exceeding 4 h) exposure.
11.8.2.3. Retinal health criteria
Laser protection standards incorporate several simplifications
that depend on the single-wavelength and point-source
characteristics of the laser. These standards may provide a too
conservative estimate of the real risk, if laser criteria are
applied to broad-band sources. No official standards exist for the
retinal risk evaluation of a broad-band source. Tentative
guidelines exist from ACGIH. To use these guidelines, both a blue-
light hazard function B lambda and a retinal thermal injury
function R lambda must be used. The source spectrum may be weighted
to indicate comparative levels of risk from the two types of
retinal injury mechanisms. Using equation 13 (section 8.4.1.3), in
which the retinal irradiance Er is directly proportional to the
radiance L of the source, the square of the pupil diameter dp, and
the transmission t of the ocular media. The retinal spectral
irradiance distribution can be calculated from the spectral
radiance distribution Llambda and knowledge of the spectral
transmission of the ocular media taulambda. In the absence of a
radiance standard, this approach can be used to calculate retinal
levels directly and to compare them directly with thresholds of
injury (Sliney & Freasier, 1973). However, the present approach is
to establish ELs for the spectrally weighted radiances. These
safety weighting functions are given in Table 14. Spectral factors
weighted against the spectral radiance are then applied as shown in
sections 11.8.2.4 and 11.8.2.5.
Table 14. Spectral weighting functions for assessing
retinal risks from broad-band optical sourcesa
-------------------------------------------------------
Blue-light Thermal
Wavelength hazard function hazard function
(nm) Blambda Rlambda
-------------------------------------------------------
400 0.10 1.0
405 0.20 2.0
410 0.40 4.0
415 0.80 8.0
420 0.90 9.0
425 0.95 9.5
430 0.98 9.8
435 1.0 10
440 1.0 10
445 0.97 9.7
450 0.94 9.4
455 0.90 9.0
460 0.80 8.0
465 0.70 7.0
470 0.62 6.2
475 0.55 5.5
-------------------------------------------------------
Table 14 (contd.)
-------------------------------------------------------
Blue-light Thermal
Wavelength hazard function hazard function
(nm) Blambda Rlambda
-------------------------------------------------------
480 0.45 4.5
485 0.40 4.0
490 0.22 2.2
495 0.16 1.6
500-600 10[(450-lambda)/50] 1.0
600-700 0.001 1.0
700-1049 0.001 10[(700-lambda)/500]
1050-1400 0.001 0.2
-------------------------------------------------------
a From: ACGIH (1981).
11.8.2.4. Retinal thermal risk evaluation
To protect against thermal retinal injury from short-term
exposures, the spectral radiance of the lamp weighted against the
function Rlambda (Table 14) should not exceed:
1400
SIGMA Llambda Rlambda delta lambda L(Haz) = ´ t/(alpha t) W/(cm2 x sr)
400 Equation (15)
where Llambda is given in W/(cm2 x sr), t is the viewing duration
(or pulse duration if the lamp is pulse limited) which is limited
to 1 ms - 10 s, and alpha is the angular subtense of the source in
radians. The angle alpha should be limited to approximately 0.1
radian. If the lamp is oblong, alpha refers to the longest
dimension (1) that can be viewed. For instance, at a viewing
distance (r) of 500 cm from a tubular lamp 50 cm long, the viewing
angle alpha is 1/r or 0.1 rad. Spectral radiance (Llambda)
measurements must be made at frequent wavelength intervals (delta
lambda) to preclude serious error. The delta lambda should be less
than 5 nm in the UV and blue end of the visible spectrum.
11.8.2.5. Retinal blue-light risk evaluation
To protect against retinal injury from blue-light exposure, the
integrated spectral radiance of the lamp weighted with the blue-
light hazard function (Blambda of Table 14) should not exceed 100
J/cm2 x sr for a duration of less that 104 or exceed 10 mW/(cm2 x
sr) for t > 104 s:
1400
SIGMA Llambda x t x Blambda x delta lambda < 100 J/(cm2 x sr) for t < 104 s
400 Equation (16)
or
1400
SIGMA Llambda x Blambda x delta lambda < 10 W/(cm2 x sr) for t > 104 s
400 Equation (17)
and for a point source (alpha < 11 mrad)
1400
SIGMA Elambda x t x Blambda x delta lambda < H(Haz) = 10 mJ/cm2 for t < 104 s
400 Equation (18)
or
1400
SIGMA Elambda x Blambda x delta lambda < E(Haz) = 1 µW/cm2 for t > 104 s
400 Equation (19)
These levels assume a constricted pupil, as would occur with
fixed viewing of any type of extended source with a radiance
approaching the EL. For a spectrally weighted source radiance (L)
that exceeds 10 mW/(cm2 x sr) in the blue-light spectral region,
the permissible exposure duration tmax in s is simply:
1400
tmax = 100 J/(cm2 x sr) / SIGMA Llambda x Blambda x delta lambda for t < 104 s
400 Equation (20)
The extended-source limits are greater than the 198. ELs for a
440-nm laser radiation source given by either ANSI or ACGIH, which
assume a 7-mm pupil rather than the 3-mm used for the broad-band
source analysis.
11.8.2.6. IR-A risk analysis
The proposed ACGIH EL also limited the IR-A and IR-B infrared
radiation beyond 770 nm to 10 mW/cm2 to avoid possible
cataractogenesis (the appearance of which may be delayed). For an
infrared heat lamp or other source that lacks a strong visual
stimulus, the radiance for wavelengths between 700 and 1400 nm for
long-term viewing should be limited to:
1400
SIGMA Llambda x delta lambda < L(Haz) = [0.6/alpha] W/(cm2 x sr)
700 Equation (21)
This limit is also based on a 7-mm pupil diameter.
NOTE: Equations 16 to 21 are empirical and are not, strictly
speaking, dimensionally correct. To make these formulae
correct, a dimensional correction factor must be inserted
into each formula. It is, therefore, important to use only
the units specified.
11.8.3. Infrared standards
There are no established non-laser, infrared (IR) health
standards. However, the laser ELs can be applied for broad-band
sources, if, in addition, the whole-body irradiation is evaluated.
Even irradiances as low as 100 W/m2 (10 mW/cm2) can place an
uncomfortable thermal load on the human body, especially when the
irradiation is not confined to one side of the body and this
radiant heat load occurs along with high ambient air temperatures.
In contrast, the IR laser EL for periods exceeding 10 s is 1 kW/m2
(100 mW/cm2), assuming that the total irradiated area of the skin
or the eye will be small. For laser exposure the irradiated area
is generally small, but this is not so likely when the body is
exposed to optical radiation from non-laser sources; and heat
stress must be evaluated.
The determination of the wet-bulb-globe-temperature (WBGT)
index requires a combination of a dry-bulb temperature with a wet-
bulb (WB) temperature (which involves humidity, air movement, etc.)
and a black-globe (BG) temperature (which includes the radiant
(predominantly infrared) contribution). These three temperatures
are weighted differently in two equations used for evaluating heat
stress - one for outdoor workers exposed to sunlight, another for
indoor workers exposed to infrared sources. The nature of the
skin's reflectance is such that much of the visible and IR-A are
reflected, whereas IR-B and IR-C are almost totally absorbed. The
spectral reflectance of most clothing is somewhat similar to that
of skin in the infrared. Obviously the second formula would be
used in any IR risk evaluation. The ACGIH formula for indoor heat
stress is:
WBGT = 0.7 WB + 0.3 GT Equation (22)
A heat-stress condition exists when this WBGT value exceeds 25 -
30 °C depending on work load.
A major problem in any infrared safety standard concerned with
wavelengths beyond 1.4 µm is ambient IR-C. The black-body radiant
exitance at 273 K (0 °C) is 32 mW/cm2; at 300 K (27.2 °C), it is 46
mW/cm2. A whole-body irradiance of 20 - 50 mW/cm2 from radiant
warmers on a cold (0 °C) winter day is comfortable; but the same
irradiance on a hot summer day could bring on heat stress.
Therefore any IR safety standard should distinguish between all the
IR bands, and IR-C limits would have to vary with ambient
conditions.
12. RISK EVALUATION
There are three broad areas of concern for any potentially
hazardous optical source: (a) the potential of the source for
causing personal injury; (b) the environment in which the laser or
optical source is used; and (c) the individuals who operate and
those who are potentially at risk from exposure to the emitted
optical radiation. For both lasers and lamp systems, it is
possible to develop a hazard classification scheme that would
greatly assist the health and safety professional in evaluating the
risk from an optical source in a particular environment (Anderson,
1980a).
It is important to understand that the laser classification
system was developed to aid the user in establishing a safety
programme for a particular laser device to relieve the user and
also the health and safety professional of the burden of detailed
and often complex measurements or calculations. The unique risks
and control measures applicable to specific environments depend on
the personnel potentially exposed and vary with each laser
application. However, fortunately, many of the protection measures
depend entirely, or to a great extent, on the laser hazard
classification.
Since the control measures required for Class 1 and Class 2
laser systems are minimal or nonexistent for the user, it is the
applications of Class 3 and Class 4 lasers that require careful
study of the risks, and the development of detailed control
measures. There are several protective methods, which can apply to
a Class 3 or a Class 4 laser product. The total enclosure of the
source is certainly the most desirable control measure. However,
since total enclosure with proper interlocks would result in a
Class 1 laser product, there is normally a reason why a laser
system was not originally designed as a Class 1 device. There are
a few instances where a specific enclosure must be developed for
each application. Where the enclosure approach is feasible, this
solution is strongly recommended.
Where the laser beam is operated without being enclosed -
either indoors or out-of-doors - the laser safety officer (a health
or safety professional or other special trained individual) has
great need of reference material and technical data. These data
include the reflective properties of materials found in the
environment, attenuating properties of filters, windows, or other
enclosures, and a working knowledge of several aspects of optical
systems.
Several system-safety items should be considered for
incorporation in laser system design, including:
beam attenuators;
interlocks;
manual switches;
the enclosure;
emission indicators;
accidental laser firing;
beam diffusers;
multiple wavelengths;
mode locking;
beam hotspots.
12.1. Laser Hazard Classification
For the classification of a laser, the following variables
concerned with output should be known: (a) the wavelength or
wavelength range; (b) the classification duration (i.e., in the
ANSI standard: how long is it possible for a person to be exposed
to an applicable EL); (c) average power output (for cw or
repetitively-pulsed lasers); and (d) total energy per pulse (or
peak power, pulse duration, PRF, and emergent beam radiant
exposures) for all pulsed lasers. The laser source radiance or
integrated radiance and the maximum viewing angular subtense is
required, if the source is an extended laser source and is
operating in the retinal hazard region (400 - 1400 nm).
If the laser is modified, after manufacture, in a way that
could affect the hazard classification, then the user or the
individual performing the modification should reclassify the
modified system.
12.2. Environmental Considerations including Reflection and the
Probability of Exposure
Environmental considerations probably play a greater role in
determining the control measures for Class 3 and Class 4 laser
systems, and these can only be evaluated by the user. These
environmental considerations include the possibility of reflections
(Gorodetski et al., 1968).
12.2.1. Reflections
The three general types of reflection that may be encountered
in many environments are shown in Fig. 28. Diffuse reflections
normally greatly reduce the hazards of the primary beam, though,
for Class 4 visible and near-infrared lasers, hazardous diffuse
reflections are likely (Komorova et al., 1978). The dividing line
between Class 3 and Class 4 visible and IR-A lasers is defined by
diffusely reflective hazard conditions. Reflections from flat
mirrors produce substantial risks of hazardous exposure at
considerable distances from the reflector as can be seen in
Fig. 28. Where random orientation of the reflectors can occur, the
potentialy hazardous area can be quite large. Curved surface
specular reflections,on the other hand, are normally hazardous only
at relatively short distances of the order of magnitude of the
radius of curvature from the reflector surface. Though specular
surfaces are of greatest concern in open laboratory situations,
they are not unheard of in the outdoor use of lasers and in medical
applications.
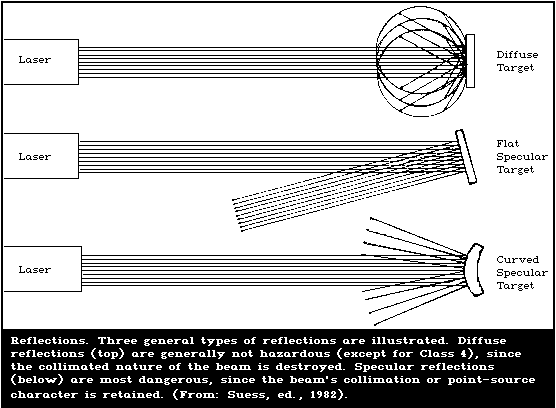 Absolute values of spectral reflectance are relatively
unimportant because such values vary only by a factor of 10 - 20,
whereas the laser beam irradiance may exceed the applicable EL by
orders of magnitude above this factor.
Most reported laser accidents have occurred, when the
probability of exposure was very high. No discussion of reflection
hazards is therefore complete without the consideration of the
probability of exposure. It must be remembered that the underlying
philosophy of the classification system is that control measures
should increase with increasing risk of exposure as well as with
increased severity of exposure.
12.2.2. Retroreflection
Some materials exhibit a property known as retrodirective
reflection. The reflection does not obey either the law of regular
(specular) reflection, or the cosine dependence of Lambertian
reflection. A collimated indigent beam may remain collimated and
be redirected along the original axis of propagation, regardless of
the angle of incidence at the retroflector. Corner cubes and some
specialized highway signs are examples of retroflectors.
12.2.3. Optically aided viewing
Nearly all laser workers know that viewing a laser source with
a telescope may substantially increase the risk. This increase in
risk is most dramatic for intra-beam viewing of a collimated
source. In this case, an increase in the power entering the eye is
possible, because the diameter of the objective (Do) of the
telescope or binocular is much larger than the pupil of the eye dp.
The actual increase in risk (G) depends on whether the pupil of the
eye is larger or smaller than the exit pupil (De) of the optical
system, the spectral transmittance (taulambda) of the optical
system at the laser wavelength(s), and the beam diameter relative
to the objective (collecting aperture) diameter.
When a bright object, larger than a point source, is viewed
through a well-designed optical system, the radiant power reaching
the retina (visible and IR-A) is theoretically increased by the
square of the instrument's magnifying power. However, since there
is a commensurate increase in the area of the retinal image, the
retinal irradiance remains unchanged, except for a slight reduction
because of reflective loss and the absorption of light in the
optical system. The retinal hazard in this case may increase in
some instances, since the thermal retinal injury threshold
decreases with increasing image size.
13. ACCIDENTAL INJURIES
At present, retinal injuries with loss of sight following
exposure to visible and IR-A laser radiation have been the most
catastrophic of all effects from laser radiation (Boldry et al.,
1981; Zhokov, 1981). Though the relatively high-powered, far-
infrared lasers such as the cw, carbon-dioxide laser, have caused
numerous burns to the hands and clothes, these are considered
inconsequential in comparison with the serious retinal injuries.
One postal survey conducted several years ago (Rockwell & Goldman,
1974) appeared to indicate that there had been at least 100
injuries to the eye from laser radiation in the USA. One
subjective account in this regard was that of Decker (1977).
Despite such reports, surprisingly few serious injuries of the
eye have been reported in the last 15 years in relation to exposure
to pulsed lasers. This low accident rate cannot be accounted for
by assuming that the ocular ELs are too conservative. The
explanation is probably that accidental exposure of the eye to a
collimated beam is normally an extremely remote possibility, if
precautions are taken to keep the eye out of the beam. One of the
few situations in which the probability of hazardous exposure is
great is during work in the laboratory and, each year, several
retinal injuries are reported under these conditions. However, it
is difficult to ascertain the exposure conditions in sufficient
detail for useful threshold or injury data to be derived. Concern
may also exist regarding the potential bias in an individual's
description of the accidental exposure conditions to support a
claim of compliance with safety measures. It is not clear whether
laser exposures are always detected by the exposed individual, and
this may be a particular problem with IR lasers (Kasuba & Akifev,
1977). It is known that retinal injury outside the macula may have
little or no effect on everyday visual performance and therefore
may not be detected subjectively.
14. CONTROL MEASURES
Risk control guidelines are not mutually exclusive. Following
one or two guidelines may reduce the risk to such an extent that
other recommended control measures, in that particular class, are
no longer essential. For example, if the beam path of a Class 4
laser were enclosed, then it would hardly be necessary to remove
all glass objects, or other specular surfaces near the beam path
but outside the enclosure, nor would it seem necessary to wear eye
protectors. However, the eye protection might be necessary if the
enclosure were being modified or during initial alignment. The
decision to use any particular set of controls depends on use
conditions and whether general population exposure is likely.
Table 15 provides a brief list of the most commonly recommended
laser control measures.
Table 15. Control measures for general population and occupational
exposure
-------------------------------------------------------------------
I Engineering control measures:
protective housing enclosure and service panel requirements;
interlocks on the protective housing;
door interlocks and remote control connector;
beam attenuator or beam shutter;
key switch or padlock over aperture cover;
filtered viewing optics and windows;
emission delay (BRH);
warning lights;
emission indicators (audible or visible);
enclosed area or room;
beam enclosure;
remote firing and/or monitoring;
II Personal protective equipment:
eyewear;
clothing;
gloves;
III Administrative and procedural controls:
laser safety officer;
standard operating procedures (SOPs);
limitations on use by class;
education and training;
maintenance and servicing manuals;
marking of protective devices;
warning signs and labels;
entry limitations for visitors, etc.;
accident procedures.
-------------------------------------------------------------------
Because of the risk associated with exposure to Class 4 high-
risk lasers, the safety precautions associated with these laser
installations indoors, generally include the installation of door
interlocks to prevent exposure of unauthorized or transient
personnel entering the laboratory, the use of baffles to terminate
the primary and any secondary beams, and the use of safety eyewear
by personnel within the interlocked facility (Klost, 1971).
At one time, it was recommended that ambient light levels
should be sufficient to constrict pupils. However, since a
constricted pupil provides only a small safety factor, the
requirement for good illumination, which remains in present safety
standards, is related to good general visibility, as the wearing of
eye protectors reduces visual capabilities. Light-coloured, matt
surfaces in the room minimize glare, and thus promote visibility.
In summary, the ability to analyse potential risks from any
laser system is enhanced by a broad knowledge of optics, general
laser technology, and the imaging process of the human eye. A
laser safety specialist should have a general background knowledge
of optics with the basic knowledge necessary to perform a risk
analysis. It has been shown that the risk analysis depends on at
least three aspects - the laser system and its potential hazards,
the type of personnel who may be exposed, and, finally, the
reflective materials and other optically important materials in the
environment that can influence the risk analysis.
15. HAZARDS OF LAMP SOURCES AND PROJECTION SYSTEMS
The optical radiation emitted by a conventional light source,
either a bare lamp, a luminaire, or a projection system, can be
evaluated using the previously mentioned tentative exposure limits
or guidelines.
Prior to exhaustive measurements and safety calculations, it
may be worthwhile to determine the need for a comprehensive risk
evaluation. Many categories of lamps or other types of light
sources can be excluded from all or several of the evaluations.
The following multi-step scheme (Sliney & Wolbarsht, 1980) may be
useful in this regard.
STEP 1 - Categorization of the lamp. Certain hazards are specific
for certain types of lamp or light source. The following grouping
is useful:
(a) incandescent lamps and incandescent heating sources;
(b) low-pressure discharge lamps;
(c) fluorescent lamps;
(d) high-intensity discharge (HID) lamps;
(e) short-arc (compact arc) lamps;
(f) carbon arcs;
(g) solid-state sources (LEDs etc.);
(h) cathode-ray tubes (CRTs).
STEP 2 - Determination of the source envelope. Any glass between
the actual source of radiation (e.g., the arc or tungsten filament)
and the point of access can greatly influence the potential hazard.
Soft (lime) glass of any reasonable thickness will greatly
attenuate UV-B and UV-C radiation.
(a) Incandescent lamps, other than quartz-halide lamps,
normally have a sufficiently thick glass envelope to
completely preclude a UVR hazard. The blue-light
hazard does not appear to be theoretically possible
at black-body temperatures below 2000 K (Sliney &
Wolbarsht, 1980), but most filaments operate at
effective temperatures exceeding 2000 K.
(b) Low-pressure discharge lamps. Low-pressure discharge
lamps do not normally present a retinal hazard,
because of the relatively low radiance. Only lamps
with quartz envelopes can transmit sufficient UV-B
and UV-C to be of concern. Of the common low-pressure
lamps, only mercury lamps can create a severe UVR
hazard. Many may be quite hot to the touch.
(c) Fluorescent lamps. Low-pressure tubular lamps in
almost all cases have a thin glass envelope, but
could often present a potential UVR hazard at the
surface. They do not represent a thermal retinal
injury hazard and seldom a blue-light hazard.
(d) HID lamps. These lamps may present both blue-light
and thermal retinal hazards, and possible UVR
hazards. Since most lamp envelopes are glass, there
is little UV-B leakage. Nevertheless, the UV-B
leakage may be of concern at very short distances.
Quartz-mercury HID lamps require a UVR risk
evaluation. If the outer glass envelope of an HID
lamp breaks, hazardous UV levels will be emitted.
Governmental regulations in Canada and the USA
require HID lamps to have a self-extinguishing
feature to preclude this hazard, unless the packaging
clearly warns against use without adequate shielding.
(e) Short-arc lamps. Of all the electric lamp categories,
this group will require the most extensive risk
evaluation. All potential hazards may be present
(UV-B/C, UV-A, blue-light, retinal thermal injury,
and skin thermal injury). Because of the high
temperature of the arc, a quartz envelope (which
transmits UV-B and C) is characteristic. These lamps
are often used in UV photocuring processes in
industry (Moss, 1980).
(f) Carbon arcs. Where a glass lens or filter plate does
not exist between the open arc and a point of access,
the carbon arc, like the short-arc lamp, is
potentially injurious.
(g) Solid-state lamps (e.g., LEDs). The present solid-
state lamps including LEDs, which emit visible
radiation, do not present any health risk, regardless
of the type of envelope.
(h) Cathode-ray tubes (CRTs). Present CRTs emit optical
radiation at levels that could pose a potential
health hazard (Wolbarsht et al., 1980).
STEP 3 - The obtaining of available manufacturers' radiometric and
photometric data and lamp descriptions. Any radiometric or
photometric specification may be of value either for calculation or
for direct intercomparison with measurements. Spectral data are
most useful. The dimensions of the emitting area of the lamp will
be required for retinal hazard evaluation.
STEP 4 - Comparison of lamp specifications with those of previously
evaluated lamps. From experience, it is often possible to complete
the risk evaluation with this step.
STEP 5 - Performance of detailed spectroradiometric measurements,
when necessary. In addition, where feasible, measurements of
luminance, illuminance, and total irradiance should be performed.
These will provide confirmation of the spectroradiometric
measurements. The pulse duration must be measured for a pulsed
source.
STEP 6 - Determination of the source dimensions. A photograph and
microdensitometer scan of the negative may be necessary for a non-
uniform source. The maximum angular subtense alpha of the source
should be calculated at the point of human access or at 15 cm from
the source, whichever is closer.
STEP 7 - Estimation of the exposure and comparison with the
exposure limits to determine the degree of risk.
STEP 8 - Consideration of potentially hazardous failure modes. For
example, breakage of the outer envelope of some high-intensity
discharge (HID) lamps can create a serious UVR hazard (Anderson,
1980b).
16. PROJECTION OPTICS
Broad-band sources involving projection optics are most
difficult to evaluate. Besides the problems encountered in
evaluating exposed lamps, the projected beam and projected source
size must be characterized. When viewing a collimated light source
from within the beam (other than a laser), a magnified view of the
actual source will be seen. The source is generally a high-
brightness lamp. The brighter the lamp, the greater the maximal
irradiance in the projected beam. This is a consequence of the Law
of Conservation of Brightness (Radiance) (see, for example, Kline,
1970; or Sliney & Wolbarsht, 1980). Some usually safe lamps become
hazardous to view through projection optics, despite the fact that
the optics cannot make the lamp brighter. The risk increases
because of the dependence of retinal injury on image size. Besides
the obvious projection sources - such as spotlights, searchlights,
slide projectors, and film projectors - solar concentrators and
other non-imaging light collectors may also require risk
evaluation. From the Law of Conservation of Radiance, it is
possible to evaluate the retinal risks from projector systems.
Collimating optics may consist of refracting elements (lenses),
reflecting elements (curved mirrors), or both.
17. SAFETY GUIDELINES FOR HIGH-INTENSITY SOURCES
Since lamp or arc sources may be hazardous from several
aspects, it may be helpful to develop a safety classification
scheme, similar to the one applied to laser products. The
following scheme of Sliney & Wolbarsht (1980) illustrates this
approach to evaluate the retinal risks from projector systems.
Both lamps and total lighting systems could be included. The
categories could be as follows:
Safety Group 1: Safe sources. These lamps are considered
safe to view throughout the day. No warning label would be
required. Examples: a frosted 15-W filament lamp or a
TV-display, cathode-ray tube.
Safety Group 2: Low-risk sources. These lamps are safe
for momentary 0.25-s, unintentional viewing. Examples:
most spotlights and film-projector lamp bulbs. A caution
label should be required on the lamp base, and possibly on
the projection system itself. No ultraviolet or infrared
hazard would exist at distances of more than 10 cm from
the lamp or projected beam.
Safety Group 3: Moderate-risk sources. These lamps would
be unsafe to view at close range, even momentarily.
Presumably, skin injury could also occur from ultraviolet
radiation as from germicidal lamps, sun lamps, and high
intensity UV-A lamps. A danger-label, clearly visible on
the equipment, could be required. A common lamp that might
fit into this category would be a 600-1000-W tungsten-
halogen lamp without a Fresnel lens, such as is used for a
home cine film spot lamp. The emergent beam irradiance is
far in excess of that required to ignite paper within half
a metre of the source. Obviously, the basis for the
determination of a hazard classification would differ
according to whether the hazard classification criteria
were based on retinal or skin injury. Each measurement for
classification would be for a specified accessible
approach distance, using a standard aperture and solid
angle of acceptance. The minimum approach distance could
vary with application. Other examples that might be
included in this category are some very high intensity,
short-pulse, laser flash tubes, and 20 kW xenon-arc
searchlights.
Safety Group 4: High-risk sources. These sources would
cause skin burns and/or erythema within a standardized
period of exposure (e.g., within 10 s) at a standardized
distance at which the effective UV irradiance would exceed
3 W/m2 (0.3 mW/cm2), or the total irradiance across the
entire spectrum would exceed 2 kW/m2 (0.2 W/cm2). Examples
of such sources are an open carbon-arc spotlight or an
open 1-kW mercury lamp. It may be that safety groups 3 and
4 are so similar in degree of risk, that they could be
combined.
18. WELDING ARCS
The most common high-intensity arc is probably the welding arc.
These arcs vary in brightness and in UVR content, primarily
according to the arc current, type of shielding gas, and the metals
being welded.
The greatest population exposed to intense sources of optical
radiation are welders and their assistants. The American Welding
Society estimated that there may be as many as 500 000 welders in
the USA alone (Emmett & Horstman, 1976). The two broad categories
of welding equipment are gas (acetylene) welding equipment and
electric-arc welding equipment. A gas welding torch or cutting
torch has a luminance not much greater than a candle flame,
typically ranging from 10 to 200 kcd/m2 (1-20 cd/cm2), and the UVR
emission is quite small. The optical radiation hazards of such
torches are virtually nonexistant. Welding filter goggles used
with such torches are to reduce glare, and are little darker than
very dark sunglasses having a shade number of the order of 3 - 5
(visual transmittance of 5 - 15 %). On the other hand, electric
welding arcs may be 1000 times brighter than gas torches and emit
UVR at proportionately higher levels (Sutter et al., 1972).
Protective shields, curtains, screens for bystanders, and
welders' goggles are the standard protective equipment used in
welding (Mayer et al., 1979; Sliney et al., 1981). Protective
procedures and protective equipment for the welder have been
developed empirically over the last three-quarters of a century.
Only very recently have detailed measurements of the radiometric
output of welding arcs been available. When these measurements
were carefully compared with exposure limits being developed for
protection against bright light sources, it was shown that the
empirically-developed protective equipment standards were adequate.
19. EYE AND SKIN PROTECTION
19.1. Laser Safety Eyewear
From a safety point of view, the most desirable laser hazard
control measure is complete enclosure of the laser or laser system;
however, this may not always be practical and laser eye protectors
are generally the best alternative. Though most industrial laser
applications do not require the use of eye protectors, this is not
always true for laser applications in the research laboratory. Eye
protectors provide the simplest solution to the laser safety
problem for a constantly changing experimental arrangement. Several
factors play a role in determining whether eyewear is necessary in
any situation. At least three output parameters of the laser must
be known: maximum exposure duration, wavelength, and output power
(or output irradiance, or radiant exposure, or energy), as well as
the applicable safe corneal radiant exposure. In addition, some
knowledge of such environmental factors as ambient lighting and the
nature of the laser operation may also be required.
Laser eye protection generally consists of a filter (often
composed of several individual filter plates) which selectively
attenuates at specific laser wavelengths, but elsewhere transmits
as much visible radiation as possible (Swope & Koester, 1965;
Schreibeis, 1968; Scherr et al., 1969; Swope, 1969, 1970; Straub,
1970; Sliney, 1974). Eyewear is available in several designs -
spectacles, coverall types with opaque side-shields, and coverall
types with somewhat transparent filter side-shields. The selection
of appropriate laser protective eyewear may be complex (Envall &
Murray, 1979). Active electronic imaging devices have also served
an additional role, as eye protection.
19.2. Welders' Filters
Eye protection filters, which were originally developed for
welders, were based more on available materials than on knowledge
of ocular protection requirements. The first organized study of
glass filter materials was carried out by Sir William Crookes
(1914) in England. Optical transmission characteristics are now
standardized as "shades" and specified for particular applications
(Coblentz et al., 1931; Stair, 1948; ANSI, 1978). Though maximum
transmittances for ultraviolet and infrared radiation are specified
for each shade, the mean photopic visual transmittance tauv, or
visual optical density Dv, has traditionally been used to define
the shade number S:
S = (7/3) Dv + 1 = - ln tauv + 1 Equation (23)
or Dv = (3/7) (S - 1) Equation (24)
where Dv = -log10 tauv Equation (25)
19.3 Eye Protection for Furnace Radiation
As well as protective clothing and equipment, many industrial
methods now used probably reduce the level of glass furnace
radiation to which the eye is exposed. For instance, the openings
to higher temperature furnaces are a great deal smaller than they
have been in past years; this would reduce the total irradiance of
the eye from infrared radiation. There are sufficient data and
cases of a very specific form of cataract in workers to suggest
that infrared does, indeed, cause glass-blower's or furnaceman's
cataract (Duke-Elder, 1972).
19.4. Eye Protection Filters for Solar Radiation
Direct viewing of the sun, for whatever reason, requires
protection against several different portions of the spectrum. A
yellowish or reddish filter generally protects against ultraviolet
radiation. Protection against intense visible rays should be
weighted to filter out more of the blue-light than the rest of the
visible spectrum. It is generally found that a shade 12 or 13
welder's filter is quite adequate to protect against ultraviolet
radiation, infrared, and visible radiation. The protection
afforded against the IR, however, is far greater than necessary.
The use of darkened coloured slides is not advisable, since
these slides (usually made by developing unexposed colour film) use
organic dyes that transmit in the near-infrared (IR-A) spectral
band.
19.5. Skin Protecting Agents for UVR (Sunscreens)
A number of topical, physical, and chemical screening agents
have been developed that provide nearly total or partial filtration
of ultraviolet radiation. Since actinic UV-B and UV-C radiation
are the most hazardous, efforts to develop topical agents have
concentrated primarily on filtering out this type of radiation. The
chemical agents in these "sunscreens" include para-aminobenzoic
acids (PABA) and its esters, salicylates, and cyanamates. These
materials are mixed in solution with substances that have good
substantivity (i.e., adhere to the skin) (Dahling et al., 1970;
Fitzpatrick et al., 1974).
19.6. Protective Garments
Aluminized fabrics were greatly improved during various manned
space programmes (Stoll & Chiantra, 1971). Such fabrics, when used
in thermal protective garments, have been shown to offer equivalent
or superior reflective and mechanical properties compared with
conventional aluminized asbestos garments (Wren et al., 1977).
Aluminized rayon (basket weave) and certain aluminized cottons were
shown to allow the least transmission of infrared radiation.
20. MEDICAL SURVEILLANCE (RATIONALE)
In the past two decades, many employees working routinely with
lasers have been subjected to preplacement, periodic, and end-of-
job eye examinations in order to obtain sufficient information
concerning the risk of retinal damage. Many of these studies
indicated that periodic eye examinations rarely located hitherto
unsuspected retinal damage. In general, published reports of
ophthalmic accidents have been those in which the acute over-
exposure was sufficient to subjectively alert the individual
(Hathaway et al., 1977). Thus, many authorities (Suess, ed., 1982)
suggest that ophthalmic examinations are unnecessary for
individuals routinely working with Class 1 and 2 lasers, and that,
if requested, the examinations should be confined to those working
with Class 3 or 4 systems only.
An examination is required within 24 - 48 h of any event in
which the worker suspects, or knows, that the eye might have been
exposed. Laser lesions change in appearance and may even tend to
disappear within the heterogeneous appearance of the fundus within
a period of time, so that ophthalmic examinations, some time after
exposure, may be difficult to interpret.
21. FORMAL TRAINING FOR LASER WORKERS
It is necessary to establish a safety programme that assures
the safe use of lasers and other radiation sources. To assure
knowledge of, and compliance with, applicable standards, a certain
amount of formalized teaching is often necessary.
At work places, a specific individual should be assigned to
maintain and enforce the safety programme (in some countries this
individual is termed a laser safety officer (LSO)).
All workers occupied with, or working near, the radiation
source should be included in the teaching programme.
The object is to make workers and work leaders aware of the
risks of lasers, how to avoid the hazards, the proper use of
protective devices, and how to realize when overexposure has taken
place.
REFERENCES
ALLEN, R.G. (1980) Retinal thermal injury. In: Kelley, W.D.,
ed. Non-ionizing radiation, Cincinnati, OH, ACGIH, pp. 161-168.
ACGIH (1976) A guide for control of laser hazards, Cincinnati,
OH, American Conference of Governmental Industrial Hygienists.
ACGIH (1981) Threshold limit values for chemical substances
and physical agents in the workroom adopted by ACGIH for 1981,
Cincinnati, OH, American Conference of Governmental Industrial
Hygienists.
ANDERSON, F.A. (1980a) The biological basis for standards,
Rockville, MD, US Dept. of Health, Education and Welfare, Food
and Drug Administration, Bureau of Radiological Health.
ANDERSON, F.A. (1980b) Sodium and mercury vaporlamps. In:
Kelley, W.D., ed. Non-ionizing radiation, Cincinnati, OH,
ACGIH, pp. 239-243.
ANDERSON, R.R. & PARRISH, J.A. (1981) The optics of human
skin. J. Invest. Derm., 77: 13-19.
ANSI (1978) Standard practice for occupational eye, and face
protection, New York, American National Standards Institute
(ANSI Standard Z-89.1).
ANSI (1980) Safe use of lasers, New York, American National
Standards Institute (ANSI Standard Z-136.1).
AVDEEV, P.S., BEREZIN, Yu.D., GUDAKOVSKII, Yu.P., MURATOV,
V.R., MURZIN, A.G., & FROMZEL, V.A. (1978) Experimental
determination of maximum permissible exposure to laser
radiation of 1.54 µ wavelength. Sov. J. quant. Electr., 8:
134-141.
BEATRICE, E.S. & LUND, D.J. (1979) Characteristics of damage
produced by non-circular retinal laser radiation, San
Francisco, CA, Letterman Army Institute of Research,
(Institute Report No. 31, AD-AD35 878/8ST).
BEATRICE, E.S. & VELEZ, S. (1978) Laser safety bioeffects
research: histopathology of retinal effects. In: SPIE Proc.,
Visual simulation: 162: 103-106.
BERGQUIST, T., HARTMANN, B., & KLEMAN, B. (1978) Imaging
properties of the eye and interaction of laser radiation with
matter. In: Tengroth, B. & Epstein, D., ed. Current concepts
in ergophthalmology, Stockholm, Karolinska Institute.
BIRNGRUBER, R. (1978) [Experimental and theoretical
investigations into thermal injury to the retina from laser
radiation.] PhD Dissertation, Frankfurt, J.W. Goethe
University (in German).
BOLDRY, E.E., LITTLE, H., FLOCKS, M., & VASSILIADIS, A. (1981)
Retinal injury due to industrial laser burns. Ophthalmol., 88:
101-107.
BORLAND, R.G., BRENNAN, D.H., & NICHOLSON, A.N. (1971)
Threshold levels for damage of the cornea following
irradiation by a continuous wave carbon dioxide (10.6 micron)
laser. Nature (Lond.), 234: l5l-l52.
BORLAND, R.G., BRENNAN, D.H., MARSHALL, I.J., & VIVASH, J.P.
(1978) The role of fluorescein angiography in the detection of
laser induced damage to the retina .. a threshold study for
Q-switched neodymium and ruby laser. Exp. Eye Res., 27:
471-493.
BROWN, J.L. (1973) Experimental investigations of flash
blindness. Hum. Factors, 6: 503-516.
CAMPBELL, C.J., RITTLER, M.C., BREDEMEIER, H., & WALLACE, R.A.
(1968) Ocular effects produced by experimental lasers. I.
Carbon dioxide laser. Am. J. Ophthalmol., 66: 604-614.
CIE (1970) International lighting vocabulary, Paris, Bureau
Central de la Commission Internationale de l'Eclairage, Vol.
3, p. 5l.
CLEVET, A. & MAYER, A. (1980) Risques liés à l'utilisation
industrielle des lasers. Cahiers de notes documentaires INRS,
No 99, 2è trimestre, pp. 207-222.
COBLENTZ, W.W., STAIR, R., & HOGUE, J.M. (1931) The spectral
erythemic reaction of the human skin to ultraviolet radiation.
Proc. Natl Acad. Sci., 17(6): 401-405.
COGAN, D.G. & KINSEY, V.E. (1946) Action spectrum of keratitis
produced by ultraviolet radiation. Arch. Ophthalmol., 77:
670-677.
CONSIDINE, P.S. (1966) Effects of coherence on imaging
systems. J. Opt. Soc. Am., 56: 1001-1009.
CORNSWEET, T.N., ed. (1966) Visual perception, New York,
Academic Press.
COURT, L., CHEVALEREAUD, J.P., & SANTUCCI, G. (1978) Exposé
général. In: Sociéte française de Radioprotection, 9è Congrès
international: Effets biologiques des Rayonnements non
ionisants. Utilisation et Risques associés. Monte-Carlo,
Monaco, pp. 367-445.
CROOKES, W. (1914) The preparation of eye-preserving glass for
spectacles. Phil. Trans. Roy. Phil. Soc., A204: 1-25.
DAHLING, R.F., SHAPIRO, S.I., BERRY, C.Z., & SCHREIBER, M.M.
(1970) A method of evaluating sun screen protection from
long-wave ultraviolet. J. Invest. Derm., 55: 164-169.
DAUTRAY, R. & WATTEAU, J.P. (1980) La fusion inertielle par
laser. Rev. gén. nucl., No. 6, pp. 562-575.
DAVIES, J.M. (1959) The effects of intense thermal radiation
on animal skin. A comparison of calculated and observed burns,
Natick, MA, Army Quartermaster Research and Engineering
Command (Report T-24, 29 April 1959, NTIS AD 456794).
DAVSON, H., ed. (1962) The eye (4 volumes), New York, Academic
Press.
DECKER, D. (1977) An accident victim's view. Laser Focus,
13(8): 6.
DECOMPS, B. (1981) Le laser, instrument de recherche et
facteur de développement. Rev. gén. d'Elect., 90(1): 11-29.
DE GRUIJL, F.R. & VAN DER LEUN, J.C. (1980) A dose-response
for skin cancer induction by chronic UV exposure of a human
population. J. Theor Biol., 83; 487-504.
DUKE-ELDER, S. (1972) Textbook of ophthalmology, Vol. VI,
Injuries, St. Louis, Mosby, C.V.
EMMETT, E.A. & HORSTMAN, S.W. (1976) Factors influencing the
output of ultraviolet radiation during welding. J. occup.
Med., 18(1): 41-44.
ENVALL, K.R. & MURRAY, R. (1979) Evaluation of commercially
available laser protective eyewear, Rockville, MD, US Dept of
Health Education and Welfare, Food and Drug administration,
Bureau of Radiological Health. (DHEW Publ. No. (FDA) 79-8086).
ERNEST, J.T. & POTTS, A.M. (1971) Pathophysiology of the
distal portion of the optic nerve. IV. Local temperature as a
measure of blood flow. Am. J. Ophthalmol., 72(2): 435-444.
FITZPATRICK, T.B., PATHAK, M.A., HARBER, L.C., SEIJI, M., &
KUKITA, A. (1974) Sunlight and man, normal and abnormal
photobiologic responses, Tokyo, University of Tokyo Press.
FRANCE, Arrêté du 30 janvier (1974) Réglementation concernant
les lasers à usage médical. J.O. 17 mars 1974, p. 3093.
FRANCE, Arrêté du 13 mai (1974) Conditions techniques
générales des lasers à usage médical. J.O. 15 juin 1974,
p. 6388.
FRANCE, Arrêté du 14 mai (1974) Conditions techniques des
lasers à usage médical de catégorie II, groupe I, sous-groupe
I. J.O. 15 juin 1974, p. 6388.
FRANCE, Arrêté du 29 décembre (1976) Classification des lasers
à usage médical de catégorie II, groupe II (émission
continue). J.O. 22 janvier 1977, (Numéro complémentaire)
p. 466.
FRANCE, Arrêté du 10 janvier (1978) Conditions techniques
d'utilisation des lasers à usage médical de catégorie II,
groupe II. J.O. 28 janvier 1978 (Numéro complémentaire) p. 822.
FRIED, D.L. (1981) Laser eye safety: The implications of
ordinary speckle and speckled-speckle statistics. J. Opt. Soc.
Am., 71(7): 914-916.
FRISCH, G.D., BEATRICE, E.S., & HOLSEN, R.C. (1971)
Comparative study of argon and ruby retinal damage thresholds.
Invest. Ophthalmol., 10: 911-919.
GABEL, V.P. & BIRNGRUBER, R. (1981) A comparative study of
threshold laser lesions in the retinae of human volunteers and
rabbits. Health Phys., 40: 238-240.
GABEL, V.P., BIRNGRUBER, R., & HILLENKAMP, F. (1976) [Light
absorption in the fundus oculi.] Munich, Association for
Research on Radiation and the Environment (GSF report A55) (in
German).
GEERAETS, W.J. & BERRY, E.R. (1968) Ocular spectral
characteristics as related to hazards from lasers and other
light sources. Am. J. Ophthalmol., 66: 15-20.
GIESE, A.C. (1976) Living with our sun's ultraviolet rays,
New York, Plenum Publishing Corporation.
GOLDMAN, L., ed. (1981) The biomedical laser technology and
clinical applications, New York, Heidelberg, Berlin, Springer
Verlag.
GOLDMAN, L., ROCKWELL, R.J., & RICHFIELD, D. (1971) Long-term
laser exposure of a senile freckle. Arch. environ. Health, 22:
401-403.
GOLDMAN, L., ROCKWELL, R.J., MICHAELSON, S.M., SLINEY, D.H.,
TENGROTH, B.M., & WOLBARSHT, M.L. (1982) Optical radiation,
with particular reference to lasers. In: Suess, M. ed.
Nonionizing radiation, Copenhagen, World Health Organization,
Regional Office for Europe.
GOLDMANN, H. (1933) Genesis of heat cataract. Arch.
Ophthalmol., 9: 314.
GORODETSKI, A.A., KIRICINSKI, B.R., EVDOKOMOB, I.R., &
KOLESNIK, V.M. (1968) [Some data on the biological action and
radiation protection of optical quantum generators.] Gig. Tr.
Prof. Zabol., 12: 37-41 (in Russian).
GREISEMANN, J.C. & MARTI, J. (1978) Risques liés à
l'utilisation des lasers de puissances. In: Société française
de Radioprotection, 9è Congrès international. Effets
biologiques des Rayonnements non ionisants. Utilisation et
Risques associés, pp. 473-482.
GREISS, G.A., BLANKENSTEIN, F., & WILLIFORD, G.G. (1980)
Ocular damage thresholds from multiple-pulse laser exposures,
Health Phys., 39: 921-927.
GRUM, F.C. & BECHERER, R., ed. (1979) Optical radiation
measurements, Vol. 1, Radiometry, New York, Academic Press,
p. 352.
GULLBERG, K., HARTMAN, B., KOCK, E., & TENGROTH, B. (1967)
Carbon dioxide laser hazards to the eye. Nature (Lond.), 215:
857-858.
HAM, W.T. Jr, WILLIAMS, R.C., MUELLER, H.A., GUERRY, D.,
CLARKE, A.M., & GEERAETS, W.J. (1966) Effects of laser
radiation on the mammalian eye. Trans. NY Acad. Sci., 28:
517-526.
HAM, W.T. Jr, CLARKE, A.M., GEERAETS, W.J., CLEARY, S.F.,
MUELLER, H.A., & WILLIAMS, R.C. (1970) The eye problem in
laser safety. Arch. environ. Health, 20: 156-160.
HAM, W.T. Jr, MUELLER, H.A., & SLINEY, D.H. (1976) Retinal
sensitivity to damage from short wavelength light. Nature
(Lond.), 260(5547): 153-155.
HAM, W.T. Jr, MUELLER, H.A., RUFFOLO, J.J., & CLARKE, A.M.
(1978) Sensitivity of the retina to radiation damage as a
function of wavelength. Photochem. Photobiol., 29: 735-743.
HAMERSKI, W. (1969) Investigations on histochemical changes in
experimental corneal lesions induced with UV radiation and on
the prevention of photophthalmia. Pol. med. J., 8: 1469-1476.
HANSEN, W.P. & FINE, S. (1968) Melanin granule models for
pulsed laser induced retinal injury. Appl. Opt., 7: 155-159.
HARDY, J.D. (1968) Pain following step increase in skin
temperature. In: Kenshalo, D.R. ed. The skin senses,
Springfield, IL, Charles C. Thomas, pp. 444-456.
HARDY, J.D., HAMMEL, H.T., & MURGATROYD, D. (1956) Spectral
transmittance and reflectance of excised human skin. J. appl.
Physiol., 9: 257.
HARLEN, F. (1978) The development of laser codes of practice
and maximum permissible exposure levels. Ann. occup. Hyg.,
2l(2): 199-211.
HARTMANN, B. & KLEMAN, B. (1980) Exposure limits for
broad-band 400-1400 nm radiation. Ocular effects of
non-ionizing radiation. Proc. SPIE, 29: 105-114.
HARWERTH, R.S. & SPERLING, H.G. (1975) Effects of intense
visible radiation on the increment threshold spectral
sensitivity of the Rhesus monkey eye. Vision Res., 15:
1193-1204.
HATFIELD, E.M. (1970) Eye injuries and the solar eclipse.
Sight Sav. Rev., pp. 79-85.
HATHAWAY, J.A., STERN, N., SOLES, E.M., & LEIGHTON, E. (1977)
Ocular medical surveillance on microwave and laser workers. J.
occup. Med., l9(10): 683-688.
HAUSSER, K.W. (1929) [Influence of wavelength in radiation
biology.] Strahlenther., 28: 25-44 (in German).
HOLZINGER, G., KROY, W., SCHREIBER, P., & SUTTER, E. (1978)
Protection from law radiation (Series on Workplace Protection,
no.14).
INTERNATIONAL ORGANIZATION FOR STANDARDIZATION (1980) Personal
eye-protectors for welding and related techniques. Welding
filters, Geneva (ISO 4850).
IRPA (1977) Overviews on nonionizing radiation, International
Radiation Protection Association Report of a Study Group.
JAMES, R.H., ed. (1976) National Conference on Measurements
of Laser Emissions for Regulatory Purposes, April, Rockville,
MD, US Dept of Health, Education and Welfare, Food and Drug
Administration, Bureau of Radiological Health (HEW Publ. (FDA)
76-8037).
KASUBA V.A. & AKIFEV, S.A. (1977) [Working conditions and
morbidity among workers preparing clock jewels using lasers
and mechanical techniques.] Gig. Tr. Prof. Zabol., 1: 37-40
(in Russian).
KAUFMANN, E. (1970) Laser hazard to the human eye. Schweiz
Arch., 36: 211.
KLINE, M.V. (1970) Optics, New York, John Wiley and Sons.
KLOST, W. (1971) [Safety measures in the use of laser rays.]
Zentralbl. Arbeitsmed., 21: 105-111 (in German).
KOGELNIK, H. & LI, T. (1966) Laser beams and resonators. In:
Levine, A.K., ed. Lasers. New York, Decker.
KOMAROVA, A.A., MOTZERENKOV, V.P., SKATSKAIA, G.K., CEMNY,
A.B., & PIVOVAROV, N.N. (1978) [Action of reflected laser
radiation on the eye.] Vestn. Oftal., l: 46-50 (in Russian).
KUWABARA, T. (1970) Retinal recovery from exposure to light.
Am. J. Ophthalmol., 70(2): 187-189.
LA VAIL, M.M. (1980) Eye pigmentation and constant light
damage in the rat retina. In: Williams, T.P. & Baker, B.N.,
ed. The effects of constant light on visual processes, New
York, London, Plenum Press, pp. 357-387.
LAWWILL, T., CROCKET, S., & CURRIER, G. (1977) Retinal damage
secondary to chronic light exposure thresholds and mechanisms.
Doc. Ophthalmol., 44(2): 379-402.
LE BODO, H. (1976) La calorimétrie appliquée à la mesure des
puissances et énergies lasers. Bulletin d'information du
Bureau National de Métrologie, No. 24, pp. 12-18.
LEIBOWITZ, H.M. & PEACOCK, G.R. (1969) Corneal injury produced
by carbon dioxide laser radiation. Arch. Ophthalmol., 8l:
712-721.
LERMAN, S. (1980a) Radiant energy and the eye, New York,
Macmillan Publ. Co.
LERMAN, S. (1980b) Human ultraviolet radiation cataracts.
Ophthal. Res., 12: 303-314.
LIVINGSTON, P.C. (1932) The study of sun glare in Iraq. Br. J.
Ophthalmol., 6: 577-625.
LOWE, D.A. (1975) A guide to international recommendations on
names and symbols for quantities and on limits of measurement.
Geneva, World Health Organization (Progress in Standardization: 2).
MAGNUS, I.A. (1976) Dermatological photobiology, London,
Blackwell Scientific Publications.
MAINSTER, M.A., WHITE, T.J., TIPS, J.H., & WILSON, P.W. (1970)
Retinal-temperature increases produced by intense light
sources. J. Opt. Soc. Am., 60: 264-270.
MARSHALL, J. (1970) Thermal and mechanical mechanisms in laser
damage to the retina. Invest. Ophthalmol., 9: 97-115.
MARSHALL, J. (1973) Laser damage to ocular tissues. Proc. R.
Soc. Med., 66(9): 842-844.
MARSHALL, J. (1978) Retinal injury from chronic exposure to
light and the delayed effects from retinal exposure to intense
light sources. In: Tengroth, B. & Epstein, D., ed. Current
concepts in ergophthalmology, Stockholm, Karolinska Institute,
pp. 81-104.
MARSHALL, J. & BIRD, A.C. (1979) A comparative histo-
pathological study of argon and krypton laser irradiations of
the human retina. Br. J. Ophthalmol., 63(10): 657-668.
MARSHALL, W.J. (1980) Optical measurement techniques. In:
Kelley, W.D., ed. Non-ionizing radiation, Cincinatti, OH,
ACGIH, pp. 175-179.
MAYER, M.A. & SALSI, M.S. (1979) Rayonnement ultraviolet,
visible et infrarouge, mésure-evaluation des risques. INRS
Cahiers de Notes documentaires, No. 96, 3e trimestre, 403-413.
MEDOVSKAYA, T.P. (1970) Data on the condition of the eye in
workers at a glass factory. Hyg. Sanit., 35: 446-447.
MESTER, E. (1980) L'effet stimulant des faisceaux laser sur la
cicatrisation des plaies. Rev. Iéna, No. 3, pp. 121-122.
MIRO, L. (1979) Le laser et ses applications médio-
chirurgicales. Semaine des hôpitaux de Paris, 55(41-42):
1956-1964.
MOON, M.E., CLARKE, A.M., RUFFALO, J.J. Jr, & MUELLER, H.A.
(1978) Visual performance in the Rhesus monkey after exposure
to blue light. Vision Res., 18: 1573-1577.
MOSS, C.E. (1980) Radiation hazards associated with
ultraviolet radiation curing processes. In: Kelley, W.D., ed.
Non-ionizing radiation, Cincinnati, OH, ACGIH, pp. 203-209.
NOELL, W.K. & ALBRECHT, R. (1971) Irreversible effects of
visible light on the retina, role of vitamin A. Science, 172:
76-79.
PARR, W.H. (1969) Skin lesion threshold values for laser
radiation as compared with safety standards, Fort Knox, KY, US
Army Medical Research Laboratory (Report 8l3, AD 688871).
PARRISH, J.A., ANDERSON, R.R., URBACH, F., & PITTS, D. (1978)
UVA biological effects of ultraviolet radiation with emphasis
on human responses to longwave ultraviolet, New York, Plenum
Publishing Corporation.
PARVER, L.M., ANKER, C., & CARPENTER, D.O. (1980) Choroidal
blood flow as a heat dissipating mechanism in the macula. Am.
J. Ophthalmol., 89: 641-646.
PECKHAM, R.H. & HARLEY, R.D. (1951) The effect of sunglasses
in protecting retinal sensitivity. Am. J. Ophthalmol., 34(11):
1499-1507.
PENNER, R. & McNAIR, J.N. (1966) Eclipse blindness. Am. J.
Ophthalmol., 61: 1452-1457.
PITTS, D.G. (1974) The human ultraviolet action spectrum. Am.
J. opt. S. physiol. Opt., 51: 946-960.
PITTS, D.G., CULLEN, A.P., & HACKER, P.D. (1977) Ocular
effects of ultraviolet radiation from 295 to 365 nm. Invest.
ophthalmol. Vis. Sci., 16(10): 932-939.
PRATESI, R. & SACCHI, C.A., ed. (1980) Lasers in photomedicine
and photobiology, Berlin, Springer-Verlag.
ROCKEROLLES, R. (1978) Dangers spécifiques du rayonnement
cohérent. Dangers habituels liés aux fortes luninances; effets
multiphotoniques et effets non linéaires. In: Société
française de Radioprotection. 9è Congrès international: Effets
biologiques des Rayonnements non ionisants. Utilisation et
Risques associés, Monte-Carlo, Monaco, pp. 453-472.
ROCKWELL, R.J. Jr, & GOLDMAN, L. (1974) Research on human skin
laser damage threshold, final report, Texas, USAF School of
Aerospace Med., Brooks AF Base (Prepared by Dept of
Dermatology and Laser Lab. Med. Centre, University of
Cincinnati, Contract F4l609-72-C-0007).
ROGER, F.C. (1973) Clinical findings, course and progress of
biatis corneal degeneration in the Dahlak Islands. Br. J.
Ophthalmol., 57: 657-661.
RUBIN, L.R. (1977) Lasers in biology, Moscow, Nauka.
SCHERR, A.D., TUCKER, R.J., & GREENWOOD, R.A. (1969) New
plastics absorb at laser wavelength. Las. Foc., 5(9): 46-48.
SCHREIBEIS, W.J. (1968) Laser eye protection goggles based on
maufacturer's information. Am. Ind. Hyg. Assoc. J., 29: 504.
SKEEN, C.H., BRUCE, W.R., TIPS, J.H. Jr, SMITH, M.G., & GARZA,
G.G. (1972) Ocular effects of repetitive laser pulses,
San Antonio, TX, Technology Inc. (Contract F41609-71-C-0018, AD
746795).
SLINEY, D.H. (1971) The development of laser safety
criteria-biological considerations. In: Wolbarsht, M.L., ed.
Laser applications in medicine and biology, New York, Plenum
Press, pp. 163-238.
SLINEY, D.H. (1972) The merits of an envelope action spectrum
for ultraviolet radiation exposure criteria. Am. Ind. Hyg.
Assoc. J., 33: 644-653.
SLINEY, D.H. (1974) Laser protective eyewear. In: Wolbarsht,
M.L., ed. Laser application in medicine and biology, New York,
Plenum Press, Vol. 2.
SLINEY, D.H. & FREASIER, B.C. (1973) The evaluation of optical
radiation hazards. Appl. Opt., 12(1): 1-24.
SLINEY, D.H. & WOLBARSHT, M.L. (1980) Safety with lasers and
other optical sources, New York, Plenum Publishing Corporation.
SLINEY, D.H., MOSS, C.E., MILLER, C.G., & STEPHENS; J.B.
(1981) Semitransparent curtains for control of optical
radiation hazards. Appl. Optics, 20(14): 2352-2366.
SMITH, H.E. (1944) Actinic macular retinal pigment
degeneration. US Nav. med. Bull., 42: 675-680.
SMITH, K.C. (1977) The science of photobiology, New York,
Plenum Press.
SMITH, K.C. (1978) Symposium on DNA repair and its role in
mutagenesis and carcinogenesis. Photochem. Photobiol., 28: 119.
STAIR, R. (1948) Spectral-transmissive properties and use of
eye-protective glasses. Washington, DC, National Bureau of
Standards (NBS Circular 471).
STOLL, A.M. & CHIANTRA, M.A. (1971) Heat transfer through
fabrics as related to thermal injury. Trans. N.Y. Acad. Sci.,
33: 649-670.
STOLWIJK, J.A.J. (1980) Infrared radiation and radiant heat
stress. In: Kelley, W.D., ed. Non-ionizing radiation,
Cincinnati, OH, ACGIH, pp. 171-174.
STRAUB, H.W. (1970) Laser eye protection in the USA.
Berufsgenossenschaft Z. Unfallv. Betrieb, 3: 83-87.
STUCK, B.E., LUND, D.J., & BEATRICE, E.A. (1981) Ocular
effects of holmium (2.06 µm) and erbium (1.54 µm) laser
radiation. Health Phys., 40: 835-846.
SUESS, ed. (1982) Nonionizing radiation protection,
Copenhagen, World Health Organization, Regional Office for
Europe.
SUTTER, E., HUEBNER, H.J., KRAUSE, E., & RUGE, J. (1972)
[Radiation measurements in various arc welding processes.]
Federal Republic of Germany, Federal Institute of Physics and
Technology (Report No. Optik 2/72) (in German).
SWOPE, C.H. (1969) The eye protection. Arch. environ. Health,
18: 428-433.
SWOPE, C.H. (1970) Design considerations for laser eye
protection. Arch. environ. Health, 20: 184-187.
SWOPE, C.H. & KOESTER, C.J. (1965) Eye protection against
lasers. Appl. Opt., 4(5): 523-525.
SYKES, S.M., ROBISON, W.G., WAXLER, M., & KUWABARA, T. (1981)
Damage to the monkey retina by broad-spectrum fluorescent
light. Invest. Ophthalmol. Vis. Sci., 20(4): 425-434.
TENGROTH, B.M. (1976) Safety glasses in welding. Env. Res.,
11:283-284.
TENGROTH, B.M., LYDAHL, E., & PHILIPSON, B.T. (1980) Infrared
cataract in furnacemen. In: Kelley, W.D., ed. Non-ionizing
radiation, Cincinnati, OH, ACGIH, pp. 169-170.
URBACH, R., ed. (1969) The biologic effects of ultraviolet
radiation, New York, Pergamon Press.
URBACH, R. (1980) Occupational skin hazards from ultraviolet
exposure. In: Kelley, W.D., ed. Non-ionizing radiation,
Cincinnati, OH, ACGIH, pp. 145-156.
US DHEW (1978) Performance standards for light emitting
products, (title 21, Code of Federal Regulations, part 1040),
Washington, DC, US Department of Health, Education and Welfare.
VAN DER LEUN, J.C. (1965) Theory of ultraviolet erythema.
Photochem. Photobiol., 4: 453-458.
VASSILIADIS, A. (1971) Ocular damage from laser radiation. In:
Wolbarsht, M.L., ed. Laser applications in medicine and
biology, New York, Plenum Press, pp. 125-162.
VASSILIADIS, A., ZWENG, H.C., & DEDRICK, K.G. (1971) Ocular
laser threshold investigations, Menlo Park, CA, Stanford
Research Institute (SRI Report No. 8209).
VOGT, A. (1919) [Experimental inducement of cataract by
isolated short-wave infrared mixed with red.] Klin. Mbl.
Augenheilkd., 63: 230-231 (in German).
VOS, J.J. (1966a) Heat-damage to the retina by lasers and
photocoagulators. Ophthalmologia (Basel), 151: 652-654.
VOS, J.J. (1966b) Some considerations on eye hazards with
lasers, Soesterberg, Institute for Perception RVO-TNO,
National Council for Applied Research in the Netherlands, 23
pp. (Report IZF 1966-4. AD 800156).
WEALE, R.A. (1982) The age variation of "senile" cataract in
various parts of the world. Br. J. Ophthalmol., 66: 31.34.
WHO SCIENTIFIC GROUP ON HEALTH FACTORS INVOLVED IN WORKING
UNDER CONDITIONS OF HEAT STRESS (1969) Report, Geneva, World
Health Organization (WHO Technical Report Series No. 412).
WHO (1979) Environmental Health Criteria 14: Ultraviolet
radiation, Geneva, World Health Organization.
WHO (l982) The SI for the health profession (reimpression)
Geneva, Switzerland, World Health Organization.
WILLIAMS, T.B. & BAKER, B.N., ed. (1980) The effects of
constant light on the visual process, New York, Plenum Press.
WOLBARSHT, M.L. (1971, 1974, 1978a) Lasers in medicine and
biology, New York, Plenum Press, Vols I, II, III.
WOLBARSHT, M.L. (1978b) The effects of optical radiation on
the anterior structures of the eye. In: Epstein, D. &
Tengroth, B., ed. Current concepts in ergophthalmology,
Stockholm, Department of Ophthalmology, Karolinska Institute,
pp. 29-46.
WOLBARSHT, M.L. & SLINEY, D.H. (1974) The formulation of
protection standards for lasers. In: Wolbarsht, M.L., ed.
Lasers in medicine and biology, New York, Plenum Press,
Vol. II, pp. 309-360.
WOLBARSHT, M.L., YAMANASHI, B.S., & ORR, M.A. (1977) The
origin of cataracts in the lens from infrared radiation,
Durham, NC, Duke University Eye Centre (Report 7-20-1977:
62772A 3E62772A813.00.013, Contract DAMD 17-74-C-4133, US Army
Med. Res. and Dev. Cmd).
WOLBARSHT, M.L., O'FEGHLUDHA, F.A., SLINEY, D.H., GUY, A.W.,
SMITH, A.A. Jr, & JOHNSON, G.A. (1980) Electromagnetic
emission from visual display units: a non-hazard. In: Kelley,
W.D., ed. Non-ionizing radiation, Cincinnati, OH, ACGIH,
pp. 193-201.
WREN, J.E., SCOTT, W.D., & BATES, C.E. (1977) Thermal and
mechanical properties of aluminized fabrics for use in ferrous
metal handling operations. Am. Ind. Hyg. Assoc. J., 38(11):
603-612.
YOUNG, R.W. (1980) A theory of central retinal disease. In:
Sears, M.L., ed. New directions in ophthalmic research,
New Haven, London, Yale University Press, pp. 237-270.
ZIGLER, J.S. & GOOSEY, J.D. (1981) Photosensitized oxidation
in the lens: evidence from photosensitizers endogenous to the
human lens. Photochem. Photobiol., 33: 689-874.
ZHOKOV, V.P., KOMAROVA, A.A., MAXIMOVA, L.I., MURATOV, V.P.,
PALTZEV, Yu.P., & SEMINOV, A.I. (1981) Occupational hygiene
and prevention of occupational diseases from lasers, Moscow,
Meditsina.
ZUCHLICH, J.A. & KURTIN, W.E. (1977) Oxygen dependence of
near-ultraviolet induced corneal damage. Photochem.
Photobiol., 25: 133-135.
ZUCHLICH, I.A. & TABOADA, J. (1978) Ocular hazard from UV
laser exhibiting self-mode-locking. Appl. Opt., 17: 1482-1484.
ZWICK, H. & BEATRICE, E.S. (1978) Long-term changes in
spectral sensitivity after low-level laser (5l4 nm) exposure.
Mod. Probl. Ophthalmol., 19: 319-325.
GLOSSARY
ACOUSTICO-OPTIC: involving the interaction of light and an acoustic
wave. Acoustico-optic devices such as Q switches and modulators
are used in manipulating laser beams.
ACTIVE MEDIUM: the atomic or molecular species which can provide
gain for laser oscillation. Also called laser medium, lasing
medium or active material.
ANGSTROM (A): a non-SI unit equal to 10-10 metre. Its use as a
unit of optical wavelength has largely been supplanted in recent
years by the nanometre (10-9 metre).
ARC LAMP: an electric lamp in which current passes through the
ionized air between two electrodes, giving off light. Applications
include laser excitation.
ATOMIC LASER: a gas laser in which the active material is an atomic
species rather than a molecule.
ATTENUATION: reduction in intensity that results when optical
radiation travels through an absorbing or scattering medium. In
optical fibre, attenuation (in decibels) equals 10 log ( Po/ Pin),
where Po is the power at the output end of the fibre and Pin is
the power launched into the fibre.
AVERAGE POWER: in a repetitively pulsed laser, the energy per pulse
times the repetition rate. When the energy per pulse is expressed
in joules and the repetition rate in hertz, the average power is
expressed in watts.
BEAM DIAMETER: the distance between the two opposing points at
which the irradiance or radiant exposure is a specified fraction
(typically 1/e or 1/e2) of the irradiance or radiant exposure of
the emitted radiation.
BEAM DIVERGENCE: the increase in beam diameter with distance from
the laser's exit aperture. Measured in milliradians at specified
points, usually where irradiance or radiant exposure is 1/e or 1/e2
the maximum value, and expressed as the "full-angle" divergence.
BOLOMETER: a type of detector which measures infrared radiation by
the temperature-induced change of resistance in a metal foil
exposed to the radiation and heated by it.
BREWSTER ANGLE: the angle between an incident beam of light and a
dielectric reflecting surface at which none of the light polarized
in the plane of incidence is reflected. Brewster's angle is
tan-1 n2/ n1, where n1, and n2 are the indexes of refraction of the
first and second media respectively. A window mounted at
Brewster's angle with respect to an incident beam is often used as
a window in laser cavities.
CALORIMETER: a type of detector that measures heat produced by
absorption of radiation.
CHEMICAL LASER: a type of laser in which the population inversion
is produced directly by an "elementary" chemical reaction (a
collision process in which one or more molecules undergo changes in
their chemical bonds).
COHERENCE: a fixed phase relationship among various points of an
electromagnetic wave in space (spatial coherence) or in time
(temporal coherence).
COLLIMATOR: an optical device for converting a diverging or
converging beam of light into a collimated or parallel beam, or for
expanding or reducing the cross-sectional area of an incident
collimated beam. A target collimator projects a parallel beam from
its own light source such that, viewed from any distance, the light
source appears to be at infinity.
CONTINUOUS WAVE (cw) LASER OPERATION: laser operation in which
radiation is emitted continuously.
CORE: the central region of an optical fibre. The core must have a
higher refractive index than the cladding for light to be
transmitted through the fibre via total internal reflection
CORNER CUBE: an optical component with three mutually perpendicular
faces and a hypotenuse face. Because light entering through the
hypotenuse is totally internally reflected at each perpendicular
face, the cube acts as a retroreflector. Also known as corner
reflector.
CRYSTAL LASER: a type of laser in which the active medium is an
atomic species in a crystal such as ruby, YAG (yttrium aluminium
garnet), or YALO (yttrium aluminate).
DETECTOR: see PHOTODETECTOR.
DIFFRACTION: deviation of light rays from the paths predicted by
geometical optics.
DIODE LASER: see SEMICONDUCTOR LASER.
DISPERSION: variation of the refractive index of an optical
material with change in wavelength, as in a prism; in an optical
fibre, the temporal spreading of a light pulse due to the fibre's
different propagation speeds for different wavelengths and modes of
light. Such spreading limits the fibre's information-carrying
capacity of bandwidth.
DIVERGENCE: see BEAM DIVERGENCE.
DYE LASER: a type of laser in which the active medium is an organic
dye, generally in solution with the liquid either flowing or
encapsulated within a cell. Experimental solid and gas dye lasers
also have been built. Also called organic-dye, tunable-dye or
liquid laser.
ELECTRON-BEAM-SUSTAINED LASER: a molecular-gas laser in which the
electrical discharge is sustained with a beam of high-energy
electrons. Usually injected transversely to the laser cavity's
optical axis, the electron beam permits laser operation at
pressures and cross-section-to-length ratios higher than possible
with an unsustained discharge. This technique is often used in
commercial carbon-dioxide lasers with very high continuous-wave
output power.
ELECTRO-OPTIC: applying to modulators, Q switches and other beam-
manipulating devices in which operation relies on modification of a
material's refractive indices by an applied electrical field. In a
Kerr cell the index change is proportional to the square of the
electrical field, and the material is usually a liquid. In a
Pockels cell the material is a crystal whose index change is linear
with the electric field.
EMISSIVITY: ratio of radiant exitance of a thermal radiator to that
of a full radiator (black body) at the same temperature - (ISO
31/VI 1980).
EXCIMER LASER: a laser in which the active medium is an excimer, a
molecule which is chemically unstable except in its excited state.
The term often is applied to lasers in which the active medium is a
rare-gas halide (or monohalide) excimer such as KrF* or XeF*.
GAS LASER: a type of laser in which the active medium is a gas.
The category is subclassified according to the active medium into
atomic (such as helium-neon), molecular (carbon dioxide, hydrogen
cyanide and water vapour), ionic (argon, krypton, xenon, and the
metal-vapour types such as helium-cadmium and helium-selenium), and
excimer (typically rare-gas halides). Loosely applied, "ion" means
argon and krypton.
GLASS LASER: a type of solid-state laser in which the active medium
is a glass rod doped with rare-earth atoms, usually neodymium.
HERTZ (Hz): the SI unit of frequency of periodic phenomena. It
replaces the non-SI unit "cycles per second". The number of pulses
per second that a laser can produce may be expressed in hertz.
HOLOGRAM: a recording of the interference of coherent light
reflected from an object with light direct from the same source or
reflected from a mirror. Illumination of the hologram reproduces
the object's three-dimensional image.
IMAGE CONVERTER: an electron tube which produces a visual replica
of an image formed on its cathode by some form of electromagnetic
radiation. In an image converter camera, the image formed by the
electron tube is focused on to photographic film for a permanent
record.
INFRARED: electromagnetic radiation with wavelength between 0.76
micrometre and about 1 millimetre. Wavelengths at the shorter end
of this range are frequently called "near" infrared, and those
longer than about 20 micrometres, "far" infrared.
INTEGRATED OPTICS: devices in which several optical components are
"integrated" on to a single substrate; analogous to integrated
electronic circuits. Although still in the research phase,
integrated optics has potential for use in optical signal
processing and in fibre-optic communications.
INTERFERENCE FILTER: an optical component which depends on
interference in a series of thin films deposited on a substrate to
limit transmission to a desired spectral band.
ION LASER: a type in which the active element is an ionized gas,
generally argon or krypton.
IRRADIANCE ( E): radiant flux per unit area, expressed in watts per
square centimetre.
LASER: acronym for "light amplication by stimulated emission of
radiation." A device which generates or amplifies electromagnetic
oscillations at wavelengths between the far infrared
(submillimetre) and ultraviolet. Like any electromagnetic
oscillator, a laser oscillator consists of two basic elements: an
amplifying (active) medium and a regeneration or feedback device
(resonant cavity). A laser's amplifying medium can be a gas,
semiconductor, dye solution, etc; feedback is typically from two
mirrors. Distinctive properties of the electromagnetic
oscillations produced include monochromaticity, high intensity,
small beam divergence, and phase coherence. As a description of a
device, "laser" refers to the active medium plus all equipment
necessary to produce the effect called lasing.
LASER DIODE: see SEMICONDUCTOR LASER.
LED: abbreviation of light-emitting diode. A semiconductor
emitting incoherent light into a broad field of view, used in low-
speed or short-haul fibre-optic links. Most LEDs used in fibre-
optic applications emit in the near infrared.
LIDAR: acronym for "light detection and ranging," a system
employing a laser beam to gather ranging information as well as
intelligence on reflection and scattering of light by clouds and
atmospheric pollutants.
LIQUID LASER: a type in which the active element is either an
organic dye or an inorganic liquid. See also DYE LASER.
MULTIMODE: emission at several frequencies simultaneously,
generally closely spaced, each frequency representing a different
mode of laser oscillation inthe resonant cavity.
Nd-GLASS: neodymium-doped glass, used in some solid state lasers.
The neodymium atoms are the active medium.
Nd-YAG: neodymium-doped yttrium-aluminium-garnet (YAG), a crystal
which is used in some solid state lasers. The neodymium atoms are
the active medium.
NEUTRAL DENSITY FILTER: a filter which reduces the intensity of
light without affecting its spectral character.
NONLINEAR EFFECTS: changes in a medium transmitting electromagnetic
waves that are proportional to the second, third or higher powers
of external electric field. Nonlinear optical effects include
harmonic generation and the electro-optic effect. See electro-
optic.
OPTICALLY PUMPED LASER: a laser whose active medium is excited by
another light source to produce a population inversion. For solid-
state and some dye lasers this source usually is an incoherent type
such as a flash- or arc-lamp. For gas and other dye lasers,
coherent laser sources generally provide such optical pumping.
PARAMETRIC OSCILLATOR: a nonlinear device, usually a crystal, which
produces tunable laser oscillations at the sum or difference
frequency of mixed laser beams. Also called tunable parametric
oscillator or optical parametric oscillator. Loosely applied to
the complete instrument containing the pump laser and the tuning
crystal.
PHOTODETECTOR: any device which detects light, generally producing
an electronic signal with intensity proportional to that of the
incident light.
PHOTON: a massless "particle" of electromagnetic radiation, with
energy equal to hc/lambda where h is Planck's constant (6.6 x 10-34
joule second) and c/lambda is the frequency of the radiation (speed
of light divided by wavelength).
POLARIZER: an optical component which only transmits lightwaves
that oscillate in a given plane.
POPULATION INVERSION: a condition in which most atoms of a species
are in an excited, metastable state. Collision of a photon with
such an atom causes the atom to relax to a lower energy state, and
to emit a second photon, amplifying the light signal. Population
inversion is required for lasing to occur.
PULSELENGTH: the duration of the burst of energy emitted by a
pulsed or Q-switched laser. Expressed in seconds and usually
measured at the half-power (half the full height of a voltage or
current pulse). Also called pulsewidth.
PULSED LASER: a laser that emits light in pulses rather than
continuously.
PUMP: the energy source (such as flashlamp, electron beam or
current supply) that drives the amplification in the active medium
of a laser by creating a population inversion.
PYROELECTRIC CRYSTAL: a type of crystal that shows electrical
effects when its temperature is changed; these effects are used to
detect infrared radiation.
Q SWITCH: essentially a "shutter" which prevents laser emission
until opened. Q stands for "quality factor" of the laser's
resonant cavity. "Active" Q switching is achieved with a rotating
mirror or prism, Kerr or Pockels cell, or acoustico-optic device;
"passive" Q switching is achieved with a saturable absorber such as
a gas or dye. In a pulsed laser a Q switch increases pulse power
by shortening pulse duration while not significantly decreasing the
energy; in a continuous wave laser the device provides shorter and
more intense pulses at a higher repetition rate than could be
achieved by pulsing the laser directly.
RADIANCE ( L): At a point of a surface and in a given direction,
the radiant intensity of an element of the surface, divided by the
area of the orthogonal projection of this element on a plane
perpendicular to the given direction (ISO 31/6-1980). Expressed in
watts per steradian square centimetre.
RADIANT FLUX: the rate of flow of radiant energy, measured in
watts.
RADIOMETER: an instrument for measuring incident radiation in
radiometric units (watts). Radiometric measurements can be made at
any wavelength, but the spectral range of a particular instrument
may be limited to a narrow range.
RADIOMETRIC UNITS: units defined for measurement of the intensity
of electromagnetic radiation; the basic unit is the SI unit watt.
RAMAN EFFECT: the appearance of additional weak lines in the
spectrum of light that has been scattered by a transparent
substance. The extra lines result from rotational or vibrational
transitions of the molecules in the scattering medium. If the
medium is illuminated with laser light of sufficient intensity, the
emission at the Raman frequencies is amplified, exhibiting
characteristics of stimulated emission (i.e., stimulated Raman
effect.).
REFLECTANCE: the ratio of wave energy reflected from a surface to
the wave energy incident on a surface.
SEMICONDUCTOR LASER: a type in which the active material is a
semiconductor, either a diode or homogeneous. Commercial
types are generally diodes in which lasing occurs at the
junction of n-type and p-type semiconductors, usually gallium-
arsenide or gallium-aluminium-arsenide. Homogeneous types are
made of undoped semiconductor material and are pumped by an
electron beam.
SOLID-STATE LASER: a type the active medium of which is an atomic
species in a glass or crystal. The atomic species may be added to
the glass or crystal, as neodymium is added to glass, or may be
instrinic, as chromium is in ruby. This term is generally not
applied to semiconductor lasers.
SUPER-RADIANT: applying to coherent optical amplification of
spontaneous emission that occurs without relaxation processes.
Commonly used to describe a laser whose gain is high enough to
permit amplification without mirrors; examples are nitrogen and
molecular hydrogen. Beam quality of a super radiant laser is
generally inferior to that of a laser with a complete optical
cavity. "Super-fluorescent" has been proposed as a more precise
description of this type of laser.
TEA LASER: acronym for transversely excited, atmospheric pressure
laser. A gas laser in which excitation of the active medium is
transverse to the flow of the medium. Because of shorter breakdown
length, this type operates in a gas-pressure range higher than that
for longitudinally excited gas lasers (but not necessarily
atmospheric) and offers a potentially higher power output per unit
volumes because of a greater density of lasing molecules.
TUNABLE LASER: a laser or a parametric oscillator whose emission
can be varied across a broad spectral range.
ULTRAVIOLET: electromagnetic radiation with wavelengths between
about 40 and 400 nanometres. Radiation between 40 and 200 nm is
termed "vacuum ultraviolet" because it is absorbed by air and
travels only through a vacuum. The "near" ultraviolet has
wavelengths close to those of visible light; the "far" ultraviolet
has shorter wavelengths.
YAG: yttrium aluminium garnet, a crystal host which can be doped
with an active laser medium, usually neodymium.
YALO: yttrium aluminate (YA103), a crystal host doped with an
active laser medium, usually neodymium.
YLF: yttrium lithium fluoride, a crystal host which can be doped
with an active laser ion, usually holmium.
Absolute values of spectral reflectance are relatively
unimportant because such values vary only by a factor of 10 - 20,
whereas the laser beam irradiance may exceed the applicable EL by
orders of magnitude above this factor.
Most reported laser accidents have occurred, when the
probability of exposure was very high. No discussion of reflection
hazards is therefore complete without the consideration of the
probability of exposure. It must be remembered that the underlying
philosophy of the classification system is that control measures
should increase with increasing risk of exposure as well as with
increased severity of exposure.
12.2.2. Retroreflection
Some materials exhibit a property known as retrodirective
reflection. The reflection does not obey either the law of regular
(specular) reflection, or the cosine dependence of Lambertian
reflection. A collimated indigent beam may remain collimated and
be redirected along the original axis of propagation, regardless of
the angle of incidence at the retroflector. Corner cubes and some
specialized highway signs are examples of retroflectors.
12.2.3. Optically aided viewing
Nearly all laser workers know that viewing a laser source with
a telescope may substantially increase the risk. This increase in
risk is most dramatic for intra-beam viewing of a collimated
source. In this case, an increase in the power entering the eye is
possible, because the diameter of the objective (Do) of the
telescope or binocular is much larger than the pupil of the eye dp.
The actual increase in risk (G) depends on whether the pupil of the
eye is larger or smaller than the exit pupil (De) of the optical
system, the spectral transmittance (taulambda) of the optical
system at the laser wavelength(s), and the beam diameter relative
to the objective (collecting aperture) diameter.
When a bright object, larger than a point source, is viewed
through a well-designed optical system, the radiant power reaching
the retina (visible and IR-A) is theoretically increased by the
square of the instrument's magnifying power. However, since there
is a commensurate increase in the area of the retinal image, the
retinal irradiance remains unchanged, except for a slight reduction
because of reflective loss and the absorption of light in the
optical system. The retinal hazard in this case may increase in
some instances, since the thermal retinal injury threshold
decreases with increasing image size.
13. ACCIDENTAL INJURIES
At present, retinal injuries with loss of sight following
exposure to visible and IR-A laser radiation have been the most
catastrophic of all effects from laser radiation (Boldry et al.,
1981; Zhokov, 1981). Though the relatively high-powered, far-
infrared lasers such as the cw, carbon-dioxide laser, have caused
numerous burns to the hands and clothes, these are considered
inconsequential in comparison with the serious retinal injuries.
One postal survey conducted several years ago (Rockwell & Goldman,
1974) appeared to indicate that there had been at least 100
injuries to the eye from laser radiation in the USA. One
subjective account in this regard was that of Decker (1977).
Despite such reports, surprisingly few serious injuries of the
eye have been reported in the last 15 years in relation to exposure
to pulsed lasers. This low accident rate cannot be accounted for
by assuming that the ocular ELs are too conservative. The
explanation is probably that accidental exposure of the eye to a
collimated beam is normally an extremely remote possibility, if
precautions are taken to keep the eye out of the beam. One of the
few situations in which the probability of hazardous exposure is
great is during work in the laboratory and, each year, several
retinal injuries are reported under these conditions. However, it
is difficult to ascertain the exposure conditions in sufficient
detail for useful threshold or injury data to be derived. Concern
may also exist regarding the potential bias in an individual's
description of the accidental exposure conditions to support a
claim of compliance with safety measures. It is not clear whether
laser exposures are always detected by the exposed individual, and
this may be a particular problem with IR lasers (Kasuba & Akifev,
1977). It is known that retinal injury outside the macula may have
little or no effect on everyday visual performance and therefore
may not be detected subjectively.
14. CONTROL MEASURES
Risk control guidelines are not mutually exclusive. Following
one or two guidelines may reduce the risk to such an extent that
other recommended control measures, in that particular class, are
no longer essential. For example, if the beam path of a Class 4
laser were enclosed, then it would hardly be necessary to remove
all glass objects, or other specular surfaces near the beam path
but outside the enclosure, nor would it seem necessary to wear eye
protectors. However, the eye protection might be necessary if the
enclosure were being modified or during initial alignment. The
decision to use any particular set of controls depends on use
conditions and whether general population exposure is likely.
Table 15 provides a brief list of the most commonly recommended
laser control measures.
Table 15. Control measures for general population and occupational
exposure
-------------------------------------------------------------------
I Engineering control measures:
protective housing enclosure and service panel requirements;
interlocks on the protective housing;
door interlocks and remote control connector;
beam attenuator or beam shutter;
key switch or padlock over aperture cover;
filtered viewing optics and windows;
emission delay (BRH);
warning lights;
emission indicators (audible or visible);
enclosed area or room;
beam enclosure;
remote firing and/or monitoring;
II Personal protective equipment:
eyewear;
clothing;
gloves;
III Administrative and procedural controls:
laser safety officer;
standard operating procedures (SOPs);
limitations on use by class;
education and training;
maintenance and servicing manuals;
marking of protective devices;
warning signs and labels;
entry limitations for visitors, etc.;
accident procedures.
-------------------------------------------------------------------
Because of the risk associated with exposure to Class 4 high-
risk lasers, the safety precautions associated with these laser
installations indoors, generally include the installation of door
interlocks to prevent exposure of unauthorized or transient
personnel entering the laboratory, the use of baffles to terminate
the primary and any secondary beams, and the use of safety eyewear
by personnel within the interlocked facility (Klost, 1971).
At one time, it was recommended that ambient light levels
should be sufficient to constrict pupils. However, since a
constricted pupil provides only a small safety factor, the
requirement for good illumination, which remains in present safety
standards, is related to good general visibility, as the wearing of
eye protectors reduces visual capabilities. Light-coloured, matt
surfaces in the room minimize glare, and thus promote visibility.
In summary, the ability to analyse potential risks from any
laser system is enhanced by a broad knowledge of optics, general
laser technology, and the imaging process of the human eye. A
laser safety specialist should have a general background knowledge
of optics with the basic knowledge necessary to perform a risk
analysis. It has been shown that the risk analysis depends on at
least three aspects - the laser system and its potential hazards,
the type of personnel who may be exposed, and, finally, the
reflective materials and other optically important materials in the
environment that can influence the risk analysis.
15. HAZARDS OF LAMP SOURCES AND PROJECTION SYSTEMS
The optical radiation emitted by a conventional light source,
either a bare lamp, a luminaire, or a projection system, can be
evaluated using the previously mentioned tentative exposure limits
or guidelines.
Prior to exhaustive measurements and safety calculations, it
may be worthwhile to determine the need for a comprehensive risk
evaluation. Many categories of lamps or other types of light
sources can be excluded from all or several of the evaluations.
The following multi-step scheme (Sliney & Wolbarsht, 1980) may be
useful in this regard.
STEP 1 - Categorization of the lamp. Certain hazards are specific
for certain types of lamp or light source. The following grouping
is useful:
(a) incandescent lamps and incandescent heating sources;
(b) low-pressure discharge lamps;
(c) fluorescent lamps;
(d) high-intensity discharge (HID) lamps;
(e) short-arc (compact arc) lamps;
(f) carbon arcs;
(g) solid-state sources (LEDs etc.);
(h) cathode-ray tubes (CRTs).
STEP 2 - Determination of the source envelope. Any glass between
the actual source of radiation (e.g., the arc or tungsten filament)
and the point of access can greatly influence the potential hazard.
Soft (lime) glass of any reasonable thickness will greatly
attenuate UV-B and UV-C radiation.
(a) Incandescent lamps, other than quartz-halide lamps,
normally have a sufficiently thick glass envelope to
completely preclude a UVR hazard. The blue-light
hazard does not appear to be theoretically possible
at black-body temperatures below 2000 K (Sliney &
Wolbarsht, 1980), but most filaments operate at
effective temperatures exceeding 2000 K.
(b) Low-pressure discharge lamps. Low-pressure discharge
lamps do not normally present a retinal hazard,
because of the relatively low radiance. Only lamps
with quartz envelopes can transmit sufficient UV-B
and UV-C to be of concern. Of the common low-pressure
lamps, only mercury lamps can create a severe UVR
hazard. Many may be quite hot to the touch.
(c) Fluorescent lamps. Low-pressure tubular lamps in
almost all cases have a thin glass envelope, but
could often present a potential UVR hazard at the
surface. They do not represent a thermal retinal
injury hazard and seldom a blue-light hazard.
(d) HID lamps. These lamps may present both blue-light
and thermal retinal hazards, and possible UVR
hazards. Since most lamp envelopes are glass, there
is little UV-B leakage. Nevertheless, the UV-B
leakage may be of concern at very short distances.
Quartz-mercury HID lamps require a UVR risk
evaluation. If the outer glass envelope of an HID
lamp breaks, hazardous UV levels will be emitted.
Governmental regulations in Canada and the USA
require HID lamps to have a self-extinguishing
feature to preclude this hazard, unless the packaging
clearly warns against use without adequate shielding.
(e) Short-arc lamps. Of all the electric lamp categories,
this group will require the most extensive risk
evaluation. All potential hazards may be present
(UV-B/C, UV-A, blue-light, retinal thermal injury,
and skin thermal injury). Because of the high
temperature of the arc, a quartz envelope (which
transmits UV-B and C) is characteristic. These lamps
are often used in UV photocuring processes in
industry (Moss, 1980).
(f) Carbon arcs. Where a glass lens or filter plate does
not exist between the open arc and a point of access,
the carbon arc, like the short-arc lamp, is
potentially injurious.
(g) Solid-state lamps (e.g., LEDs). The present solid-
state lamps including LEDs, which emit visible
radiation, do not present any health risk, regardless
of the type of envelope.
(h) Cathode-ray tubes (CRTs). Present CRTs emit optical
radiation at levels that could pose a potential
health hazard (Wolbarsht et al., 1980).
STEP 3 - The obtaining of available manufacturers' radiometric and
photometric data and lamp descriptions. Any radiometric or
photometric specification may be of value either for calculation or
for direct intercomparison with measurements. Spectral data are
most useful. The dimensions of the emitting area of the lamp will
be required for retinal hazard evaluation.
STEP 4 - Comparison of lamp specifications with those of previously
evaluated lamps. From experience, it is often possible to complete
the risk evaluation with this step.
STEP 5 - Performance of detailed spectroradiometric measurements,
when necessary. In addition, where feasible, measurements of
luminance, illuminance, and total irradiance should be performed.
These will provide confirmation of the spectroradiometric
measurements. The pulse duration must be measured for a pulsed
source.
STEP 6 - Determination of the source dimensions. A photograph and
microdensitometer scan of the negative may be necessary for a non-
uniform source. The maximum angular subtense alpha of the source
should be calculated at the point of human access or at 15 cm from
the source, whichever is closer.
STEP 7 - Estimation of the exposure and comparison with the
exposure limits to determine the degree of risk.
STEP 8 - Consideration of potentially hazardous failure modes. For
example, breakage of the outer envelope of some high-intensity
discharge (HID) lamps can create a serious UVR hazard (Anderson,
1980b).
16. PROJECTION OPTICS
Broad-band sources involving projection optics are most
difficult to evaluate. Besides the problems encountered in
evaluating exposed lamps, the projected beam and projected source
size must be characterized. When viewing a collimated light source
from within the beam (other than a laser), a magnified view of the
actual source will be seen. The source is generally a high-
brightness lamp. The brighter the lamp, the greater the maximal
irradiance in the projected beam. This is a consequence of the Law
of Conservation of Brightness (Radiance) (see, for example, Kline,
1970; or Sliney & Wolbarsht, 1980). Some usually safe lamps become
hazardous to view through projection optics, despite the fact that
the optics cannot make the lamp brighter. The risk increases
because of the dependence of retinal injury on image size. Besides
the obvious projection sources - such as spotlights, searchlights,
slide projectors, and film projectors - solar concentrators and
other non-imaging light collectors may also require risk
evaluation. From the Law of Conservation of Radiance, it is
possible to evaluate the retinal risks from projector systems.
Collimating optics may consist of refracting elements (lenses),
reflecting elements (curved mirrors), or both.
17. SAFETY GUIDELINES FOR HIGH-INTENSITY SOURCES
Since lamp or arc sources may be hazardous from several
aspects, it may be helpful to develop a safety classification
scheme, similar to the one applied to laser products. The
following scheme of Sliney & Wolbarsht (1980) illustrates this
approach to evaluate the retinal risks from projector systems.
Both lamps and total lighting systems could be included. The
categories could be as follows:
Safety Group 1: Safe sources. These lamps are considered
safe to view throughout the day. No warning label would be
required. Examples: a frosted 15-W filament lamp or a
TV-display, cathode-ray tube.
Safety Group 2: Low-risk sources. These lamps are safe
for momentary 0.25-s, unintentional viewing. Examples:
most spotlights and film-projector lamp bulbs. A caution
label should be required on the lamp base, and possibly on
the projection system itself. No ultraviolet or infrared
hazard would exist at distances of more than 10 cm from
the lamp or projected beam.
Safety Group 3: Moderate-risk sources. These lamps would
be unsafe to view at close range, even momentarily.
Presumably, skin injury could also occur from ultraviolet
radiation as from germicidal lamps, sun lamps, and high
intensity UV-A lamps. A danger-label, clearly visible on
the equipment, could be required. A common lamp that might
fit into this category would be a 600-1000-W tungsten-
halogen lamp without a Fresnel lens, such as is used for a
home cine film spot lamp. The emergent beam irradiance is
far in excess of that required to ignite paper within half
a metre of the source. Obviously, the basis for the
determination of a hazard classification would differ
according to whether the hazard classification criteria
were based on retinal or skin injury. Each measurement for
classification would be for a specified accessible
approach distance, using a standard aperture and solid
angle of acceptance. The minimum approach distance could
vary with application. Other examples that might be
included in this category are some very high intensity,
short-pulse, laser flash tubes, and 20 kW xenon-arc
searchlights.
Safety Group 4: High-risk sources. These sources would
cause skin burns and/or erythema within a standardized
period of exposure (e.g., within 10 s) at a standardized
distance at which the effective UV irradiance would exceed
3 W/m2 (0.3 mW/cm2), or the total irradiance across the
entire spectrum would exceed 2 kW/m2 (0.2 W/cm2). Examples
of such sources are an open carbon-arc spotlight or an
open 1-kW mercury lamp. It may be that safety groups 3 and
4 are so similar in degree of risk, that they could be
combined.
18. WELDING ARCS
The most common high-intensity arc is probably the welding arc.
These arcs vary in brightness and in UVR content, primarily
according to the arc current, type of shielding gas, and the metals
being welded.
The greatest population exposed to intense sources of optical
radiation are welders and their assistants. The American Welding
Society estimated that there may be as many as 500 000 welders in
the USA alone (Emmett & Horstman, 1976). The two broad categories
of welding equipment are gas (acetylene) welding equipment and
electric-arc welding equipment. A gas welding torch or cutting
torch has a luminance not much greater than a candle flame,
typically ranging from 10 to 200 kcd/m2 (1-20 cd/cm2), and the UVR
emission is quite small. The optical radiation hazards of such
torches are virtually nonexistant. Welding filter goggles used
with such torches are to reduce glare, and are little darker than
very dark sunglasses having a shade number of the order of 3 - 5
(visual transmittance of 5 - 15 %). On the other hand, electric
welding arcs may be 1000 times brighter than gas torches and emit
UVR at proportionately higher levels (Sutter et al., 1972).
Protective shields, curtains, screens for bystanders, and
welders' goggles are the standard protective equipment used in
welding (Mayer et al., 1979; Sliney et al., 1981). Protective
procedures and protective equipment for the welder have been
developed empirically over the last three-quarters of a century.
Only very recently have detailed measurements of the radiometric
output of welding arcs been available. When these measurements
were carefully compared with exposure limits being developed for
protection against bright light sources, it was shown that the
empirically-developed protective equipment standards were adequate.
19. EYE AND SKIN PROTECTION
19.1. Laser Safety Eyewear
From a safety point of view, the most desirable laser hazard
control measure is complete enclosure of the laser or laser system;
however, this may not always be practical and laser eye protectors
are generally the best alternative. Though most industrial laser
applications do not require the use of eye protectors, this is not
always true for laser applications in the research laboratory. Eye
protectors provide the simplest solution to the laser safety
problem for a constantly changing experimental arrangement. Several
factors play a role in determining whether eyewear is necessary in
any situation. At least three output parameters of the laser must
be known: maximum exposure duration, wavelength, and output power
(or output irradiance, or radiant exposure, or energy), as well as
the applicable safe corneal radiant exposure. In addition, some
knowledge of such environmental factors as ambient lighting and the
nature of the laser operation may also be required.
Laser eye protection generally consists of a filter (often
composed of several individual filter plates) which selectively
attenuates at specific laser wavelengths, but elsewhere transmits
as much visible radiation as possible (Swope & Koester, 1965;
Schreibeis, 1968; Scherr et al., 1969; Swope, 1969, 1970; Straub,
1970; Sliney, 1974). Eyewear is available in several designs -
spectacles, coverall types with opaque side-shields, and coverall
types with somewhat transparent filter side-shields. The selection
of appropriate laser protective eyewear may be complex (Envall &
Murray, 1979). Active electronic imaging devices have also served
an additional role, as eye protection.
19.2. Welders' Filters
Eye protection filters, which were originally developed for
welders, were based more on available materials than on knowledge
of ocular protection requirements. The first organized study of
glass filter materials was carried out by Sir William Crookes
(1914) in England. Optical transmission characteristics are now
standardized as "shades" and specified for particular applications
(Coblentz et al., 1931; Stair, 1948; ANSI, 1978). Though maximum
transmittances for ultraviolet and infrared radiation are specified
for each shade, the mean photopic visual transmittance tauv, or
visual optical density Dv, has traditionally been used to define
the shade number S:
S = (7/3) Dv + 1 = - ln tauv + 1 Equation (23)
or Dv = (3/7) (S - 1) Equation (24)
where Dv = -log10 tauv Equation (25)
19.3 Eye Protection for Furnace Radiation
As well as protective clothing and equipment, many industrial
methods now used probably reduce the level of glass furnace
radiation to which the eye is exposed. For instance, the openings
to higher temperature furnaces are a great deal smaller than they
have been in past years; this would reduce the total irradiance of
the eye from infrared radiation. There are sufficient data and
cases of a very specific form of cataract in workers to suggest
that infrared does, indeed, cause glass-blower's or furnaceman's
cataract (Duke-Elder, 1972).
19.4. Eye Protection Filters for Solar Radiation
Direct viewing of the sun, for whatever reason, requires
protection against several different portions of the spectrum. A
yellowish or reddish filter generally protects against ultraviolet
radiation. Protection against intense visible rays should be
weighted to filter out more of the blue-light than the rest of the
visible spectrum. It is generally found that a shade 12 or 13
welder's filter is quite adequate to protect against ultraviolet
radiation, infrared, and visible radiation. The protection
afforded against the IR, however, is far greater than necessary.
The use of darkened coloured slides is not advisable, since
these slides (usually made by developing unexposed colour film) use
organic dyes that transmit in the near-infrared (IR-A) spectral
band.
19.5. Skin Protecting Agents for UVR (Sunscreens)
A number of topical, physical, and chemical screening agents
have been developed that provide nearly total or partial filtration
of ultraviolet radiation. Since actinic UV-B and UV-C radiation
are the most hazardous, efforts to develop topical agents have
concentrated primarily on filtering out this type of radiation. The
chemical agents in these "sunscreens" include para-aminobenzoic
acids (PABA) and its esters, salicylates, and cyanamates. These
materials are mixed in solution with substances that have good
substantivity (i.e., adhere to the skin) (Dahling et al., 1970;
Fitzpatrick et al., 1974).
19.6. Protective Garments
Aluminized fabrics were greatly improved during various manned
space programmes (Stoll & Chiantra, 1971). Such fabrics, when used
in thermal protective garments, have been shown to offer equivalent
or superior reflective and mechanical properties compared with
conventional aluminized asbestos garments (Wren et al., 1977).
Aluminized rayon (basket weave) and certain aluminized cottons were
shown to allow the least transmission of infrared radiation.
20. MEDICAL SURVEILLANCE (RATIONALE)
In the past two decades, many employees working routinely with
lasers have been subjected to preplacement, periodic, and end-of-
job eye examinations in order to obtain sufficient information
concerning the risk of retinal damage. Many of these studies
indicated that periodic eye examinations rarely located hitherto
unsuspected retinal damage. In general, published reports of
ophthalmic accidents have been those in which the acute over-
exposure was sufficient to subjectively alert the individual
(Hathaway et al., 1977). Thus, many authorities (Suess, ed., 1982)
suggest that ophthalmic examinations are unnecessary for
individuals routinely working with Class 1 and 2 lasers, and that,
if requested, the examinations should be confined to those working
with Class 3 or 4 systems only.
An examination is required within 24 - 48 h of any event in
which the worker suspects, or knows, that the eye might have been
exposed. Laser lesions change in appearance and may even tend to
disappear within the heterogeneous appearance of the fundus within
a period of time, so that ophthalmic examinations, some time after
exposure, may be difficult to interpret.
21. FORMAL TRAINING FOR LASER WORKERS
It is necessary to establish a safety programme that assures
the safe use of lasers and other radiation sources. To assure
knowledge of, and compliance with, applicable standards, a certain
amount of formalized teaching is often necessary.
At work places, a specific individual should be assigned to
maintain and enforce the safety programme (in some countries this
individual is termed a laser safety officer (LSO)).
All workers occupied with, or working near, the radiation
source should be included in the teaching programme.
The object is to make workers and work leaders aware of the
risks of lasers, how to avoid the hazards, the proper use of
protective devices, and how to realize when overexposure has taken
place.
REFERENCES
ALLEN, R.G. (1980) Retinal thermal injury. In: Kelley, W.D.,
ed. Non-ionizing radiation, Cincinnati, OH, ACGIH, pp. 161-168.
ACGIH (1976) A guide for control of laser hazards, Cincinnati,
OH, American Conference of Governmental Industrial Hygienists.
ACGIH (1981) Threshold limit values for chemical substances
and physical agents in the workroom adopted by ACGIH for 1981,
Cincinnati, OH, American Conference of Governmental Industrial
Hygienists.
ANDERSON, F.A. (1980a) The biological basis for standards,
Rockville, MD, US Dept. of Health, Education and Welfare, Food
and Drug Administration, Bureau of Radiological Health.
ANDERSON, F.A. (1980b) Sodium and mercury vaporlamps. In:
Kelley, W.D., ed. Non-ionizing radiation, Cincinnati, OH,
ACGIH, pp. 239-243.
ANDERSON, R.R. & PARRISH, J.A. (1981) The optics of human
skin. J. Invest. Derm., 77: 13-19.
ANSI (1978) Standard practice for occupational eye, and face
protection, New York, American National Standards Institute
(ANSI Standard Z-89.1).
ANSI (1980) Safe use of lasers, New York, American National
Standards Institute (ANSI Standard Z-136.1).
AVDEEV, P.S., BEREZIN, Yu.D., GUDAKOVSKII, Yu.P., MURATOV,
V.R., MURZIN, A.G., & FROMZEL, V.A. (1978) Experimental
determination of maximum permissible exposure to laser
radiation of 1.54 µ wavelength. Sov. J. quant. Electr., 8:
134-141.
BEATRICE, E.S. & LUND, D.J. (1979) Characteristics of damage
produced by non-circular retinal laser radiation, San
Francisco, CA, Letterman Army Institute of Research,
(Institute Report No. 31, AD-AD35 878/8ST).
BEATRICE, E.S. & VELEZ, S. (1978) Laser safety bioeffects
research: histopathology of retinal effects. In: SPIE Proc.,
Visual simulation: 162: 103-106.
BERGQUIST, T., HARTMANN, B., & KLEMAN, B. (1978) Imaging
properties of the eye and interaction of laser radiation with
matter. In: Tengroth, B. & Epstein, D., ed. Current concepts
in ergophthalmology, Stockholm, Karolinska Institute.
BIRNGRUBER, R. (1978) [Experimental and theoretical
investigations into thermal injury to the retina from laser
radiation.] PhD Dissertation, Frankfurt, J.W. Goethe
University (in German).
BOLDRY, E.E., LITTLE, H., FLOCKS, M., & VASSILIADIS, A. (1981)
Retinal injury due to industrial laser burns. Ophthalmol., 88:
101-107.
BORLAND, R.G., BRENNAN, D.H., & NICHOLSON, A.N. (1971)
Threshold levels for damage of the cornea following
irradiation by a continuous wave carbon dioxide (10.6 micron)
laser. Nature (Lond.), 234: l5l-l52.
BORLAND, R.G., BRENNAN, D.H., MARSHALL, I.J., & VIVASH, J.P.
(1978) The role of fluorescein angiography in the detection of
laser induced damage to the retina .. a threshold study for
Q-switched neodymium and ruby laser. Exp. Eye Res., 27:
471-493.
BROWN, J.L. (1973) Experimental investigations of flash
blindness. Hum. Factors, 6: 503-516.
CAMPBELL, C.J., RITTLER, M.C., BREDEMEIER, H., & WALLACE, R.A.
(1968) Ocular effects produced by experimental lasers. I.
Carbon dioxide laser. Am. J. Ophthalmol., 66: 604-614.
CIE (1970) International lighting vocabulary, Paris, Bureau
Central de la Commission Internationale de l'Eclairage, Vol.
3, p. 5l.
CLEVET, A. & MAYER, A. (1980) Risques liés à l'utilisation
industrielle des lasers. Cahiers de notes documentaires INRS,
No 99, 2è trimestre, pp. 207-222.
COBLENTZ, W.W., STAIR, R., & HOGUE, J.M. (1931) The spectral
erythemic reaction of the human skin to ultraviolet radiation.
Proc. Natl Acad. Sci., 17(6): 401-405.
COGAN, D.G. & KINSEY, V.E. (1946) Action spectrum of keratitis
produced by ultraviolet radiation. Arch. Ophthalmol., 77:
670-677.
CONSIDINE, P.S. (1966) Effects of coherence on imaging
systems. J. Opt. Soc. Am., 56: 1001-1009.
CORNSWEET, T.N., ed. (1966) Visual perception, New York,
Academic Press.
COURT, L., CHEVALEREAUD, J.P., & SANTUCCI, G. (1978) Exposé
général. In: Sociéte française de Radioprotection, 9è Congrès
international: Effets biologiques des Rayonnements non
ionisants. Utilisation et Risques associés. Monte-Carlo,
Monaco, pp. 367-445.
CROOKES, W. (1914) The preparation of eye-preserving glass for
spectacles. Phil. Trans. Roy. Phil. Soc., A204: 1-25.
DAHLING, R.F., SHAPIRO, S.I., BERRY, C.Z., & SCHREIBER, M.M.
(1970) A method of evaluating sun screen protection from
long-wave ultraviolet. J. Invest. Derm., 55: 164-169.
DAUTRAY, R. & WATTEAU, J.P. (1980) La fusion inertielle par
laser. Rev. gén. nucl., No. 6, pp. 562-575.
DAVIES, J.M. (1959) The effects of intense thermal radiation
on animal skin. A comparison of calculated and observed burns,
Natick, MA, Army Quartermaster Research and Engineering
Command (Report T-24, 29 April 1959, NTIS AD 456794).
DAVSON, H., ed. (1962) The eye (4 volumes), New York, Academic
Press.
DECKER, D. (1977) An accident victim's view. Laser Focus,
13(8): 6.
DECOMPS, B. (1981) Le laser, instrument de recherche et
facteur de développement. Rev. gén. d'Elect., 90(1): 11-29.
DE GRUIJL, F.R. & VAN DER LEUN, J.C. (1980) A dose-response
for skin cancer induction by chronic UV exposure of a human
population. J. Theor Biol., 83; 487-504.
DUKE-ELDER, S. (1972) Textbook of ophthalmology, Vol. VI,
Injuries, St. Louis, Mosby, C.V.
EMMETT, E.A. & HORSTMAN, S.W. (1976) Factors influencing the
output of ultraviolet radiation during welding. J. occup.
Med., 18(1): 41-44.
ENVALL, K.R. & MURRAY, R. (1979) Evaluation of commercially
available laser protective eyewear, Rockville, MD, US Dept of
Health Education and Welfare, Food and Drug administration,
Bureau of Radiological Health. (DHEW Publ. No. (FDA) 79-8086).
ERNEST, J.T. & POTTS, A.M. (1971) Pathophysiology of the
distal portion of the optic nerve. IV. Local temperature as a
measure of blood flow. Am. J. Ophthalmol., 72(2): 435-444.
FITZPATRICK, T.B., PATHAK, M.A., HARBER, L.C., SEIJI, M., &
KUKITA, A. (1974) Sunlight and man, normal and abnormal
photobiologic responses, Tokyo, University of Tokyo Press.
FRANCE, Arrêté du 30 janvier (1974) Réglementation concernant
les lasers à usage médical. J.O. 17 mars 1974, p. 3093.
FRANCE, Arrêté du 13 mai (1974) Conditions techniques
générales des lasers à usage médical. J.O. 15 juin 1974,
p. 6388.
FRANCE, Arrêté du 14 mai (1974) Conditions techniques des
lasers à usage médical de catégorie II, groupe I, sous-groupe
I. J.O. 15 juin 1974, p. 6388.
FRANCE, Arrêté du 29 décembre (1976) Classification des lasers
à usage médical de catégorie II, groupe II (émission
continue). J.O. 22 janvier 1977, (Numéro complémentaire)
p. 466.
FRANCE, Arrêté du 10 janvier (1978) Conditions techniques
d'utilisation des lasers à usage médical de catégorie II,
groupe II. J.O. 28 janvier 1978 (Numéro complémentaire) p. 822.
FRIED, D.L. (1981) Laser eye safety: The implications of
ordinary speckle and speckled-speckle statistics. J. Opt. Soc.
Am., 71(7): 914-916.
FRISCH, G.D., BEATRICE, E.S., & HOLSEN, R.C. (1971)
Comparative study of argon and ruby retinal damage thresholds.
Invest. Ophthalmol., 10: 911-919.
GABEL, V.P. & BIRNGRUBER, R. (1981) A comparative study of
threshold laser lesions in the retinae of human volunteers and
rabbits. Health Phys., 40: 238-240.
GABEL, V.P., BIRNGRUBER, R., & HILLENKAMP, F. (1976) [Light
absorption in the fundus oculi.] Munich, Association for
Research on Radiation and the Environment (GSF report A55) (in
German).
GEERAETS, W.J. & BERRY, E.R. (1968) Ocular spectral
characteristics as related to hazards from lasers and other
light sources. Am. J. Ophthalmol., 66: 15-20.
GIESE, A.C. (1976) Living with our sun's ultraviolet rays,
New York, Plenum Publishing Corporation.
GOLDMAN, L., ed. (1981) The biomedical laser technology and
clinical applications, New York, Heidelberg, Berlin, Springer
Verlag.
GOLDMAN, L., ROCKWELL, R.J., & RICHFIELD, D. (1971) Long-term
laser exposure of a senile freckle. Arch. environ. Health, 22:
401-403.
GOLDMAN, L., ROCKWELL, R.J., MICHAELSON, S.M., SLINEY, D.H.,
TENGROTH, B.M., & WOLBARSHT, M.L. (1982) Optical radiation,
with particular reference to lasers. In: Suess, M. ed.
Nonionizing radiation, Copenhagen, World Health Organization,
Regional Office for Europe.
GOLDMANN, H. (1933) Genesis of heat cataract. Arch.
Ophthalmol., 9: 314.
GORODETSKI, A.A., KIRICINSKI, B.R., EVDOKOMOB, I.R., &
KOLESNIK, V.M. (1968) [Some data on the biological action and
radiation protection of optical quantum generators.] Gig. Tr.
Prof. Zabol., 12: 37-41 (in Russian).
GREISEMANN, J.C. & MARTI, J. (1978) Risques liés à
l'utilisation des lasers de puissances. In: Société française
de Radioprotection, 9è Congrès international. Effets
biologiques des Rayonnements non ionisants. Utilisation et
Risques associés, pp. 473-482.
GREISS, G.A., BLANKENSTEIN, F., & WILLIFORD, G.G. (1980)
Ocular damage thresholds from multiple-pulse laser exposures,
Health Phys., 39: 921-927.
GRUM, F.C. & BECHERER, R., ed. (1979) Optical radiation
measurements, Vol. 1, Radiometry, New York, Academic Press,
p. 352.
GULLBERG, K., HARTMAN, B., KOCK, E., & TENGROTH, B. (1967)
Carbon dioxide laser hazards to the eye. Nature (Lond.), 215:
857-858.
HAM, W.T. Jr, WILLIAMS, R.C., MUELLER, H.A., GUERRY, D.,
CLARKE, A.M., & GEERAETS, W.J. (1966) Effects of laser
radiation on the mammalian eye. Trans. NY Acad. Sci., 28:
517-526.
HAM, W.T. Jr, CLARKE, A.M., GEERAETS, W.J., CLEARY, S.F.,
MUELLER, H.A., & WILLIAMS, R.C. (1970) The eye problem in
laser safety. Arch. environ. Health, 20: 156-160.
HAM, W.T. Jr, MUELLER, H.A., & SLINEY, D.H. (1976) Retinal
sensitivity to damage from short wavelength light. Nature
(Lond.), 260(5547): 153-155.
HAM, W.T. Jr, MUELLER, H.A., RUFFOLO, J.J., & CLARKE, A.M.
(1978) Sensitivity of the retina to radiation damage as a
function of wavelength. Photochem. Photobiol., 29: 735-743.
HAMERSKI, W. (1969) Investigations on histochemical changes in
experimental corneal lesions induced with UV radiation and on
the prevention of photophthalmia. Pol. med. J., 8: 1469-1476.
HANSEN, W.P. & FINE, S. (1968) Melanin granule models for
pulsed laser induced retinal injury. Appl. Opt., 7: 155-159.
HARDY, J.D. (1968) Pain following step increase in skin
temperature. In: Kenshalo, D.R. ed. The skin senses,
Springfield, IL, Charles C. Thomas, pp. 444-456.
HARDY, J.D., HAMMEL, H.T., & MURGATROYD, D. (1956) Spectral
transmittance and reflectance of excised human skin. J. appl.
Physiol., 9: 257.
HARLEN, F. (1978) The development of laser codes of practice
and maximum permissible exposure levels. Ann. occup. Hyg.,
2l(2): 199-211.
HARTMANN, B. & KLEMAN, B. (1980) Exposure limits for
broad-band 400-1400 nm radiation. Ocular effects of
non-ionizing radiation. Proc. SPIE, 29: 105-114.
HARWERTH, R.S. & SPERLING, H.G. (1975) Effects of intense
visible radiation on the increment threshold spectral
sensitivity of the Rhesus monkey eye. Vision Res., 15:
1193-1204.
HATFIELD, E.M. (1970) Eye injuries and the solar eclipse.
Sight Sav. Rev., pp. 79-85.
HATHAWAY, J.A., STERN, N., SOLES, E.M., & LEIGHTON, E. (1977)
Ocular medical surveillance on microwave and laser workers. J.
occup. Med., l9(10): 683-688.
HAUSSER, K.W. (1929) [Influence of wavelength in radiation
biology.] Strahlenther., 28: 25-44 (in German).
HOLZINGER, G., KROY, W., SCHREIBER, P., & SUTTER, E. (1978)
Protection from law radiation (Series on Workplace Protection,
no.14).
INTERNATIONAL ORGANIZATION FOR STANDARDIZATION (1980) Personal
eye-protectors for welding and related techniques. Welding
filters, Geneva (ISO 4850).
IRPA (1977) Overviews on nonionizing radiation, International
Radiation Protection Association Report of a Study Group.
JAMES, R.H., ed. (1976) National Conference on Measurements
of Laser Emissions for Regulatory Purposes, April, Rockville,
MD, US Dept of Health, Education and Welfare, Food and Drug
Administration, Bureau of Radiological Health (HEW Publ. (FDA)
76-8037).
KASUBA V.A. & AKIFEV, S.A. (1977) [Working conditions and
morbidity among workers preparing clock jewels using lasers
and mechanical techniques.] Gig. Tr. Prof. Zabol., 1: 37-40
(in Russian).
KAUFMANN, E. (1970) Laser hazard to the human eye. Schweiz
Arch., 36: 211.
KLINE, M.V. (1970) Optics, New York, John Wiley and Sons.
KLOST, W. (1971) [Safety measures in the use of laser rays.]
Zentralbl. Arbeitsmed., 21: 105-111 (in German).
KOGELNIK, H. & LI, T. (1966) Laser beams and resonators. In:
Levine, A.K., ed. Lasers. New York, Decker.
KOMAROVA, A.A., MOTZERENKOV, V.P., SKATSKAIA, G.K., CEMNY,
A.B., & PIVOVAROV, N.N. (1978) [Action of reflected laser
radiation on the eye.] Vestn. Oftal., l: 46-50 (in Russian).
KUWABARA, T. (1970) Retinal recovery from exposure to light.
Am. J. Ophthalmol., 70(2): 187-189.
LA VAIL, M.M. (1980) Eye pigmentation and constant light
damage in the rat retina. In: Williams, T.P. & Baker, B.N.,
ed. The effects of constant light on visual processes, New
York, London, Plenum Press, pp. 357-387.
LAWWILL, T., CROCKET, S., & CURRIER, G. (1977) Retinal damage
secondary to chronic light exposure thresholds and mechanisms.
Doc. Ophthalmol., 44(2): 379-402.
LE BODO, H. (1976) La calorimétrie appliquée à la mesure des
puissances et énergies lasers. Bulletin d'information du
Bureau National de Métrologie, No. 24, pp. 12-18.
LEIBOWITZ, H.M. & PEACOCK, G.R. (1969) Corneal injury produced
by carbon dioxide laser radiation. Arch. Ophthalmol., 8l:
712-721.
LERMAN, S. (1980a) Radiant energy and the eye, New York,
Macmillan Publ. Co.
LERMAN, S. (1980b) Human ultraviolet radiation cataracts.
Ophthal. Res., 12: 303-314.
LIVINGSTON, P.C. (1932) The study of sun glare in Iraq. Br. J.
Ophthalmol., 6: 577-625.
LOWE, D.A. (1975) A guide to international recommendations on
names and symbols for quantities and on limits of measurement.
Geneva, World Health Organization (Progress in Standardization: 2).
MAGNUS, I.A. (1976) Dermatological photobiology, London,
Blackwell Scientific Publications.
MAINSTER, M.A., WHITE, T.J., TIPS, J.H., & WILSON, P.W. (1970)
Retinal-temperature increases produced by intense light
sources. J. Opt. Soc. Am., 60: 264-270.
MARSHALL, J. (1970) Thermal and mechanical mechanisms in laser
damage to the retina. Invest. Ophthalmol., 9: 97-115.
MARSHALL, J. (1973) Laser damage to ocular tissues. Proc. R.
Soc. Med., 66(9): 842-844.
MARSHALL, J. (1978) Retinal injury from chronic exposure to
light and the delayed effects from retinal exposure to intense
light sources. In: Tengroth, B. & Epstein, D., ed. Current
concepts in ergophthalmology, Stockholm, Karolinska Institute,
pp. 81-104.
MARSHALL, J. & BIRD, A.C. (1979) A comparative histo-
pathological study of argon and krypton laser irradiations of
the human retina. Br. J. Ophthalmol., 63(10): 657-668.
MARSHALL, W.J. (1980) Optical measurement techniques. In:
Kelley, W.D., ed. Non-ionizing radiation, Cincinatti, OH,
ACGIH, pp. 175-179.
MAYER, M.A. & SALSI, M.S. (1979) Rayonnement ultraviolet,
visible et infrarouge, mésure-evaluation des risques. INRS
Cahiers de Notes documentaires, No. 96, 3e trimestre, 403-413.
MEDOVSKAYA, T.P. (1970) Data on the condition of the eye in
workers at a glass factory. Hyg. Sanit., 35: 446-447.
MESTER, E. (1980) L'effet stimulant des faisceaux laser sur la
cicatrisation des plaies. Rev. Iéna, No. 3, pp. 121-122.
MIRO, L. (1979) Le laser et ses applications médio-
chirurgicales. Semaine des hôpitaux de Paris, 55(41-42):
1956-1964.
MOON, M.E., CLARKE, A.M., RUFFALO, J.J. Jr, & MUELLER, H.A.
(1978) Visual performance in the Rhesus monkey after exposure
to blue light. Vision Res., 18: 1573-1577.
MOSS, C.E. (1980) Radiation hazards associated with
ultraviolet radiation curing processes. In: Kelley, W.D., ed.
Non-ionizing radiation, Cincinnati, OH, ACGIH, pp. 203-209.
NOELL, W.K. & ALBRECHT, R. (1971) Irreversible effects of
visible light on the retina, role of vitamin A. Science, 172:
76-79.
PARR, W.H. (1969) Skin lesion threshold values for laser
radiation as compared with safety standards, Fort Knox, KY, US
Army Medical Research Laboratory (Report 8l3, AD 688871).
PARRISH, J.A., ANDERSON, R.R., URBACH, F., & PITTS, D. (1978)
UVA biological effects of ultraviolet radiation with emphasis
on human responses to longwave ultraviolet, New York, Plenum
Publishing Corporation.
PARVER, L.M., ANKER, C., & CARPENTER, D.O. (1980) Choroidal
blood flow as a heat dissipating mechanism in the macula. Am.
J. Ophthalmol., 89: 641-646.
PECKHAM, R.H. & HARLEY, R.D. (1951) The effect of sunglasses
in protecting retinal sensitivity. Am. J. Ophthalmol., 34(11):
1499-1507.
PENNER, R. & McNAIR, J.N. (1966) Eclipse blindness. Am. J.
Ophthalmol., 61: 1452-1457.
PITTS, D.G. (1974) The human ultraviolet action spectrum. Am.
J. opt. S. physiol. Opt., 51: 946-960.
PITTS, D.G., CULLEN, A.P., & HACKER, P.D. (1977) Ocular
effects of ultraviolet radiation from 295 to 365 nm. Invest.
ophthalmol. Vis. Sci., 16(10): 932-939.
PRATESI, R. & SACCHI, C.A., ed. (1980) Lasers in photomedicine
and photobiology, Berlin, Springer-Verlag.
ROCKEROLLES, R. (1978) Dangers spécifiques du rayonnement
cohérent. Dangers habituels liés aux fortes luninances; effets
multiphotoniques et effets non linéaires. In: Société
française de Radioprotection. 9è Congrès international: Effets
biologiques des Rayonnements non ionisants. Utilisation et
Risques associés, Monte-Carlo, Monaco, pp. 453-472.
ROCKWELL, R.J. Jr, & GOLDMAN, L. (1974) Research on human skin
laser damage threshold, final report, Texas, USAF School of
Aerospace Med., Brooks AF Base (Prepared by Dept of
Dermatology and Laser Lab. Med. Centre, University of
Cincinnati, Contract F4l609-72-C-0007).
ROGER, F.C. (1973) Clinical findings, course and progress of
biatis corneal degeneration in the Dahlak Islands. Br. J.
Ophthalmol., 57: 657-661.
RUBIN, L.R. (1977) Lasers in biology, Moscow, Nauka.
SCHERR, A.D., TUCKER, R.J., & GREENWOOD, R.A. (1969) New
plastics absorb at laser wavelength. Las. Foc., 5(9): 46-48.
SCHREIBEIS, W.J. (1968) Laser eye protection goggles based on
maufacturer's information. Am. Ind. Hyg. Assoc. J., 29: 504.
SKEEN, C.H., BRUCE, W.R., TIPS, J.H. Jr, SMITH, M.G., & GARZA,
G.G. (1972) Ocular effects of repetitive laser pulses,
San Antonio, TX, Technology Inc. (Contract F41609-71-C-0018, AD
746795).
SLINEY, D.H. (1971) The development of laser safety
criteria-biological considerations. In: Wolbarsht, M.L., ed.
Laser applications in medicine and biology, New York, Plenum
Press, pp. 163-238.
SLINEY, D.H. (1972) The merits of an envelope action spectrum
for ultraviolet radiation exposure criteria. Am. Ind. Hyg.
Assoc. J., 33: 644-653.
SLINEY, D.H. (1974) Laser protective eyewear. In: Wolbarsht,
M.L., ed. Laser application in medicine and biology, New York,
Plenum Press, Vol. 2.
SLINEY, D.H. & FREASIER, B.C. (1973) The evaluation of optical
radiation hazards. Appl. Opt., 12(1): 1-24.
SLINEY, D.H. & WOLBARSHT, M.L. (1980) Safety with lasers and
other optical sources, New York, Plenum Publishing Corporation.
SLINEY, D.H., MOSS, C.E., MILLER, C.G., & STEPHENS; J.B.
(1981) Semitransparent curtains for control of optical
radiation hazards. Appl. Optics, 20(14): 2352-2366.
SMITH, H.E. (1944) Actinic macular retinal pigment
degeneration. US Nav. med. Bull., 42: 675-680.
SMITH, K.C. (1977) The science of photobiology, New York,
Plenum Press.
SMITH, K.C. (1978) Symposium on DNA repair and its role in
mutagenesis and carcinogenesis. Photochem. Photobiol., 28: 119.
STAIR, R. (1948) Spectral-transmissive properties and use of
eye-protective glasses. Washington, DC, National Bureau of
Standards (NBS Circular 471).
STOLL, A.M. & CHIANTRA, M.A. (1971) Heat transfer through
fabrics as related to thermal injury. Trans. N.Y. Acad. Sci.,
33: 649-670.
STOLWIJK, J.A.J. (1980) Infrared radiation and radiant heat
stress. In: Kelley, W.D., ed. Non-ionizing radiation,
Cincinnati, OH, ACGIH, pp. 171-174.
STRAUB, H.W. (1970) Laser eye protection in the USA.
Berufsgenossenschaft Z. Unfallv. Betrieb, 3: 83-87.
STUCK, B.E., LUND, D.J., & BEATRICE, E.A. (1981) Ocular
effects of holmium (2.06 µm) and erbium (1.54 µm) laser
radiation. Health Phys., 40: 835-846.
SUESS, ed. (1982) Nonionizing radiation protection,
Copenhagen, World Health Organization, Regional Office for
Europe.
SUTTER, E., HUEBNER, H.J., KRAUSE, E., & RUGE, J. (1972)
[Radiation measurements in various arc welding processes.]
Federal Republic of Germany, Federal Institute of Physics and
Technology (Report No. Optik 2/72) (in German).
SWOPE, C.H. (1969) The eye protection. Arch. environ. Health,
18: 428-433.
SWOPE, C.H. (1970) Design considerations for laser eye
protection. Arch. environ. Health, 20: 184-187.
SWOPE, C.H. & KOESTER, C.J. (1965) Eye protection against
lasers. Appl. Opt., 4(5): 523-525.
SYKES, S.M., ROBISON, W.G., WAXLER, M., & KUWABARA, T. (1981)
Damage to the monkey retina by broad-spectrum fluorescent
light. Invest. Ophthalmol. Vis. Sci., 20(4): 425-434.
TENGROTH, B.M. (1976) Safety glasses in welding. Env. Res.,
11:283-284.
TENGROTH, B.M., LYDAHL, E., & PHILIPSON, B.T. (1980) Infrared
cataract in furnacemen. In: Kelley, W.D., ed. Non-ionizing
radiation, Cincinnati, OH, ACGIH, pp. 169-170.
URBACH, R., ed. (1969) The biologic effects of ultraviolet
radiation, New York, Pergamon Press.
URBACH, R. (1980) Occupational skin hazards from ultraviolet
exposure. In: Kelley, W.D., ed. Non-ionizing radiation,
Cincinnati, OH, ACGIH, pp. 145-156.
US DHEW (1978) Performance standards for light emitting
products, (title 21, Code of Federal Regulations, part 1040),
Washington, DC, US Department of Health, Education and Welfare.
VAN DER LEUN, J.C. (1965) Theory of ultraviolet erythema.
Photochem. Photobiol., 4: 453-458.
VASSILIADIS, A. (1971) Ocular damage from laser radiation. In:
Wolbarsht, M.L., ed. Laser applications in medicine and
biology, New York, Plenum Press, pp. 125-162.
VASSILIADIS, A., ZWENG, H.C., & DEDRICK, K.G. (1971) Ocular
laser threshold investigations, Menlo Park, CA, Stanford
Research Institute (SRI Report No. 8209).
VOGT, A. (1919) [Experimental inducement of cataract by
isolated short-wave infrared mixed with red.] Klin. Mbl.
Augenheilkd., 63: 230-231 (in German).
VOS, J.J. (1966a) Heat-damage to the retina by lasers and
photocoagulators. Ophthalmologia (Basel), 151: 652-654.
VOS, J.J. (1966b) Some considerations on eye hazards with
lasers, Soesterberg, Institute for Perception RVO-TNO,
National Council for Applied Research in the Netherlands, 23
pp. (Report IZF 1966-4. AD 800156).
WEALE, R.A. (1982) The age variation of "senile" cataract in
various parts of the world. Br. J. Ophthalmol., 66: 31.34.
WHO SCIENTIFIC GROUP ON HEALTH FACTORS INVOLVED IN WORKING
UNDER CONDITIONS OF HEAT STRESS (1969) Report, Geneva, World
Health Organization (WHO Technical Report Series No. 412).
WHO (1979) Environmental Health Criteria 14: Ultraviolet
radiation, Geneva, World Health Organization.
WHO (l982) The SI for the health profession (reimpression)
Geneva, Switzerland, World Health Organization.
WILLIAMS, T.B. & BAKER, B.N., ed. (1980) The effects of
constant light on the visual process, New York, Plenum Press.
WOLBARSHT, M.L. (1971, 1974, 1978a) Lasers in medicine and
biology, New York, Plenum Press, Vols I, II, III.
WOLBARSHT, M.L. (1978b) The effects of optical radiation on
the anterior structures of the eye. In: Epstein, D. &
Tengroth, B., ed. Current concepts in ergophthalmology,
Stockholm, Department of Ophthalmology, Karolinska Institute,
pp. 29-46.
WOLBARSHT, M.L. & SLINEY, D.H. (1974) The formulation of
protection standards for lasers. In: Wolbarsht, M.L., ed.
Lasers in medicine and biology, New York, Plenum Press,
Vol. II, pp. 309-360.
WOLBARSHT, M.L., YAMANASHI, B.S., & ORR, M.A. (1977) The
origin of cataracts in the lens from infrared radiation,
Durham, NC, Duke University Eye Centre (Report 7-20-1977:
62772A 3E62772A813.00.013, Contract DAMD 17-74-C-4133, US Army
Med. Res. and Dev. Cmd).
WOLBARSHT, M.L., O'FEGHLUDHA, F.A., SLINEY, D.H., GUY, A.W.,
SMITH, A.A. Jr, & JOHNSON, G.A. (1980) Electromagnetic
emission from visual display units: a non-hazard. In: Kelley,
W.D., ed. Non-ionizing radiation, Cincinnati, OH, ACGIH,
pp. 193-201.
WREN, J.E., SCOTT, W.D., & BATES, C.E. (1977) Thermal and
mechanical properties of aluminized fabrics for use in ferrous
metal handling operations. Am. Ind. Hyg. Assoc. J., 38(11):
603-612.
YOUNG, R.W. (1980) A theory of central retinal disease. In:
Sears, M.L., ed. New directions in ophthalmic research,
New Haven, London, Yale University Press, pp. 237-270.
ZIGLER, J.S. & GOOSEY, J.D. (1981) Photosensitized oxidation
in the lens: evidence from photosensitizers endogenous to the
human lens. Photochem. Photobiol., 33: 689-874.
ZHOKOV, V.P., KOMAROVA, A.A., MAXIMOVA, L.I., MURATOV, V.P.,
PALTZEV, Yu.P., & SEMINOV, A.I. (1981) Occupational hygiene
and prevention of occupational diseases from lasers, Moscow,
Meditsina.
ZUCHLICH, J.A. & KURTIN, W.E. (1977) Oxygen dependence of
near-ultraviolet induced corneal damage. Photochem.
Photobiol., 25: 133-135.
ZUCHLICH, I.A. & TABOADA, J. (1978) Ocular hazard from UV
laser exhibiting self-mode-locking. Appl. Opt., 17: 1482-1484.
ZWICK, H. & BEATRICE, E.S. (1978) Long-term changes in
spectral sensitivity after low-level laser (5l4 nm) exposure.
Mod. Probl. Ophthalmol., 19: 319-325.
GLOSSARY
ACOUSTICO-OPTIC: involving the interaction of light and an acoustic
wave. Acoustico-optic devices such as Q switches and modulators
are used in manipulating laser beams.
ACTIVE MEDIUM: the atomic or molecular species which can provide
gain for laser oscillation. Also called laser medium, lasing
medium or active material.
ANGSTROM (A): a non-SI unit equal to 10-10 metre. Its use as a
unit of optical wavelength has largely been supplanted in recent
years by the nanometre (10-9 metre).
ARC LAMP: an electric lamp in which current passes through the
ionized air between two electrodes, giving off light. Applications
include laser excitation.
ATOMIC LASER: a gas laser in which the active material is an atomic
species rather than a molecule.
ATTENUATION: reduction in intensity that results when optical
radiation travels through an absorbing or scattering medium. In
optical fibre, attenuation (in decibels) equals 10 log ( Po/ Pin),
where Po is the power at the output end of the fibre and Pin is
the power launched into the fibre.
AVERAGE POWER: in a repetitively pulsed laser, the energy per pulse
times the repetition rate. When the energy per pulse is expressed
in joules and the repetition rate in hertz, the average power is
expressed in watts.
BEAM DIAMETER: the distance between the two opposing points at
which the irradiance or radiant exposure is a specified fraction
(typically 1/e or 1/e2) of the irradiance or radiant exposure of
the emitted radiation.
BEAM DIVERGENCE: the increase in beam diameter with distance from
the laser's exit aperture. Measured in milliradians at specified
points, usually where irradiance or radiant exposure is 1/e or 1/e2
the maximum value, and expressed as the "full-angle" divergence.
BOLOMETER: a type of detector which measures infrared radiation by
the temperature-induced change of resistance in a metal foil
exposed to the radiation and heated by it.
BREWSTER ANGLE: the angle between an incident beam of light and a
dielectric reflecting surface at which none of the light polarized
in the plane of incidence is reflected. Brewster's angle is
tan-1 n2/ n1, where n1, and n2 are the indexes of refraction of the
first and second media respectively. A window mounted at
Brewster's angle with respect to an incident beam is often used as
a window in laser cavities.
CALORIMETER: a type of detector that measures heat produced by
absorption of radiation.
CHEMICAL LASER: a type of laser in which the population inversion
is produced directly by an "elementary" chemical reaction (a
collision process in which one or more molecules undergo changes in
their chemical bonds).
COHERENCE: a fixed phase relationship among various points of an
electromagnetic wave in space (spatial coherence) or in time
(temporal coherence).
COLLIMATOR: an optical device for converting a diverging or
converging beam of light into a collimated or parallel beam, or for
expanding or reducing the cross-sectional area of an incident
collimated beam. A target collimator projects a parallel beam from
its own light source such that, viewed from any distance, the light
source appears to be at infinity.
CONTINUOUS WAVE (cw) LASER OPERATION: laser operation in which
radiation is emitted continuously.
CORE: the central region of an optical fibre. The core must have a
higher refractive index than the cladding for light to be
transmitted through the fibre via total internal reflection
CORNER CUBE: an optical component with three mutually perpendicular
faces and a hypotenuse face. Because light entering through the
hypotenuse is totally internally reflected at each perpendicular
face, the cube acts as a retroreflector. Also known as corner
reflector.
CRYSTAL LASER: a type of laser in which the active medium is an
atomic species in a crystal such as ruby, YAG (yttrium aluminium
garnet), or YALO (yttrium aluminate).
DETECTOR: see PHOTODETECTOR.
DIFFRACTION: deviation of light rays from the paths predicted by
geometical optics.
DIODE LASER: see SEMICONDUCTOR LASER.
DISPERSION: variation of the refractive index of an optical
material with change in wavelength, as in a prism; in an optical
fibre, the temporal spreading of a light pulse due to the fibre's
different propagation speeds for different wavelengths and modes of
light. Such spreading limits the fibre's information-carrying
capacity of bandwidth.
DIVERGENCE: see BEAM DIVERGENCE.
DYE LASER: a type of laser in which the active medium is an organic
dye, generally in solution with the liquid either flowing or
encapsulated within a cell. Experimental solid and gas dye lasers
also have been built. Also called organic-dye, tunable-dye or
liquid laser.
ELECTRON-BEAM-SUSTAINED LASER: a molecular-gas laser in which the
electrical discharge is sustained with a beam of high-energy
electrons. Usually injected transversely to the laser cavity's
optical axis, the electron beam permits laser operation at
pressures and cross-section-to-length ratios higher than possible
with an unsustained discharge. This technique is often used in
commercial carbon-dioxide lasers with very high continuous-wave
output power.
ELECTRO-OPTIC: applying to modulators, Q switches and other beam-
manipulating devices in which operation relies on modification of a
material's refractive indices by an applied electrical field. In a
Kerr cell the index change is proportional to the square of the
electrical field, and the material is usually a liquid. In a
Pockels cell the material is a crystal whose index change is linear
with the electric field.
EMISSIVITY: ratio of radiant exitance of a thermal radiator to that
of a full radiator (black body) at the same temperature - (ISO
31/VI 1980).
EXCIMER LASER: a laser in which the active medium is an excimer, a
molecule which is chemically unstable except in its excited state.
The term often is applied to lasers in which the active medium is a
rare-gas halide (or monohalide) excimer such as KrF* or XeF*.
GAS LASER: a type of laser in which the active medium is a gas.
The category is subclassified according to the active medium into
atomic (such as helium-neon), molecular (carbon dioxide, hydrogen
cyanide and water vapour), ionic (argon, krypton, xenon, and the
metal-vapour types such as helium-cadmium and helium-selenium), and
excimer (typically rare-gas halides). Loosely applied, "ion" means
argon and krypton.
GLASS LASER: a type of solid-state laser in which the active medium
is a glass rod doped with rare-earth atoms, usually neodymium.
HERTZ (Hz): the SI unit of frequency of periodic phenomena. It
replaces the non-SI unit "cycles per second". The number of pulses
per second that a laser can produce may be expressed in hertz.
HOLOGRAM: a recording of the interference of coherent light
reflected from an object with light direct from the same source or
reflected from a mirror. Illumination of the hologram reproduces
the object's three-dimensional image.
IMAGE CONVERTER: an electron tube which produces a visual replica
of an image formed on its cathode by some form of electromagnetic
radiation. In an image converter camera, the image formed by the
electron tube is focused on to photographic film for a permanent
record.
INFRARED: electromagnetic radiation with wavelength between 0.76
micrometre and about 1 millimetre. Wavelengths at the shorter end
of this range are frequently called "near" infrared, and those
longer than about 20 micrometres, "far" infrared.
INTEGRATED OPTICS: devices in which several optical components are
"integrated" on to a single substrate; analogous to integrated
electronic circuits. Although still in the research phase,
integrated optics has potential for use in optical signal
processing and in fibre-optic communications.
INTERFERENCE FILTER: an optical component which depends on
interference in a series of thin films deposited on a substrate to
limit transmission to a desired spectral band.
ION LASER: a type in which the active element is an ionized gas,
generally argon or krypton.
IRRADIANCE ( E): radiant flux per unit area, expressed in watts per
square centimetre.
LASER: acronym for "light amplication by stimulated emission of
radiation." A device which generates or amplifies electromagnetic
oscillations at wavelengths between the far infrared
(submillimetre) and ultraviolet. Like any electromagnetic
oscillator, a laser oscillator consists of two basic elements: an
amplifying (active) medium and a regeneration or feedback device
(resonant cavity). A laser's amplifying medium can be a gas,
semiconductor, dye solution, etc; feedback is typically from two
mirrors. Distinctive properties of the electromagnetic
oscillations produced include monochromaticity, high intensity,
small beam divergence, and phase coherence. As a description of a
device, "laser" refers to the active medium plus all equipment
necessary to produce the effect called lasing.
LASER DIODE: see SEMICONDUCTOR LASER.
LED: abbreviation of light-emitting diode. A semiconductor
emitting incoherent light into a broad field of view, used in low-
speed or short-haul fibre-optic links. Most LEDs used in fibre-
optic applications emit in the near infrared.
LIDAR: acronym for "light detection and ranging," a system
employing a laser beam to gather ranging information as well as
intelligence on reflection and scattering of light by clouds and
atmospheric pollutants.
LIQUID LASER: a type in which the active element is either an
organic dye or an inorganic liquid. See also DYE LASER.
MULTIMODE: emission at several frequencies simultaneously,
generally closely spaced, each frequency representing a different
mode of laser oscillation inthe resonant cavity.
Nd-GLASS: neodymium-doped glass, used in some solid state lasers.
The neodymium atoms are the active medium.
Nd-YAG: neodymium-doped yttrium-aluminium-garnet (YAG), a crystal
which is used in some solid state lasers. The neodymium atoms are
the active medium.
NEUTRAL DENSITY FILTER: a filter which reduces the intensity of
light without affecting its spectral character.
NONLINEAR EFFECTS: changes in a medium transmitting electromagnetic
waves that are proportional to the second, third or higher powers
of external electric field. Nonlinear optical effects include
harmonic generation and the electro-optic effect. See electro-
optic.
OPTICALLY PUMPED LASER: a laser whose active medium is excited by
another light source to produce a population inversion. For solid-
state and some dye lasers this source usually is an incoherent type
such as a flash- or arc-lamp. For gas and other dye lasers,
coherent laser sources generally provide such optical pumping.
PARAMETRIC OSCILLATOR: a nonlinear device, usually a crystal, which
produces tunable laser oscillations at the sum or difference
frequency of mixed laser beams. Also called tunable parametric
oscillator or optical parametric oscillator. Loosely applied to
the complete instrument containing the pump laser and the tuning
crystal.
PHOTODETECTOR: any device which detects light, generally producing
an electronic signal with intensity proportional to that of the
incident light.
PHOTON: a massless "particle" of electromagnetic radiation, with
energy equal to hc/lambda where h is Planck's constant (6.6 x 10-34
joule second) and c/lambda is the frequency of the radiation (speed
of light divided by wavelength).
POLARIZER: an optical component which only transmits lightwaves
that oscillate in a given plane.
POPULATION INVERSION: a condition in which most atoms of a species
are in an excited, metastable state. Collision of a photon with
such an atom causes the atom to relax to a lower energy state, and
to emit a second photon, amplifying the light signal. Population
inversion is required for lasing to occur.
PULSELENGTH: the duration of the burst of energy emitted by a
pulsed or Q-switched laser. Expressed in seconds and usually
measured at the half-power (half the full height of a voltage or
current pulse). Also called pulsewidth.
PULSED LASER: a laser that emits light in pulses rather than
continuously.
PUMP: the energy source (such as flashlamp, electron beam or
current supply) that drives the amplification in the active medium
of a laser by creating a population inversion.
PYROELECTRIC CRYSTAL: a type of crystal that shows electrical
effects when its temperature is changed; these effects are used to
detect infrared radiation.
Q SWITCH: essentially a "shutter" which prevents laser emission
until opened. Q stands for "quality factor" of the laser's
resonant cavity. "Active" Q switching is achieved with a rotating
mirror or prism, Kerr or Pockels cell, or acoustico-optic device;
"passive" Q switching is achieved with a saturable absorber such as
a gas or dye. In a pulsed laser a Q switch increases pulse power
by shortening pulse duration while not significantly decreasing the
energy; in a continuous wave laser the device provides shorter and
more intense pulses at a higher repetition rate than could be
achieved by pulsing the laser directly.
RADIANCE ( L): At a point of a surface and in a given direction,
the radiant intensity of an element of the surface, divided by the
area of the orthogonal projection of this element on a plane
perpendicular to the given direction (ISO 31/6-1980). Expressed in
watts per steradian square centimetre.
RADIANT FLUX: the rate of flow of radiant energy, measured in
watts.
RADIOMETER: an instrument for measuring incident radiation in
radiometric units (watts). Radiometric measurements can be made at
any wavelength, but the spectral range of a particular instrument
may be limited to a narrow range.
RADIOMETRIC UNITS: units defined for measurement of the intensity
of electromagnetic radiation; the basic unit is the SI unit watt.
RAMAN EFFECT: the appearance of additional weak lines in the
spectrum of light that has been scattered by a transparent
substance. The extra lines result from rotational or vibrational
transitions of the molecules in the scattering medium. If the
medium is illuminated with laser light of sufficient intensity, the
emission at the Raman frequencies is amplified, exhibiting
characteristics of stimulated emission (i.e., stimulated Raman
effect.).
REFLECTANCE: the ratio of wave energy reflected from a surface to
the wave energy incident on a surface.
SEMICONDUCTOR LASER: a type in which the active material is a
semiconductor, either a diode or homogeneous. Commercial
types are generally diodes in which lasing occurs at the
junction of n-type and p-type semiconductors, usually gallium-
arsenide or gallium-aluminium-arsenide. Homogeneous types are
made of undoped semiconductor material and are pumped by an
electron beam.
SOLID-STATE LASER: a type the active medium of which is an atomic
species in a glass or crystal. The atomic species may be added to
the glass or crystal, as neodymium is added to glass, or may be
instrinic, as chromium is in ruby. This term is generally not
applied to semiconductor lasers.
SUPER-RADIANT: applying to coherent optical amplification of
spontaneous emission that occurs without relaxation processes.
Commonly used to describe a laser whose gain is high enough to
permit amplification without mirrors; examples are nitrogen and
molecular hydrogen. Beam quality of a super radiant laser is
generally inferior to that of a laser with a complete optical
cavity. "Super-fluorescent" has been proposed as a more precise
description of this type of laser.
TEA LASER: acronym for transversely excited, atmospheric pressure
laser. A gas laser in which excitation of the active medium is
transverse to the flow of the medium. Because of shorter breakdown
length, this type operates in a gas-pressure range higher than that
for longitudinally excited gas lasers (but not necessarily
atmospheric) and offers a potentially higher power output per unit
volumes because of a greater density of lasing molecules.
TUNABLE LASER: a laser or a parametric oscillator whose emission
can be varied across a broad spectral range.
ULTRAVIOLET: electromagnetic radiation with wavelengths between
about 40 and 400 nanometres. Radiation between 40 and 200 nm is
termed "vacuum ultraviolet" because it is absorbed by air and
travels only through a vacuum. The "near" ultraviolet has
wavelengths close to those of visible light; the "far" ultraviolet
has shorter wavelengths.
YAG: yttrium aluminium garnet, a crystal host which can be doped
with an active laser medium, usually neodymium.
YALO: yttrium aluminate (YA103), a crystal host doped with an
active laser medium, usually neodymium.
YLF: yttrium lithium fluoride, a crystal host which can be doped
with an active laser ion, usually holmium.
 Equation 1 can be modified for electromagnetic radiation by
giving the velocity of the radiation the value of the velocity of
light, usually written as c. In a vacuum:
co = lambda nu Equation (1)
The velocity rhoo has been set as 299792458 m/s or about 3 x 108
m/s = 3 x 1010 cm/s.
The ratio of the velocity of light co in a vacuum to the
velocity c in a medium is termed the refractive index n of that
medium (n = co/c). Equation 1 can also be expressed as
lambda = c/nu, or nu = c/lambda Equation (2)
-------------------------------------------------------------------
a Light by definition is visible radiation; hence, it is incorrect
(but commmon) to speak of "ultraviolet light" or "infrared
light".
The inverse relationship between frequency and wavelength is
clearly evident in Fig. 1. If n is constant at all points within
the medium, then the medium is called optically homogeneous; if n
is independent of direction, the medium is termed isotropic. If n
is considered independent of the amplitude or intensity of the
optical field, the interaction with the medium is termed "linear";
if not, it is "non-linear".
As the frequency increases from microwave radiation through the
optical radiations to gamma radiation, the wavelength becomes
shorter and shorter. The electromagnetic radiations have a
characteristic energy associated with each photon and the photon
energy increases with an increase in frequency. Reference to one
region or another as the "gamma-radiation region" or the "microwave
region" is arbitrary and no internationally accepted set of terms
exist for specifying all of the spectral regions.
The spectral bands represent wavelength intervals within which
a common state of the art and technology exists in sources,
detectors, or in modes of interaction with matter. The upper and
lower limits of the entire electromagnetic spectrum have not been
defined at present. The units used to describe energy, wavelength,
and frequency often differ between spectral regions, as a matter of
convention.
Ultraviolet, visible (light), and infrared radiation,
collectively known as optical radiation are described in terms of
wavelength. Sometimes, the spectral region of wavelengths shorter
than approximately 100 nm is termed ionizing radiation, and
wavelengths longer than 100 nm are placed in the non-ionizing
radiation spectrum. These terms are useful for those who wish to
distinguish between the biological effects of different types of
radiation, but divisions between adjacent spectral bands vary
according to different disciplines. For the physicist, the optical
spectrum generally consists of 5 decades of wavelengths between
10 nm and 1 mm. On the other hand, photobiologists and health
specialists, who are not concerned about vacuum ultraviolet
radiation, begin at approximately 180 - 200 nm (which is the
approximate long-wave edge of the vacuum ultraviolet) and go to
far-infrared radiation at 1 mm. The Commission Internationale de
l'Eclairage (CIE) Committee on Photobiology has provided spectral
band designations that are quite convenient in discussing
biological effects. Three common schemes of dividing the optical
spectrum are given in Table 3 (CIE, 1970).
2.2. Interaction of Electromagnetic Radiation with Matter
Electromagnetic radiation interacting with matter is absorbed,
transmitted, reflected, scattered, and diffracted. In most
instances, one of these effects dominates, almost to the exclusion
of others. However, all effects are always present to some extent.
For instance, if a beam of light passes through a sheet of
transparent glass, at least 4% of the incident light is reflected
from each surface. On the other hand, only a very small percentage
(less than 1%) is usually absorbed within the clear glass, even
when marked refraction or bending of the light takes place.
Similar effects occur in all spectral regions including the
radiofrequency and gamma-radiation bands.
2.2.1. Interaction at an interface
2.2.1.1. Reflection
Reflection takes place at an interface. There are two basic
types of reflections that are of interest, i.e., specular (mirror-
like) and diffuse. Specular reflection is sometimes referred to as
regular reflection. With specular reflection from a mirror or
other very smooth surface, light obeys the law of reflection, which
states that the angle of reflection equals the angle of incidence.
Table 3. Several schemes for dividing the optical spectrum
-----------------------------------------------------------------------
Physical No. 1 Physical No. 2 Photobiological (CIE)a
-----------------------------------------------------------------------
extreme UVR vacuum or extreme UVR UV-C
(1-10 nm to 100 nm) (1-10 nm to 180 nm) (100 nm to 280 nm)
far UVR middle UVR UV-Bb
(200 nm to 300 nm) (180 nm to 300 nm) (280 nm to 315 nm)
near UVR near UVR UV-Ab
(300 nm to 400 nm) (300 nm to 400 nm) (315 nm to 380-400 nm)
light light light
(380 nm to 760 nm) (400 nm to 700 nm) (380-400 nm to 760-780 nm)
near IR near IR IR-A
(760 nm to 4000 nm) (700 nm to 1200 nm) (760-780 nm to 1400 nm)
middle IR middle IR IR-B
(4 µm to 14 µm) (1.2 µm to 7 µm) (1.4 µm to 3 µm)
far IR far IR IR-C
(14 µm to 100 µm) (7 µm to 1 mm) (3 µm to 1 mm)
submillimetre
(100 µm to 1 mm)
-----------------------------------------------------------------------
a Based on the recommendation of the Committee on photobiology of the
Commission Internationale de l'Eclairage (CIE, 1970). The scheme
was originally proposed by W.W. Coblentz of the US National Bureau
of Standards in the 1930s.
b The dividing line between UV-B and UV-A is often taken as 320 nm,
but may be taken as 315 nm. For the purposes of this document,
315 nm is used unless otherwise stated.
Specular reflection can occur, when the size of surface
irregularities or roughness is less than the wavelength of the
incident radiation. This description of specular reflection is
important to keep in mind. Diffuse reflection occurs, when the
surface irregularities are randomly oriented and are much greater
than the wavelength of the incident radiation; for example, when
light is reflected from chalk or a rough granite surface. Perfect
diffuse reflection obeys Lambert's Law, i.e., the Cosine Law of
Reflection. A useful formula in radiometry is:
E = phi rho x cos theta/pi r12 Equation (3)
where E is the irradiance reflected from the surface at angle theta
relative to the surface's normal, phi, the optical beam power upon
the surface, rho, the diffuse reflection coefficient of the surface
for the wavelength, r1 the distance from the beam spot on the
diffuse target to the detector, and phi equals 3.14159.
It is important to remember that diffuse and specular
reflections are strongly dependent on wavelength. A given surface
may produce a reflection that is specular at one wavelength but may
or may not be specular at a different wavelength.
The fraction of incident radiation specularly reflected from
the surface of a transparent medium depends on the index of
refraction, the polarization of the incident beam, and the angle of
incidence. This is illustrated for glass in Fig 2.
Equation 1 can be modified for electromagnetic radiation by
giving the velocity of the radiation the value of the velocity of
light, usually written as c. In a vacuum:
co = lambda nu Equation (1)
The velocity rhoo has been set as 299792458 m/s or about 3 x 108
m/s = 3 x 1010 cm/s.
The ratio of the velocity of light co in a vacuum to the
velocity c in a medium is termed the refractive index n of that
medium (n = co/c). Equation 1 can also be expressed as
lambda = c/nu, or nu = c/lambda Equation (2)
-------------------------------------------------------------------
a Light by definition is visible radiation; hence, it is incorrect
(but commmon) to speak of "ultraviolet light" or "infrared
light".
The inverse relationship between frequency and wavelength is
clearly evident in Fig. 1. If n is constant at all points within
the medium, then the medium is called optically homogeneous; if n
is independent of direction, the medium is termed isotropic. If n
is considered independent of the amplitude or intensity of the
optical field, the interaction with the medium is termed "linear";
if not, it is "non-linear".
As the frequency increases from microwave radiation through the
optical radiations to gamma radiation, the wavelength becomes
shorter and shorter. The electromagnetic radiations have a
characteristic energy associated with each photon and the photon
energy increases with an increase in frequency. Reference to one
region or another as the "gamma-radiation region" or the "microwave
region" is arbitrary and no internationally accepted set of terms
exist for specifying all of the spectral regions.
The spectral bands represent wavelength intervals within which
a common state of the art and technology exists in sources,
detectors, or in modes of interaction with matter. The upper and
lower limits of the entire electromagnetic spectrum have not been
defined at present. The units used to describe energy, wavelength,
and frequency often differ between spectral regions, as a matter of
convention.
Ultraviolet, visible (light), and infrared radiation,
collectively known as optical radiation are described in terms of
wavelength. Sometimes, the spectral region of wavelengths shorter
than approximately 100 nm is termed ionizing radiation, and
wavelengths longer than 100 nm are placed in the non-ionizing
radiation spectrum. These terms are useful for those who wish to
distinguish between the biological effects of different types of
radiation, but divisions between adjacent spectral bands vary
according to different disciplines. For the physicist, the optical
spectrum generally consists of 5 decades of wavelengths between
10 nm and 1 mm. On the other hand, photobiologists and health
specialists, who are not concerned about vacuum ultraviolet
radiation, begin at approximately 180 - 200 nm (which is the
approximate long-wave edge of the vacuum ultraviolet) and go to
far-infrared radiation at 1 mm. The Commission Internationale de
l'Eclairage (CIE) Committee on Photobiology has provided spectral
band designations that are quite convenient in discussing
biological effects. Three common schemes of dividing the optical
spectrum are given in Table 3 (CIE, 1970).
2.2. Interaction of Electromagnetic Radiation with Matter
Electromagnetic radiation interacting with matter is absorbed,
transmitted, reflected, scattered, and diffracted. In most
instances, one of these effects dominates, almost to the exclusion
of others. However, all effects are always present to some extent.
For instance, if a beam of light passes through a sheet of
transparent glass, at least 4% of the incident light is reflected
from each surface. On the other hand, only a very small percentage
(less than 1%) is usually absorbed within the clear glass, even
when marked refraction or bending of the light takes place.
Similar effects occur in all spectral regions including the
radiofrequency and gamma-radiation bands.
2.2.1. Interaction at an interface
2.2.1.1. Reflection
Reflection takes place at an interface. There are two basic
types of reflections that are of interest, i.e., specular (mirror-
like) and diffuse. Specular reflection is sometimes referred to as
regular reflection. With specular reflection from a mirror or
other very smooth surface, light obeys the law of reflection, which
states that the angle of reflection equals the angle of incidence.
Table 3. Several schemes for dividing the optical spectrum
-----------------------------------------------------------------------
Physical No. 1 Physical No. 2 Photobiological (CIE)a
-----------------------------------------------------------------------
extreme UVR vacuum or extreme UVR UV-C
(1-10 nm to 100 nm) (1-10 nm to 180 nm) (100 nm to 280 nm)
far UVR middle UVR UV-Bb
(200 nm to 300 nm) (180 nm to 300 nm) (280 nm to 315 nm)
near UVR near UVR UV-Ab
(300 nm to 400 nm) (300 nm to 400 nm) (315 nm to 380-400 nm)
light light light
(380 nm to 760 nm) (400 nm to 700 nm) (380-400 nm to 760-780 nm)
near IR near IR IR-A
(760 nm to 4000 nm) (700 nm to 1200 nm) (760-780 nm to 1400 nm)
middle IR middle IR IR-B
(4 µm to 14 µm) (1.2 µm to 7 µm) (1.4 µm to 3 µm)
far IR far IR IR-C
(14 µm to 100 µm) (7 µm to 1 mm) (3 µm to 1 mm)
submillimetre
(100 µm to 1 mm)
-----------------------------------------------------------------------
a Based on the recommendation of the Committee on photobiology of the
Commission Internationale de l'Eclairage (CIE, 1970). The scheme
was originally proposed by W.W. Coblentz of the US National Bureau
of Standards in the 1930s.
b The dividing line between UV-B and UV-A is often taken as 320 nm,
but may be taken as 315 nm. For the purposes of this document,
315 nm is used unless otherwise stated.
Specular reflection can occur, when the size of surface
irregularities or roughness is less than the wavelength of the
incident radiation. This description of specular reflection is
important to keep in mind. Diffuse reflection occurs, when the
surface irregularities are randomly oriented and are much greater
than the wavelength of the incident radiation; for example, when
light is reflected from chalk or a rough granite surface. Perfect
diffuse reflection obeys Lambert's Law, i.e., the Cosine Law of
Reflection. A useful formula in radiometry is:
E = phi rho x cos theta/pi r12 Equation (3)
where E is the irradiance reflected from the surface at angle theta
relative to the surface's normal, phi, the optical beam power upon
the surface, rho, the diffuse reflection coefficient of the surface
for the wavelength, r1 the distance from the beam spot on the
diffuse target to the detector, and phi equals 3.14159.
It is important to remember that diffuse and specular
reflections are strongly dependent on wavelength. A given surface
may produce a reflection that is specular at one wavelength but may
or may not be specular at a different wavelength.
The fraction of incident radiation specularly reflected from
the surface of a transparent medium depends on the index of
refraction, the polarization of the incident beam, and the angle of
incidence. This is illustrated for glass in Fig 2.
 2.2.1.2. Refraction
Refraction also takes place at an interface. Refraction
occurs, whenever a beam of light passes from one transmitting
medium to another having a different refractive index (n). For
example, refraction is the bending of light at air-water and air-
glass interfaces. The law of refraction, which is also known as
Snell's Law, states that the angle of incidence (theta1) and the
angle of refraction (theta2) are related by the equation:
sin thetal/sin theta2 = n2/n1 Equation (4)
where n1 and n2 are the indices of refraction of the first medium and
the second medium respectively.
Lenses and prisms are optical components that depend
principally on the phenomenon of refraction. The variation in the
index of refraction with wavelength is termed dispersion. Thus a
simple prism bends blue light and red light differently for the
same angle of incidence, the two angles of refraction differ, and
blue light can be separated from red light. In lenses, this effect
is called chromatic aberration. It can be reduced by choosing a
glass with very little dispersion or by combining two lenses that
have complementary dispersion characteristics.
2.2.2. Interaction with a medium
2.2.2.1. Transmission
The nature of transmitted light that emerges from a medium
depends on the phenomena of absorption and scattering and also on
the reflection of some of the light at the interfaces between
media. The transmittance of a medium is usually represented by tau
and specified at a certain wavelength and for a certain path length
at normal incidence. The transmittance of most materials varies
markedly across the optical spectrum.
2.2.2.2. Attenuation
The absorption and transmission of a beam of optical radiation
in any homogenous, isotropic medium is expressed in terms of the
following equation:
phi = phioe-(alpha+rho)x=phioe-µx Equation (5)
where phi is the radiant power (radiant flux) leaving the medium,
phio the initial radiant power in the beam entering the absorbing
medium, x the thickness of the medium (path length of the beam),
alpha the absorption coefficient, rho the scattering coefficient,
and µ (Greek "mu") the attenuation coefficient of the absorbing
medium.
In the Exponential Law of Absorption (Beer's Law), the constant
alpha is the absorption coefficient. The law shows that the
radiant power diminishes exponentially with distance during
transmission through a uniformly absorbing medium. For a
scattering medium, the same approach may be applied with the
absorption coefficient alpha being replaced by a scattering
coefficient sigma. The attenuation coefficient varies with
wavelength as does the scattering coefficient sigma. Equation 5 is
only an approximation for weak scattering. It can be rewritten to
the base 10 instead of to the base e of natural logarithms and the
constants µ, rho, and alpha will then be different. "Attenuation
depth" and "absorption depth" are useful terms to describe
attenuation and absorption in tissue. The most popular convention
is to define this depth as the distance into the tissue at which
the incident irradiance is reduced to 1/e (37%) of its initial
value. Another convention sets the value at 1/10.
Absorption in all substances is strongly dependent on the
wavelength of the incident radiation. Atoms or molecules become
excited when they absorb a quantum of radiant energy. Following
absorption, this energy may be released in a variety of ways. When
the energy is released as more photons of radiant energy, it is
known as luminescence.
At very high irradiances, non-linear effects can occur as a
result of the direct interaction of the high electric-field
intensities with matter. Saturable absorption and enhanced
absorption are examples that alter the absorption coefficient.
2.2.3. Interference, diffraction, and scattering effects
2.2.3.1. Interference and diffraction
When considering interference and diffraction effects, it is
convenient to use the wave description of light. The bending or
spreading of waves after passing an edge or passing through a small
aperture is a wave phenomenon termed diffraction. The diffraction
effects result from the constructive and destructive interference
of adjacent waves. When the size of the barrier is comparable or
smaller in size than the incident wavelength, the wave is bent
around the barrier considerably. Thus, particles diffract light
most dramatically, when they are approximately the size of the
wavelength of the incident radiation. In this case, the sum of the
diffraction effects is known as scattering.
In the treatment of plane waves impinging on an aperture such
as a circular aperture, Huygens principle may be employed. Each
point within the area of the aperture is regarded as a source of
wavelets to explain the interference effects that produce a
diffraction pattern on a screen some distance away.
2.2.3.2. Scattering
Small particles, the size of which approaches that of a
wavelength of light, scatter light, as do atoms, and molecules. If
the particles are much smaller than the wavelength of light (e.g.,
gas molecules), Rayleigh scattering takes place. For Rayleigh
scattering, the fraction of scattered radiation from a beam is
inversely proportional to the fourth power of the wavelength of the
radiation. That is to say, that this type of scattering increases
dramatically for shorter wavelengths. Rayleigh scattered, non-
polarized light goes in all directions and becomes polarized to
some extent. If light is scattered by particles the size of the
order of the wavelength of light or greater, this strong wavelength
preference is not seen in the scattered light. The type of large-
particle scattering is termed Mie scattering. Unlike Rayleigh
scattering, Mie scattering is strongly directional. Normally, the
forward component of Mie scattered radiation is much greater than
the backscatter.
The scattering of a beam of light passing through a homogeneous
medium can be expressed in terms of the exponential function
(Equation 5).
3. SOURCES OF RADIATION
Sources of optical radiation can be grouped according to the
type of emitting material, the type of apparatus, or the manner in
which the radiation originates.
Incandescent bodies are probably the most common sources of
optical radiation. When the temperature of a body is elevated,
more photons are emitted. If the temperature of the body is
approximately that of the human body (37 °C or 310 K), most of the
emitted photons have wavelengths in the far infrared, in the
vicinity of 10 µm. If a material body is heated to incandescence,
e.g., to 2000 K, the material may be described as "red hot". The
higher the temperature, the greater the percentage of high energy
photons released. But, in all cases, a wide range of photon
energies is associated with the emitted incandescent radiation. A
theoretically perfect incandescent source has a characteristic
"black-body" spectrum. Fig. 3 shows the black-body spectra for
several different temperatures. In practice, no material actually
emits a perfect black-body spectrum, but some materials such as
solid tungsten or molten metals approach this distribution.
2.2.1.2. Refraction
Refraction also takes place at an interface. Refraction
occurs, whenever a beam of light passes from one transmitting
medium to another having a different refractive index (n). For
example, refraction is the bending of light at air-water and air-
glass interfaces. The law of refraction, which is also known as
Snell's Law, states that the angle of incidence (theta1) and the
angle of refraction (theta2) are related by the equation:
sin thetal/sin theta2 = n2/n1 Equation (4)
where n1 and n2 are the indices of refraction of the first medium and
the second medium respectively.
Lenses and prisms are optical components that depend
principally on the phenomenon of refraction. The variation in the
index of refraction with wavelength is termed dispersion. Thus a
simple prism bends blue light and red light differently for the
same angle of incidence, the two angles of refraction differ, and
blue light can be separated from red light. In lenses, this effect
is called chromatic aberration. It can be reduced by choosing a
glass with very little dispersion or by combining two lenses that
have complementary dispersion characteristics.
2.2.2. Interaction with a medium
2.2.2.1. Transmission
The nature of transmitted light that emerges from a medium
depends on the phenomena of absorption and scattering and also on
the reflection of some of the light at the interfaces between
media. The transmittance of a medium is usually represented by tau
and specified at a certain wavelength and for a certain path length
at normal incidence. The transmittance of most materials varies
markedly across the optical spectrum.
2.2.2.2. Attenuation
The absorption and transmission of a beam of optical radiation
in any homogenous, isotropic medium is expressed in terms of the
following equation:
phi = phioe-(alpha+rho)x=phioe-µx Equation (5)
where phi is the radiant power (radiant flux) leaving the medium,
phio the initial radiant power in the beam entering the absorbing
medium, x the thickness of the medium (path length of the beam),
alpha the absorption coefficient, rho the scattering coefficient,
and µ (Greek "mu") the attenuation coefficient of the absorbing
medium.
In the Exponential Law of Absorption (Beer's Law), the constant
alpha is the absorption coefficient. The law shows that the
radiant power diminishes exponentially with distance during
transmission through a uniformly absorbing medium. For a
scattering medium, the same approach may be applied with the
absorption coefficient alpha being replaced by a scattering
coefficient sigma. The attenuation coefficient varies with
wavelength as does the scattering coefficient sigma. Equation 5 is
only an approximation for weak scattering. It can be rewritten to
the base 10 instead of to the base e of natural logarithms and the
constants µ, rho, and alpha will then be different. "Attenuation
depth" and "absorption depth" are useful terms to describe
attenuation and absorption in tissue. The most popular convention
is to define this depth as the distance into the tissue at which
the incident irradiance is reduced to 1/e (37%) of its initial
value. Another convention sets the value at 1/10.
Absorption in all substances is strongly dependent on the
wavelength of the incident radiation. Atoms or molecules become
excited when they absorb a quantum of radiant energy. Following
absorption, this energy may be released in a variety of ways. When
the energy is released as more photons of radiant energy, it is
known as luminescence.
At very high irradiances, non-linear effects can occur as a
result of the direct interaction of the high electric-field
intensities with matter. Saturable absorption and enhanced
absorption are examples that alter the absorption coefficient.
2.2.3. Interference, diffraction, and scattering effects
2.2.3.1. Interference and diffraction
When considering interference and diffraction effects, it is
convenient to use the wave description of light. The bending or
spreading of waves after passing an edge or passing through a small
aperture is a wave phenomenon termed diffraction. The diffraction
effects result from the constructive and destructive interference
of adjacent waves. When the size of the barrier is comparable or
smaller in size than the incident wavelength, the wave is bent
around the barrier considerably. Thus, particles diffract light
most dramatically, when they are approximately the size of the
wavelength of the incident radiation. In this case, the sum of the
diffraction effects is known as scattering.
In the treatment of plane waves impinging on an aperture such
as a circular aperture, Huygens principle may be employed. Each
point within the area of the aperture is regarded as a source of
wavelets to explain the interference effects that produce a
diffraction pattern on a screen some distance away.
2.2.3.2. Scattering
Small particles, the size of which approaches that of a
wavelength of light, scatter light, as do atoms, and molecules. If
the particles are much smaller than the wavelength of light (e.g.,
gas molecules), Rayleigh scattering takes place. For Rayleigh
scattering, the fraction of scattered radiation from a beam is
inversely proportional to the fourth power of the wavelength of the
radiation. That is to say, that this type of scattering increases
dramatically for shorter wavelengths. Rayleigh scattered, non-
polarized light goes in all directions and becomes polarized to
some extent. If light is scattered by particles the size of the
order of the wavelength of light or greater, this strong wavelength
preference is not seen in the scattered light. The type of large-
particle scattering is termed Mie scattering. Unlike Rayleigh
scattering, Mie scattering is strongly directional. Normally, the
forward component of Mie scattered radiation is much greater than
the backscatter.
The scattering of a beam of light passing through a homogeneous
medium can be expressed in terms of the exponential function
(Equation 5).
3. SOURCES OF RADIATION
Sources of optical radiation can be grouped according to the
type of emitting material, the type of apparatus, or the manner in
which the radiation originates.
Incandescent bodies are probably the most common sources of
optical radiation. When the temperature of a body is elevated,
more photons are emitted. If the temperature of the body is
approximately that of the human body (37 °C or 310 K), most of the
emitted photons have wavelengths in the far infrared, in the
vicinity of 10 µm. If a material body is heated to incandescence,
e.g., to 2000 K, the material may be described as "red hot". The
higher the temperature, the greater the percentage of high energy
photons released. But, in all cases, a wide range of photon
energies is associated with the emitted incandescent radiation. A
theoretically perfect incandescent source has a characteristic
"black-body" spectrum. Fig. 3 shows the black-body spectra for
several different temperatures. In practice, no material actually
emits a perfect black-body spectrum, but some materials such as
solid tungsten or molten metals approach this distribution.
 The ratio of the theoretically possible spectral emittance to
the actual emittance of a grey body is the emissivity. For
instance, the emissivity of tungsten throughout the visible is
approximately 0.4.
A useful relation for black-body sources is the Stefan-
Boltzmann Law, which states that the radiant exitance W integrated
over all wavelengths of a black body is proportional to the fourth
power of the absolute temperature of the body, i.e.:
W = sigmaT4
3.1. Molecular and Atomic Transitions
Other sources of light such as carbon arcs, gas-filled arc
lamps, or gas discharge lamps, depart widely from black-body
characteristics, i.e., vary greatly with the wavelength in the
visible region. In these cases, a stream of electrons flowing
through a gas induces an emission of photons, characteristic of
that particular gas. If gas has a low pressure and the current is
not great, a line spectrum is emitted. Line spectra are the result
of atomic transition. As the gas pressure and the current density
increase, the gas temperature increases and a continuous spectrum
appears. At high current densities and gas pressures, this type of
emission (a continuum) predominates.
The energy Qq of a single photon, emitted because of an atomic
transition, is determined by the frequency of the emitted radiation
as defined by the condition:
Qq = xi1 - xi2 = h nu Equation (6)
where xi1 and xi2 are energies corresponding to the initial and
final energy states, h is the Plank constant (6.625 x 10-34J x s),
and nu is the frequency of radiation (in Hz).
Energy transitions in molecular systems can result in a
radiation emission according to rules similar to those that apply
to atomic systems. The energies (0.001-0.1 eV) of molecular
vibrational or rotational transitions are, typically, less than
those characteristic of electron transitions in atoms or molecules
(1-100 eV). In addition to the electron "orbital" potential and
kinetic energies, part of the energy of molecular systems is
associated with rotational and vibrational modes. Emissions of
this type occur in the infrared and microwave regions of the
electromagnetic spectrum. Heat is the vibrational energy of
molecular systems.
4. LASERS
All lasers have three basic components: (a) a laser (active)
medium; (b) an energy source (pumping system); and (c) a resonant
optical cavity. Lenses, mirrors, shutters, saturable absorbers,
and other accessories may be added to the system to obtain greater
power, shorter pulses, or special beam shapes, but only the three
basic components (a, b, and c) are necessary for laser action.
4.1. The Laser Medium
Laser action depends on the ability of the laser (active)
medium to undergo population inversion (i.e., more atoms or
molecules in the excited state than in the lower state). Once
population inversion occurs, an avalanche of photons can be
generated by stimulated emission. Initial, spontaneously emitted
photons stimulate other excited atoms to emit photons of the same
energy in phase with one another. This process is Light
Amplification by Stimulated Emission of Radiation, with the
acronym, LASER.
Fig. 4 shows a simplified 3-level energy diagram for a laser
material. This is just one of the many possible systems of energy
levels. Though laser action is possible with only 3 energy levels,
most such actions involve 4 or more levels.
The ratio of the theoretically possible spectral emittance to
the actual emittance of a grey body is the emissivity. For
instance, the emissivity of tungsten throughout the visible is
approximately 0.4.
A useful relation for black-body sources is the Stefan-
Boltzmann Law, which states that the radiant exitance W integrated
over all wavelengths of a black body is proportional to the fourth
power of the absolute temperature of the body, i.e.:
W = sigmaT4
3.1. Molecular and Atomic Transitions
Other sources of light such as carbon arcs, gas-filled arc
lamps, or gas discharge lamps, depart widely from black-body
characteristics, i.e., vary greatly with the wavelength in the
visible region. In these cases, a stream of electrons flowing
through a gas induces an emission of photons, characteristic of
that particular gas. If gas has a low pressure and the current is
not great, a line spectrum is emitted. Line spectra are the result
of atomic transition. As the gas pressure and the current density
increase, the gas temperature increases and a continuous spectrum
appears. At high current densities and gas pressures, this type of
emission (a continuum) predominates.
The energy Qq of a single photon, emitted because of an atomic
transition, is determined by the frequency of the emitted radiation
as defined by the condition:
Qq = xi1 - xi2 = h nu Equation (6)
where xi1 and xi2 are energies corresponding to the initial and
final energy states, h is the Plank constant (6.625 x 10-34J x s),
and nu is the frequency of radiation (in Hz).
Energy transitions in molecular systems can result in a
radiation emission according to rules similar to those that apply
to atomic systems. The energies (0.001-0.1 eV) of molecular
vibrational or rotational transitions are, typically, less than
those characteristic of electron transitions in atoms or molecules
(1-100 eV). In addition to the electron "orbital" potential and
kinetic energies, part of the energy of molecular systems is
associated with rotational and vibrational modes. Emissions of
this type occur in the infrared and microwave regions of the
electromagnetic spectrum. Heat is the vibrational energy of
molecular systems.
4. LASERS
All lasers have three basic components: (a) a laser (active)
medium; (b) an energy source (pumping system); and (c) a resonant
optical cavity. Lenses, mirrors, shutters, saturable absorbers,
and other accessories may be added to the system to obtain greater
power, shorter pulses, or special beam shapes, but only the three
basic components (a, b, and c) are necessary for laser action.
4.1. The Laser Medium
Laser action depends on the ability of the laser (active)
medium to undergo population inversion (i.e., more atoms or
molecules in the excited state than in the lower state). Once
population inversion occurs, an avalanche of photons can be
generated by stimulated emission. Initial, spontaneously emitted
photons stimulate other excited atoms to emit photons of the same
energy in phase with one another. This process is Light
Amplification by Stimulated Emission of Radiation, with the
acronym, LASER.
Fig. 4 shows a simplified 3-level energy diagram for a laser
material. This is just one of the many possible systems of energy
levels. Though laser action is possible with only 3 energy levels,
most such actions involve 4 or more levels.
 4.2. The Pumping System
Pumping systems are necessary to raise electrons to a higher
energy level in lasers. These systems pump energy into the laser
material, increasing the number of atoms or molecules trapped in
the metastable energy level, until a population inversion exists
large enough to make laser action possible (Fig. 4). Several
different pumping systems are available including optical, electron
collision, and chemical reaction.
In optical pumping, a strong source of light is used, such as a
xenon flashtube or another laser (e.g., an argon or nitrogen
laser), generally of a shorter wavelength than that emitted by the
medium.
Electron collision pumping is accomplished by passing an
electric current through a laser medium, usually a gas (e.g.,
helium-neon laser) or a semiconductor junction (e.g., gallium-
arsenide laser), or by accelerating electrons in an electron gun to
impact on the laser material, as in some semiconductor or gas
lasers.
Chemical pumping is based on energy released in the making and
breaking of chemical bonds. For example, some hydrogen fluoride
(HF) or deuterium fluoride (DF) lasers are pumped in this manner.
4.3. The Resonant Optical Cavity
A resonant optical cavity is formed by placing a mirror at each
end of the laser medium so that a beam of UVR, light, or IR
radiation may be reflected from one mirror to the other. Lasers
are constructed in this way so that the beam passes through the
laser medium one or more times and the number of emitted photons is
amplified at each passage. One of the mirrors is only partially
reflecting and permits part of the beam to be transmitted out of
the cavity at each reflection (Fig. 5). The alignment, curvature,
and separation distance of the mirrors determine the shape (mode
structure) of the emitted laser beam.
4.2. The Pumping System
Pumping systems are necessary to raise electrons to a higher
energy level in lasers. These systems pump energy into the laser
material, increasing the number of atoms or molecules trapped in
the metastable energy level, until a population inversion exists
large enough to make laser action possible (Fig. 4). Several
different pumping systems are available including optical, electron
collision, and chemical reaction.
In optical pumping, a strong source of light is used, such as a
xenon flashtube or another laser (e.g., an argon or nitrogen
laser), generally of a shorter wavelength than that emitted by the
medium.
Electron collision pumping is accomplished by passing an
electric current through a laser medium, usually a gas (e.g.,
helium-neon laser) or a semiconductor junction (e.g., gallium-
arsenide laser), or by accelerating electrons in an electron gun to
impact on the laser material, as in some semiconductor or gas
lasers.
Chemical pumping is based on energy released in the making and
breaking of chemical bonds. For example, some hydrogen fluoride
(HF) or deuterium fluoride (DF) lasers are pumped in this manner.
4.3. The Resonant Optical Cavity
A resonant optical cavity is formed by placing a mirror at each
end of the laser medium so that a beam of UVR, light, or IR
radiation may be reflected from one mirror to the other. Lasers
are constructed in this way so that the beam passes through the
laser medium one or more times and the number of emitted photons is
amplified at each passage. One of the mirrors is only partially
reflecting and permits part of the beam to be transmitted out of
the cavity at each reflection (Fig. 5). The alignment, curvature,
and separation distance of the mirrors determine the shape (mode
structure) of the emitted laser beam.
 4.4. Types of Lasers
Lasers can be categorized in a variety of ways, e.g., according
to the active medium or temporal mode of operation.
4.4.1. Active media
Lasers are often designated according to the type of laser
medium, as follows:
(a) Solid-state lasers: a glass or crystalline medium
into which active atoms are introduced;
(b) Gas lasers: a medium of pure gas or a mixture of
gases; this category also includes metal vapour
lasers;
(c) Semi-conductor lasers: a medium of n-type and p-type
semiconducting element material;
(d) Liquid lasers: a liquid medium containing an active
material, such as an organic dye, in solution or
suspension.
Optical pumping (both coherent and incoherent) is usually used
in the production of solid-state and liquid lasers while collision
pumping is usually employed to produce gas lasers. However,
chemical-reaction pumping is also used for some types of liquid
and gas lasers. Semiconductor lasers may be optically pumped by an
electric current, another laser beam, or electron-collision from an
electron beam. Table 4 provides an abbreviated list of
commercially available laser wavelengths.
4.4.2. Temporal modes of operation
Some lasers operate continuously, and are termed continuous
wave (cw). In this type of operation, the peak power is equal to
the average power output; that is, the beam irradiance is constant
with time. Many lasers that appear to be cw may actually have a
temporal structure that can only be resolved with very
sophisticated systems of measurement.
The different temporal modes of operation of a laser are
distinguished by the rate at which energy is delivered. In
general, lasers operating in the normal pulse (or "long pulse")
temporal mode have pulse durations of a few tens of µs to a few ms
(Descomps, 1981).
Pulsed lasers can be operated to produce repetitive pulses.
The pulse repetition frequency of a laser is the number of pulses
that a particular laser produces per unit time duration. Lasers
are now available with pulse repetition frequencies as high as
several million pulses per s (MHz).
Table 4. Common lasers
-------------------------------------------------------------------
CIE band Wavelength (nm) Medium Typical operation
-------------------------------------------------------------------
Excimer UVC + B XeCl, XeFl, etc. pulsed
UV-A 325 He-Cd cw
UV-A 337 Nitrogen pulse train
UV-A 350 Argon cw
-------------------------------------------------------------------
Light 441.6 He-Cd cw
Light 458, 488, 514.5 Argon cw
Light 458, 568, 647 Krypton cw
Light 530 or 532 Nd frequency-doubled pulsed
Light 632.8 He-Ne cw
Light 694.3 Ruby pulsed/Q-pulsed
Light 560-640 Rhodamine 6G dye cw/pulsed
-------------------------------------------------------------------
IR-A 850 GaAlAs pulse train
IR-A 905 GaAs pulse train
IR-A 1060 Nd: glass pulsed/Q-pulsed
IR-A 1064 Nd: YAG cw/pulsed/Q-pulsed
-------------------------------------------------------------------
IR-C 5000 CO cw/pulsed
IR-C 10 600 CO2 cw/pulsed
-------------------------------------------------------------------
The resonant quality of the optical cavity of a laser can be
altered by rotating one mirror or by placing a shutter between the
mirrors. The shutter may be active (e.g., pockels cell) or passive
(a saturable absorber). This enables the beam to be turned on and
off rapidly and normally creates pulses with a duration of a few ns
to a few µs. This operation is normally called Q-switching (or
Q-spoiling or giant pulsing) (Fig. 6). The "Q" refers to the
resonant quality of the optical cavity. A Q-switched laser usually
emits less energy than the same laser emitting normal pulses, but
the energy is emitted in a much shorter period of time. Thus,
Q-switched lasers are capable of delivering very high peak powers
of several megawatts or even gigawatts. Fig. 6 shows a variety of
oscilloscope traces including a normal pulse and a Q-switched
pulse.
When the phases of a number of oscillating modes in a laser
resonator are forced to maintain a fixed relation to one another
through a non-linear absorber placed in the resonator, the laser
output observed is a train of regularly spaced ultra-short pulses.
This is termed a mode-locked laser. In a train of pulses, each
pulse has a duration of a few picoseconds (ps) to a few ns. A
mode-locked laser can deliver higher peak powers than the same
laser when Q-switched (Dautray & Watteau, 1980). Fig. 6 also shows
a mode-locked pulse train from a pulsed Nd-YAG laser.
4.4. Types of Lasers
Lasers can be categorized in a variety of ways, e.g., according
to the active medium or temporal mode of operation.
4.4.1. Active media
Lasers are often designated according to the type of laser
medium, as follows:
(a) Solid-state lasers: a glass or crystalline medium
into which active atoms are introduced;
(b) Gas lasers: a medium of pure gas or a mixture of
gases; this category also includes metal vapour
lasers;
(c) Semi-conductor lasers: a medium of n-type and p-type
semiconducting element material;
(d) Liquid lasers: a liquid medium containing an active
material, such as an organic dye, in solution or
suspension.
Optical pumping (both coherent and incoherent) is usually used
in the production of solid-state and liquid lasers while collision
pumping is usually employed to produce gas lasers. However,
chemical-reaction pumping is also used for some types of liquid
and gas lasers. Semiconductor lasers may be optically pumped by an
electric current, another laser beam, or electron-collision from an
electron beam. Table 4 provides an abbreviated list of
commercially available laser wavelengths.
4.4.2. Temporal modes of operation
Some lasers operate continuously, and are termed continuous
wave (cw). In this type of operation, the peak power is equal to
the average power output; that is, the beam irradiance is constant
with time. Many lasers that appear to be cw may actually have a
temporal structure that can only be resolved with very
sophisticated systems of measurement.
The different temporal modes of operation of a laser are
distinguished by the rate at which energy is delivered. In
general, lasers operating in the normal pulse (or "long pulse")
temporal mode have pulse durations of a few tens of µs to a few ms
(Descomps, 1981).
Pulsed lasers can be operated to produce repetitive pulses.
The pulse repetition frequency of a laser is the number of pulses
that a particular laser produces per unit time duration. Lasers
are now available with pulse repetition frequencies as high as
several million pulses per s (MHz).
Table 4. Common lasers
-------------------------------------------------------------------
CIE band Wavelength (nm) Medium Typical operation
-------------------------------------------------------------------
Excimer UVC + B XeCl, XeFl, etc. pulsed
UV-A 325 He-Cd cw
UV-A 337 Nitrogen pulse train
UV-A 350 Argon cw
-------------------------------------------------------------------
Light 441.6 He-Cd cw
Light 458, 488, 514.5 Argon cw
Light 458, 568, 647 Krypton cw
Light 530 or 532 Nd frequency-doubled pulsed
Light 632.8 He-Ne cw
Light 694.3 Ruby pulsed/Q-pulsed
Light 560-640 Rhodamine 6G dye cw/pulsed
-------------------------------------------------------------------
IR-A 850 GaAlAs pulse train
IR-A 905 GaAs pulse train
IR-A 1060 Nd: glass pulsed/Q-pulsed
IR-A 1064 Nd: YAG cw/pulsed/Q-pulsed
-------------------------------------------------------------------
IR-C 5000 CO cw/pulsed
IR-C 10 600 CO2 cw/pulsed
-------------------------------------------------------------------
The resonant quality of the optical cavity of a laser can be
altered by rotating one mirror or by placing a shutter between the
mirrors. The shutter may be active (e.g., pockels cell) or passive
(a saturable absorber). This enables the beam to be turned on and
off rapidly and normally creates pulses with a duration of a few ns
to a few µs. This operation is normally called Q-switching (or
Q-spoiling or giant pulsing) (Fig. 6). The "Q" refers to the
resonant quality of the optical cavity. A Q-switched laser usually
emits less energy than the same laser emitting normal pulses, but
the energy is emitted in a much shorter period of time. Thus,
Q-switched lasers are capable of delivering very high peak powers
of several megawatts or even gigawatts. Fig. 6 shows a variety of
oscilloscope traces including a normal pulse and a Q-switched
pulse.
When the phases of a number of oscillating modes in a laser
resonator are forced to maintain a fixed relation to one another
through a non-linear absorber placed in the resonator, the laser
output observed is a train of regularly spaced ultra-short pulses.
This is termed a mode-locked laser. In a train of pulses, each
pulse has a duration of a few picoseconds (ps) to a few ns. A
mode-locked laser can deliver higher peak powers than the same
laser when Q-switched (Dautray & Watteau, 1980). Fig. 6 also shows
a mode-locked pulse train from a pulsed Nd-YAG laser.
 4.5. Spatial (TEM) Modes
A cross-sectional wave pattern is characteristic of all laser
beam geometries (transverse electromagnetic wave or TEM). These
wave patterns across the beam are identified with TEM mode
notation. Fig. 7 illustrates how some of the more common modes
would appear in cross section. The TEM01 mode is similar to the
TEM10 mode rotated through 90°.
4.5. Spatial (TEM) Modes
A cross-sectional wave pattern is characteristic of all laser
beam geometries (transverse electromagnetic wave or TEM). These
wave patterns across the beam are identified with TEM mode
notation. Fig. 7 illustrates how some of the more common modes
would appear in cross section. The TEM01 mode is similar to the
TEM10 mode rotated through 90°.
 Longitudinal (or axial) modes do not influence the emergent
beam profile, but influence the degree of coherency of the spatial
and the temporal frequency spectrum and are, therefore, of no great
significance in the consideration of biological effects (unless
they are intentionally or accidentally mode-locked to produce ps
pulses).
4.6. Beam Characteristics
4.6.1. Beam diameter
The beam diameter of a laser operating in the TEM00 mode has
been variously defined as the circle where the irradiance or
radiant exposure is 1/2, 1/e, 1/e2, or 1/10 of the maximum (Fig. 8).
In almost all discussions in the health and safety literature, the
edge of the beam is defined as 1/e or 0.37 of the maximum, whereas
the beam diameter is almost always defined at 1/e2 points in the
laser industry.
Longitudinal (or axial) modes do not influence the emergent
beam profile, but influence the degree of coherency of the spatial
and the temporal frequency spectrum and are, therefore, of no great
significance in the consideration of biological effects (unless
they are intentionally or accidentally mode-locked to produce ps
pulses).
4.6. Beam Characteristics
4.6.1. Beam diameter
The beam diameter of a laser operating in the TEM00 mode has
been variously defined as the circle where the irradiance or
radiant exposure is 1/2, 1/e, 1/e2, or 1/10 of the maximum (Fig. 8).
In almost all discussions in the health and safety literature, the
edge of the beam is defined as 1/e or 0.37 of the maximum, whereas
the beam diameter is almost always defined at 1/e2 points in the
laser industry.
 4.6.2. Beam divergence
The wave nature of light prevents lasers from producing
perfectly collimated beams. However, the divergence or beam
spreading is much smaller than that of a searchlight or other
conventional sources of optical radiation.
4.6.3. Beam irradiance versus range for a circular beam
To define potential exposure conditions, it is necessary to
characterize the beam emitted from a laser. The beam's
characteristics may be required near the output of the laser or at
some considerable distance from the laser, after it has been
collimated or focused. The optical radiation emitted by most
lasers is confined to a rather narrow beam that slowly diverges or
fans out as the beam propagates. The beam diameter DL increases
from an initial diameter a at the laser exit port as a result of
the divergence phi:
DL = a + r phi Equation (7)
where r is the range (distance from the laser).
With the beam diameter defined as a function of distance from
the laser, it is a simple matter to derive a formula to estimate
the beam irradiance or radiant exposure at any distance r. The
beam irradiance E (in W/m2 or W/cm2) would be the total power phi
in the beam (in watts) divided by the area of the cross section of
the beam (usually expressed in m2 or cm2). For health risk
assessment, a defining aperture of irradiance measurement is
normally specified (e.g., 7-mm circular aperture).
The effect of atmospheric attenuation may become a major factor
in evaluating the irradiance or radiant exposure at distances
greater than a few kilometres. This attenuation is the result of
three effects: (a) Mie (or large particle) scattering; (b)
Rayleigh (or molecular) scattering; and (c) absorption by gas
molecules. Rayleigh scattering is the most wavelength dependent;
shorter wavelengths are predominantly scattered. The atmospheric
attenuation may best be expressed by an exponential function. The
attenuation of optical radiation could be described by a term (eµr)
where µ is termed the attenuation coefficient of the medium. It is
the sum of scattering coefficients and absorption coefficients of
the medium through which the laser beam propagates. One equation
that is a close approximation for calculating the axial beam
irradiance is:
E = 1.27 phi e-µr/(a + r phi)2 Equation (8)
and a corresponding equation for radiant exposure H from a pulsed
laser of output energy Q is:
H = 1.27 Qe-µr/(a + r phi)2 Equation (9)
These equations can be adjusted for other beam profiles using
simple geometry. The emergent beam diameter term, a, may be
dropped at distances where a << rphi. Equations 7, 8, and 9 are
close approximations to rigorous formulations of Gaussian optics.
4.6.4. Hot spots
Hot spots are defined as areas of the beam, where the localized
beam irradiance is much greater than the average across the beam.
As the irradiance of hot spots may be many times higher than the
average beam irradiance, they are of considerable concern in
relation to health. There are several sources of hot spots:
inhomogeneities in the laser cavity or areas of the active medium,
where more energy is emitted than in other areas; imperfections in
the mirrors and lenses of the laser system; and changes caused by
atmospheric conditions. Atmospheric inhomogeneities along the beam
path produce lenticular effects (scintillation) that are
responsible for atmospheric hot spots. Fog, rain, snow, dust,
smoke, or haze absorb and/or scatter the laser beam but do not
cause hot spots. Such scattering reduces the severity of hot
spots.
4.6.5. Coherence
Two types of coherence are characteristic of laser light:
spatial and temporal. The term spatial coherence indicates that
the optical radiation is spatially in phase, i.e., electromagnetic
waves at different points in space oscillate in synchronism. Laser
speckle is a consequence of spatial coherence. Temporal coherence
indicates that the radiation is strictly monochromatic (of one
wavelength). No light source is either totally coherent or totally
incoherent; the differences between individual lasers and, for that
matter, non-laser sources are merely a matter of degree. The term
"coherence length" is used to describe the degree of spatial
coherence.
5. RADIOMETRIC CONCEPTS
5.1. Radiometric and Photometric Terminology
Two systems of quantities and units are used to describe
optical radiation. One is a physical system called the radiometric
system. The other, the photometric system, attempts to describe
the optical radiation in terms of its ability to elicit the
sensation of light by the eye. Table 5 gives the most commonly
used quantities and the preferred units for each system. There are
generally analogous units in each of the 2 systems. The table is
arranged to illustrate these similarities. Though the radiometric
system of units may be used across the entire spectrum, the
photometric system is limited to describe light (i.e.,
electromagnetic radiation that is visible) from approximately
380 - 400 nm to 760 - 780 nm.
It is important to remember that some terms refer only to
extended sources (e.g., radiance) and other terms (e.g., radiant
intensity) refer only to "point" sources.
5.2. Extended Sources Versus Point Sources
Lasers are often treated as "point" sources, whereas most
conventional light sources are considered to be extended sources,
at least at close distances. An extended source is one that
appears to have some angular extent as seen by the viewer. The
moon is an extended source; a star is a "point" source. Apart from
lasers, a light source can be considered a point source only at a
great distance, or if a pinhole diaphragm is placed in front of the
light source. All other light sources are considered to be
extended sources.
5.3. Inverse Square Law
The inverse square law for calculating the irradiance or
radiant exposure at a distance from a source applies only to a
point source. For example, the ratio of irradiance E1, at one
distance r1 to E2 at another distance r2 is:
El = r22 Equation (10)
E2 r12
For practical purposes, extended sources can be considered as
"point" sources at a distance many times greater than the source
dimension. Both r1 and r2 should be at least as great as 10 source
diameters for a diffuse lambertian source. This also applies to
equation 3. The irradiance E at a distance r from a point source
is:
E = I/r2 Equation (11)
This equation applies to collimated extended sources (e.g.,
searchlights) or lasers, only at considerable distances from the
source.
Table 5. Useful CIE radiometric and photometric quantitities and unitsa,b
-------------------------------------------------------------------------------------
RADIOMETRIC
-------------------------------------------------------------------------------------
Term Symbol Defining equation Quantity SI units &
applicablec abbreviations
-------------------------------------------------------------------------------------
Radiant energy Qe S, R joule (J)
-------------------------------------------------------------------------------------
Radiant energy dQe F joule per cubic
density We We = dV metre (J/m3)
-------------------------------------------------------------------------------------
Radiant power dQe S, R watt (W)
(radiant flux) phieP phie = dt
-------------------------------------------------------------------------------------
Radiant d phie S watt per square
exitance Me Me = dA metre (W/m2)
= /Le x cos x d omega
-------------------------------------------------------------------------------------
Irradiance or d phie R watt per square
flux density Ee Ee = dA metre (W/m2)
(dose rate in
photobiology)
-------------------------------------------------------------------------------------
Radiant d phie S watt per
intensity Ie Ie = d omega steradian
(W/sr1)
-------------------------------------------------------------------------------------
Radiance d d2phie S, F, R watt per
------------------------ steradian and
Le 1e = d omega x dA x cos theta per square metre
(W/sr/m2)
--------------------------------------------------------------------------------------
Radiant dQe R joule per square
exposure He He = dA metre (J/m2)
(dose in
photobiology)
--------------------------------------------------------------------------------------
Radiant P S unitless
efficiencye etae etae = Pi
(of a source)
--------------------------------------------------------------------------------------
Optical De De = -log10taue R unitless
--------------------------------------------------------------------------------------
Table 5. (contd.)
------------------------------------------------------------------------------------
PHOTOMETRIC
------------------------------------------------------------------------------------
Term Symbol Defining equation SI abbreviations
& units
------------------------------------------------------------------------------------
Quantity of Qnu Qnu = /phinudt lumen-second
light (lm x s)
------------------------------------------------------------------------------------
Luminous dQnu lumen-second per
energy density Wnu Wnu = dV cubic metre
(lm x s/m3)
------------------------------------------------------------------------------------
Luminous flux phinu d phie lumen (lm)
-----------------------
phinu = 680 / d lamdaV(lamda)d lamda
------------------------------------------------------------------------------------
Luminous d phinu lumen per square
exitance Mnu Mnu = dA metre (lm/m2)
= /Inu x cos phi x d omega
------------------------------------------------------------------------------------
Illuminance d phinu lumen per square
(luminous Enu Enu = dA metre (lm/m2)
density)
------------------------------------------------------------------------------------
Luminous d phinu lumen per
intensity Inu Inu = dr steradian (lm x sr)
(candlepower) or candela (cd)
------------------------------------------------------------------------------------
Luminance d Lnu d2phie candela per square
------------------- metre (cd/m2)
Lnu = dr x dA x cos theta
------------------------------------------------------------------------------------
Light exposure dQnu lux-second
Hnu Hnu = dA (lx x s)
= /Enudt
------------------------------------------------------------------------------------
Luminous phinu lumen per watt
efficacy (of K K = phie (lm/W)
radiation)
------------------------------------------------------------------------------------
Luminous K K unitless
efficiency V(*) V(*) = / Km = 680
(of a broad
band radiation)
------------------------------------------------------------------------------------
Luminous phinu lumen per watt
efficacye etanu etanu = Pi (lm/W)
------------------------------------------------------------------------------------
Table 5. (contd.)
------------------------------------------------------------------------------------
PHOTOMETRIC
------------------------------------------------------------------------------------
Term Symbol Defining equation SI abbreviations
& units
------------------------------------------------------------------------------------
Optical unitless
densityf Dnu Dnu = -log10taunu
------------------------------------------------------------------------------------
Retinal Troland (td) =
illuminance Et Et = Lnu x Sp luminance of 1 cd/
(in trolands) m2 times pupil
area in mm2
------------------------------------------------------------------------------------
a The quantities may be altered to refer to narrow spectral bands, in which case
the term is preceded by the word spectral, and the unit is then per unit of
wavelength and the symbol has a subscript lambda. For example, spectral
irradiance Hlambda has units of W/(m2 x m) or more often, W/(cm2 x nm).
b While the metre is the preferred unit of length, the centimetre is still the
most commonly used unit of length for many of the above terms and the nm or µm
are most commonly used to express wavelength.
c Some radiometric quantities refer only to the source, field, or receiver. This
noted in this column.
d At the source, dM ; at a receptor, dE
L = d omega x cos theta L = d omega x cos theta
e Pi is electrical input power in watts.
f tau is the transmission; Dnu is also abbreviated as O.D.
6. RADIOMETRIC AND PHOTOMETRIC MEASUREMENT
6.1. Introduction
Reliable radiometric techniques and instruments are available
that make it possible to analyse risks for the skin and eye from
exposure to lasers and other sources of optical radiation.
However, the cost of accurate equipment remains relatively high
compared with that of survey equipment now available to evaluate
many other environmental risks. Radiometric formulae and
manufacturers' specifications of lasers will often be an adequate
substitute for measurement.
There are many types of measurements for defining conditions or
characterizing a source's output. The types of measurements
considered in this section fall under the broad term of
"radiometric". For characterizing a conventional light source,
radiance is generally the most useful. For laser output
measurements, radiant power and radiant energy are by far the most
important. Irradiance and radiant exposure are of greater
importance in defining hazardous exposure conditions from all
optical sources.
In any discussion of the measurement of laser radiation for
purposes of evaluating health risks, it is important first to
clarify the conditions and requirements for such measurements.
Industrial and environmental health specialists and health
physicists usually rely heavily on instruments to detect or
estimate a chemical or physical agent that their own human senses
cannot detect. The presence of a laser beam can generally be
detected by the human eye or through the use of an image converter,
thus raising the question "Why should the laser beam be measured?".
It soon becomes evident that, in most cases, even routine
monitoring of either a work area or an individual by
instrumentation is a hopeless task. A more logical approach to
risk assessment is to develop a means of analysing the potential
risk of a laser, based on the laser's output parameters.
As a general rule, present standards require only measurement
of the laser-output characteristics for laser risk classification.
Routine monitoring is seldom considered necessary and all
measurements are normally performed only once, by (or for) the
manufacturer of the laser equipment. Periodic measurements may be
considered worthwhile for certain lasers that are near the
borderline between two classes in the hazard classification and
field measurements of outdoor laser propagation paths have often
been found useful. Unlike most noxious agents, a high-powered
laser beam is almost always hazardous for a considerable distance
and its hazard generally exceeds exposure limits by orders of
magnitude. Diagnostics of the beam profile and measurement of beam
divergence have been discussed.
The evaluation of more conventional broad-band sources is more
complex, since spectral characteristics and source size must be
considered. To evaluate a broad-band optical source, it is
normally necessary to determine the spectral distribution of
optical radiation emitted from the source at the point or points of
human access. The spectral distribution of the accessible
emission, which is of interest for a lighting system, may differ
from that actually being emitted by the lamp alone because of
apertures or filtration by any optical elements in the light path.
Secondly, the size, or projected size, of the source must be
characterized in the retinal hazard spectral region. Thirdly, it
may be necessary to determine the variation of irradiance and
radiance with distance. The necessary measurements are normally
complex. The spectrum of an arc lamp, a gas discharge lamp, or a
fluorescent lamp consists of both line structure and a continuum.
Significant errors can be introduced in the representation of the
spectrum and in the weighting of the spectrum against a biological-
or a safety-action spectrum, if the fraction of energy in each line
is not properly added to the continuum.
6.2. Measurement Instrumentation
The radiometric instruments of interest in this discussion
generally consist of detectors that produce a voltage, a current, a
resistance change, or an electronic charge, one of which is
measured by a sensitive electronic meter. The type of read-out
meter for the radiometric instrument is not normally of great
concern and seldom determines the selection of the instrument.
There are both advantages and disadvantages associated with each
type of detector and each has certain characteristics that may be
useful for measuring a specific level of optical radiation in a
wavelength range of interest. No single detector is best for
measuring all wavelengths and radiant powers of optical radiation.
A very sensitive detector can be readily damaged or its response
distorted by a high-powered laser beam, whereas a detector designed
to measure very high-powered laser radiation is normally
insensitive to low-power radiation. Narrow-band detectors have the
advantage of being insensitive to extraneous radiation, though
their usefulness is limited to measurement of lasers operating in
that particular spectral band.
In many countries, national physical standards laboratories
exist, which offer calibration services for some radiometric
instruments. Examples are: Laboratoire National d'Essais (France);
National Physical Laboratory (United Kingdom); Assistance Committee
for Measures and Standards (USSR); National Bureau of Standards
(USA); and Physikalisch-Technische Bundesanstalt (Federal Republic
of Germany).
6.2.1. Thermal detectors
Thermal detectors are mainly used for measuring the output
power or energy of lasers and total irradiances from broad-band
optical sources, in particular infrared sources. Some of these
detectors are particularly useful for absolute measurements.
Thermopiles, bolometers, disc calorimeters, and pyroelectric
detectors are characterized by a relatively flat response as a
function of wavelength. The spectral response of these detectors
is dictated by the "black" absorbers that are normally used to coat
the detector's metal or crystalline substrate. As optical energy
falls on the detector, the temperature increases. The temperature
rise in the substrate is then converted into an electrical voltage
or current. Because of the thermal mass of the metal, the time
required to heat or cool the detector element limits the response
time of the instrument. The absorber in a disc calorimeter may be
a black painted disc or a glass volume absorber (James, ed. 1976).
In recent years, the response time of thermopiles has been
shortened by using thin-film techniques. Low powers (typically
0.01 - 100 mW) can be measured and the response time reduced.
Pyroelectric detectors measure the rate of temperature change in a
crystalline material rather than the final temperature elevation in
a metal. Radiometric calorimeters can be used to measure cw
radiation over the power range from 1 mW to over 1 kW, depending on
the detector and wavelength. Pulsed radiant energy can be measured
over the range from 10 mJ to 10 kJ.
The detector may be covered by a window, which limits spectral
response. Quartz windows are necessary for UVR, but there is
probably no window material that is universally flat from 200 to
20 000 nm.
6.2.2. Quantum detectors
Quantum detectors operate normally at room temperature and
offer by far the most sensitive means of measuring optical
radiation, therefore, their principle use is in spectroradiometers
and detectors required for the measurement of lower powers and
irradiances or for temporal resolution of pulses. The spectral
sensitivity of photoemissive detectors depends on the photocathode
material used in vacuum photodiodes or photomultiplier tubes, or
in the characteristics of (doped) silicon. All detectors that
operate by means of the photoelectric effect have a characteristic
cutoff wavelength. At wavelengths greater than this cutoff,
photons are largely ineffective in producing photoelectrons and the
resulting photocurrent.
Because of the strong spectral dependence of the photodiode,
these instruments are often not direct reading and the meter
reading may have to be multiplied by one of several calibration
factors.
Simple silicon-detector instruments can be quite useful, when
the natural spectral response of silicon (approx 200 - 1100 nm) is
changed by an appropriate input filter to yield a flat spectral
response from 450 to 950 nm (Marshall, 1980).
6.2.3. Detectors to resolve short pulses
A variety of techniques have been developed to resolve the
temporal behaviour of short laser pulses. An ultrafast
oscilloscope with a solid-state silicon detector or biplanar vacuum
photodiode is most often used to display the pulse shape of a
Q-switched (1.0 - 100 ns) pulse. For temporal domains of less than
1 ns, streak cameras and some non-linear optical techniques are
used to resolve the structure of a train of mode-locked laser
pulses.
The techniques used in photometry and radiometry are far too
numerous and complex to detail here (see for example: Grum &
Becherer, ed. 1979; Le Bodo, 1976; or Sliney & Wolbarsht, 1980).
Differences in measured values for the same source from each of two
different laboratories may arise through a problem of "geometry" or
incorrect allowance for extraneous light.
6.2.4. Safety meters
At present, inexpensive, portable radiometric measuring
instruments that have been designed specifically for the risk
analysis of a great variety of lasers, are not available. Indeed,
it is unlikely that such instruments will be made in the future,
because of the great variation in exposure criteria for different
wavelengths and different exposure durations. The same holds true
for non-laser optical source survey instruments. However, some
relatively expensive, microprocessor-based instruments have been
developed to cover a wide range of measurements. Simple
instruments are possible for the purpose of measuring one type of
laser or optical source.
Because of the great interest in photometry, there are many
satisfactory photometers that measure both luminance and
illuminance and follow the CIE photopic function Vlambda quite
well. This is not always the case for the other weighting
functions. Direct reading UVR instruments are a case in point.
The principal difficulty in developing a suitable UVR instrument is
the rejection of unwanted wavelengths. It is difficult to measure
only the UV-B and UV-C radiation with sufficient sensitivity, while
still rejecting all of the UV-A and visible light.
6.2.5. Spectroradiometers
As well as broad-band measurements, it is often necessary to
measure the spectrum of a conventional source. A grating or prism
monochromator is used to resolve the spectrum.
An important part of measuring the spectral distribution of a
broad-band lamp source or an arc process is the specification of
the desired bandwidth, and the intervals at which data will be
recorded. One of the most useful approaches is to scan through a
spectrum and record the detector output in analogue fashion on an
X-Y recorder, rather than to record digitized data.
An X-Y recorder can indicate the bandwidth of the monochromator
and may quite often indicate the regions of the spectrum in which
problems may arise from stray light or extraneous signals.
The required bandwidth and sampling interval are determined by
comparing the so-called "slit function" of the monochromator system
with the need for sufficient spectral resolution to make possible
accurate weighting against action spectra used in risk analysis.
Two common difficulties are encountered in obtaining an
accurate radiometric description of a broad-band, extended source.
The first problem is to achieve adequate rejection of unwanted
wavelengths from the passband of the monochromator (e.g., rejecting
"stray light"). The second is the proper definition of the actual
or effective source size of an arc or a discharge lamp. Several
other special problem areas (such as background isolation,
wavelength calibration, and the proper separation of line and
continuous values) are also encountered in specific situations.
6.3. Biological Weighting of Spectroradiometric Data
Many of the calculations that are useful in risk analyses
require weighting of the measured spectrum against a biological
action spectrum. There are several, including the erythemal and
the photokeratitic action spectra, the photopic response V lambda
of the eye, and the retinal photochemical injury action spectrum B
lambda (Ham, et al., 1976; ACGIH, 1981; Sliney & Wolbarsht, 1980)
(Fig. 9).
4.6.2. Beam divergence
The wave nature of light prevents lasers from producing
perfectly collimated beams. However, the divergence or beam
spreading is much smaller than that of a searchlight or other
conventional sources of optical radiation.
4.6.3. Beam irradiance versus range for a circular beam
To define potential exposure conditions, it is necessary to
characterize the beam emitted from a laser. The beam's
characteristics may be required near the output of the laser or at
some considerable distance from the laser, after it has been
collimated or focused. The optical radiation emitted by most
lasers is confined to a rather narrow beam that slowly diverges or
fans out as the beam propagates. The beam diameter DL increases
from an initial diameter a at the laser exit port as a result of
the divergence phi:
DL = a + r phi Equation (7)
where r is the range (distance from the laser).
With the beam diameter defined as a function of distance from
the laser, it is a simple matter to derive a formula to estimate
the beam irradiance or radiant exposure at any distance r. The
beam irradiance E (in W/m2 or W/cm2) would be the total power phi
in the beam (in watts) divided by the area of the cross section of
the beam (usually expressed in m2 or cm2). For health risk
assessment, a defining aperture of irradiance measurement is
normally specified (e.g., 7-mm circular aperture).
The effect of atmospheric attenuation may become a major factor
in evaluating the irradiance or radiant exposure at distances
greater than a few kilometres. This attenuation is the result of
three effects: (a) Mie (or large particle) scattering; (b)
Rayleigh (or molecular) scattering; and (c) absorption by gas
molecules. Rayleigh scattering is the most wavelength dependent;
shorter wavelengths are predominantly scattered. The atmospheric
attenuation may best be expressed by an exponential function. The
attenuation of optical radiation could be described by a term (eµr)
where µ is termed the attenuation coefficient of the medium. It is
the sum of scattering coefficients and absorption coefficients of
the medium through which the laser beam propagates. One equation
that is a close approximation for calculating the axial beam
irradiance is:
E = 1.27 phi e-µr/(a + r phi)2 Equation (8)
and a corresponding equation for radiant exposure H from a pulsed
laser of output energy Q is:
H = 1.27 Qe-µr/(a + r phi)2 Equation (9)
These equations can be adjusted for other beam profiles using
simple geometry. The emergent beam diameter term, a, may be
dropped at distances where a << rphi. Equations 7, 8, and 9 are
close approximations to rigorous formulations of Gaussian optics.
4.6.4. Hot spots
Hot spots are defined as areas of the beam, where the localized
beam irradiance is much greater than the average across the beam.
As the irradiance of hot spots may be many times higher than the
average beam irradiance, they are of considerable concern in
relation to health. There are several sources of hot spots:
inhomogeneities in the laser cavity or areas of the active medium,
where more energy is emitted than in other areas; imperfections in
the mirrors and lenses of the laser system; and changes caused by
atmospheric conditions. Atmospheric inhomogeneities along the beam
path produce lenticular effects (scintillation) that are
responsible for atmospheric hot spots. Fog, rain, snow, dust,
smoke, or haze absorb and/or scatter the laser beam but do not
cause hot spots. Such scattering reduces the severity of hot
spots.
4.6.5. Coherence
Two types of coherence are characteristic of laser light:
spatial and temporal. The term spatial coherence indicates that
the optical radiation is spatially in phase, i.e., electromagnetic
waves at different points in space oscillate in synchronism. Laser
speckle is a consequence of spatial coherence. Temporal coherence
indicates that the radiation is strictly monochromatic (of one
wavelength). No light source is either totally coherent or totally
incoherent; the differences between individual lasers and, for that
matter, non-laser sources are merely a matter of degree. The term
"coherence length" is used to describe the degree of spatial
coherence.
5. RADIOMETRIC CONCEPTS
5.1. Radiometric and Photometric Terminology
Two systems of quantities and units are used to describe
optical radiation. One is a physical system called the radiometric
system. The other, the photometric system, attempts to describe
the optical radiation in terms of its ability to elicit the
sensation of light by the eye. Table 5 gives the most commonly
used quantities and the preferred units for each system. There are
generally analogous units in each of the 2 systems. The table is
arranged to illustrate these similarities. Though the radiometric
system of units may be used across the entire spectrum, the
photometric system is limited to describe light (i.e.,
electromagnetic radiation that is visible) from approximately
380 - 400 nm to 760 - 780 nm.
It is important to remember that some terms refer only to
extended sources (e.g., radiance) and other terms (e.g., radiant
intensity) refer only to "point" sources.
5.2. Extended Sources Versus Point Sources
Lasers are often treated as "point" sources, whereas most
conventional light sources are considered to be extended sources,
at least at close distances. An extended source is one that
appears to have some angular extent as seen by the viewer. The
moon is an extended source; a star is a "point" source. Apart from
lasers, a light source can be considered a point source only at a
great distance, or if a pinhole diaphragm is placed in front of the
light source. All other light sources are considered to be
extended sources.
5.3. Inverse Square Law
The inverse square law for calculating the irradiance or
radiant exposure at a distance from a source applies only to a
point source. For example, the ratio of irradiance E1, at one
distance r1 to E2 at another distance r2 is:
El = r22 Equation (10)
E2 r12
For practical purposes, extended sources can be considered as
"point" sources at a distance many times greater than the source
dimension. Both r1 and r2 should be at least as great as 10 source
diameters for a diffuse lambertian source. This also applies to
equation 3. The irradiance E at a distance r from a point source
is:
E = I/r2 Equation (11)
This equation applies to collimated extended sources (e.g.,
searchlights) or lasers, only at considerable distances from the
source.
Table 5. Useful CIE radiometric and photometric quantitities and unitsa,b
-------------------------------------------------------------------------------------
RADIOMETRIC
-------------------------------------------------------------------------------------
Term Symbol Defining equation Quantity SI units &
applicablec abbreviations
-------------------------------------------------------------------------------------
Radiant energy Qe S, R joule (J)
-------------------------------------------------------------------------------------
Radiant energy dQe F joule per cubic
density We We = dV metre (J/m3)
-------------------------------------------------------------------------------------
Radiant power dQe S, R watt (W)
(radiant flux) phieP phie = dt
-------------------------------------------------------------------------------------
Radiant d phie S watt per square
exitance Me Me = dA metre (W/m2)
= /Le x cos x d omega
-------------------------------------------------------------------------------------
Irradiance or d phie R watt per square
flux density Ee Ee = dA metre (W/m2)
(dose rate in
photobiology)
-------------------------------------------------------------------------------------
Radiant d phie S watt per
intensity Ie Ie = d omega steradian
(W/sr1)
-------------------------------------------------------------------------------------
Radiance d d2phie S, F, R watt per
------------------------ steradian and
Le 1e = d omega x dA x cos theta per square metre
(W/sr/m2)
--------------------------------------------------------------------------------------
Radiant dQe R joule per square
exposure He He = dA metre (J/m2)
(dose in
photobiology)
--------------------------------------------------------------------------------------
Radiant P S unitless
efficiencye etae etae = Pi
(of a source)
--------------------------------------------------------------------------------------
Optical De De = -log10taue R unitless
--------------------------------------------------------------------------------------
Table 5. (contd.)
------------------------------------------------------------------------------------
PHOTOMETRIC
------------------------------------------------------------------------------------
Term Symbol Defining equation SI abbreviations
& units
------------------------------------------------------------------------------------
Quantity of Qnu Qnu = /phinudt lumen-second
light (lm x s)
------------------------------------------------------------------------------------
Luminous dQnu lumen-second per
energy density Wnu Wnu = dV cubic metre
(lm x s/m3)
------------------------------------------------------------------------------------
Luminous flux phinu d phie lumen (lm)
-----------------------
phinu = 680 / d lamdaV(lamda)d lamda
------------------------------------------------------------------------------------
Luminous d phinu lumen per square
exitance Mnu Mnu = dA metre (lm/m2)
= /Inu x cos phi x d omega
------------------------------------------------------------------------------------
Illuminance d phinu lumen per square
(luminous Enu Enu = dA metre (lm/m2)
density)
------------------------------------------------------------------------------------
Luminous d phinu lumen per
intensity Inu Inu = dr steradian (lm x sr)
(candlepower) or candela (cd)
------------------------------------------------------------------------------------
Luminance d Lnu d2phie candela per square
------------------- metre (cd/m2)
Lnu = dr x dA x cos theta
------------------------------------------------------------------------------------
Light exposure dQnu lux-second
Hnu Hnu = dA (lx x s)
= /Enudt
------------------------------------------------------------------------------------
Luminous phinu lumen per watt
efficacy (of K K = phie (lm/W)
radiation)
------------------------------------------------------------------------------------
Luminous K K unitless
efficiency V(*) V(*) = / Km = 680
(of a broad
band radiation)
------------------------------------------------------------------------------------
Luminous phinu lumen per watt
efficacye etanu etanu = Pi (lm/W)
------------------------------------------------------------------------------------
Table 5. (contd.)
------------------------------------------------------------------------------------
PHOTOMETRIC
------------------------------------------------------------------------------------
Term Symbol Defining equation SI abbreviations
& units
------------------------------------------------------------------------------------
Optical unitless
densityf Dnu Dnu = -log10taunu
------------------------------------------------------------------------------------
Retinal Troland (td) =
illuminance Et Et = Lnu x Sp luminance of 1 cd/
(in trolands) m2 times pupil
area in mm2
------------------------------------------------------------------------------------
a The quantities may be altered to refer to narrow spectral bands, in which case
the term is preceded by the word spectral, and the unit is then per unit of
wavelength and the symbol has a subscript lambda. For example, spectral
irradiance Hlambda has units of W/(m2 x m) or more often, W/(cm2 x nm).
b While the metre is the preferred unit of length, the centimetre is still the
most commonly used unit of length for many of the above terms and the nm or µm
are most commonly used to express wavelength.
c Some radiometric quantities refer only to the source, field, or receiver. This
noted in this column.
d At the source, dM ; at a receptor, dE
L = d omega x cos theta L = d omega x cos theta
e Pi is electrical input power in watts.
f tau is the transmission; Dnu is also abbreviated as O.D.
6. RADIOMETRIC AND PHOTOMETRIC MEASUREMENT
6.1. Introduction
Reliable radiometric techniques and instruments are available
that make it possible to analyse risks for the skin and eye from
exposure to lasers and other sources of optical radiation.
However, the cost of accurate equipment remains relatively high
compared with that of survey equipment now available to evaluate
many other environmental risks. Radiometric formulae and
manufacturers' specifications of lasers will often be an adequate
substitute for measurement.
There are many types of measurements for defining conditions or
characterizing a source's output. The types of measurements
considered in this section fall under the broad term of
"radiometric". For characterizing a conventional light source,
radiance is generally the most useful. For laser output
measurements, radiant power and radiant energy are by far the most
important. Irradiance and radiant exposure are of greater
importance in defining hazardous exposure conditions from all
optical sources.
In any discussion of the measurement of laser radiation for
purposes of evaluating health risks, it is important first to
clarify the conditions and requirements for such measurements.
Industrial and environmental health specialists and health
physicists usually rely heavily on instruments to detect or
estimate a chemical or physical agent that their own human senses
cannot detect. The presence of a laser beam can generally be
detected by the human eye or through the use of an image converter,
thus raising the question "Why should the laser beam be measured?".
It soon becomes evident that, in most cases, even routine
monitoring of either a work area or an individual by
instrumentation is a hopeless task. A more logical approach to
risk assessment is to develop a means of analysing the potential
risk of a laser, based on the laser's output parameters.
As a general rule, present standards require only measurement
of the laser-output characteristics for laser risk classification.
Routine monitoring is seldom considered necessary and all
measurements are normally performed only once, by (or for) the
manufacturer of the laser equipment. Periodic measurements may be
considered worthwhile for certain lasers that are near the
borderline between two classes in the hazard classification and
field measurements of outdoor laser propagation paths have often
been found useful. Unlike most noxious agents, a high-powered
laser beam is almost always hazardous for a considerable distance
and its hazard generally exceeds exposure limits by orders of
magnitude. Diagnostics of the beam profile and measurement of beam
divergence have been discussed.
The evaluation of more conventional broad-band sources is more
complex, since spectral characteristics and source size must be
considered. To evaluate a broad-band optical source, it is
normally necessary to determine the spectral distribution of
optical radiation emitted from the source at the point or points of
human access. The spectral distribution of the accessible
emission, which is of interest for a lighting system, may differ
from that actually being emitted by the lamp alone because of
apertures or filtration by any optical elements in the light path.
Secondly, the size, or projected size, of the source must be
characterized in the retinal hazard spectral region. Thirdly, it
may be necessary to determine the variation of irradiance and
radiance with distance. The necessary measurements are normally
complex. The spectrum of an arc lamp, a gas discharge lamp, or a
fluorescent lamp consists of both line structure and a continuum.
Significant errors can be introduced in the representation of the
spectrum and in the weighting of the spectrum against a biological-
or a safety-action spectrum, if the fraction of energy in each line
is not properly added to the continuum.
6.2. Measurement Instrumentation
The radiometric instruments of interest in this discussion
generally consist of detectors that produce a voltage, a current, a
resistance change, or an electronic charge, one of which is
measured by a sensitive electronic meter. The type of read-out
meter for the radiometric instrument is not normally of great
concern and seldom determines the selection of the instrument.
There are both advantages and disadvantages associated with each
type of detector and each has certain characteristics that may be
useful for measuring a specific level of optical radiation in a
wavelength range of interest. No single detector is best for
measuring all wavelengths and radiant powers of optical radiation.
A very sensitive detector can be readily damaged or its response
distorted by a high-powered laser beam, whereas a detector designed
to measure very high-powered laser radiation is normally
insensitive to low-power radiation. Narrow-band detectors have the
advantage of being insensitive to extraneous radiation, though
their usefulness is limited to measurement of lasers operating in
that particular spectral band.
In many countries, national physical standards laboratories
exist, which offer calibration services for some radiometric
instruments. Examples are: Laboratoire National d'Essais (France);
National Physical Laboratory (United Kingdom); Assistance Committee
for Measures and Standards (USSR); National Bureau of Standards
(USA); and Physikalisch-Technische Bundesanstalt (Federal Republic
of Germany).
6.2.1. Thermal detectors
Thermal detectors are mainly used for measuring the output
power or energy of lasers and total irradiances from broad-band
optical sources, in particular infrared sources. Some of these
detectors are particularly useful for absolute measurements.
Thermopiles, bolometers, disc calorimeters, and pyroelectric
detectors are characterized by a relatively flat response as a
function of wavelength. The spectral response of these detectors
is dictated by the "black" absorbers that are normally used to coat
the detector's metal or crystalline substrate. As optical energy
falls on the detector, the temperature increases. The temperature
rise in the substrate is then converted into an electrical voltage
or current. Because of the thermal mass of the metal, the time
required to heat or cool the detector element limits the response
time of the instrument. The absorber in a disc calorimeter may be
a black painted disc or a glass volume absorber (James, ed. 1976).
In recent years, the response time of thermopiles has been
shortened by using thin-film techniques. Low powers (typically
0.01 - 100 mW) can be measured and the response time reduced.
Pyroelectric detectors measure the rate of temperature change in a
crystalline material rather than the final temperature elevation in
a metal. Radiometric calorimeters can be used to measure cw
radiation over the power range from 1 mW to over 1 kW, depending on
the detector and wavelength. Pulsed radiant energy can be measured
over the range from 10 mJ to 10 kJ.
The detector may be covered by a window, which limits spectral
response. Quartz windows are necessary for UVR, but there is
probably no window material that is universally flat from 200 to
20 000 nm.
6.2.2. Quantum detectors
Quantum detectors operate normally at room temperature and
offer by far the most sensitive means of measuring optical
radiation, therefore, their principle use is in spectroradiometers
and detectors required for the measurement of lower powers and
irradiances or for temporal resolution of pulses. The spectral
sensitivity of photoemissive detectors depends on the photocathode
material used in vacuum photodiodes or photomultiplier tubes, or
in the characteristics of (doped) silicon. All detectors that
operate by means of the photoelectric effect have a characteristic
cutoff wavelength. At wavelengths greater than this cutoff,
photons are largely ineffective in producing photoelectrons and the
resulting photocurrent.
Because of the strong spectral dependence of the photodiode,
these instruments are often not direct reading and the meter
reading may have to be multiplied by one of several calibration
factors.
Simple silicon-detector instruments can be quite useful, when
the natural spectral response of silicon (approx 200 - 1100 nm) is
changed by an appropriate input filter to yield a flat spectral
response from 450 to 950 nm (Marshall, 1980).
6.2.3. Detectors to resolve short pulses
A variety of techniques have been developed to resolve the
temporal behaviour of short laser pulses. An ultrafast
oscilloscope with a solid-state silicon detector or biplanar vacuum
photodiode is most often used to display the pulse shape of a
Q-switched (1.0 - 100 ns) pulse. For temporal domains of less than
1 ns, streak cameras and some non-linear optical techniques are
used to resolve the structure of a train of mode-locked laser
pulses.
The techniques used in photometry and radiometry are far too
numerous and complex to detail here (see for example: Grum &
Becherer, ed. 1979; Le Bodo, 1976; or Sliney & Wolbarsht, 1980).
Differences in measured values for the same source from each of two
different laboratories may arise through a problem of "geometry" or
incorrect allowance for extraneous light.
6.2.4. Safety meters
At present, inexpensive, portable radiometric measuring
instruments that have been designed specifically for the risk
analysis of a great variety of lasers, are not available. Indeed,
it is unlikely that such instruments will be made in the future,
because of the great variation in exposure criteria for different
wavelengths and different exposure durations. The same holds true
for non-laser optical source survey instruments. However, some
relatively expensive, microprocessor-based instruments have been
developed to cover a wide range of measurements. Simple
instruments are possible for the purpose of measuring one type of
laser or optical source.
Because of the great interest in photometry, there are many
satisfactory photometers that measure both luminance and
illuminance and follow the CIE photopic function Vlambda quite
well. This is not always the case for the other weighting
functions. Direct reading UVR instruments are a case in point.
The principal difficulty in developing a suitable UVR instrument is
the rejection of unwanted wavelengths. It is difficult to measure
only the UV-B and UV-C radiation with sufficient sensitivity, while
still rejecting all of the UV-A and visible light.
6.2.5. Spectroradiometers
As well as broad-band measurements, it is often necessary to
measure the spectrum of a conventional source. A grating or prism
monochromator is used to resolve the spectrum.
An important part of measuring the spectral distribution of a
broad-band lamp source or an arc process is the specification of
the desired bandwidth, and the intervals at which data will be
recorded. One of the most useful approaches is to scan through a
spectrum and record the detector output in analogue fashion on an
X-Y recorder, rather than to record digitized data.
An X-Y recorder can indicate the bandwidth of the monochromator
and may quite often indicate the regions of the spectrum in which
problems may arise from stray light or extraneous signals.
The required bandwidth and sampling interval are determined by
comparing the so-called "slit function" of the monochromator system
with the need for sufficient spectral resolution to make possible
accurate weighting against action spectra used in risk analysis.
Two common difficulties are encountered in obtaining an
accurate radiometric description of a broad-band, extended source.
The first problem is to achieve adequate rejection of unwanted
wavelengths from the passband of the monochromator (e.g., rejecting
"stray light"). The second is the proper definition of the actual
or effective source size of an arc or a discharge lamp. Several
other special problem areas (such as background isolation,
wavelength calibration, and the proper separation of line and
continuous values) are also encountered in specific situations.
6.3. Biological Weighting of Spectroradiometric Data
Many of the calculations that are useful in risk analyses
require weighting of the measured spectrum against a biological
action spectrum. There are several, including the erythemal and
the photokeratitic action spectra, the photopic response V lambda
of the eye, and the retinal photochemical injury action spectrum B
lambda (Ham, et al., 1976; ACGIH, 1981; Sliney & Wolbarsht, 1980)
(Fig. 9).
 7. BIOLOGICAL EFFECTS
For biological effects to take place, some of the incident
radiation must be absorbed. This is known as Draper's Law (Smith,
1977).
The primary effects can be related to two general mechanisms,
thermal and photochemical injury. In some special instances (as
with ps pulses), non-linear effects related to the direct electric
field of photons may be important. The observable biological
effects are the result of secondary events. Under certain
circumstances, these effects can be changed in size and direction.
A number of these modifying factors are treated in the text such as
pigmentation, increased body temperature, and photosensitizing
substances.
7.1. Thermal Injury
Thermal injury mechanisms all require that sufficient radiant
energy is absorbed in a tissue, sufficiently fast, to create a
substantial increase above normal tissue temperature (typically
10 - 25 °C for short periods of a min or less). There is no
dependence on photon energy, though energy must be absorbed. Heat
conduction away from an irradiated area is of great importance.
Thus, the presence of blood vessels and the size of the irradiated
volume, as well as spectral absorption, influence the threshold of
injury (Marshall, 1970).
For every short exposure, changes of state may occur so rapidly
that micro-explosions (Hanson & Fine, 1968) or thermo-mechanical
effects may become important (Vos, 1966a; Ham et al., 1970).
7.2. Photochemical Injury
Significant adverse effects have now been shown to result
initially from a photochemical reaction rather than through a
thermal damage mechanism. A photochemical reaction takes place
when single photons have sufficient quantum energy to convert
individual molecules to one or more different chemical molecules.
A photochemical injury mechanism is demonstrated, when a
reciprocity relation between irradiance (dose-rate) and exposure
duration exists. That is, a constant radiant exposure (dose) is
required to elicit the response over a wide variation of exposure
durations, up to durations at which biological repair comes into
play. An additional characteristic of any photochemical reaction
is a rather steep drop-off of the action spectrum in the long
wavelength end. The yield of the photochemical reaction products
is propotional to the photon flux and each photon must have the
amount of energy required for the reaction. At the long-wavelength
end of the induced response (action spectrum), the energy of a
single photon coupled with available thermal energy is generally
insufficient to induce an effect.
Most photochemical effects of radiation are still not
understood in detail. The relative spectral effectiveness of
radiation in eliciting any particular biological effect is referred
to by photobiologists as an "action spectrum". The steep slopes of
many ultraviolet action spectra demonstrate the importance of not
routinely extrapolating biological data concerning injury occurring
at one wavelength to another wavelength, and of not assuming that
any smooth curve does not have fine structures.
There are some instances where both photochemical and thermal
effects contribute to the final biological effect. In general,
they will enhance one another.
7.3. Threshold of Injury
All thermal injury has a macroscopically apparent threshold.
Individual photons in the long-wavelength range do not have
sufficient energy, normally, to cause more than temporary
biological change at the molecular level. Acute pathological
changes can only be demonstrated, when a sufficient thermal photon
flux exists to cause temperature rises so rapid that normal heat
dissipation and molecular repair are overwhelmed. In the case of
photochemical injury, individual photons may alter or damage an
individual molecule. However, it has been shown that many critical
biomolecules have repair mechanisms to correct such damage (Smith,
1978). For very high photon flux densities the repair processes
may be overwhelmed and macroscopic damage will be apparent.
Occupational exposure limits can thus be set for any type of
radiation in which the reciprocal relation of progressively lower
power levels and longer exposure duration seems to show a marked
deviation from linearity (non-reciprocity). At this irradiance
level, any increases in the exposure duration may not be followed
by pathological changes in the exposed tissues. This would not be
accepted as a true threshold of injury by some investigators, since
it could always be argued that a repair mechanism could fail.
Thus, it must be admitted that there may be some finite, albeit
extremely slight, risk of injury or delayed effects in a small
population (Sliney & Wolbarsht, 1980).
7.3.1. Means of determining thresholds of injury
There are several different criteria that have been used in
studying potential injury in tissue (Beatrice & Velez, 1978).
Examples are:
(a) direct observation of irradiated tissue at low
magnification
(i) without special techniques
(ii) with special visualization techniques such as
fundoscopy or fluorescein angiography (eye)
(Borland et al., 1978);
(b) histology
(i) light microscopy
(ii) electron microscopy (EM)
(iii) histochemical studies;
(c) biochemical studies;
(d) electrophysiological tests (e.g., the eye) (Court et al.,
1978);
(e) functional studies;
(f) epidemiological studies (i.e., skin cancer).
In setting exposure limits, all of these studies must be taken
into account. In studies of skin reaction to optical radiation,
the first criteria of direct observation of erythema mainly has
been used, though histological and histochemical techniques have
been used in a few studies. The threshold criteria just listed
will be discussed briefly, as they apply to studies of injury from
optical radiation.
8. EFFECTS OF OPTICAL RADIATION ON THE EYE
The attendant hazards of optical radiation vary greatly
depending on the type of the source and its application. Generally,
the effects of laser radiation are not different from the effects
of optical radiation from a conventional source with the same
wavelength, exposure duration, and given irradiance.
The effects of optical radiation on the eye vary significantly
with wavelength. For this reason, the subject will be discussed in
three sections. First, the effects of UVR, which are generally
photochemical, on the lens and cornea will be considered. The main
discussion will relate to the retinal hazard region (the visible
and IR-A) where the eye is particularly vulnerable to injury,
because of its imaging characteristics. Finally, IR effects on the
anterior structures of the eye will be discussed.
There are many end points that can be used in establishing
injury. Damage to the retina of the eye from visible radiation can
appear as an altered light reflex or a white patch on the retina,
visible during ophthalmoscopic examination. This criterion has
been used in most injury studies. The end point could also be any
histologically-defined injury seen with the light microscope; or,
it could be consistently observed ultrastructural changes only
visible with an electron microscope (transmission or scanning EM).
Histochemical techniques can also serve to document an end point
for injury. There is also the detection of functional alterations
in sensory (behavioural) responses of task-oriented animal
subjects, e.g., visual acuity, colour vision, dark adaptation.
Often, these functional changes can also be detected by
electrophysiological recordings of altered neural function within
the visual system. A problem arises, when different investigators
define the "threshold" for any one of these end points in different
ways. The most meaningful thresholds for health criteria are those
related to a persistent functional decrement.
8.1. Anatomy and Physiology of the Human Eye
In the human eye, light passes through the various ocular
structures (Fig. 10) to fall on the retina, where it triggers a
photochemical process that evokes the neural impulses that lead to
vision. The light first passes through the structures in the
anterior portion of the eye - the cornea, the aqueous humor in the
anterior chamber, the pupil (and sometimes the iris), the somewhat
pliable crystalline lens, then into the posterior part, the
vitreous humor and the numerous layers of the retina. Only the
three structures of the eye that are critical in relation to the
subject of optical radiation hazards will be discussed, i.e., the
cornea, the lens, and the retina.
8.1.1. The cornea
The cornea and the conjuctiva of the eye are exposed directly
to the environmental elements. These structures are protected from
drying by the tear film, which is 6 - 10 µ in thickness.
7. BIOLOGICAL EFFECTS
For biological effects to take place, some of the incident
radiation must be absorbed. This is known as Draper's Law (Smith,
1977).
The primary effects can be related to two general mechanisms,
thermal and photochemical injury. In some special instances (as
with ps pulses), non-linear effects related to the direct electric
field of photons may be important. The observable biological
effects are the result of secondary events. Under certain
circumstances, these effects can be changed in size and direction.
A number of these modifying factors are treated in the text such as
pigmentation, increased body temperature, and photosensitizing
substances.
7.1. Thermal Injury
Thermal injury mechanisms all require that sufficient radiant
energy is absorbed in a tissue, sufficiently fast, to create a
substantial increase above normal tissue temperature (typically
10 - 25 °C for short periods of a min or less). There is no
dependence on photon energy, though energy must be absorbed. Heat
conduction away from an irradiated area is of great importance.
Thus, the presence of blood vessels and the size of the irradiated
volume, as well as spectral absorption, influence the threshold of
injury (Marshall, 1970).
For every short exposure, changes of state may occur so rapidly
that micro-explosions (Hanson & Fine, 1968) or thermo-mechanical
effects may become important (Vos, 1966a; Ham et al., 1970).
7.2. Photochemical Injury
Significant adverse effects have now been shown to result
initially from a photochemical reaction rather than through a
thermal damage mechanism. A photochemical reaction takes place
when single photons have sufficient quantum energy to convert
individual molecules to one or more different chemical molecules.
A photochemical injury mechanism is demonstrated, when a
reciprocity relation between irradiance (dose-rate) and exposure
duration exists. That is, a constant radiant exposure (dose) is
required to elicit the response over a wide variation of exposure
durations, up to durations at which biological repair comes into
play. An additional characteristic of any photochemical reaction
is a rather steep drop-off of the action spectrum in the long
wavelength end. The yield of the photochemical reaction products
is propotional to the photon flux and each photon must have the
amount of energy required for the reaction. At the long-wavelength
end of the induced response (action spectrum), the energy of a
single photon coupled with available thermal energy is generally
insufficient to induce an effect.
Most photochemical effects of radiation are still not
understood in detail. The relative spectral effectiveness of
radiation in eliciting any particular biological effect is referred
to by photobiologists as an "action spectrum". The steep slopes of
many ultraviolet action spectra demonstrate the importance of not
routinely extrapolating biological data concerning injury occurring
at one wavelength to another wavelength, and of not assuming that
any smooth curve does not have fine structures.
There are some instances where both photochemical and thermal
effects contribute to the final biological effect. In general,
they will enhance one another.
7.3. Threshold of Injury
All thermal injury has a macroscopically apparent threshold.
Individual photons in the long-wavelength range do not have
sufficient energy, normally, to cause more than temporary
biological change at the molecular level. Acute pathological
changes can only be demonstrated, when a sufficient thermal photon
flux exists to cause temperature rises so rapid that normal heat
dissipation and molecular repair are overwhelmed. In the case of
photochemical injury, individual photons may alter or damage an
individual molecule. However, it has been shown that many critical
biomolecules have repair mechanisms to correct such damage (Smith,
1978). For very high photon flux densities the repair processes
may be overwhelmed and macroscopic damage will be apparent.
Occupational exposure limits can thus be set for any type of
radiation in which the reciprocal relation of progressively lower
power levels and longer exposure duration seems to show a marked
deviation from linearity (non-reciprocity). At this irradiance
level, any increases in the exposure duration may not be followed
by pathological changes in the exposed tissues. This would not be
accepted as a true threshold of injury by some investigators, since
it could always be argued that a repair mechanism could fail.
Thus, it must be admitted that there may be some finite, albeit
extremely slight, risk of injury or delayed effects in a small
population (Sliney & Wolbarsht, 1980).
7.3.1. Means of determining thresholds of injury
There are several different criteria that have been used in
studying potential injury in tissue (Beatrice & Velez, 1978).
Examples are:
(a) direct observation of irradiated tissue at low
magnification
(i) without special techniques
(ii) with special visualization techniques such as
fundoscopy or fluorescein angiography (eye)
(Borland et al., 1978);
(b) histology
(i) light microscopy
(ii) electron microscopy (EM)
(iii) histochemical studies;
(c) biochemical studies;
(d) electrophysiological tests (e.g., the eye) (Court et al.,
1978);
(e) functional studies;
(f) epidemiological studies (i.e., skin cancer).
In setting exposure limits, all of these studies must be taken
into account. In studies of skin reaction to optical radiation,
the first criteria of direct observation of erythema mainly has
been used, though histological and histochemical techniques have
been used in a few studies. The threshold criteria just listed
will be discussed briefly, as they apply to studies of injury from
optical radiation.
8. EFFECTS OF OPTICAL RADIATION ON THE EYE
The attendant hazards of optical radiation vary greatly
depending on the type of the source and its application. Generally,
the effects of laser radiation are not different from the effects
of optical radiation from a conventional source with the same
wavelength, exposure duration, and given irradiance.
The effects of optical radiation on the eye vary significantly
with wavelength. For this reason, the subject will be discussed in
three sections. First, the effects of UVR, which are generally
photochemical, on the lens and cornea will be considered. The main
discussion will relate to the retinal hazard region (the visible
and IR-A) where the eye is particularly vulnerable to injury,
because of its imaging characteristics. Finally, IR effects on the
anterior structures of the eye will be discussed.
There are many end points that can be used in establishing
injury. Damage to the retina of the eye from visible radiation can
appear as an altered light reflex or a white patch on the retina,
visible during ophthalmoscopic examination. This criterion has
been used in most injury studies. The end point could also be any
histologically-defined injury seen with the light microscope; or,
it could be consistently observed ultrastructural changes only
visible with an electron microscope (transmission or scanning EM).
Histochemical techniques can also serve to document an end point
for injury. There is also the detection of functional alterations
in sensory (behavioural) responses of task-oriented animal
subjects, e.g., visual acuity, colour vision, dark adaptation.
Often, these functional changes can also be detected by
electrophysiological recordings of altered neural function within
the visual system. A problem arises, when different investigators
define the "threshold" for any one of these end points in different
ways. The most meaningful thresholds for health criteria are those
related to a persistent functional decrement.
8.1. Anatomy and Physiology of the Human Eye
In the human eye, light passes through the various ocular
structures (Fig. 10) to fall on the retina, where it triggers a
photochemical process that evokes the neural impulses that lead to
vision. The light first passes through the structures in the
anterior portion of the eye - the cornea, the aqueous humor in the
anterior chamber, the pupil (and sometimes the iris), the somewhat
pliable crystalline lens, then into the posterior part, the
vitreous humor and the numerous layers of the retina. Only the
three structures of the eye that are critical in relation to the
subject of optical radiation hazards will be discussed, i.e., the
cornea, the lens, and the retina.
8.1.1. The cornea
The cornea and the conjuctiva of the eye are exposed directly
to the environmental elements. These structures are protected from
drying by the tear film, which is 6 - 10 µ in thickness.
 The cornea and conjuctiva are tissues rich in sensory receptors
and nerve endings serving as triggers of protective reflexes for
mechanical and thermal agents.
As the epithelial cells must survive a harsh environment, they
have a very short life span of approximately 2 - 5 days. If the
cell death rate increases (as in photokerititis) and replacement is
not in step with the loss, small erosions will develop that elicit
a pain sensation.
The corneal stroma is built in a very regular fashion, which
accounts for its transparency. If this regularity is distorted,
i.e., by an oedema, the cornea will be less transparent or even
opaque. A disturbance of the epithelium, or, more important still,
of the inner cell layer of the cornea (the endothelium) will result
in an oedema. Any scar formation will also alter the regular
construction and hence will result in an opaque cornea. Thus
serious visual handicap will be the result of irreversible corneal
damage.
8.1.2. The lens
The lens is a tissue built up from cells that progressively
deform to produce the lens fibres. These are arranged in an onion-
like way and are covered with an elastic capsule. The capsule is
attached through fine ligaments to the cilary muscle which alters
the shape of the lens.
As new cells are formed, older cells become fibres and are
progressively displaced towards the centre of the lens. The more
superficial fibres form the cortex while the central fibres
constitute the nucleus.
The lens fibres are transparent, ribbon-like cells, each of
which runs completely around from the front of the lens to the
back. Injury to any single fibre will, in time, extend throughout
the entire fibre cell and will be more apparent in the thicker
posterior part of the lens (posterior subcapsular cataract).
The lens, like the cornea, is not optically homogeneous but it
is transparent in the visible range of the spectrum. However,
increasing absorption of short-wavelength light occurs with age
(Wolbarsht et al., 1977). The transparancy is the result of a
precise relation of the various minute, optically well ordered,
constituents. A disturbance of the cell elements or the fibre will
result in the hydration of the fibre. Damage to the lens disturbs
this relation resulting in increased light scattering. The lens
becomes milky (a cataract).
8.1.3. The retina and choroid
The retina is divided into two major components - a pigmented
monolayer - the retinal pigmented epithelium (RPE) and a
multilayered lamina of neural cells called the neural retina. The
light-sensitive cells are adjacent to the RPE. There are two types
of photoreceptor cells: rods and cones, named according to the
shape of the distal (away from the synaptic end) extension of the
photoreceptor cells. Light entering the eye must first pass
through all of the neural retina before striking the receptor
cells. In the retina, there are probably 120 million rods
approximately 60 µm long and 2 µm in diameter and 6 million cones
approximately 50 µm long and 3 - 5 µm in diameter. These receptor
cells are interconnected by other specialized cells. Rods are
mainly concerned with vision at low light levels and are
predominant in the periphery of the retina. Cones are responsible
for colour vision and high acuity visual tasks. They are most
concentrated in a specialized central region of the retina, the
fovea. The fovea is responsible for central vision used for
reading. The anatomical aspects of the retinal pigment epithelium
(RPE) and adjacent layers are of particular importance in a study
of retinal injury from light sources. The outer segments of the
rods and cones (the light-sensitive section of the cell) are
immediately anterior to the RPE.
There are very small protrusions (microvilli) of the RPE that
extend upward around the outer segments (Fig. 11). As the cones do
not extend as near to the RPE as the rods, the microvilli extend
out further to the cone outer segments. It is known that the RPE
plays a critical role in the retinal metabolism and photochemistry,
hence proper functioning of the REP is essential for normal vision.
The outer segments of both rods and cones contain a stack of coin-
like membranes on which their visual pigments are oriented. These
discs are in a continuous state of flux. In rods, 10 - 30 new
discs are made each day, while a similar number are phagocytized by
the RPE cells (Fig. 11); the rate of shedding is greatest in the
early morning. The life span of a disc is two weeks. The cone
lamellar membranes do not form complete discs and do not appear to
shed in the same manner as in the rods. The renewal activity of
the cones is slower than that of the rods and it occurs at night.
Bruch's membrane separates the RPE from the blood supply in the
capillary layer of the choriocapillaries which is the innermost
layer of the choroid, and is where the smallest vessels are found.
The choroid is an extremely vascular spongy tissue with many
pigmented cells scattered throughout it. The thickness is
variable; the average is about 250 µm. The blood vessels
progressively increase in size towards the scleral surface. It has
been suggested by Ernest & Potts (1971) that the primary function
of the blood in the choroid is to keep the eye warm and at a
uniform temperature. Because of this extreme vascularity, heat
from laser exposures introduced in this region under steady-state
conditions will do little to elevate the temperature unless high
power levels are used.
The cornea and conjuctiva are tissues rich in sensory receptors
and nerve endings serving as triggers of protective reflexes for
mechanical and thermal agents.
As the epithelial cells must survive a harsh environment, they
have a very short life span of approximately 2 - 5 days. If the
cell death rate increases (as in photokerititis) and replacement is
not in step with the loss, small erosions will develop that elicit
a pain sensation.
The corneal stroma is built in a very regular fashion, which
accounts for its transparency. If this regularity is distorted,
i.e., by an oedema, the cornea will be less transparent or even
opaque. A disturbance of the epithelium, or, more important still,
of the inner cell layer of the cornea (the endothelium) will result
in an oedema. Any scar formation will also alter the regular
construction and hence will result in an opaque cornea. Thus
serious visual handicap will be the result of irreversible corneal
damage.
8.1.2. The lens
The lens is a tissue built up from cells that progressively
deform to produce the lens fibres. These are arranged in an onion-
like way and are covered with an elastic capsule. The capsule is
attached through fine ligaments to the cilary muscle which alters
the shape of the lens.
As new cells are formed, older cells become fibres and are
progressively displaced towards the centre of the lens. The more
superficial fibres form the cortex while the central fibres
constitute the nucleus.
The lens fibres are transparent, ribbon-like cells, each of
which runs completely around from the front of the lens to the
back. Injury to any single fibre will, in time, extend throughout
the entire fibre cell and will be more apparent in the thicker
posterior part of the lens (posterior subcapsular cataract).
The lens, like the cornea, is not optically homogeneous but it
is transparent in the visible range of the spectrum. However,
increasing absorption of short-wavelength light occurs with age
(Wolbarsht et al., 1977). The transparancy is the result of a
precise relation of the various minute, optically well ordered,
constituents. A disturbance of the cell elements or the fibre will
result in the hydration of the fibre. Damage to the lens disturbs
this relation resulting in increased light scattering. The lens
becomes milky (a cataract).
8.1.3. The retina and choroid
The retina is divided into two major components - a pigmented
monolayer - the retinal pigmented epithelium (RPE) and a
multilayered lamina of neural cells called the neural retina. The
light-sensitive cells are adjacent to the RPE. There are two types
of photoreceptor cells: rods and cones, named according to the
shape of the distal (away from the synaptic end) extension of the
photoreceptor cells. Light entering the eye must first pass
through all of the neural retina before striking the receptor
cells. In the retina, there are probably 120 million rods
approximately 60 µm long and 2 µm in diameter and 6 million cones
approximately 50 µm long and 3 - 5 µm in diameter. These receptor
cells are interconnected by other specialized cells. Rods are
mainly concerned with vision at low light levels and are
predominant in the periphery of the retina. Cones are responsible
for colour vision and high acuity visual tasks. They are most
concentrated in a specialized central region of the retina, the
fovea. The fovea is responsible for central vision used for
reading. The anatomical aspects of the retinal pigment epithelium
(RPE) and adjacent layers are of particular importance in a study
of retinal injury from light sources. The outer segments of the
rods and cones (the light-sensitive section of the cell) are
immediately anterior to the RPE.
There are very small protrusions (microvilli) of the RPE that
extend upward around the outer segments (Fig. 11). As the cones do
not extend as near to the RPE as the rods, the microvilli extend
out further to the cone outer segments. It is known that the RPE
plays a critical role in the retinal metabolism and photochemistry,
hence proper functioning of the REP is essential for normal vision.
The outer segments of both rods and cones contain a stack of coin-
like membranes on which their visual pigments are oriented. These
discs are in a continuous state of flux. In rods, 10 - 30 new
discs are made each day, while a similar number are phagocytized by
the RPE cells (Fig. 11); the rate of shedding is greatest in the
early morning. The life span of a disc is two weeks. The cone
lamellar membranes do not form complete discs and do not appear to
shed in the same manner as in the rods. The renewal activity of
the cones is slower than that of the rods and it occurs at night.
Bruch's membrane separates the RPE from the blood supply in the
capillary layer of the choriocapillaries which is the innermost
layer of the choroid, and is where the smallest vessels are found.
The choroid is an extremely vascular spongy tissue with many
pigmented cells scattered throughout it. The thickness is
variable; the average is about 250 µm. The blood vessels
progressively increase in size towards the scleral surface. It has
been suggested by Ernest & Potts (1971) that the primary function
of the blood in the choroid is to keep the eye warm and at a
uniform temperature. Because of this extreme vascularity, heat
from laser exposures introduced in this region under steady-state
conditions will do little to elevate the temperature unless high
power levels are used.
 8.2. Spectral Properties of the Eye
To understand the biological effects of different optical
spectral bands on different ocular structures, it is first
necessary to consider the relative spectral absorption of the
different ocular media. Fig. 12 shows the spectral absorption for
each of the media.
Essentially all incident optical radiation at very short
wavelengths in the ultraviolet and long wavelengths in the infrared
is absorbed in the cornea. Clearly an ocular structure cannot be
damaged unless optical radiation is absorbed. In some instances,
particularly in the UV region, less than 1% of the total incident
radiation absorbed in a structure can be significant, if the
radiation contains critically effective wavelengths.
8.2. Spectral Properties of the Eye
To understand the biological effects of different optical
spectral bands on different ocular structures, it is first
necessary to consider the relative spectral absorption of the
different ocular media. Fig. 12 shows the spectral absorption for
each of the media.
Essentially all incident optical radiation at very short
wavelengths in the ultraviolet and long wavelengths in the infrared
is absorbed in the cornea. Clearly an ocular structure cannot be
damaged unless optical radiation is absorbed. In some instances,
particularly in the UV region, less than 1% of the total incident
radiation absorbed in a structure can be significant, if the
radiation contains critically effective wavelengths.
 8.3. Injury to the Anterior Portion of the Eye
The anterior structures of the eye are the cornea, conjunctiva,
aqueous humor, iris, and lens. The cornea, aqueous humor, and lens
are part of the optical pathway and, as such, must be transparent
to light. Loss of transparency is serious. Because of the rapid
turnover of corneal epithelial cells, damage limited to this outer
layer can be expected to be temporary. Indeed, injury to this
tissue by exposure to UV-B and UV-C, as occurs in a particular
keratoconjuntivitis, the ultraviolet photokeratitis or
photoophthalmia (known also as "arc eye", or "welder's flash"),
seldom lasts more than one or two days. Unless deeper tissues of
the cornea are also affected, surface epithelium injuries are
rarely permanent.
Near-ultraviolet and near-infrared radiation (UV-A, IR-A, and
possibly IR-B) are strongly absorbed in the lens of the eye.
Damage to this structure is of great concern in that the lens has a
very slow turnover of cells. A one-day exposure may result in
effects that will not become evident for many years. This is
probably the case of glass-blower's or steel puddler's cataract and
in cataracts caused by ionizing radiation. Long-term exposure may
also result in delayed effects (Tengroth et al., 1980).
8.3.1. Effects on the cornea
UV-B and UV-C radiation are absorbed in the cornea and
conjunctiva and sufficiently high doses will cause kerato-
conjunctivitis. The initial effect of UVR exposure is damage to,
or destruction of, the epithelial cells. Under normal conditions,
the corneal epithelial layer is completely replaced in a matter of
a day or so. After exposure, there is a latent period, generally
shorter than 12 h, which varies inversely with the exposure dose.
Healing of the corneal and conjuctival epithelium takes 1 - 2 days.
In severe exposures, damage to Bowman's membrane and the stroma may
occur and is commonly followed by scar formation (usually of a
milky appearance) and sometimes by invasion of the entire cornea by
blood vessels. Some limited recovery of moderate damage may occur
in months or years.
The action spectrum and threshold dose for ultraviolet
keratoconjunctivitis (Fig. 13) have been generally agreed on by
several groups of investigators.
8.3. Injury to the Anterior Portion of the Eye
The anterior structures of the eye are the cornea, conjunctiva,
aqueous humor, iris, and lens. The cornea, aqueous humor, and lens
are part of the optical pathway and, as such, must be transparent
to light. Loss of transparency is serious. Because of the rapid
turnover of corneal epithelial cells, damage limited to this outer
layer can be expected to be temporary. Indeed, injury to this
tissue by exposure to UV-B and UV-C, as occurs in a particular
keratoconjuntivitis, the ultraviolet photokeratitis or
photoophthalmia (known also as "arc eye", or "welder's flash"),
seldom lasts more than one or two days. Unless deeper tissues of
the cornea are also affected, surface epithelium injuries are
rarely permanent.
Near-ultraviolet and near-infrared radiation (UV-A, IR-A, and
possibly IR-B) are strongly absorbed in the lens of the eye.
Damage to this structure is of great concern in that the lens has a
very slow turnover of cells. A one-day exposure may result in
effects that will not become evident for many years. This is
probably the case of glass-blower's or steel puddler's cataract and
in cataracts caused by ionizing radiation. Long-term exposure may
also result in delayed effects (Tengroth et al., 1980).
8.3.1. Effects on the cornea
UV-B and UV-C radiation are absorbed in the cornea and
conjunctiva and sufficiently high doses will cause kerato-
conjunctivitis. The initial effect of UVR exposure is damage to,
or destruction of, the epithelial cells. Under normal conditions,
the corneal epithelial layer is completely replaced in a matter of
a day or so. After exposure, there is a latent period, generally
shorter than 12 h, which varies inversely with the exposure dose.
Healing of the corneal and conjuctival epithelium takes 1 - 2 days.
In severe exposures, damage to Bowman's membrane and the stroma may
occur and is commonly followed by scar formation (usually of a
milky appearance) and sometimes by invasion of the entire cornea by
blood vessels. Some limited recovery of moderate damage may occur
in months or years.
The action spectrum and threshold dose for ultraviolet
keratoconjunctivitis (Fig. 13) have been generally agreed on by
several groups of investigators.
 The reciprocity or irradiance and exposure duration probably
hold for time periods similar to those for ultraviolet erythema
(reddening) of the skin. Specifically, it matters little whether
radiant exposure of the cornea occurs in 1 µs or in 2 h. The
product of the irradiance and the duration of exposure required for
the same effect is a constant for periods up to several h.
The cornea is quite transparent in the IR-A. In the IR-B,
there are some fairly narrow water absorption bands at 1430 nm and
1959 nm. Above 2000 nm, absorption is very high, making the cornea
very susceptible to far-infrared radiation. Thus, as might be
expected, the threshold for damage corresponds to the absorption
bands. Radiation in the IR-C band can induce a burn on the cornea
similar to that on the skin.
The nerve endings of the cornea are quite sensitive to all
temperature elevations and an elevation of 10 °C causes a pain
response. With full-face exposure, a temperature rise can be felt
before corneal pain appears.
Infrared lasers such as CO2 lasers (10.69 µm), HF, and DF
lasers (2.7 - 4.0 µm) or CO lasers (5 µm), having cw output
irradiances of the order of 10 W/cm2 or more can produce corneal
lesions by delivering at least 0.5 - 10 J/cm2, before the blink
reflex is operative (Fig. 14).
The reciprocity or irradiance and exposure duration probably
hold for time periods similar to those for ultraviolet erythema
(reddening) of the skin. Specifically, it matters little whether
radiant exposure of the cornea occurs in 1 µs or in 2 h. The
product of the irradiance and the duration of exposure required for
the same effect is a constant for periods up to several h.
The cornea is quite transparent in the IR-A. In the IR-B,
there are some fairly narrow water absorption bands at 1430 nm and
1959 nm. Above 2000 nm, absorption is very high, making the cornea
very susceptible to far-infrared radiation. Thus, as might be
expected, the threshold for damage corresponds to the absorption
bands. Radiation in the IR-C band can induce a burn on the cornea
similar to that on the skin.
The nerve endings of the cornea are quite sensitive to all
temperature elevations and an elevation of 10 °C causes a pain
response. With full-face exposure, a temperature rise can be felt
before corneal pain appears.
Infrared lasers such as CO2 lasers (10.69 µm), HF, and DF
lasers (2.7 - 4.0 µm) or CO lasers (5 µm), having cw output
irradiances of the order of 10 W/cm2 or more can produce corneal
lesions by delivering at least 0.5 - 10 J/cm2, before the blink
reflex is operative (Fig. 14).
 8.3.2. UVR lenticular effects
The lens has much the same sensitivity to UVR as the cornea.
With exposure to UV-A, there is substantial transmission in the
cornea and high absorption in the lens (Fig. 12).
Acute exposures of the order of 105 to 3 x 106 J/m2 (10 to
300 J/cm2) to radiation in the 320 - 400 nm region cause corneal
opacities, but only exposure to radiation in the UV-B region
appears to be strongly effective in causing lenticular opacities
under acute exposure conditions (Pitts et al., 1977; Zuchlich &
Kurtin, 1977) (Fig. 15). The lenticular opacity may only last for
a few days at low exposures.
8.3.2. UVR lenticular effects
The lens has much the same sensitivity to UVR as the cornea.
With exposure to UV-A, there is substantial transmission in the
cornea and high absorption in the lens (Fig. 12).
Acute exposures of the order of 105 to 3 x 106 J/m2 (10 to
300 J/cm2) to radiation in the 320 - 400 nm region cause corneal
opacities, but only exposure to radiation in the UV-B region
appears to be strongly effective in causing lenticular opacities
under acute exposure conditions (Pitts et al., 1977; Zuchlich &
Kurtin, 1977) (Fig. 15). The lenticular opacity may only last for
a few days at low exposures.
 On the other hand, since long-term exposure to UVR at ambient
outdoor levels may be associated with a reduction in the ability of
the lens to transmit short-wavelength light (Lerman, 1980b) and
with senile cataracts (Weale, 1982), the effects of UVR on the lens
may be cummulative. In addition, there is experimental evidence
that UV-A radiation can induce photosensitized oxidation of the
ocular lens (Zigler & Goosey, 1981).
8.3.3. Infrared cataract
As explained earlier, the ocular media absorb an increasing
amount of the radiant energy incident upon the cornea for
increasing wavelengths in the near infrared (IR-A). For infrared
wavelengths greater than 1400 nm (IR-B and IR-C), the cornea and
aqueous absorb essentially all of the incident radiation, and,
beyond 1900 nm, the cornea is considered to be the sole absorber
(Fig. 12). This absorbed energy may be conducted to interior
structures of the eyes elevating the temperature of the lens, as
well as that of the cornea itself. Heating of the iris by
absorption of visible and near-infrared radiation is considered to
play a role in the development of opacities in the lens, at least
for short exposure times (Goldmann, 1933). Hence, it would be
expected that the spectral absorption and reflectance of the iris
would determine the action spectrum for this effect, for such
exposure times. However, radiation of the lens alone, at lower
levels for longer exposures induces cataracts in the part of the
lens not covered by the iris (Vogt, 1919; Wolbarsht, 1978b). Most
IR-B and IR-C lasers cause damage only to the cornea (Andeev et
al., 1978; Stuck et al., 1981).
8.4. Retinal Injury
The retina is particularly vulnerable to visible and near-
infrared radiation, a spectral domain known as the retinal hazard
region. In most real situations, the refractive power of the
cornea and lens leads to a dramatic increase in irradiance between
the cornea and the retina. When an object is viewed directly, the
light forms an image on the fovea, the centre of the macula, which,
in man, is approximately 0.25 mm in diameter. The typical result
of a retinal injury is a blind spot (i.e., a scotoma) within the
irradiated area. A peripheral scotoma, unless very large, may go
unnoticed. However, if the scotoma results from a lesion located
in the fovea, severe visual handicap results. A central scotoma
could result from looking directly at a hazardous source. The size
of the scotoma depends on the irradiance relative to threshold, the
angular extent of the source, and the extent of accommodation.
Laser lesions of the retina resulting from exposures to light
cause many alterations in structure that can only be seen
histologically (Marshall, 1973). Fig. 16 shows two typical lesions
in the macula of a human being.
The subjective loss of vision associated with laser-induced
retinal injury may be immediate or may develop progressively over a
period of hours or days (Gabel & Birngruber, 1981). The extent to
which visual function recovers depends on the size of the initial
injury and the types of retinal cells involved, as well as the
presence and extent of retinal haemorrhages and their subsequent
degree of resorption (Boldry, et al., 1981). Retinal neurons do
not undergo cell division so repair by cell replacement does not
occur. In small lesions, recovery may result from either growth of
new parts of damaged cells such as photoreceptor outer segments, or
by migration of viable cells into the damaged site. Severe damage
is irreversible and visual loss is permanent.
On the other hand, since long-term exposure to UVR at ambient
outdoor levels may be associated with a reduction in the ability of
the lens to transmit short-wavelength light (Lerman, 1980b) and
with senile cataracts (Weale, 1982), the effects of UVR on the lens
may be cummulative. In addition, there is experimental evidence
that UV-A radiation can induce photosensitized oxidation of the
ocular lens (Zigler & Goosey, 1981).
8.3.3. Infrared cataract
As explained earlier, the ocular media absorb an increasing
amount of the radiant energy incident upon the cornea for
increasing wavelengths in the near infrared (IR-A). For infrared
wavelengths greater than 1400 nm (IR-B and IR-C), the cornea and
aqueous absorb essentially all of the incident radiation, and,
beyond 1900 nm, the cornea is considered to be the sole absorber
(Fig. 12). This absorbed energy may be conducted to interior
structures of the eyes elevating the temperature of the lens, as
well as that of the cornea itself. Heating of the iris by
absorption of visible and near-infrared radiation is considered to
play a role in the development of opacities in the lens, at least
for short exposure times (Goldmann, 1933). Hence, it would be
expected that the spectral absorption and reflectance of the iris
would determine the action spectrum for this effect, for such
exposure times. However, radiation of the lens alone, at lower
levels for longer exposures induces cataracts in the part of the
lens not covered by the iris (Vogt, 1919; Wolbarsht, 1978b). Most
IR-B and IR-C lasers cause damage only to the cornea (Andeev et
al., 1978; Stuck et al., 1981).
8.4. Retinal Injury
The retina is particularly vulnerable to visible and near-
infrared radiation, a spectral domain known as the retinal hazard
region. In most real situations, the refractive power of the
cornea and lens leads to a dramatic increase in irradiance between
the cornea and the retina. When an object is viewed directly, the
light forms an image on the fovea, the centre of the macula, which,
in man, is approximately 0.25 mm in diameter. The typical result
of a retinal injury is a blind spot (i.e., a scotoma) within the
irradiated area. A peripheral scotoma, unless very large, may go
unnoticed. However, if the scotoma results from a lesion located
in the fovea, severe visual handicap results. A central scotoma
could result from looking directly at a hazardous source. The size
of the scotoma depends on the irradiance relative to threshold, the
angular extent of the source, and the extent of accommodation.
Laser lesions of the retina resulting from exposures to light
cause many alterations in structure that can only be seen
histologically (Marshall, 1973). Fig. 16 shows two typical lesions
in the macula of a human being.
The subjective loss of vision associated with laser-induced
retinal injury may be immediate or may develop progressively over a
period of hours or days (Gabel & Birngruber, 1981). The extent to
which visual function recovers depends on the size of the initial
injury and the types of retinal cells involved, as well as the
presence and extent of retinal haemorrhages and their subsequent
degree of resorption (Boldry, et al., 1981). Retinal neurons do
not undergo cell division so repair by cell replacement does not
occur. In small lesions, recovery may result from either growth of
new parts of damaged cells such as photoreceptor outer segments, or
by migration of viable cells into the damaged site. Severe damage
is irreversible and visual loss is permanent.
 Only an extremely small fraction of UVR incident on the cornea
reaches the retina. Nevertheless, the fraction of a percent of
UV-A that reaches the retina can have adverse effects, as has been
demonstrated by Zuchlich & Taboada (1978). Retinal lesions were
seen following exposure to a He-Cd laser at 325 nm. Because of the
strong scattering of UV-A in the ocular media, it is difficult to
estimate the retinal exposure. Young rhesus monkeys were used,
hence, the transmission of the ocular media was still relatively
high (perhaps 1%), whereas, in adult human beings this transmission
is much less.
Aphakics (persons with the lens removed) are special exceptions
to this rule and would be expected to be extremely susceptible to
UV-A injury of the retina, particularly as their corrective lenses
will usually transmit UV-A radiation very well.
8.4.1. Determining the retinal exposure
The optical properties of the eye play an important role in
determining retinal injury. Such factors as the image quality,
pupil size, spectral absorption, and scattering by the cornea,
aqueous, lens, and vitreous, as well as the spectral reflectance of
the fundus and absorption and scattering in the various retinal
layers, must be known for a definitive description of retinal
exposure. These factors will be considered separately.
8.4.1.1. Pupil size
The limiting aperture of the eye determines the amount of
radiant energy entering the eye, and thus reaching the retina. It
is therefore proportional to the area of the pupil. For the
normal, dark-adapted eye, pupil sizes range from approximately 7 to
8 mm; for outdoor daylight, the normal pupil constricts to
approximately 1.6 - 2.0 mm. The ratio of areas between a 2-mm and
an 8-mm pupil is: 1:16; hence, a 2-mm pupil permits the entry of
one-sixteenth of the light admitted by a 8-mm pupil. The angle
subtended by the source also plays a role; thus a light source of a
given size and luminance causes a different pupil size, depending
on the viewing distance (i.e., the image area on the retina), and
the luminance of the surrounding field.
The pupilomotor reflex will constrict the pupil on exposure to
a bright light source within a period of the order of 20 ms
(Davson, ed., 1962). Some medications and drugs will create an
abnormal pupil size. Therefore, in a large population, the pupil
size may vary greatly under the same environmental exposure
conditions.
8.4.1.2. Spectral transmission of the ocular media and spectral
absorption by the retina and choroid
The transmission of the ocular media between 300 nm and 1400 nm
has been studied by several investigators and results vary
(Geeraets & Berry, 1968; Gabel et al., 1976). Fig. 17 shows a
representative spectral transmission of the human ocular media.
Only an extremely small fraction of UVR incident on the cornea
reaches the retina. Nevertheless, the fraction of a percent of
UV-A that reaches the retina can have adverse effects, as has been
demonstrated by Zuchlich & Taboada (1978). Retinal lesions were
seen following exposure to a He-Cd laser at 325 nm. Because of the
strong scattering of UV-A in the ocular media, it is difficult to
estimate the retinal exposure. Young rhesus monkeys were used,
hence, the transmission of the ocular media was still relatively
high (perhaps 1%), whereas, in adult human beings this transmission
is much less.
Aphakics (persons with the lens removed) are special exceptions
to this rule and would be expected to be extremely susceptible to
UV-A injury of the retina, particularly as their corrective lenses
will usually transmit UV-A radiation very well.
8.4.1. Determining the retinal exposure
The optical properties of the eye play an important role in
determining retinal injury. Such factors as the image quality,
pupil size, spectral absorption, and scattering by the cornea,
aqueous, lens, and vitreous, as well as the spectral reflectance of
the fundus and absorption and scattering in the various retinal
layers, must be known for a definitive description of retinal
exposure. These factors will be considered separately.
8.4.1.1. Pupil size
The limiting aperture of the eye determines the amount of
radiant energy entering the eye, and thus reaching the retina. It
is therefore proportional to the area of the pupil. For the
normal, dark-adapted eye, pupil sizes range from approximately 7 to
8 mm; for outdoor daylight, the normal pupil constricts to
approximately 1.6 - 2.0 mm. The ratio of areas between a 2-mm and
an 8-mm pupil is: 1:16; hence, a 2-mm pupil permits the entry of
one-sixteenth of the light admitted by a 8-mm pupil. The angle
subtended by the source also plays a role; thus a light source of a
given size and luminance causes a different pupil size, depending
on the viewing distance (i.e., the image area on the retina), and
the luminance of the surrounding field.
The pupilomotor reflex will constrict the pupil on exposure to
a bright light source within a period of the order of 20 ms
(Davson, ed., 1962). Some medications and drugs will create an
abnormal pupil size. Therefore, in a large population, the pupil
size may vary greatly under the same environmental exposure
conditions.
8.4.1.2. Spectral transmission of the ocular media and spectral
absorption by the retina and choroid
The transmission of the ocular media between 300 nm and 1400 nm
has been studied by several investigators and results vary
(Geeraets & Berry, 1968; Gabel et al., 1976). Fig. 17 shows a
representative spectral transmission of the human ocular media.
 There is considerable individual variability in these spectral
quantities and this must be remembered when using the data in an
accurate calculation. The other factor that must not be forgotten
is the shift of the short-wavelength cutoff at 390 - 410 nm with
age. The lens transmits less UV-A and blue light with increasing
age as it yellows. With the above factors taken into account, it
is possible to multiply the spectral absorption data of the retina
and choroid by the spectral transmission data for the ocular media
to arrive at an estimate of the absorbed spectral exposure dose in
the retina and choroid, relative to the spectral radiant exposure
at the cornea. This spectral effectiveness curve for retinal
thermal injury is applicable, at least, to exposure durations of
less than approximately 10 s (Fig. 17).
8.4.1.3. Optical image quality
The retinal image size can be calculated for most extended
sources by geometrical optics. As shown in Fig. 18, the angle
subtended by an extended source defines the image size. The
effective focal length of the relaxed normal eye fe is approx.
1.7 cm. With fe known, the retinal image size dr can be
calculated, if the viewing distance r and the dimension of the
light source DL are known:
dr = DLfe/r Equation (12)
From this, the quantitative relation can be obtained of retinal
irradiance Er to source radiance L (or retinal illuminance to
source luminance) for small angles:
Er = (pi x dp2 L x tau)/4fe2
= 0.27 dp2 x L x tau(for dp in cm) Equation (13)
where dp is the pupillary diameter and tau is the spectral
transmission of the ocular media.
From equation 13, it is possible to define a permissible
radiance (luminance) from a permissible retinal irradiance for any
source of known radiance or luminance, without taking into account
the viewing angle or viewing distance.
Each source point has a corresponding image point, hence, the
retinal irradiance in an incremental area of the image is related
to the radiance of a corresponding incremental area of the source
(Hartman & Kleman, 1980).
8.4.1.4. Small images
Equation 13 breaks down for very small images (or for very
small hot spots in an image), where the source or source element in
question subtends an angle of less than 10 minutes-of-arc (i.e.,
image size is less than 50 µm).
There is considerable individual variability in these spectral
quantities and this must be remembered when using the data in an
accurate calculation. The other factor that must not be forgotten
is the shift of the short-wavelength cutoff at 390 - 410 nm with
age. The lens transmits less UV-A and blue light with increasing
age as it yellows. With the above factors taken into account, it
is possible to multiply the spectral absorption data of the retina
and choroid by the spectral transmission data for the ocular media
to arrive at an estimate of the absorbed spectral exposure dose in
the retina and choroid, relative to the spectral radiant exposure
at the cornea. This spectral effectiveness curve for retinal
thermal injury is applicable, at least, to exposure durations of
less than approximately 10 s (Fig. 17).
8.4.1.3. Optical image quality
The retinal image size can be calculated for most extended
sources by geometrical optics. As shown in Fig. 18, the angle
subtended by an extended source defines the image size. The
effective focal length of the relaxed normal eye fe is approx.
1.7 cm. With fe known, the retinal image size dr can be
calculated, if the viewing distance r and the dimension of the
light source DL are known:
dr = DLfe/r Equation (12)
From this, the quantitative relation can be obtained of retinal
irradiance Er to source radiance L (or retinal illuminance to
source luminance) for small angles:
Er = (pi x dp2 L x tau)/4fe2
= 0.27 dp2 x L x tau(for dp in cm) Equation (13)
where dp is the pupillary diameter and tau is the spectral
transmission of the ocular media.
From equation 13, it is possible to define a permissible
radiance (luminance) from a permissible retinal irradiance for any
source of known radiance or luminance, without taking into account
the viewing angle or viewing distance.
Each source point has a corresponding image point, hence, the
retinal irradiance in an incremental area of the image is related
to the radiance of a corresponding incremental area of the source
(Hartman & Kleman, 1980).
8.4.1.4. Small images
Equation 13 breaks down for very small images (or for very
small hot spots in an image), where the source or source element in
question subtends an angle of less than 10 minutes-of-arc (i.e.,
image size is less than 50 µm).
 The diffraction theory can be applied to estimate the minimal
retinal image size for viewing a point source such as a laser.
However, scattering in the ocular media and corneal aberations
limits this image diameter to approximately 10 - 20 µm (Sliney,
1971).
It would be expected that, in the case of small-sized images,
the retinal hazard would increase in proportion to the area of the
pupil. Therefore, night-time viewing of a point source would be
expected to be far more dangerous than day-time viewing; however,
this is not the case, since the image blur increases with larger
pupil sizes. It is worthwhile noting that the increase in
irradiance from cornea to retina, when the relaxed eye views a
point source, is about 105 (100 000 times) (Sliney & Freasier,
1973). Almost any directly viewed laser can appear as a point
source.
8.4.1.5. Retinal pigment epithelium (RPE) absorption
As previously indicated, visible and near-infrared radiation is
transmitted through the ocular media and is absorbed principally in
the retina. The radiation passes through the neural layers of the
retina before reaching the RPE and choroid. The visual pigments in
the rods and cones absorb only a small fraction of light to
initiate the visual response, perhaps only 5% of the total energy
entering the eye. The RPE absorbs a substantial fraction of the
light (about 50% in the green) and is optically the most absorbent
layer. As the absorption takes place in a highly concentrated
layer of melanin granules approximately 3 - 6 µm thick, the greatest
temperature rise occurs in this layer (Bergquist et al., 1978;
Birngruber, 1978). The actual size, shape, distribution, and
physical characteristics of individual melanin granules become
quite important for a thermal model adequate to describe the
behaviour of this layer, during very short pulse exposures
(Wolbarsht, et al., 1980). The granules may be heated to
incandescence during Q-switched exposures, and this incandescence
can be seen, if viewed during a 1064-nm (neodymium-YAG) laser
experiment (Mueller & Ham, 1980, private communication).
8.4.2. Chorioretinal thermal injury
The retinal injury mechanism is considered to be largely
thermal for accidental exposures from arc lamps, cw lasers, or
optically aided viewing of the sun, for durations of the order of
1 ms to ~10 s. Since injury appears to result principally from
protein denaturation and enzyme inactivation, the variation in
retinal temperature during and following the insult must be
considered (Beatrice & Velez, 1975). Several efforts to develop
mathematical models for light absorption, heat flow, and the rate-
process injury mechanisms within the complex structure of the
retina have been moderately successful, over periods of exposure
lasting from 1 ms to 10 s (Vos, 1966a; Mainster et al., 1970;
Allen, 1980).
The tissue surrounding the absorption site can much more
readily conduct away the absorbed heat for images, 10 - 50 µm in
diameter, than it can for large images of the order of 1000 µm
(1 mm). Indeed, retinal injury thresholds for the same time range
of 0.1 - 10 s are very closely related to image size, as would be
expected from calculations of heat flow in the retina. For
example, exposure to irradiances of 10-100 kW/m2 (i.e., 1-10 W/cm2)
results in a minimal retinal injury threshold for a 1000-µm image,
whereas an irradiance of 10 MW/m2 (1 kW/cm2) is required to produce
the same type of threshold lesion in a 20-µm image (Ham et al.,
1970).
For short-pulse durations, the reason for the spot-size
dependence of the threshold is not clear (Frisch et al., 1971).
The expectation, when exposure durations are of the order of 1 ms,
is that injury will take place before there is significant heat
flow. Indeed, the variation of threshold with pulse duration
itself is also rather puzzling, especially the increase in
threshold for 20-ns, Q-switched pulses over those of 1-µs duration
(Hansen & Fine, 1968; Harlen, 1978; Anderson, 1980b). Obviously,
the Q-switched pulse energy is being dissipated in some mechanism
such as a mechanical displacement of tissue (an acoustic
transient), which does not contribute to the normal thermal injury
process that determines the minimum threshold.
In studies conducted by Beatrice & Lund (1979) with image
distributions that were non-circular, such as line images on the
retina, circular lesions were produced after long-term exposures.
This would be predicted by thermal injury and heat flow
calculations. Very short, Q-switched exposures with similar line
image distributions produced lesions that were very elongated, as,
again, would be predicted by a simple thermal model or injury. It
might be thought that the contribution of acoustic transients from
such a short exposure would have been to enlarge the lesion.
Photoacoustic effects should certainly make a considerable
contribution; but whether the acoustic transient adds to, or
subtracts from the injury mechanism is not yet clear.
For short-term exposures (< 1 µs) resulting from Q-switched
lasers, exploding wires, super-radiant light, and mode-locked
lasers, the exposure thresholds of injury are lowest. Although it
is believed that, for a Q-switched exposure, the injury mechanism
is largely thermal, the effect of acoustic transients due to rapid
heating and thermal expansion in the immediate vicinity of the
absorption site (individual melanin granules) may play a role. For
still shorter durations of exposure, direct electric field effects,
Raman and Brillouin scattering, and multiphoton absorption could
play a role in the damage mechanism (Greisemann & Marti, 1978;
Rockerolles, 1978).
8.4.3. Location of retinal burns
As previously explained, the different regions of the retina
play different roles in vision. Thus, the significance of
functional loss of all or part of any one of these regions, because
of retinal injury, varies. The loss of foveal vision seriously
reduces visual performance. Limited peripheral loss could be
unnoticed, subjectively (Kaufman, 1970; Holzinger et al., 1978).
8.5. Photochemical Retinal Injury
8.5.1. Very long-term exposure
The human retina is normally subjected to irradiances below
1 W/m2 (10-4 W/cm2), as shown in Fig. 19, except for occasional
momentary exposure to the sun, welding arcs, and similar bright
sources. The retinal images resulting from viewing such sources
are often quite small (for example 0.15 mm for the sun) and the
duration of exposure is normally limited to the duration of the
blink reflex (0.15 - 0.2 s). Natural aversion to bright light
usually limits further retinal exposures above 10-4 W/cm2. Until
recently, few studies of adverse retinal effects existed for the
irradiance range of 10-4-1 W/cm2. Studies in this range have
generally centred on flash blindness effects following light
exposures lasting up to 1 s.
Exposure of large areas of the retina to moderately high
luminance light of the order of 105 cd/m2 (~100 µW/cm2, i.e.,
1 W/m2 at the retina) for durations of one to several hours has
been investigated in experimental animals. Generally, the light
sources employed in these studies were fluorescent lamps. A
thermally-enhanced photochemical mechanism of injury or a
phototoxic effect appears to be most likely (Kuwabara, 1970; Noell
& Albrecht, 1971). More recently, similar fluorescent light
exposure of rhesus monkeys with dilated pupils showed that this
effect was not limited to nocturnal animals but could conceivably
be related to very lengthy direct-viewing by man (Sykes, et al.,
1981). Collectively, the results of these studies suggest that
abnormally high environmental levels of retinal illumination cause
retinal degeneration for any species. This is particularly marked
in albinos (LaVail, 1980). The effects are most dramatic when the
normal, diurnal cycle of light and dark is eliminated by constant
illumination (Williams & Baker, 1980). The levels and durations of
these retinal exposures exceed those encountered during normal
human behaviour. Only rarely have investigators reported that
continual exposure to high luminance levels in the natural
environment (or work environment) has elicited significant
functional changes in the human retina (Livingston, 1932; Smith,
1944; Peckham & Harley, 1951; Medvedovskaja, 1970; Roger, 1973).
The diffraction theory can be applied to estimate the minimal
retinal image size for viewing a point source such as a laser.
However, scattering in the ocular media and corneal aberations
limits this image diameter to approximately 10 - 20 µm (Sliney,
1971).
It would be expected that, in the case of small-sized images,
the retinal hazard would increase in proportion to the area of the
pupil. Therefore, night-time viewing of a point source would be
expected to be far more dangerous than day-time viewing; however,
this is not the case, since the image blur increases with larger
pupil sizes. It is worthwhile noting that the increase in
irradiance from cornea to retina, when the relaxed eye views a
point source, is about 105 (100 000 times) (Sliney & Freasier,
1973). Almost any directly viewed laser can appear as a point
source.
8.4.1.5. Retinal pigment epithelium (RPE) absorption
As previously indicated, visible and near-infrared radiation is
transmitted through the ocular media and is absorbed principally in
the retina. The radiation passes through the neural layers of the
retina before reaching the RPE and choroid. The visual pigments in
the rods and cones absorb only a small fraction of light to
initiate the visual response, perhaps only 5% of the total energy
entering the eye. The RPE absorbs a substantial fraction of the
light (about 50% in the green) and is optically the most absorbent
layer. As the absorption takes place in a highly concentrated
layer of melanin granules approximately 3 - 6 µm thick, the greatest
temperature rise occurs in this layer (Bergquist et al., 1978;
Birngruber, 1978). The actual size, shape, distribution, and
physical characteristics of individual melanin granules become
quite important for a thermal model adequate to describe the
behaviour of this layer, during very short pulse exposures
(Wolbarsht, et al., 1980). The granules may be heated to
incandescence during Q-switched exposures, and this incandescence
can be seen, if viewed during a 1064-nm (neodymium-YAG) laser
experiment (Mueller & Ham, 1980, private communication).
8.4.2. Chorioretinal thermal injury
The retinal injury mechanism is considered to be largely
thermal for accidental exposures from arc lamps, cw lasers, or
optically aided viewing of the sun, for durations of the order of
1 ms to ~10 s. Since injury appears to result principally from
protein denaturation and enzyme inactivation, the variation in
retinal temperature during and following the insult must be
considered (Beatrice & Velez, 1975). Several efforts to develop
mathematical models for light absorption, heat flow, and the rate-
process injury mechanisms within the complex structure of the
retina have been moderately successful, over periods of exposure
lasting from 1 ms to 10 s (Vos, 1966a; Mainster et al., 1970;
Allen, 1980).
The tissue surrounding the absorption site can much more
readily conduct away the absorbed heat for images, 10 - 50 µm in
diameter, than it can for large images of the order of 1000 µm
(1 mm). Indeed, retinal injury thresholds for the same time range
of 0.1 - 10 s are very closely related to image size, as would be
expected from calculations of heat flow in the retina. For
example, exposure to irradiances of 10-100 kW/m2 (i.e., 1-10 W/cm2)
results in a minimal retinal injury threshold for a 1000-µm image,
whereas an irradiance of 10 MW/m2 (1 kW/cm2) is required to produce
the same type of threshold lesion in a 20-µm image (Ham et al.,
1970).
For short-pulse durations, the reason for the spot-size
dependence of the threshold is not clear (Frisch et al., 1971).
The expectation, when exposure durations are of the order of 1 ms,
is that injury will take place before there is significant heat
flow. Indeed, the variation of threshold with pulse duration
itself is also rather puzzling, especially the increase in
threshold for 20-ns, Q-switched pulses over those of 1-µs duration
(Hansen & Fine, 1968; Harlen, 1978; Anderson, 1980b). Obviously,
the Q-switched pulse energy is being dissipated in some mechanism
such as a mechanical displacement of tissue (an acoustic
transient), which does not contribute to the normal thermal injury
process that determines the minimum threshold.
In studies conducted by Beatrice & Lund (1979) with image
distributions that were non-circular, such as line images on the
retina, circular lesions were produced after long-term exposures.
This would be predicted by thermal injury and heat flow
calculations. Very short, Q-switched exposures with similar line
image distributions produced lesions that were very elongated, as,
again, would be predicted by a simple thermal model or injury. It
might be thought that the contribution of acoustic transients from
such a short exposure would have been to enlarge the lesion.
Photoacoustic effects should certainly make a considerable
contribution; but whether the acoustic transient adds to, or
subtracts from the injury mechanism is not yet clear.
For short-term exposures (< 1 µs) resulting from Q-switched
lasers, exploding wires, super-radiant light, and mode-locked
lasers, the exposure thresholds of injury are lowest. Although it
is believed that, for a Q-switched exposure, the injury mechanism
is largely thermal, the effect of acoustic transients due to rapid
heating and thermal expansion in the immediate vicinity of the
absorption site (individual melanin granules) may play a role. For
still shorter durations of exposure, direct electric field effects,
Raman and Brillouin scattering, and multiphoton absorption could
play a role in the damage mechanism (Greisemann & Marti, 1978;
Rockerolles, 1978).
8.4.3. Location of retinal burns
As previously explained, the different regions of the retina
play different roles in vision. Thus, the significance of
functional loss of all or part of any one of these regions, because
of retinal injury, varies. The loss of foveal vision seriously
reduces visual performance. Limited peripheral loss could be
unnoticed, subjectively (Kaufman, 1970; Holzinger et al., 1978).
8.5. Photochemical Retinal Injury
8.5.1. Very long-term exposure
The human retina is normally subjected to irradiances below
1 W/m2 (10-4 W/cm2), as shown in Fig. 19, except for occasional
momentary exposure to the sun, welding arcs, and similar bright
sources. The retinal images resulting from viewing such sources
are often quite small (for example 0.15 mm for the sun) and the
duration of exposure is normally limited to the duration of the
blink reflex (0.15 - 0.2 s). Natural aversion to bright light
usually limits further retinal exposures above 10-4 W/cm2. Until
recently, few studies of adverse retinal effects existed for the
irradiance range of 10-4-1 W/cm2. Studies in this range have
generally centred on flash blindness effects following light
exposures lasting up to 1 s.
Exposure of large areas of the retina to moderately high
luminance light of the order of 105 cd/m2 (~100 µW/cm2, i.e.,
1 W/m2 at the retina) for durations of one to several hours has
been investigated in experimental animals. Generally, the light
sources employed in these studies were fluorescent lamps. A
thermally-enhanced photochemical mechanism of injury or a
phototoxic effect appears to be most likely (Kuwabara, 1970; Noell
& Albrecht, 1971). More recently, similar fluorescent light
exposure of rhesus monkeys with dilated pupils showed that this
effect was not limited to nocturnal animals but could conceivably
be related to very lengthy direct-viewing by man (Sykes, et al.,
1981). Collectively, the results of these studies suggest that
abnormally high environmental levels of retinal illumination cause
retinal degeneration for any species. This is particularly marked
in albinos (LaVail, 1980). The effects are most dramatic when the
normal, diurnal cycle of light and dark is eliminated by constant
illumination (Williams & Baker, 1980). The levels and durations of
these retinal exposures exceed those encountered during normal
human behaviour. Only rarely have investigators reported that
continual exposure to high luminance levels in the natural
environment (or work environment) has elicited significant
functional changes in the human retina (Livingston, 1932; Smith,
1944; Peckham & Harley, 1951; Medvedovskaja, 1970; Roger, 1973).
 It has been shown that short-wavelength exposures are most
effective in inducing photochemical retinal injury (Ham et al.,
1976, 1978; Lawwill et al., 1977). The adverse effect is normally
centralized in the pigment layer and adjacent outer receptor layer.
Other retinal layers may be affected, but this generally follows
changes in the RPE. The effect appears first where pigment is
located.
Results of studies of photochemical retinal injury in
experimental rhesus monkeys (Ham et al., 1978; Moon et al., 1978)
agree with clinical experience reviewed by Sliney (1978) concerning
the development of eclipse-burn photoretinitis after staring at the
sun. Until recently, it was generally accepted that solar retinal
injury was permanent; however Hatfield (1970) and Penner & McNair
(1966) reported significant numbers of patients who recovered
within 30 days.
Repeated exposure of large retinal areas in trained monkeys to
incoherent light at retinal irradiances just above those
experienced in a bright natural outdoor environment, showed a
permanent decrease in functional sensitivity to blue light
(Harwerth & Sperling, 1975). Exposure of the monkeys to narrow
bands of wavelengths from the green to the red elicited a similar,
but not lasting, reaction. These types of studies, repeated by
Zwick & Beatrice (1978), showed more dramatic changes with coherent
light having a speckle pattern. Prolonged erythropsia (red vision)
in aphakics has also been reported following exposure to large-
area, high-luminance sources with large amounts of ultraviolet such
as snow fields.
Follow-up studies conducted during the 1940s showed the effects
on vision of the prolonged exposure of beach lifeguards to bright
outdoor environments. Temporary reductions in sensitivity for both
daylight and night vision lasting for periods of several days were
reported (Peckham & Harley, 1951).
There is growing concern among some investigators, who have
studied the adverse retinal effects of intense light sources, that
life-long exposure to light plays a role in retinal aging
(Marshall, 1978). Certain age-degenerative retinal effects may be
light-initiated. This opinion is prompted by the strong similarity
between histological and ultrastructural changes in aged retinae
and those in retinae exposed to intense light sources including
disorganization of the outer receptors; depigmentation of the RPE,
and a decrease in the total number of receptors. Clearly,
considerably more research will be required before this opinion can
be confirmed.
8.6. Flash Blindness
Flash blindness is a normal physiological process, being a
transitory loss of visual function. This phenomenon is a function
of the preadaptive state of the subject, the nature of the visual
task (i.e., task luminance, position in the visual field, and
acuity), and the luminance of the stimulating source. The
mechanism is complex and not fully understood, as it involves both
biochemical and neural processes. The recovery time is a measure
of the degree of flash blindness.
Flash blindness has been intensively investigated, both in
predicting functional loss that might be expected from a given
exposure and in the design of protective devices. The response
times of present-day protective devices range from a few ms down to
several µs. Even within this long delay, great difficulty has been
encountered in producing a device that can attenuate the luminance
of the source by a factor of more than 1000.
In dealing with the data on flash blindness and attempting to
relate it to retinal mechanisms, it is well to keep in mind the
ideas originally expressed by Brown (1973), who showed that
recovery from flash blindness did not involve a single, simple
mechanism. It involves both dark adaptation and neurophysiological
effects not usually seen in studies of dark adaption.
8.7. Discomfort Glare
If a very bright light source is suddenly switched on after the
eye has adapted to a luminance much lower than that of the source,
the viewer experiences discomfort, blinks, and tends to turn the
head or eyes. This effect is much more dramatic when the ambient
luminance is low. Out-of-doors, in full daylight, the luminance of
a large extended source required to elicit this phenomenon is of
the order of 100 000 cd/m2 (10 cd/cm2 or 29 000 foot-lamberts);
however, the luminance of this source must be far greater to elicit
a response, if the source subtends an angle of less than about 4.5
mrad (0.25 degree).
8.8. Flashing Lights
Classical studies of vision suggest that a strobe operating at
10 Hz can appear subjectively brighter than a cw source of the same
peak brightness, due to the Bartley Effect for flashing light
sources. Similarly, the brightness of a single pulse appears
brighter than it really is; this phenomenon is termed the Broca-
Sulzer Effect (Cornsweet, 1966).
Strobe light sources produce little annoyance during daylight
hours. However, at night, if a strobe illuminates an area that
would otherwise be dark, at a frequency of 5 - 10 Hz, the static
objects illuminated by the strobe appear to float around, because
of loss of a fixation point during off-periods of the light.
The medical literature suggests that epileptic seizures in
susceptible individuals represent the only well-documented health
hazard from exposure to low-frequency intermittent light. The most
sensitive frequency range is from 8 to l6 Hz. Various estimates
indicate that approximately 1.0% of the epileptic population, which
itself constitutes less than 1.0% of the general population, will
experience these "flicker-induced" seizures.
9. THE SKIN
9.1. Anatomy
The skin is normally of less interest than the eye as far as
optical radiation hazards are concerned. However, under certain
conditions, it may be more vulnerable than the eye, which can be
protected by the blink reflex or by eye protectors.
The outermost layer, the stratum corneum or horny layer,
consists of flattened, epidermal cells. They originate in the
germinative layer (a single cell layer of collumnar germinative
basal cells) at the bottom of the epidermis, grow, and are
gradually pushed outward until they die and are flattened to form a
protective layer over the living cells.
The stratum corneum is approximately 10 - 20 µm thick over most
parts of the body, except the soles of the feet and the palms of
the hand, where it is much thicker (500 - 600 µm).
The epidermis is relatively uniform in thickness throughout the
body (50 - 150 µm) and can be separated into a number of layers
with the growing cells in the lowest level toward the basal
membrane.
Melanocytes, specialized cells that produce melanin pigment
granules, are located in the basal layer of the epidermis. The
melanocytes send out dendritic processes that interdigitate within
the keratinocytes. Melanosomes (the pigment granules) are then
transferred into the keratinocytes. The pigment is thus
distributed throughout the epidermis and stratum corneum by
migration of the keratinocytes.
The dermis, or corium, is thicker than the epidermis, and
consists largely of connective tissue which gives the skin its
elasticity and supportive strength. The sweat glands extend into
the corium.
9.2. Body Heat Regulation
The skin plays a major role in the thermoregulatory system of
the human body. At incident irradiances less than those that cause
thermal skin burns, the body can be subjected to heat stress.
Several physical means are employed by the skin for cooling
(conductive, convective, and radiative cooling).
The sweat glands produce sweat, which permits evaporative
cooling as well as conductive cooling. The reflectance of human
skin in the far infrared is very low with a correspondingly high
emissivity for wavelengths in the 8 - 13 µm infrared region. The
high emissivity at these wavelengths permits highly efficient
radiative cooling of the skin at body temperature.
Comparison of the reflectance spectrum of the human skin with
the solar emission spectrum shows a striking similarity. The skin
reflects largely in the visible part and near-infrared parts of the
spectrum, where solar radiation is greatest, and absorbs heavily in
the ultraviolet and far infrared, where there is very little solar
radiation. Any good radiator of infrared energy (a black body)
must have very high absorption, hence very low total reflection.
The skin does indeed have low reflectance in the far infrared, and
seems well adapted to the natural environment. The skin both
reflects direct solar radiation and reradiates internally generated
infrared radiation with the greatest possible efficiency. However,
the human body is less capable of reflecting the infrared radiation
from man-made sources such as fire, or more specifically from
molten steel in a steel mill (Hardy, 1968; Sliney & Freasier, 1973;
Stolwijk, 1980).
9.3. Optical Properties
The stratum corneum strongly absorbs actinic UVR, which causes
sunburn. This layer also strongly absorbs far-infrared radiation.
Melanin granules are small (1 µm diameter) and not only protect the
dermis by absorption of UVR, but also by scattering optical
radiation. Melanin scatters rather than absorbs radiation in the
near-infrared region. For this and other reasons, near-infrared
radiation penetrates deeply into the tissue. Since the index of
refraction of the stratum corneum is about 1.5, the Fresnel
reflective component is somewhat similar to that of glass (Fig. 2).
Optical radiation incident on the skin at grazing angles of
incidence is hardly absorbed at all. The relative effectiveness of
optical radiation in penetrating the epidermis (and dermis) varies
approximately as the cosine of the angle of incidence. Since light
penetrates the outermost layers of the skin, undergoes multiple
scattering, and some light is scattered back out of the skin, the
skin has an appearance that cannot easily be duplicated by a non-
translucent surface (Anderson & Parrish, 1981).
9.4. Penetration Depth and Reflection
Studies of the effects of pulsed visible and IR laser radiation
on pig skin, performed in the 1960s, provided single-wavelength
thresholds for injury for very short-term exposures of the order of
1 ms and 20 ns. For such short durations of exposure, the
influence of heat flow from the absorbing site is not a major
factor. For this reason, these studies aptly showed that the
threshold of injury depended on the reflectance of the skin and the
depth of penetration of the optical radiation into the skin (Fig.
20).
The reflectance of the skin also plays a role in determining
how much radiation can effectively be absorbed. The skin's
spectral reflectance varies with pigmentation and is significant
only in the visible and near-infrared spectrum. The skin's
reflectance at wavelengths of less than 310 nm and above 2.5 µm is
less than 5%.
It has been shown that short-wavelength exposures are most
effective in inducing photochemical retinal injury (Ham et al.,
1976, 1978; Lawwill et al., 1977). The adverse effect is normally
centralized in the pigment layer and adjacent outer receptor layer.
Other retinal layers may be affected, but this generally follows
changes in the RPE. The effect appears first where pigment is
located.
Results of studies of photochemical retinal injury in
experimental rhesus monkeys (Ham et al., 1978; Moon et al., 1978)
agree with clinical experience reviewed by Sliney (1978) concerning
the development of eclipse-burn photoretinitis after staring at the
sun. Until recently, it was generally accepted that solar retinal
injury was permanent; however Hatfield (1970) and Penner & McNair
(1966) reported significant numbers of patients who recovered
within 30 days.
Repeated exposure of large retinal areas in trained monkeys to
incoherent light at retinal irradiances just above those
experienced in a bright natural outdoor environment, showed a
permanent decrease in functional sensitivity to blue light
(Harwerth & Sperling, 1975). Exposure of the monkeys to narrow
bands of wavelengths from the green to the red elicited a similar,
but not lasting, reaction. These types of studies, repeated by
Zwick & Beatrice (1978), showed more dramatic changes with coherent
light having a speckle pattern. Prolonged erythropsia (red vision)
in aphakics has also been reported following exposure to large-
area, high-luminance sources with large amounts of ultraviolet such
as snow fields.
Follow-up studies conducted during the 1940s showed the effects
on vision of the prolonged exposure of beach lifeguards to bright
outdoor environments. Temporary reductions in sensitivity for both
daylight and night vision lasting for periods of several days were
reported (Peckham & Harley, 1951).
There is growing concern among some investigators, who have
studied the adverse retinal effects of intense light sources, that
life-long exposure to light plays a role in retinal aging
(Marshall, 1978). Certain age-degenerative retinal effects may be
light-initiated. This opinion is prompted by the strong similarity
between histological and ultrastructural changes in aged retinae
and those in retinae exposed to intense light sources including
disorganization of the outer receptors; depigmentation of the RPE,
and a decrease in the total number of receptors. Clearly,
considerably more research will be required before this opinion can
be confirmed.
8.6. Flash Blindness
Flash blindness is a normal physiological process, being a
transitory loss of visual function. This phenomenon is a function
of the preadaptive state of the subject, the nature of the visual
task (i.e., task luminance, position in the visual field, and
acuity), and the luminance of the stimulating source. The
mechanism is complex and not fully understood, as it involves both
biochemical and neural processes. The recovery time is a measure
of the degree of flash blindness.
Flash blindness has been intensively investigated, both in
predicting functional loss that might be expected from a given
exposure and in the design of protective devices. The response
times of present-day protective devices range from a few ms down to
several µs. Even within this long delay, great difficulty has been
encountered in producing a device that can attenuate the luminance
of the source by a factor of more than 1000.
In dealing with the data on flash blindness and attempting to
relate it to retinal mechanisms, it is well to keep in mind the
ideas originally expressed by Brown (1973), who showed that
recovery from flash blindness did not involve a single, simple
mechanism. It involves both dark adaptation and neurophysiological
effects not usually seen in studies of dark adaption.
8.7. Discomfort Glare
If a very bright light source is suddenly switched on after the
eye has adapted to a luminance much lower than that of the source,
the viewer experiences discomfort, blinks, and tends to turn the
head or eyes. This effect is much more dramatic when the ambient
luminance is low. Out-of-doors, in full daylight, the luminance of
a large extended source required to elicit this phenomenon is of
the order of 100 000 cd/m2 (10 cd/cm2 or 29 000 foot-lamberts);
however, the luminance of this source must be far greater to elicit
a response, if the source subtends an angle of less than about 4.5
mrad (0.25 degree).
8.8. Flashing Lights
Classical studies of vision suggest that a strobe operating at
10 Hz can appear subjectively brighter than a cw source of the same
peak brightness, due to the Bartley Effect for flashing light
sources. Similarly, the brightness of a single pulse appears
brighter than it really is; this phenomenon is termed the Broca-
Sulzer Effect (Cornsweet, 1966).
Strobe light sources produce little annoyance during daylight
hours. However, at night, if a strobe illuminates an area that
would otherwise be dark, at a frequency of 5 - 10 Hz, the static
objects illuminated by the strobe appear to float around, because
of loss of a fixation point during off-periods of the light.
The medical literature suggests that epileptic seizures in
susceptible individuals represent the only well-documented health
hazard from exposure to low-frequency intermittent light. The most
sensitive frequency range is from 8 to l6 Hz. Various estimates
indicate that approximately 1.0% of the epileptic population, which
itself constitutes less than 1.0% of the general population, will
experience these "flicker-induced" seizures.
9. THE SKIN
9.1. Anatomy
The skin is normally of less interest than the eye as far as
optical radiation hazards are concerned. However, under certain
conditions, it may be more vulnerable than the eye, which can be
protected by the blink reflex or by eye protectors.
The outermost layer, the stratum corneum or horny layer,
consists of flattened, epidermal cells. They originate in the
germinative layer (a single cell layer of collumnar germinative
basal cells) at the bottom of the epidermis, grow, and are
gradually pushed outward until they die and are flattened to form a
protective layer over the living cells.
The stratum corneum is approximately 10 - 20 µm thick over most
parts of the body, except the soles of the feet and the palms of
the hand, where it is much thicker (500 - 600 µm).
The epidermis is relatively uniform in thickness throughout the
body (50 - 150 µm) and can be separated into a number of layers
with the growing cells in the lowest level toward the basal
membrane.
Melanocytes, specialized cells that produce melanin pigment
granules, are located in the basal layer of the epidermis. The
melanocytes send out dendritic processes that interdigitate within
the keratinocytes. Melanosomes (the pigment granules) are then
transferred into the keratinocytes. The pigment is thus
distributed throughout the epidermis and stratum corneum by
migration of the keratinocytes.
The dermis, or corium, is thicker than the epidermis, and
consists largely of connective tissue which gives the skin its
elasticity and supportive strength. The sweat glands extend into
the corium.
9.2. Body Heat Regulation
The skin plays a major role in the thermoregulatory system of
the human body. At incident irradiances less than those that cause
thermal skin burns, the body can be subjected to heat stress.
Several physical means are employed by the skin for cooling
(conductive, convective, and radiative cooling).
The sweat glands produce sweat, which permits evaporative
cooling as well as conductive cooling. The reflectance of human
skin in the far infrared is very low with a correspondingly high
emissivity for wavelengths in the 8 - 13 µm infrared region. The
high emissivity at these wavelengths permits highly efficient
radiative cooling of the skin at body temperature.
Comparison of the reflectance spectrum of the human skin with
the solar emission spectrum shows a striking similarity. The skin
reflects largely in the visible part and near-infrared parts of the
spectrum, where solar radiation is greatest, and absorbs heavily in
the ultraviolet and far infrared, where there is very little solar
radiation. Any good radiator of infrared energy (a black body)
must have very high absorption, hence very low total reflection.
The skin does indeed have low reflectance in the far infrared, and
seems well adapted to the natural environment. The skin both
reflects direct solar radiation and reradiates internally generated
infrared radiation with the greatest possible efficiency. However,
the human body is less capable of reflecting the infrared radiation
from man-made sources such as fire, or more specifically from
molten steel in a steel mill (Hardy, 1968; Sliney & Freasier, 1973;
Stolwijk, 1980).
9.3. Optical Properties
The stratum corneum strongly absorbs actinic UVR, which causes
sunburn. This layer also strongly absorbs far-infrared radiation.
Melanin granules are small (1 µm diameter) and not only protect the
dermis by absorption of UVR, but also by scattering optical
radiation. Melanin scatters rather than absorbs radiation in the
near-infrared region. For this and other reasons, near-infrared
radiation penetrates deeply into the tissue. Since the index of
refraction of the stratum corneum is about 1.5, the Fresnel
reflective component is somewhat similar to that of glass (Fig. 2).
Optical radiation incident on the skin at grazing angles of
incidence is hardly absorbed at all. The relative effectiveness of
optical radiation in penetrating the epidermis (and dermis) varies
approximately as the cosine of the angle of incidence. Since light
penetrates the outermost layers of the skin, undergoes multiple
scattering, and some light is scattered back out of the skin, the
skin has an appearance that cannot easily be duplicated by a non-
translucent surface (Anderson & Parrish, 1981).
9.4. Penetration Depth and Reflection
Studies of the effects of pulsed visible and IR laser radiation
on pig skin, performed in the 1960s, provided single-wavelength
thresholds for injury for very short-term exposures of the order of
1 ms and 20 ns. For such short durations of exposure, the
influence of heat flow from the absorbing site is not a major
factor. For this reason, these studies aptly showed that the
threshold of injury depended on the reflectance of the skin and the
depth of penetration of the optical radiation into the skin (Fig.
20).
The reflectance of the skin also plays a role in determining
how much radiation can effectively be absorbed. The skin's
spectral reflectance varies with pigmentation and is significant
only in the visible and near-infrared spectrum. The skin's
reflectance at wavelengths of less than 310 nm and above 2.5 µm is
less than 5%.
 It must be remembered that small amounts of optical radiation
penetrate deeply into the body, where it may react with
photosensitive cells. This may give rise to physiological
reactions of great importance, such as circadian rhythms and annual
rhythms. Artificial constant irradiation may suppress the
circadian rhythms, giving rise to health problems.
9.4.1. Injury to the skin
Laser radiation injury to the skin is normally considered less
important than injury to the eye, despite the fact that injury
thresholds for the skin and eye are comparable, except in the
retinal hazard region (400 - 1400 nm). In the IR-C and UV-C
spectral regions, where optical radiation is not focused on the
retina, skin injury thresholds are approximately the same as
corneal injury thresholds. The probability of exposure is greater
for the skin than for the eye, because of the skin's greater
surface area, and yet injury to the eye is still considered to be
of greater significance. For a comparable area of tissue
destruction, the functional losses associated with the eye are more
debilitating than with the skin. Threshold injuries resulting from
the short-term (i.e., less than 10 s) exposure of the skin to far-
infrared (IR-C) and UV-C radiation are also very superficial and
may only involve changes to the outer dead layer - the "horny
layer" - of the skin cells. A temporary injury to the skin may be
painful, if sufficiently severe, but eventually it will heal, often
without any sign of the injury. Burns (thermal injuries) to larger
areas of skin are far more serious, as they may lead to serious
loss of body fluids, toxaemia, and systematic infections.
Thermal injury of the skin has been the subject of many studies
in this century. Hardy et al. (1956) found that severe pain could
always be induced in human skin tissue, when the tissue temperature
was elevated to 45 °C. This temperature also corresponds to an
injury threshold, if the exposure to optical radiation lasts for
many seconds.
Skin injury resulting from momentary but very intense exposures
to optical radiation are generally termed "flash burns". Flash
burns of the skin following exposure to optical radiation in
industry are rare. Most conventional sources such as open-arc
processes and industrial furnaces do not create significant
irradiances in work areas where skin injury could occur
sufficiently fast to preclude a natural protective reaction to the
intense heat. The flash burns that do occur are more often the
result of conductive heating of the skin by exceedingly hot gases
or steam. Though the eye is protected from most flash burns, the
eye lid may be injured with resulting complications in vision. The
threshold depends on the area of irradiated tissue. Heat
conduction in tissue is far more efficient for small than for
larger irradiated areas (e.g., 1 mm2) and exposure to higher levels
of irradiance would be possible before injury occurred. With
extensive irradiation, injury would occur at a far lower level of
irradiance. Hazardous exposure of large areas of skin is unlikely
to be encountered in the normal work environment, as the heat alone
from a source that could produce heat stress due to elevation of
deep body temperature, would require protective measures at lower
irradiance levels.
The threshold of injury obviously depends also on the duration
of exposure. The previously mentioned thresholds are for just one
exposure duration of 0.5 s. For exposures lasting less than 0.5 s
the irradiance required for an injury would significantly increase
as the duration of exposure decreased.
Studies of the process of thermal injury in skin show that the
longer the length of exposure, the lower the temperature required
to coagulate proteins and destroy tissue by elevated temperature.
Fig. 21 shows this time dependence of threshold for white-light,
arc-source burns (upper curve), and for far infrared laser
radiation (lower curve). The explanation for these threshold
differences lies in the fact that thermal injury depends on energy
absorbed per unit volume (or mass) to produce a critical
temperature elevation. Skin reflectance and penetration greatly
influence this absorption. Skin disorders are common and may
change the reaction of the skin to irradiation. Some disorders may
be aggravated while, in others, healing may be enhanced by optical
radiation.
It must be remembered that small amounts of optical radiation
penetrate deeply into the body, where it may react with
photosensitive cells. This may give rise to physiological
reactions of great importance, such as circadian rhythms and annual
rhythms. Artificial constant irradiation may suppress the
circadian rhythms, giving rise to health problems.
9.4.1. Injury to the skin
Laser radiation injury to the skin is normally considered less
important than injury to the eye, despite the fact that injury
thresholds for the skin and eye are comparable, except in the
retinal hazard region (400 - 1400 nm). In the IR-C and UV-C
spectral regions, where optical radiation is not focused on the
retina, skin injury thresholds are approximately the same as
corneal injury thresholds. The probability of exposure is greater
for the skin than for the eye, because of the skin's greater
surface area, and yet injury to the eye is still considered to be
of greater significance. For a comparable area of tissue
destruction, the functional losses associated with the eye are more
debilitating than with the skin. Threshold injuries resulting from
the short-term (i.e., less than 10 s) exposure of the skin to far-
infrared (IR-C) and UV-C radiation are also very superficial and
may only involve changes to the outer dead layer - the "horny
layer" - of the skin cells. A temporary injury to the skin may be
painful, if sufficiently severe, but eventually it will heal, often
without any sign of the injury. Burns (thermal injuries) to larger
areas of skin are far more serious, as they may lead to serious
loss of body fluids, toxaemia, and systematic infections.
Thermal injury of the skin has been the subject of many studies
in this century. Hardy et al. (1956) found that severe pain could
always be induced in human skin tissue, when the tissue temperature
was elevated to 45 °C. This temperature also corresponds to an
injury threshold, if the exposure to optical radiation lasts for
many seconds.
Skin injury resulting from momentary but very intense exposures
to optical radiation are generally termed "flash burns". Flash
burns of the skin following exposure to optical radiation in
industry are rare. Most conventional sources such as open-arc
processes and industrial furnaces do not create significant
irradiances in work areas where skin injury could occur
sufficiently fast to preclude a natural protective reaction to the
intense heat. The flash burns that do occur are more often the
result of conductive heating of the skin by exceedingly hot gases
or steam. Though the eye is protected from most flash burns, the
eye lid may be injured with resulting complications in vision. The
threshold depends on the area of irradiated tissue. Heat
conduction in tissue is far more efficient for small than for
larger irradiated areas (e.g., 1 mm2) and exposure to higher levels
of irradiance would be possible before injury occurred. With
extensive irradiation, injury would occur at a far lower level of
irradiance. Hazardous exposure of large areas of skin is unlikely
to be encountered in the normal work environment, as the heat alone
from a source that could produce heat stress due to elevation of
deep body temperature, would require protective measures at lower
irradiance levels.
The threshold of injury obviously depends also on the duration
of exposure. The previously mentioned thresholds are for just one
exposure duration of 0.5 s. For exposures lasting less than 0.5 s
the irradiance required for an injury would significantly increase
as the duration of exposure decreased.
Studies of the process of thermal injury in skin show that the
longer the length of exposure, the lower the temperature required
to coagulate proteins and destroy tissue by elevated temperature.
Fig. 21 shows this time dependence of threshold for white-light,
arc-source burns (upper curve), and for far infrared laser
radiation (lower curve). The explanation for these threshold
differences lies in the fact that thermal injury depends on energy
absorbed per unit volume (or mass) to produce a critical
temperature elevation. Skin reflectance and penetration greatly
influence this absorption. Skin disorders are common and may
change the reaction of the skin to irradiation. Some disorders may
be aggravated while, in others, healing may be enhanced by optical
radiation.
 9.4.2. The sensation of warmth and heat flow
The sensation of warmth, resulting from the absorption of
radiant energy, normally provides adequate warning for avoiding
action to prevent thermal injury of the skin from almost all
sources except the nuclear fireball and some high-powered, far-
infrared lasers. The spot size dependence of this sensation is
illustrated by irradiating human skin with a beam of CO2-laser
radiation at 10.6 µm. An irradiance of 0.1 W/cm2 produces a
definite sensation of warmth for beam diameters larger than 1 cm.
On the other hand, one-tenth this level (0.01 W/cm2) can readily be
sensed, if the whole body or a larger portion of the body is
exposed. The dependence on the size of the irradiated area results
from conduction of heat away from the absorbing area, thus limitng
surface temperature rise, the sensation of heat being a function
of temperature rise. As noted previously, the skin temperature
elevation required to elicit persistent pain (as well as thermal
injury after several s) is approximately 45 °C (Hardy et al., 1956;
Hardy, 1968).
9.4.3. Thermal injury threshold for the skin
Fig. 22 presents data reported by Rockwell & Goldman (1974),
which illustrate that for some wavelengths, the threshold depends
on skin pigmentation. In the far-infrared, however, all tissue
absorbs heavily, not just melanin pigment granules.
9.4.2. The sensation of warmth and heat flow
The sensation of warmth, resulting from the absorption of
radiant energy, normally provides adequate warning for avoiding
action to prevent thermal injury of the skin from almost all
sources except the nuclear fireball and some high-powered, far-
infrared lasers. The spot size dependence of this sensation is
illustrated by irradiating human skin with a beam of CO2-laser
radiation at 10.6 µm. An irradiance of 0.1 W/cm2 produces a
definite sensation of warmth for beam diameters larger than 1 cm.
On the other hand, one-tenth this level (0.01 W/cm2) can readily be
sensed, if the whole body or a larger portion of the body is
exposed. The dependence on the size of the irradiated area results
from conduction of heat away from the absorbing area, thus limitng
surface temperature rise, the sensation of heat being a function
of temperature rise. As noted previously, the skin temperature
elevation required to elicit persistent pain (as well as thermal
injury after several s) is approximately 45 °C (Hardy et al., 1956;
Hardy, 1968).
9.4.3. Thermal injury threshold for the skin
Fig. 22 presents data reported by Rockwell & Goldman (1974),
which illustrate that for some wavelengths, the threshold depends
on skin pigmentation. In the far-infrared, however, all tissue
absorbs heavily, not just melanin pigment granules.
 9.4.4. Delayed effects
The possibility of adverse effects from repeated or long-term
laser irradiation of the skin is normally discounted, if scarring
does not occur (Goldman et al., 1971). Only UVR has been shown to
cause long-term, delayed effects. These effects are accelerated
skin aging and skin cancer. It is difficult to quantitatively
evaluate the role of UVR in the induction of skin cancer. For
solar radiation, the high-risk wavelengths are around 310 nm. Some
attempts to calculate the dose-effect relationship have now been
made (de Gruijl & van der Leun, 1980). At present, laser safety
standards for exposure of the skin do attempt to take into account
all of these adverse effects.
9.4.5. Ambient environment and heat stress
The temperature of the ambient environment can play a role in
adding to or subtracting from, the temperature rise through
continuous exposure of the skin to optical radiation, particularly
if full-profile exposure is possible. Though full-profile exposure
to laser radiation is uncommon, it is not impossible. Just as
full-profile exposure to far-infrared radiation from furnaces can
cause heat stress, so also can exposure to far-infrared laser
radiation. Radiant absorption is, however, only one factor in
defining heat stress (WHO Scientific Group ..., 1969; Stolwijk,
1980). Increased body temperature due to fever or other causes
generally lowers the irradiance threshold of the effects of optical
radiation.
Man in his natural environment is already exposed to
significant optical radiation out-of-doors. The sun's irradiance
on a clear day may vary from 0.5 to 1.1 kW/m2 (50 to 110 mW/cm2) at
midday. The human body is well designed to reflect direct solar
radiation. In the far-infrared region of the spectrum, the skin's
low reflectance and high emissivity make it possible for the body
to both radiate and strongly absorb 10-µm radiation. The ambient
radiant exitance of surrounding structures and the ground may vary
from 10 to 400 W/m2 (1 to 40 mW/cm2).
9.4.6. UVR effects on the skin
UVR gives rise to acute and delayed visible effects. The acute
effects are erythema (skin reddening), thickening of the stratum
corneum and pigmentation through melanogenesis (Van der Leun,
1965). The delayed effects are accelerated skin aging and
carcinogenesis (Urbach, 1980).
Threshold levels for the acute effects from UV-A are generally
of the order of 1000 times greater than those of UV-B or UV-C. The
effects depend, to a large extent, on skin pigmentation at the time
of exposure. These subjects have been dealt with in detail in the
WHO Environmental Health Criteria document on ultraviolet radiation
(WHO, 1980).
9.4.7. Photosensitization
Light-induced damage to the skin in the presence of certain
chemicals (photosensitizers) may be considered phototoxic if an
allergic mechanism is not ivolved. It can occur in any type of
skin exposed to UVR of the proper wavelength and looks like a
normal erythema. In some cases the reaction may be delayed, but in
general it will appear immediately after exposure. A number of
systemic photosensitizers have been identified and examples are
given in Table 6.
9.4.8. Photoallergy
Photoallergy is an acquired altered capacity of the skin to
react to light (and UVR) alone or in the presence of a
photosensitizer. This subject has been treated in detail in WHO
(1979).
Table 6. Systemic photosensitizers: Chemicals that induce
photosensitivitya
-------------------------------------------------------------------
Uses Name
-------------------------------------------------------------------
Antibacterial nalidixic acid
Anticonvulsant carbamazepine
Antimycotic griseofulvin
-------------------------------------------------------------------
Table 6. (contd.)
-------------------------------------------------------------------
Uses Name
-------------------------------------------------------------------
Artificial sweeteners cyclamates, calcium
cyclamate sodium
cyclohexylsulfamate
Broad spectrum antibiotic antibiotics
Chemotherapeutic, antibacterial sulfonamides
Diuretics, antihypertensive chlorthiazides
Hypoglycaemic or antidiabetic drugs sulfonylurea
In vitiligo for sun tolerance furocoumarins
and increased pigment formation
Laxative triacetyldiphenolisatin
Oral contraceptives estrogens and progesterones
Tranquillizer, nematode infestation phenothiazines
control urinary antiseptic,
antihistamine
Tranquilizer, psychotropic chlordiazepoxide
-------------------------------------------------------------------
a Adapted from: Fitzpatrick et al. (1974).
10. LASER SAFETY STANDARDS: RATIONALE AND CURRENT STANDARDS
10.1. Introduction
Laser safety standards may take several forms. The standard
may be simply a list of guidelines concerning laser operation or
equipment design with no mention of exposure limits or a list of
personnel exposure limits (ELs) or product emission limits. Today,
most safety standards incorporate all of these aspects, to some
extent. This section explains the scientific and philosophical
problems encountered in the development of today's standards. The
distinction between occupational exposure standards and equipment
performance standards will also be discussed.
Exposure limits may be applied in three general categories of
standards, i.e., occupational safety and health standards,
environmental quality standards and equipment performance
standards. ELs for laser radiation for general population and
occupational exposure were developed in many countries during the
late 1960s and throughout the 1970s. A general consensus for many
of these limits can be found in the 1982 draft international
standard of the International Electrotechnical Commission (IEC, in
preparation).
10.2. Laser Hazard Classification
It was recognized during the early development of laser safety
standards that some form of risk classification was necessary.
This resulted from many complaints from research scientists in the
1960s that they were being needlessly constrained in their use of
small He-Ne lasers by safety specialists, who were attempting to
apply guidelines originally drafted for high-power ruby and
neodymium lasers.
Most recent laser safety standards therefore include a hazard
classification scheme to simplify risk evaluation on which to base
control measures (Harlen, 1978).
The safety procedures necessary for any laser operation vary
according to three aspects: (a) the laser hazard classification;
(b) the environment in which the laser is to used, and (c) the
people operating or within the vicinity of the laser beam. Hazard
classification schemes differ only slightly, depending on which
standard is being followed; and a brief explanation of the most
commonly used hazard classification system follows.
Class 1 lasers are the lowest powered lasers. This group is
normally limited to certain gallium-arsenide lasers or enclosed
lasers. These lasers are not considered hazardous, even if the
output laser beam can be collected by 80-mm collecting optics and
concentrated into the pupil of the eye. An infrared or ultraviolet
laser is Class 1 if the radiation concentrated on the skin or eye
will not cause injury within the maximum exposure duration possible
during one day of laser operation. Most lasers are not Class 1,
however, when they are incorporated into consumer or office machine
equipment, the resulting system may become Class 1. If a Class 1
system contains a more dangerous laser, the access panel to it must
be interlocked or contain a warning to alert the user of the
hazardous laser radiation that may be encountered, when the panel
is removed.
Class 2 lasers, often termed "low-power" or "low-risk" laser
systems, are those that are only hazardous if the viewer overcomes
the natural aversion response to bright light and stares
continuously into the source - an unlikely event. This could just
as readily occur by forcing oneself to stare at the sun for more
than a minute or to stare into a film projector source for several
minutes. This hazard, though rare, is as real as eclipse
blindness, hence Class 2 lasers should have a caution label affixed
to indicate that purposeful staring into the laser should be
avoided. Since the aversion response only occurs for light, the
Class 2 category is limited to the visible spectrum from 400 to
700 nm.
Class 3 "moderate-risk" or "medium-power" laser systems are
those that can cause eye injury within the natural aversion
response time, i.e., during the blink reflex (0.25 s). Class 3
lasers do not cause serious skin injury or hazardous diffuse
reflections under normal use. However, these must have danger
labels and the safety precautions required are often considerable.
Class 4 laser systems are the highest powered lasers and
present the greatest potential for injury or combustion of
flammable materials. They may also cause diffuse reflections that
are hazardous to view or induce serious skin injury from direct
exposure. More restrictive control measures and additional
warnings are necessary (Clevet & Mayer, 1980).
Fig. 23 summarizes the most typical classification
scheme. Some standards further refine the above
classification scheme to include special subclasses referred
to as Class 2a, Class 3a, and Class 4a. Relaxed restrictions
may apply to these subclasses.
9.4.4. Delayed effects
The possibility of adverse effects from repeated or long-term
laser irradiation of the skin is normally discounted, if scarring
does not occur (Goldman et al., 1971). Only UVR has been shown to
cause long-term, delayed effects. These effects are accelerated
skin aging and skin cancer. It is difficult to quantitatively
evaluate the role of UVR in the induction of skin cancer. For
solar radiation, the high-risk wavelengths are around 310 nm. Some
attempts to calculate the dose-effect relationship have now been
made (de Gruijl & van der Leun, 1980). At present, laser safety
standards for exposure of the skin do attempt to take into account
all of these adverse effects.
9.4.5. Ambient environment and heat stress
The temperature of the ambient environment can play a role in
adding to or subtracting from, the temperature rise through
continuous exposure of the skin to optical radiation, particularly
if full-profile exposure is possible. Though full-profile exposure
to laser radiation is uncommon, it is not impossible. Just as
full-profile exposure to far-infrared radiation from furnaces can
cause heat stress, so also can exposure to far-infrared laser
radiation. Radiant absorption is, however, only one factor in
defining heat stress (WHO Scientific Group ..., 1969; Stolwijk,
1980). Increased body temperature due to fever or other causes
generally lowers the irradiance threshold of the effects of optical
radiation.
Man in his natural environment is already exposed to
significant optical radiation out-of-doors. The sun's irradiance
on a clear day may vary from 0.5 to 1.1 kW/m2 (50 to 110 mW/cm2) at
midday. The human body is well designed to reflect direct solar
radiation. In the far-infrared region of the spectrum, the skin's
low reflectance and high emissivity make it possible for the body
to both radiate and strongly absorb 10-µm radiation. The ambient
radiant exitance of surrounding structures and the ground may vary
from 10 to 400 W/m2 (1 to 40 mW/cm2).
9.4.6. UVR effects on the skin
UVR gives rise to acute and delayed visible effects. The acute
effects are erythema (skin reddening), thickening of the stratum
corneum and pigmentation through melanogenesis (Van der Leun,
1965). The delayed effects are accelerated skin aging and
carcinogenesis (Urbach, 1980).
Threshold levels for the acute effects from UV-A are generally
of the order of 1000 times greater than those of UV-B or UV-C. The
effects depend, to a large extent, on skin pigmentation at the time
of exposure. These subjects have been dealt with in detail in the
WHO Environmental Health Criteria document on ultraviolet radiation
(WHO, 1980).
9.4.7. Photosensitization
Light-induced damage to the skin in the presence of certain
chemicals (photosensitizers) may be considered phototoxic if an
allergic mechanism is not ivolved. It can occur in any type of
skin exposed to UVR of the proper wavelength and looks like a
normal erythema. In some cases the reaction may be delayed, but in
general it will appear immediately after exposure. A number of
systemic photosensitizers have been identified and examples are
given in Table 6.
9.4.8. Photoallergy
Photoallergy is an acquired altered capacity of the skin to
react to light (and UVR) alone or in the presence of a
photosensitizer. This subject has been treated in detail in WHO
(1979).
Table 6. Systemic photosensitizers: Chemicals that induce
photosensitivitya
-------------------------------------------------------------------
Uses Name
-------------------------------------------------------------------
Antibacterial nalidixic acid
Anticonvulsant carbamazepine
Antimycotic griseofulvin
-------------------------------------------------------------------
Table 6. (contd.)
-------------------------------------------------------------------
Uses Name
-------------------------------------------------------------------
Artificial sweeteners cyclamates, calcium
cyclamate sodium
cyclohexylsulfamate
Broad spectrum antibiotic antibiotics
Chemotherapeutic, antibacterial sulfonamides
Diuretics, antihypertensive chlorthiazides
Hypoglycaemic or antidiabetic drugs sulfonylurea
In vitiligo for sun tolerance furocoumarins
and increased pigment formation
Laxative triacetyldiphenolisatin
Oral contraceptives estrogens and progesterones
Tranquillizer, nematode infestation phenothiazines
control urinary antiseptic,
antihistamine
Tranquilizer, psychotropic chlordiazepoxide
-------------------------------------------------------------------
a Adapted from: Fitzpatrick et al. (1974).
10. LASER SAFETY STANDARDS: RATIONALE AND CURRENT STANDARDS
10.1. Introduction
Laser safety standards may take several forms. The standard
may be simply a list of guidelines concerning laser operation or
equipment design with no mention of exposure limits or a list of
personnel exposure limits (ELs) or product emission limits. Today,
most safety standards incorporate all of these aspects, to some
extent. This section explains the scientific and philosophical
problems encountered in the development of today's standards. The
distinction between occupational exposure standards and equipment
performance standards will also be discussed.
Exposure limits may be applied in three general categories of
standards, i.e., occupational safety and health standards,
environmental quality standards and equipment performance
standards. ELs for laser radiation for general population and
occupational exposure were developed in many countries during the
late 1960s and throughout the 1970s. A general consensus for many
of these limits can be found in the 1982 draft international
standard of the International Electrotechnical Commission (IEC, in
preparation).
10.2. Laser Hazard Classification
It was recognized during the early development of laser safety
standards that some form of risk classification was necessary.
This resulted from many complaints from research scientists in the
1960s that they were being needlessly constrained in their use of
small He-Ne lasers by safety specialists, who were attempting to
apply guidelines originally drafted for high-power ruby and
neodymium lasers.
Most recent laser safety standards therefore include a hazard
classification scheme to simplify risk evaluation on which to base
control measures (Harlen, 1978).
The safety procedures necessary for any laser operation vary
according to three aspects: (a) the laser hazard classification;
(b) the environment in which the laser is to used, and (c) the
people operating or within the vicinity of the laser beam. Hazard
classification schemes differ only slightly, depending on which
standard is being followed; and a brief explanation of the most
commonly used hazard classification system follows.
Class 1 lasers are the lowest powered lasers. This group is
normally limited to certain gallium-arsenide lasers or enclosed
lasers. These lasers are not considered hazardous, even if the
output laser beam can be collected by 80-mm collecting optics and
concentrated into the pupil of the eye. An infrared or ultraviolet
laser is Class 1 if the radiation concentrated on the skin or eye
will not cause injury within the maximum exposure duration possible
during one day of laser operation. Most lasers are not Class 1,
however, when they are incorporated into consumer or office machine
equipment, the resulting system may become Class 1. If a Class 1
system contains a more dangerous laser, the access panel to it must
be interlocked or contain a warning to alert the user of the
hazardous laser radiation that may be encountered, when the panel
is removed.
Class 2 lasers, often termed "low-power" or "low-risk" laser
systems, are those that are only hazardous if the viewer overcomes
the natural aversion response to bright light and stares
continuously into the source - an unlikely event. This could just
as readily occur by forcing oneself to stare at the sun for more
than a minute or to stare into a film projector source for several
minutes. This hazard, though rare, is as real as eclipse
blindness, hence Class 2 lasers should have a caution label affixed
to indicate that purposeful staring into the laser should be
avoided. Since the aversion response only occurs for light, the
Class 2 category is limited to the visible spectrum from 400 to
700 nm.
Class 3 "moderate-risk" or "medium-power" laser systems are
those that can cause eye injury within the natural aversion
response time, i.e., during the blink reflex (0.25 s). Class 3
lasers do not cause serious skin injury or hazardous diffuse
reflections under normal use. However, these must have danger
labels and the safety precautions required are often considerable.
Class 4 laser systems are the highest powered lasers and
present the greatest potential for injury or combustion of
flammable materials. They may also cause diffuse reflections that
are hazardous to view or induce serious skin injury from direct
exposure. More restrictive control measures and additional
warnings are necessary (Clevet & Mayer, 1980).
Fig. 23 summarizes the most typical classification
scheme. Some standards further refine the above
classification scheme to include special subclasses referred
to as Class 2a, Class 3a, and Class 4a. Relaxed restrictions
may apply to these subclasses.
 11. EXPOSURE LIMITS
11.1. Rationale
Exposure limits for lasers and optical radiation cover a wide
range of wavelengths and exposure conditions, and biological
effects may apply to both the eye and skin. For this reason, no
single rationale can apply to all of the specific ELs. It is first
important to distinguish between acute and chronic (or delayed)
effects. For acute effects, thresholds exist and statistical
(probit analysis) techniques can indicate this threshold with a
degree of uncertainty. The method of assessing the acute effect
may not always be the most sensitive, but is often chosen for
reasons of simplicity and repeatability. However, this approach is
feasible only because the relationship between this assessment
threshold and the onset of irreversible damage is known from more
rigorous studies using the most sensitive techniques for damage
assessment. While a threshold for most chronic effects can be
expected on theoretical grounds, this threshold can best be
estimated from careful evaluation of epidemiological data. ELs are
set by considering both types of effects and the degree of
uncertainty in thresholds.
Scientists working in the field of ionizing radiation are used
to the problems of cumulative doses and total lifetime exposure.
In describing the adverse biological effects of optical radiation
at wavelengths greater than 320 nm, few scientists would argue that
a linear hypothesis applies with total integration of the lifetime
exposure.
Optical radiation is usually absorbed in a thin layer of tissue
and its effects are thermal in nature, except for the ultraviolet
and visible photochemical processes. For both of these acute
effects, there is a definite threshold; that is, an exposure level
exists below which no adverse change will occur and no real risk
exists. Of course, the threshold can vary with the individual and
with environmental conditions. However, if the safety level is set
well below these variations, then the exposure conditions are not
hazardous.
To establish a rationale for developing exposure limits from
the biological data requires careful analysis of the spread of the
empirical data. These include the variables influencing potential
for injury in exposed individuals, the increase in severity of
injury for suprathreshold exposure doses, and the degree of repair
of injury.
The accuracy of available measuring instruments and the desire
for simplicity in expressing the limits have also influenced the
exposure limits. It is difficult to inter-relate all these
factors; however, most specialists agree on the final limits, even
though they may have derived them in different ways.
Separate high risk occupational limits - in contrast to
exposure limits for the general population - have not been
developed. Unlike ionizing radiation, there has been little debate
as to whether a threshold of injury actually exists. However,
there can be a debate concerning the exact "threshold values" for
specific wavelengths and exposure durations. UV-B and UV-C laser
radiation could, in theory, have delayed effects with no real
threshold, but has nevertheless been treated like longer wavelength
laser radiation. Long-term effects of low-level exposure have been
indicted as a possible contributing agents in senile degenerative
processes in the retina (Marshall, 1978; Young, 1981). If true, a
simple threshold for these effects probably does not exist.
11.2. Assessment of the "Safety Factor"
It is very difficult to decide on the margin that should be
introduced, to account for individual variation in experimental
error, in deriving the ELs. This margin is sometimes loosely
termed the safety factor; however, this is not correct. The
threshold of injury is actually the result of considering the
probit analysis of many data points.
The most reliable statistical method for describing any
biological threshold is probit analysis. One point on the curve,
the 50% damage probability, is often assigned a special
significance. This point is known as the ED50 and is the exposure
dose required, for example, to produce an ophthalmoscopically
visible (or an otherwise measurable) lesion in 50% of the exposures
in a group of animals or in a single animal, where several
exposures have taken place. The ED50 point has in the past been
termed a threshold point by some investigators, though clearly the
use of the term threshold in describing a 50% probability of injury
seems rather inappropriate. In toxicological studies of the
effects of chemicals on biological systems, the term threshold has
often been used to define a 10% probability of a biological
response.
Probit analysis is a powerful tool in determining safety
information but was not originally applied, e.g., to retinal damage
from laser exposure. In the early studies on retinal damage, the
experimental design was usually such as to facilitate calculations
of only the ED50 point.
When the data are plotted on probit paper, a line results that
can easily be extrapolated to the clinical damage probability.
Indeed, studies should be designed to give the slope with maximum
precision. For this, two points at low and high probability, e.g.,
the 20% and 80% probability points are more important than the ED50
point. Once this information is available together with the
criterion for injury and the accepted degree of safety, it is
possible to determine the exposure limit. Present-day laser ELs
are typically a factor of 5 - 20 below an ED50 for observable acute
injury, this ratio varying as a result of functional-loss,
histological, and suprathreshold-severity studies.
11.3. Environmental Considerations
Though laboratory studies of the adverse effects of optical
radiation provide the basic insight into thresholds, locations, and
mechanisms of tissue injury, it is difficult to extrapolate these
findings to protection standards. Of special importance, is the
separation of acute temporary effects from those leading to delayed
permanent detrimental effects.
In this regard, it will also be necessary to take the actual
exposure conditions of man into consideration - both from natural
environmental sources or from artificial sources. It must be
remembered, for instance, that terrestrial solar radiation changes,
both in total irradiance and in spectral distribution, throughout
the day. Furthermore, the direction of illumination is of great
importance because of the reflection from the cornea, as seen in
Fig. 24.
11. EXPOSURE LIMITS
11.1. Rationale
Exposure limits for lasers and optical radiation cover a wide
range of wavelengths and exposure conditions, and biological
effects may apply to both the eye and skin. For this reason, no
single rationale can apply to all of the specific ELs. It is first
important to distinguish between acute and chronic (or delayed)
effects. For acute effects, thresholds exist and statistical
(probit analysis) techniques can indicate this threshold with a
degree of uncertainty. The method of assessing the acute effect
may not always be the most sensitive, but is often chosen for
reasons of simplicity and repeatability. However, this approach is
feasible only because the relationship between this assessment
threshold and the onset of irreversible damage is known from more
rigorous studies using the most sensitive techniques for damage
assessment. While a threshold for most chronic effects can be
expected on theoretical grounds, this threshold can best be
estimated from careful evaluation of epidemiological data. ELs are
set by considering both types of effects and the degree of
uncertainty in thresholds.
Scientists working in the field of ionizing radiation are used
to the problems of cumulative doses and total lifetime exposure.
In describing the adverse biological effects of optical radiation
at wavelengths greater than 320 nm, few scientists would argue that
a linear hypothesis applies with total integration of the lifetime
exposure.
Optical radiation is usually absorbed in a thin layer of tissue
and its effects are thermal in nature, except for the ultraviolet
and visible photochemical processes. For both of these acute
effects, there is a definite threshold; that is, an exposure level
exists below which no adverse change will occur and no real risk
exists. Of course, the threshold can vary with the individual and
with environmental conditions. However, if the safety level is set
well below these variations, then the exposure conditions are not
hazardous.
To establish a rationale for developing exposure limits from
the biological data requires careful analysis of the spread of the
empirical data. These include the variables influencing potential
for injury in exposed individuals, the increase in severity of
injury for suprathreshold exposure doses, and the degree of repair
of injury.
The accuracy of available measuring instruments and the desire
for simplicity in expressing the limits have also influenced the
exposure limits. It is difficult to inter-relate all these
factors; however, most specialists agree on the final limits, even
though they may have derived them in different ways.
Separate high risk occupational limits - in contrast to
exposure limits for the general population - have not been
developed. Unlike ionizing radiation, there has been little debate
as to whether a threshold of injury actually exists. However,
there can be a debate concerning the exact "threshold values" for
specific wavelengths and exposure durations. UV-B and UV-C laser
radiation could, in theory, have delayed effects with no real
threshold, but has nevertheless been treated like longer wavelength
laser radiation. Long-term effects of low-level exposure have been
indicted as a possible contributing agents in senile degenerative
processes in the retina (Marshall, 1978; Young, 1981). If true, a
simple threshold for these effects probably does not exist.
11.2. Assessment of the "Safety Factor"
It is very difficult to decide on the margin that should be
introduced, to account for individual variation in experimental
error, in deriving the ELs. This margin is sometimes loosely
termed the safety factor; however, this is not correct. The
threshold of injury is actually the result of considering the
probit analysis of many data points.
The most reliable statistical method for describing any
biological threshold is probit analysis. One point on the curve,
the 50% damage probability, is often assigned a special
significance. This point is known as the ED50 and is the exposure
dose required, for example, to produce an ophthalmoscopically
visible (or an otherwise measurable) lesion in 50% of the exposures
in a group of animals or in a single animal, where several
exposures have taken place. The ED50 point has in the past been
termed a threshold point by some investigators, though clearly the
use of the term threshold in describing a 50% probability of injury
seems rather inappropriate. In toxicological studies of the
effects of chemicals on biological systems, the term threshold has
often been used to define a 10% probability of a biological
response.
Probit analysis is a powerful tool in determining safety
information but was not originally applied, e.g., to retinal damage
from laser exposure. In the early studies on retinal damage, the
experimental design was usually such as to facilitate calculations
of only the ED50 point.
When the data are plotted on probit paper, a line results that
can easily be extrapolated to the clinical damage probability.
Indeed, studies should be designed to give the slope with maximum
precision. For this, two points at low and high probability, e.g.,
the 20% and 80% probability points are more important than the ED50
point. Once this information is available together with the
criterion for injury and the accepted degree of safety, it is
possible to determine the exposure limit. Present-day laser ELs
are typically a factor of 5 - 20 below an ED50 for observable acute
injury, this ratio varying as a result of functional-loss,
histological, and suprathreshold-severity studies.
11.3. Environmental Considerations
Though laboratory studies of the adverse effects of optical
radiation provide the basic insight into thresholds, locations, and
mechanisms of tissue injury, it is difficult to extrapolate these
findings to protection standards. Of special importance, is the
separation of acute temporary effects from those leading to delayed
permanent detrimental effects.
In this regard, it will also be necessary to take the actual
exposure conditions of man into consideration - both from natural
environmental sources or from artificial sources. It must be
remembered, for instance, that terrestrial solar radiation changes,
both in total irradiance and in spectral distribution, throughout
the day. Furthermore, the direction of illumination is of great
importance because of the reflection from the cornea, as seen in
Fig. 24.
 11.4. Limiting Apertures
One difficulty in developing ELs is the specification of the
limiting aperture over which the values must be either measured or
calculated. For the skin, where no self-focusing effect takes
place, the smallest feasible aperture is most desirable.
Unfortunately, the smaller the aperture, the higher the sensitivity
required for the measuring instrument and the greater the
inaccuracy that will result from calibration problems associated
with diffraction and other optical effects. Since various
biological effects are influenced differently by the size of an
incident beam, the limiting aperture varies for different
conditions.
11.4.1. The 1-mm aperture
A 1-mm aperture has been typically considered the smallest
practical aperture size for specifying ELs. Under continuous
exposure conditions, heat flow and scattering within the layers of
the skin tend to eliminate any adverse effects from hot spots
smaller than 1 mm in diameter.
11.4.2. The 11-mm aperture
Wavelengths greater than 0.1 mm present a further difficulty.
At these far-infrared, submillimetre wavelengths, a 1-mm aperture
creates significant diffraction effects and calibration becomes a
problem. Hot spots predicted by physical optics are larger than at
shorter wavelengths. For these reasons, a 1-cm square, or 11-mm
diameter (1 cm2) circular aperture has typically been chosen as the
limiting aperture for wavelengths between 0.1 mm and 1 mm.
11.4.3. The 7-mm aperture
For ocular ELs in the "retinal hazard region", from
approximately 400 nm to 1400 nm, the averaging (sampling) aperture
is determined by the pupil of the eye. A pupil size of 7-mm has
been decided as typical, though not without a great deal of debate.
11.4.4. The 80-mm aperture
A still larger measuring aperture of 80 mm is conventionally
used for power and energy measurements to account for intrabeam
viewing conditions with optical telescopes or binoculars.
11.5. Spectral Dependence of Exposure Limits
Eye and skin injury thresholds vary considerably with
wavelength. To establish the spectral dependence of ELs, it is
generally accepted that the biological data can only be followed
approximately. The ELs have been adjusted for variation in
wavelength, but do not precisely follow the empirical biological
data. Fig. 25 shows an example of theoretical variation of
susceptibility modified to provide a spectral correction factor,
useful for calculating the EL.
Fig. 25 provides the reciprocal of the product of the relative
spectral transmission of the ocular media with the retinal
absorption (Fig. 17). This indicates the relative effectiveness of
different wavelengths for causing retinal thermal injury. However,
this curve still does not show the relative spectral hazard to the
lens of the eye in the near infrared. Also plotted in this graph
is the spectral modification factor used for pulsed retinal
exposure limits in the American National Standards Institute
standard (ANSI, 1980). This modification factor is used for other
limits for protection against thermal injury. Because of variation
of threshold with image size and variation of image size with
wavelength, a further increase in the ratio between IR-A and
visible ELs is given in the ANSI Z-136.1 standard for IR-A
wavelengths between 1050 nm and 1400 nm, but only for durations of
exposure of less than 0.05 ms.
11.4. Limiting Apertures
One difficulty in developing ELs is the specification of the
limiting aperture over which the values must be either measured or
calculated. For the skin, where no self-focusing effect takes
place, the smallest feasible aperture is most desirable.
Unfortunately, the smaller the aperture, the higher the sensitivity
required for the measuring instrument and the greater the
inaccuracy that will result from calibration problems associated
with diffraction and other optical effects. Since various
biological effects are influenced differently by the size of an
incident beam, the limiting aperture varies for different
conditions.
11.4.1. The 1-mm aperture
A 1-mm aperture has been typically considered the smallest
practical aperture size for specifying ELs. Under continuous
exposure conditions, heat flow and scattering within the layers of
the skin tend to eliminate any adverse effects from hot spots
smaller than 1 mm in diameter.
11.4.2. The 11-mm aperture
Wavelengths greater than 0.1 mm present a further difficulty.
At these far-infrared, submillimetre wavelengths, a 1-mm aperture
creates significant diffraction effects and calibration becomes a
problem. Hot spots predicted by physical optics are larger than at
shorter wavelengths. For these reasons, a 1-cm square, or 11-mm
diameter (1 cm2) circular aperture has typically been chosen as the
limiting aperture for wavelengths between 0.1 mm and 1 mm.
11.4.3. The 7-mm aperture
For ocular ELs in the "retinal hazard region", from
approximately 400 nm to 1400 nm, the averaging (sampling) aperture
is determined by the pupil of the eye. A pupil size of 7-mm has
been decided as typical, though not without a great deal of debate.
11.4.4. The 80-mm aperture
A still larger measuring aperture of 80 mm is conventionally
used for power and energy measurements to account for intrabeam
viewing conditions with optical telescopes or binoculars.
11.5. Spectral Dependence of Exposure Limits
Eye and skin injury thresholds vary considerably with
wavelength. To establish the spectral dependence of ELs, it is
generally accepted that the biological data can only be followed
approximately. The ELs have been adjusted for variation in
wavelength, but do not precisely follow the empirical biological
data. Fig. 25 shows an example of theoretical variation of
susceptibility modified to provide a spectral correction factor,
useful for calculating the EL.
Fig. 25 provides the reciprocal of the product of the relative
spectral transmission of the ocular media with the retinal
absorption (Fig. 17). This indicates the relative effectiveness of
different wavelengths for causing retinal thermal injury. However,
this curve still does not show the relative spectral hazard to the
lens of the eye in the near infrared. Also plotted in this graph
is the spectral modification factor used for pulsed retinal
exposure limits in the American National Standards Institute
standard (ANSI, 1980). This modification factor is used for other
limits for protection against thermal injury. Because of variation
of threshold with image size and variation of image size with
wavelength, a further increase in the ratio between IR-A and
visible ELs is given in the ANSI Z-136.1 standard for IR-A
wavelengths between 1050 nm and 1400 nm, but only for durations of
exposure of less than 0.05 ms.
 11.6. Repetitively Pulsed Laser Exposure
The values in the present standards for repetitive ocular
exposure have been based on limited data and developed from purely
empirical extrapolations. The cumulative effect of repetitive
pulses was considered to be a function of the duration of the
individual pulse in a pulse train. For short pulses (duration less
than 10 µs), the EL for a single pulse was multiplied by a
correction factor to provide a reduced exposure on a per-pulse
basis. This value was then compared with the EL values for the
total energy and for a total exposure of the duration of the entire
train of exposures, to determine which limit would apply. For a
train of pulses, where the individual pulse duration exceeded 10
ms, a criterion based on total on-time Tt of the train of pulses
was applied to each individual pulse. This resulted in a reduced
EL for each pulse. However, all of these approaches were based
largely on studies in which the eye of the rhesus monkey was
exposed to single pulses of "minimal image size".
More recent studies (Greiss et al., 1980) suggest that the
pulse thresholds add as a function of N-¨ for small image sizes,
but not for large image sizes. The letter N refers to the number
of pulses in the train.
11.7. Restrictions for Special Applications (Class 3a)
The low risk of Class 2 lasers differs little from the lack of
risk of Class 1 lasers, in practice. Class 2 lasers emit a power
of 0.4 µW - 1 mW, a light level difficult to stare into because of
the aversion response. The risk increases significantly, when the
eye is unable to protect itself, as occurs when a visible laser
beam irradiance exceeds 2.5 mW/cm2 (i.e., a total of 1 mW entering
the 7-mm pupil of the eye by either unaided or optically-aided
viewing). The laser classification denotes risk, when the laser is
viewed under worse-case conditions. In practice, if worst-case
conditions are seldom experienced, further relaxations can be
applied for certain limited applications. An example of this is
the 5 mW limit applied to the total power for surveying/ alignment
of lasers. This recognizes that "moderate-risk" (Class 3) lasers
are sometimes needed in this application but that the benefit in
this application outweighs the moderate risk of the 1-5 mW visible
laser group (US DHEW, 1979).
11.8. Present Standards of Exposure
11.8.1. Laser standards
A number of national and international standards have been
promulgated that show only minor differences, some of which may be
partly resolved, when future editions of the American National
Standards Institute (ANSI), British Standards Institute (BSI),
GOST, and the International Electrotechnical Commission (IEC)
appear.
Tables 7-11 present the most recent set of occupational ELs,
those promulgated by the ANSI Z-136.1 Standard (ANSI, 1980) and the
threshold limit values (TLVs) of the American Conference of
Governmental Industrial Hygienists (ACGIH, 1981), those given in
the draft International Electrotechnical Commission standard (IEC,
in preparation), and the values mentioned as "best available" in
Suess, ed. (1982).
11.8.1.1. Exposure limits
The tables and figures presented in this section are from the
ACGIH booklet Threshold limit values for chemical substances and
physical agents in the workroom environment with intended changes
for 1981 (ACGIH, 1981). For this criteria document, the term
"exposure limit" is used.
While the concept of an EL (or TLV) is that neither the general
population nor workers should be intentionally exposed above the
limit, accidental over-exposure may not always result in injury.
It is helpful to quote the TLV preamble given by ACGIH: "The
threshold limit values are for exposure to laser radiation under
conditions to which nearly all workers may be exposed without
adverse effects. The values should be used as guides in the
control of exposures and should not be regarded as fine lines
between safe and dangerous levels. They are based on the best
available information from experimental studies".
11.8.1.2. Repetitively pulsed lasers
Since the additive effects of multiple pulses are not fully
understood, caution must be used in the evaluation of such
exposures. The exposure limits for irradiance or radiant exposure
in multiple pulse trains have the following limitations:
(a) The exposure from any single pulse in the train is limited to
the exposure limit for a single comparable pulse;
(b) The average irradiance for a group of pulses is limited to the
EL (as given in Tables 7, 8, and 9) of a single pulse of the
same duration as the entire pulse group;
(c) When the instantaneous Pulse Repetition Frequency (PRF) of any
pulses within a train exceeds 1, the EL, applicable to each
pulse, is reduced by a factor (Cp), as shown in Fig. 26 for
pulse durations of less than 10-5 s. For pulses of greater
duration, the EL of a pulse in the train is found by dividing
the EL of a longer pulse of duration Nt by N, where N is the
number of pulses in the train, t is the duration of a single
pulse in the train, and the EL of Nt is the exposure limit of
one pulse having a duration equal to Nt s. The "pulse"
duration Nt is known as the TOTP (total on time pulse), Tt in
the ANSI standard. For a short group of N pulses, the reduced
EL will not be less than the single pulse EL divided by N.
Repeated exposures at repetition rates of less than 1 Hz should
be considered additive over a 24-h period.
11.6. Repetitively Pulsed Laser Exposure
The values in the present standards for repetitive ocular
exposure have been based on limited data and developed from purely
empirical extrapolations. The cumulative effect of repetitive
pulses was considered to be a function of the duration of the
individual pulse in a pulse train. For short pulses (duration less
than 10 µs), the EL for a single pulse was multiplied by a
correction factor to provide a reduced exposure on a per-pulse
basis. This value was then compared with the EL values for the
total energy and for a total exposure of the duration of the entire
train of exposures, to determine which limit would apply. For a
train of pulses, where the individual pulse duration exceeded 10
ms, a criterion based on total on-time Tt of the train of pulses
was applied to each individual pulse. This resulted in a reduced
EL for each pulse. However, all of these approaches were based
largely on studies in which the eye of the rhesus monkey was
exposed to single pulses of "minimal image size".
More recent studies (Greiss et al., 1980) suggest that the
pulse thresholds add as a function of N-¨ for small image sizes,
but not for large image sizes. The letter N refers to the number
of pulses in the train.
11.7. Restrictions for Special Applications (Class 3a)
The low risk of Class 2 lasers differs little from the lack of
risk of Class 1 lasers, in practice. Class 2 lasers emit a power
of 0.4 µW - 1 mW, a light level difficult to stare into because of
the aversion response. The risk increases significantly, when the
eye is unable to protect itself, as occurs when a visible laser
beam irradiance exceeds 2.5 mW/cm2 (i.e., a total of 1 mW entering
the 7-mm pupil of the eye by either unaided or optically-aided
viewing). The laser classification denotes risk, when the laser is
viewed under worse-case conditions. In practice, if worst-case
conditions are seldom experienced, further relaxations can be
applied for certain limited applications. An example of this is
the 5 mW limit applied to the total power for surveying/ alignment
of lasers. This recognizes that "moderate-risk" (Class 3) lasers
are sometimes needed in this application but that the benefit in
this application outweighs the moderate risk of the 1-5 mW visible
laser group (US DHEW, 1979).
11.8. Present Standards of Exposure
11.8.1. Laser standards
A number of national and international standards have been
promulgated that show only minor differences, some of which may be
partly resolved, when future editions of the American National
Standards Institute (ANSI), British Standards Institute (BSI),
GOST, and the International Electrotechnical Commission (IEC)
appear.
Tables 7-11 present the most recent set of occupational ELs,
those promulgated by the ANSI Z-136.1 Standard (ANSI, 1980) and the
threshold limit values (TLVs) of the American Conference of
Governmental Industrial Hygienists (ACGIH, 1981), those given in
the draft International Electrotechnical Commission standard (IEC,
in preparation), and the values mentioned as "best available" in
Suess, ed. (1982).
11.8.1.1. Exposure limits
The tables and figures presented in this section are from the
ACGIH booklet Threshold limit values for chemical substances and
physical agents in the workroom environment with intended changes
for 1981 (ACGIH, 1981). For this criteria document, the term
"exposure limit" is used.
While the concept of an EL (or TLV) is that neither the general
population nor workers should be intentionally exposed above the
limit, accidental over-exposure may not always result in injury.
It is helpful to quote the TLV preamble given by ACGIH: "The
threshold limit values are for exposure to laser radiation under
conditions to which nearly all workers may be exposed without
adverse effects. The values should be used as guides in the
control of exposures and should not be regarded as fine lines
between safe and dangerous levels. They are based on the best
available information from experimental studies".
11.8.1.2. Repetitively pulsed lasers
Since the additive effects of multiple pulses are not fully
understood, caution must be used in the evaluation of such
exposures. The exposure limits for irradiance or radiant exposure
in multiple pulse trains have the following limitations:
(a) The exposure from any single pulse in the train is limited to
the exposure limit for a single comparable pulse;
(b) The average irradiance for a group of pulses is limited to the
EL (as given in Tables 7, 8, and 9) of a single pulse of the
same duration as the entire pulse group;
(c) When the instantaneous Pulse Repetition Frequency (PRF) of any
pulses within a train exceeds 1, the EL, applicable to each
pulse, is reduced by a factor (Cp), as shown in Fig. 26 for
pulse durations of less than 10-5 s. For pulses of greater
duration, the EL of a pulse in the train is found by dividing
the EL of a longer pulse of duration Nt by N, where N is the
number of pulses in the train, t is the duration of a single
pulse in the train, and the EL of Nt is the exposure limit of
one pulse having a duration equal to Nt s. The "pulse"
duration Nt is known as the TOTP (total on time pulse), Tt in
the ANSI standard. For a short group of N pulses, the reduced
EL will not be less than the single pulse EL divided by N.
Repeated exposures at repetition rates of less than 1 Hz should
be considered additive over a 24-h period.
 Table 7. Exposure limits for direct ocular exposures (intrabeam viewing)
from a laser beam
-------------------------------------------------------------------------
Spectral Wavelength Exposure time (t) Exposure limits
region seconds (s)
-------------------------------------------------------------------------
UVC 200 nm to 280 nm 10-9 to 3 x 104 3 mJ/cm2
UVB 280 nm to 302 nm 10-9 to 3 x 104 3 mJ/cm2
303 nm 10-9 to 3 x 104 4 mJ/cm2
304 nm 10-9 to 3 x 104 6 mJ/cm2
305 nm 10-9 to 3 x 104 10 mJ/cm2
306 nm 10-9 to 3 x 104 16 mJ/cm2 )
307 nm 10-9 to 3 x 104 25 mJ/cm2 )
308 nm 10-9 to 3 x 104 40 mJ/cm2 ) not to
309 nm 10-9 to 3 x 104 63 mJ/cm2 ) exceed
310 nm 10-9 to 3 x 104 100 mJ/cm2) 0.56t¨
311 nm 10-9 to 3 x 104 160 mJ/cm2) J/cm2
312 nm 10-9 to 3 x 104 250 mJ/cm2)
313 nm 10-9 to 3 x 104 400 mJ/cm2)
314 nm 10-9 to 3 x 104 630 mJ/cm2)
315 nm 10-9 to 3 x 104 1.0 J/cm2)
315 nm to 400 nm 10-9 to 10 0.56t1/4 J/cm2
UVA 315 nm to 400 nm 10 to 103 1.0 J/cm2
315 nm to 400 nm 103 to 3 x 104 1.0 mW/cm2
-------------------------------------------------------------------------
Table 7 (contd.)
-------------------------------------------------------------------------
Spectral Wavelength Exposure time (t) Exposure limits
region seconds (s)
-------------------------------------------------------------------------
Light 400 nm to 700 nm 10-9 to 1.8 x 10-5 5 x 10-7J/cm2
400 nm to 700 nm 1.8 x 10-5 to 10 1.8(t/4 ´t) mJ/cm2
400 nm to 549 nm 10 to 104 10 mJ/cm2
500 nm to 700 nm 10 to T1 1.8(t/4 ´t) mJ/cm2
550 nm to 700 nm T1 to 104 10CB mJ/cm2
400 nm to 700 nm 104 to 3 x 104 CB µW/cm2
IR-A 700 nm to 1049 nm 10-9 to 1.8 x 10-5 5 CA x 10-7 J/cm2
700 nm to 1049 nm 1.8 x 10-5 to 103 1.8CA(t/4 ´/t) mJ/cm2
1050 nm to 1400 nm 10-9 to 5 x 10-4 5 x 10-6 J/cm2
1050 nm to 1400 nm 5 x 10-4 to 103 9(t/4 ´/t) mJ/cm2
700 nm to 1400 nm 103 to 3 x 104 320 CA µW/cm2
IR-B & C 1.4 µm to 103 µm 10-9 to 10-7 10-2 J/cm2
1.4 µm to 103 µm 10-7 to 10 0.56 4 ´/t) J/cm2
1.4 µm to 103 µm 10 to 3 x 104 0.1 W/cm2
-------------------------------------------------------------------------
The formula for Correction Factor CA (Fig. 25) is
CA = 1 for wavelength (lambda) of 400 nm - 700 nm;
CA = 10(0.002[lambda-700 nm]) for 700 nm < lambda < 1050 nm; and
CA = 5 for 1050 < lambda < 1400 nm.
CB = 1 for lambda = 400 - 550 nm;
CB = 10(0.015[lambda-550]) for lambda = 550 - 700 nm.
T1 = 10 s for g = 400 - 550 nm; T1 = 10 x 10(0.02[lambda-550]) for
lambda = 550 - 700 nm.
For lambda = 1.5 to 1.6 xi m increase EL by 100 for periods of less
than 1 µs.
Table 8. Exposure limits for viewing a diffuse reflection of a
laser beam or an extended source laser
-------------------------------------------------------------------------
Spectral Exposure limits Wave-length Exposure time (t) (s)
region
-------------------------------------------------------------------------
UV 200 nm to 400 nm 10-9 to 3 x 104 Same as Table 7
Light 400 nm to 700 nm 10-9 to 10 10 3 ´t J/(cm2 x sr)
400 nm to 549 nm 10 to 104 21 J/(cm2 x sr)
550 nm to 700 nm 10 to T1 3.83 (t/ 4 ´t) J/(cm2 x sr)
550 nm to 700 nm T1 to 104 21/CB J/(cm2 x sr)
400 nm to 700 nm 104 to 3 x 104 2.1/CB x 10-3 W/(cm2 x sr)
IR-A 700 nm to 1400 nm 10-9 to 10 10CA 3 ´t J/(cm2 x sr)
700 nm to 1400 nm 10 to 103 3.83CA(t/4 ´t)J/(cm2 x sr)
700 nm to 1400 nm 103 to 3 x 104 0.64CA W/(cm2 x sr)
IR-B & C 1.4 µm to 1 mm 10-9 to 3 x 104 Same as Table 7
-------------------------------------------------------------------------
CA, CB, and T1 are the same as in footnote to Table 7.
Table 9. Exposure limits for skin exposure from a laser beam
---------------------------------------------------------------
Spectral Wave-length Exposure time Exposure limits
region (t) (s)
---------------------------------------------------------------
UV 200 nm to 400 nm 10-9 to 3x104 Same as Table 7
Light & 400 nm to 1400 nm 10-9 to 10-7 2CA x 10-2 J/cm2
IR-A 400 nm to 1400 nm 10-7 to 10 1.1CA 4´t J/cm2
IR-B & C 1.4 µm to 1 mm 10-9 to 3 x 104 Same as Table 6
---------------------------------------------------------------
CA = 1.0 for lambda = 400 - 700 nm; see Fig. 25 for value at
greater wavelengths.
NOTE: To aid in the determination of ELs for exposure
durations requiring calculations of fractional powers,
Fig. 25 may be used.
Table 10. Additivity of effects on eye and skin from different spectral regionsa
---------------------------------------------------------------------------------
UV-C and UV-B UV-A Visible and IR-A IR-B and IR-C
Spectral region 200-315 nm 315-400 nm 400-1400 nm 1400-106 nm
---------------------------------------------------------------------------------
UV-C and UV-B eye
200-314 nm skin
UV-A eye eye
315 nm skin skin skin
Visible and IR-A eye
400-1400 nm skin skin skin
IR-B and IR-C eye eye
1400-106 nm skin skin skin
---------------------------------------------------------------------------------
a Some synergism is expected when 2 spectral bands illuminate the same tissue
simultaneously. Exact formulae to treat these additive effects have not been
developed for most standards.
Table 11. Selected values of the minimum angle of an extended
source that may be used for applying extended source ELs
--------------------------------
Exposure duration Angle alpha
(s) (mrad)
--------------------------------
10-9 8.0a
10-8 5.4a
10-7 3.7a
10-6 2.5a
10-5 1.7a
10-4 2.2
10-3 3.6
10-2 5.7
10-1 9.2
--------------------------------
Table 11 (contd.)
--------------------------------
Exposure duration Angle alpha
(s) (mrad)
--------------------------------
1.0 15
10 24
102 24
103 24
104 24
--------------------------------
a For exposure durations of less
than 0.05 ms alphamin is less
for lambda = 1050 to 1400 nm.
11.8.1.3. Extended source laser exposure
The ELs for "extended sources" apply to sources that subtend an
angle greater than alphamin (Table 11), which varies with exposure
duration (t). This angle is not the beam divergence of the source.
Limits expressed as either radiance or integrated radiance may be
averaged over an angle as great as alphamin or sampled over a
source area as small as 1 mm in diameter.
Table 8 should be used to calculate the EL (as a brightness)
for an extended source such as a holographic display or a screen
illuminated by a static or scanning laser beam. The values in
Table 8 apply to viewing a diffuse reflection from a laser beam,
where a truly extensive retinal image occurs. Some laser devices
are intentionally designed as diffuse sources (e.g., beacons) to
radiate monochromatic optical power and still remain Class 1. The
extended source ELs of Table 8 apply to the direct output of the
laser system if the source is diffuse. As a further example, a
low-quality semiconductor diode laser or a semiconductor laser
diode array may be "extended". In this case, the average radiance
of the diode array might be applied against the extended source EL.
It must be emphasized that, in almost all instances, a laser source
is still a "point source" within definitions used by the standards.
To aid in determining when extended-source ELs are applicable,
the concept of alphamin was invented. The value of alphamin is a
linear angle expressed in mrads and is the minimum viewing angle at
which extended-source ELs apply. For viewing distances beyond the
location where the source angle subtends an angle less than
alphamin, the source is considered from a safety standpoint to be a
"point source" and the intrabeam viewing criteria of Table 7 apply.
Because the extended source ELs and the point source ELs do not
vary in exactly the same way as a function of pulse duration (or
exposure duration) (t), this limiting angle alphamin varies with
exposure duration (Table 11). Indeed alphamin is nothing more than:
alphamin = (4/pi) (EL [point source]/EL [extended source])´ Equation (14)
11.8.1.4. Restriction on ELs
The ELs were developed for conditions of occupational exposure
and the underlying assumption is that nearly all workers may be
exposed to the levels without adverse effects. However, some
photosensitive individuals may experience adverse effects at lower
levels for wavelengths of less than 500 nm.
11.8.2. Standards for non-laser sources
11.8.2.1. Introduction
The most commonly occurring hazardous effects from arcs and
high-intensity lamps are ultraviolet erythema and photokeratitis.
Retinal injury from such sources is seldom recognized though it is
not unheard of. Considering that much was known about optical
radiation hazards prior to the development of the laser, it seems
somewhat surprising that ELs and safety standards for lamps and
arcs did not exist prior to laser safety standards. Standards were
developed empirically for eye protective filters for welders, but
were not based on ELs.
Bright sources emitting cw light elicit a normal aversion or
pain response that serves to protect the eye and skin from injury.
Visual comfort has often been used as an approximate hazard index.
Eye protection baffles and other controls have been provided on
this basis. The determination of shade number for welding goggles
is one example. The present standards for welding goggle
specifications were simply based on a comfort index for viewing the
arc. Since UVR and infrared radiation were considered to be of no
value in viewing welding arcs, they were deliberately filtered out.
UV and IR filtration factors exceeding those for light were
specified as the best that could be achieved with readily available
glass materials.
Quantitative guidance is often sought with regard to both eye
and skin safety in relation to new sources of radiation. Though
several safety limits for optical radiation have been proposed in
the literature within recent years, it is only for the ultraviolet
spectral region that there have been any widely accepted limits,
but even these have provoked controversy.
ELs applicable to broad-band sources such as open-arc
processes, arc lamps, incandescent lamps, and gas discharge lamps
may differ considerably from laser ELs for two main reasons. The
first is that the source normally emits in a broad spectral band.
Therefore, effects due to narrow wavelength absorption or
coherence, which are potentially of concern with laser exposure,
are not likely to have a substantial impact on the hazards from a
broad-band source. All of the composite optical spectral bands for
conventional sources must be evaluated separately. For instance,
ultraviolet hazard criteria differ completely from light hazard
criteria.
The second major difference between laser and non-laser health
criteria results from the fact that most hazardous laser exposures
result from viewing a point source, whereas hazardous lamps and
arcs are usually extended sources. In the development of a new
lamp, any unwanted ultraviolet radiation should be filtered out by
the choice of an appropriately thick glass envelope, based on
computation, and assessments of both acute and chronic risks and
actual UVR measurements. In the past, manufacturers have watched
for acute effects in people exposed to prototype lamps.
The radiance from a conventional source is generally physically
limited compared with that of a laser source. The exposure of an
individual from a lamp source is seldom likely to exceed that under
normal operating conditions. Laser output powers can change
enormously with slight changes in the laser cavity.
11.8.2.2. UVR Criteria
As previously noted, the health hazards associated with UV-B + C
exposure of the eye and skin are often considered separately from
those associated with UV-A.
In the development of health criteria for industrial UVR
exposure, the prime consideration must be ELs that would prevent
unwanted acute and chronic effects. At the same time, simplicity
of measurement and application are important. If a single
instrument having a spectral response weighted against the envelope
action spectrum for UV-B and UV-C injury were developed, then a
direct measurement could be made of the UVR risk. Without a
spectrally integrating instrument, the spectral irradiance from the
source of interest can be measured at the point of greatest concern
(normally the nearest point of access). This spectral irradiance
Elambda is then weighted by the ACGIH envelope action curve Slambda
(Fig. 27, Table 12 and 13) for wavelengths of less than 320 nm.
Table 7. Exposure limits for direct ocular exposures (intrabeam viewing)
from a laser beam
-------------------------------------------------------------------------
Spectral Wavelength Exposure time (t) Exposure limits
region seconds (s)
-------------------------------------------------------------------------
UVC 200 nm to 280 nm 10-9 to 3 x 104 3 mJ/cm2
UVB 280 nm to 302 nm 10-9 to 3 x 104 3 mJ/cm2
303 nm 10-9 to 3 x 104 4 mJ/cm2
304 nm 10-9 to 3 x 104 6 mJ/cm2
305 nm 10-9 to 3 x 104 10 mJ/cm2
306 nm 10-9 to 3 x 104 16 mJ/cm2 )
307 nm 10-9 to 3 x 104 25 mJ/cm2 )
308 nm 10-9 to 3 x 104 40 mJ/cm2 ) not to
309 nm 10-9 to 3 x 104 63 mJ/cm2 ) exceed
310 nm 10-9 to 3 x 104 100 mJ/cm2) 0.56t¨
311 nm 10-9 to 3 x 104 160 mJ/cm2) J/cm2
312 nm 10-9 to 3 x 104 250 mJ/cm2)
313 nm 10-9 to 3 x 104 400 mJ/cm2)
314 nm 10-9 to 3 x 104 630 mJ/cm2)
315 nm 10-9 to 3 x 104 1.0 J/cm2)
315 nm to 400 nm 10-9 to 10 0.56t1/4 J/cm2
UVA 315 nm to 400 nm 10 to 103 1.0 J/cm2
315 nm to 400 nm 103 to 3 x 104 1.0 mW/cm2
-------------------------------------------------------------------------
Table 7 (contd.)
-------------------------------------------------------------------------
Spectral Wavelength Exposure time (t) Exposure limits
region seconds (s)
-------------------------------------------------------------------------
Light 400 nm to 700 nm 10-9 to 1.8 x 10-5 5 x 10-7J/cm2
400 nm to 700 nm 1.8 x 10-5 to 10 1.8(t/4 ´t) mJ/cm2
400 nm to 549 nm 10 to 104 10 mJ/cm2
500 nm to 700 nm 10 to T1 1.8(t/4 ´t) mJ/cm2
550 nm to 700 nm T1 to 104 10CB mJ/cm2
400 nm to 700 nm 104 to 3 x 104 CB µW/cm2
IR-A 700 nm to 1049 nm 10-9 to 1.8 x 10-5 5 CA x 10-7 J/cm2
700 nm to 1049 nm 1.8 x 10-5 to 103 1.8CA(t/4 ´/t) mJ/cm2
1050 nm to 1400 nm 10-9 to 5 x 10-4 5 x 10-6 J/cm2
1050 nm to 1400 nm 5 x 10-4 to 103 9(t/4 ´/t) mJ/cm2
700 nm to 1400 nm 103 to 3 x 104 320 CA µW/cm2
IR-B & C 1.4 µm to 103 µm 10-9 to 10-7 10-2 J/cm2
1.4 µm to 103 µm 10-7 to 10 0.56 4 ´/t) J/cm2
1.4 µm to 103 µm 10 to 3 x 104 0.1 W/cm2
-------------------------------------------------------------------------
The formula for Correction Factor CA (Fig. 25) is
CA = 1 for wavelength (lambda) of 400 nm - 700 nm;
CA = 10(0.002[lambda-700 nm]) for 700 nm < lambda < 1050 nm; and
CA = 5 for 1050 < lambda < 1400 nm.
CB = 1 for lambda = 400 - 550 nm;
CB = 10(0.015[lambda-550]) for lambda = 550 - 700 nm.
T1 = 10 s for g = 400 - 550 nm; T1 = 10 x 10(0.02[lambda-550]) for
lambda = 550 - 700 nm.
For lambda = 1.5 to 1.6 xi m increase EL by 100 for periods of less
than 1 µs.
Table 8. Exposure limits for viewing a diffuse reflection of a
laser beam or an extended source laser
-------------------------------------------------------------------------
Spectral Exposure limits Wave-length Exposure time (t) (s)
region
-------------------------------------------------------------------------
UV 200 nm to 400 nm 10-9 to 3 x 104 Same as Table 7
Light 400 nm to 700 nm 10-9 to 10 10 3 ´t J/(cm2 x sr)
400 nm to 549 nm 10 to 104 21 J/(cm2 x sr)
550 nm to 700 nm 10 to T1 3.83 (t/ 4 ´t) J/(cm2 x sr)
550 nm to 700 nm T1 to 104 21/CB J/(cm2 x sr)
400 nm to 700 nm 104 to 3 x 104 2.1/CB x 10-3 W/(cm2 x sr)
IR-A 700 nm to 1400 nm 10-9 to 10 10CA 3 ´t J/(cm2 x sr)
700 nm to 1400 nm 10 to 103 3.83CA(t/4 ´t)J/(cm2 x sr)
700 nm to 1400 nm 103 to 3 x 104 0.64CA W/(cm2 x sr)
IR-B & C 1.4 µm to 1 mm 10-9 to 3 x 104 Same as Table 7
-------------------------------------------------------------------------
CA, CB, and T1 are the same as in footnote to Table 7.
Table 9. Exposure limits for skin exposure from a laser beam
---------------------------------------------------------------
Spectral Wave-length Exposure time Exposure limits
region (t) (s)
---------------------------------------------------------------
UV 200 nm to 400 nm 10-9 to 3x104 Same as Table 7
Light & 400 nm to 1400 nm 10-9 to 10-7 2CA x 10-2 J/cm2
IR-A 400 nm to 1400 nm 10-7 to 10 1.1CA 4´t J/cm2
IR-B & C 1.4 µm to 1 mm 10-9 to 3 x 104 Same as Table 6
---------------------------------------------------------------
CA = 1.0 for lambda = 400 - 700 nm; see Fig. 25 for value at
greater wavelengths.
NOTE: To aid in the determination of ELs for exposure
durations requiring calculations of fractional powers,
Fig. 25 may be used.
Table 10. Additivity of effects on eye and skin from different spectral regionsa
---------------------------------------------------------------------------------
UV-C and UV-B UV-A Visible and IR-A IR-B and IR-C
Spectral region 200-315 nm 315-400 nm 400-1400 nm 1400-106 nm
---------------------------------------------------------------------------------
UV-C and UV-B eye
200-314 nm skin
UV-A eye eye
315 nm skin skin skin
Visible and IR-A eye
400-1400 nm skin skin skin
IR-B and IR-C eye eye
1400-106 nm skin skin skin
---------------------------------------------------------------------------------
a Some synergism is expected when 2 spectral bands illuminate the same tissue
simultaneously. Exact formulae to treat these additive effects have not been
developed for most standards.
Table 11. Selected values of the minimum angle of an extended
source that may be used for applying extended source ELs
--------------------------------
Exposure duration Angle alpha
(s) (mrad)
--------------------------------
10-9 8.0a
10-8 5.4a
10-7 3.7a
10-6 2.5a
10-5 1.7a
10-4 2.2
10-3 3.6
10-2 5.7
10-1 9.2
--------------------------------
Table 11 (contd.)
--------------------------------
Exposure duration Angle alpha
(s) (mrad)
--------------------------------
1.0 15
10 24
102 24
103 24
104 24
--------------------------------
a For exposure durations of less
than 0.05 ms alphamin is less
for lambda = 1050 to 1400 nm.
11.8.1.3. Extended source laser exposure
The ELs for "extended sources" apply to sources that subtend an
angle greater than alphamin (Table 11), which varies with exposure
duration (t). This angle is not the beam divergence of the source.
Limits expressed as either radiance or integrated radiance may be
averaged over an angle as great as alphamin or sampled over a
source area as small as 1 mm in diameter.
Table 8 should be used to calculate the EL (as a brightness)
for an extended source such as a holographic display or a screen
illuminated by a static or scanning laser beam. The values in
Table 8 apply to viewing a diffuse reflection from a laser beam,
where a truly extensive retinal image occurs. Some laser devices
are intentionally designed as diffuse sources (e.g., beacons) to
radiate monochromatic optical power and still remain Class 1. The
extended source ELs of Table 8 apply to the direct output of the
laser system if the source is diffuse. As a further example, a
low-quality semiconductor diode laser or a semiconductor laser
diode array may be "extended". In this case, the average radiance
of the diode array might be applied against the extended source EL.
It must be emphasized that, in almost all instances, a laser source
is still a "point source" within definitions used by the standards.
To aid in determining when extended-source ELs are applicable,
the concept of alphamin was invented. The value of alphamin is a
linear angle expressed in mrads and is the minimum viewing angle at
which extended-source ELs apply. For viewing distances beyond the
location where the source angle subtends an angle less than
alphamin, the source is considered from a safety standpoint to be a
"point source" and the intrabeam viewing criteria of Table 7 apply.
Because the extended source ELs and the point source ELs do not
vary in exactly the same way as a function of pulse duration (or
exposure duration) (t), this limiting angle alphamin varies with
exposure duration (Table 11). Indeed alphamin is nothing more than:
alphamin = (4/pi) (EL [point source]/EL [extended source])´ Equation (14)
11.8.1.4. Restriction on ELs
The ELs were developed for conditions of occupational exposure
and the underlying assumption is that nearly all workers may be
exposed to the levels without adverse effects. However, some
photosensitive individuals may experience adverse effects at lower
levels for wavelengths of less than 500 nm.
11.8.2. Standards for non-laser sources
11.8.2.1. Introduction
The most commonly occurring hazardous effects from arcs and
high-intensity lamps are ultraviolet erythema and photokeratitis.
Retinal injury from such sources is seldom recognized though it is
not unheard of. Considering that much was known about optical
radiation hazards prior to the development of the laser, it seems
somewhat surprising that ELs and safety standards for lamps and
arcs did not exist prior to laser safety standards. Standards were
developed empirically for eye protective filters for welders, but
were not based on ELs.
Bright sources emitting cw light elicit a normal aversion or
pain response that serves to protect the eye and skin from injury.
Visual comfort has often been used as an approximate hazard index.
Eye protection baffles and other controls have been provided on
this basis. The determination of shade number for welding goggles
is one example. The present standards for welding goggle
specifications were simply based on a comfort index for viewing the
arc. Since UVR and infrared radiation were considered to be of no
value in viewing welding arcs, they were deliberately filtered out.
UV and IR filtration factors exceeding those for light were
specified as the best that could be achieved with readily available
glass materials.
Quantitative guidance is often sought with regard to both eye
and skin safety in relation to new sources of radiation. Though
several safety limits for optical radiation have been proposed in
the literature within recent years, it is only for the ultraviolet
spectral region that there have been any widely accepted limits,
but even these have provoked controversy.
ELs applicable to broad-band sources such as open-arc
processes, arc lamps, incandescent lamps, and gas discharge lamps
may differ considerably from laser ELs for two main reasons. The
first is that the source normally emits in a broad spectral band.
Therefore, effects due to narrow wavelength absorption or
coherence, which are potentially of concern with laser exposure,
are not likely to have a substantial impact on the hazards from a
broad-band source. All of the composite optical spectral bands for
conventional sources must be evaluated separately. For instance,
ultraviolet hazard criteria differ completely from light hazard
criteria.
The second major difference between laser and non-laser health
criteria results from the fact that most hazardous laser exposures
result from viewing a point source, whereas hazardous lamps and
arcs are usually extended sources. In the development of a new
lamp, any unwanted ultraviolet radiation should be filtered out by
the choice of an appropriately thick glass envelope, based on
computation, and assessments of both acute and chronic risks and
actual UVR measurements. In the past, manufacturers have watched
for acute effects in people exposed to prototype lamps.
The radiance from a conventional source is generally physically
limited compared with that of a laser source. The exposure of an
individual from a lamp source is seldom likely to exceed that under
normal operating conditions. Laser output powers can change
enormously with slight changes in the laser cavity.
11.8.2.2. UVR Criteria
As previously noted, the health hazards associated with UV-B + C
exposure of the eye and skin are often considered separately from
those associated with UV-A.
In the development of health criteria for industrial UVR
exposure, the prime consideration must be ELs that would prevent
unwanted acute and chronic effects. At the same time, simplicity
of measurement and application are important. If a single
instrument having a spectral response weighted against the envelope
action spectrum for UV-B and UV-C injury were developed, then a
direct measurement could be made of the UVR risk. Without a
spectrally integrating instrument, the spectral irradiance from the
source of interest can be measured at the point of greatest concern
(normally the nearest point of access). This spectral irradiance
Elambda is then weighted by the ACGIH envelope action curve Slambda
(Fig. 27, Table 12 and 13) for wavelengths of less than 320 nm.
 Table 12. Relative spectral
effectiveness for selected wavelengths
--------------------------------------
Relative
spectral
Wavelength Elambda effectiveness
(nm) (mJ/cm2) Slambda
--------------------------------------
200 100 0.03
210 40 0.075
220 25 0.12
230 16 0.19
240 10 0.30
250 7.0 0.43
254 6.0 0.5
260 4.6 0.65
270 3.0 1.0
280 3.4 0.88
290 4.7 0.64
300 10 0.30
305 50 0.06
310 200 0.015
315 1000 0.003
--------------------------------------
Table 13. ACGIH ultraviolet exposure limits
--------------------------------------------
Duration of exposure Effective irradiance,
per day Eeff (µW/cm2)
--------------------------------------------
8 h 0.1
4 h 0.2
2 h 0.4
1 h 0.8
30 min 1.7
15 min 3.3
10 min 5
5 min 10
1 min 50
30 s 100
10 s 300
1 s 3000
0.5 s 6000
0.1 s 30 000
--------------------------------------------
All the preceding ELs for ultraviolet energy apply to sources
that subtend an angle less than 80°. Sources that subtend a
greater angle need to be measured only over an angle of 80°.
ACGIH recommended values: The threshold limit values for
occupational exposure to UVR incident on skin or eye, where
irradiance values are known and exposure time is controlled, are as
follows:
1. For the near ultraviolet spectral region (320-400 nm),
total irradiance incident on the unprotected skin or eye
should not exceed 1 mW/cm2 for periods greater than 103 s
(approximately 16 min) and for exposure times less than
103 s should not exceed one J/cm2.
2. For the actinic ultraviolet spectral region (200-315 nm),
radiant exposure incident on the unprotected skin or eye
should not exceed the values given in Table 10, within an
8-h period.
3. To determine the effective irradiance of a broad-band
source weighted against the peak of the spectral
effectiveness curve (270 nm), the following weighting
formula should be used:
Eeff = SIGMA Elambda Slambda delta lambda where:
Eeff = effective irradiance relative to a monochromatic
source at 270 nm in W/cm2 (J/s/cm2)
Elambda = spectral irradiance in W/cm2/nm
Slambda = relative spectral effectiveness (unitless)
delta lambda = band width (nm)
4. Permissible exposure time in seconds for exposure to
actinic ultraviolet radiation incident on the unprotected
skin or eye may be computed by dividing 0.003 J/cm2 by
Eeff in W/cm2. The exposure time may also be determined
using Table 13, which provides exposure times
corresponding to effective irradiances in µW/cm2.
Conditioned (tanned) individuals can tolerate skin exposure in
excess of the TLV without erythemal effects. However, such
conditioning may not protect persons against skin cancer.
For the UV-A, ACGIH considered it reasonable to propose a
guideline for ocular exposure so low that no conceivable thermal or
photochemical injury mechanisms were likely to be demonstrated. To
prevent thermal injury, it was assumed that, for exposure durations
of less than 100 s, the eye should be protected against exposures
above 10 kJ/m2 (1 J/cm2). Because of the lack of adverse effects
reported in individuals working with ultraviolet "black light"
sources at levels of 1 mW/cm2 (or above), it was presumed that a
level of 1 mW/cm2, the approximate level of exposure of the eye to
UVA-A in outdoor reflected sunlight, would be a reasonable upper
limit for exposures lasting 1000 s or more. The skin exposure limit
could presumably be increased by a factor of 5 for the longer
exposure durations. To avoid thermal effects at very short
exposure durations, the total UVR corneal irradiance was also
limited to 1 W/cm2. It is now known that photochemical effects
occur in both the eye and skin and that total daily doses of 20 -
100 J/cm2 cause acute corneal opacities (Pitts et al., 1977;
Zuchlich & Kurtin, 1977) and skin erythema from the UV-A (Parrish
et al., 1978). Hence, these UV-A criteria must be applied with
great caution for conditions of very long (exceeding 4 h) exposure.
11.8.2.3. Retinal health criteria
Laser protection standards incorporate several simplifications
that depend on the single-wavelength and point-source
characteristics of the laser. These standards may provide a too
conservative estimate of the real risk, if laser criteria are
applied to broad-band sources. No official standards exist for the
retinal risk evaluation of a broad-band source. Tentative
guidelines exist from ACGIH. To use these guidelines, both a blue-
light hazard function B lambda and a retinal thermal injury
function R lambda must be used. The source spectrum may be weighted
to indicate comparative levels of risk from the two types of
retinal injury mechanisms. Using equation 13 (section 8.4.1.3), in
which the retinal irradiance Er is directly proportional to the
radiance L of the source, the square of the pupil diameter dp, and
the transmission t of the ocular media. The retinal spectral
irradiance distribution can be calculated from the spectral
radiance distribution Llambda and knowledge of the spectral
transmission of the ocular media taulambda. In the absence of a
radiance standard, this approach can be used to calculate retinal
levels directly and to compare them directly with thresholds of
injury (Sliney & Freasier, 1973). However, the present approach is
to establish ELs for the spectrally weighted radiances. These
safety weighting functions are given in Table 14. Spectral factors
weighted against the spectral radiance are then applied as shown in
sections 11.8.2.4 and 11.8.2.5.
Table 14. Spectral weighting functions for assessing
retinal risks from broad-band optical sourcesa
-------------------------------------------------------
Blue-light Thermal
Wavelength hazard function hazard function
(nm) Blambda Rlambda
-------------------------------------------------------
400 0.10 1.0
405 0.20 2.0
410 0.40 4.0
415 0.80 8.0
420 0.90 9.0
425 0.95 9.5
430 0.98 9.8
435 1.0 10
440 1.0 10
445 0.97 9.7
450 0.94 9.4
455 0.90 9.0
460 0.80 8.0
465 0.70 7.0
470 0.62 6.2
475 0.55 5.5
-------------------------------------------------------
Table 14 (contd.)
-------------------------------------------------------
Blue-light Thermal
Wavelength hazard function hazard function
(nm) Blambda Rlambda
-------------------------------------------------------
480 0.45 4.5
485 0.40 4.0
490 0.22 2.2
495 0.16 1.6
500-600 10[(450-lambda)/50] 1.0
600-700 0.001 1.0
700-1049 0.001 10[(700-lambda)/500]
1050-1400 0.001 0.2
-------------------------------------------------------
a From: ACGIH (1981).
11.8.2.4. Retinal thermal risk evaluation
To protect against thermal retinal injury from short-term
exposures, the spectral radiance of the lamp weighted against the
function Rlambda (Table 14) should not exceed:
1400
SIGMA Llambda Rlambda delta lambda L(Haz) = ´ t/(alpha t) W/(cm2 x sr)
400 Equation (15)
where Llambda is given in W/(cm2 x sr), t is the viewing duration
(or pulse duration if the lamp is pulse limited) which is limited
to 1 ms - 10 s, and alpha is the angular subtense of the source in
radians. The angle alpha should be limited to approximately 0.1
radian. If the lamp is oblong, alpha refers to the longest
dimension (1) that can be viewed. For instance, at a viewing
distance (r) of 500 cm from a tubular lamp 50 cm long, the viewing
angle alpha is 1/r or 0.1 rad. Spectral radiance (Llambda)
measurements must be made at frequent wavelength intervals (delta
lambda) to preclude serious error. The delta lambda should be less
than 5 nm in the UV and blue end of the visible spectrum.
11.8.2.5. Retinal blue-light risk evaluation
To protect against retinal injury from blue-light exposure, the
integrated spectral radiance of the lamp weighted with the blue-
light hazard function (Blambda of Table 14) should not exceed 100
J/cm2 x sr for a duration of less that 104 or exceed 10 mW/(cm2 x
sr) for t > 104 s:
1400
SIGMA Llambda x t x Blambda x delta lambda < 100 J/(cm2 x sr) for t < 104 s
400 Equation (16)
or
1400
SIGMA Llambda x Blambda x delta lambda < 10 W/(cm2 x sr) for t > 104 s
400 Equation (17)
and for a point source (alpha < 11 mrad)
1400
SIGMA Elambda x t x Blambda x delta lambda < H(Haz) = 10 mJ/cm2 for t < 104 s
400 Equation (18)
or
1400
SIGMA Elambda x Blambda x delta lambda < E(Haz) = 1 µW/cm2 for t > 104 s
400 Equation (19)
These levels assume a constricted pupil, as would occur with
fixed viewing of any type of extended source with a radiance
approaching the EL. For a spectrally weighted source radiance (L)
that exceeds 10 mW/(cm2 x sr) in the blue-light spectral region,
the permissible exposure duration tmax in s is simply:
1400
tmax = 100 J/(cm2 x sr) / SIGMA Llambda x Blambda x delta lambda for t < 104 s
400 Equation (20)
The extended-source limits are greater than the 198. ELs for a
440-nm laser radiation source given by either ANSI or ACGIH, which
assume a 7-mm pupil rather than the 3-mm used for the broad-band
source analysis.
11.8.2.6. IR-A risk analysis
The proposed ACGIH EL also limited the IR-A and IR-B infrared
radiation beyond 770 nm to 10 mW/cm2 to avoid possible
cataractogenesis (the appearance of which may be delayed). For an
infrared heat lamp or other source that lacks a strong visual
stimulus, the radiance for wavelengths between 700 and 1400 nm for
long-term viewing should be limited to:
1400
SIGMA Llambda x delta lambda < L(Haz) = [0.6/alpha] W/(cm2 x sr)
700 Equation (21)
This limit is also based on a 7-mm pupil diameter.
NOTE: Equations 16 to 21 are empirical and are not, strictly
speaking, dimensionally correct. To make these formulae
correct, a dimensional correction factor must be inserted
into each formula. It is, therefore, important to use only
the units specified.
11.8.3. Infrared standards
There are no established non-laser, infrared (IR) health
standards. However, the laser ELs can be applied for broad-band
sources, if, in addition, the whole-body irradiation is evaluated.
Even irradiances as low as 100 W/m2 (10 mW/cm2) can place an
uncomfortable thermal load on the human body, especially when the
irradiation is not confined to one side of the body and this
radiant heat load occurs along with high ambient air temperatures.
In contrast, the IR laser EL for periods exceeding 10 s is 1 kW/m2
(100 mW/cm2), assuming that the total irradiated area of the skin
or the eye will be small. For laser exposure the irradiated area
is generally small, but this is not so likely when the body is
exposed to optical radiation from non-laser sources; and heat
stress must be evaluated.
The determination of the wet-bulb-globe-temperature (WBGT)
index requires a combination of a dry-bulb temperature with a wet-
bulb (WB) temperature (which involves humidity, air movement, etc.)
and a black-globe (BG) temperature (which includes the radiant
(predominantly infrared) contribution). These three temperatures
are weighted differently in two equations used for evaluating heat
stress - one for outdoor workers exposed to sunlight, another for
indoor workers exposed to infrared sources. The nature of the
skin's reflectance is such that much of the visible and IR-A are
reflected, whereas IR-B and IR-C are almost totally absorbed. The
spectral reflectance of most clothing is somewhat similar to that
of skin in the infrared. Obviously the second formula would be
used in any IR risk evaluation. The ACGIH formula for indoor heat
stress is:
WBGT = 0.7 WB + 0.3 GT Equation (22)
A heat-stress condition exists when this WBGT value exceeds 25 -
30 °C depending on work load.
A major problem in any infrared safety standard concerned with
wavelengths beyond 1.4 µm is ambient IR-C. The black-body radiant
exitance at 273 K (0 °C) is 32 mW/cm2; at 300 K (27.2 °C), it is 46
mW/cm2. A whole-body irradiance of 20 - 50 mW/cm2 from radiant
warmers on a cold (0 °C) winter day is comfortable; but the same
irradiance on a hot summer day could bring on heat stress.
Therefore any IR safety standard should distinguish between all the
IR bands, and IR-C limits would have to vary with ambient
conditions.
12. RISK EVALUATION
There are three broad areas of concern for any potentially
hazardous optical source: (a) the potential of the source for
causing personal injury; (b) the environment in which the laser or
optical source is used; and (c) the individuals who operate and
those who are potentially at risk from exposure to the emitted
optical radiation. For both lasers and lamp systems, it is
possible to develop a hazard classification scheme that would
greatly assist the health and safety professional in evaluating the
risk from an optical source in a particular environment (Anderson,
1980a).
It is important to understand that the laser classification
system was developed to aid the user in establishing a safety
programme for a particular laser device to relieve the user and
also the health and safety professional of the burden of detailed
and often complex measurements or calculations. The unique risks
and control measures applicable to specific environments depend on
the personnel potentially exposed and vary with each laser
application. However, fortunately, many of the protection measures
depend entirely, or to a great extent, on the laser hazard
classification.
Since the control measures required for Class 1 and Class 2
laser systems are minimal or nonexistent for the user, it is the
applications of Class 3 and Class 4 lasers that require careful
study of the risks, and the development of detailed control
measures. There are several protective methods, which can apply to
a Class 3 or a Class 4 laser product. The total enclosure of the
source is certainly the most desirable control measure. However,
since total enclosure with proper interlocks would result in a
Class 1 laser product, there is normally a reason why a laser
system was not originally designed as a Class 1 device. There are
a few instances where a specific enclosure must be developed for
each application. Where the enclosure approach is feasible, this
solution is strongly recommended.
Where the laser beam is operated without being enclosed -
either indoors or out-of-doors - the laser safety officer (a health
or safety professional or other special trained individual) has
great need of reference material and technical data. These data
include the reflective properties of materials found in the
environment, attenuating properties of filters, windows, or other
enclosures, and a working knowledge of several aspects of optical
systems.
Several system-safety items should be considered for
incorporation in laser system design, including:
beam attenuators;
interlocks;
manual switches;
the enclosure;
emission indicators;
accidental laser firing;
beam diffusers;
multiple wavelengths;
mode locking;
beam hotspots.
12.1. Laser Hazard Classification
For the classification of a laser, the following variables
concerned with output should be known: (a) the wavelength or
wavelength range; (b) the classification duration (i.e., in the
ANSI standard: how long is it possible for a person to be exposed
to an applicable EL); (c) average power output (for cw or
repetitively-pulsed lasers); and (d) total energy per pulse (or
peak power, pulse duration, PRF, and emergent beam radiant
exposures) for all pulsed lasers. The laser source radiance or
integrated radiance and the maximum viewing angular subtense is
required, if the source is an extended laser source and is
operating in the retinal hazard region (400 - 1400 nm).
If the laser is modified, after manufacture, in a way that
could affect the hazard classification, then the user or the
individual performing the modification should reclassify the
modified system.
12.2. Environmental Considerations including Reflection and the
Probability of Exposure
Environmental considerations probably play a greater role in
determining the control measures for Class 3 and Class 4 laser
systems, and these can only be evaluated by the user. These
environmental considerations include the possibility of reflections
(Gorodetski et al., 1968).
12.2.1. Reflections
The three general types of reflection that may be encountered
in many environments are shown in Fig. 28. Diffuse reflections
normally greatly reduce the hazards of the primary beam, though,
for Class 4 visible and near-infrared lasers, hazardous diffuse
reflections are likely (Komorova et al., 1978). The dividing line
between Class 3 and Class 4 visible and IR-A lasers is defined by
diffusely reflective hazard conditions. Reflections from flat
mirrors produce substantial risks of hazardous exposure at
considerable distances from the reflector as can be seen in
Fig. 28. Where random orientation of the reflectors can occur, the
potentialy hazardous area can be quite large. Curved surface
specular reflections,on the other hand, are normally hazardous only
at relatively short distances of the order of magnitude of the
radius of curvature from the reflector surface. Though specular
surfaces are of greatest concern in open laboratory situations,
they are not unheard of in the outdoor use of lasers and in medical
applications.
Table 12. Relative spectral
effectiveness for selected wavelengths
--------------------------------------
Relative
spectral
Wavelength Elambda effectiveness
(nm) (mJ/cm2) Slambda
--------------------------------------
200 100 0.03
210 40 0.075
220 25 0.12
230 16 0.19
240 10 0.30
250 7.0 0.43
254 6.0 0.5
260 4.6 0.65
270 3.0 1.0
280 3.4 0.88
290 4.7 0.64
300 10 0.30
305 50 0.06
310 200 0.015
315 1000 0.003
--------------------------------------
Table 13. ACGIH ultraviolet exposure limits
--------------------------------------------
Duration of exposure Effective irradiance,
per day Eeff (µW/cm2)
--------------------------------------------
8 h 0.1
4 h 0.2
2 h 0.4
1 h 0.8
30 min 1.7
15 min 3.3
10 min 5
5 min 10
1 min 50
30 s 100
10 s 300
1 s 3000
0.5 s 6000
0.1 s 30 000
--------------------------------------------
All the preceding ELs for ultraviolet energy apply to sources
that subtend an angle less than 80°. Sources that subtend a
greater angle need to be measured only over an angle of 80°.
ACGIH recommended values: The threshold limit values for
occupational exposure to UVR incident on skin or eye, where
irradiance values are known and exposure time is controlled, are as
follows:
1. For the near ultraviolet spectral region (320-400 nm),
total irradiance incident on the unprotected skin or eye
should not exceed 1 mW/cm2 for periods greater than 103 s
(approximately 16 min) and for exposure times less than
103 s should not exceed one J/cm2.
2. For the actinic ultraviolet spectral region (200-315 nm),
radiant exposure incident on the unprotected skin or eye
should not exceed the values given in Table 10, within an
8-h period.
3. To determine the effective irradiance of a broad-band
source weighted against the peak of the spectral
effectiveness curve (270 nm), the following weighting
formula should be used:
Eeff = SIGMA Elambda Slambda delta lambda where:
Eeff = effective irradiance relative to a monochromatic
source at 270 nm in W/cm2 (J/s/cm2)
Elambda = spectral irradiance in W/cm2/nm
Slambda = relative spectral effectiveness (unitless)
delta lambda = band width (nm)
4. Permissible exposure time in seconds for exposure to
actinic ultraviolet radiation incident on the unprotected
skin or eye may be computed by dividing 0.003 J/cm2 by
Eeff in W/cm2. The exposure time may also be determined
using Table 13, which provides exposure times
corresponding to effective irradiances in µW/cm2.
Conditioned (tanned) individuals can tolerate skin exposure in
excess of the TLV without erythemal effects. However, such
conditioning may not protect persons against skin cancer.
For the UV-A, ACGIH considered it reasonable to propose a
guideline for ocular exposure so low that no conceivable thermal or
photochemical injury mechanisms were likely to be demonstrated. To
prevent thermal injury, it was assumed that, for exposure durations
of less than 100 s, the eye should be protected against exposures
above 10 kJ/m2 (1 J/cm2). Because of the lack of adverse effects
reported in individuals working with ultraviolet "black light"
sources at levels of 1 mW/cm2 (or above), it was presumed that a
level of 1 mW/cm2, the approximate level of exposure of the eye to
UVA-A in outdoor reflected sunlight, would be a reasonable upper
limit for exposures lasting 1000 s or more. The skin exposure limit
could presumably be increased by a factor of 5 for the longer
exposure durations. To avoid thermal effects at very short
exposure durations, the total UVR corneal irradiance was also
limited to 1 W/cm2. It is now known that photochemical effects
occur in both the eye and skin and that total daily doses of 20 -
100 J/cm2 cause acute corneal opacities (Pitts et al., 1977;
Zuchlich & Kurtin, 1977) and skin erythema from the UV-A (Parrish
et al., 1978). Hence, these UV-A criteria must be applied with
great caution for conditions of very long (exceeding 4 h) exposure.
11.8.2.3. Retinal health criteria
Laser protection standards incorporate several simplifications
that depend on the single-wavelength and point-source
characteristics of the laser. These standards may provide a too
conservative estimate of the real risk, if laser criteria are
applied to broad-band sources. No official standards exist for the
retinal risk evaluation of a broad-band source. Tentative
guidelines exist from ACGIH. To use these guidelines, both a blue-
light hazard function B lambda and a retinal thermal injury
function R lambda must be used. The source spectrum may be weighted
to indicate comparative levels of risk from the two types of
retinal injury mechanisms. Using equation 13 (section 8.4.1.3), in
which the retinal irradiance Er is directly proportional to the
radiance L of the source, the square of the pupil diameter dp, and
the transmission t of the ocular media. The retinal spectral
irradiance distribution can be calculated from the spectral
radiance distribution Llambda and knowledge of the spectral
transmission of the ocular media taulambda. In the absence of a
radiance standard, this approach can be used to calculate retinal
levels directly and to compare them directly with thresholds of
injury (Sliney & Freasier, 1973). However, the present approach is
to establish ELs for the spectrally weighted radiances. These
safety weighting functions are given in Table 14. Spectral factors
weighted against the spectral radiance are then applied as shown in
sections 11.8.2.4 and 11.8.2.5.
Table 14. Spectral weighting functions for assessing
retinal risks from broad-band optical sourcesa
-------------------------------------------------------
Blue-light Thermal
Wavelength hazard function hazard function
(nm) Blambda Rlambda
-------------------------------------------------------
400 0.10 1.0
405 0.20 2.0
410 0.40 4.0
415 0.80 8.0
420 0.90 9.0
425 0.95 9.5
430 0.98 9.8
435 1.0 10
440 1.0 10
445 0.97 9.7
450 0.94 9.4
455 0.90 9.0
460 0.80 8.0
465 0.70 7.0
470 0.62 6.2
475 0.55 5.5
-------------------------------------------------------
Table 14 (contd.)
-------------------------------------------------------
Blue-light Thermal
Wavelength hazard function hazard function
(nm) Blambda Rlambda
-------------------------------------------------------
480 0.45 4.5
485 0.40 4.0
490 0.22 2.2
495 0.16 1.6
500-600 10[(450-lambda)/50] 1.0
600-700 0.001 1.0
700-1049 0.001 10[(700-lambda)/500]
1050-1400 0.001 0.2
-------------------------------------------------------
a From: ACGIH (1981).
11.8.2.4. Retinal thermal risk evaluation
To protect against thermal retinal injury from short-term
exposures, the spectral radiance of the lamp weighted against the
function Rlambda (Table 14) should not exceed:
1400
SIGMA Llambda Rlambda delta lambda L(Haz) = ´ t/(alpha t) W/(cm2 x sr)
400 Equation (15)
where Llambda is given in W/(cm2 x sr), t is the viewing duration
(or pulse duration if the lamp is pulse limited) which is limited
to 1 ms - 10 s, and alpha is the angular subtense of the source in
radians. The angle alpha should be limited to approximately 0.1
radian. If the lamp is oblong, alpha refers to the longest
dimension (1) that can be viewed. For instance, at a viewing
distance (r) of 500 cm from a tubular lamp 50 cm long, the viewing
angle alpha is 1/r or 0.1 rad. Spectral radiance (Llambda)
measurements must be made at frequent wavelength intervals (delta
lambda) to preclude serious error. The delta lambda should be less
than 5 nm in the UV and blue end of the visible spectrum.
11.8.2.5. Retinal blue-light risk evaluation
To protect against retinal injury from blue-light exposure, the
integrated spectral radiance of the lamp weighted with the blue-
light hazard function (Blambda of Table 14) should not exceed 100
J/cm2 x sr for a duration of less that 104 or exceed 10 mW/(cm2 x
sr) for t > 104 s:
1400
SIGMA Llambda x t x Blambda x delta lambda < 100 J/(cm2 x sr) for t < 104 s
400 Equation (16)
or
1400
SIGMA Llambda x Blambda x delta lambda < 10 W/(cm2 x sr) for t > 104 s
400 Equation (17)
and for a point source (alpha < 11 mrad)
1400
SIGMA Elambda x t x Blambda x delta lambda < H(Haz) = 10 mJ/cm2 for t < 104 s
400 Equation (18)
or
1400
SIGMA Elambda x Blambda x delta lambda < E(Haz) = 1 µW/cm2 for t > 104 s
400 Equation (19)
These levels assume a constricted pupil, as would occur with
fixed viewing of any type of extended source with a radiance
approaching the EL. For a spectrally weighted source radiance (L)
that exceeds 10 mW/(cm2 x sr) in the blue-light spectral region,
the permissible exposure duration tmax in s is simply:
1400
tmax = 100 J/(cm2 x sr) / SIGMA Llambda x Blambda x delta lambda for t < 104 s
400 Equation (20)
The extended-source limits are greater than the 198. ELs for a
440-nm laser radiation source given by either ANSI or ACGIH, which
assume a 7-mm pupil rather than the 3-mm used for the broad-band
source analysis.
11.8.2.6. IR-A risk analysis
The proposed ACGIH EL also limited the IR-A and IR-B infrared
radiation beyond 770 nm to 10 mW/cm2 to avoid possible
cataractogenesis (the appearance of which may be delayed). For an
infrared heat lamp or other source that lacks a strong visual
stimulus, the radiance for wavelengths between 700 and 1400 nm for
long-term viewing should be limited to:
1400
SIGMA Llambda x delta lambda < L(Haz) = [0.6/alpha] W/(cm2 x sr)
700 Equation (21)
This limit is also based on a 7-mm pupil diameter.
NOTE: Equations 16 to 21 are empirical and are not, strictly
speaking, dimensionally correct. To make these formulae
correct, a dimensional correction factor must be inserted
into each formula. It is, therefore, important to use only
the units specified.
11.8.3. Infrared standards
There are no established non-laser, infrared (IR) health
standards. However, the laser ELs can be applied for broad-band
sources, if, in addition, the whole-body irradiation is evaluated.
Even irradiances as low as 100 W/m2 (10 mW/cm2) can place an
uncomfortable thermal load on the human body, especially when the
irradiation is not confined to one side of the body and this
radiant heat load occurs along with high ambient air temperatures.
In contrast, the IR laser EL for periods exceeding 10 s is 1 kW/m2
(100 mW/cm2), assuming that the total irradiated area of the skin
or the eye will be small. For laser exposure the irradiated area
is generally small, but this is not so likely when the body is
exposed to optical radiation from non-laser sources; and heat
stress must be evaluated.
The determination of the wet-bulb-globe-temperature (WBGT)
index requires a combination of a dry-bulb temperature with a wet-
bulb (WB) temperature (which involves humidity, air movement, etc.)
and a black-globe (BG) temperature (which includes the radiant
(predominantly infrared) contribution). These three temperatures
are weighted differently in two equations used for evaluating heat
stress - one for outdoor workers exposed to sunlight, another for
indoor workers exposed to infrared sources. The nature of the
skin's reflectance is such that much of the visible and IR-A are
reflected, whereas IR-B and IR-C are almost totally absorbed. The
spectral reflectance of most clothing is somewhat similar to that
of skin in the infrared. Obviously the second formula would be
used in any IR risk evaluation. The ACGIH formula for indoor heat
stress is:
WBGT = 0.7 WB + 0.3 GT Equation (22)
A heat-stress condition exists when this WBGT value exceeds 25 -
30 °C depending on work load.
A major problem in any infrared safety standard concerned with
wavelengths beyond 1.4 µm is ambient IR-C. The black-body radiant
exitance at 273 K (0 °C) is 32 mW/cm2; at 300 K (27.2 °C), it is 46
mW/cm2. A whole-body irradiance of 20 - 50 mW/cm2 from radiant
warmers on a cold (0 °C) winter day is comfortable; but the same
irradiance on a hot summer day could bring on heat stress.
Therefore any IR safety standard should distinguish between all the
IR bands, and IR-C limits would have to vary with ambient
conditions.
12. RISK EVALUATION
There are three broad areas of concern for any potentially
hazardous optical source: (a) the potential of the source for
causing personal injury; (b) the environment in which the laser or
optical source is used; and (c) the individuals who operate and
those who are potentially at risk from exposure to the emitted
optical radiation. For both lasers and lamp systems, it is
possible to develop a hazard classification scheme that would
greatly assist the health and safety professional in evaluating the
risk from an optical source in a particular environment (Anderson,
1980a).
It is important to understand that the laser classification
system was developed to aid the user in establishing a safety
programme for a particular laser device to relieve the user and
also the health and safety professional of the burden of detailed
and often complex measurements or calculations. The unique risks
and control measures applicable to specific environments depend on
the personnel potentially exposed and vary with each laser
application. However, fortunately, many of the protection measures
depend entirely, or to a great extent, on the laser hazard
classification.
Since the control measures required for Class 1 and Class 2
laser systems are minimal or nonexistent for the user, it is the
applications of Class 3 and Class 4 lasers that require careful
study of the risks, and the development of detailed control
measures. There are several protective methods, which can apply to
a Class 3 or a Class 4 laser product. The total enclosure of the
source is certainly the most desirable control measure. However,
since total enclosure with proper interlocks would result in a
Class 1 laser product, there is normally a reason why a laser
system was not originally designed as a Class 1 device. There are
a few instances where a specific enclosure must be developed for
each application. Where the enclosure approach is feasible, this
solution is strongly recommended.
Where the laser beam is operated without being enclosed -
either indoors or out-of-doors - the laser safety officer (a health
or safety professional or other special trained individual) has
great need of reference material and technical data. These data
include the reflective properties of materials found in the
environment, attenuating properties of filters, windows, or other
enclosures, and a working knowledge of several aspects of optical
systems.
Several system-safety items should be considered for
incorporation in laser system design, including:
beam attenuators;
interlocks;
manual switches;
the enclosure;
emission indicators;
accidental laser firing;
beam diffusers;
multiple wavelengths;
mode locking;
beam hotspots.
12.1. Laser Hazard Classification
For the classification of a laser, the following variables
concerned with output should be known: (a) the wavelength or
wavelength range; (b) the classification duration (i.e., in the
ANSI standard: how long is it possible for a person to be exposed
to an applicable EL); (c) average power output (for cw or
repetitively-pulsed lasers); and (d) total energy per pulse (or
peak power, pulse duration, PRF, and emergent beam radiant
exposures) for all pulsed lasers. The laser source radiance or
integrated radiance and the maximum viewing angular subtense is
required, if the source is an extended laser source and is
operating in the retinal hazard region (400 - 1400 nm).
If the laser is modified, after manufacture, in a way that
could affect the hazard classification, then the user or the
individual performing the modification should reclassify the
modified system.
12.2. Environmental Considerations including Reflection and the
Probability of Exposure
Environmental considerations probably play a greater role in
determining the control measures for Class 3 and Class 4 laser
systems, and these can only be evaluated by the user. These
environmental considerations include the possibility of reflections
(Gorodetski et al., 1968).
12.2.1. Reflections
The three general types of reflection that may be encountered
in many environments are shown in Fig. 28. Diffuse reflections
normally greatly reduce the hazards of the primary beam, though,
for Class 4 visible and near-infrared lasers, hazardous diffuse
reflections are likely (Komorova et al., 1978). The dividing line
between Class 3 and Class 4 visible and IR-A lasers is defined by
diffusely reflective hazard conditions. Reflections from flat
mirrors produce substantial risks of hazardous exposure at
considerable distances from the reflector as can be seen in
Fig. 28. Where random orientation of the reflectors can occur, the
potentialy hazardous area can be quite large. Curved surface
specular reflections,on the other hand, are normally hazardous only
at relatively short distances of the order of magnitude of the
radius of curvature from the reflector surface. Though specular
surfaces are of greatest concern in open laboratory situations,
they are not unheard of in the outdoor use of lasers and in medical
applications.
 Absolute values of spectral reflectance are relatively
unimportant because such values vary only by a factor of 10 - 20,
whereas the laser beam irradiance may exceed the applicable EL by
orders of magnitude above this factor.
Most reported laser accidents have occurred, when the
probability of exposure was very high. No discussion of reflection
hazards is therefore complete without the consideration of the
probability of exposure. It must be remembered that the underlying
philosophy of the classification system is that control measures
should increase with increasing risk of exposure as well as with
increased severity of exposure.
12.2.2. Retroreflection
Some materials exhibit a property known as retrodirective
reflection. The reflection does not obey either the law of regular
(specular) reflection, or the cosine dependence of Lambertian
reflection. A collimated indigent beam may remain collimated and
be redirected along the original axis of propagation, regardless of
the angle of incidence at the retroflector. Corner cubes and some
specialized highway signs are examples of retroflectors.
12.2.3. Optically aided viewing
Nearly all laser workers know that viewing a laser source with
a telescope may substantially increase the risk. This increase in
risk is most dramatic for intra-beam viewing of a collimated
source. In this case, an increase in the power entering the eye is
possible, because the diameter of the objective (Do) of the
telescope or binocular is much larger than the pupil of the eye dp.
The actual increase in risk (G) depends on whether the pupil of the
eye is larger or smaller than the exit pupil (De) of the optical
system, the spectral transmittance (taulambda) of the optical
system at the laser wavelength(s), and the beam diameter relative
to the objective (collecting aperture) diameter.
When a bright object, larger than a point source, is viewed
through a well-designed optical system, the radiant power reaching
the retina (visible and IR-A) is theoretically increased by the
square of the instrument's magnifying power. However, since there
is a commensurate increase in the area of the retinal image, the
retinal irradiance remains unchanged, except for a slight reduction
because of reflective loss and the absorption of light in the
optical system. The retinal hazard in this case may increase in
some instances, since the thermal retinal injury threshold
decreases with increasing image size.
13. ACCIDENTAL INJURIES
At present, retinal injuries with loss of sight following
exposure to visible and IR-A laser radiation have been the most
catastrophic of all effects from laser radiation (Boldry et al.,
1981; Zhokov, 1981). Though the relatively high-powered, far-
infrared lasers such as the cw, carbon-dioxide laser, have caused
numerous burns to the hands and clothes, these are considered
inconsequential in comparison with the serious retinal injuries.
One postal survey conducted several years ago (Rockwell & Goldman,
1974) appeared to indicate that there had been at least 100
injuries to the eye from laser radiation in the USA. One
subjective account in this regard was that of Decker (1977).
Despite such reports, surprisingly few serious injuries of the
eye have been reported in the last 15 years in relation to exposure
to pulsed lasers. This low accident rate cannot be accounted for
by assuming that the ocular ELs are too conservative. The
explanation is probably that accidental exposure of the eye to a
collimated beam is normally an extremely remote possibility, if
precautions are taken to keep the eye out of the beam. One of the
few situations in which the probability of hazardous exposure is
great is during work in the laboratory and, each year, several
retinal injuries are reported under these conditions. However, it
is difficult to ascertain the exposure conditions in sufficient
detail for useful threshold or injury data to be derived. Concern
may also exist regarding the potential bias in an individual's
description of the accidental exposure conditions to support a
claim of compliance with safety measures. It is not clear whether
laser exposures are always detected by the exposed individual, and
this may be a particular problem with IR lasers (Kasuba & Akifev,
1977). It is known that retinal injury outside the macula may have
little or no effect on everyday visual performance and therefore
may not be detected subjectively.
14. CONTROL MEASURES
Risk control guidelines are not mutually exclusive. Following
one or two guidelines may reduce the risk to such an extent that
other recommended control measures, in that particular class, are
no longer essential. For example, if the beam path of a Class 4
laser were enclosed, then it would hardly be necessary to remove
all glass objects, or other specular surfaces near the beam path
but outside the enclosure, nor would it seem necessary to wear eye
protectors. However, the eye protection might be necessary if the
enclosure were being modified or during initial alignment. The
decision to use any particular set of controls depends on use
conditions and whether general population exposure is likely.
Table 15 provides a brief list of the most commonly recommended
laser control measures.
Table 15. Control measures for general population and occupational
exposure
-------------------------------------------------------------------
I Engineering control measures:
protective housing enclosure and service panel requirements;
interlocks on the protective housing;
door interlocks and remote control connector;
beam attenuator or beam shutter;
key switch or padlock over aperture cover;
filtered viewing optics and windows;
emission delay (BRH);
warning lights;
emission indicators (audible or visible);
enclosed area or room;
beam enclosure;
remote firing and/or monitoring;
II Personal protective equipment:
eyewear;
clothing;
gloves;
III Administrative and procedural controls:
laser safety officer;
standard operating procedures (SOPs);
limitations on use by class;
education and training;
maintenance and servicing manuals;
marking of protective devices;
warning signs and labels;
entry limitations for visitors, etc.;
accident procedures.
-------------------------------------------------------------------
Because of the risk associated with exposure to Class 4 high-
risk lasers, the safety precautions associated with these laser
installations indoors, generally include the installation of door
interlocks to prevent exposure of unauthorized or transient
personnel entering the laboratory, the use of baffles to terminate
the primary and any secondary beams, and the use of safety eyewear
by personnel within the interlocked facility (Klost, 1971).
At one time, it was recommended that ambient light levels
should be sufficient to constrict pupils. However, since a
constricted pupil provides only a small safety factor, the
requirement for good illumination, which remains in present safety
standards, is related to good general visibility, as the wearing of
eye protectors reduces visual capabilities. Light-coloured, matt
surfaces in the room minimize glare, and thus promote visibility.
In summary, the ability to analyse potential risks from any
laser system is enhanced by a broad knowledge of optics, general
laser technology, and the imaging process of the human eye. A
laser safety specialist should have a general background knowledge
of optics with the basic knowledge necessary to perform a risk
analysis. It has been shown that the risk analysis depends on at
least three aspects - the laser system and its potential hazards,
the type of personnel who may be exposed, and, finally, the
reflective materials and other optically important materials in the
environment that can influence the risk analysis.
15. HAZARDS OF LAMP SOURCES AND PROJECTION SYSTEMS
The optical radiation emitted by a conventional light source,
either a bare lamp, a luminaire, or a projection system, can be
evaluated using the previously mentioned tentative exposure limits
or guidelines.
Prior to exhaustive measurements and safety calculations, it
may be worthwhile to determine the need for a comprehensive risk
evaluation. Many categories of lamps or other types of light
sources can be excluded from all or several of the evaluations.
The following multi-step scheme (Sliney & Wolbarsht, 1980) may be
useful in this regard.
STEP 1 - Categorization of the lamp. Certain hazards are specific
for certain types of lamp or light source. The following grouping
is useful:
(a) incandescent lamps and incandescent heating sources;
(b) low-pressure discharge lamps;
(c) fluorescent lamps;
(d) high-intensity discharge (HID) lamps;
(e) short-arc (compact arc) lamps;
(f) carbon arcs;
(g) solid-state sources (LEDs etc.);
(h) cathode-ray tubes (CRTs).
STEP 2 - Determination of the source envelope. Any glass between
the actual source of radiation (e.g., the arc or tungsten filament)
and the point of access can greatly influence the potential hazard.
Soft (lime) glass of any reasonable thickness will greatly
attenuate UV-B and UV-C radiation.
(a) Incandescent lamps, other than quartz-halide lamps,
normally have a sufficiently thick glass envelope to
completely preclude a UVR hazard. The blue-light
hazard does not appear to be theoretically possible
at black-body temperatures below 2000 K (Sliney &
Wolbarsht, 1980), but most filaments operate at
effective temperatures exceeding 2000 K.
(b) Low-pressure discharge lamps. Low-pressure discharge
lamps do not normally present a retinal hazard,
because of the relatively low radiance. Only lamps
with quartz envelopes can transmit sufficient UV-B
and UV-C to be of concern. Of the common low-pressure
lamps, only mercury lamps can create a severe UVR
hazard. Many may be quite hot to the touch.
(c) Fluorescent lamps. Low-pressure tubular lamps in
almost all cases have a thin glass envelope, but
could often present a potential UVR hazard at the
surface. They do not represent a thermal retinal
injury hazard and seldom a blue-light hazard.
(d) HID lamps. These lamps may present both blue-light
and thermal retinal hazards, and possible UVR
hazards. Since most lamp envelopes are glass, there
is little UV-B leakage. Nevertheless, the UV-B
leakage may be of concern at very short distances.
Quartz-mercury HID lamps require a UVR risk
evaluation. If the outer glass envelope of an HID
lamp breaks, hazardous UV levels will be emitted.
Governmental regulations in Canada and the USA
require HID lamps to have a self-extinguishing
feature to preclude this hazard, unless the packaging
clearly warns against use without adequate shielding.
(e) Short-arc lamps. Of all the electric lamp categories,
this group will require the most extensive risk
evaluation. All potential hazards may be present
(UV-B/C, UV-A, blue-light, retinal thermal injury,
and skin thermal injury). Because of the high
temperature of the arc, a quartz envelope (which
transmits UV-B and C) is characteristic. These lamps
are often used in UV photocuring processes in
industry (Moss, 1980).
(f) Carbon arcs. Where a glass lens or filter plate does
not exist between the open arc and a point of access,
the carbon arc, like the short-arc lamp, is
potentially injurious.
(g) Solid-state lamps (e.g., LEDs). The present solid-
state lamps including LEDs, which emit visible
radiation, do not present any health risk, regardless
of the type of envelope.
(h) Cathode-ray tubes (CRTs). Present CRTs emit optical
radiation at levels that could pose a potential
health hazard (Wolbarsht et al., 1980).
STEP 3 - The obtaining of available manufacturers' radiometric and
photometric data and lamp descriptions. Any radiometric or
photometric specification may be of value either for calculation or
for direct intercomparison with measurements. Spectral data are
most useful. The dimensions of the emitting area of the lamp will
be required for retinal hazard evaluation.
STEP 4 - Comparison of lamp specifications with those of previously
evaluated lamps. From experience, it is often possible to complete
the risk evaluation with this step.
STEP 5 - Performance of detailed spectroradiometric measurements,
when necessary. In addition, where feasible, measurements of
luminance, illuminance, and total irradiance should be performed.
These will provide confirmation of the spectroradiometric
measurements. The pulse duration must be measured for a pulsed
source.
STEP 6 - Determination of the source dimensions. A photograph and
microdensitometer scan of the negative may be necessary for a non-
uniform source. The maximum angular subtense alpha of the source
should be calculated at the point of human access or at 15 cm from
the source, whichever is closer.
STEP 7 - Estimation of the exposure and comparison with the
exposure limits to determine the degree of risk.
STEP 8 - Consideration of potentially hazardous failure modes. For
example, breakage of the outer envelope of some high-intensity
discharge (HID) lamps can create a serious UVR hazard (Anderson,
1980b).
16. PROJECTION OPTICS
Broad-band sources involving projection optics are most
difficult to evaluate. Besides the problems encountered in
evaluating exposed lamps, the projected beam and projected source
size must be characterized. When viewing a collimated light source
from within the beam (other than a laser), a magnified view of the
actual source will be seen. The source is generally a high-
brightness lamp. The brighter the lamp, the greater the maximal
irradiance in the projected beam. This is a consequence of the Law
of Conservation of Brightness (Radiance) (see, for example, Kline,
1970; or Sliney & Wolbarsht, 1980). Some usually safe lamps become
hazardous to view through projection optics, despite the fact that
the optics cannot make the lamp brighter. The risk increases
because of the dependence of retinal injury on image size. Besides
the obvious projection sources - such as spotlights, searchlights,
slide projectors, and film projectors - solar concentrators and
other non-imaging light collectors may also require risk
evaluation. From the Law of Conservation of Radiance, it is
possible to evaluate the retinal risks from projector systems.
Collimating optics may consist of refracting elements (lenses),
reflecting elements (curved mirrors), or both.
17. SAFETY GUIDELINES FOR HIGH-INTENSITY SOURCES
Since lamp or arc sources may be hazardous from several
aspects, it may be helpful to develop a safety classification
scheme, similar to the one applied to laser products. The
following scheme of Sliney & Wolbarsht (1980) illustrates this
approach to evaluate the retinal risks from projector systems.
Both lamps and total lighting systems could be included. The
categories could be as follows:
Safety Group 1: Safe sources. These lamps are considered
safe to view throughout the day. No warning label would be
required. Examples: a frosted 15-W filament lamp or a
TV-display, cathode-ray tube.
Safety Group 2: Low-risk sources. These lamps are safe
for momentary 0.25-s, unintentional viewing. Examples:
most spotlights and film-projector lamp bulbs. A caution
label should be required on the lamp base, and possibly on
the projection system itself. No ultraviolet or infrared
hazard would exist at distances of more than 10 cm from
the lamp or projected beam.
Safety Group 3: Moderate-risk sources. These lamps would
be unsafe to view at close range, even momentarily.
Presumably, skin injury could also occur from ultraviolet
radiation as from germicidal lamps, sun lamps, and high
intensity UV-A lamps. A danger-label, clearly visible on
the equipment, could be required. A common lamp that might
fit into this category would be a 600-1000-W tungsten-
halogen lamp without a Fresnel lens, such as is used for a
home cine film spot lamp. The emergent beam irradiance is
far in excess of that required to ignite paper within half
a metre of the source. Obviously, the basis for the
determination of a hazard classification would differ
according to whether the hazard classification criteria
were based on retinal or skin injury. Each measurement for
classification would be for a specified accessible
approach distance, using a standard aperture and solid
angle of acceptance. The minimum approach distance could
vary with application. Other examples that might be
included in this category are some very high intensity,
short-pulse, laser flash tubes, and 20 kW xenon-arc
searchlights.
Safety Group 4: High-risk sources. These sources would
cause skin burns and/or erythema within a standardized
period of exposure (e.g., within 10 s) at a standardized
distance at which the effective UV irradiance would exceed
3 W/m2 (0.3 mW/cm2), or the total irradiance across the
entire spectrum would exceed 2 kW/m2 (0.2 W/cm2). Examples
of such sources are an open carbon-arc spotlight or an
open 1-kW mercury lamp. It may be that safety groups 3 and
4 are so similar in degree of risk, that they could be
combined.
18. WELDING ARCS
The most common high-intensity arc is probably the welding arc.
These arcs vary in brightness and in UVR content, primarily
according to the arc current, type of shielding gas, and the metals
being welded.
The greatest population exposed to intense sources of optical
radiation are welders and their assistants. The American Welding
Society estimated that there may be as many as 500 000 welders in
the USA alone (Emmett & Horstman, 1976). The two broad categories
of welding equipment are gas (acetylene) welding equipment and
electric-arc welding equipment. A gas welding torch or cutting
torch has a luminance not much greater than a candle flame,
typically ranging from 10 to 200 kcd/m2 (1-20 cd/cm2), and the UVR
emission is quite small. The optical radiation hazards of such
torches are virtually nonexistant. Welding filter goggles used
with such torches are to reduce glare, and are little darker than
very dark sunglasses having a shade number of the order of 3 - 5
(visual transmittance of 5 - 15 %). On the other hand, electric
welding arcs may be 1000 times brighter than gas torches and emit
UVR at proportionately higher levels (Sutter et al., 1972).
Protective shields, curtains, screens for bystanders, and
welders' goggles are the standard protective equipment used in
welding (Mayer et al., 1979; Sliney et al., 1981). Protective
procedures and protective equipment for the welder have been
developed empirically over the last three-quarters of a century.
Only very recently have detailed measurements of the radiometric
output of welding arcs been available. When these measurements
were carefully compared with exposure limits being developed for
protection against bright light sources, it was shown that the
empirically-developed protective equipment standards were adequate.
19. EYE AND SKIN PROTECTION
19.1. Laser Safety Eyewear
From a safety point of view, the most desirable laser hazard
control measure is complete enclosure of the laser or laser system;
however, this may not always be practical and laser eye protectors
are generally the best alternative. Though most industrial laser
applications do not require the use of eye protectors, this is not
always true for laser applications in the research laboratory. Eye
protectors provide the simplest solution to the laser safety
problem for a constantly changing experimental arrangement. Several
factors play a role in determining whether eyewear is necessary in
any situation. At least three output parameters of the laser must
be known: maximum exposure duration, wavelength, and output power
(or output irradiance, or radiant exposure, or energy), as well as
the applicable safe corneal radiant exposure. In addition, some
knowledge of such environmental factors as ambient lighting and the
nature of the laser operation may also be required.
Laser eye protection generally consists of a filter (often
composed of several individual filter plates) which selectively
attenuates at specific laser wavelengths, but elsewhere transmits
as much visible radiation as possible (Swope & Koester, 1965;
Schreibeis, 1968; Scherr et al., 1969; Swope, 1969, 1970; Straub,
1970; Sliney, 1974). Eyewear is available in several designs -
spectacles, coverall types with opaque side-shields, and coverall
types with somewhat transparent filter side-shields. The selection
of appropriate laser protective eyewear may be complex (Envall &
Murray, 1979). Active electronic imaging devices have also served
an additional role, as eye protection.
19.2. Welders' Filters
Eye protection filters, which were originally developed for
welders, were based more on available materials than on knowledge
of ocular protection requirements. The first organized study of
glass filter materials was carried out by Sir William Crookes
(1914) in England. Optical transmission characteristics are now
standardized as "shades" and specified for particular applications
(Coblentz et al., 1931; Stair, 1948; ANSI, 1978). Though maximum
transmittances for ultraviolet and infrared radiation are specified
for each shade, the mean photopic visual transmittance tauv, or
visual optical density Dv, has traditionally been used to define
the shade number S:
S = (7/3) Dv + 1 = - ln tauv + 1 Equation (23)
or Dv = (3/7) (S - 1) Equation (24)
where Dv = -log10 tauv Equation (25)
19.3 Eye Protection for Furnace Radiation
As well as protective clothing and equipment, many industrial
methods now used probably reduce the level of glass furnace
radiation to which the eye is exposed. For instance, the openings
to higher temperature furnaces are a great deal smaller than they
have been in past years; this would reduce the total irradiance of
the eye from infrared radiation. There are sufficient data and
cases of a very specific form of cataract in workers to suggest
that infrared does, indeed, cause glass-blower's or furnaceman's
cataract (Duke-Elder, 1972).
19.4. Eye Protection Filters for Solar Radiation
Direct viewing of the sun, for whatever reason, requires
protection against several different portions of the spectrum. A
yellowish or reddish filter generally protects against ultraviolet
radiation. Protection against intense visible rays should be
weighted to filter out more of the blue-light than the rest of the
visible spectrum. It is generally found that a shade 12 or 13
welder's filter is quite adequate to protect against ultraviolet
radiation, infrared, and visible radiation. The protection
afforded against the IR, however, is far greater than necessary.
The use of darkened coloured slides is not advisable, since
these slides (usually made by developing unexposed colour film) use
organic dyes that transmit in the near-infrared (IR-A) spectral
band.
19.5. Skin Protecting Agents for UVR (Sunscreens)
A number of topical, physical, and chemical screening agents
have been developed that provide nearly total or partial filtration
of ultraviolet radiation. Since actinic UV-B and UV-C radiation
are the most hazardous, efforts to develop topical agents have
concentrated primarily on filtering out this type of radiation. The
chemical agents in these "sunscreens" include para-aminobenzoic
acids (PABA) and its esters, salicylates, and cyanamates. These
materials are mixed in solution with substances that have good
substantivity (i.e., adhere to the skin) (Dahling et al., 1970;
Fitzpatrick et al., 1974).
19.6. Protective Garments
Aluminized fabrics were greatly improved during various manned
space programmes (Stoll & Chiantra, 1971). Such fabrics, when used
in thermal protective garments, have been shown to offer equivalent
or superior reflective and mechanical properties compared with
conventional aluminized asbestos garments (Wren et al., 1977).
Aluminized rayon (basket weave) and certain aluminized cottons were
shown to allow the least transmission of infrared radiation.
20. MEDICAL SURVEILLANCE (RATIONALE)
In the past two decades, many employees working routinely with
lasers have been subjected to preplacement, periodic, and end-of-
job eye examinations in order to obtain sufficient information
concerning the risk of retinal damage. Many of these studies
indicated that periodic eye examinations rarely located hitherto
unsuspected retinal damage. In general, published reports of
ophthalmic accidents have been those in which the acute over-
exposure was sufficient to subjectively alert the individual
(Hathaway et al., 1977). Thus, many authorities (Suess, ed., 1982)
suggest that ophthalmic examinations are unnecessary for
individuals routinely working with Class 1 and 2 lasers, and that,
if requested, the examinations should be confined to those working
with Class 3 or 4 systems only.
An examination is required within 24 - 48 h of any event in
which the worker suspects, or knows, that the eye might have been
exposed. Laser lesions change in appearance and may even tend to
disappear within the heterogeneous appearance of the fundus within
a period of time, so that ophthalmic examinations, some time after
exposure, may be difficult to interpret.
21. FORMAL TRAINING FOR LASER WORKERS
It is necessary to establish a safety programme that assures
the safe use of lasers and other radiation sources. To assure
knowledge of, and compliance with, applicable standards, a certain
amount of formalized teaching is often necessary.
At work places, a specific individual should be assigned to
maintain and enforce the safety programme (in some countries this
individual is termed a laser safety officer (LSO)).
All workers occupied with, or working near, the radiation
source should be included in the teaching programme.
The object is to make workers and work leaders aware of the
risks of lasers, how to avoid the hazards, the proper use of
protective devices, and how to realize when overexposure has taken
place.
REFERENCES
ALLEN, R.G. (1980) Retinal thermal injury. In: Kelley, W.D.,
ed. Non-ionizing radiation, Cincinnati, OH, ACGIH, pp. 161-168.
ACGIH (1976) A guide for control of laser hazards, Cincinnati,
OH, American Conference of Governmental Industrial Hygienists.
ACGIH (1981) Threshold limit values for chemical substances
and physical agents in the workroom adopted by ACGIH for 1981,
Cincinnati, OH, American Conference of Governmental Industrial
Hygienists.
ANDERSON, F.A. (1980a) The biological basis for standards,
Rockville, MD, US Dept. of Health, Education and Welfare, Food
and Drug Administration, Bureau of Radiological Health.
ANDERSON, F.A. (1980b) Sodium and mercury vaporlamps. In:
Kelley, W.D., ed. Non-ionizing radiation, Cincinnati, OH,
ACGIH, pp. 239-243.
ANDERSON, R.R. & PARRISH, J.A. (1981) The optics of human
skin. J. Invest. Derm., 77: 13-19.
ANSI (1978) Standard practice for occupational eye, and face
protection, New York, American National Standards Institute
(ANSI Standard Z-89.1).
ANSI (1980) Safe use of lasers, New York, American National
Standards Institute (ANSI Standard Z-136.1).
AVDEEV, P.S., BEREZIN, Yu.D., GUDAKOVSKII, Yu.P., MURATOV,
V.R., MURZIN, A.G., & FROMZEL, V.A. (1978) Experimental
determination of maximum permissible exposure to laser
radiation of 1.54 µ wavelength. Sov. J. quant. Electr., 8:
134-141.
BEATRICE, E.S. & LUND, D.J. (1979) Characteristics of damage
produced by non-circular retinal laser radiation, San
Francisco, CA, Letterman Army Institute of Research,
(Institute Report No. 31, AD-AD35 878/8ST).
BEATRICE, E.S. & VELEZ, S. (1978) Laser safety bioeffects
research: histopathology of retinal effects. In: SPIE Proc.,
Visual simulation: 162: 103-106.
BERGQUIST, T., HARTMANN, B., & KLEMAN, B. (1978) Imaging
properties of the eye and interaction of laser radiation with
matter. In: Tengroth, B. & Epstein, D., ed. Current concepts
in ergophthalmology, Stockholm, Karolinska Institute.
BIRNGRUBER, R. (1978) [Experimental and theoretical
investigations into thermal injury to the retina from laser
radiation.] PhD Dissertation, Frankfurt, J.W. Goethe
University (in German).
BOLDRY, E.E., LITTLE, H., FLOCKS, M., & VASSILIADIS, A. (1981)
Retinal injury due to industrial laser burns. Ophthalmol., 88:
101-107.
BORLAND, R.G., BRENNAN, D.H., & NICHOLSON, A.N. (1971)
Threshold levels for damage of the cornea following
irradiation by a continuous wave carbon dioxide (10.6 micron)
laser. Nature (Lond.), 234: l5l-l52.
BORLAND, R.G., BRENNAN, D.H., MARSHALL, I.J., & VIVASH, J.P.
(1978) The role of fluorescein angiography in the detection of
laser induced damage to the retina .. a threshold study for
Q-switched neodymium and ruby laser. Exp. Eye Res., 27:
471-493.
BROWN, J.L. (1973) Experimental investigations of flash
blindness. Hum. Factors, 6: 503-516.
CAMPBELL, C.J., RITTLER, M.C., BREDEMEIER, H., & WALLACE, R.A.
(1968) Ocular effects produced by experimental lasers. I.
Carbon dioxide laser. Am. J. Ophthalmol., 66: 604-614.
CIE (1970) International lighting vocabulary, Paris, Bureau
Central de la Commission Internationale de l'Eclairage, Vol.
3, p. 5l.
CLEVET, A. & MAYER, A. (1980) Risques liés à l'utilisation
industrielle des lasers. Cahiers de notes documentaires INRS,
No 99, 2è trimestre, pp. 207-222.
COBLENTZ, W.W., STAIR, R., & HOGUE, J.M. (1931) The spectral
erythemic reaction of the human skin to ultraviolet radiation.
Proc. Natl Acad. Sci., 17(6): 401-405.
COGAN, D.G. & KINSEY, V.E. (1946) Action spectrum of keratitis
produced by ultraviolet radiation. Arch. Ophthalmol., 77:
670-677.
CONSIDINE, P.S. (1966) Effects of coherence on imaging
systems. J. Opt. Soc. Am., 56: 1001-1009.
CORNSWEET, T.N., ed. (1966) Visual perception, New York,
Academic Press.
COURT, L., CHEVALEREAUD, J.P., & SANTUCCI, G. (1978) Exposé
général. In: Sociéte française de Radioprotection, 9è Congrès
international: Effets biologiques des Rayonnements non
ionisants. Utilisation et Risques associés. Monte-Carlo,
Monaco, pp. 367-445.
CROOKES, W. (1914) The preparation of eye-preserving glass for
spectacles. Phil. Trans. Roy. Phil. Soc., A204: 1-25.
DAHLING, R.F., SHAPIRO, S.I., BERRY, C.Z., & SCHREIBER, M.M.
(1970) A method of evaluating sun screen protection from
long-wave ultraviolet. J. Invest. Derm., 55: 164-169.
DAUTRAY, R. & WATTEAU, J.P. (1980) La fusion inertielle par
laser. Rev. gén. nucl., No. 6, pp. 562-575.
DAVIES, J.M. (1959) The effects of intense thermal radiation
on animal skin. A comparison of calculated and observed burns,
Natick, MA, Army Quartermaster Research and Engineering
Command (Report T-24, 29 April 1959, NTIS AD 456794).
DAVSON, H., ed. (1962) The eye (4 volumes), New York, Academic
Press.
DECKER, D. (1977) An accident victim's view. Laser Focus,
13(8): 6.
DECOMPS, B. (1981) Le laser, instrument de recherche et
facteur de développement. Rev. gén. d'Elect., 90(1): 11-29.
DE GRUIJL, F.R. & VAN DER LEUN, J.C. (1980) A dose-response
for skin cancer induction by chronic UV exposure of a human
population. J. Theor Biol., 83; 487-504.
DUKE-ELDER, S. (1972) Textbook of ophthalmology, Vol. VI,
Injuries, St. Louis, Mosby, C.V.
EMMETT, E.A. & HORSTMAN, S.W. (1976) Factors influencing the
output of ultraviolet radiation during welding. J. occup.
Med., 18(1): 41-44.
ENVALL, K.R. & MURRAY, R. (1979) Evaluation of commercially
available laser protective eyewear, Rockville, MD, US Dept of
Health Education and Welfare, Food and Drug administration,
Bureau of Radiological Health. (DHEW Publ. No. (FDA) 79-8086).
ERNEST, J.T. & POTTS, A.M. (1971) Pathophysiology of the
distal portion of the optic nerve. IV. Local temperature as a
measure of blood flow. Am. J. Ophthalmol., 72(2): 435-444.
FITZPATRICK, T.B., PATHAK, M.A., HARBER, L.C., SEIJI, M., &
KUKITA, A. (1974) Sunlight and man, normal and abnormal
photobiologic responses, Tokyo, University of Tokyo Press.
FRANCE, Arrêté du 30 janvier (1974) Réglementation concernant
les lasers à usage médical. J.O. 17 mars 1974, p. 3093.
FRANCE, Arrêté du 13 mai (1974) Conditions techniques
générales des lasers à usage médical. J.O. 15 juin 1974,
p. 6388.
FRANCE, Arrêté du 14 mai (1974) Conditions techniques des
lasers à usage médical de catégorie II, groupe I, sous-groupe
I. J.O. 15 juin 1974, p. 6388.
FRANCE, Arrêté du 29 décembre (1976) Classification des lasers
à usage médical de catégorie II, groupe II (émission
continue). J.O. 22 janvier 1977, (Numéro complémentaire)
p. 466.
FRANCE, Arrêté du 10 janvier (1978) Conditions techniques
d'utilisation des lasers à usage médical de catégorie II,
groupe II. J.O. 28 janvier 1978 (Numéro complémentaire) p. 822.
FRIED, D.L. (1981) Laser eye safety: The implications of
ordinary speckle and speckled-speckle statistics. J. Opt. Soc.
Am., 71(7): 914-916.
FRISCH, G.D., BEATRICE, E.S., & HOLSEN, R.C. (1971)
Comparative study of argon and ruby retinal damage thresholds.
Invest. Ophthalmol., 10: 911-919.
GABEL, V.P. & BIRNGRUBER, R. (1981) A comparative study of
threshold laser lesions in the retinae of human volunteers and
rabbits. Health Phys., 40: 238-240.
GABEL, V.P., BIRNGRUBER, R., & HILLENKAMP, F. (1976) [Light
absorption in the fundus oculi.] Munich, Association for
Research on Radiation and the Environment (GSF report A55) (in
German).
GEERAETS, W.J. & BERRY, E.R. (1968) Ocular spectral
characteristics as related to hazards from lasers and other
light sources. Am. J. Ophthalmol., 66: 15-20.
GIESE, A.C. (1976) Living with our sun's ultraviolet rays,
New York, Plenum Publishing Corporation.
GOLDMAN, L., ed. (1981) The biomedical laser technology and
clinical applications, New York, Heidelberg, Berlin, Springer
Verlag.
GOLDMAN, L., ROCKWELL, R.J., & RICHFIELD, D. (1971) Long-term
laser exposure of a senile freckle. Arch. environ. Health, 22:
401-403.
GOLDMAN, L., ROCKWELL, R.J., MICHAELSON, S.M., SLINEY, D.H.,
TENGROTH, B.M., & WOLBARSHT, M.L. (1982) Optical radiation,
with particular reference to lasers. In: Suess, M. ed.
Nonionizing radiation, Copenhagen, World Health Organization,
Regional Office for Europe.
GOLDMANN, H. (1933) Genesis of heat cataract. Arch.
Ophthalmol., 9: 314.
GORODETSKI, A.A., KIRICINSKI, B.R., EVDOKOMOB, I.R., &
KOLESNIK, V.M. (1968) [Some data on the biological action and
radiation protection of optical quantum generators.] Gig. Tr.
Prof. Zabol., 12: 37-41 (in Russian).
GREISEMANN, J.C. & MARTI, J. (1978) Risques liés à
l'utilisation des lasers de puissances. In: Société française
de Radioprotection, 9è Congrès international. Effets
biologiques des Rayonnements non ionisants. Utilisation et
Risques associés, pp. 473-482.
GREISS, G.A., BLANKENSTEIN, F., & WILLIFORD, G.G. (1980)
Ocular damage thresholds from multiple-pulse laser exposures,
Health Phys., 39: 921-927.
GRUM, F.C. & BECHERER, R., ed. (1979) Optical radiation
measurements, Vol. 1, Radiometry, New York, Academic Press,
p. 352.
GULLBERG, K., HARTMAN, B., KOCK, E., & TENGROTH, B. (1967)
Carbon dioxide laser hazards to the eye. Nature (Lond.), 215:
857-858.
HAM, W.T. Jr, WILLIAMS, R.C., MUELLER, H.A., GUERRY, D.,
CLARKE, A.M., & GEERAETS, W.J. (1966) Effects of laser
radiation on the mammalian eye. Trans. NY Acad. Sci., 28:
517-526.
HAM, W.T. Jr, CLARKE, A.M., GEERAETS, W.J., CLEARY, S.F.,
MUELLER, H.A., & WILLIAMS, R.C. (1970) The eye problem in
laser safety. Arch. environ. Health, 20: 156-160.
HAM, W.T. Jr, MUELLER, H.A., & SLINEY, D.H. (1976) Retinal
sensitivity to damage from short wavelength light. Nature
(Lond.), 260(5547): 153-155.
HAM, W.T. Jr, MUELLER, H.A., RUFFOLO, J.J., & CLARKE, A.M.
(1978) Sensitivity of the retina to radiation damage as a
function of wavelength. Photochem. Photobiol., 29: 735-743.
HAMERSKI, W. (1969) Investigations on histochemical changes in
experimental corneal lesions induced with UV radiation and on
the prevention of photophthalmia. Pol. med. J., 8: 1469-1476.
HANSEN, W.P. & FINE, S. (1968) Melanin granule models for
pulsed laser induced retinal injury. Appl. Opt., 7: 155-159.
HARDY, J.D. (1968) Pain following step increase in skin
temperature. In: Kenshalo, D.R. ed. The skin senses,
Springfield, IL, Charles C. Thomas, pp. 444-456.
HARDY, J.D., HAMMEL, H.T., & MURGATROYD, D. (1956) Spectral
transmittance and reflectance of excised human skin. J. appl.
Physiol., 9: 257.
HARLEN, F. (1978) The development of laser codes of practice
and maximum permissible exposure levels. Ann. occup. Hyg.,
2l(2): 199-211.
HARTMANN, B. & KLEMAN, B. (1980) Exposure limits for
broad-band 400-1400 nm radiation. Ocular effects of
non-ionizing radiation. Proc. SPIE, 29: 105-114.
HARWERTH, R.S. & SPERLING, H.G. (1975) Effects of intense
visible radiation on the increment threshold spectral
sensitivity of the Rhesus monkey eye. Vision Res., 15:
1193-1204.
HATFIELD, E.M. (1970) Eye injuries and the solar eclipse.
Sight Sav. Rev., pp. 79-85.
HATHAWAY, J.A., STERN, N., SOLES, E.M., & LEIGHTON, E. (1977)
Ocular medical surveillance on microwave and laser workers. J.
occup. Med., l9(10): 683-688.
HAUSSER, K.W. (1929) [Influence of wavelength in radiation
biology.] Strahlenther., 28: 25-44 (in German).
HOLZINGER, G., KROY, W., SCHREIBER, P., & SUTTER, E. (1978)
Protection from law radiation (Series on Workplace Protection,
no.14).
INTERNATIONAL ORGANIZATION FOR STANDARDIZATION (1980) Personal
eye-protectors for welding and related techniques. Welding
filters, Geneva (ISO 4850).
IRPA (1977) Overviews on nonionizing radiation, International
Radiation Protection Association Report of a Study Group.
JAMES, R.H., ed. (1976) National Conference on Measurements
of Laser Emissions for Regulatory Purposes, April, Rockville,
MD, US Dept of Health, Education and Welfare, Food and Drug
Administration, Bureau of Radiological Health (HEW Publ. (FDA)
76-8037).
KASUBA V.A. & AKIFEV, S.A. (1977) [Working conditions and
morbidity among workers preparing clock jewels using lasers
and mechanical techniques.] Gig. Tr. Prof. Zabol., 1: 37-40
(in Russian).
KAUFMANN, E. (1970) Laser hazard to the human eye. Schweiz
Arch., 36: 211.
KLINE, M.V. (1970) Optics, New York, John Wiley and Sons.
KLOST, W. (1971) [Safety measures in the use of laser rays.]
Zentralbl. Arbeitsmed., 21: 105-111 (in German).
KOGELNIK, H. & LI, T. (1966) Laser beams and resonators. In:
Levine, A.K., ed. Lasers. New York, Decker.
KOMAROVA, A.A., MOTZERENKOV, V.P., SKATSKAIA, G.K., CEMNY,
A.B., & PIVOVAROV, N.N. (1978) [Action of reflected laser
radiation on the eye.] Vestn. Oftal., l: 46-50 (in Russian).
KUWABARA, T. (1970) Retinal recovery from exposure to light.
Am. J. Ophthalmol., 70(2): 187-189.
LA VAIL, M.M. (1980) Eye pigmentation and constant light
damage in the rat retina. In: Williams, T.P. & Baker, B.N.,
ed. The effects of constant light on visual processes, New
York, London, Plenum Press, pp. 357-387.
LAWWILL, T., CROCKET, S., & CURRIER, G. (1977) Retinal damage
secondary to chronic light exposure thresholds and mechanisms.
Doc. Ophthalmol., 44(2): 379-402.
LE BODO, H. (1976) La calorimétrie appliquée à la mesure des
puissances et énergies lasers. Bulletin d'information du
Bureau National de Métrologie, No. 24, pp. 12-18.
LEIBOWITZ, H.M. & PEACOCK, G.R. (1969) Corneal injury produced
by carbon dioxide laser radiation. Arch. Ophthalmol., 8l:
712-721.
LERMAN, S. (1980a) Radiant energy and the eye, New York,
Macmillan Publ. Co.
LERMAN, S. (1980b) Human ultraviolet radiation cataracts.
Ophthal. Res., 12: 303-314.
LIVINGSTON, P.C. (1932) The study of sun glare in Iraq. Br. J.
Ophthalmol., 6: 577-625.
LOWE, D.A. (1975) A guide to international recommendations on
names and symbols for quantities and on limits of measurement.
Geneva, World Health Organization (Progress in Standardization: 2).
MAGNUS, I.A. (1976) Dermatological photobiology, London,
Blackwell Scientific Publications.
MAINSTER, M.A., WHITE, T.J., TIPS, J.H., & WILSON, P.W. (1970)
Retinal-temperature increases produced by intense light
sources. J. Opt. Soc. Am., 60: 264-270.
MARSHALL, J. (1970) Thermal and mechanical mechanisms in laser
damage to the retina. Invest. Ophthalmol., 9: 97-115.
MARSHALL, J. (1973) Laser damage to ocular tissues. Proc. R.
Soc. Med., 66(9): 842-844.
MARSHALL, J. (1978) Retinal injury from chronic exposure to
light and the delayed effects from retinal exposure to intense
light sources. In: Tengroth, B. & Epstein, D., ed. Current
concepts in ergophthalmology, Stockholm, Karolinska Institute,
pp. 81-104.
MARSHALL, J. & BIRD, A.C. (1979) A comparative histo-
pathological study of argon and krypton laser irradiations of
the human retina. Br. J. Ophthalmol., 63(10): 657-668.
MARSHALL, W.J. (1980) Optical measurement techniques. In:
Kelley, W.D., ed. Non-ionizing radiation, Cincinatti, OH,
ACGIH, pp. 175-179.
MAYER, M.A. & SALSI, M.S. (1979) Rayonnement ultraviolet,
visible et infrarouge, mésure-evaluation des risques. INRS
Cahiers de Notes documentaires, No. 96, 3e trimestre, 403-413.
MEDOVSKAYA, T.P. (1970) Data on the condition of the eye in
workers at a glass factory. Hyg. Sanit., 35: 446-447.
MESTER, E. (1980) L'effet stimulant des faisceaux laser sur la
cicatrisation des plaies. Rev. Iéna, No. 3, pp. 121-122.
MIRO, L. (1979) Le laser et ses applications médio-
chirurgicales. Semaine des hôpitaux de Paris, 55(41-42):
1956-1964.
MOON, M.E., CLARKE, A.M., RUFFALO, J.J. Jr, & MUELLER, H.A.
(1978) Visual performance in the Rhesus monkey after exposure
to blue light. Vision Res., 18: 1573-1577.
MOSS, C.E. (1980) Radiation hazards associated with
ultraviolet radiation curing processes. In: Kelley, W.D., ed.
Non-ionizing radiation, Cincinnati, OH, ACGIH, pp. 203-209.
NOELL, W.K. & ALBRECHT, R. (1971) Irreversible effects of
visible light on the retina, role of vitamin A. Science, 172:
76-79.
PARR, W.H. (1969) Skin lesion threshold values for laser
radiation as compared with safety standards, Fort Knox, KY, US
Army Medical Research Laboratory (Report 8l3, AD 688871).
PARRISH, J.A., ANDERSON, R.R., URBACH, F., & PITTS, D. (1978)
UVA biological effects of ultraviolet radiation with emphasis
on human responses to longwave ultraviolet, New York, Plenum
Publishing Corporation.
PARVER, L.M., ANKER, C., & CARPENTER, D.O. (1980) Choroidal
blood flow as a heat dissipating mechanism in the macula. Am.
J. Ophthalmol., 89: 641-646.
PECKHAM, R.H. & HARLEY, R.D. (1951) The effect of sunglasses
in protecting retinal sensitivity. Am. J. Ophthalmol., 34(11):
1499-1507.
PENNER, R. & McNAIR, J.N. (1966) Eclipse blindness. Am. J.
Ophthalmol., 61: 1452-1457.
PITTS, D.G. (1974) The human ultraviolet action spectrum. Am.
J. opt. S. physiol. Opt., 51: 946-960.
PITTS, D.G., CULLEN, A.P., & HACKER, P.D. (1977) Ocular
effects of ultraviolet radiation from 295 to 365 nm. Invest.
ophthalmol. Vis. Sci., 16(10): 932-939.
PRATESI, R. & SACCHI, C.A., ed. (1980) Lasers in photomedicine
and photobiology, Berlin, Springer-Verlag.
ROCKEROLLES, R. (1978) Dangers spécifiques du rayonnement
cohérent. Dangers habituels liés aux fortes luninances; effets
multiphotoniques et effets non linéaires. In: Société
française de Radioprotection. 9è Congrès international: Effets
biologiques des Rayonnements non ionisants. Utilisation et
Risques associés, Monte-Carlo, Monaco, pp. 453-472.
ROCKWELL, R.J. Jr, & GOLDMAN, L. (1974) Research on human skin
laser damage threshold, final report, Texas, USAF School of
Aerospace Med., Brooks AF Base (Prepared by Dept of
Dermatology and Laser Lab. Med. Centre, University of
Cincinnati, Contract F4l609-72-C-0007).
ROGER, F.C. (1973) Clinical findings, course and progress of
biatis corneal degeneration in the Dahlak Islands. Br. J.
Ophthalmol., 57: 657-661.
RUBIN, L.R. (1977) Lasers in biology, Moscow, Nauka.
SCHERR, A.D., TUCKER, R.J., & GREENWOOD, R.A. (1969) New
plastics absorb at laser wavelength. Las. Foc., 5(9): 46-48.
SCHREIBEIS, W.J. (1968) Laser eye protection goggles based on
maufacturer's information. Am. Ind. Hyg. Assoc. J., 29: 504.
SKEEN, C.H., BRUCE, W.R., TIPS, J.H. Jr, SMITH, M.G., & GARZA,
G.G. (1972) Ocular effects of repetitive laser pulses,
San Antonio, TX, Technology Inc. (Contract F41609-71-C-0018, AD
746795).
SLINEY, D.H. (1971) The development of laser safety
criteria-biological considerations. In: Wolbarsht, M.L., ed.
Laser applications in medicine and biology, New York, Plenum
Press, pp. 163-238.
SLINEY, D.H. (1972) The merits of an envelope action spectrum
for ultraviolet radiation exposure criteria. Am. Ind. Hyg.
Assoc. J., 33: 644-653.
SLINEY, D.H. (1974) Laser protective eyewear. In: Wolbarsht,
M.L., ed. Laser application in medicine and biology, New York,
Plenum Press, Vol. 2.
SLINEY, D.H. & FREASIER, B.C. (1973) The evaluation of optical
radiation hazards. Appl. Opt., 12(1): 1-24.
SLINEY, D.H. & WOLBARSHT, M.L. (1980) Safety with lasers and
other optical sources, New York, Plenum Publishing Corporation.
SLINEY, D.H., MOSS, C.E., MILLER, C.G., & STEPHENS; J.B.
(1981) Semitransparent curtains for control of optical
radiation hazards. Appl. Optics, 20(14): 2352-2366.
SMITH, H.E. (1944) Actinic macular retinal pigment
degeneration. US Nav. med. Bull., 42: 675-680.
SMITH, K.C. (1977) The science of photobiology, New York,
Plenum Press.
SMITH, K.C. (1978) Symposium on DNA repair and its role in
mutagenesis and carcinogenesis. Photochem. Photobiol., 28: 119.
STAIR, R. (1948) Spectral-transmissive properties and use of
eye-protective glasses. Washington, DC, National Bureau of
Standards (NBS Circular 471).
STOLL, A.M. & CHIANTRA, M.A. (1971) Heat transfer through
fabrics as related to thermal injury. Trans. N.Y. Acad. Sci.,
33: 649-670.
STOLWIJK, J.A.J. (1980) Infrared radiation and radiant heat
stress. In: Kelley, W.D., ed. Non-ionizing radiation,
Cincinnati, OH, ACGIH, pp. 171-174.
STRAUB, H.W. (1970) Laser eye protection in the USA.
Berufsgenossenschaft Z. Unfallv. Betrieb, 3: 83-87.
STUCK, B.E., LUND, D.J., & BEATRICE, E.A. (1981) Ocular
effects of holmium (2.06 µm) and erbium (1.54 µm) laser
radiation. Health Phys., 40: 835-846.
SUESS, ed. (1982) Nonionizing radiation protection,
Copenhagen, World Health Organization, Regional Office for
Europe.
SUTTER, E., HUEBNER, H.J., KRAUSE, E., & RUGE, J. (1972)
[Radiation measurements in various arc welding processes.]
Federal Republic of Germany, Federal Institute of Physics and
Technology (Report No. Optik 2/72) (in German).
SWOPE, C.H. (1969) The eye protection. Arch. environ. Health,
18: 428-433.
SWOPE, C.H. (1970) Design considerations for laser eye
protection. Arch. environ. Health, 20: 184-187.
SWOPE, C.H. & KOESTER, C.J. (1965) Eye protection against
lasers. Appl. Opt., 4(5): 523-525.
SYKES, S.M., ROBISON, W.G., WAXLER, M., & KUWABARA, T. (1981)
Damage to the monkey retina by broad-spectrum fluorescent
light. Invest. Ophthalmol. Vis. Sci., 20(4): 425-434.
TENGROTH, B.M. (1976) Safety glasses in welding. Env. Res.,
11:283-284.
TENGROTH, B.M., LYDAHL, E., & PHILIPSON, B.T. (1980) Infrared
cataract in furnacemen. In: Kelley, W.D., ed. Non-ionizing
radiation, Cincinnati, OH, ACGIH, pp. 169-170.
URBACH, R., ed. (1969) The biologic effects of ultraviolet
radiation, New York, Pergamon Press.
URBACH, R. (1980) Occupational skin hazards from ultraviolet
exposure. In: Kelley, W.D., ed. Non-ionizing radiation,
Cincinnati, OH, ACGIH, pp. 145-156.
US DHEW (1978) Performance standards for light emitting
products, (title 21, Code of Federal Regulations, part 1040),
Washington, DC, US Department of Health, Education and Welfare.
VAN DER LEUN, J.C. (1965) Theory of ultraviolet erythema.
Photochem. Photobiol., 4: 453-458.
VASSILIADIS, A. (1971) Ocular damage from laser radiation. In:
Wolbarsht, M.L., ed. Laser applications in medicine and
biology, New York, Plenum Press, pp. 125-162.
VASSILIADIS, A., ZWENG, H.C., & DEDRICK, K.G. (1971) Ocular
laser threshold investigations, Menlo Park, CA, Stanford
Research Institute (SRI Report No. 8209).
VOGT, A. (1919) [Experimental inducement of cataract by
isolated short-wave infrared mixed with red.] Klin. Mbl.
Augenheilkd., 63: 230-231 (in German).
VOS, J.J. (1966a) Heat-damage to the retina by lasers and
photocoagulators. Ophthalmologia (Basel), 151: 652-654.
VOS, J.J. (1966b) Some considerations on eye hazards with
lasers, Soesterberg, Institute for Perception RVO-TNO,
National Council for Applied Research in the Netherlands, 23
pp. (Report IZF 1966-4. AD 800156).
WEALE, R.A. (1982) The age variation of "senile" cataract in
various parts of the world. Br. J. Ophthalmol., 66: 31.34.
WHO SCIENTIFIC GROUP ON HEALTH FACTORS INVOLVED IN WORKING
UNDER CONDITIONS OF HEAT STRESS (1969) Report, Geneva, World
Health Organization (WHO Technical Report Series No. 412).
WHO (1979) Environmental Health Criteria 14: Ultraviolet
radiation, Geneva, World Health Organization.
WHO (l982) The SI for the health profession (reimpression)
Geneva, Switzerland, World Health Organization.
WILLIAMS, T.B. & BAKER, B.N., ed. (1980) The effects of
constant light on the visual process, New York, Plenum Press.
WOLBARSHT, M.L. (1971, 1974, 1978a) Lasers in medicine and
biology, New York, Plenum Press, Vols I, II, III.
WOLBARSHT, M.L. (1978b) The effects of optical radiation on
the anterior structures of the eye. In: Epstein, D. &
Tengroth, B., ed. Current concepts in ergophthalmology,
Stockholm, Department of Ophthalmology, Karolinska Institute,
pp. 29-46.
WOLBARSHT, M.L. & SLINEY, D.H. (1974) The formulation of
protection standards for lasers. In: Wolbarsht, M.L., ed.
Lasers in medicine and biology, New York, Plenum Press,
Vol. II, pp. 309-360.
WOLBARSHT, M.L., YAMANASHI, B.S., & ORR, M.A. (1977) The
origin of cataracts in the lens from infrared radiation,
Durham, NC, Duke University Eye Centre (Report 7-20-1977:
62772A 3E62772A813.00.013, Contract DAMD 17-74-C-4133, US Army
Med. Res. and Dev. Cmd).
WOLBARSHT, M.L., O'FEGHLUDHA, F.A., SLINEY, D.H., GUY, A.W.,
SMITH, A.A. Jr, & JOHNSON, G.A. (1980) Electromagnetic
emission from visual display units: a non-hazard. In: Kelley,
W.D., ed. Non-ionizing radiation, Cincinnati, OH, ACGIH,
pp. 193-201.
WREN, J.E., SCOTT, W.D., & BATES, C.E. (1977) Thermal and
mechanical properties of aluminized fabrics for use in ferrous
metal handling operations. Am. Ind. Hyg. Assoc. J., 38(11):
603-612.
YOUNG, R.W. (1980) A theory of central retinal disease. In:
Sears, M.L., ed. New directions in ophthalmic research,
New Haven, London, Yale University Press, pp. 237-270.
ZIGLER, J.S. & GOOSEY, J.D. (1981) Photosensitized oxidation
in the lens: evidence from photosensitizers endogenous to the
human lens. Photochem. Photobiol., 33: 689-874.
ZHOKOV, V.P., KOMAROVA, A.A., MAXIMOVA, L.I., MURATOV, V.P.,
PALTZEV, Yu.P., & SEMINOV, A.I. (1981) Occupational hygiene
and prevention of occupational diseases from lasers, Moscow,
Meditsina.
ZUCHLICH, J.A. & KURTIN, W.E. (1977) Oxygen dependence of
near-ultraviolet induced corneal damage. Photochem.
Photobiol., 25: 133-135.
ZUCHLICH, I.A. & TABOADA, J. (1978) Ocular hazard from UV
laser exhibiting self-mode-locking. Appl. Opt., 17: 1482-1484.
ZWICK, H. & BEATRICE, E.S. (1978) Long-term changes in
spectral sensitivity after low-level laser (5l4 nm) exposure.
Mod. Probl. Ophthalmol., 19: 319-325.
GLOSSARY
ACOUSTICO-OPTIC: involving the interaction of light and an acoustic
wave. Acoustico-optic devices such as Q switches and modulators
are used in manipulating laser beams.
ACTIVE MEDIUM: the atomic or molecular species which can provide
gain for laser oscillation. Also called laser medium, lasing
medium or active material.
ANGSTROM (A): a non-SI unit equal to 10-10 metre. Its use as a
unit of optical wavelength has largely been supplanted in recent
years by the nanometre (10-9 metre).
ARC LAMP: an electric lamp in which current passes through the
ionized air between two electrodes, giving off light. Applications
include laser excitation.
ATOMIC LASER: a gas laser in which the active material is an atomic
species rather than a molecule.
ATTENUATION: reduction in intensity that results when optical
radiation travels through an absorbing or scattering medium. In
optical fibre, attenuation (in decibels) equals 10 log ( Po/ Pin),
where Po is the power at the output end of the fibre and Pin is
the power launched into the fibre.
AVERAGE POWER: in a repetitively pulsed laser, the energy per pulse
times the repetition rate. When the energy per pulse is expressed
in joules and the repetition rate in hertz, the average power is
expressed in watts.
BEAM DIAMETER: the distance between the two opposing points at
which the irradiance or radiant exposure is a specified fraction
(typically 1/e or 1/e2) of the irradiance or radiant exposure of
the emitted radiation.
BEAM DIVERGENCE: the increase in beam diameter with distance from
the laser's exit aperture. Measured in milliradians at specified
points, usually where irradiance or radiant exposure is 1/e or 1/e2
the maximum value, and expressed as the "full-angle" divergence.
BOLOMETER: a type of detector which measures infrared radiation by
the temperature-induced change of resistance in a metal foil
exposed to the radiation and heated by it.
BREWSTER ANGLE: the angle between an incident beam of light and a
dielectric reflecting surface at which none of the light polarized
in the plane of incidence is reflected. Brewster's angle is
tan-1 n2/ n1, where n1, and n2 are the indexes of refraction of the
first and second media respectively. A window mounted at
Brewster's angle with respect to an incident beam is often used as
a window in laser cavities.
CALORIMETER: a type of detector that measures heat produced by
absorption of radiation.
CHEMICAL LASER: a type of laser in which the population inversion
is produced directly by an "elementary" chemical reaction (a
collision process in which one or more molecules undergo changes in
their chemical bonds).
COHERENCE: a fixed phase relationship among various points of an
electromagnetic wave in space (spatial coherence) or in time
(temporal coherence).
COLLIMATOR: an optical device for converting a diverging or
converging beam of light into a collimated or parallel beam, or for
expanding or reducing the cross-sectional area of an incident
collimated beam. A target collimator projects a parallel beam from
its own light source such that, viewed from any distance, the light
source appears to be at infinity.
CONTINUOUS WAVE (cw) LASER OPERATION: laser operation in which
radiation is emitted continuously.
CORE: the central region of an optical fibre. The core must have a
higher refractive index than the cladding for light to be
transmitted through the fibre via total internal reflection
CORNER CUBE: an optical component with three mutually perpendicular
faces and a hypotenuse face. Because light entering through the
hypotenuse is totally internally reflected at each perpendicular
face, the cube acts as a retroreflector. Also known as corner
reflector.
CRYSTAL LASER: a type of laser in which the active medium is an
atomic species in a crystal such as ruby, YAG (yttrium aluminium
garnet), or YALO (yttrium aluminate).
DETECTOR: see PHOTODETECTOR.
DIFFRACTION: deviation of light rays from the paths predicted by
geometical optics.
DIODE LASER: see SEMICONDUCTOR LASER.
DISPERSION: variation of the refractive index of an optical
material with change in wavelength, as in a prism; in an optical
fibre, the temporal spreading of a light pulse due to the fibre's
different propagation speeds for different wavelengths and modes of
light. Such spreading limits the fibre's information-carrying
capacity of bandwidth.
DIVERGENCE: see BEAM DIVERGENCE.
DYE LASER: a type of laser in which the active medium is an organic
dye, generally in solution with the liquid either flowing or
encapsulated within a cell. Experimental solid and gas dye lasers
also have been built. Also called organic-dye, tunable-dye or
liquid laser.
ELECTRON-BEAM-SUSTAINED LASER: a molecular-gas laser in which the
electrical discharge is sustained with a beam of high-energy
electrons. Usually injected transversely to the laser cavity's
optical axis, the electron beam permits laser operation at
pressures and cross-section-to-length ratios higher than possible
with an unsustained discharge. This technique is often used in
commercial carbon-dioxide lasers with very high continuous-wave
output power.
ELECTRO-OPTIC: applying to modulators, Q switches and other beam-
manipulating devices in which operation relies on modification of a
material's refractive indices by an applied electrical field. In a
Kerr cell the index change is proportional to the square of the
electrical field, and the material is usually a liquid. In a
Pockels cell the material is a crystal whose index change is linear
with the electric field.
EMISSIVITY: ratio of radiant exitance of a thermal radiator to that
of a full radiator (black body) at the same temperature - (ISO
31/VI 1980).
EXCIMER LASER: a laser in which the active medium is an excimer, a
molecule which is chemically unstable except in its excited state.
The term often is applied to lasers in which the active medium is a
rare-gas halide (or monohalide) excimer such as KrF* or XeF*.
GAS LASER: a type of laser in which the active medium is a gas.
The category is subclassified according to the active medium into
atomic (such as helium-neon), molecular (carbon dioxide, hydrogen
cyanide and water vapour), ionic (argon, krypton, xenon, and the
metal-vapour types such as helium-cadmium and helium-selenium), and
excimer (typically rare-gas halides). Loosely applied, "ion" means
argon and krypton.
GLASS LASER: a type of solid-state laser in which the active medium
is a glass rod doped with rare-earth atoms, usually neodymium.
HERTZ (Hz): the SI unit of frequency of periodic phenomena. It
replaces the non-SI unit "cycles per second". The number of pulses
per second that a laser can produce may be expressed in hertz.
HOLOGRAM: a recording of the interference of coherent light
reflected from an object with light direct from the same source or
reflected from a mirror. Illumination of the hologram reproduces
the object's three-dimensional image.
IMAGE CONVERTER: an electron tube which produces a visual replica
of an image formed on its cathode by some form of electromagnetic
radiation. In an image converter camera, the image formed by the
electron tube is focused on to photographic film for a permanent
record.
INFRARED: electromagnetic radiation with wavelength between 0.76
micrometre and about 1 millimetre. Wavelengths at the shorter end
of this range are frequently called "near" infrared, and those
longer than about 20 micrometres, "far" infrared.
INTEGRATED OPTICS: devices in which several optical components are
"integrated" on to a single substrate; analogous to integrated
electronic circuits. Although still in the research phase,
integrated optics has potential for use in optical signal
processing and in fibre-optic communications.
INTERFERENCE FILTER: an optical component which depends on
interference in a series of thin films deposited on a substrate to
limit transmission to a desired spectral band.
ION LASER: a type in which the active element is an ionized gas,
generally argon or krypton.
IRRADIANCE ( E): radiant flux per unit area, expressed in watts per
square centimetre.
LASER: acronym for "light amplication by stimulated emission of
radiation." A device which generates or amplifies electromagnetic
oscillations at wavelengths between the far infrared
(submillimetre) and ultraviolet. Like any electromagnetic
oscillator, a laser oscillator consists of two basic elements: an
amplifying (active) medium and a regeneration or feedback device
(resonant cavity). A laser's amplifying medium can be a gas,
semiconductor, dye solution, etc; feedback is typically from two
mirrors. Distinctive properties of the electromagnetic
oscillations produced include monochromaticity, high intensity,
small beam divergence, and phase coherence. As a description of a
device, "laser" refers to the active medium plus all equipment
necessary to produce the effect called lasing.
LASER DIODE: see SEMICONDUCTOR LASER.
LED: abbreviation of light-emitting diode. A semiconductor
emitting incoherent light into a broad field of view, used in low-
speed or short-haul fibre-optic links. Most LEDs used in fibre-
optic applications emit in the near infrared.
LIDAR: acronym for "light detection and ranging," a system
employing a laser beam to gather ranging information as well as
intelligence on reflection and scattering of light by clouds and
atmospheric pollutants.
LIQUID LASER: a type in which the active element is either an
organic dye or an inorganic liquid. See also DYE LASER.
MULTIMODE: emission at several frequencies simultaneously,
generally closely spaced, each frequency representing a different
mode of laser oscillation inthe resonant cavity.
Nd-GLASS: neodymium-doped glass, used in some solid state lasers.
The neodymium atoms are the active medium.
Nd-YAG: neodymium-doped yttrium-aluminium-garnet (YAG), a crystal
which is used in some solid state lasers. The neodymium atoms are
the active medium.
NEUTRAL DENSITY FILTER: a filter which reduces the intensity of
light without affecting its spectral character.
NONLINEAR EFFECTS: changes in a medium transmitting electromagnetic
waves that are proportional to the second, third or higher powers
of external electric field. Nonlinear optical effects include
harmonic generation and the electro-optic effect. See electro-
optic.
OPTICALLY PUMPED LASER: a laser whose active medium is excited by
another light source to produce a population inversion. For solid-
state and some dye lasers this source usually is an incoherent type
such as a flash- or arc-lamp. For gas and other dye lasers,
coherent laser sources generally provide such optical pumping.
PARAMETRIC OSCILLATOR: a nonlinear device, usually a crystal, which
produces tunable laser oscillations at the sum or difference
frequency of mixed laser beams. Also called tunable parametric
oscillator or optical parametric oscillator. Loosely applied to
the complete instrument containing the pump laser and the tuning
crystal.
PHOTODETECTOR: any device which detects light, generally producing
an electronic signal with intensity proportional to that of the
incident light.
PHOTON: a massless "particle" of electromagnetic radiation, with
energy equal to hc/lambda where h is Planck's constant (6.6 x 10-34
joule second) and c/lambda is the frequency of the radiation (speed
of light divided by wavelength).
POLARIZER: an optical component which only transmits lightwaves
that oscillate in a given plane.
POPULATION INVERSION: a condition in which most atoms of a species
are in an excited, metastable state. Collision of a photon with
such an atom causes the atom to relax to a lower energy state, and
to emit a second photon, amplifying the light signal. Population
inversion is required for lasing to occur.
PULSELENGTH: the duration of the burst of energy emitted by a
pulsed or Q-switched laser. Expressed in seconds and usually
measured at the half-power (half the full height of a voltage or
current pulse). Also called pulsewidth.
PULSED LASER: a laser that emits light in pulses rather than
continuously.
PUMP: the energy source (such as flashlamp, electron beam or
current supply) that drives the amplification in the active medium
of a laser by creating a population inversion.
PYROELECTRIC CRYSTAL: a type of crystal that shows electrical
effects when its temperature is changed; these effects are used to
detect infrared radiation.
Q SWITCH: essentially a "shutter" which prevents laser emission
until opened. Q stands for "quality factor" of the laser's
resonant cavity. "Active" Q switching is achieved with a rotating
mirror or prism, Kerr or Pockels cell, or acoustico-optic device;
"passive" Q switching is achieved with a saturable absorber such as
a gas or dye. In a pulsed laser a Q switch increases pulse power
by shortening pulse duration while not significantly decreasing the
energy; in a continuous wave laser the device provides shorter and
more intense pulses at a higher repetition rate than could be
achieved by pulsing the laser directly.
RADIANCE ( L): At a point of a surface and in a given direction,
the radiant intensity of an element of the surface, divided by the
area of the orthogonal projection of this element on a plane
perpendicular to the given direction (ISO 31/6-1980). Expressed in
watts per steradian square centimetre.
RADIANT FLUX: the rate of flow of radiant energy, measured in
watts.
RADIOMETER: an instrument for measuring incident radiation in
radiometric units (watts). Radiometric measurements can be made at
any wavelength, but the spectral range of a particular instrument
may be limited to a narrow range.
RADIOMETRIC UNITS: units defined for measurement of the intensity
of electromagnetic radiation; the basic unit is the SI unit watt.
RAMAN EFFECT: the appearance of additional weak lines in the
spectrum of light that has been scattered by a transparent
substance. The extra lines result from rotational or vibrational
transitions of the molecules in the scattering medium. If the
medium is illuminated with laser light of sufficient intensity, the
emission at the Raman frequencies is amplified, exhibiting
characteristics of stimulated emission (i.e., stimulated Raman
effect.).
REFLECTANCE: the ratio of wave energy reflected from a surface to
the wave energy incident on a surface.
SEMICONDUCTOR LASER: a type in which the active material is a
semiconductor, either a diode or homogeneous. Commercial
types are generally diodes in which lasing occurs at the
junction of n-type and p-type semiconductors, usually gallium-
arsenide or gallium-aluminium-arsenide. Homogeneous types are
made of undoped semiconductor material and are pumped by an
electron beam.
SOLID-STATE LASER: a type the active medium of which is an atomic
species in a glass or crystal. The atomic species may be added to
the glass or crystal, as neodymium is added to glass, or may be
instrinic, as chromium is in ruby. This term is generally not
applied to semiconductor lasers.
SUPER-RADIANT: applying to coherent optical amplification of
spontaneous emission that occurs without relaxation processes.
Commonly used to describe a laser whose gain is high enough to
permit amplification without mirrors; examples are nitrogen and
molecular hydrogen. Beam quality of a super radiant laser is
generally inferior to that of a laser with a complete optical
cavity. "Super-fluorescent" has been proposed as a more precise
description of this type of laser.
TEA LASER: acronym for transversely excited, atmospheric pressure
laser. A gas laser in which excitation of the active medium is
transverse to the flow of the medium. Because of shorter breakdown
length, this type operates in a gas-pressure range higher than that
for longitudinally excited gas lasers (but not necessarily
atmospheric) and offers a potentially higher power output per unit
volumes because of a greater density of lasing molecules.
TUNABLE LASER: a laser or a parametric oscillator whose emission
can be varied across a broad spectral range.
ULTRAVIOLET: electromagnetic radiation with wavelengths between
about 40 and 400 nanometres. Radiation between 40 and 200 nm is
termed "vacuum ultraviolet" because it is absorbed by air and
travels only through a vacuum. The "near" ultraviolet has
wavelengths close to those of visible light; the "far" ultraviolet
has shorter wavelengths.
YAG: yttrium aluminium garnet, a crystal host which can be doped
with an active laser medium, usually neodymium.
YALO: yttrium aluminate (YA103), a crystal host doped with an
active laser medium, usually neodymium.
YLF: yttrium lithium fluoride, a crystal host which can be doped
with an active laser ion, usually holmium.
Absolute values of spectral reflectance are relatively
unimportant because such values vary only by a factor of 10 - 20,
whereas the laser beam irradiance may exceed the applicable EL by
orders of magnitude above this factor.
Most reported laser accidents have occurred, when the
probability of exposure was very high. No discussion of reflection
hazards is therefore complete without the consideration of the
probability of exposure. It must be remembered that the underlying
philosophy of the classification system is that control measures
should increase with increasing risk of exposure as well as with
increased severity of exposure.
12.2.2. Retroreflection
Some materials exhibit a property known as retrodirective
reflection. The reflection does not obey either the law of regular
(specular) reflection, or the cosine dependence of Lambertian
reflection. A collimated indigent beam may remain collimated and
be redirected along the original axis of propagation, regardless of
the angle of incidence at the retroflector. Corner cubes and some
specialized highway signs are examples of retroflectors.
12.2.3. Optically aided viewing
Nearly all laser workers know that viewing a laser source with
a telescope may substantially increase the risk. This increase in
risk is most dramatic for intra-beam viewing of a collimated
source. In this case, an increase in the power entering the eye is
possible, because the diameter of the objective (Do) of the
telescope or binocular is much larger than the pupil of the eye dp.
The actual increase in risk (G) depends on whether the pupil of the
eye is larger or smaller than the exit pupil (De) of the optical
system, the spectral transmittance (taulambda) of the optical
system at the laser wavelength(s), and the beam diameter relative
to the objective (collecting aperture) diameter.
When a bright object, larger than a point source, is viewed
through a well-designed optical system, the radiant power reaching
the retina (visible and IR-A) is theoretically increased by the
square of the instrument's magnifying power. However, since there
is a commensurate increase in the area of the retinal image, the
retinal irradiance remains unchanged, except for a slight reduction
because of reflective loss and the absorption of light in the
optical system. The retinal hazard in this case may increase in
some instances, since the thermal retinal injury threshold
decreases with increasing image size.
13. ACCIDENTAL INJURIES
At present, retinal injuries with loss of sight following
exposure to visible and IR-A laser radiation have been the most
catastrophic of all effects from laser radiation (Boldry et al.,
1981; Zhokov, 1981). Though the relatively high-powered, far-
infrared lasers such as the cw, carbon-dioxide laser, have caused
numerous burns to the hands and clothes, these are considered
inconsequential in comparison with the serious retinal injuries.
One postal survey conducted several years ago (Rockwell & Goldman,
1974) appeared to indicate that there had been at least 100
injuries to the eye from laser radiation in the USA. One
subjective account in this regard was that of Decker (1977).
Despite such reports, surprisingly few serious injuries of the
eye have been reported in the last 15 years in relation to exposure
to pulsed lasers. This low accident rate cannot be accounted for
by assuming that the ocular ELs are too conservative. The
explanation is probably that accidental exposure of the eye to a
collimated beam is normally an extremely remote possibility, if
precautions are taken to keep the eye out of the beam. One of the
few situations in which the probability of hazardous exposure is
great is during work in the laboratory and, each year, several
retinal injuries are reported under these conditions. However, it
is difficult to ascertain the exposure conditions in sufficient
detail for useful threshold or injury data to be derived. Concern
may also exist regarding the potential bias in an individual's
description of the accidental exposure conditions to support a
claim of compliance with safety measures. It is not clear whether
laser exposures are always detected by the exposed individual, and
this may be a particular problem with IR lasers (Kasuba & Akifev,
1977). It is known that retinal injury outside the macula may have
little or no effect on everyday visual performance and therefore
may not be detected subjectively.
14. CONTROL MEASURES
Risk control guidelines are not mutually exclusive. Following
one or two guidelines may reduce the risk to such an extent that
other recommended control measures, in that particular class, are
no longer essential. For example, if the beam path of a Class 4
laser were enclosed, then it would hardly be necessary to remove
all glass objects, or other specular surfaces near the beam path
but outside the enclosure, nor would it seem necessary to wear eye
protectors. However, the eye protection might be necessary if the
enclosure were being modified or during initial alignment. The
decision to use any particular set of controls depends on use
conditions and whether general population exposure is likely.
Table 15 provides a brief list of the most commonly recommended
laser control measures.
Table 15. Control measures for general population and occupational
exposure
-------------------------------------------------------------------
I Engineering control measures:
protective housing enclosure and service panel requirements;
interlocks on the protective housing;
door interlocks and remote control connector;
beam attenuator or beam shutter;
key switch or padlock over aperture cover;
filtered viewing optics and windows;
emission delay (BRH);
warning lights;
emission indicators (audible or visible);
enclosed area or room;
beam enclosure;
remote firing and/or monitoring;
II Personal protective equipment:
eyewear;
clothing;
gloves;
III Administrative and procedural controls:
laser safety officer;
standard operating procedures (SOPs);
limitations on use by class;
education and training;
maintenance and servicing manuals;
marking of protective devices;
warning signs and labels;
entry limitations for visitors, etc.;
accident procedures.
-------------------------------------------------------------------
Because of the risk associated with exposure to Class 4 high-
risk lasers, the safety precautions associated with these laser
installations indoors, generally include the installation of door
interlocks to prevent exposure of unauthorized or transient
personnel entering the laboratory, the use of baffles to terminate
the primary and any secondary beams, and the use of safety eyewear
by personnel within the interlocked facility (Klost, 1971).
At one time, it was recommended that ambient light levels
should be sufficient to constrict pupils. However, since a
constricted pupil provides only a small safety factor, the
requirement for good illumination, which remains in present safety
standards, is related to good general visibility, as the wearing of
eye protectors reduces visual capabilities. Light-coloured, matt
surfaces in the room minimize glare, and thus promote visibility.
In summary, the ability to analyse potential risks from any
laser system is enhanced by a broad knowledge of optics, general
laser technology, and the imaging process of the human eye. A
laser safety specialist should have a general background knowledge
of optics with the basic knowledge necessary to perform a risk
analysis. It has been shown that the risk analysis depends on at
least three aspects - the laser system and its potential hazards,
the type of personnel who may be exposed, and, finally, the
reflective materials and other optically important materials in the
environment that can influence the risk analysis.
15. HAZARDS OF LAMP SOURCES AND PROJECTION SYSTEMS
The optical radiation emitted by a conventional light source,
either a bare lamp, a luminaire, or a projection system, can be
evaluated using the previously mentioned tentative exposure limits
or guidelines.
Prior to exhaustive measurements and safety calculations, it
may be worthwhile to determine the need for a comprehensive risk
evaluation. Many categories of lamps or other types of light
sources can be excluded from all or several of the evaluations.
The following multi-step scheme (Sliney & Wolbarsht, 1980) may be
useful in this regard.
STEP 1 - Categorization of the lamp. Certain hazards are specific
for certain types of lamp or light source. The following grouping
is useful:
(a) incandescent lamps and incandescent heating sources;
(b) low-pressure discharge lamps;
(c) fluorescent lamps;
(d) high-intensity discharge (HID) lamps;
(e) short-arc (compact arc) lamps;
(f) carbon arcs;
(g) solid-state sources (LEDs etc.);
(h) cathode-ray tubes (CRTs).
STEP 2 - Determination of the source envelope. Any glass between
the actual source of radiation (e.g., the arc or tungsten filament)
and the point of access can greatly influence the potential hazard.
Soft (lime) glass of any reasonable thickness will greatly
attenuate UV-B and UV-C radiation.
(a) Incandescent lamps, other than quartz-halide lamps,
normally have a sufficiently thick glass envelope to
completely preclude a UVR hazard. The blue-light
hazard does not appear to be theoretically possible
at black-body temperatures below 2000 K (Sliney &
Wolbarsht, 1980), but most filaments operate at
effective temperatures exceeding 2000 K.
(b) Low-pressure discharge lamps. Low-pressure discharge
lamps do not normally present a retinal hazard,
because of the relatively low radiance. Only lamps
with quartz envelopes can transmit sufficient UV-B
and UV-C to be of concern. Of the common low-pressure
lamps, only mercury lamps can create a severe UVR
hazard. Many may be quite hot to the touch.
(c) Fluorescent lamps. Low-pressure tubular lamps in
almost all cases have a thin glass envelope, but
could often present a potential UVR hazard at the
surface. They do not represent a thermal retinal
injury hazard and seldom a blue-light hazard.
(d) HID lamps. These lamps may present both blue-light
and thermal retinal hazards, and possible UVR
hazards. Since most lamp envelopes are glass, there
is little UV-B leakage. Nevertheless, the UV-B
leakage may be of concern at very short distances.
Quartz-mercury HID lamps require a UVR risk
evaluation. If the outer glass envelope of an HID
lamp breaks, hazardous UV levels will be emitted.
Governmental regulations in Canada and the USA
require HID lamps to have a self-extinguishing
feature to preclude this hazard, unless the packaging
clearly warns against use without adequate shielding.
(e) Short-arc lamps. Of all the electric lamp categories,
this group will require the most extensive risk
evaluation. All potential hazards may be present
(UV-B/C, UV-A, blue-light, retinal thermal injury,
and skin thermal injury). Because of the high
temperature of the arc, a quartz envelope (which
transmits UV-B and C) is characteristic. These lamps
are often used in UV photocuring processes in
industry (Moss, 1980).
(f) Carbon arcs. Where a glass lens or filter plate does
not exist between the open arc and a point of access,
the carbon arc, like the short-arc lamp, is
potentially injurious.
(g) Solid-state lamps (e.g., LEDs). The present solid-
state lamps including LEDs, which emit visible
radiation, do not present any health risk, regardless
of the type of envelope.
(h) Cathode-ray tubes (CRTs). Present CRTs emit optical
radiation at levels that could pose a potential
health hazard (Wolbarsht et al., 1980).
STEP 3 - The obtaining of available manufacturers' radiometric and
photometric data and lamp descriptions. Any radiometric or
photometric specification may be of value either for calculation or
for direct intercomparison with measurements. Spectral data are
most useful. The dimensions of the emitting area of the lamp will
be required for retinal hazard evaluation.
STEP 4 - Comparison of lamp specifications with those of previously
evaluated lamps. From experience, it is often possible to complete
the risk evaluation with this step.
STEP 5 - Performance of detailed spectroradiometric measurements,
when necessary. In addition, where feasible, measurements of
luminance, illuminance, and total irradiance should be performed.
These will provide confirmation of the spectroradiometric
measurements. The pulse duration must be measured for a pulsed
source.
STEP 6 - Determination of the source dimensions. A photograph and
microdensitometer scan of the negative may be necessary for a non-
uniform source. The maximum angular subtense alpha of the source
should be calculated at the point of human access or at 15 cm from
the source, whichever is closer.
STEP 7 - Estimation of the exposure and comparison with the
exposure limits to determine the degree of risk.
STEP 8 - Consideration of potentially hazardous failure modes. For
example, breakage of the outer envelope of some high-intensity
discharge (HID) lamps can create a serious UVR hazard (Anderson,
1980b).
16. PROJECTION OPTICS
Broad-band sources involving projection optics are most
difficult to evaluate. Besides the problems encountered in
evaluating exposed lamps, the projected beam and projected source
size must be characterized. When viewing a collimated light source
from within the beam (other than a laser), a magnified view of the
actual source will be seen. The source is generally a high-
brightness lamp. The brighter the lamp, the greater the maximal
irradiance in the projected beam. This is a consequence of the Law
of Conservation of Brightness (Radiance) (see, for example, Kline,
1970; or Sliney & Wolbarsht, 1980). Some usually safe lamps become
hazardous to view through projection optics, despite the fact that
the optics cannot make the lamp brighter. The risk increases
because of the dependence of retinal injury on image size. Besides
the obvious projection sources - such as spotlights, searchlights,
slide projectors, and film projectors - solar concentrators and
other non-imaging light collectors may also require risk
evaluation. From the Law of Conservation of Radiance, it is
possible to evaluate the retinal risks from projector systems.
Collimating optics may consist of refracting elements (lenses),
reflecting elements (curved mirrors), or both.
17. SAFETY GUIDELINES FOR HIGH-INTENSITY SOURCES
Since lamp or arc sources may be hazardous from several
aspects, it may be helpful to develop a safety classification
scheme, similar to the one applied to laser products. The
following scheme of Sliney & Wolbarsht (1980) illustrates this
approach to evaluate the retinal risks from projector systems.
Both lamps and total lighting systems could be included. The
categories could be as follows:
Safety Group 1: Safe sources. These lamps are considered
safe to view throughout the day. No warning label would be
required. Examples: a frosted 15-W filament lamp or a
TV-display, cathode-ray tube.
Safety Group 2: Low-risk sources. These lamps are safe
for momentary 0.25-s, unintentional viewing. Examples:
most spotlights and film-projector lamp bulbs. A caution
label should be required on the lamp base, and possibly on
the projection system itself. No ultraviolet or infrared
hazard would exist at distances of more than 10 cm from
the lamp or projected beam.
Safety Group 3: Moderate-risk sources. These lamps would
be unsafe to view at close range, even momentarily.
Presumably, skin injury could also occur from ultraviolet
radiation as from germicidal lamps, sun lamps, and high
intensity UV-A lamps. A danger-label, clearly visible on
the equipment, could be required. A common lamp that might
fit into this category would be a 600-1000-W tungsten-
halogen lamp without a Fresnel lens, such as is used for a
home cine film spot lamp. The emergent beam irradiance is
far in excess of that required to ignite paper within half
a metre of the source. Obviously, the basis for the
determination of a hazard classification would differ
according to whether the hazard classification criteria
were based on retinal or skin injury. Each measurement for
classification would be for a specified accessible
approach distance, using a standard aperture and solid
angle of acceptance. The minimum approach distance could
vary with application. Other examples that might be
included in this category are some very high intensity,
short-pulse, laser flash tubes, and 20 kW xenon-arc
searchlights.
Safety Group 4: High-risk sources. These sources would
cause skin burns and/or erythema within a standardized
period of exposure (e.g., within 10 s) at a standardized
distance at which the effective UV irradiance would exceed
3 W/m2 (0.3 mW/cm2), or the total irradiance across the
entire spectrum would exceed 2 kW/m2 (0.2 W/cm2). Examples
of such sources are an open carbon-arc spotlight or an
open 1-kW mercury lamp. It may be that safety groups 3 and
4 are so similar in degree of risk, that they could be
combined.
18. WELDING ARCS
The most common high-intensity arc is probably the welding arc.
These arcs vary in brightness and in UVR content, primarily
according to the arc current, type of shielding gas, and the metals
being welded.
The greatest population exposed to intense sources of optical
radiation are welders and their assistants. The American Welding
Society estimated that there may be as many as 500 000 welders in
the USA alone (Emmett & Horstman, 1976). The two broad categories
of welding equipment are gas (acetylene) welding equipment and
electric-arc welding equipment. A gas welding torch or cutting
torch has a luminance not much greater than a candle flame,
typically ranging from 10 to 200 kcd/m2 (1-20 cd/cm2), and the UVR
emission is quite small. The optical radiation hazards of such
torches are virtually nonexistant. Welding filter goggles used
with such torches are to reduce glare, and are little darker than
very dark sunglasses having a shade number of the order of 3 - 5
(visual transmittance of 5 - 15 %). On the other hand, electric
welding arcs may be 1000 times brighter than gas torches and emit
UVR at proportionately higher levels (Sutter et al., 1972).
Protective shields, curtains, screens for bystanders, and
welders' goggles are the standard protective equipment used in
welding (Mayer et al., 1979; Sliney et al., 1981). Protective
procedures and protective equipment for the welder have been
developed empirically over the last three-quarters of a century.
Only very recently have detailed measurements of the radiometric
output of welding arcs been available. When these measurements
were carefully compared with exposure limits being developed for
protection against bright light sources, it was shown that the
empirically-developed protective equipment standards were adequate.
19. EYE AND SKIN PROTECTION
19.1. Laser Safety Eyewear
From a safety point of view, the most desirable laser hazard
control measure is complete enclosure of the laser or laser system;
however, this may not always be practical and laser eye protectors
are generally the best alternative. Though most industrial laser
applications do not require the use of eye protectors, this is not
always true for laser applications in the research laboratory. Eye
protectors provide the simplest solution to the laser safety
problem for a constantly changing experimental arrangement. Several
factors play a role in determining whether eyewear is necessary in
any situation. At least three output parameters of the laser must
be known: maximum exposure duration, wavelength, and output power
(or output irradiance, or radiant exposure, or energy), as well as
the applicable safe corneal radiant exposure. In addition, some
knowledge of such environmental factors as ambient lighting and the
nature of the laser operation may also be required.
Laser eye protection generally consists of a filter (often
composed of several individual filter plates) which selectively
attenuates at specific laser wavelengths, but elsewhere transmits
as much visible radiation as possible (Swope & Koester, 1965;
Schreibeis, 1968; Scherr et al., 1969; Swope, 1969, 1970; Straub,
1970; Sliney, 1974). Eyewear is available in several designs -
spectacles, coverall types with opaque side-shields, and coverall
types with somewhat transparent filter side-shields. The selection
of appropriate laser protective eyewear may be complex (Envall &
Murray, 1979). Active electronic imaging devices have also served
an additional role, as eye protection.
19.2. Welders' Filters
Eye protection filters, which were originally developed for
welders, were based more on available materials than on knowledge
of ocular protection requirements. The first organized study of
glass filter materials was carried out by Sir William Crookes
(1914) in England. Optical transmission characteristics are now
standardized as "shades" and specified for particular applications
(Coblentz et al., 1931; Stair, 1948; ANSI, 1978). Though maximum
transmittances for ultraviolet and infrared radiation are specified
for each shade, the mean photopic visual transmittance tauv, or
visual optical density Dv, has traditionally been used to define
the shade number S:
S = (7/3) Dv + 1 = - ln tauv + 1 Equation (23)
or Dv = (3/7) (S - 1) Equation (24)
where Dv = -log10 tauv Equation (25)
19.3 Eye Protection for Furnace Radiation
As well as protective clothing and equipment, many industrial
methods now used probably reduce the level of glass furnace
radiation to which the eye is exposed. For instance, the openings
to higher temperature furnaces are a great deal smaller than they
have been in past years; this would reduce the total irradiance of
the eye from infrared radiation. There are sufficient data and
cases of a very specific form of cataract in workers to suggest
that infrared does, indeed, cause glass-blower's or furnaceman's
cataract (Duke-Elder, 1972).
19.4. Eye Protection Filters for Solar Radiation
Direct viewing of the sun, for whatever reason, requires
protection against several different portions of the spectrum. A
yellowish or reddish filter generally protects against ultraviolet
radiation. Protection against intense visible rays should be
weighted to filter out more of the blue-light than the rest of the
visible spectrum. It is generally found that a shade 12 or 13
welder's filter is quite adequate to protect against ultraviolet
radiation, infrared, and visible radiation. The protection
afforded against the IR, however, is far greater than necessary.
The use of darkened coloured slides is not advisable, since
these slides (usually made by developing unexposed colour film) use
organic dyes that transmit in the near-infrared (IR-A) spectral
band.
19.5. Skin Protecting Agents for UVR (Sunscreens)
A number of topical, physical, and chemical screening agents
have been developed that provide nearly total or partial filtration
of ultraviolet radiation. Since actinic UV-B and UV-C radiation
are the most hazardous, efforts to develop topical agents have
concentrated primarily on filtering out this type of radiation. The
chemical agents in these "sunscreens" include para-aminobenzoic
acids (PABA) and its esters, salicylates, and cyanamates. These
materials are mixed in solution with substances that have good
substantivity (i.e., adhere to the skin) (Dahling et al., 1970;
Fitzpatrick et al., 1974).
19.6. Protective Garments
Aluminized fabrics were greatly improved during various manned
space programmes (Stoll & Chiantra, 1971). Such fabrics, when used
in thermal protective garments, have been shown to offer equivalent
or superior reflective and mechanical properties compared with
conventional aluminized asbestos garments (Wren et al., 1977).
Aluminized rayon (basket weave) and certain aluminized cottons were
shown to allow the least transmission of infrared radiation.
20. MEDICAL SURVEILLANCE (RATIONALE)
In the past two decades, many employees working routinely with
lasers have been subjected to preplacement, periodic, and end-of-
job eye examinations in order to obtain sufficient information
concerning the risk of retinal damage. Many of these studies
indicated that periodic eye examinations rarely located hitherto
unsuspected retinal damage. In general, published reports of
ophthalmic accidents have been those in which the acute over-
exposure was sufficient to subjectively alert the individual
(Hathaway et al., 1977). Thus, many authorities (Suess, ed., 1982)
suggest that ophthalmic examinations are unnecessary for
individuals routinely working with Class 1 and 2 lasers, and that,
if requested, the examinations should be confined to those working
with Class 3 or 4 systems only.
An examination is required within 24 - 48 h of any event in
which the worker suspects, or knows, that the eye might have been
exposed. Laser lesions change in appearance and may even tend to
disappear within the heterogeneous appearance of the fundus within
a period of time, so that ophthalmic examinations, some time after
exposure, may be difficult to interpret.
21. FORMAL TRAINING FOR LASER WORKERS
It is necessary to establish a safety programme that assures
the safe use of lasers and other radiation sources. To assure
knowledge of, and compliance with, applicable standards, a certain
amount of formalized teaching is often necessary.
At work places, a specific individual should be assigned to
maintain and enforce the safety programme (in some countries this
individual is termed a laser safety officer (LSO)).
All workers occupied with, or working near, the radiation
source should be included in the teaching programme.
The object is to make workers and work leaders aware of the
risks of lasers, how to avoid the hazards, the proper use of
protective devices, and how to realize when overexposure has taken
place.
REFERENCES
ALLEN, R.G. (1980) Retinal thermal injury. In: Kelley, W.D.,
ed. Non-ionizing radiation, Cincinnati, OH, ACGIH, pp. 161-168.
ACGIH (1976) A guide for control of laser hazards, Cincinnati,
OH, American Conference of Governmental Industrial Hygienists.
ACGIH (1981) Threshold limit values for chemical substances
and physical agents in the workroom adopted by ACGIH for 1981,
Cincinnati, OH, American Conference of Governmental Industrial
Hygienists.
ANDERSON, F.A. (1980a) The biological basis for standards,
Rockville, MD, US Dept. of Health, Education and Welfare, Food
and Drug Administration, Bureau of Radiological Health.
ANDERSON, F.A. (1980b) Sodium and mercury vaporlamps. In:
Kelley, W.D., ed. Non-ionizing radiation, Cincinnati, OH,
ACGIH, pp. 239-243.
ANDERSON, R.R. & PARRISH, J.A. (1981) The optics of human
skin. J. Invest. Derm., 77: 13-19.
ANSI (1978) Standard practice for occupational eye, and face
protection, New York, American National Standards Institute
(ANSI Standard Z-89.1).
ANSI (1980) Safe use of lasers, New York, American National
Standards Institute (ANSI Standard Z-136.1).
AVDEEV, P.S., BEREZIN, Yu.D., GUDAKOVSKII, Yu.P., MURATOV,
V.R., MURZIN, A.G., & FROMZEL, V.A. (1978) Experimental
determination of maximum permissible exposure to laser
radiation of 1.54 µ wavelength. Sov. J. quant. Electr., 8:
134-141.
BEATRICE, E.S. & LUND, D.J. (1979) Characteristics of damage
produced by non-circular retinal laser radiation, San
Francisco, CA, Letterman Army Institute of Research,
(Institute Report No. 31, AD-AD35 878/8ST).
BEATRICE, E.S. & VELEZ, S. (1978) Laser safety bioeffects
research: histopathology of retinal effects. In: SPIE Proc.,
Visual simulation: 162: 103-106.
BERGQUIST, T., HARTMANN, B., & KLEMAN, B. (1978) Imaging
properties of the eye and interaction of laser radiation with
matter. In: Tengroth, B. & Epstein, D., ed. Current concepts
in ergophthalmology, Stockholm, Karolinska Institute.
BIRNGRUBER, R. (1978) [Experimental and theoretical
investigations into thermal injury to the retina from laser
radiation.] PhD Dissertation, Frankfurt, J.W. Goethe
University (in German).
BOLDRY, E.E., LITTLE, H., FLOCKS, M., & VASSILIADIS, A. (1981)
Retinal injury due to industrial laser burns. Ophthalmol., 88:
101-107.
BORLAND, R.G., BRENNAN, D.H., & NICHOLSON, A.N. (1971)
Threshold levels for damage of the cornea following
irradiation by a continuous wave carbon dioxide (10.6 micron)
laser. Nature (Lond.), 234: l5l-l52.
BORLAND, R.G., BRENNAN, D.H., MARSHALL, I.J., & VIVASH, J.P.
(1978) The role of fluorescein angiography in the detection of
laser induced damage to the retina .. a threshold study for
Q-switched neodymium and ruby laser. Exp. Eye Res., 27:
471-493.
BROWN, J.L. (1973) Experimental investigations of flash
blindness. Hum. Factors, 6: 503-516.
CAMPBELL, C.J., RITTLER, M.C., BREDEMEIER, H., & WALLACE, R.A.
(1968) Ocular effects produced by experimental lasers. I.
Carbon dioxide laser. Am. J. Ophthalmol., 66: 604-614.
CIE (1970) International lighting vocabulary, Paris, Bureau
Central de la Commission Internationale de l'Eclairage, Vol.
3, p. 5l.
CLEVET, A. & MAYER, A. (1980) Risques liés à l'utilisation
industrielle des lasers. Cahiers de notes documentaires INRS,
No 99, 2è trimestre, pp. 207-222.
COBLENTZ, W.W., STAIR, R., & HOGUE, J.M. (1931) The spectral
erythemic reaction of the human skin to ultraviolet radiation.
Proc. Natl Acad. Sci., 17(6): 401-405.
COGAN, D.G. & KINSEY, V.E. (1946) Action spectrum of keratitis
produced by ultraviolet radiation. Arch. Ophthalmol., 77:
670-677.
CONSIDINE, P.S. (1966) Effects of coherence on imaging
systems. J. Opt. Soc. Am., 56: 1001-1009.
CORNSWEET, T.N., ed. (1966) Visual perception, New York,
Academic Press.
COURT, L., CHEVALEREAUD, J.P., & SANTUCCI, G. (1978) Exposé
général. In: Sociéte française de Radioprotection, 9è Congrès
international: Effets biologiques des Rayonnements non
ionisants. Utilisation et Risques associés. Monte-Carlo,
Monaco, pp. 367-445.
CROOKES, W. (1914) The preparation of eye-preserving glass for
spectacles. Phil. Trans. Roy. Phil. Soc., A204: 1-25.
DAHLING, R.F., SHAPIRO, S.I., BERRY, C.Z., & SCHREIBER, M.M.
(1970) A method of evaluating sun screen protection from
long-wave ultraviolet. J. Invest. Derm., 55: 164-169.
DAUTRAY, R. & WATTEAU, J.P. (1980) La fusion inertielle par
laser. Rev. gén. nucl., No. 6, pp. 562-575.
DAVIES, J.M. (1959) The effects of intense thermal radiation
on animal skin. A comparison of calculated and observed burns,
Natick, MA, Army Quartermaster Research and Engineering
Command (Report T-24, 29 April 1959, NTIS AD 456794).
DAVSON, H., ed. (1962) The eye (4 volumes), New York, Academic
Press.
DECKER, D. (1977) An accident victim's view. Laser Focus,
13(8): 6.
DECOMPS, B. (1981) Le laser, instrument de recherche et
facteur de développement. Rev. gén. d'Elect., 90(1): 11-29.
DE GRUIJL, F.R. & VAN DER LEUN, J.C. (1980) A dose-response
for skin cancer induction by chronic UV exposure of a human
population. J. Theor Biol., 83; 487-504.
DUKE-ELDER, S. (1972) Textbook of ophthalmology, Vol. VI,
Injuries, St. Louis, Mosby, C.V.
EMMETT, E.A. & HORSTMAN, S.W. (1976) Factors influencing the
output of ultraviolet radiation during welding. J. occup.
Med., 18(1): 41-44.
ENVALL, K.R. & MURRAY, R. (1979) Evaluation of commercially
available laser protective eyewear, Rockville, MD, US Dept of
Health Education and Welfare, Food and Drug administration,
Bureau of Radiological Health. (DHEW Publ. No. (FDA) 79-8086).
ERNEST, J.T. & POTTS, A.M. (1971) Pathophysiology of the
distal portion of the optic nerve. IV. Local temperature as a
measure of blood flow. Am. J. Ophthalmol., 72(2): 435-444.
FITZPATRICK, T.B., PATHAK, M.A., HARBER, L.C., SEIJI, M., &
KUKITA, A. (1974) Sunlight and man, normal and abnormal
photobiologic responses, Tokyo, University of Tokyo Press.
FRANCE, Arrêté du 30 janvier (1974) Réglementation concernant
les lasers à usage médical. J.O. 17 mars 1974, p. 3093.
FRANCE, Arrêté du 13 mai (1974) Conditions techniques
générales des lasers à usage médical. J.O. 15 juin 1974,
p. 6388.
FRANCE, Arrêté du 14 mai (1974) Conditions techniques des
lasers à usage médical de catégorie II, groupe I, sous-groupe
I. J.O. 15 juin 1974, p. 6388.
FRANCE, Arrêté du 29 décembre (1976) Classification des lasers
à usage médical de catégorie II, groupe II (émission
continue). J.O. 22 janvier 1977, (Numéro complémentaire)
p. 466.
FRANCE, Arrêté du 10 janvier (1978) Conditions techniques
d'utilisation des lasers à usage médical de catégorie II,
groupe II. J.O. 28 janvier 1978 (Numéro complémentaire) p. 822.
FRIED, D.L. (1981) Laser eye safety: The implications of
ordinary speckle and speckled-speckle statistics. J. Opt. Soc.
Am., 71(7): 914-916.
FRISCH, G.D., BEATRICE, E.S., & HOLSEN, R.C. (1971)
Comparative study of argon and ruby retinal damage thresholds.
Invest. Ophthalmol., 10: 911-919.
GABEL, V.P. & BIRNGRUBER, R. (1981) A comparative study of
threshold laser lesions in the retinae of human volunteers and
rabbits. Health Phys., 40: 238-240.
GABEL, V.P., BIRNGRUBER, R., & HILLENKAMP, F. (1976) [Light
absorption in the fundus oculi.] Munich, Association for
Research on Radiation and the Environment (GSF report A55) (in
German).
GEERAETS, W.J. & BERRY, E.R. (1968) Ocular spectral
characteristics as related to hazards from lasers and other
light sources. Am. J. Ophthalmol., 66: 15-20.
GIESE, A.C. (1976) Living with our sun's ultraviolet rays,
New York, Plenum Publishing Corporation.
GOLDMAN, L., ed. (1981) The biomedical laser technology and
clinical applications, New York, Heidelberg, Berlin, Springer
Verlag.
GOLDMAN, L., ROCKWELL, R.J., & RICHFIELD, D. (1971) Long-term
laser exposure of a senile freckle. Arch. environ. Health, 22:
401-403.
GOLDMAN, L., ROCKWELL, R.J., MICHAELSON, S.M., SLINEY, D.H.,
TENGROTH, B.M., & WOLBARSHT, M.L. (1982) Optical radiation,
with particular reference to lasers. In: Suess, M. ed.
Nonionizing radiation, Copenhagen, World Health Organization,
Regional Office for Europe.
GOLDMANN, H. (1933) Genesis of heat cataract. Arch.
Ophthalmol., 9: 314.
GORODETSKI, A.A., KIRICINSKI, B.R., EVDOKOMOB, I.R., &
KOLESNIK, V.M. (1968) [Some data on the biological action and
radiation protection of optical quantum generators.] Gig. Tr.
Prof. Zabol., 12: 37-41 (in Russian).
GREISEMANN, J.C. & MARTI, J. (1978) Risques liés à
l'utilisation des lasers de puissances. In: Société française
de Radioprotection, 9è Congrès international. Effets
biologiques des Rayonnements non ionisants. Utilisation et
Risques associés, pp. 473-482.
GREISS, G.A., BLANKENSTEIN, F., & WILLIFORD, G.G. (1980)
Ocular damage thresholds from multiple-pulse laser exposures,
Health Phys., 39: 921-927.
GRUM, F.C. & BECHERER, R., ed. (1979) Optical radiation
measurements, Vol. 1, Radiometry, New York, Academic Press,
p. 352.
GULLBERG, K., HARTMAN, B., KOCK, E., & TENGROTH, B. (1967)
Carbon dioxide laser hazards to the eye. Nature (Lond.), 215:
857-858.
HAM, W.T. Jr, WILLIAMS, R.C., MUELLER, H.A., GUERRY, D.,
CLARKE, A.M., & GEERAETS, W.J. (1966) Effects of laser
radiation on the mammalian eye. Trans. NY Acad. Sci., 28:
517-526.
HAM, W.T. Jr, CLARKE, A.M., GEERAETS, W.J., CLEARY, S.F.,
MUELLER, H.A., & WILLIAMS, R.C. (1970) The eye problem in
laser safety. Arch. environ. Health, 20: 156-160.
HAM, W.T. Jr, MUELLER, H.A., & SLINEY, D.H. (1976) Retinal
sensitivity to damage from short wavelength light. Nature
(Lond.), 260(5547): 153-155.
HAM, W.T. Jr, MUELLER, H.A., RUFFOLO, J.J., & CLARKE, A.M.
(1978) Sensitivity of the retina to radiation damage as a
function of wavelength. Photochem. Photobiol., 29: 735-743.
HAMERSKI, W. (1969) Investigations on histochemical changes in
experimental corneal lesions induced with UV radiation and on
the prevention of photophthalmia. Pol. med. J., 8: 1469-1476.
HANSEN, W.P. & FINE, S. (1968) Melanin granule models for
pulsed laser induced retinal injury. Appl. Opt., 7: 155-159.
HARDY, J.D. (1968) Pain following step increase in skin
temperature. In: Kenshalo, D.R. ed. The skin senses,
Springfield, IL, Charles C. Thomas, pp. 444-456.
HARDY, J.D., HAMMEL, H.T., & MURGATROYD, D. (1956) Spectral
transmittance and reflectance of excised human skin. J. appl.
Physiol., 9: 257.
HARLEN, F. (1978) The development of laser codes of practice
and maximum permissible exposure levels. Ann. occup. Hyg.,
2l(2): 199-211.
HARTMANN, B. & KLEMAN, B. (1980) Exposure limits for
broad-band 400-1400 nm radiation. Ocular effects of
non-ionizing radiation. Proc. SPIE, 29: 105-114.
HARWERTH, R.S. & SPERLING, H.G. (1975) Effects of intense
visible radiation on the increment threshold spectral
sensitivity of the Rhesus monkey eye. Vision Res., 15:
1193-1204.
HATFIELD, E.M. (1970) Eye injuries and the solar eclipse.
Sight Sav. Rev., pp. 79-85.
HATHAWAY, J.A., STERN, N., SOLES, E.M., & LEIGHTON, E. (1977)
Ocular medical surveillance on microwave and laser workers. J.
occup. Med., l9(10): 683-688.
HAUSSER, K.W. (1929) [Influence of wavelength in radiation
biology.] Strahlenther., 28: 25-44 (in German).
HOLZINGER, G., KROY, W., SCHREIBER, P., & SUTTER, E. (1978)
Protection from law radiation (Series on Workplace Protection,
no.14).
INTERNATIONAL ORGANIZATION FOR STANDARDIZATION (1980) Personal
eye-protectors for welding and related techniques. Welding
filters, Geneva (ISO 4850).
IRPA (1977) Overviews on nonionizing radiation, International
Radiation Protection Association Report of a Study Group.
JAMES, R.H., ed. (1976) National Conference on Measurements
of Laser Emissions for Regulatory Purposes, April, Rockville,
MD, US Dept of Health, Education and Welfare, Food and Drug
Administration, Bureau of Radiological Health (HEW Publ. (FDA)
76-8037).
KASUBA V.A. & AKIFEV, S.A. (1977) [Working conditions and
morbidity among workers preparing clock jewels using lasers
and mechanical techniques.] Gig. Tr. Prof. Zabol., 1: 37-40
(in Russian).
KAUFMANN, E. (1970) Laser hazard to the human eye. Schweiz
Arch., 36: 211.
KLINE, M.V. (1970) Optics, New York, John Wiley and Sons.
KLOST, W. (1971) [Safety measures in the use of laser rays.]
Zentralbl. Arbeitsmed., 21: 105-111 (in German).
KOGELNIK, H. & LI, T. (1966) Laser beams and resonators. In:
Levine, A.K., ed. Lasers. New York, Decker.
KOMAROVA, A.A., MOTZERENKOV, V.P., SKATSKAIA, G.K., CEMNY,
A.B., & PIVOVAROV, N.N. (1978) [Action of reflected laser
radiation on the eye.] Vestn. Oftal., l: 46-50 (in Russian).
KUWABARA, T. (1970) Retinal recovery from exposure to light.
Am. J. Ophthalmol., 70(2): 187-189.
LA VAIL, M.M. (1980) Eye pigmentation and constant light
damage in the rat retina. In: Williams, T.P. & Baker, B.N.,
ed. The effects of constant light on visual processes, New
York, London, Plenum Press, pp. 357-387.
LAWWILL, T., CROCKET, S., & CURRIER, G. (1977) Retinal damage
secondary to chronic light exposure thresholds and mechanisms.
Doc. Ophthalmol., 44(2): 379-402.
LE BODO, H. (1976) La calorimétrie appliquée à la mesure des
puissances et énergies lasers. Bulletin d'information du
Bureau National de Métrologie, No. 24, pp. 12-18.
LEIBOWITZ, H.M. & PEACOCK, G.R. (1969) Corneal injury produced
by carbon dioxide laser radiation. Arch. Ophthalmol., 8l:
712-721.
LERMAN, S. (1980a) Radiant energy and the eye, New York,
Macmillan Publ. Co.
LERMAN, S. (1980b) Human ultraviolet radiation cataracts.
Ophthal. Res., 12: 303-314.
LIVINGSTON, P.C. (1932) The study of sun glare in Iraq. Br. J.
Ophthalmol., 6: 577-625.
LOWE, D.A. (1975) A guide to international recommendations on
names and symbols for quantities and on limits of measurement.
Geneva, World Health Organization (Progress in Standardization: 2).
MAGNUS, I.A. (1976) Dermatological photobiology, London,
Blackwell Scientific Publications.
MAINSTER, M.A., WHITE, T.J., TIPS, J.H., & WILSON, P.W. (1970)
Retinal-temperature increases produced by intense light
sources. J. Opt. Soc. Am., 60: 264-270.
MARSHALL, J. (1970) Thermal and mechanical mechanisms in laser
damage to the retina. Invest. Ophthalmol., 9: 97-115.
MARSHALL, J. (1973) Laser damage to ocular tissues. Proc. R.
Soc. Med., 66(9): 842-844.
MARSHALL, J. (1978) Retinal injury from chronic exposure to
light and the delayed effects from retinal exposure to intense
light sources. In: Tengroth, B. & Epstein, D., ed. Current
concepts in ergophthalmology, Stockholm, Karolinska Institute,
pp. 81-104.
MARSHALL, J. & BIRD, A.C. (1979) A comparative histo-
pathological study of argon and krypton laser irradiations of
the human retina. Br. J. Ophthalmol., 63(10): 657-668.
MARSHALL, W.J. (1980) Optical measurement techniques. In:
Kelley, W.D., ed. Non-ionizing radiation, Cincinatti, OH,
ACGIH, pp. 175-179.
MAYER, M.A. & SALSI, M.S. (1979) Rayonnement ultraviolet,
visible et infrarouge, mésure-evaluation des risques. INRS
Cahiers de Notes documentaires, No. 96, 3e trimestre, 403-413.
MEDOVSKAYA, T.P. (1970) Data on the condition of the eye in
workers at a glass factory. Hyg. Sanit., 35: 446-447.
MESTER, E. (1980) L'effet stimulant des faisceaux laser sur la
cicatrisation des plaies. Rev. Iéna, No. 3, pp. 121-122.
MIRO, L. (1979) Le laser et ses applications médio-
chirurgicales. Semaine des hôpitaux de Paris, 55(41-42):
1956-1964.
MOON, M.E., CLARKE, A.M., RUFFALO, J.J. Jr, & MUELLER, H.A.
(1978) Visual performance in the Rhesus monkey after exposure
to blue light. Vision Res., 18: 1573-1577.
MOSS, C.E. (1980) Radiation hazards associated with
ultraviolet radiation curing processes. In: Kelley, W.D., ed.
Non-ionizing radiation, Cincinnati, OH, ACGIH, pp. 203-209.
NOELL, W.K. & ALBRECHT, R. (1971) Irreversible effects of
visible light on the retina, role of vitamin A. Science, 172:
76-79.
PARR, W.H. (1969) Skin lesion threshold values for laser
radiation as compared with safety standards, Fort Knox, KY, US
Army Medical Research Laboratory (Report 8l3, AD 688871).
PARRISH, J.A., ANDERSON, R.R., URBACH, F., & PITTS, D. (1978)
UVA biological effects of ultraviolet radiation with emphasis
on human responses to longwave ultraviolet, New York, Plenum
Publishing Corporation.
PARVER, L.M., ANKER, C., & CARPENTER, D.O. (1980) Choroidal
blood flow as a heat dissipating mechanism in the macula. Am.
J. Ophthalmol., 89: 641-646.
PECKHAM, R.H. & HARLEY, R.D. (1951) The effect of sunglasses
in protecting retinal sensitivity. Am. J. Ophthalmol., 34(11):
1499-1507.
PENNER, R. & McNAIR, J.N. (1966) Eclipse blindness. Am. J.
Ophthalmol., 61: 1452-1457.
PITTS, D.G. (1974) The human ultraviolet action spectrum. Am.
J. opt. S. physiol. Opt., 51: 946-960.
PITTS, D.G., CULLEN, A.P., & HACKER, P.D. (1977) Ocular
effects of ultraviolet radiation from 295 to 365 nm. Invest.
ophthalmol. Vis. Sci., 16(10): 932-939.
PRATESI, R. & SACCHI, C.A., ed. (1980) Lasers in photomedicine
and photobiology, Berlin, Springer-Verlag.
ROCKEROLLES, R. (1978) Dangers spécifiques du rayonnement
cohérent. Dangers habituels liés aux fortes luninances; effets
multiphotoniques et effets non linéaires. In: Société
française de Radioprotection. 9è Congrès international: Effets
biologiques des Rayonnements non ionisants. Utilisation et
Risques associés, Monte-Carlo, Monaco, pp. 453-472.
ROCKWELL, R.J. Jr, & GOLDMAN, L. (1974) Research on human skin
laser damage threshold, final report, Texas, USAF School of
Aerospace Med., Brooks AF Base (Prepared by Dept of
Dermatology and Laser Lab. Med. Centre, University of
Cincinnati, Contract F4l609-72-C-0007).
ROGER, F.C. (1973) Clinical findings, course and progress of
biatis corneal degeneration in the Dahlak Islands. Br. J.
Ophthalmol., 57: 657-661.
RUBIN, L.R. (1977) Lasers in biology, Moscow, Nauka.
SCHERR, A.D., TUCKER, R.J., & GREENWOOD, R.A. (1969) New
plastics absorb at laser wavelength. Las. Foc., 5(9): 46-48.
SCHREIBEIS, W.J. (1968) Laser eye protection goggles based on
maufacturer's information. Am. Ind. Hyg. Assoc. J., 29: 504.
SKEEN, C.H., BRUCE, W.R., TIPS, J.H. Jr, SMITH, M.G., & GARZA,
G.G. (1972) Ocular effects of repetitive laser pulses,
San Antonio, TX, Technology Inc. (Contract F41609-71-C-0018, AD
746795).
SLINEY, D.H. (1971) The development of laser safety
criteria-biological considerations. In: Wolbarsht, M.L., ed.
Laser applications in medicine and biology, New York, Plenum
Press, pp. 163-238.
SLINEY, D.H. (1972) The merits of an envelope action spectrum
for ultraviolet radiation exposure criteria. Am. Ind. Hyg.
Assoc. J., 33: 644-653.
SLINEY, D.H. (1974) Laser protective eyewear. In: Wolbarsht,
M.L., ed. Laser application in medicine and biology, New York,
Plenum Press, Vol. 2.
SLINEY, D.H. & FREASIER, B.C. (1973) The evaluation of optical
radiation hazards. Appl. Opt., 12(1): 1-24.
SLINEY, D.H. & WOLBARSHT, M.L. (1980) Safety with lasers and
other optical sources, New York, Plenum Publishing Corporation.
SLINEY, D.H., MOSS, C.E., MILLER, C.G., & STEPHENS; J.B.
(1981) Semitransparent curtains for control of optical
radiation hazards. Appl. Optics, 20(14): 2352-2366.
SMITH, H.E. (1944) Actinic macular retinal pigment
degeneration. US Nav. med. Bull., 42: 675-680.
SMITH, K.C. (1977) The science of photobiology, New York,
Plenum Press.
SMITH, K.C. (1978) Symposium on DNA repair and its role in
mutagenesis and carcinogenesis. Photochem. Photobiol., 28: 119.
STAIR, R. (1948) Spectral-transmissive properties and use of
eye-protective glasses. Washington, DC, National Bureau of
Standards (NBS Circular 471).
STOLL, A.M. & CHIANTRA, M.A. (1971) Heat transfer through
fabrics as related to thermal injury. Trans. N.Y. Acad. Sci.,
33: 649-670.
STOLWIJK, J.A.J. (1980) Infrared radiation and radiant heat
stress. In: Kelley, W.D., ed. Non-ionizing radiation,
Cincinnati, OH, ACGIH, pp. 171-174.
STRAUB, H.W. (1970) Laser eye protection in the USA.
Berufsgenossenschaft Z. Unfallv. Betrieb, 3: 83-87.
STUCK, B.E., LUND, D.J., & BEATRICE, E.A. (1981) Ocular
effects of holmium (2.06 µm) and erbium (1.54 µm) laser
radiation. Health Phys., 40: 835-846.
SUESS, ed. (1982) Nonionizing radiation protection,
Copenhagen, World Health Organization, Regional Office for
Europe.
SUTTER, E., HUEBNER, H.J., KRAUSE, E., & RUGE, J. (1972)
[Radiation measurements in various arc welding processes.]
Federal Republic of Germany, Federal Institute of Physics and
Technology (Report No. Optik 2/72) (in German).
SWOPE, C.H. (1969) The eye protection. Arch. environ. Health,
18: 428-433.
SWOPE, C.H. (1970) Design considerations for laser eye
protection. Arch. environ. Health, 20: 184-187.
SWOPE, C.H. & KOESTER, C.J. (1965) Eye protection against
lasers. Appl. Opt., 4(5): 523-525.
SYKES, S.M., ROBISON, W.G., WAXLER, M., & KUWABARA, T. (1981)
Damage to the monkey retina by broad-spectrum fluorescent
light. Invest. Ophthalmol. Vis. Sci., 20(4): 425-434.
TENGROTH, B.M. (1976) Safety glasses in welding. Env. Res.,
11:283-284.
TENGROTH, B.M., LYDAHL, E., & PHILIPSON, B.T. (1980) Infrared
cataract in furnacemen. In: Kelley, W.D., ed. Non-ionizing
radiation, Cincinnati, OH, ACGIH, pp. 169-170.
URBACH, R., ed. (1969) The biologic effects of ultraviolet
radiation, New York, Pergamon Press.
URBACH, R. (1980) Occupational skin hazards from ultraviolet
exposure. In: Kelley, W.D., ed. Non-ionizing radiation,
Cincinnati, OH, ACGIH, pp. 145-156.
US DHEW (1978) Performance standards for light emitting
products, (title 21, Code of Federal Regulations, part 1040),
Washington, DC, US Department of Health, Education and Welfare.
VAN DER LEUN, J.C. (1965) Theory of ultraviolet erythema.
Photochem. Photobiol., 4: 453-458.
VASSILIADIS, A. (1971) Ocular damage from laser radiation. In:
Wolbarsht, M.L., ed. Laser applications in medicine and
biology, New York, Plenum Press, pp. 125-162.
VASSILIADIS, A., ZWENG, H.C., & DEDRICK, K.G. (1971) Ocular
laser threshold investigations, Menlo Park, CA, Stanford
Research Institute (SRI Report No. 8209).
VOGT, A. (1919) [Experimental inducement of cataract by
isolated short-wave infrared mixed with red.] Klin. Mbl.
Augenheilkd., 63: 230-231 (in German).
VOS, J.J. (1966a) Heat-damage to the retina by lasers and
photocoagulators. Ophthalmologia (Basel), 151: 652-654.
VOS, J.J. (1966b) Some considerations on eye hazards with
lasers, Soesterberg, Institute for Perception RVO-TNO,
National Council for Applied Research in the Netherlands, 23
pp. (Report IZF 1966-4. AD 800156).
WEALE, R.A. (1982) The age variation of "senile" cataract in
various parts of the world. Br. J. Ophthalmol., 66: 31.34.
WHO SCIENTIFIC GROUP ON HEALTH FACTORS INVOLVED IN WORKING
UNDER CONDITIONS OF HEAT STRESS (1969) Report, Geneva, World
Health Organization (WHO Technical Report Series No. 412).
WHO (1979) Environmental Health Criteria 14: Ultraviolet
radiation, Geneva, World Health Organization.
WHO (l982) The SI for the health profession (reimpression)
Geneva, Switzerland, World Health Organization.
WILLIAMS, T.B. & BAKER, B.N., ed. (1980) The effects of
constant light on the visual process, New York, Plenum Press.
WOLBARSHT, M.L. (1971, 1974, 1978a) Lasers in medicine and
biology, New York, Plenum Press, Vols I, II, III.
WOLBARSHT, M.L. (1978b) The effects of optical radiation on
the anterior structures of the eye. In: Epstein, D. &
Tengroth, B., ed. Current concepts in ergophthalmology,
Stockholm, Department of Ophthalmology, Karolinska Institute,
pp. 29-46.
WOLBARSHT, M.L. & SLINEY, D.H. (1974) The formulation of
protection standards for lasers. In: Wolbarsht, M.L., ed.
Lasers in medicine and biology, New York, Plenum Press,
Vol. II, pp. 309-360.
WOLBARSHT, M.L., YAMANASHI, B.S., & ORR, M.A. (1977) The
origin of cataracts in the lens from infrared radiation,
Durham, NC, Duke University Eye Centre (Report 7-20-1977:
62772A 3E62772A813.00.013, Contract DAMD 17-74-C-4133, US Army
Med. Res. and Dev. Cmd).
WOLBARSHT, M.L., O'FEGHLUDHA, F.A., SLINEY, D.H., GUY, A.W.,
SMITH, A.A. Jr, & JOHNSON, G.A. (1980) Electromagnetic
emission from visual display units: a non-hazard. In: Kelley,
W.D., ed. Non-ionizing radiation, Cincinnati, OH, ACGIH,
pp. 193-201.
WREN, J.E., SCOTT, W.D., & BATES, C.E. (1977) Thermal and
mechanical properties of aluminized fabrics for use in ferrous
metal handling operations. Am. Ind. Hyg. Assoc. J., 38(11):
603-612.
YOUNG, R.W. (1980) A theory of central retinal disease. In:
Sears, M.L., ed. New directions in ophthalmic research,
New Haven, London, Yale University Press, pp. 237-270.
ZIGLER, J.S. & GOOSEY, J.D. (1981) Photosensitized oxidation
in the lens: evidence from photosensitizers endogenous to the
human lens. Photochem. Photobiol., 33: 689-874.
ZHOKOV, V.P., KOMAROVA, A.A., MAXIMOVA, L.I., MURATOV, V.P.,
PALTZEV, Yu.P., & SEMINOV, A.I. (1981) Occupational hygiene
and prevention of occupational diseases from lasers, Moscow,
Meditsina.
ZUCHLICH, J.A. & KURTIN, W.E. (1977) Oxygen dependence of
near-ultraviolet induced corneal damage. Photochem.
Photobiol., 25: 133-135.
ZUCHLICH, I.A. & TABOADA, J. (1978) Ocular hazard from UV
laser exhibiting self-mode-locking. Appl. Opt., 17: 1482-1484.
ZWICK, H. & BEATRICE, E.S. (1978) Long-term changes in
spectral sensitivity after low-level laser (5l4 nm) exposure.
Mod. Probl. Ophthalmol., 19: 319-325.
GLOSSARY
ACOUSTICO-OPTIC: involving the interaction of light and an acoustic
wave. Acoustico-optic devices such as Q switches and modulators
are used in manipulating laser beams.
ACTIVE MEDIUM: the atomic or molecular species which can provide
gain for laser oscillation. Also called laser medium, lasing
medium or active material.
ANGSTROM (A): a non-SI unit equal to 10-10 metre. Its use as a
unit of optical wavelength has largely been supplanted in recent
years by the nanometre (10-9 metre).
ARC LAMP: an electric lamp in which current passes through the
ionized air between two electrodes, giving off light. Applications
include laser excitation.
ATOMIC LASER: a gas laser in which the active material is an atomic
species rather than a molecule.
ATTENUATION: reduction in intensity that results when optical
radiation travels through an absorbing or scattering medium. In
optical fibre, attenuation (in decibels) equals 10 log ( Po/ Pin),
where Po is the power at the output end of the fibre and Pin is
the power launched into the fibre.
AVERAGE POWER: in a repetitively pulsed laser, the energy per pulse
times the repetition rate. When the energy per pulse is expressed
in joules and the repetition rate in hertz, the average power is
expressed in watts.
BEAM DIAMETER: the distance between the two opposing points at
which the irradiance or radiant exposure is a specified fraction
(typically 1/e or 1/e2) of the irradiance or radiant exposure of
the emitted radiation.
BEAM DIVERGENCE: the increase in beam diameter with distance from
the laser's exit aperture. Measured in milliradians at specified
points, usually where irradiance or radiant exposure is 1/e or 1/e2
the maximum value, and expressed as the "full-angle" divergence.
BOLOMETER: a type of detector which measures infrared radiation by
the temperature-induced change of resistance in a metal foil
exposed to the radiation and heated by it.
BREWSTER ANGLE: the angle between an incident beam of light and a
dielectric reflecting surface at which none of the light polarized
in the plane of incidence is reflected. Brewster's angle is
tan-1 n2/ n1, where n1, and n2 are the indexes of refraction of the
first and second media respectively. A window mounted at
Brewster's angle with respect to an incident beam is often used as
a window in laser cavities.
CALORIMETER: a type of detector that measures heat produced by
absorption of radiation.
CHEMICAL LASER: a type of laser in which the population inversion
is produced directly by an "elementary" chemical reaction (a
collision process in which one or more molecules undergo changes in
their chemical bonds).
COHERENCE: a fixed phase relationship among various points of an
electromagnetic wave in space (spatial coherence) or in time
(temporal coherence).
COLLIMATOR: an optical device for converting a diverging or
converging beam of light into a collimated or parallel beam, or for
expanding or reducing the cross-sectional area of an incident
collimated beam. A target collimator projects a parallel beam from
its own light source such that, viewed from any distance, the light
source appears to be at infinity.
CONTINUOUS WAVE (cw) LASER OPERATION: laser operation in which
radiation is emitted continuously.
CORE: the central region of an optical fibre. The core must have a
higher refractive index than the cladding for light to be
transmitted through the fibre via total internal reflection
CORNER CUBE: an optical component with three mutually perpendicular
faces and a hypotenuse face. Because light entering through the
hypotenuse is totally internally reflected at each perpendicular
face, the cube acts as a retroreflector. Also known as corner
reflector.
CRYSTAL LASER: a type of laser in which the active medium is an
atomic species in a crystal such as ruby, YAG (yttrium aluminium
garnet), or YALO (yttrium aluminate).
DETECTOR: see PHOTODETECTOR.
DIFFRACTION: deviation of light rays from the paths predicted by
geometical optics.
DIODE LASER: see SEMICONDUCTOR LASER.
DISPERSION: variation of the refractive index of an optical
material with change in wavelength, as in a prism; in an optical
fibre, the temporal spreading of a light pulse due to the fibre's
different propagation speeds for different wavelengths and modes of
light. Such spreading limits the fibre's information-carrying
capacity of bandwidth.
DIVERGENCE: see BEAM DIVERGENCE.
DYE LASER: a type of laser in which the active medium is an organic
dye, generally in solution with the liquid either flowing or
encapsulated within a cell. Experimental solid and gas dye lasers
also have been built. Also called organic-dye, tunable-dye or
liquid laser.
ELECTRON-BEAM-SUSTAINED LASER: a molecular-gas laser in which the
electrical discharge is sustained with a beam of high-energy
electrons. Usually injected transversely to the laser cavity's
optical axis, the electron beam permits laser operation at
pressures and cross-section-to-length ratios higher than possible
with an unsustained discharge. This technique is often used in
commercial carbon-dioxide lasers with very high continuous-wave
output power.
ELECTRO-OPTIC: applying to modulators, Q switches and other beam-
manipulating devices in which operation relies on modification of a
material's refractive indices by an applied electrical field. In a
Kerr cell the index change is proportional to the square of the
electrical field, and the material is usually a liquid. In a
Pockels cell the material is a crystal whose index change is linear
with the electric field.
EMISSIVITY: ratio of radiant exitance of a thermal radiator to that
of a full radiator (black body) at the same temperature - (ISO
31/VI 1980).
EXCIMER LASER: a laser in which the active medium is an excimer, a
molecule which is chemically unstable except in its excited state.
The term often is applied to lasers in which the active medium is a
rare-gas halide (or monohalide) excimer such as KrF* or XeF*.
GAS LASER: a type of laser in which the active medium is a gas.
The category is subclassified according to the active medium into
atomic (such as helium-neon), molecular (carbon dioxide, hydrogen
cyanide and water vapour), ionic (argon, krypton, xenon, and the
metal-vapour types such as helium-cadmium and helium-selenium), and
excimer (typically rare-gas halides). Loosely applied, "ion" means
argon and krypton.
GLASS LASER: a type of solid-state laser in which the active medium
is a glass rod doped with rare-earth atoms, usually neodymium.
HERTZ (Hz): the SI unit of frequency of periodic phenomena. It
replaces the non-SI unit "cycles per second". The number of pulses
per second that a laser can produce may be expressed in hertz.
HOLOGRAM: a recording of the interference of coherent light
reflected from an object with light direct from the same source or
reflected from a mirror. Illumination of the hologram reproduces
the object's three-dimensional image.
IMAGE CONVERTER: an electron tube which produces a visual replica
of an image formed on its cathode by some form of electromagnetic
radiation. In an image converter camera, the image formed by the
electron tube is focused on to photographic film for a permanent
record.
INFRARED: electromagnetic radiation with wavelength between 0.76
micrometre and about 1 millimetre. Wavelengths at the shorter end
of this range are frequently called "near" infrared, and those
longer than about 20 micrometres, "far" infrared.
INTEGRATED OPTICS: devices in which several optical components are
"integrated" on to a single substrate; analogous to integrated
electronic circuits. Although still in the research phase,
integrated optics has potential for use in optical signal
processing and in fibre-optic communications.
INTERFERENCE FILTER: an optical component which depends on
interference in a series of thin films deposited on a substrate to
limit transmission to a desired spectral band.
ION LASER: a type in which the active element is an ionized gas,
generally argon or krypton.
IRRADIANCE ( E): radiant flux per unit area, expressed in watts per
square centimetre.
LASER: acronym for "light amplication by stimulated emission of
radiation." A device which generates or amplifies electromagnetic
oscillations at wavelengths between the far infrared
(submillimetre) and ultraviolet. Like any electromagnetic
oscillator, a laser oscillator consists of two basic elements: an
amplifying (active) medium and a regeneration or feedback device
(resonant cavity). A laser's amplifying medium can be a gas,
semiconductor, dye solution, etc; feedback is typically from two
mirrors. Distinctive properties of the electromagnetic
oscillations produced include monochromaticity, high intensity,
small beam divergence, and phase coherence. As a description of a
device, "laser" refers to the active medium plus all equipment
necessary to produce the effect called lasing.
LASER DIODE: see SEMICONDUCTOR LASER.
LED: abbreviation of light-emitting diode. A semiconductor
emitting incoherent light into a broad field of view, used in low-
speed or short-haul fibre-optic links. Most LEDs used in fibre-
optic applications emit in the near infrared.
LIDAR: acronym for "light detection and ranging," a system
employing a laser beam to gather ranging information as well as
intelligence on reflection and scattering of light by clouds and
atmospheric pollutants.
LIQUID LASER: a type in which the active element is either an
organic dye or an inorganic liquid. See also DYE LASER.
MULTIMODE: emission at several frequencies simultaneously,
generally closely spaced, each frequency representing a different
mode of laser oscillation inthe resonant cavity.
Nd-GLASS: neodymium-doped glass, used in some solid state lasers.
The neodymium atoms are the active medium.
Nd-YAG: neodymium-doped yttrium-aluminium-garnet (YAG), a crystal
which is used in some solid state lasers. The neodymium atoms are
the active medium.
NEUTRAL DENSITY FILTER: a filter which reduces the intensity of
light without affecting its spectral character.
NONLINEAR EFFECTS: changes in a medium transmitting electromagnetic
waves that are proportional to the second, third or higher powers
of external electric field. Nonlinear optical effects include
harmonic generation and the electro-optic effect. See electro-
optic.
OPTICALLY PUMPED LASER: a laser whose active medium is excited by
another light source to produce a population inversion. For solid-
state and some dye lasers this source usually is an incoherent type
such as a flash- or arc-lamp. For gas and other dye lasers,
coherent laser sources generally provide such optical pumping.
PARAMETRIC OSCILLATOR: a nonlinear device, usually a crystal, which
produces tunable laser oscillations at the sum or difference
frequency of mixed laser beams. Also called tunable parametric
oscillator or optical parametric oscillator. Loosely applied to
the complete instrument containing the pump laser and the tuning
crystal.
PHOTODETECTOR: any device which detects light, generally producing
an electronic signal with intensity proportional to that of the
incident light.
PHOTON: a massless "particle" of electromagnetic radiation, with
energy equal to hc/lambda where h is Planck's constant (6.6 x 10-34
joule second) and c/lambda is the frequency of the radiation (speed
of light divided by wavelength).
POLARIZER: an optical component which only transmits lightwaves
that oscillate in a given plane.
POPULATION INVERSION: a condition in which most atoms of a species
are in an excited, metastable state. Collision of a photon with
such an atom causes the atom to relax to a lower energy state, and
to emit a second photon, amplifying the light signal. Population
inversion is required for lasing to occur.
PULSELENGTH: the duration of the burst of energy emitted by a
pulsed or Q-switched laser. Expressed in seconds and usually
measured at the half-power (half the full height of a voltage or
current pulse). Also called pulsewidth.
PULSED LASER: a laser that emits light in pulses rather than
continuously.
PUMP: the energy source (such as flashlamp, electron beam or
current supply) that drives the amplification in the active medium
of a laser by creating a population inversion.
PYROELECTRIC CRYSTAL: a type of crystal that shows electrical
effects when its temperature is changed; these effects are used to
detect infrared radiation.
Q SWITCH: essentially a "shutter" which prevents laser emission
until opened. Q stands for "quality factor" of the laser's
resonant cavity. "Active" Q switching is achieved with a rotating
mirror or prism, Kerr or Pockels cell, or acoustico-optic device;
"passive" Q switching is achieved with a saturable absorber such as
a gas or dye. In a pulsed laser a Q switch increases pulse power
by shortening pulse duration while not significantly decreasing the
energy; in a continuous wave laser the device provides shorter and
more intense pulses at a higher repetition rate than could be
achieved by pulsing the laser directly.
RADIANCE ( L): At a point of a surface and in a given direction,
the radiant intensity of an element of the surface, divided by the
area of the orthogonal projection of this element on a plane
perpendicular to the given direction (ISO 31/6-1980). Expressed in
watts per steradian square centimetre.
RADIANT FLUX: the rate of flow of radiant energy, measured in
watts.
RADIOMETER: an instrument for measuring incident radiation in
radiometric units (watts). Radiometric measurements can be made at
any wavelength, but the spectral range of a particular instrument
may be limited to a narrow range.
RADIOMETRIC UNITS: units defined for measurement of the intensity
of electromagnetic radiation; the basic unit is the SI unit watt.
RAMAN EFFECT: the appearance of additional weak lines in the
spectrum of light that has been scattered by a transparent
substance. The extra lines result from rotational or vibrational
transitions of the molecules in the scattering medium. If the
medium is illuminated with laser light of sufficient intensity, the
emission at the Raman frequencies is amplified, exhibiting
characteristics of stimulated emission (i.e., stimulated Raman
effect.).
REFLECTANCE: the ratio of wave energy reflected from a surface to
the wave energy incident on a surface.
SEMICONDUCTOR LASER: a type in which the active material is a
semiconductor, either a diode or homogeneous. Commercial
types are generally diodes in which lasing occurs at the
junction of n-type and p-type semiconductors, usually gallium-
arsenide or gallium-aluminium-arsenide. Homogeneous types are
made of undoped semiconductor material and are pumped by an
electron beam.
SOLID-STATE LASER: a type the active medium of which is an atomic
species in a glass or crystal. The atomic species may be added to
the glass or crystal, as neodymium is added to glass, or may be
instrinic, as chromium is in ruby. This term is generally not
applied to semiconductor lasers.
SUPER-RADIANT: applying to coherent optical amplification of
spontaneous emission that occurs without relaxation processes.
Commonly used to describe a laser whose gain is high enough to
permit amplification without mirrors; examples are nitrogen and
molecular hydrogen. Beam quality of a super radiant laser is
generally inferior to that of a laser with a complete optical
cavity. "Super-fluorescent" has been proposed as a more precise
description of this type of laser.
TEA LASER: acronym for transversely excited, atmospheric pressure
laser. A gas laser in which excitation of the active medium is
transverse to the flow of the medium. Because of shorter breakdown
length, this type operates in a gas-pressure range higher than that
for longitudinally excited gas lasers (but not necessarily
atmospheric) and offers a potentially higher power output per unit
volumes because of a greater density of lasing molecules.
TUNABLE LASER: a laser or a parametric oscillator whose emission
can be varied across a broad spectral range.
ULTRAVIOLET: electromagnetic radiation with wavelengths between
about 40 and 400 nanometres. Radiation between 40 and 200 nm is
termed "vacuum ultraviolet" because it is absorbed by air and
travels only through a vacuum. The "near" ultraviolet has
wavelengths close to those of visible light; the "far" ultraviolet
has shorter wavelengths.
YAG: yttrium aluminium garnet, a crystal host which can be doped
with an active laser medium, usually neodymium.
YALO: yttrium aluminate (YA103), a crystal host doped with an
active laser medium, usually neodymium.
YLF: yttrium lithium fluoride, a crystal host which can be doped
with an active laser ion, usually holmium.
