
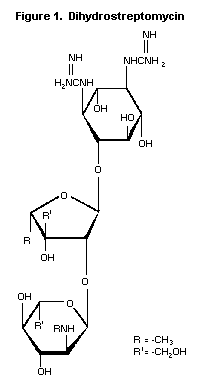
DIHYDROSTREPTOMYCIN
First draft prepared by
Dr Leena Gajjar
Veterinary Medicines Directorate
Ministry of Agriculture, Fisheries and Food
Addlestone, Surrey, United Kingdom
1. EXPLANATION
Both dihydrostreptomycin and streptomycin were evaluated at the
twelfth meeting of the Committee (Annex 1, Reference 17). An ADI was
not established for either compound at that time.
The two compounds are aminoglycoside antibiotics, and are closely
related in structure as shown in Figures 1 and 2 below.
 Both dihydrostreptomycin and streptomycin are used for treatment
of bacterial infections in food-producing animals.
Dihydrostreptomycin is formed by reduction of streptomycin. As
a result, pharmacokinetic properties, toxicological profiles, and
spectrum of antimicrobial and biological activity of the two compounds
are similar. Therefore, data on the two compounds were considered
together for the purpose of establishing a single ADI. The Committee
noted that the two compounds are generally considered together in the
published literature and in the report of the twelfth meeting of the
Committee. Complete toxicological monographs were prepared for each
compound and are provided in their entirety below.
2. BIOLOGICAL DATA
2.1 Biochemical aspects
2.1.1 Absorption, distribution and excretion
2.1.1.1 Rats
The sulfate and calcium chloride complex salts of streptomycin,
and the sulfate and hydrochloride salts of dihydrostreptomycin, were
administered orally in solution to groups of 5 rats at a single dose
of 7.5 g of antibiotic base per kg bw. Heart blood was withdrawn at
0.5, 1, 2, 3, and 4 hours, and assayed microbiologically using
Staphylococcus aureus. Peak blood levels of all four compounds were
measured at 1-2 hours. Streptomycin calcium chloride complex and
dihydrostreptomycin hydrochloride were better absorbed (peak blood
levels of 3200 to 4300 µg/ml, respectively) compared to the two
sulfate salts of each compound (peak blood levels of 200-300 µg/ml).
The elimination half-lives and AUCs were not calculated for this study
(Edison et al., 1951).
2.1.1.2 Cats
Nine female cats aged 4 to 6 months and weighing approximately 2
to 3 kg were given single intramuscular injections of 10 mg/kg bw each
of penicillin G and dihydrostreptomycin. Serum levels of each drug
were assayed by microbiological agar diffusion methods up to 32 hours
after injection. Dihydrostreptomycin was assayed using Bacillus
pumilis, and penicillin was assayed using either Bacillus subtilis
or Bacillus stearothermophilus. One cat had detectable penicillin
levels in the pre-treatment sample (0.04 µg/ml). Another cat died
within two minutes of the six-hour blood sample, which was taken by
heart puncture. Death was considered to be caused by the blood
sampling method, and therefore was not treatment-related.
Peak plasma levels of approximately 25 µg/ml were reached at
approximately 1 hour. The plasma elimination half-life was
approximately 1 hour, and the AUC was 61.4 ± 15.1 µg/ml/hour.
Dihydrostreptomycin was below the limit of detection (0.6 µg/ml) in
all animals by 24 hours after injection (Rudd & Silley, 1987d).
2.1.1.3 Dogs
Ten dogs (six females, four males, aged 1.5 to 4 years and
weighing approximately 11 to 22 kg) were given single intramuscular
injections of 10 mg/kg bw each of penicillin G and
dihydrostreptomycin. Serum levels of each drug were assayed by
microbiological agar diffusion methods up to 72 hours after injection.
Dihydrostreptomycin was assayed using Bacillus pumilis, and
penicillin was assayed using either Bacillus subtilis or Bacillus
stearothermophilus.
Peak plasma levels of approximately 41 µg/ml were reached at
approximately 1 hour. The plasma elimination half-life was
approximately 1 hour, and the AUC was 74.1 ± 8.50 µg/ml/hour.
Dihydrostreptomycin was below the limit of detection (0.6 µg/ml) in
all animals by 8 hours after injection (Rudd & Silley, 1987c).
2.1.1.4 Sheep
Ten female sheep aged 15 to 18 months and weighing approximately
60 to 90 kg were given single intramuscular injections of 10 mg/kg bw
each of penicillin G and dihydrostreptomycin. Serum levels of each
drug were assayed by microbiological agar diffusion methods up to 72
hours after injection. Dihydrostreptomycin was assayed using Bacillus
pumilis, and penicillin was assayed using either Bacillus subtilis
or Bacillus stearothermophilus.
Peak plasma levels of approximately 45 µg/ml were reached at
approximately 1 hour. The plasma elimination half-life was
approximately 2 hours, and the AUC was 151.5 ± 35.9 µg/ml/hour.
Dihydrostreptomycin was below the limit of detection (0.3 µg/ml) in
all animals by 24 hours after injection (Rudd & Silley, 1987b).
2.1.1.5 Cattle
Ten cattle (one male, nine females, weighing approximately 200
to 450 kg) were given single intramuscular injections of 10 mg/kg bw
each of penicillin G and dihydrostreptomycin. Serum levels of each
drug were assayed by microbiological agar diffusion methods up to 72
hours after injection. Dihydrostreptomycin was assayed using Bacillus
pumilis, and penicillin was assayed using either Bacillus subtilis
or Bacillus stearothermophilus.
Peak plasma levels of approximately 44 µg/ml were reached at
approximately 1 hour. The plasma elimination half-life was
approximately 5 hours, and the AUC was 207.2 ± 33.8 µg/ml/hour.
Dihydrostreptomycin was below the limit of detection (0.3 µg/ml) in
all animals by 48 hours after injection (Rudd & Silley, 1987a).
Two young Holstein-Friesian steers weighing approximately 300 kg
each were injected intramuscularly with uniformly tritiated
dihydrostreptomycin (specific activity 262 mCi/mmol) plus carrier drug
at a single dose of 25 mg/kg bw, given as three separate injections
into the scapular region. Plasma, urine, saliva and lachrymal
secretions were sampled up to 5 days after the injection. The maximal
concentrations in plasma and urine were 78 and 1875 µg/ml,
respectively, and were achieved at 3-4 hours after injection. Low drug
concentrations (1.7 µg/ml) were still detectable in urine at 96 hours
after injection. No radioactivity was detected in saliva or lachrymal
secretions. The apparent volume of distribution was 23%,
corresponding to the extra-cellular fluid. The absorption and
excretion rates were similar when assayed microbiologically with
Staphylococcus aureus (Stalheim, 1970).
Dihydrostreptomycin was administered intramuscularly to 21
heifers and 6 dairy cows at 5 and 7.5 mg/lb bw (11 and 16.5 mg/kg bw),
respectively. Peak blood levels were reached at 1-2 hours after
injection and averaged approximately 45 µg/ml (with a range of 8.5-
100 µg/ml) for the 11 mg/kg bw dose, and 65.0 µg/ml (with a range of
40-122 µg/ml) for the 16.5 mg/kg bw dose. Dihydrostreptomycin was
assayed in the milk of 7 cows which had been injected with 11 mg/kg
bw. The drug was detected in 4 cows only, at concentrations ranging
from trace levels to 6.25 µg/ml, at 4 to 18 hours after injection. The
limit of detection of the assay was not stated for either blood or
milk (Hammond, 1953).
After intramuscular administration of 0.5 g dihydrostreptomycin
per 100 lb (11.1 mg/kg bw) to 26 dairy cows, drug concentrations were
detectable in the milk from 11 animals. At 36 hours milk levels were
at the limit of detection of 0.04 µg/ml for 8 cows. At 48 hours the
drug was undetectable in all animals. When administered at 1 to 2
g per 100 lb bw (22 to 44 mg/kg bw) peak levels of 0.07 to 0.12 µg/ml
were reached in milk at 24 hours, but were below the limit of
detection at 48 hours (Blobel & Burch, 1960).
2.1.1.6 Pigs
Three cross-bred barrows weighing approximately 100 kg each were
injected intramuscularly with uniformly tritiated dihydrostreptomycin
(specific activity 262 mCi/mmol) plus carrier drug at a single dose of
25 mg/kg bw/day, given as three separate injections. Plasma and urine
were sampled up to 5 days after the injection. The maximal
concentrations in plasma and urine were approximately 90 and 7100
µg/ml, respectively, and were achieved 1-2 hours after injection. Low
drug concentrations (approximately 3 µg/ml) were still detectable in
urine at 86 hours after injection. The apparent volume of distribution
was 21%, corresponding to the extracellular fluid. The absorption and
excretion rates were similar when assayed microbiologically with
Staphylococcus aureus (Stalheim, 1970).
The results of the foregoing studies are summarized in Table 1.
2.1.1.7 Humans
As a class, aminoglycoside antibiotics cross membranes very
poorly and only about 1% of an oral dose is absorbed, even when there
is intestinal inflammation or ulceration (Pratt & Fekaty, 1986).
Dollery (1991) reported that after oral administration of
streptomycin, 60%-100% of the drug can be recovered unchanged from the
faeces.
Table 1. Pharmacokinetics parameters for dihydrostreptomycin after intramuscular administration to various species
(Values represent ± standard deviation or range)
Species Dose (i.m.) Cmax (plasma) Tmax hours AUC mcg/ Cmax urine t´ hours Vd Reference
(mg/kg bw) (µg/ml) (ml/hour) (µg/ml)
Cats 10 25.1 ± 8.6 1.2 ± 0.4 61.4 ± 15.1 - 1.4 ± 0.1 - Rudd & Silley, 1987d
Dogs 10 41.2 ± 8.07 0.8 ± 0.26 74.1 ± 8.50 - 1.0 ± 0.17 - Rudd & Silley, 1987c
Sheep 10 44.8 ± 14.3 0.8 ± 0.3 151.5 ± 35.9 - 2.3 ± 0.3 - Rudd & Silley, 1987b
Cattle 10 44.3 ± 15.2 1.1 ± 0.4 207.2 ± 33.8 - 4.9 ± 0.5 - Rudd & Silley, 1987a
Cattle 11 44.7 (8.5-100) 1 - 2 - - - - Hammond, 1953
Cattle 16.5 65.0 (40.0-122) 1 - 2 - - - - Hammond, 1953
Cattle 25 78 3 - 4 - 1875 - 23% Stalheim, 1970
Pigs 25 87 1 - 2 - 7120 - 21% Stalheim, 1970
The aminoglycosides are reported to have a volume of distribution
of 25% of lean body mass in adults, corresponding to the extracellular
fluid volume. The volume of distribution in neonates may average 60%
of body weight. The volume of distribution in obese individuals is
less than in those with normal body weight. The volume of distribution
also varies with edema, which tends to reduce serum concentrations,
and dehydration which increases serum concentrations. The presence of
fever reduces serum concentrations by up to 40%, due to increased
renal blood flow and glomerular filtration.
Aminoglycosides accumulate in the kidney relative to plasma
levels, and detectable concentrations of aminoglycosides persist in
urine for several weeks, suggesting binding of the drug to kidney.
Accumulation also occurs in the perilymph of the inner ear, where the
elimination half-life is much longer than in serum (10-12 hours in
perilymph compared to 2 hours in serum).
Aminoglycoside levels in interstitial fluid approximate serum
levels. In bile, 25-50% of serum levels are obtained in the absence of
biliary obstruction. In sputum and bronchial secretions 25-67% of
serum levels may be achieved; in pericardial, pleural and ascitic
fluids approximately 50% of serum levels are obtained; and synovial
fluid may contain 50-100% of serum levels. Penetration into the eye,
cerebrospinal fluid and ventricular fluid is very poor. Placental
transfer occurs and fetal serum concentrations range from 20-40% of
maternal serum levels (Pratt & Fekaty, 1986).
Approximately 20% of a parenteral dose of streptomycin cannot be
accounted for in urine, but no metabolites have yet been identified.
Approximately 1% is excreted in bile (Dollery, 1991).
The excretion rate after parenteral administration of
amino-glycosides is dependent on renal function and is linearly
related to the creatinine clearance rate. The elimination half-life in
adults is 2 hours, but 5-6 hours in neonates due to their lower
glomerular filtration rate (Pratt & Fekaty, 1986).
2.1.2 Biotransformation
The aminoglycosides are reported not to be metabolized in humans
and are excreted in their active forms by glomerular filtration (Pratt
& Fekaty, 1986).
2.1.3 Effects on enzymes and other biochemical parameters
No information available
2.2 Toxicological studies
2.2.1 Acute toxicity studies
2.2.1.1 Mice
The oral LD50 of different dihydrostreptomycin salts was compared
in male Carworth CF1 mice weighing 20 g on average.
Dihydrostreptomycin hydrochloride gave an LD50 of 12 500 mg/kg bw,
whereas the sulfate salt gave an LD50 of greater than 30 000 mg/kg bw
(Edison et al., 1951).
2.2.1.2 Chickens
The LD50 for dihydrostreptomycin sulfate administered
intramuscularly to groups of fifty 1, 2, 3, or 4 week-old chicks was
743, 1090, 1738, and 1868 mg/kg bw, respectively. Clinical signs of
toxicity in all birds were depression, drooping wings, closed eyes,
muscular weakness and slowed respiration (Huebner et al., 1956).
Dihydrostreptomycin sulfate was administered intramuscularly to
groups of 3 white Leghorn chickens weighing 600 g, at doses of 800 to
2500 mg/kg bw. Clinical signs of toxicity included ataxia,
prostration, gasping, and coma. The LD50 was 2167 mg/kg bw (Gray &
Purmalis, 1958).
2.2.1.3 Pigeons
Dihydrostreptomycin sulfate was administered intramuscularly at
doses of 400 to 1000 mg/kg bw to groups of 5 racing pigeons weighing
an average of 360 g. Clinical signs of toxicity included emesis,
somnolence, ataxia, depression, and coma. The LD50 was determined as
715 mg/kg bw (Gray & Purmalis, 1958).
2.2.1.4 Gerbils
A group of 10 gerbils (5/sex), 7-10 weeks of age and weighing
55-65 g were given single intramuscular injections of 50 mg
dihydrostreptomycin sulfate (equivalent to 769-909 mg/kg bw).
Ascending flaccid paralysis was observed in 10/10 animals at 2 to 5
minutes after injection, and 8/10 animals died within 4 to 25 minutes
after injection. The 2 surviving animals gradually regained muscle
control and awareness with apparently complete recovery at 65 and 120
minutes post-injection, respectively (Wightman et al., 1980).
The results of acute toxicity studies on dihydrostreptomycin are
summarized in Table 2.
Table 2. Acute toxicity of dihydrostreptomycin
Species Number Route LD50 mg/kg bw Reference
(age/weight) (salt)
Mice - oral >30 000 Edison et al., 1951
(20g) (sulfate)
12 500
(hydrochloride)
Chickens 50/group i.m. 743 - 1868 Huebner et al., 1956
(1-4 weeks) (sulfate)
Chickens 3/group i.m. 2167 Gray & Purmalis,
(600g) (sulfate) 1958
Pigeons 5/group i.m. 715 Gray & Purmalis,
(360g) (sulfate) 1958
Gerbil 10 i.m. < 769 Wightman et al., 1980
(7-10 weeks,
55-65g)
2.2.2 Short-term toxicity studies
2.2.2.1 Guinea-pigs
Three groups of 30 young adult guinea-pigs (15/sex/group) were
treated for 90 days with either 40 mg dihydrostreptomycin/kg bw/day in
distilled water by gavage, an equal volume of distilled water alone by
gavage (negative control), or 200 mg kanamycin/kg bw/day, s.c.
(positive control).
The kanamycin-treated animals exhibited spastic twitching
immediately after dosing, injection site reactions and some animals
became ataxic. Body-weight gain was depressed in the kanamycin group,
but was comparable to controls in the dihydrostreptomycin group.
Auditory function was assessed using the pinna twitch reflex
(Preyer reflex) in response to a whistle. Hearing loss was observed in
all the animals in the kanamycin group after week 6, and in two
negative control animals after weeks 7 to 9, which were later found to
be suffering from an inner ear infection. No hearing loss was observed
in the dihydrostreptomycin treated animals.
A large number of animals died during the study (7 negative
controls, 6 positive controls, and 6 treated with
dihydrostreptomycin). These were necropsied, as were all surviving
animals at the end of the study. All tissues with observed gross
lesions, plus the organ of Corti from all animals, were examined
histologically.
Of the animals treated by gavage, several animals died of a
ruptured oesophagus (3 negative controls and 3 in the
dihydrostreptomycin group). Almost all of the remaining animals dying
on test had lesions of the lungs due to pneumonia.
The authors reported that because the organs of Corti were
inadequately preserved they showed signs of degeneration,
histologically. However, the architecture of the cell layers and the
hair cells were still discernible. The positive control animals
(kanamycin group) demonstrated either no hair cells at any level of
the cochlea, or very few and damaged hair cells. The majority of
dihydrostreptomycin-treated animals had hair cells with largely normal
architecture, although hair cell damage was noted as being more severe
in males than females treated with dihydrostreptomycin (Tisdel &
Harris, 1976).
2.2.2.2 Cats
Dihydrostreptomycin was administered orally in a food vehicle
(liver cat food) to 3 groups of 10 cats (5/sex/group) weighing between
1.5 and 4.6 kg, for 90 days at doses of 1, 5 or 10 mg/kg bw/day. Ten
cats of each sex were used as controls.
One male cat in the mid-dose group died during the ninth week of
treatment. A watery red urethral discharge and a distended bladder
were observed in this animal the day prior to death, and pathological
examination revealed acute cystitis with concomitant peritonitis. All
other cats survived the 90 days of treatment and no compound-related
effects were observed on body-weight gain, food consumption,
haematology, blood chemistry, urinalysis, gross pathology or
histopathology (only liver and kidneys of controls and 10 mg/kg/day-
treated cats were examined) (Wazeter, 1970a).
Vestibular function was assessed in 10 cats (5/sex) treated daily
with oral doses of 40 mg dihydrostreptomycin/kg bw/day for 90 days.
Streptomycin sulfate was used as the positive control (200 mg/kg
bw/day, s.c.). Animals in the negative control group were
administered water by gavage.
Three cats died, one in each of the negative control, positive
control, and dihydrostreptomycin groups, due to urinary obstruction
which was considered unrelated to treatment.
For the dihydrostreptomycin group, no treatment-related effects
were observed on body weight, haematology, blood chemistry,
ophthalmoscopic examination, bone marrow smears, or gross pathology.
Vestibular function remained normal throughout the treatment period
based on results of righting reflex tests in which animals were
dropped from an inverted position two feet above a cushioned mat. The
NOEL was 40 mg/kg bw/day dihydrostreptomycin in this study. The
results with streptomycin are described in section 2.2.2.5 of the
monograph on streptomycin (Tisdel et al., 1976).
2.2.2.3 Sheep
A target animal safety study was conducted with
dihydro-streptomycin in 3 groups of 4 sheep (2/sex/group) aged 13 to
16 months and weighing approximately 45 kg to 70 kg. Animals were
treated with daily intramuscular injections of 10 mg procaine
penicillin G plus 10 mg dihydrostreptomycin/kg bw/day for 5
consecutive days (the recommended therapeutic treatment regime), the
second group received 30 mg of each drug/kg bw/day for 5 days, and the
third group received 10 mg of each drug/kg bw/day for 15 days. A
treatment-free control group was not included, although pre-treatment
parameters were measured in each animal.
Behaviour was normal and there were no clinical signs of
neuromuscular blockade. No localized injection site reactions were
observed. Pathological changes observed in skeletal muscle and liver
at post-mortem examination were largely due to parasitic infestations.
Slight congestion/consolidation was observed in the lungs at necropsy,
which was not examined further. There was no evidence of ototoxicity
based on results of a crude hearing test and normal histology of the
VIIIth cranial nerve. There was no pathological evidence of
nephrotoxicity at post-mortem examination. Urinalyses were not
performed.
Some haematological and biochemical parameters were altered
during and after treatment. Differences reached statistical
significance in some groups compared with pre-treatment values,
whereas other parameters were altered then subsequently recovered to
pre-treatment values. The haematological changes included a reduction
in haemoglobin, red cells, haematocrit and mean cell volume.
Biochemical changes included a decrease in sodium, phosphorus,
creatinine, and bilirubin, and an increase in chloride. The only
consistent dose-related trends were decreased sodium and increased
chloride levels during prolonged treatment (15-day group), and a lower
haematocrit in all treatment groups. These changes, although
statistically significant were small and were considered by the
authors not to be clinically relevant (Brooks & Rolph, 1989b).
2.2.2.4 Pigs
A target animal safety study was conducted with
dihydrostreptomycin in 3 groups of 4 pigs (2/sex/group in groups 2 and
3, 1 female and 3 males in group 1) approximately 8 weeks of age and
weighing between 23 and 29 kg. Animals were treated with daily i.m.
injections of 10 mg procaine penicillin G plus 10 mg
dihydrostreptomycin/kg initial bw/day for 5 consecutive days (the
recommended therapeutic treatment regime, group 1), the second group
received 30 mg of each drug/kg initial bw/day for 5 days (group 2),
and the third group received 10 mg of each drug/kg initial bw/day for
15 days (group 3). An untreated control group was not included,
although pre-treatment parameters were measured in all animals.
Body weights increased rapidly in all groups (in group 3 body
weights had increased by 50% after 15 days). Therefore the dose
administered on a body-weight basis was reduced with time,
particularly in group 3. A crude hearing test revealed no auditory
impairment, and behaviour was normal, except for 2 animals in group 3
that showed symptoms that were attributed to stress (vomiting,
inactivity, haematemesis and slight cyanosis of ears and legs) on days
1 and 15, respectively.
Changes were observed compared with pretreatment values in
haematology and serum chemistry values (reduced haemoglobin, red cells
and haematocrit, reduced neutrophils, increased mean corpuscular
haemoglobin, decreased creatinine, and increased calcium), some of
which reached statistical significance. However, there were no obvious
drug-related or time-related trends, and although statistically
significant, the changes were small and were considered by the authors
not to be clinically relevant.
The VIIIth cranial nerve was histologically normal in all but one
animal in group 1 in which focal chronic inflammation was observed.
Focal interstitial nephritis was observed in one pig in group 1 and
two pigs in group 2. These effects were not considered by the authors
to be treatment-related. No local injection site reactions were
observed (Brooks et al., 1989).
2.2.2.5 Cattle
A target animal safety study was conducted with
dihydrostreptomycin in 3 groups of 4 cattle (2/sex/group),
approximately 6 months of age and weighing between 100 and 170 kg.
Animals were treated with daily i.m. injections of 10 mg procaine
penicillin G plus 10 mg dihydrostreptomycin/kg bw/day for 5
consecutive days (the recommended therapeutic treatment regime), the
second group received 30 mg of each drug/kg bw/day for 5 days, and the
third group received 10 mg of each drug/kg bw/day for 15 days. An
untreated control group was not included, although pre-treatment
parameters were measured in each animal.
No consistent treatment-related effects on haematological or
biochemical parameters were observed. Behaviour was normal and there
were no clinical signs of neuromuscular blockade. The few injection
site reactions that were observed were minor in nature. The only
pathological changes present in tissues and organs at post-mortem
examination were in the lungs, which were attributed to respiratory
tract infection. There was no evidence of ototoxicity based on results
of a crude hearing test and normal histology of the VIIIth cranial
nerve. There was no histological evidence of nephrotoxicity at
post-mortem examination. Urinalyses were not performed (Brooks &
Rolph, 1989a).
2.2.3 Long-term toxicity/carcinogenicity studies
2.2.3.1 Rats
Dihydrostreptomycin was administered in the diet to Charles River
CD rats, (35/sex/group), to achieve dosages of approximately 1, 5, or
10 mg/kg bw/day for up to 2 years (dietary concentrations were
adjusted weekly to compensate for changes in food consumption and body
weight). Two control groups were included in the study. Five
rat/sex/group were scheduled for interim kills at 6 and 12 months. The
remaining 25 animals/sex/group were administered dihydro-streptomycin
for 2 years. Interim study reports were submitted at 6 and 18 months,
and a final report at 2 years.
In the 6-month interim report, it was reported that 2 rats died
in the low-dose group during the first week of treatment (cause of
death unknown), and were replaced. One male control rat died after its
6-month blood sample was taken. There were no treatment-related
effects observed on food consumption, haematology or urinalysis
(analyses from 5 rats/ sex/group at 3 and 6 months), hearing or
vestibular function (measured in all rats at 3 and 6 months). Serum
chemistry was not evaluated in this study. Body weights were slightly
decreased in males in all treatment groups compared with controls,
which reached statistical significance for all groups; however, no
clear dose-response relationship was established. One male rat in the
5 mg/kg bw/day group had a grossly abnormal posture from the seventh
treatment onwards, and was found to have severe bilateral suppurative
otitis media when necropsied at 6 months. One to two rats in all
treated groups, but no controls, were also reported to have this
condition at the 6 month necropsy when 5 animals per sex/group were
killed. No other treatment-related effects were noted on gross
pathology or histopathology. Histological examination of the auditory
system or associated nerves was not performed (Wazeter, 1970b).
In the 18-month interim report, the body weights of male rats in
the high-dose group were significantly reduced when compared to
control group 1 but not control group 2. Body weights in all other
male treatment groups were comparable to controls. No
treatment-related effects were observed on food consumption,
haematology, or urinalysis. No effects were reported on hearing or
vestibular function as defined by the tests used. One female rat in
the high-dose group had an abnormal posture and occasional slowed
righting reflex from week 73 onwards, and two males in the mid-dose
group had "impaired use of the hindquarters" from week 64 onwards, one
of which subsequently died in week 69. Mortality rates were similar
for all treatment and control groups at 78 weeks, ranging from 0 to 4
deaths per group of 25 animals. None of the deaths were considered by
the author to be treatment-related. Causes of death were reported as
due primarily to spontaneous neoplasias (usually of the pituitary or
mammary glands) and infectious processes; however, no gross pathology
or histopathology data were provided with the report (Wazeter, 1971).
In the two-year report, 12 to 17 out of 25 rats/sex in treated
groups had survived up to two years. No treatment-related effects were
observed on survival, food consumption, urinalysis, haematology, or
hearing. Body-weight gain was reduced in males in the high-dose group
compared to control group 2, but not control group 1. Body weights
were comparable to controls in all other groups. Vestibular function
was impaired in both control and treated groups (inability to remain
on a bar or abnormal gait was observed in 5 control rats, 2 rats each
in the low- and mid-dose groups, and 3 rats in the high-dose group, no
sex differences were observed). On necropsy, 2 rats in the high-dose
group had gross lesions of the middle ear (purulent otitis media). All
other gross pathological changes and histopathological changes
(examined in controls and high-dose group only) occurred with similar
frequency in all rats examined at two years. Neoplasms were observed
with comparable frequency in both treatment and control groups and
were similar to the historical control incidence for this facility.
Although this study did not meet current standards regarding the
number of animals started on the two-year phase of the study
(25/sex/group), the Committee concluded that survival of more than 50%
of all treated animals in the 2-year phase of the study (24/50, 33/50,
and 29/50 in the low-, mid-, and high-dose groups, respectively),
represented an adequate test of the carcinogenic potential of the
compound. The NOEL was 5 mg/kg bw/day based on decreased body-weight
gain in males at the high dose (Wazeter & Goldenthal, 1972).
2.2.4 Reproductive toxicity studies
No information available
2.2.5 Special studies on embryotoxicity/teratogenicity
2.2.5.1 Guinea-pigs
Streptomycin and dihydrostreptomycin were administered by daily
i.m. injection to groups of 2 to 4 pregnant guinea-pigs at doses of
10, 25, 50, 100 or 200 mg/kg bw/day. The duration of the treatment
period was not stated. A dose of 100-200 mg/kg bw/day of both drugs
caused abortion or death within 8-10 days. All fetusus were macerated,
indicating that death occurred prior to abortion or death of dams. At
doses of 25-50 mg/kg bw/day, some animals aborted, some survived, and
some stillbirths were observed. A dose of 10 mg/kg bw/day for 24 days
caused no abortions. The surviving F1 animals were clinically normal
with respect to vestibular and auditory function, and the CNS was
normal on histological examination. The placentae from streptomycin-
or dihydrostreptomycin-treated animals showed marked hyperaemia,
haemorrhage, and endometrial necrosis 24 hours after a single
intramuscular dose of 100 mg/kg bw. These changes progressed with
further treatment. Serum concentrations of dihydrostreptomycin and
streptomycin measured in the fetus were 2-4% of those in the dams
(Riskaer et al., 1952).
2.2.5.2 Rabbits
Groups of 31, 23, and 26 pregnant female Dutch rabbits, weighing
approximately 2 to 4 kg, were treated by oral intubation with 0, 5, or
10 mg dihydrostreptomycin/kg bw/day, respectively, from days 6 to 18
of gestation. The vehicle control group received 0.5% aqueous
methylcellulose.
One rabbit in the 5 mg/kg bw/day group was found dead on
gestation day 10. Four control rabbits and 1 in the 10 mg/kg bw/day
treatment group aborted, all after gestation day 14. No
treatment-related effects were observed on maternal behaviour,
appearance, or body-weight gain. On day 30, all animals were killed
for pathological examination. There were no treatment-related effects
on the pregnancy rate, number of corpora lutea, number of viable
fetuses, percentage of abnormal fetuses, litter size, mean fetal body
weight, or 24-hour survival rate. The number of abortions and
resorptions/empty implantation sites were higher in controls compared
to treated groups. Presence of a 13th rib was a frequently noted fetal
abnormality; however the incidence was similar in all groups. One
control fetus was acephalic with a ventral hernia, and one fetus in
the 5 mg/kg bw/day group had agenesis of skin and soft tissue over the
left lateral nasal and buccal area, and absent hind claws. All of
these findings were considered by the authors as unrelated to
treatment.
Because no maternal toxicity was observed, the Committee
concluded that the dose levels may not have been high enough to fully
exclude teratogenic potential (Wazeter, 1970c).
2.2.5.3 Humans
Auditory toxicity has been reported in children whose mothers
were treated with streptomycin and dihydrostreptomycin during
pregnancy. However, details of the dose administered and the timing
in relation to the pregnancy are often not stated (Davies, 1991;
Robinson & Cambon, 1964; Snider et al., 1980; Varpela et al.,
1969; Warkany, 1979).
Organogenesis of the inner ear occurs at week 7 of pregnancy, and
cochlear development continues up to mid-term (Varpela et al.,
1969). It is the only organ in the body to reach full adult size and
complete differentiation by midterm (Robinson & Cambon, 1964).
However, unlike teratogens, the toxic effects of streptomycin and
dihydrostreptomycin on the fetus are independent of the critical
periods of embryogenesis. Ototoxicity can occur throughout the
gestation period (Snider et al., 1980), as well as in adults (see
effects in humans, section 2.3.1 below). In children of streptomycin-
and dihydrostreptomycin-treated mothers, as well as in adults,
high-tone hearing is primarily affected first, which is outside of the
range of normal speech frequencies (Donald & Sellars, 1981).
The results of a literature review of pregnancy outcomes in women
receiving streptomycin or dihydrostreptomycin for tuberculosis is
presented by Snider et al., 1980. Of a total of 203 women, 206
pregnancies were followed to term. Seventy-two women received
streptomycin or dihydrostreptomycin during the first 4 months of
pregnancy, 73 women received one or the other after the fourth month,
and the timing was unknown for 61 women. The dose of streptomycin or
dihydrostreptomycin administered in these cases, where stated, was
between 1 g to 2 g daily or twice weekly, with total doses ranging
from 2 g to 202 g. Several other drugs were administered concomitantly
for tuberculosis, i.e. 88 women also received isoniazid, 1 received
rifampicin, 1 received ethambutol, 83 received p-amino-salicylic acid,
and for 59 women the other drug was not known. There were 2
spontaneous abortions, no premature births and no stillbirths, and 170
normal term infants were delivered. Abnormalities were observed in 35
infants (a rate of 169 per 1000, roughly 1 in 6, is reported by the
authors). The majority of these consisted of vestibular dysfunction
and varying degrees of hearing loss. Hearing loss occurred in the
high-tone range first, i.e. before the range of normal speech
frequencies was affected. No other abnormalities were reported (Snider
et al., 1980).
2.2.6 Special studies on genotoxicity
Streptomycin and dihydrostreptomycin bind to and alter the
configuration of the 30S subunit of ribosomes, thus inhibiting protein
synthesis and causing misreading of the genetic code. RNA and DNA
synthesis are unaffected (Goldberg, 1965; Davies et al., 1964).
The results of genotoxicity assays with dihydrostreptomycin are
summarized in Table 3.
Table 3. Results of genotoxicity assays on dihydrostreptomycin
Test system Test object Concentration Results Reference
In vitro
Cytogenetics Human lymphocytes 4.7-13.7 mg/ml Negative Obe, 1970
2.2.7 Special studies on immune responses
The incidence of allergic reactions in humans to systemically
administered aminoglycosides is reported to be very low (Pratt &
Fekaty, 1986).
2.2.8 Special studies on ototoxicity
2.2.8.1 Cats
The ototoxicity of streptomycin and dihydrostreptomycin was
investigated in cats after they had recovered from surgical
destruction of one ear. Seven cats were treated with streptomycin at
doses and treatment periods ranging from 200 mg/kg bw/day for 9.5 days
to 25 mg/kg bw/day for 84 days. Six cats were treated with
dihydrostreptomycin at doses and treatment periods ranging from 300
mg/kg bw/day for 21 days to 100 mg/kg bw/day for 60 days. After the
last dose, animals were kept treatment-free for 1 year then necropsied
for histopathological examination of the inner ear and the brain stem
nuclei.
Clinical signs of ototoxicity were similar in both groups, which
included permanent high frequency hearing loss, loss of
post-rotational nystagmus, and ataxia. Weight loss was also noted as
a treatment-related effect in both groups. With dihydrostreptomycin
treatment, the hearing loss was delayed and occurred several weeks to
several months after treatment.
In the inner ear, loss of hair cells in the cochlea, and damage
to the sensorimotor epithelium and hair loss in the cristae of the
vestibular canals were observed. The cristae appeared to be more
susceptable to toxic effects than the maculae of the saccule and
utricle.
In the brain stem, no lesions were found in the vestibular
nuclei. The vestibular portion of the VIIIth nerve was normal,
despite the fact that the sensorimotor epithelium and supporting cells
of the vestibular apparatus had been destroyed (surgically on one
side, and due to streptomycin and dihydrostreptomycin treatment on the
other side).
Effects observed in the brain stem included degenerative changes
in the ventral and dorsal cochlear nuclei, occurring primarily in
those parts corresponding to the ear which had been surgically
destroyed. In 2 animals treated with streptomycin, these lesions were
observed on the side corresponding to the ear which had not been
destroyed surgically. In these 2 animals, degeneration of the spiral
ganglion was also observed.
The authors described these degenerative changes as being typical
of trans-synaptic atrophy. The nuclei were smaller, containing smaller
nerve cells arranged more compactly, and changes were observed in the
myeloarchitecture. The cochlear branch of the VIIIth nerve appeared
shrunken with only a few myelinated fibres. There were no lesions in
the cerebellum or any other part of the brain stem.
The authors concluded that the lesions produced by both
streptomycin and dihydrostreptomycin were limited to the vestibular
end-organ of the inner ear in cats (McGee & Olszewski, 1962).
Dihydrostreptomycin was administered subcutaneously to groups of
2 cats at a dose of 800 mg/kg bw/day for 15 days or 200 mg/kg bw/day
for 120 days. Moderate to severe ataxia was observed from days 8 and
10 in the 800 mg/kg bw/day group, and from days 28 and 78 in the 200
mg/kg bw/day group. Animals were necropsied at the end of the
treatment period and the inner ear examined. Scattered degeneration of
the hair cells was observed in the cristae of the horizontal
semicircular canals, and was more severe in the high-dose group. The
cochlea of dihydrostreptomycin-treated cats was comparable to controls
as judged by electrophysiological studies of voltage changes at the
round window in response to tones of varying frequencies. The authors
reported that streptomycin produced more severe vestibular and
cochlear changes in a previous study than those produced by
dihydrostreptomycin; however, the doses of streptomycin used were not
stated. The authors also reported that cochlea of the cat appears to
be more sensitive to streptomycin than dihydrostreptomycin, whereas
the opposite is true in humans (Hawkins & Lurie, 1953).
2.2.9 Special studies on microbiological effects
2.2.9.1 Hamsters
Groups of 6 hamsters were fed a diet containing 0 or 10 mg/kg
dihydrostreptomycin. After 47 days, oxytetracycline (10 mg/kg) was
added to the diet and a suspension of E. coli (106 organisms/ml)
susceptible to both drugs was added to the drinking-water for two
weeks. Faecal samples were collected throughout the study and analyzed
for lactose-fermenting enteric organisms resistant to either
dihydrostreptomycin or oxytetracycline. No dihydrostreptomycin- or
oxytetracycline-resistant organisms were detected in the faeces at any
time (Rollins et al., 1975).
2.2.9.2 Dogs
Groups of 5 beagle dogs with an average weight of 15 kg were fed
a diet containing 0, 2, or 10 mg dihydrostreptomycin per kg of feed
(equivalent to 50 or 250 µg/kg bw/day) for 35 days. In both treatment
groups there was a shift in the faecal flora from predominantly
dihydrostreptomycin-susceptible lactose fermenting coliforms to a
resistant population after 15 days, which was significant (p < 0.01)
in both groups. This persisted throughout the 28-day post-treatment
phase of the study. A definitive response was not seen in the control
group. The authors concluded that the NOEL for development of drug
resistance in enteric bacteria was less than 2 mg/ kg of diet,
equivalent to 50 µg/kg bw/day (Gaines et al., 1978).
2.2.9.3 Humans
Healthy human volunteers were treated with 0.75 mg of
dihydrostreptomycin administered orally in a hamburger patty, 4 days
per week, for 7 weeks. Faecal samples were examined weekly for the
presence of coliforms bearing R-factor mediated resistance to
dihydrostreptomycin. The presence of resistant coliforms fluctuated
from week to week in about 30% of untreated controls. Fluctuations
were also observed in treated subjects. Four of 25 treated subjects
and 6/29 controls never excreted resistant coliforms; however, when
resistant coliforms were acquired, they tended to persist longer and
to multiply to greater numbers in the presence of dihydrostreptomycin
than in controls (Snyder et al., 1972).
2.2.9.4 Dairy starter cultures
Five strains each of various bacterial species were tested for
their sensitivity to dihydrostreptomycin by measuring zones of
inhibition of bacterial growth around discs impregnated with 2 or 10
µg/disc. The bacteria used were strains of Streptococcus (S.
lactis, S. cremoris, S. diacetilactis, S. thermophilus, S. durans, S.
faecalis) Lactobacillus bulgaricus, Brevibacterium linens,
Leuconostoc dextranicum, Staphylococcus (S. aureus, S. epidermidis),
and Micrococcus varians. All were susceptible except all
strains of Streptococcus faecalis and 3/5 strains of Streptococcus
durans (Reinbold & Reddy, 1974).
2.2.9.5 Minimum inhibitory concentrations in vitro
The minimum inhibitory concentration (MIC) of dihydrostreptomycin
sulfate was determined in vitro for bacteria isolated from the
intestines or faeces of healthy human adults. Over 100 isolates were
tested which represented 17 species and covered the 10 most common
genera of human intestinal microbes. The methods and controls used
were those proposed by the National Council for Clinical Laboratory
Standards (NCCLS) describing MIC assays for anaerobic bacteria.
E. coli was additionally assayed under aerobic conditions. The agar
dilution method was used, with Wilkins Chalgren agar or BHI agar
supplemented with 5% rabbit's blood, and incubations were for 48 hours
at 37 ± 2 °C. Dihydrostreptomycin was tested at serial double
dilutions from 128 µg/ml to 2 µg/ml. At each concentration, bacterial
cells were tested at two densities, 1 x 105 cells per spot, which is
recommended by NCCLS for clinical isolates, and 1 x 107 cells per
spot, which is considered to be more representative of the bacterial
concentration within the intestinal ecosystem. The results of this
study are summarized in Table 4.
Bifidobacterium spp. were found to be the most sensitive. Data
available for 5 strains of Bifidobacterium adolescentis gave an
MIC50 value of 32 µg/ml and a MIC range of 16-64 µg/ml, and data on
5 strains of Bifidobacterium longum gave an MIC50 value of 16 µg/ml
and a MIC range of 8-32 µg/ml.
The MIC50 value for dihydrostreptomycin in most of the other
bacterial species tested (17 bacterial species, with 5-11 strains
tested per species) was higher than 32 µg/ml, with the highest MIC50
values being more than 128 µg/ml.
An MIC50 value of 32 µg/ml was therefore established as the
concentration without effect on the human gut flora (Carman, 1994).
Table 4. MIC values for bacterial isolates from human intestinal material
(All values represent mcg/ml)
Species 1 x 107 cells / spot 1 x 105 cells / spot
n = no. of strains MIC50 MIC90 Range MIC50 MIC90 Range
E. coli 16 64 8-64 16 32 8-64
(aerobic) n=11
E. coli 64 128 32->128 32 64 16-128
(anaerobic) n=11
Bacteroides vulgatus >128 >128 128-128 >128 >128 64->128
n=5
Bacteroides uniformis >128 >128 >128 >128 >128 >128
n=5
Bifidobacterium 32 64 16-64 32 32 8-32
adolescentis
n=5
Bifidobacterium 16 32 8-32 16 16 8-32
longum n=5
Lactobacillus >128 >128 64->128 128 >128 32->128
acidophilus n=10
Fusobacterium >128 >128 128->128 >128 >128 128->128
russi n=5
Fusobacterium >128 >128 128->128 >128 >128 64->128
prauznitii n=5
Peptostreptococcus >128 >128 64->128 >128 >128 64->128
DZ n=5
Peptostreptococcus >128 >128 128->128 >128 >128 128->128
productus 1 n=5
Ruminococcus 64 64 64 64 64 32-64
gnavus n=5
Ruminococcus 64 64 64-128 64 64 64
bromii n=5
Table 4 (contd)
Species 1 x 107 cells / spot 1 x 105 cells / spot
n = no. of strains MIC50 MIC90 Range MIC50 MIC90 Range
Eubacterium >128 >128 128->128 >128 >128 64->128
aerofaciens n=5
Eubacterium >128 >128 >128 >128 >128 128->128
rectale n=5
Coprococcus 64 64 64-128 32 64 32-64
eutactus n=5
Coprococcus 64 64 32-64 32 64 32-64
comes n=5
Gemmiger 64 128 64->128 64 128 32->128
formicilis n=10
2.3 Observations In humans
2.3.1 Ototoxicity
The aminoglycosides are all potentially toxic to the inner ear at
therapeutic doses. Streptomycin-induced ototoxicity primarily affects
the vestibular system before auditory function is affected, whereas
dihydrostreptomycin primarily affects the cochlea before vestibular
function is affected. With both streptomycin and dihydrostreptomycin
hearing loss occurs in the high tone range first, i.e. before the
range of frequencies associated with normal speech is affected
(Martindale, 1993; Davies, 1991; Shambaugh et al., 1959; Hawkins &
Lurie, 1953; Pratt & Fekaty, 1986).
The primary toxic effect of both streptomycin and
dihydrostreptomycin is on the peripheral sensory portions of the inner
ear rather than on the eighth cranial nerve itself, which results in
progressive destruction of the hair cells of the Organ of Corti from
the basal region (responsive to high-frequency sounds) to the apex of
the cochlea (responsive to low-frequency sounds) as dosage and
duration of treatment are increased (Davies, 1991).
Dihydrostreptomycin causes delayed ototoxicity in humans
manifested as a sensorineural hearing loss which may involve any or
all frequencies. Hearing loss may occur from 1 to 6 months after drug
treatment, it is permanent, and it is not related to the size of the
dose (McGee & Olszewski, 1962; Shambaugh et al., 1959).
Aminoglycosides, including streptomycin and dihydrostreptomycin,
accumulate in the perilymph of the inner ear (Davies, 1991). A large
proportion of both drugs are excreted unchanged by the kidneys (Pratt
& Fekaty, 1986), and the risk of ototoxicity is therefore increased
when renal function is compromised (Erlansen & Lundgren, 1964).
Patients presenting with ototoxic side effects after treatment
with streptomycin, dihydrostreptomycin or kanamycin, for various
clinical conditions, were studied in a retrospective study. The route
of administration was not stated, although it was probably
intramuscular injection.
Two patients receiving a 50:50 mixture of streptomycin and
dihydrostreptomycin at doses of 0.5 or 1.0 mg/kg bw/day of each drug
(total dose 5 or 14.5 g of each drug) reported vertigo at the end of
the course of treatment. Four patients receiving dihydro-streptomycin
at a dose of 1 g per day (equivalent to 14 to 20 mg/kg bw/day, total
dose 6 to 36 g) reported tinnitus or impaired hearing (as assessed by
tone audiometry) between 2 weeks and 3 months after the course of
treatment. None of the patients in this group reported vertigo. Three
of these patients had impairment of renal function which may have
increased blood levels of dihydrostreptomycin and hence increased the
risk of ototoxicity. It was not stated whether the renal impairment
was pre-existing or caused by dihydrostreptomycin treatment (Erlanson
& Lundgren, 1964).
Dihydrostreptomycin has been reported to be more likely to cause
partial or complete hearing loss than streptomycin and was therefore
not recommended for use in humans (Martindale, 1993).
2.3.2 Renal toxicity
Nephrotoxicity due to aminoglycosides usually presents in humans
as an acute tubular necrosis manifested as proteinuria, cylinduria and
inability to concentrate the urine. This is followed by a reduction in
glomerular filtration rate with a rise in serum creatinine and blood
urea nitrogen. Aminoglycosides bind to the luminal surface of the
proximal tubules, are internalized by pinocytosis and fuse with
lysosomes. It is postulated that they become sequestered in lysosomes
where they disrupt phospholipid metabolism (prominant myeloid bodies
have been observed in renal tubular cells exposed to gentamicin), and
renal cell death occurs consequent to changes in lysosomal
biochemistry (Pratt & Fekaty, 1986).
2.3.3 Neuromuscular blockade
Aminoglycosides can produce a non-depolarizing type of
neuromuscular blockade due to reduced acetylcholine release from motor
nerve endings and reduced sensitivity of the post-junctional endplate;
this effect is completely reversed by administration of calcium (Pratt
& Fekaty, 1986).
2.3.4 Allergic reactions
The incidence of allergic reactions to systemically administered
aminoglycosides is reported to be very low. The incidence of allergic
reactions to dihydrostreptomycin specifically was not reported (Pratt
& Fekaty 1986).
2.3.5 Other effects
Aminoglycosides have been reported to cause neutropenia,
agranulocytosis, and aplastic anaemia on rare occasions. Transient
elevation of hepatic enzymes occurs occasionally with
amino-glycosides. The incidence of specific effects associated with
dihydrostreptomycin were not reported (Pratt & Fekaty, 1986).
5. REFERENCES
ANDERSON, D.G. & JEWELL, M. (1945). The absorption, excretion and
toxicity of streptomycin in man. New Engl. J. Med., 233: 485-491.
BACHARACH, A.L., CLARK, B.J., McCULLOCH, M., & TOMICH, E.G. (1959).
Comparative toxicity studies on ten antibiotics in current use.
J. Pharm. & Pharmacol., 11: 737-741.
BEEK, B., GÖBEL, D., OBE, G., & RADENBACH K.L. (1974). Prospective
controlled clinical trial of antitubercular agents in triple
combinations for mutagenicity in leukocyte cultures (short report).
Prax. Pneumol., 28: 970.
BERG, K. (1951). The toxic effect of streptomycin on the vestibular
and cochlear apparatus: an experimental study on cats. Acta Otolaryn
(Stoch), suppl. 97: 1-77.
BLOBEL, H., & BURCH, C.W. (1960). Diffusion of dihydrostreptomycin and
chlortetracycline into milk of dairy cows following parenteral
administration. J. Amer. Vet. Med. Assoc., 137 698-700.
BOUCHER, D & DELOST, P. (1964). Developpement post-natal des
descendants issus de meres traités par la streptomycine au cours de la
gestation chez la souris. C.R. Soc, Biol. (Paris), 158: 2065-2069.
BRITISH PHARMACEUTICAL CODEX (1968). The Pharmaceutical Press, London.
BROOKS, C., & ROLPH, T.P. (1989a). The effect of streptopen injection
on the health of cattle. Unpublished report No. AnH89/R/65 from
Pitman-Moore Ltd., Uxbridge, Middlesex, England. Submitted to WHO by
Pitman-Moore, Inc., Mundelein, IL, USA.
BROOKS, C., & ROLPH, T.P. (1989b). The effect of streptopen injection
on the health of sheep. Unpublished report No. AnH89/R/66 from Pitman-
Moore Ltd., Uxbridge, Middlesex, England. Submitted to WHO by Pitman-
Moore, Inc., Mundelein, IL, USA.
BROOKS, C., EASTWOOD, B., & ROLPH, T.P. (1989). The effect of
streptopen injection on the health of pigs. Unpublished report No.
AnH89/R/75 from Pitman-Moore Ltd., Uxbridge, Middlesex, England.
Submitted to WHO by Pitman-Moore, Inc., Mundelein, IL, USA.
BYWATER, R.J. (1982). Aminoglycoside antibiotics. In: Brander, G.C.,
Pugh, D.M. & Bywater, R.J. (eds.), Veterinary Applied Pharmacology and
Therapeutics, 4th edition, Balliere Tindall, London, pp. 387-393.
CARMAN, R.J. (1994). Dihydrostreptomycin MIC determinations for human
gut flora. Unpublished report from TechLab Inc., VPI Research Park,
Blacksburg, Virginia 24060, USA. Submitted to WHO by Norbrook
Laboratories Ltd., Newry, Northern Ireland.
CHRISTENSEN, E., HERTZ, H., RISKAER, N. & VRA-JENSEN, G. (1951).
Histological investigations in chronic streptomycin poisoning in
guinea-pigs. Ann. Otol., 60: 343-349.
CLARK, C.H. (1977). Toxicity of aminoglycoside antibiotics. Modern
Veterinary Practice, Part 7, 58: 594-598.
DAS, B.C., & SHARMA, T. (1983). Reduced frequency of baseline sister
chromatid exchanges in lymphocytes grown in antibiotics- and serum-
excluded culture medium. Hum Gen., 64: 249-253.
DAVIES, D.M. (1991). Textbook of adverse drug reactions. Fourth
edition, Oxford University Press, London, p. 51.
DAVIES, J., GILBERT, W., & GORINI, L. (1964). Streptomycin suppression
and the code. Proc. Nat. Acad. Sci., 51: 883-890.
DESALVA, S.J., EVANS, R.A., & MARCUSSEN, H.W. (1969). Lethal effects
of antibiotics in hamsters. Toxicol. Appl. Pharmacol., 14: 510-514.
DOLLERY, C. (1991). Therapeutic Drugs, C. Dollery (ed.), Churchill
Livingston, London, pp. 100-103.
DONALD, P.R. & SELLARS, S.L. (1981). Streptomycin ototoxicity in the
unborn child. S. Afr. Med. J., 60: 316-318.
EDISON, A.O., KUNA, S., CUCHIE, F.T. & HANSON, J.T. (1951). Relative
absorption of salts of streptomycin and dihydrosreptomycin after oral
administration. Antibiotics & Chemotherapy, 1: 49-53.
ELIAS, W.F. & DURSO, J. (1945). Blood, urine and faecal levels of
streptomycin in the treatment of human infections of E. Typhosa.
Science, 101: 589-591.
ERICSON-STRANDVIK, B. & GYLLENSTEN L. (1963). The central nervous
system of fetal mice after administration of streptomycin. Acta
Pathol. Microbiol. Scand., 59: 292-300.
ERLANSON, P., & LUNDGREN, A. (1964). Ototoxic side effects following
treatment with streptomycin, dihydrostreptomycin and kanamycin. Acta
Medica Scandinavica, 176: fasc. 2.
GAINES, S.A., ROLLINS, L.D., SILVER, R.P, & WASHINGTON, M. (1978).
Effects of low concentrations of dihydrostreptomycin on drug
resistance in enteric bacteria. Antimicrobial agents and
chemotherapy, 14: 252-256.
GOLDBERG, I.H. (1965). Mode of action of antibiotics. II. Drugs
affecting nucleic acid and protein synthesis. Am. J. Med., 39: 722-
752.
GRAHAM, B.E., VANDER BROOK, N.J. & KUIZENGA, M.H. (1946). Preliminary
studies on the absorption and excretion of streptomycin in dogs.
Science, 103: 364-365.
GRAY, J.E. & PURMALIS A. (1958). The acute toxicity of procaine
penicillin G and of dihydrostreptomycin sulfate in the pigeon and the
chicken. Avian Disease, 2: 187-196.
HAMMOND P.B. (1953). Dihydrostreptomycin dose-serum level relationship
in cattle. J. Amer. Vet. Med. Assoc., 122: 203-206.
HAWKINS, J.E. & LURIE, M.H. (1953). The ototoxicty of
dihydrostreptomycin and neomycin in the cat. Ann. Otol., 62: 1128-
1148.
HUBER, W.G. (1966). Streptomycin. In: Veterinary Pharmacology and
Therapeutics, Leo Meyer Jones (ed), 3rd edition, Iowa State College
Press, pp. 519-530.
HUEBNER, R.A., GLASSMAN, J.M., HUDYMA, G.M. & SEIFTER, J. (1956). The
toxic dose of dihydrostreptomycin in fowl. Cornell Vet., 46: 219-
212.
JAJU, M., JAJU, M., & AHUJA, Y.R. (1983). Cytogenetic effects of
chemotherapy with three combinations of anti-tubercular drugs
involving isoniazid, thiacetazone, para-amino-salicylic acid and
streptomycin on human lymphocytes: chromosome aberrations, sister
chromatids exchanges and mitotic index. Hum. Gen., 64: 42-49.
KERN, G. (1962). Zur Frage der Intrauterine Streptomycin Schadigung.
Schweiz. Med. Wochenschr., 92: 77-79.
KODAMA, F., FUKUSHIMA, F., & UMEDA, M. (1980). Chromosome aberrations
induced by clinical medicines. J. Tox. Sci., 5: 141-150.
MARSHALL, E.K. (1948). The absorption, distribution and excretion of
streptomycin. J. Pharmacol. Exper. Therapeut., 92: 43-48.
MARTINDALE, (1993). The extra pharmacopoeia. Reynolds, J.E.F. (ed.),
30th Edition, Pharmaceutical Press, pp. 159-160.
MARYNOWSKI, A., & SIANOZECKA, E. (1972). Comparison of the incidence
of congenital malformations in neonates from healthy mothers and from
patients treated for tuberculosis. Ginekol. Pol., 43: 713-715.
McGEE, T.M., & OLSZEWSKI, J. (1962). Streptomycin sulphate and
dihydrostreptomycin toxicity. Arch. Otolaryngol., 75: 295-311.
MOLITOR, H., GRAESSLE, O.E., KUNA, S., MUSHETT, C.W., SILBER, R.H.
(1946). Some toxicological and pharmacological properties of
streptomycin. J. Pharm. Exp. Ther., 86: 151-173.
NAKAMOTO, Y., OTANI, H., & TANAKA, O. (1985). Effects of
aminoglycosides administered to pregnant mice on postnatal development
of inner ear in their offspring. Teratology, 32: 34B.
NEU, R., ASPILLAGA, M.J., & GARDNER, L.I. (1965). Effects of
antibiotics on chromosomes of cultured human leucocytes. Nature
(London), 205: 171-172.
NOMURA, T., KIMURA, S., KANZAKI, T., ET AL. (1984). Induction of
tumors and malformations in mice after prenatal treatment with some
antibiotic drugs. Med. J. Osaka Univ., 35: 13-17.
OBE, G. (1970). The effect of streptomycin and dihydrostreptomycin on
human chromosomes in vitro. Molec. Gen. Genetics, 107: 361-365.
PRATT, W.B., & FEKATY, R. (1986). Bactericidal inhibitors of protein
synthesis, the aminoglycosides. In: The antimicrobial drugs, Chapter
7, Oxford University Press, Oxford, pp. 153-183.
REINBOLD, G.W., & REDDY, M.S. (1974). Sensitivity or resistance (of)
dairy starter and associated micro-organisms to selected antibiotics.
J. Milk Food Technol., 37: pp. 517-521.
RISKAER, N., CHRISTENSEN, E. & HERTZ, H. (1952). The toxic effects of
streptomycin and dihydrostreptomycin in pregnncy, illustrated
experimentally. Acta Tuber. Pneumol. Scand., 27: 211-216.
ROBINSON, C.G. & CAMBON, K.G. (1964). Hearing loss in infants of
tuberculous mothers treated with streptomycin during pregnancy.
N. Engl. J. Med., 271: 949-951.
ROLLINS, L.D., GAINES, S.A., POCURULL, D.W., & MERCER, H.D. (1975).
Animal model for determining the no-effect level of an antimicrobial
drug on drug resistance in the lactose-fermenting enteric flora.
Antimicrobial Agents and Chemotherapy, 7: 661-665.
RUDD, A.P., & SILLEY, P. (1987a). Antibiotic concentrations in cattle
serum following a single intramuscular injection of Streptopen
injection. Unpublished report No. An.H.87/R/22 from Pitman-Moore Ltd.,
Uxbridge, Middlesex, England. Submitted to WHO by Pitman-Moore, Inc.,
Mundelein, IL, USA.
RUDD, A.P., & SILLEY, P. (1987b). Antibiotic concentrations in sheep
serum following a single intramuscular injection of Streptopen
injection. Unpublished report No. An.H.87/R/27 from Pitman-Moore Ltd.,
Uxbridge, Middlesex, England. Submitted to WHO by Pitman-Moore, Inc.,
Mundelein, IL, USA.
RUDD, A.P., & SILLEY, P. (1987c). Antibiotic concentrations in dog
serum following a single intramuscular injection of Streptopen
injection. Unpublished report No. An.H.87/R/34 from Pitman-Moore Ltd.,
Uxbridge, Middlesex, England. Submitted to WHO by Pitman-Moore, Inc.,
Mundelein, IL, USA.
RUDD, A.P., & SILLEY, P. (1987d). Antibiotic concentrations in cat
serum following a single intramuscular injection of Streptopen
injection. Unpublished report No. An.H.87/R/42 from Pitman-Moore Ltd.,
Uxbridge, Middlesex, England. Submitted to WHO by Pitman-Moore, Inc.,
Mundelein, IL, USA.
SHAMBAUGH, G.E., DERLACKI, E.L., HARRISON, W.H., HOUSE, H., HOUSE, W.,
HILDYARD, V., SCHUKNECHT, H., & SHEA, J.J. (1959). Dihydrostreptomycin
deafness. JAMA, 170: 1657-1660.
SNIDER, D.E., LAYDE, P.M., JOHNSON, M.W. & LYLE, M.A. (1980).
Treatment of tuberculosis during pregnancy. Am. Rev. Resp. Dis.,
122: 65-79.
SNYDER, M. J., AL-IBRAHIM, M., & HORNICK, R. B. (1972). The effect of
oral DHS on resistance development in the intestinal microflora of
man. Unpublished report from the Division of Infectious Diseases,
Department of Medicine, University of Maryland School of Medicine.
Submitted to WHO by FDA.
STALHEIM, O.H.V. (1970). Absorption and excretion of tritiated
dihydrostreptomycin in cattle and swine. American Journal of
Veterinary Research, 31: 497-499.
STEBBINS, R.B., GRAESSLE, O.E., & ROBINSON H.J. (1945). Studies on the
absorption and excretion of streptomycin in animals. Proc. Soc. Exp.
Biol. Med., 60: 68-72.
STEVENSON, L.D., ALVORD, E.C., & CORRELL, J. W. (1947). Degeneration
and necrosis of neurones in eighth cranial nuclei caused by
streptomycin. Proc. Soc. Exp. Biol. Med., 65: 86-88.
TISDEL, M., & HARRIS, D.L. (1976). Dihydrostreptomycin: 90-day
toxicity study in guinea pigs. Unpublished report, Warf Study Code T-
615 from Warf Institute, Inc., Madison, Wisconsin, USA, on behalf of
Animal Health Institute. Submitted to WHO by FDA.
TISDEL, M., HARRIS, D.L., HAARS, R., & NEES, P.O. (1976).
Dihydrostreptomycin: 90-day toxicity study in cats. Unpublished
report, Warf Study Code T-614 from Warf Institute, Inc., Madison,
Wisconsin, USA, on behalf of Animal Health Institute. Submitted to WHO
by FDA.
TSANG, Y.C., & CHIN, T.C. (1963). Neurotoxicity of streptomycin.
Scientia Sinica, 12: 1019-1040.
VARPELA, E., HIETALAHTI, J., & ARO, M.J.T. (1969). Streptomycin and
dihydrostreptomycin medication during pregnancy and their effect on
the child's inner ear. Scand. J. Resp. Dis., 50: 101-109.
WARKANY, J. (1979). Antituberculous drugs. Teratology, 20: 133-138.
WAZETER, F. X. (1970a). Dihydrostreptomycin: Ninety-day toxicity study
in cats. Unpublished report from International Research and
Development Corporation on behalf of Animal Health Institute.
Submitted to WHO by FDA.
WAZETER, F. X. (1970b). Dihydrostreptomycin: Two-year oral toxicity
study in rats (six month interim report). Unpublished report from
International Research and Development Corporation on behalf of Animal
Health Institute. Submitted to WHO by FDA.
WAZETER, F. X. (1970c). Dihydrostreptomycin: Rabbit teratogenic study.
Unpublished report from International Research and Development
Corporation on behalf of Animal Health Institute. Submitted to WHO by
FDA.
WAZETER, F. X. (1971). Dihydrostreptomycin: Two-year oral toxicity
study in rats (18 month interim report). Unpublished report from
International Research and Development Corporation on behalf of Animal
Health Institute. Submitted to WHO by FDA.
WAZETER, F. X., & GOLDENTHAL, E.I. (1972). Dihydrostreptomycin: Two-
year oral toxicity study in rats. Unpublished report from
International Research and Development Corporation on behalf of Animal
Health Institute. Submitted to WHO by FDA.
WIGHTMAN, S.R., MANN, P.C., & WAGNER, J.E. (1980). Dihydrostreptomycin
toxicity in the Mongolian gerbil, Meriones unguiculatus. Laboratory
Animal Science, 30: 71-75.
Both dihydrostreptomycin and streptomycin are used for treatment
of bacterial infections in food-producing animals.
Dihydrostreptomycin is formed by reduction of streptomycin. As
a result, pharmacokinetic properties, toxicological profiles, and
spectrum of antimicrobial and biological activity of the two compounds
are similar. Therefore, data on the two compounds were considered
together for the purpose of establishing a single ADI. The Committee
noted that the two compounds are generally considered together in the
published literature and in the report of the twelfth meeting of the
Committee. Complete toxicological monographs were prepared for each
compound and are provided in their entirety below.
2. BIOLOGICAL DATA
2.1 Biochemical aspects
2.1.1 Absorption, distribution and excretion
2.1.1.1 Rats
The sulfate and calcium chloride complex salts of streptomycin,
and the sulfate and hydrochloride salts of dihydrostreptomycin, were
administered orally in solution to groups of 5 rats at a single dose
of 7.5 g of antibiotic base per kg bw. Heart blood was withdrawn at
0.5, 1, 2, 3, and 4 hours, and assayed microbiologically using
Staphylococcus aureus. Peak blood levels of all four compounds were
measured at 1-2 hours. Streptomycin calcium chloride complex and
dihydrostreptomycin hydrochloride were better absorbed (peak blood
levels of 3200 to 4300 µg/ml, respectively) compared to the two
sulfate salts of each compound (peak blood levels of 200-300 µg/ml).
The elimination half-lives and AUCs were not calculated for this study
(Edison et al., 1951).
2.1.1.2 Cats
Nine female cats aged 4 to 6 months and weighing approximately 2
to 3 kg were given single intramuscular injections of 10 mg/kg bw each
of penicillin G and dihydrostreptomycin. Serum levels of each drug
were assayed by microbiological agar diffusion methods up to 32 hours
after injection. Dihydrostreptomycin was assayed using Bacillus
pumilis, and penicillin was assayed using either Bacillus subtilis
or Bacillus stearothermophilus. One cat had detectable penicillin
levels in the pre-treatment sample (0.04 µg/ml). Another cat died
within two minutes of the six-hour blood sample, which was taken by
heart puncture. Death was considered to be caused by the blood
sampling method, and therefore was not treatment-related.
Peak plasma levels of approximately 25 µg/ml were reached at
approximately 1 hour. The plasma elimination half-life was
approximately 1 hour, and the AUC was 61.4 ± 15.1 µg/ml/hour.
Dihydrostreptomycin was below the limit of detection (0.6 µg/ml) in
all animals by 24 hours after injection (Rudd & Silley, 1987d).
2.1.1.3 Dogs
Ten dogs (six females, four males, aged 1.5 to 4 years and
weighing approximately 11 to 22 kg) were given single intramuscular
injections of 10 mg/kg bw each of penicillin G and
dihydrostreptomycin. Serum levels of each drug were assayed by
microbiological agar diffusion methods up to 72 hours after injection.
Dihydrostreptomycin was assayed using Bacillus pumilis, and
penicillin was assayed using either Bacillus subtilis or Bacillus
stearothermophilus.
Peak plasma levels of approximately 41 µg/ml were reached at
approximately 1 hour. The plasma elimination half-life was
approximately 1 hour, and the AUC was 74.1 ± 8.50 µg/ml/hour.
Dihydrostreptomycin was below the limit of detection (0.6 µg/ml) in
all animals by 8 hours after injection (Rudd & Silley, 1987c).
2.1.1.4 Sheep
Ten female sheep aged 15 to 18 months and weighing approximately
60 to 90 kg were given single intramuscular injections of 10 mg/kg bw
each of penicillin G and dihydrostreptomycin. Serum levels of each
drug were assayed by microbiological agar diffusion methods up to 72
hours after injection. Dihydrostreptomycin was assayed using Bacillus
pumilis, and penicillin was assayed using either Bacillus subtilis
or Bacillus stearothermophilus.
Peak plasma levels of approximately 45 µg/ml were reached at
approximately 1 hour. The plasma elimination half-life was
approximately 2 hours, and the AUC was 151.5 ± 35.9 µg/ml/hour.
Dihydrostreptomycin was below the limit of detection (0.3 µg/ml) in
all animals by 24 hours after injection (Rudd & Silley, 1987b).
2.1.1.5 Cattle
Ten cattle (one male, nine females, weighing approximately 200
to 450 kg) were given single intramuscular injections of 10 mg/kg bw
each of penicillin G and dihydrostreptomycin. Serum levels of each
drug were assayed by microbiological agar diffusion methods up to 72
hours after injection. Dihydrostreptomycin was assayed using Bacillus
pumilis, and penicillin was assayed using either Bacillus subtilis
or Bacillus stearothermophilus.
Peak plasma levels of approximately 44 µg/ml were reached at
approximately 1 hour. The plasma elimination half-life was
approximately 5 hours, and the AUC was 207.2 ± 33.8 µg/ml/hour.
Dihydrostreptomycin was below the limit of detection (0.3 µg/ml) in
all animals by 48 hours after injection (Rudd & Silley, 1987a).
Two young Holstein-Friesian steers weighing approximately 300 kg
each were injected intramuscularly with uniformly tritiated
dihydrostreptomycin (specific activity 262 mCi/mmol) plus carrier drug
at a single dose of 25 mg/kg bw, given as three separate injections
into the scapular region. Plasma, urine, saliva and lachrymal
secretions were sampled up to 5 days after the injection. The maximal
concentrations in plasma and urine were 78 and 1875 µg/ml,
respectively, and were achieved at 3-4 hours after injection. Low drug
concentrations (1.7 µg/ml) were still detectable in urine at 96 hours
after injection. No radioactivity was detected in saliva or lachrymal
secretions. The apparent volume of distribution was 23%,
corresponding to the extra-cellular fluid. The absorption and
excretion rates were similar when assayed microbiologically with
Staphylococcus aureus (Stalheim, 1970).
Dihydrostreptomycin was administered intramuscularly to 21
heifers and 6 dairy cows at 5 and 7.5 mg/lb bw (11 and 16.5 mg/kg bw),
respectively. Peak blood levels were reached at 1-2 hours after
injection and averaged approximately 45 µg/ml (with a range of 8.5-
100 µg/ml) for the 11 mg/kg bw dose, and 65.0 µg/ml (with a range of
40-122 µg/ml) for the 16.5 mg/kg bw dose. Dihydrostreptomycin was
assayed in the milk of 7 cows which had been injected with 11 mg/kg
bw. The drug was detected in 4 cows only, at concentrations ranging
from trace levels to 6.25 µg/ml, at 4 to 18 hours after injection. The
limit of detection of the assay was not stated for either blood or
milk (Hammond, 1953).
After intramuscular administration of 0.5 g dihydrostreptomycin
per 100 lb (11.1 mg/kg bw) to 26 dairy cows, drug concentrations were
detectable in the milk from 11 animals. At 36 hours milk levels were
at the limit of detection of 0.04 µg/ml for 8 cows. At 48 hours the
drug was undetectable in all animals. When administered at 1 to 2
g per 100 lb bw (22 to 44 mg/kg bw) peak levels of 0.07 to 0.12 µg/ml
were reached in milk at 24 hours, but were below the limit of
detection at 48 hours (Blobel & Burch, 1960).
2.1.1.6 Pigs
Three cross-bred barrows weighing approximately 100 kg each were
injected intramuscularly with uniformly tritiated dihydrostreptomycin
(specific activity 262 mCi/mmol) plus carrier drug at a single dose of
25 mg/kg bw/day, given as three separate injections. Plasma and urine
were sampled up to 5 days after the injection. The maximal
concentrations in plasma and urine were approximately 90 and 7100
µg/ml, respectively, and were achieved 1-2 hours after injection. Low
drug concentrations (approximately 3 µg/ml) were still detectable in
urine at 86 hours after injection. The apparent volume of distribution
was 21%, corresponding to the extracellular fluid. The absorption and
excretion rates were similar when assayed microbiologically with
Staphylococcus aureus (Stalheim, 1970).
The results of the foregoing studies are summarized in Table 1.
2.1.1.7 Humans
As a class, aminoglycoside antibiotics cross membranes very
poorly and only about 1% of an oral dose is absorbed, even when there
is intestinal inflammation or ulceration (Pratt & Fekaty, 1986).
Dollery (1991) reported that after oral administration of
streptomycin, 60%-100% of the drug can be recovered unchanged from the
faeces.
Table 1. Pharmacokinetics parameters for dihydrostreptomycin after intramuscular administration to various species
(Values represent ± standard deviation or range)
Species Dose (i.m.) Cmax (plasma) Tmax hours AUC mcg/ Cmax urine t´ hours Vd Reference
(mg/kg bw) (µg/ml) (ml/hour) (µg/ml)
Cats 10 25.1 ± 8.6 1.2 ± 0.4 61.4 ± 15.1 - 1.4 ± 0.1 - Rudd & Silley, 1987d
Dogs 10 41.2 ± 8.07 0.8 ± 0.26 74.1 ± 8.50 - 1.0 ± 0.17 - Rudd & Silley, 1987c
Sheep 10 44.8 ± 14.3 0.8 ± 0.3 151.5 ± 35.9 - 2.3 ± 0.3 - Rudd & Silley, 1987b
Cattle 10 44.3 ± 15.2 1.1 ± 0.4 207.2 ± 33.8 - 4.9 ± 0.5 - Rudd & Silley, 1987a
Cattle 11 44.7 (8.5-100) 1 - 2 - - - - Hammond, 1953
Cattle 16.5 65.0 (40.0-122) 1 - 2 - - - - Hammond, 1953
Cattle 25 78 3 - 4 - 1875 - 23% Stalheim, 1970
Pigs 25 87 1 - 2 - 7120 - 21% Stalheim, 1970
The aminoglycosides are reported to have a volume of distribution
of 25% of lean body mass in adults, corresponding to the extracellular
fluid volume. The volume of distribution in neonates may average 60%
of body weight. The volume of distribution in obese individuals is
less than in those with normal body weight. The volume of distribution
also varies with edema, which tends to reduce serum concentrations,
and dehydration which increases serum concentrations. The presence of
fever reduces serum concentrations by up to 40%, due to increased
renal blood flow and glomerular filtration.
Aminoglycosides accumulate in the kidney relative to plasma
levels, and detectable concentrations of aminoglycosides persist in
urine for several weeks, suggesting binding of the drug to kidney.
Accumulation also occurs in the perilymph of the inner ear, where the
elimination half-life is much longer than in serum (10-12 hours in
perilymph compared to 2 hours in serum).
Aminoglycoside levels in interstitial fluid approximate serum
levels. In bile, 25-50% of serum levels are obtained in the absence of
biliary obstruction. In sputum and bronchial secretions 25-67% of
serum levels may be achieved; in pericardial, pleural and ascitic
fluids approximately 50% of serum levels are obtained; and synovial
fluid may contain 50-100% of serum levels. Penetration into the eye,
cerebrospinal fluid and ventricular fluid is very poor. Placental
transfer occurs and fetal serum concentrations range from 20-40% of
maternal serum levels (Pratt & Fekaty, 1986).
Approximately 20% of a parenteral dose of streptomycin cannot be
accounted for in urine, but no metabolites have yet been identified.
Approximately 1% is excreted in bile (Dollery, 1991).
The excretion rate after parenteral administration of
amino-glycosides is dependent on renal function and is linearly
related to the creatinine clearance rate. The elimination half-life in
adults is 2 hours, but 5-6 hours in neonates due to their lower
glomerular filtration rate (Pratt & Fekaty, 1986).
2.1.2 Biotransformation
The aminoglycosides are reported not to be metabolized in humans
and are excreted in their active forms by glomerular filtration (Pratt
& Fekaty, 1986).
2.1.3 Effects on enzymes and other biochemical parameters
No information available
2.2 Toxicological studies
2.2.1 Acute toxicity studies
2.2.1.1 Mice
The oral LD50 of different dihydrostreptomycin salts was compared
in male Carworth CF1 mice weighing 20 g on average.
Dihydrostreptomycin hydrochloride gave an LD50 of 12 500 mg/kg bw,
whereas the sulfate salt gave an LD50 of greater than 30 000 mg/kg bw
(Edison et al., 1951).
2.2.1.2 Chickens
The LD50 for dihydrostreptomycin sulfate administered
intramuscularly to groups of fifty 1, 2, 3, or 4 week-old chicks was
743, 1090, 1738, and 1868 mg/kg bw, respectively. Clinical signs of
toxicity in all birds were depression, drooping wings, closed eyes,
muscular weakness and slowed respiration (Huebner et al., 1956).
Dihydrostreptomycin sulfate was administered intramuscularly to
groups of 3 white Leghorn chickens weighing 600 g, at doses of 800 to
2500 mg/kg bw. Clinical signs of toxicity included ataxia,
prostration, gasping, and coma. The LD50 was 2167 mg/kg bw (Gray &
Purmalis, 1958).
2.2.1.3 Pigeons
Dihydrostreptomycin sulfate was administered intramuscularly at
doses of 400 to 1000 mg/kg bw to groups of 5 racing pigeons weighing
an average of 360 g. Clinical signs of toxicity included emesis,
somnolence, ataxia, depression, and coma. The LD50 was determined as
715 mg/kg bw (Gray & Purmalis, 1958).
2.2.1.4 Gerbils
A group of 10 gerbils (5/sex), 7-10 weeks of age and weighing
55-65 g were given single intramuscular injections of 50 mg
dihydrostreptomycin sulfate (equivalent to 769-909 mg/kg bw).
Ascending flaccid paralysis was observed in 10/10 animals at 2 to 5
minutes after injection, and 8/10 animals died within 4 to 25 minutes
after injection. The 2 surviving animals gradually regained muscle
control and awareness with apparently complete recovery at 65 and 120
minutes post-injection, respectively (Wightman et al., 1980).
The results of acute toxicity studies on dihydrostreptomycin are
summarized in Table 2.
Table 2. Acute toxicity of dihydrostreptomycin
Species Number Route LD50 mg/kg bw Reference
(age/weight) (salt)
Mice - oral >30 000 Edison et al., 1951
(20g) (sulfate)
12 500
(hydrochloride)
Chickens 50/group i.m. 743 - 1868 Huebner et al., 1956
(1-4 weeks) (sulfate)
Chickens 3/group i.m. 2167 Gray & Purmalis,
(600g) (sulfate) 1958
Pigeons 5/group i.m. 715 Gray & Purmalis,
(360g) (sulfate) 1958
Gerbil 10 i.m. < 769 Wightman et al., 1980
(7-10 weeks,
55-65g)
2.2.2 Short-term toxicity studies
2.2.2.1 Guinea-pigs
Three groups of 30 young adult guinea-pigs (15/sex/group) were
treated for 90 days with either 40 mg dihydrostreptomycin/kg bw/day in
distilled water by gavage, an equal volume of distilled water alone by
gavage (negative control), or 200 mg kanamycin/kg bw/day, s.c.
(positive control).
The kanamycin-treated animals exhibited spastic twitching
immediately after dosing, injection site reactions and some animals
became ataxic. Body-weight gain was depressed in the kanamycin group,
but was comparable to controls in the dihydrostreptomycin group.
Auditory function was assessed using the pinna twitch reflex
(Preyer reflex) in response to a whistle. Hearing loss was observed in
all the animals in the kanamycin group after week 6, and in two
negative control animals after weeks 7 to 9, which were later found to
be suffering from an inner ear infection. No hearing loss was observed
in the dihydrostreptomycin treated animals.
A large number of animals died during the study (7 negative
controls, 6 positive controls, and 6 treated with
dihydrostreptomycin). These were necropsied, as were all surviving
animals at the end of the study. All tissues with observed gross
lesions, plus the organ of Corti from all animals, were examined
histologically.
Of the animals treated by gavage, several animals died of a
ruptured oesophagus (3 negative controls and 3 in the
dihydrostreptomycin group). Almost all of the remaining animals dying
on test had lesions of the lungs due to pneumonia.
The authors reported that because the organs of Corti were
inadequately preserved they showed signs of degeneration,
histologically. However, the architecture of the cell layers and the
hair cells were still discernible. The positive control animals
(kanamycin group) demonstrated either no hair cells at any level of
the cochlea, or very few and damaged hair cells. The majority of
dihydrostreptomycin-treated animals had hair cells with largely normal
architecture, although hair cell damage was noted as being more severe
in males than females treated with dihydrostreptomycin (Tisdel &
Harris, 1976).
2.2.2.2 Cats
Dihydrostreptomycin was administered orally in a food vehicle
(liver cat food) to 3 groups of 10 cats (5/sex/group) weighing between
1.5 and 4.6 kg, for 90 days at doses of 1, 5 or 10 mg/kg bw/day. Ten
cats of each sex were used as controls.
One male cat in the mid-dose group died during the ninth week of
treatment. A watery red urethral discharge and a distended bladder
were observed in this animal the day prior to death, and pathological
examination revealed acute cystitis with concomitant peritonitis. All
other cats survived the 90 days of treatment and no compound-related
effects were observed on body-weight gain, food consumption,
haematology, blood chemistry, urinalysis, gross pathology or
histopathology (only liver and kidneys of controls and 10 mg/kg/day-
treated cats were examined) (Wazeter, 1970a).
Vestibular function was assessed in 10 cats (5/sex) treated daily
with oral doses of 40 mg dihydrostreptomycin/kg bw/day for 90 days.
Streptomycin sulfate was used as the positive control (200 mg/kg
bw/day, s.c.). Animals in the negative control group were
administered water by gavage.
Three cats died, one in each of the negative control, positive
control, and dihydrostreptomycin groups, due to urinary obstruction
which was considered unrelated to treatment.
For the dihydrostreptomycin group, no treatment-related effects
were observed on body weight, haematology, blood chemistry,
ophthalmoscopic examination, bone marrow smears, or gross pathology.
Vestibular function remained normal throughout the treatment period
based on results of righting reflex tests in which animals were
dropped from an inverted position two feet above a cushioned mat. The
NOEL was 40 mg/kg bw/day dihydrostreptomycin in this study. The
results with streptomycin are described in section 2.2.2.5 of the
monograph on streptomycin (Tisdel et al., 1976).
2.2.2.3 Sheep
A target animal safety study was conducted with
dihydro-streptomycin in 3 groups of 4 sheep (2/sex/group) aged 13 to
16 months and weighing approximately 45 kg to 70 kg. Animals were
treated with daily intramuscular injections of 10 mg procaine
penicillin G plus 10 mg dihydrostreptomycin/kg bw/day for 5
consecutive days (the recommended therapeutic treatment regime), the
second group received 30 mg of each drug/kg bw/day for 5 days, and the
third group received 10 mg of each drug/kg bw/day for 15 days. A
treatment-free control group was not included, although pre-treatment
parameters were measured in each animal.
Behaviour was normal and there were no clinical signs of
neuromuscular blockade. No localized injection site reactions were
observed. Pathological changes observed in skeletal muscle and liver
at post-mortem examination were largely due to parasitic infestations.
Slight congestion/consolidation was observed in the lungs at necropsy,
which was not examined further. There was no evidence of ototoxicity
based on results of a crude hearing test and normal histology of the
VIIIth cranial nerve. There was no pathological evidence of
nephrotoxicity at post-mortem examination. Urinalyses were not
performed.
Some haematological and biochemical parameters were altered
during and after treatment. Differences reached statistical
significance in some groups compared with pre-treatment values,
whereas other parameters were altered then subsequently recovered to
pre-treatment values. The haematological changes included a reduction
in haemoglobin, red cells, haematocrit and mean cell volume.
Biochemical changes included a decrease in sodium, phosphorus,
creatinine, and bilirubin, and an increase in chloride. The only
consistent dose-related trends were decreased sodium and increased
chloride levels during prolonged treatment (15-day group), and a lower
haematocrit in all treatment groups. These changes, although
statistically significant were small and were considered by the
authors not to be clinically relevant (Brooks & Rolph, 1989b).
2.2.2.4 Pigs
A target animal safety study was conducted with
dihydrostreptomycin in 3 groups of 4 pigs (2/sex/group in groups 2 and
3, 1 female and 3 males in group 1) approximately 8 weeks of age and
weighing between 23 and 29 kg. Animals were treated with daily i.m.
injections of 10 mg procaine penicillin G plus 10 mg
dihydrostreptomycin/kg initial bw/day for 5 consecutive days (the
recommended therapeutic treatment regime, group 1), the second group
received 30 mg of each drug/kg initial bw/day for 5 days (group 2),
and the third group received 10 mg of each drug/kg initial bw/day for
15 days (group 3). An untreated control group was not included,
although pre-treatment parameters were measured in all animals.
Body weights increased rapidly in all groups (in group 3 body
weights had increased by 50% after 15 days). Therefore the dose
administered on a body-weight basis was reduced with time,
particularly in group 3. A crude hearing test revealed no auditory
impairment, and behaviour was normal, except for 2 animals in group 3
that showed symptoms that were attributed to stress (vomiting,
inactivity, haematemesis and slight cyanosis of ears and legs) on days
1 and 15, respectively.
Changes were observed compared with pretreatment values in
haematology and serum chemistry values (reduced haemoglobin, red cells
and haematocrit, reduced neutrophils, increased mean corpuscular
haemoglobin, decreased creatinine, and increased calcium), some of
which reached statistical significance. However, there were no obvious
drug-related or time-related trends, and although statistically
significant, the changes were small and were considered by the authors
not to be clinically relevant.
The VIIIth cranial nerve was histologically normal in all but one
animal in group 1 in which focal chronic inflammation was observed.
Focal interstitial nephritis was observed in one pig in group 1 and
two pigs in group 2. These effects were not considered by the authors
to be treatment-related. No local injection site reactions were
observed (Brooks et al., 1989).
2.2.2.5 Cattle
A target animal safety study was conducted with
dihydrostreptomycin in 3 groups of 4 cattle (2/sex/group),
approximately 6 months of age and weighing between 100 and 170 kg.
Animals were treated with daily i.m. injections of 10 mg procaine
penicillin G plus 10 mg dihydrostreptomycin/kg bw/day for 5
consecutive days (the recommended therapeutic treatment regime), the
second group received 30 mg of each drug/kg bw/day for 5 days, and the
third group received 10 mg of each drug/kg bw/day for 15 days. An
untreated control group was not included, although pre-treatment
parameters were measured in each animal.
No consistent treatment-related effects on haematological or
biochemical parameters were observed. Behaviour was normal and there
were no clinical signs of neuromuscular blockade. The few injection
site reactions that were observed were minor in nature. The only
pathological changes present in tissues and organs at post-mortem
examination were in the lungs, which were attributed to respiratory
tract infection. There was no evidence of ototoxicity based on results
of a crude hearing test and normal histology of the VIIIth cranial
nerve. There was no histological evidence of nephrotoxicity at
post-mortem examination. Urinalyses were not performed (Brooks &
Rolph, 1989a).
2.2.3 Long-term toxicity/carcinogenicity studies
2.2.3.1 Rats
Dihydrostreptomycin was administered in the diet to Charles River
CD rats, (35/sex/group), to achieve dosages of approximately 1, 5, or
10 mg/kg bw/day for up to 2 years (dietary concentrations were
adjusted weekly to compensate for changes in food consumption and body
weight). Two control groups were included in the study. Five
rat/sex/group were scheduled for interim kills at 6 and 12 months. The
remaining 25 animals/sex/group were administered dihydro-streptomycin
for 2 years. Interim study reports were submitted at 6 and 18 months,
and a final report at 2 years.
In the 6-month interim report, it was reported that 2 rats died
in the low-dose group during the first week of treatment (cause of
death unknown), and were replaced. One male control rat died after its
6-month blood sample was taken. There were no treatment-related
effects observed on food consumption, haematology or urinalysis
(analyses from 5 rats/ sex/group at 3 and 6 months), hearing or
vestibular function (measured in all rats at 3 and 6 months). Serum
chemistry was not evaluated in this study. Body weights were slightly
decreased in males in all treatment groups compared with controls,
which reached statistical significance for all groups; however, no
clear dose-response relationship was established. One male rat in the
5 mg/kg bw/day group had a grossly abnormal posture from the seventh
treatment onwards, and was found to have severe bilateral suppurative
otitis media when necropsied at 6 months. One to two rats in all
treated groups, but no controls, were also reported to have this
condition at the 6 month necropsy when 5 animals per sex/group were
killed. No other treatment-related effects were noted on gross
pathology or histopathology. Histological examination of the auditory
system or associated nerves was not performed (Wazeter, 1970b).
In the 18-month interim report, the body weights of male rats in
the high-dose group were significantly reduced when compared to
control group 1 but not control group 2. Body weights in all other
male treatment groups were comparable to controls. No
treatment-related effects were observed on food consumption,
haematology, or urinalysis. No effects were reported on hearing or
vestibular function as defined by the tests used. One female rat in
the high-dose group had an abnormal posture and occasional slowed
righting reflex from week 73 onwards, and two males in the mid-dose
group had "impaired use of the hindquarters" from week 64 onwards, one
of which subsequently died in week 69. Mortality rates were similar
for all treatment and control groups at 78 weeks, ranging from 0 to 4
deaths per group of 25 animals. None of the deaths were considered by
the author to be treatment-related. Causes of death were reported as
due primarily to spontaneous neoplasias (usually of the pituitary or
mammary glands) and infectious processes; however, no gross pathology
or histopathology data were provided with the report (Wazeter, 1971).
In the two-year report, 12 to 17 out of 25 rats/sex in treated
groups had survived up to two years. No treatment-related effects were
observed on survival, food consumption, urinalysis, haematology, or
hearing. Body-weight gain was reduced in males in the high-dose group
compared to control group 2, but not control group 1. Body weights
were comparable to controls in all other groups. Vestibular function
was impaired in both control and treated groups (inability to remain
on a bar or abnormal gait was observed in 5 control rats, 2 rats each
in the low- and mid-dose groups, and 3 rats in the high-dose group, no
sex differences were observed). On necropsy, 2 rats in the high-dose
group had gross lesions of the middle ear (purulent otitis media). All
other gross pathological changes and histopathological changes
(examined in controls and high-dose group only) occurred with similar
frequency in all rats examined at two years. Neoplasms were observed
with comparable frequency in both treatment and control groups and
were similar to the historical control incidence for this facility.
Although this study did not meet current standards regarding the
number of animals started on the two-year phase of the study
(25/sex/group), the Committee concluded that survival of more than 50%
of all treated animals in the 2-year phase of the study (24/50, 33/50,
and 29/50 in the low-, mid-, and high-dose groups, respectively),
represented an adequate test of the carcinogenic potential of the
compound. The NOEL was 5 mg/kg bw/day based on decreased body-weight
gain in males at the high dose (Wazeter & Goldenthal, 1972).
2.2.4 Reproductive toxicity studies
No information available
2.2.5 Special studies on embryotoxicity/teratogenicity
2.2.5.1 Guinea-pigs
Streptomycin and dihydrostreptomycin were administered by daily
i.m. injection to groups of 2 to 4 pregnant guinea-pigs at doses of
10, 25, 50, 100 or 200 mg/kg bw/day. The duration of the treatment
period was not stated. A dose of 100-200 mg/kg bw/day of both drugs
caused abortion or death within 8-10 days. All fetusus were macerated,
indicating that death occurred prior to abortion or death of dams. At
doses of 25-50 mg/kg bw/day, some animals aborted, some survived, and
some stillbirths were observed. A dose of 10 mg/kg bw/day for 24 days
caused no abortions. The surviving F1 animals were clinically normal
with respect to vestibular and auditory function, and the CNS was
normal on histological examination. The placentae from streptomycin-
or dihydrostreptomycin-treated animals showed marked hyperaemia,
haemorrhage, and endometrial necrosis 24 hours after a single
intramuscular dose of 100 mg/kg bw. These changes progressed with
further treatment. Serum concentrations of dihydrostreptomycin and
streptomycin measured in the fetus were 2-4% of those in the dams
(Riskaer et al., 1952).
2.2.5.2 Rabbits
Groups of 31, 23, and 26 pregnant female Dutch rabbits, weighing
approximately 2 to 4 kg, were treated by oral intubation with 0, 5, or
10 mg dihydrostreptomycin/kg bw/day, respectively, from days 6 to 18
of gestation. The vehicle control group received 0.5% aqueous
methylcellulose.
One rabbit in the 5 mg/kg bw/day group was found dead on
gestation day 10. Four control rabbits and 1 in the 10 mg/kg bw/day
treatment group aborted, all after gestation day 14. No
treatment-related effects were observed on maternal behaviour,
appearance, or body-weight gain. On day 30, all animals were killed
for pathological examination. There were no treatment-related effects
on the pregnancy rate, number of corpora lutea, number of viable
fetuses, percentage of abnormal fetuses, litter size, mean fetal body
weight, or 24-hour survival rate. The number of abortions and
resorptions/empty implantation sites were higher in controls compared
to treated groups. Presence of a 13th rib was a frequently noted fetal
abnormality; however the incidence was similar in all groups. One
control fetus was acephalic with a ventral hernia, and one fetus in
the 5 mg/kg bw/day group had agenesis of skin and soft tissue over the
left lateral nasal and buccal area, and absent hind claws. All of
these findings were considered by the authors as unrelated to
treatment.
Because no maternal toxicity was observed, the Committee
concluded that the dose levels may not have been high enough to fully
exclude teratogenic potential (Wazeter, 1970c).
2.2.5.3 Humans
Auditory toxicity has been reported in children whose mothers
were treated with streptomycin and dihydrostreptomycin during
pregnancy. However, details of the dose administered and the timing
in relation to the pregnancy are often not stated (Davies, 1991;
Robinson & Cambon, 1964; Snider et al., 1980; Varpela et al.,
1969; Warkany, 1979).
Organogenesis of the inner ear occurs at week 7 of pregnancy, and
cochlear development continues up to mid-term (Varpela et al.,
1969). It is the only organ in the body to reach full adult size and
complete differentiation by midterm (Robinson & Cambon, 1964).
However, unlike teratogens, the toxic effects of streptomycin and
dihydrostreptomycin on the fetus are independent of the critical
periods of embryogenesis. Ototoxicity can occur throughout the
gestation period (Snider et al., 1980), as well as in adults (see
effects in humans, section 2.3.1 below). In children of streptomycin-
and dihydrostreptomycin-treated mothers, as well as in adults,
high-tone hearing is primarily affected first, which is outside of the
range of normal speech frequencies (Donald & Sellars, 1981).
The results of a literature review of pregnancy outcomes in women
receiving streptomycin or dihydrostreptomycin for tuberculosis is
presented by Snider et al., 1980. Of a total of 203 women, 206
pregnancies were followed to term. Seventy-two women received
streptomycin or dihydrostreptomycin during the first 4 months of
pregnancy, 73 women received one or the other after the fourth month,
and the timing was unknown for 61 women. The dose of streptomycin or
dihydrostreptomycin administered in these cases, where stated, was
between 1 g to 2 g daily or twice weekly, with total doses ranging
from 2 g to 202 g. Several other drugs were administered concomitantly
for tuberculosis, i.e. 88 women also received isoniazid, 1 received
rifampicin, 1 received ethambutol, 83 received p-amino-salicylic acid,
and for 59 women the other drug was not known. There were 2
spontaneous abortions, no premature births and no stillbirths, and 170
normal term infants were delivered. Abnormalities were observed in 35
infants (a rate of 169 per 1000, roughly 1 in 6, is reported by the
authors). The majority of these consisted of vestibular dysfunction
and varying degrees of hearing loss. Hearing loss occurred in the
high-tone range first, i.e. before the range of normal speech
frequencies was affected. No other abnormalities were reported (Snider
et al., 1980).
2.2.6 Special studies on genotoxicity
Streptomycin and dihydrostreptomycin bind to and alter the
configuration of the 30S subunit of ribosomes, thus inhibiting protein
synthesis and causing misreading of the genetic code. RNA and DNA
synthesis are unaffected (Goldberg, 1965; Davies et al., 1964).
The results of genotoxicity assays with dihydrostreptomycin are
summarized in Table 3.
Table 3. Results of genotoxicity assays on dihydrostreptomycin
Test system Test object Concentration Results Reference
In vitro
Cytogenetics Human lymphocytes 4.7-13.7 mg/ml Negative Obe, 1970
2.2.7 Special studies on immune responses
The incidence of allergic reactions in humans to systemically
administered aminoglycosides is reported to be very low (Pratt &
Fekaty, 1986).
2.2.8 Special studies on ototoxicity
2.2.8.1 Cats
The ototoxicity of streptomycin and dihydrostreptomycin was
investigated in cats after they had recovered from surgical
destruction of one ear. Seven cats were treated with streptomycin at
doses and treatment periods ranging from 200 mg/kg bw/day for 9.5 days
to 25 mg/kg bw/day for 84 days. Six cats were treated with
dihydrostreptomycin at doses and treatment periods ranging from 300
mg/kg bw/day for 21 days to 100 mg/kg bw/day for 60 days. After the
last dose, animals were kept treatment-free for 1 year then necropsied
for histopathological examination of the inner ear and the brain stem
nuclei.
Clinical signs of ototoxicity were similar in both groups, which
included permanent high frequency hearing loss, loss of
post-rotational nystagmus, and ataxia. Weight loss was also noted as
a treatment-related effect in both groups. With dihydrostreptomycin
treatment, the hearing loss was delayed and occurred several weeks to
several months after treatment.
In the inner ear, loss of hair cells in the cochlea, and damage
to the sensorimotor epithelium and hair loss in the cristae of the
vestibular canals were observed. The cristae appeared to be more
susceptable to toxic effects than the maculae of the saccule and
utricle.
In the brain stem, no lesions were found in the vestibular
nuclei. The vestibular portion of the VIIIth nerve was normal,
despite the fact that the sensorimotor epithelium and supporting cells
of the vestibular apparatus had been destroyed (surgically on one
side, and due to streptomycin and dihydrostreptomycin treatment on the
other side).
Effects observed in the brain stem included degenerative changes
in the ventral and dorsal cochlear nuclei, occurring primarily in
those parts corresponding to the ear which had been surgically
destroyed. In 2 animals treated with streptomycin, these lesions were
observed on the side corresponding to the ear which had not been
destroyed surgically. In these 2 animals, degeneration of the spiral
ganglion was also observed.
The authors described these degenerative changes as being typical
of trans-synaptic atrophy. The nuclei were smaller, containing smaller
nerve cells arranged more compactly, and changes were observed in the
myeloarchitecture. The cochlear branch of the VIIIth nerve appeared
shrunken with only a few myelinated fibres. There were no lesions in
the cerebellum or any other part of the brain stem.
The authors concluded that the lesions produced by both
streptomycin and dihydrostreptomycin were limited to the vestibular
end-organ of the inner ear in cats (McGee & Olszewski, 1962).
Dihydrostreptomycin was administered subcutaneously to groups of
2 cats at a dose of 800 mg/kg bw/day for 15 days or 200 mg/kg bw/day
for 120 days. Moderate to severe ataxia was observed from days 8 and
10 in the 800 mg/kg bw/day group, and from days 28 and 78 in the 200
mg/kg bw/day group. Animals were necropsied at the end of the
treatment period and the inner ear examined. Scattered degeneration of
the hair cells was observed in the cristae of the horizontal
semicircular canals, and was more severe in the high-dose group. The
cochlea of dihydrostreptomycin-treated cats was comparable to controls
as judged by electrophysiological studies of voltage changes at the
round window in response to tones of varying frequencies. The authors
reported that streptomycin produced more severe vestibular and
cochlear changes in a previous study than those produced by
dihydrostreptomycin; however, the doses of streptomycin used were not
stated. The authors also reported that cochlea of the cat appears to
be more sensitive to streptomycin than dihydrostreptomycin, whereas
the opposite is true in humans (Hawkins & Lurie, 1953).
2.2.9 Special studies on microbiological effects
2.2.9.1 Hamsters
Groups of 6 hamsters were fed a diet containing 0 or 10 mg/kg
dihydrostreptomycin. After 47 days, oxytetracycline (10 mg/kg) was
added to the diet and a suspension of E. coli (106 organisms/ml)
susceptible to both drugs was added to the drinking-water for two
weeks. Faecal samples were collected throughout the study and analyzed
for lactose-fermenting enteric organisms resistant to either
dihydrostreptomycin or oxytetracycline. No dihydrostreptomycin- or
oxytetracycline-resistant organisms were detected in the faeces at any
time (Rollins et al., 1975).
2.2.9.2 Dogs
Groups of 5 beagle dogs with an average weight of 15 kg were fed
a diet containing 0, 2, or 10 mg dihydrostreptomycin per kg of feed
(equivalent to 50 or 250 µg/kg bw/day) for 35 days. In both treatment
groups there was a shift in the faecal flora from predominantly
dihydrostreptomycin-susceptible lactose fermenting coliforms to a
resistant population after 15 days, which was significant (p < 0.01)
in both groups. This persisted throughout the 28-day post-treatment
phase of the study. A definitive response was not seen in the control
group. The authors concluded that the NOEL for development of drug
resistance in enteric bacteria was less than 2 mg/ kg of diet,
equivalent to 50 µg/kg bw/day (Gaines et al., 1978).
2.2.9.3 Humans
Healthy human volunteers were treated with 0.75 mg of
dihydrostreptomycin administered orally in a hamburger patty, 4 days
per week, for 7 weeks. Faecal samples were examined weekly for the
presence of coliforms bearing R-factor mediated resistance to
dihydrostreptomycin. The presence of resistant coliforms fluctuated
from week to week in about 30% of untreated controls. Fluctuations
were also observed in treated subjects. Four of 25 treated subjects
and 6/29 controls never excreted resistant coliforms; however, when
resistant coliforms were acquired, they tended to persist longer and
to multiply to greater numbers in the presence of dihydrostreptomycin
than in controls (Snyder et al., 1972).
2.2.9.4 Dairy starter cultures
Five strains each of various bacterial species were tested for
their sensitivity to dihydrostreptomycin by measuring zones of
inhibition of bacterial growth around discs impregnated with 2 or 10
µg/disc. The bacteria used were strains of Streptococcus (S.
lactis, S. cremoris, S. diacetilactis, S. thermophilus, S. durans, S.
faecalis) Lactobacillus bulgaricus, Brevibacterium linens,
Leuconostoc dextranicum, Staphylococcus (S. aureus, S. epidermidis),
and Micrococcus varians. All were susceptible except all
strains of Streptococcus faecalis and 3/5 strains of Streptococcus
durans (Reinbold & Reddy, 1974).
2.2.9.5 Minimum inhibitory concentrations in vitro
The minimum inhibitory concentration (MIC) of dihydrostreptomycin
sulfate was determined in vitro for bacteria isolated from the
intestines or faeces of healthy human adults. Over 100 isolates were
tested which represented 17 species and covered the 10 most common
genera of human intestinal microbes. The methods and controls used
were those proposed by the National Council for Clinical Laboratory
Standards (NCCLS) describing MIC assays for anaerobic bacteria.
E. coli was additionally assayed under aerobic conditions. The agar
dilution method was used, with Wilkins Chalgren agar or BHI agar
supplemented with 5% rabbit's blood, and incubations were for 48 hours
at 37 ± 2 °C. Dihydrostreptomycin was tested at serial double
dilutions from 128 µg/ml to 2 µg/ml. At each concentration, bacterial
cells were tested at two densities, 1 x 105 cells per spot, which is
recommended by NCCLS for clinical isolates, and 1 x 107 cells per
spot, which is considered to be more representative of the bacterial
concentration within the intestinal ecosystem. The results of this
study are summarized in Table 4.
Bifidobacterium spp. were found to be the most sensitive. Data
available for 5 strains of Bifidobacterium adolescentis gave an
MIC50 value of 32 µg/ml and a MIC range of 16-64 µg/ml, and data on
5 strains of Bifidobacterium longum gave an MIC50 value of 16 µg/ml
and a MIC range of 8-32 µg/ml.
The MIC50 value for dihydrostreptomycin in most of the other
bacterial species tested (17 bacterial species, with 5-11 strains
tested per species) was higher than 32 µg/ml, with the highest MIC50
values being more than 128 µg/ml.
An MIC50 value of 32 µg/ml was therefore established as the
concentration without effect on the human gut flora (Carman, 1994).
Table 4. MIC values for bacterial isolates from human intestinal material
(All values represent mcg/ml)
Species 1 x 107 cells / spot 1 x 105 cells / spot
n = no. of strains MIC50 MIC90 Range MIC50 MIC90 Range
E. coli 16 64 8-64 16 32 8-64
(aerobic) n=11
E. coli 64 128 32->128 32 64 16-128
(anaerobic) n=11
Bacteroides vulgatus >128 >128 128-128 >128 >128 64->128
n=5
Bacteroides uniformis >128 >128 >128 >128 >128 >128
n=5
Bifidobacterium 32 64 16-64 32 32 8-32
adolescentis
n=5
Bifidobacterium 16 32 8-32 16 16 8-32
longum n=5
Lactobacillus >128 >128 64->128 128 >128 32->128
acidophilus n=10
Fusobacterium >128 >128 128->128 >128 >128 128->128
russi n=5
Fusobacterium >128 >128 128->128 >128 >128 64->128
prauznitii n=5
Peptostreptococcus >128 >128 64->128 >128 >128 64->128
DZ n=5
Peptostreptococcus >128 >128 128->128 >128 >128 128->128
productus 1 n=5
Ruminococcus 64 64 64 64 64 32-64
gnavus n=5
Ruminococcus 64 64 64-128 64 64 64
bromii n=5
Table 4 (contd)
Species 1 x 107 cells / spot 1 x 105 cells / spot
n = no. of strains MIC50 MIC90 Range MIC50 MIC90 Range
Eubacterium >128 >128 128->128 >128 >128 64->128
aerofaciens n=5
Eubacterium >128 >128 >128 >128 >128 128->128
rectale n=5
Coprococcus 64 64 64-128 32 64 32-64
eutactus n=5
Coprococcus 64 64 32-64 32 64 32-64
comes n=5
Gemmiger 64 128 64->128 64 128 32->128
formicilis n=10
2.3 Observations In humans
2.3.1 Ototoxicity
The aminoglycosides are all potentially toxic to the inner ear at
therapeutic doses. Streptomycin-induced ototoxicity primarily affects
the vestibular system before auditory function is affected, whereas
dihydrostreptomycin primarily affects the cochlea before vestibular
function is affected. With both streptomycin and dihydrostreptomycin
hearing loss occurs in the high tone range first, i.e. before the
range of frequencies associated with normal speech is affected
(Martindale, 1993; Davies, 1991; Shambaugh et al., 1959; Hawkins &
Lurie, 1953; Pratt & Fekaty, 1986).
The primary toxic effect of both streptomycin and
dihydrostreptomycin is on the peripheral sensory portions of the inner
ear rather than on the eighth cranial nerve itself, which results in
progressive destruction of the hair cells of the Organ of Corti from
the basal region (responsive to high-frequency sounds) to the apex of
the cochlea (responsive to low-frequency sounds) as dosage and
duration of treatment are increased (Davies, 1991).
Dihydrostreptomycin causes delayed ototoxicity in humans
manifested as a sensorineural hearing loss which may involve any or
all frequencies. Hearing loss may occur from 1 to 6 months after drug
treatment, it is permanent, and it is not related to the size of the
dose (McGee & Olszewski, 1962; Shambaugh et al., 1959).
Aminoglycosides, including streptomycin and dihydrostreptomycin,
accumulate in the perilymph of the inner ear (Davies, 1991). A large
proportion of both drugs are excreted unchanged by the kidneys (Pratt
& Fekaty, 1986), and the risk of ototoxicity is therefore increased
when renal function is compromised (Erlansen & Lundgren, 1964).
Patients presenting with ototoxic side effects after treatment
with streptomycin, dihydrostreptomycin or kanamycin, for various
clinical conditions, were studied in a retrospective study. The route
of administration was not stated, although it was probably
intramuscular injection.
Two patients receiving a 50:50 mixture of streptomycin and
dihydrostreptomycin at doses of 0.5 or 1.0 mg/kg bw/day of each drug
(total dose 5 or 14.5 g of each drug) reported vertigo at the end of
the course of treatment. Four patients receiving dihydro-streptomycin
at a dose of 1 g per day (equivalent to 14 to 20 mg/kg bw/day, total
dose 6 to 36 g) reported tinnitus or impaired hearing (as assessed by
tone audiometry) between 2 weeks and 3 months after the course of
treatment. None of the patients in this group reported vertigo. Three
of these patients had impairment of renal function which may have
increased blood levels of dihydrostreptomycin and hence increased the
risk of ototoxicity. It was not stated whether the renal impairment
was pre-existing or caused by dihydrostreptomycin treatment (Erlanson
& Lundgren, 1964).
Dihydrostreptomycin has been reported to be more likely to cause
partial or complete hearing loss than streptomycin and was therefore
not recommended for use in humans (Martindale, 1993).
2.3.2 Renal toxicity
Nephrotoxicity due to aminoglycosides usually presents in humans
as an acute tubular necrosis manifested as proteinuria, cylinduria and
inability to concentrate the urine. This is followed by a reduction in
glomerular filtration rate with a rise in serum creatinine and blood
urea nitrogen. Aminoglycosides bind to the luminal surface of the
proximal tubules, are internalized by pinocytosis and fuse with
lysosomes. It is postulated that they become sequestered in lysosomes
where they disrupt phospholipid metabolism (prominant myeloid bodies
have been observed in renal tubular cells exposed to gentamicin), and
renal cell death occurs consequent to changes in lysosomal
biochemistry (Pratt & Fekaty, 1986).
2.3.3 Neuromuscular blockade
Aminoglycosides can produce a non-depolarizing type of
neuromuscular blockade due to reduced acetylcholine release from motor
nerve endings and reduced sensitivity of the post-junctional endplate;
this effect is completely reversed by administration of calcium (Pratt
& Fekaty, 1986).
2.3.4 Allergic reactions
The incidence of allergic reactions to systemically administered
aminoglycosides is reported to be very low. The incidence of allergic
reactions to dihydrostreptomycin specifically was not reported (Pratt
& Fekaty 1986).
2.3.5 Other effects
Aminoglycosides have been reported to cause neutropenia,
agranulocytosis, and aplastic anaemia on rare occasions. Transient
elevation of hepatic enzymes occurs occasionally with
amino-glycosides. The incidence of specific effects associated with
dihydrostreptomycin were not reported (Pratt & Fekaty, 1986).
5. REFERENCES
ANDERSON, D.G. & JEWELL, M. (1945). The absorption, excretion and
toxicity of streptomycin in man. New Engl. J. Med., 233: 485-491.
BACHARACH, A.L., CLARK, B.J., McCULLOCH, M., & TOMICH, E.G. (1959).
Comparative toxicity studies on ten antibiotics in current use.
J. Pharm. & Pharmacol., 11: 737-741.
BEEK, B., GÖBEL, D., OBE, G., & RADENBACH K.L. (1974). Prospective
controlled clinical trial of antitubercular agents in triple
combinations for mutagenicity in leukocyte cultures (short report).
Prax. Pneumol., 28: 970.
BERG, K. (1951). The toxic effect of streptomycin on the vestibular
and cochlear apparatus: an experimental study on cats. Acta Otolaryn
(Stoch), suppl. 97: 1-77.
BLOBEL, H., & BURCH, C.W. (1960). Diffusion of dihydrostreptomycin and
chlortetracycline into milk of dairy cows following parenteral
administration. J. Amer. Vet. Med. Assoc., 137 698-700.
BOUCHER, D & DELOST, P. (1964). Developpement post-natal des
descendants issus de meres traités par la streptomycine au cours de la
gestation chez la souris. C.R. Soc, Biol. (Paris), 158: 2065-2069.
BRITISH PHARMACEUTICAL CODEX (1968). The Pharmaceutical Press, London.
BROOKS, C., & ROLPH, T.P. (1989a). The effect of streptopen injection
on the health of cattle. Unpublished report No. AnH89/R/65 from
Pitman-Moore Ltd., Uxbridge, Middlesex, England. Submitted to WHO by
Pitman-Moore, Inc., Mundelein, IL, USA.
BROOKS, C., & ROLPH, T.P. (1989b). The effect of streptopen injection
on the health of sheep. Unpublished report No. AnH89/R/66 from Pitman-
Moore Ltd., Uxbridge, Middlesex, England. Submitted to WHO by Pitman-
Moore, Inc., Mundelein, IL, USA.
BROOKS, C., EASTWOOD, B., & ROLPH, T.P. (1989). The effect of
streptopen injection on the health of pigs. Unpublished report No.
AnH89/R/75 from Pitman-Moore Ltd., Uxbridge, Middlesex, England.
Submitted to WHO by Pitman-Moore, Inc., Mundelein, IL, USA.
BYWATER, R.J. (1982). Aminoglycoside antibiotics. In: Brander, G.C.,
Pugh, D.M. & Bywater, R.J. (eds.), Veterinary Applied Pharmacology and
Therapeutics, 4th edition, Balliere Tindall, London, pp. 387-393.
CARMAN, R.J. (1994). Dihydrostreptomycin MIC determinations for human
gut flora. Unpublished report from TechLab Inc., VPI Research Park,
Blacksburg, Virginia 24060, USA. Submitted to WHO by Norbrook
Laboratories Ltd., Newry, Northern Ireland.
CHRISTENSEN, E., HERTZ, H., RISKAER, N. & VRA-JENSEN, G. (1951).
Histological investigations in chronic streptomycin poisoning in
guinea-pigs. Ann. Otol., 60: 343-349.
CLARK, C.H. (1977). Toxicity of aminoglycoside antibiotics. Modern
Veterinary Practice, Part 7, 58: 594-598.
DAS, B.C., & SHARMA, T. (1983). Reduced frequency of baseline sister
chromatid exchanges in lymphocytes grown in antibiotics- and serum-
excluded culture medium. Hum Gen., 64: 249-253.
DAVIES, D.M. (1991). Textbook of adverse drug reactions. Fourth
edition, Oxford University Press, London, p. 51.
DAVIES, J., GILBERT, W., & GORINI, L. (1964). Streptomycin suppression
and the code. Proc. Nat. Acad. Sci., 51: 883-890.
DESALVA, S.J., EVANS, R.A., & MARCUSSEN, H.W. (1969). Lethal effects
of antibiotics in hamsters. Toxicol. Appl. Pharmacol., 14: 510-514.
DOLLERY, C. (1991). Therapeutic Drugs, C. Dollery (ed.), Churchill
Livingston, London, pp. 100-103.
DONALD, P.R. & SELLARS, S.L. (1981). Streptomycin ototoxicity in the
unborn child. S. Afr. Med. J., 60: 316-318.
EDISON, A.O., KUNA, S., CUCHIE, F.T. & HANSON, J.T. (1951). Relative
absorption of salts of streptomycin and dihydrosreptomycin after oral
administration. Antibiotics & Chemotherapy, 1: 49-53.
ELIAS, W.F. & DURSO, J. (1945). Blood, urine and faecal levels of
streptomycin in the treatment of human infections of E. Typhosa.
Science, 101: 589-591.
ERICSON-STRANDVIK, B. & GYLLENSTEN L. (1963). The central nervous
system of fetal mice after administration of streptomycin. Acta
Pathol. Microbiol. Scand., 59: 292-300.
ERLANSON, P., & LUNDGREN, A. (1964). Ototoxic side effects following
treatment with streptomycin, dihydrostreptomycin and kanamycin. Acta
Medica Scandinavica, 176: fasc. 2.
GAINES, S.A., ROLLINS, L.D., SILVER, R.P, & WASHINGTON, M. (1978).
Effects of low concentrations of dihydrostreptomycin on drug
resistance in enteric bacteria. Antimicrobial agents and
chemotherapy, 14: 252-256.
GOLDBERG, I.H. (1965). Mode of action of antibiotics. II. Drugs
affecting nucleic acid and protein synthesis. Am. J. Med., 39: 722-
752.
GRAHAM, B.E., VANDER BROOK, N.J. & KUIZENGA, M.H. (1946). Preliminary
studies on the absorption and excretion of streptomycin in dogs.
Science, 103: 364-365.
GRAY, J.E. & PURMALIS A. (1958). The acute toxicity of procaine
penicillin G and of dihydrostreptomycin sulfate in the pigeon and the
chicken. Avian Disease, 2: 187-196.
HAMMOND P.B. (1953). Dihydrostreptomycin dose-serum level relationship
in cattle. J. Amer. Vet. Med. Assoc., 122: 203-206.
HAWKINS, J.E. & LURIE, M.H. (1953). The ototoxicty of
dihydrostreptomycin and neomycin in the cat. Ann. Otol., 62: 1128-
1148.
HUBER, W.G. (1966). Streptomycin. In: Veterinary Pharmacology and
Therapeutics, Leo Meyer Jones (ed), 3rd edition, Iowa State College
Press, pp. 519-530.
HUEBNER, R.A., GLASSMAN, J.M., HUDYMA, G.M. & SEIFTER, J. (1956). The
toxic dose of dihydrostreptomycin in fowl. Cornell Vet., 46: 219-
212.
JAJU, M., JAJU, M., & AHUJA, Y.R. (1983). Cytogenetic effects of
chemotherapy with three combinations of anti-tubercular drugs
involving isoniazid, thiacetazone, para-amino-salicylic acid and
streptomycin on human lymphocytes: chromosome aberrations, sister
chromatids exchanges and mitotic index. Hum. Gen., 64: 42-49.
KERN, G. (1962). Zur Frage der Intrauterine Streptomycin Schadigung.
Schweiz. Med. Wochenschr., 92: 77-79.
KODAMA, F., FUKUSHIMA, F., & UMEDA, M. (1980). Chromosome aberrations
induced by clinical medicines. J. Tox. Sci., 5: 141-150.
MARSHALL, E.K. (1948). The absorption, distribution and excretion of
streptomycin. J. Pharmacol. Exper. Therapeut., 92: 43-48.
MARTINDALE, (1993). The extra pharmacopoeia. Reynolds, J.E.F. (ed.),
30th Edition, Pharmaceutical Press, pp. 159-160.
MARYNOWSKI, A., & SIANOZECKA, E. (1972). Comparison of the incidence
of congenital malformations in neonates from healthy mothers and from
patients treated for tuberculosis. Ginekol. Pol., 43: 713-715.
McGEE, T.M., & OLSZEWSKI, J. (1962). Streptomycin sulphate and
dihydrostreptomycin toxicity. Arch. Otolaryngol., 75: 295-311.
MOLITOR, H., GRAESSLE, O.E., KUNA, S., MUSHETT, C.W., SILBER, R.H.
(1946). Some toxicological and pharmacological properties of
streptomycin. J. Pharm. Exp. Ther., 86: 151-173.
NAKAMOTO, Y., OTANI, H., & TANAKA, O. (1985). Effects of
aminoglycosides administered to pregnant mice on postnatal development
of inner ear in their offspring. Teratology, 32: 34B.
NEU, R., ASPILLAGA, M.J., & GARDNER, L.I. (1965). Effects of
antibiotics on chromosomes of cultured human leucocytes. Nature
(London), 205: 171-172.
NOMURA, T., KIMURA, S., KANZAKI, T., ET AL. (1984). Induction of
tumors and malformations in mice after prenatal treatment with some
antibiotic drugs. Med. J. Osaka Univ., 35: 13-17.
OBE, G. (1970). The effect of streptomycin and dihydrostreptomycin on
human chromosomes in vitro. Molec. Gen. Genetics, 107: 361-365.
PRATT, W.B., & FEKATY, R. (1986). Bactericidal inhibitors of protein
synthesis, the aminoglycosides. In: The antimicrobial drugs, Chapter
7, Oxford University Press, Oxford, pp. 153-183.
REINBOLD, G.W., & REDDY, M.S. (1974). Sensitivity or resistance (of)
dairy starter and associated micro-organisms to selected antibiotics.
J. Milk Food Technol., 37: pp. 517-521.
RISKAER, N., CHRISTENSEN, E. & HERTZ, H. (1952). The toxic effects of
streptomycin and dihydrostreptomycin in pregnncy, illustrated
experimentally. Acta Tuber. Pneumol. Scand., 27: 211-216.
ROBINSON, C.G. & CAMBON, K.G. (1964). Hearing loss in infants of
tuberculous mothers treated with streptomycin during pregnancy.
N. Engl. J. Med., 271: 949-951.
ROLLINS, L.D., GAINES, S.A., POCURULL, D.W., & MERCER, H.D. (1975).
Animal model for determining the no-effect level of an antimicrobial
drug on drug resistance in the lactose-fermenting enteric flora.
Antimicrobial Agents and Chemotherapy, 7: 661-665.
RUDD, A.P., & SILLEY, P. (1987a). Antibiotic concentrations in cattle
serum following a single intramuscular injection of Streptopen
injection. Unpublished report No. An.H.87/R/22 from Pitman-Moore Ltd.,
Uxbridge, Middlesex, England. Submitted to WHO by Pitman-Moore, Inc.,
Mundelein, IL, USA.
RUDD, A.P., & SILLEY, P. (1987b). Antibiotic concentrations in sheep
serum following a single intramuscular injection of Streptopen
injection. Unpublished report No. An.H.87/R/27 from Pitman-Moore Ltd.,
Uxbridge, Middlesex, England. Submitted to WHO by Pitman-Moore, Inc.,
Mundelein, IL, USA.
RUDD, A.P., & SILLEY, P. (1987c). Antibiotic concentrations in dog
serum following a single intramuscular injection of Streptopen
injection. Unpublished report No. An.H.87/R/34 from Pitman-Moore Ltd.,
Uxbridge, Middlesex, England. Submitted to WHO by Pitman-Moore, Inc.,
Mundelein, IL, USA.
RUDD, A.P., & SILLEY, P. (1987d). Antibiotic concentrations in cat
serum following a single intramuscular injection of Streptopen
injection. Unpublished report No. An.H.87/R/42 from Pitman-Moore Ltd.,
Uxbridge, Middlesex, England. Submitted to WHO by Pitman-Moore, Inc.,
Mundelein, IL, USA.
SHAMBAUGH, G.E., DERLACKI, E.L., HARRISON, W.H., HOUSE, H., HOUSE, W.,
HILDYARD, V., SCHUKNECHT, H., & SHEA, J.J. (1959). Dihydrostreptomycin
deafness. JAMA, 170: 1657-1660.
SNIDER, D.E., LAYDE, P.M., JOHNSON, M.W. & LYLE, M.A. (1980).
Treatment of tuberculosis during pregnancy. Am. Rev. Resp. Dis.,
122: 65-79.
SNYDER, M. J., AL-IBRAHIM, M., & HORNICK, R. B. (1972). The effect of
oral DHS on resistance development in the intestinal microflora of
man. Unpublished report from the Division of Infectious Diseases,
Department of Medicine, University of Maryland School of Medicine.
Submitted to WHO by FDA.
STALHEIM, O.H.V. (1970). Absorption and excretion of tritiated
dihydrostreptomycin in cattle and swine. American Journal of
Veterinary Research, 31: 497-499.
STEBBINS, R.B., GRAESSLE, O.E., & ROBINSON H.J. (1945). Studies on the
absorption and excretion of streptomycin in animals. Proc. Soc. Exp.
Biol. Med., 60: 68-72.
STEVENSON, L.D., ALVORD, E.C., & CORRELL, J. W. (1947). Degeneration
and necrosis of neurones in eighth cranial nuclei caused by
streptomycin. Proc. Soc. Exp. Biol. Med., 65: 86-88.
TISDEL, M., & HARRIS, D.L. (1976). Dihydrostreptomycin: 90-day
toxicity study in guinea pigs. Unpublished report, Warf Study Code T-
615 from Warf Institute, Inc., Madison, Wisconsin, USA, on behalf of
Animal Health Institute. Submitted to WHO by FDA.
TISDEL, M., HARRIS, D.L., HAARS, R., & NEES, P.O. (1976).
Dihydrostreptomycin: 90-day toxicity study in cats. Unpublished
report, Warf Study Code T-614 from Warf Institute, Inc., Madison,
Wisconsin, USA, on behalf of Animal Health Institute. Submitted to WHO
by FDA.
TSANG, Y.C., & CHIN, T.C. (1963). Neurotoxicity of streptomycin.
Scientia Sinica, 12: 1019-1040.
VARPELA, E., HIETALAHTI, J., & ARO, M.J.T. (1969). Streptomycin and
dihydrostreptomycin medication during pregnancy and their effect on
the child's inner ear. Scand. J. Resp. Dis., 50: 101-109.
WARKANY, J. (1979). Antituberculous drugs. Teratology, 20: 133-138.
WAZETER, F. X. (1970a). Dihydrostreptomycin: Ninety-day toxicity study
in cats. Unpublished report from International Research and
Development Corporation on behalf of Animal Health Institute.
Submitted to WHO by FDA.
WAZETER, F. X. (1970b). Dihydrostreptomycin: Two-year oral toxicity
study in rats (six month interim report). Unpublished report from
International Research and Development Corporation on behalf of Animal
Health Institute. Submitted to WHO by FDA.
WAZETER, F. X. (1970c). Dihydrostreptomycin: Rabbit teratogenic study.
Unpublished report from International Research and Development
Corporation on behalf of Animal Health Institute. Submitted to WHO by
FDA.
WAZETER, F. X. (1971). Dihydrostreptomycin: Two-year oral toxicity
study in rats (18 month interim report). Unpublished report from
International Research and Development Corporation on behalf of Animal
Health Institute. Submitted to WHO by FDA.
WAZETER, F. X., & GOLDENTHAL, E.I. (1972). Dihydrostreptomycin: Two-
year oral toxicity study in rats. Unpublished report from
International Research and Development Corporation on behalf of Animal
Health Institute. Submitted to WHO by FDA.
WIGHTMAN, S.R., MANN, P.C., & WAGNER, J.E. (1980). Dihydrostreptomycin
toxicity in the Mongolian gerbil, Meriones unguiculatus. Laboratory
Animal Science, 30: 71-75.
 Both dihydrostreptomycin and streptomycin are used for treatment
of bacterial infections in food-producing animals.
Dihydrostreptomycin is formed by reduction of streptomycin. As
a result, pharmacokinetic properties, toxicological profiles, and
spectrum of antimicrobial and biological activity of the two compounds
are similar. Therefore, data on the two compounds were considered
together for the purpose of establishing a single ADI. The Committee
noted that the two compounds are generally considered together in the
published literature and in the report of the twelfth meeting of the
Committee. Complete toxicological monographs were prepared for each
compound and are provided in their entirety below.
2. BIOLOGICAL DATA
2.1 Biochemical aspects
2.1.1 Absorption, distribution and excretion
2.1.1.1 Rats
The sulfate and calcium chloride complex salts of streptomycin,
and the sulfate and hydrochloride salts of dihydrostreptomycin, were
administered orally in solution to groups of 5 rats at a single dose
of 7.5 g of antibiotic base per kg bw. Heart blood was withdrawn at
0.5, 1, 2, 3, and 4 hours, and assayed microbiologically using
Staphylococcus aureus. Peak blood levels of all four compounds were
measured at 1-2 hours. Streptomycin calcium chloride complex and
dihydrostreptomycin hydrochloride were better absorbed (peak blood
levels of 3200 to 4300 µg/ml, respectively) compared to the two
sulfate salts of each compound (peak blood levels of 200-300 µg/ml).
The elimination half-lives and AUCs were not calculated for this study
(Edison et al., 1951).
2.1.1.2 Cats
Nine female cats aged 4 to 6 months and weighing approximately 2
to 3 kg were given single intramuscular injections of 10 mg/kg bw each
of penicillin G and dihydrostreptomycin. Serum levels of each drug
were assayed by microbiological agar diffusion methods up to 32 hours
after injection. Dihydrostreptomycin was assayed using Bacillus
pumilis, and penicillin was assayed using either Bacillus subtilis
or Bacillus stearothermophilus. One cat had detectable penicillin
levels in the pre-treatment sample (0.04 µg/ml). Another cat died
within two minutes of the six-hour blood sample, which was taken by
heart puncture. Death was considered to be caused by the blood
sampling method, and therefore was not treatment-related.
Peak plasma levels of approximately 25 µg/ml were reached at
approximately 1 hour. The plasma elimination half-life was
approximately 1 hour, and the AUC was 61.4 ± 15.1 µg/ml/hour.
Dihydrostreptomycin was below the limit of detection (0.6 µg/ml) in
all animals by 24 hours after injection (Rudd & Silley, 1987d).
2.1.1.3 Dogs
Ten dogs (six females, four males, aged 1.5 to 4 years and
weighing approximately 11 to 22 kg) were given single intramuscular
injections of 10 mg/kg bw each of penicillin G and
dihydrostreptomycin. Serum levels of each drug were assayed by
microbiological agar diffusion methods up to 72 hours after injection.
Dihydrostreptomycin was assayed using Bacillus pumilis, and
penicillin was assayed using either Bacillus subtilis or Bacillus
stearothermophilus.
Peak plasma levels of approximately 41 µg/ml were reached at
approximately 1 hour. The plasma elimination half-life was
approximately 1 hour, and the AUC was 74.1 ± 8.50 µg/ml/hour.
Dihydrostreptomycin was below the limit of detection (0.6 µg/ml) in
all animals by 8 hours after injection (Rudd & Silley, 1987c).
2.1.1.4 Sheep
Ten female sheep aged 15 to 18 months and weighing approximately
60 to 90 kg were given single intramuscular injections of 10 mg/kg bw
each of penicillin G and dihydrostreptomycin. Serum levels of each
drug were assayed by microbiological agar diffusion methods up to 72
hours after injection. Dihydrostreptomycin was assayed using Bacillus
pumilis, and penicillin was assayed using either Bacillus subtilis
or Bacillus stearothermophilus.
Peak plasma levels of approximately 45 µg/ml were reached at
approximately 1 hour. The plasma elimination half-life was
approximately 2 hours, and the AUC was 151.5 ± 35.9 µg/ml/hour.
Dihydrostreptomycin was below the limit of detection (0.3 µg/ml) in
all animals by 24 hours after injection (Rudd & Silley, 1987b).
2.1.1.5 Cattle
Ten cattle (one male, nine females, weighing approximately 200
to 450 kg) were given single intramuscular injections of 10 mg/kg bw
each of penicillin G and dihydrostreptomycin. Serum levels of each
drug were assayed by microbiological agar diffusion methods up to 72
hours after injection. Dihydrostreptomycin was assayed using Bacillus
pumilis, and penicillin was assayed using either Bacillus subtilis
or Bacillus stearothermophilus.
Peak plasma levels of approximately 44 µg/ml were reached at
approximately 1 hour. The plasma elimination half-life was
approximately 5 hours, and the AUC was 207.2 ± 33.8 µg/ml/hour.
Dihydrostreptomycin was below the limit of detection (0.3 µg/ml) in
all animals by 48 hours after injection (Rudd & Silley, 1987a).
Two young Holstein-Friesian steers weighing approximately 300 kg
each were injected intramuscularly with uniformly tritiated
dihydrostreptomycin (specific activity 262 mCi/mmol) plus carrier drug
at a single dose of 25 mg/kg bw, given as three separate injections
into the scapular region. Plasma, urine, saliva and lachrymal
secretions were sampled up to 5 days after the injection. The maximal
concentrations in plasma and urine were 78 and 1875 µg/ml,
respectively, and were achieved at 3-4 hours after injection. Low drug
concentrations (1.7 µg/ml) were still detectable in urine at 96 hours
after injection. No radioactivity was detected in saliva or lachrymal
secretions. The apparent volume of distribution was 23%,
corresponding to the extra-cellular fluid. The absorption and
excretion rates were similar when assayed microbiologically with
Staphylococcus aureus (Stalheim, 1970).
Dihydrostreptomycin was administered intramuscularly to 21
heifers and 6 dairy cows at 5 and 7.5 mg/lb bw (11 and 16.5 mg/kg bw),
respectively. Peak blood levels were reached at 1-2 hours after
injection and averaged approximately 45 µg/ml (with a range of 8.5-
100 µg/ml) for the 11 mg/kg bw dose, and 65.0 µg/ml (with a range of
40-122 µg/ml) for the 16.5 mg/kg bw dose. Dihydrostreptomycin was
assayed in the milk of 7 cows which had been injected with 11 mg/kg
bw. The drug was detected in 4 cows only, at concentrations ranging
from trace levels to 6.25 µg/ml, at 4 to 18 hours after injection. The
limit of detection of the assay was not stated for either blood or
milk (Hammond, 1953).
After intramuscular administration of 0.5 g dihydrostreptomycin
per 100 lb (11.1 mg/kg bw) to 26 dairy cows, drug concentrations were
detectable in the milk from 11 animals. At 36 hours milk levels were
at the limit of detection of 0.04 µg/ml for 8 cows. At 48 hours the
drug was undetectable in all animals. When administered at 1 to 2
g per 100 lb bw (22 to 44 mg/kg bw) peak levels of 0.07 to 0.12 µg/ml
were reached in milk at 24 hours, but were below the limit of
detection at 48 hours (Blobel & Burch, 1960).
2.1.1.6 Pigs
Three cross-bred barrows weighing approximately 100 kg each were
injected intramuscularly with uniformly tritiated dihydrostreptomycin
(specific activity 262 mCi/mmol) plus carrier drug at a single dose of
25 mg/kg bw/day, given as three separate injections. Plasma and urine
were sampled up to 5 days after the injection. The maximal
concentrations in plasma and urine were approximately 90 and 7100
µg/ml, respectively, and were achieved 1-2 hours after injection. Low
drug concentrations (approximately 3 µg/ml) were still detectable in
urine at 86 hours after injection. The apparent volume of distribution
was 21%, corresponding to the extracellular fluid. The absorption and
excretion rates were similar when assayed microbiologically with
Staphylococcus aureus (Stalheim, 1970).
The results of the foregoing studies are summarized in Table 1.
2.1.1.7 Humans
As a class, aminoglycoside antibiotics cross membranes very
poorly and only about 1% of an oral dose is absorbed, even when there
is intestinal inflammation or ulceration (Pratt & Fekaty, 1986).
Dollery (1991) reported that after oral administration of
streptomycin, 60%-100% of the drug can be recovered unchanged from the
faeces.
Table 1. Pharmacokinetics parameters for dihydrostreptomycin after intramuscular administration to various species
(Values represent ± standard deviation or range)
Species Dose (i.m.) Cmax (plasma) Tmax hours AUC mcg/ Cmax urine t´ hours Vd Reference
(mg/kg bw) (µg/ml) (ml/hour) (µg/ml)
Cats 10 25.1 ± 8.6 1.2 ± 0.4 61.4 ± 15.1 - 1.4 ± 0.1 - Rudd & Silley, 1987d
Dogs 10 41.2 ± 8.07 0.8 ± 0.26 74.1 ± 8.50 - 1.0 ± 0.17 - Rudd & Silley, 1987c
Sheep 10 44.8 ± 14.3 0.8 ± 0.3 151.5 ± 35.9 - 2.3 ± 0.3 - Rudd & Silley, 1987b
Cattle 10 44.3 ± 15.2 1.1 ± 0.4 207.2 ± 33.8 - 4.9 ± 0.5 - Rudd & Silley, 1987a
Cattle 11 44.7 (8.5-100) 1 - 2 - - - - Hammond, 1953
Cattle 16.5 65.0 (40.0-122) 1 - 2 - - - - Hammond, 1953
Cattle 25 78 3 - 4 - 1875 - 23% Stalheim, 1970
Pigs 25 87 1 - 2 - 7120 - 21% Stalheim, 1970
The aminoglycosides are reported to have a volume of distribution
of 25% of lean body mass in adults, corresponding to the extracellular
fluid volume. The volume of distribution in neonates may average 60%
of body weight. The volume of distribution in obese individuals is
less than in those with normal body weight. The volume of distribution
also varies with edema, which tends to reduce serum concentrations,
and dehydration which increases serum concentrations. The presence of
fever reduces serum concentrations by up to 40%, due to increased
renal blood flow and glomerular filtration.
Aminoglycosides accumulate in the kidney relative to plasma
levels, and detectable concentrations of aminoglycosides persist in
urine for several weeks, suggesting binding of the drug to kidney.
Accumulation also occurs in the perilymph of the inner ear, where the
elimination half-life is much longer than in serum (10-12 hours in
perilymph compared to 2 hours in serum).
Aminoglycoside levels in interstitial fluid approximate serum
levels. In bile, 25-50% of serum levels are obtained in the absence of
biliary obstruction. In sputum and bronchial secretions 25-67% of
serum levels may be achieved; in pericardial, pleural and ascitic
fluids approximately 50% of serum levels are obtained; and synovial
fluid may contain 50-100% of serum levels. Penetration into the eye,
cerebrospinal fluid and ventricular fluid is very poor. Placental
transfer occurs and fetal serum concentrations range from 20-40% of
maternal serum levels (Pratt & Fekaty, 1986).
Approximately 20% of a parenteral dose of streptomycin cannot be
accounted for in urine, but no metabolites have yet been identified.
Approximately 1% is excreted in bile (Dollery, 1991).
The excretion rate after parenteral administration of
amino-glycosides is dependent on renal function and is linearly
related to the creatinine clearance rate. The elimination half-life in
adults is 2 hours, but 5-6 hours in neonates due to their lower
glomerular filtration rate (Pratt & Fekaty, 1986).
2.1.2 Biotransformation
The aminoglycosides are reported not to be metabolized in humans
and are excreted in their active forms by glomerular filtration (Pratt
& Fekaty, 1986).
2.1.3 Effects on enzymes and other biochemical parameters
No information available
2.2 Toxicological studies
2.2.1 Acute toxicity studies
2.2.1.1 Mice
The oral LD50 of different dihydrostreptomycin salts was compared
in male Carworth CF1 mice weighing 20 g on average.
Dihydrostreptomycin hydrochloride gave an LD50 of 12 500 mg/kg bw,
whereas the sulfate salt gave an LD50 of greater than 30 000 mg/kg bw
(Edison et al., 1951).
2.2.1.2 Chickens
The LD50 for dihydrostreptomycin sulfate administered
intramuscularly to groups of fifty 1, 2, 3, or 4 week-old chicks was
743, 1090, 1738, and 1868 mg/kg bw, respectively. Clinical signs of
toxicity in all birds were depression, drooping wings, closed eyes,
muscular weakness and slowed respiration (Huebner et al., 1956).
Dihydrostreptomycin sulfate was administered intramuscularly to
groups of 3 white Leghorn chickens weighing 600 g, at doses of 800 to
2500 mg/kg bw. Clinical signs of toxicity included ataxia,
prostration, gasping, and coma. The LD50 was 2167 mg/kg bw (Gray &
Purmalis, 1958).
2.2.1.3 Pigeons
Dihydrostreptomycin sulfate was administered intramuscularly at
doses of 400 to 1000 mg/kg bw to groups of 5 racing pigeons weighing
an average of 360 g. Clinical signs of toxicity included emesis,
somnolence, ataxia, depression, and coma. The LD50 was determined as
715 mg/kg bw (Gray & Purmalis, 1958).
2.2.1.4 Gerbils
A group of 10 gerbils (5/sex), 7-10 weeks of age and weighing
55-65 g were given single intramuscular injections of 50 mg
dihydrostreptomycin sulfate (equivalent to 769-909 mg/kg bw).
Ascending flaccid paralysis was observed in 10/10 animals at 2 to 5
minutes after injection, and 8/10 animals died within 4 to 25 minutes
after injection. The 2 surviving animals gradually regained muscle
control and awareness with apparently complete recovery at 65 and 120
minutes post-injection, respectively (Wightman et al., 1980).
The results of acute toxicity studies on dihydrostreptomycin are
summarized in Table 2.
Table 2. Acute toxicity of dihydrostreptomycin
Species Number Route LD50 mg/kg bw Reference
(age/weight) (salt)
Mice - oral >30 000 Edison et al., 1951
(20g) (sulfate)
12 500
(hydrochloride)
Chickens 50/group i.m. 743 - 1868 Huebner et al., 1956
(1-4 weeks) (sulfate)
Chickens 3/group i.m. 2167 Gray & Purmalis,
(600g) (sulfate) 1958
Pigeons 5/group i.m. 715 Gray & Purmalis,
(360g) (sulfate) 1958
Gerbil 10 i.m. < 769 Wightman et al., 1980
(7-10 weeks,
55-65g)
2.2.2 Short-term toxicity studies
2.2.2.1 Guinea-pigs
Three groups of 30 young adult guinea-pigs (15/sex/group) were
treated for 90 days with either 40 mg dihydrostreptomycin/kg bw/day in
distilled water by gavage, an equal volume of distilled water alone by
gavage (negative control), or 200 mg kanamycin/kg bw/day, s.c.
(positive control).
The kanamycin-treated animals exhibited spastic twitching
immediately after dosing, injection site reactions and some animals
became ataxic. Body-weight gain was depressed in the kanamycin group,
but was comparable to controls in the dihydrostreptomycin group.
Auditory function was assessed using the pinna twitch reflex
(Preyer reflex) in response to a whistle. Hearing loss was observed in
all the animals in the kanamycin group after week 6, and in two
negative control animals after weeks 7 to 9, which were later found to
be suffering from an inner ear infection. No hearing loss was observed
in the dihydrostreptomycin treated animals.
A large number of animals died during the study (7 negative
controls, 6 positive controls, and 6 treated with
dihydrostreptomycin). These were necropsied, as were all surviving
animals at the end of the study. All tissues with observed gross
lesions, plus the organ of Corti from all animals, were examined
histologically.
Of the animals treated by gavage, several animals died of a
ruptured oesophagus (3 negative controls and 3 in the
dihydrostreptomycin group). Almost all of the remaining animals dying
on test had lesions of the lungs due to pneumonia.
The authors reported that because the organs of Corti were
inadequately preserved they showed signs of degeneration,
histologically. However, the architecture of the cell layers and the
hair cells were still discernible. The positive control animals
(kanamycin group) demonstrated either no hair cells at any level of
the cochlea, or very few and damaged hair cells. The majority of
dihydrostreptomycin-treated animals had hair cells with largely normal
architecture, although hair cell damage was noted as being more severe
in males than females treated with dihydrostreptomycin (Tisdel &
Harris, 1976).
2.2.2.2 Cats
Dihydrostreptomycin was administered orally in a food vehicle
(liver cat food) to 3 groups of 10 cats (5/sex/group) weighing between
1.5 and 4.6 kg, for 90 days at doses of 1, 5 or 10 mg/kg bw/day. Ten
cats of each sex were used as controls.
One male cat in the mid-dose group died during the ninth week of
treatment. A watery red urethral discharge and a distended bladder
were observed in this animal the day prior to death, and pathological
examination revealed acute cystitis with concomitant peritonitis. All
other cats survived the 90 days of treatment and no compound-related
effects were observed on body-weight gain, food consumption,
haematology, blood chemistry, urinalysis, gross pathology or
histopathology (only liver and kidneys of controls and 10 mg/kg/day-
treated cats were examined) (Wazeter, 1970a).
Vestibular function was assessed in 10 cats (5/sex) treated daily
with oral doses of 40 mg dihydrostreptomycin/kg bw/day for 90 days.
Streptomycin sulfate was used as the positive control (200 mg/kg
bw/day, s.c.). Animals in the negative control group were
administered water by gavage.
Three cats died, one in each of the negative control, positive
control, and dihydrostreptomycin groups, due to urinary obstruction
which was considered unrelated to treatment.
For the dihydrostreptomycin group, no treatment-related effects
were observed on body weight, haematology, blood chemistry,
ophthalmoscopic examination, bone marrow smears, or gross pathology.
Vestibular function remained normal throughout the treatment period
based on results of righting reflex tests in which animals were
dropped from an inverted position two feet above a cushioned mat. The
NOEL was 40 mg/kg bw/day dihydrostreptomycin in this study. The
results with streptomycin are described in section 2.2.2.5 of the
monograph on streptomycin (Tisdel et al., 1976).
2.2.2.3 Sheep
A target animal safety study was conducted with
dihydro-streptomycin in 3 groups of 4 sheep (2/sex/group) aged 13 to
16 months and weighing approximately 45 kg to 70 kg. Animals were
treated with daily intramuscular injections of 10 mg procaine
penicillin G plus 10 mg dihydrostreptomycin/kg bw/day for 5
consecutive days (the recommended therapeutic treatment regime), the
second group received 30 mg of each drug/kg bw/day for 5 days, and the
third group received 10 mg of each drug/kg bw/day for 15 days. A
treatment-free control group was not included, although pre-treatment
parameters were measured in each animal.
Behaviour was normal and there were no clinical signs of
neuromuscular blockade. No localized injection site reactions were
observed. Pathological changes observed in skeletal muscle and liver
at post-mortem examination were largely due to parasitic infestations.
Slight congestion/consolidation was observed in the lungs at necropsy,
which was not examined further. There was no evidence of ototoxicity
based on results of a crude hearing test and normal histology of the
VIIIth cranial nerve. There was no pathological evidence of
nephrotoxicity at post-mortem examination. Urinalyses were not
performed.
Some haematological and biochemical parameters were altered
during and after treatment. Differences reached statistical
significance in some groups compared with pre-treatment values,
whereas other parameters were altered then subsequently recovered to
pre-treatment values. The haematological changes included a reduction
in haemoglobin, red cells, haematocrit and mean cell volume.
Biochemical changes included a decrease in sodium, phosphorus,
creatinine, and bilirubin, and an increase in chloride. The only
consistent dose-related trends were decreased sodium and increased
chloride levels during prolonged treatment (15-day group), and a lower
haematocrit in all treatment groups. These changes, although
statistically significant were small and were considered by the
authors not to be clinically relevant (Brooks & Rolph, 1989b).
2.2.2.4 Pigs
A target animal safety study was conducted with
dihydrostreptomycin in 3 groups of 4 pigs (2/sex/group in groups 2 and
3, 1 female and 3 males in group 1) approximately 8 weeks of age and
weighing between 23 and 29 kg. Animals were treated with daily i.m.
injections of 10 mg procaine penicillin G plus 10 mg
dihydrostreptomycin/kg initial bw/day for 5 consecutive days (the
recommended therapeutic treatment regime, group 1), the second group
received 30 mg of each drug/kg initial bw/day for 5 days (group 2),
and the third group received 10 mg of each drug/kg initial bw/day for
15 days (group 3). An untreated control group was not included,
although pre-treatment parameters were measured in all animals.
Body weights increased rapidly in all groups (in group 3 body
weights had increased by 50% after 15 days). Therefore the dose
administered on a body-weight basis was reduced with time,
particularly in group 3. A crude hearing test revealed no auditory
impairment, and behaviour was normal, except for 2 animals in group 3
that showed symptoms that were attributed to stress (vomiting,
inactivity, haematemesis and slight cyanosis of ears and legs) on days
1 and 15, respectively.
Changes were observed compared with pretreatment values in
haematology and serum chemistry values (reduced haemoglobin, red cells
and haematocrit, reduced neutrophils, increased mean corpuscular
haemoglobin, decreased creatinine, and increased calcium), some of
which reached statistical significance. However, there were no obvious
drug-related or time-related trends, and although statistically
significant, the changes were small and were considered by the authors
not to be clinically relevant.
The VIIIth cranial nerve was histologically normal in all but one
animal in group 1 in which focal chronic inflammation was observed.
Focal interstitial nephritis was observed in one pig in group 1 and
two pigs in group 2. These effects were not considered by the authors
to be treatment-related. No local injection site reactions were
observed (Brooks et al., 1989).
2.2.2.5 Cattle
A target animal safety study was conducted with
dihydrostreptomycin in 3 groups of 4 cattle (2/sex/group),
approximately 6 months of age and weighing between 100 and 170 kg.
Animals were treated with daily i.m. injections of 10 mg procaine
penicillin G plus 10 mg dihydrostreptomycin/kg bw/day for 5
consecutive days (the recommended therapeutic treatment regime), the
second group received 30 mg of each drug/kg bw/day for 5 days, and the
third group received 10 mg of each drug/kg bw/day for 15 days. An
untreated control group was not included, although pre-treatment
parameters were measured in each animal.
No consistent treatment-related effects on haematological or
biochemical parameters were observed. Behaviour was normal and there
were no clinical signs of neuromuscular blockade. The few injection
site reactions that were observed were minor in nature. The only
pathological changes present in tissues and organs at post-mortem
examination were in the lungs, which were attributed to respiratory
tract infection. There was no evidence of ototoxicity based on results
of a crude hearing test and normal histology of the VIIIth cranial
nerve. There was no histological evidence of nephrotoxicity at
post-mortem examination. Urinalyses were not performed (Brooks &
Rolph, 1989a).
2.2.3 Long-term toxicity/carcinogenicity studies
2.2.3.1 Rats
Dihydrostreptomycin was administered in the diet to Charles River
CD rats, (35/sex/group), to achieve dosages of approximately 1, 5, or
10 mg/kg bw/day for up to 2 years (dietary concentrations were
adjusted weekly to compensate for changes in food consumption and body
weight). Two control groups were included in the study. Five
rat/sex/group were scheduled for interim kills at 6 and 12 months. The
remaining 25 animals/sex/group were administered dihydro-streptomycin
for 2 years. Interim study reports were submitted at 6 and 18 months,
and a final report at 2 years.
In the 6-month interim report, it was reported that 2 rats died
in the low-dose group during the first week of treatment (cause of
death unknown), and were replaced. One male control rat died after its
6-month blood sample was taken. There were no treatment-related
effects observed on food consumption, haematology or urinalysis
(analyses from 5 rats/ sex/group at 3 and 6 months), hearing or
vestibular function (measured in all rats at 3 and 6 months). Serum
chemistry was not evaluated in this study. Body weights were slightly
decreased in males in all treatment groups compared with controls,
which reached statistical significance for all groups; however, no
clear dose-response relationship was established. One male rat in the
5 mg/kg bw/day group had a grossly abnormal posture from the seventh
treatment onwards, and was found to have severe bilateral suppurative
otitis media when necropsied at 6 months. One to two rats in all
treated groups, but no controls, were also reported to have this
condition at the 6 month necropsy when 5 animals per sex/group were
killed. No other treatment-related effects were noted on gross
pathology or histopathology. Histological examination of the auditory
system or associated nerves was not performed (Wazeter, 1970b).
In the 18-month interim report, the body weights of male rats in
the high-dose group were significantly reduced when compared to
control group 1 but not control group 2. Body weights in all other
male treatment groups were comparable to controls. No
treatment-related effects were observed on food consumption,
haematology, or urinalysis. No effects were reported on hearing or
vestibular function as defined by the tests used. One female rat in
the high-dose group had an abnormal posture and occasional slowed
righting reflex from week 73 onwards, and two males in the mid-dose
group had "impaired use of the hindquarters" from week 64 onwards, one
of which subsequently died in week 69. Mortality rates were similar
for all treatment and control groups at 78 weeks, ranging from 0 to 4
deaths per group of 25 animals. None of the deaths were considered by
the author to be treatment-related. Causes of death were reported as
due primarily to spontaneous neoplasias (usually of the pituitary or
mammary glands) and infectious processes; however, no gross pathology
or histopathology data were provided with the report (Wazeter, 1971).
In the two-year report, 12 to 17 out of 25 rats/sex in treated
groups had survived up to two years. No treatment-related effects were
observed on survival, food consumption, urinalysis, haematology, or
hearing. Body-weight gain was reduced in males in the high-dose group
compared to control group 2, but not control group 1. Body weights
were comparable to controls in all other groups. Vestibular function
was impaired in both control and treated groups (inability to remain
on a bar or abnormal gait was observed in 5 control rats, 2 rats each
in the low- and mid-dose groups, and 3 rats in the high-dose group, no
sex differences were observed). On necropsy, 2 rats in the high-dose
group had gross lesions of the middle ear (purulent otitis media). All
other gross pathological changes and histopathological changes
(examined in controls and high-dose group only) occurred with similar
frequency in all rats examined at two years. Neoplasms were observed
with comparable frequency in both treatment and control groups and
were similar to the historical control incidence for this facility.
Although this study did not meet current standards regarding the
number of animals started on the two-year phase of the study
(25/sex/group), the Committee concluded that survival of more than 50%
of all treated animals in the 2-year phase of the study (24/50, 33/50,
and 29/50 in the low-, mid-, and high-dose groups, respectively),
represented an adequate test of the carcinogenic potential of the
compound. The NOEL was 5 mg/kg bw/day based on decreased body-weight
gain in males at the high dose (Wazeter & Goldenthal, 1972).
2.2.4 Reproductive toxicity studies
No information available
2.2.5 Special studies on embryotoxicity/teratogenicity
2.2.5.1 Guinea-pigs
Streptomycin and dihydrostreptomycin were administered by daily
i.m. injection to groups of 2 to 4 pregnant guinea-pigs at doses of
10, 25, 50, 100 or 200 mg/kg bw/day. The duration of the treatment
period was not stated. A dose of 100-200 mg/kg bw/day of both drugs
caused abortion or death within 8-10 days. All fetusus were macerated,
indicating that death occurred prior to abortion or death of dams. At
doses of 25-50 mg/kg bw/day, some animals aborted, some survived, and
some stillbirths were observed. A dose of 10 mg/kg bw/day for 24 days
caused no abortions. The surviving F1 animals were clinically normal
with respect to vestibular and auditory function, and the CNS was
normal on histological examination. The placentae from streptomycin-
or dihydrostreptomycin-treated animals showed marked hyperaemia,
haemorrhage, and endometrial necrosis 24 hours after a single
intramuscular dose of 100 mg/kg bw. These changes progressed with
further treatment. Serum concentrations of dihydrostreptomycin and
streptomycin measured in the fetus were 2-4% of those in the dams
(Riskaer et al., 1952).
2.2.5.2 Rabbits
Groups of 31, 23, and 26 pregnant female Dutch rabbits, weighing
approximately 2 to 4 kg, were treated by oral intubation with 0, 5, or
10 mg dihydrostreptomycin/kg bw/day, respectively, from days 6 to 18
of gestation. The vehicle control group received 0.5% aqueous
methylcellulose.
One rabbit in the 5 mg/kg bw/day group was found dead on
gestation day 10. Four control rabbits and 1 in the 10 mg/kg bw/day
treatment group aborted, all after gestation day 14. No
treatment-related effects were observed on maternal behaviour,
appearance, or body-weight gain. On day 30, all animals were killed
for pathological examination. There were no treatment-related effects
on the pregnancy rate, number of corpora lutea, number of viable
fetuses, percentage of abnormal fetuses, litter size, mean fetal body
weight, or 24-hour survival rate. The number of abortions and
resorptions/empty implantation sites were higher in controls compared
to treated groups. Presence of a 13th rib was a frequently noted fetal
abnormality; however the incidence was similar in all groups. One
control fetus was acephalic with a ventral hernia, and one fetus in
the 5 mg/kg bw/day group had agenesis of skin and soft tissue over the
left lateral nasal and buccal area, and absent hind claws. All of
these findings were considered by the authors as unrelated to
treatment.
Because no maternal toxicity was observed, the Committee
concluded that the dose levels may not have been high enough to fully
exclude teratogenic potential (Wazeter, 1970c).
2.2.5.3 Humans
Auditory toxicity has been reported in children whose mothers
were treated with streptomycin and dihydrostreptomycin during
pregnancy. However, details of the dose administered and the timing
in relation to the pregnancy are often not stated (Davies, 1991;
Robinson & Cambon, 1964; Snider et al., 1980; Varpela et al.,
1969; Warkany, 1979).
Organogenesis of the inner ear occurs at week 7 of pregnancy, and
cochlear development continues up to mid-term (Varpela et al.,
1969). It is the only organ in the body to reach full adult size and
complete differentiation by midterm (Robinson & Cambon, 1964).
However, unlike teratogens, the toxic effects of streptomycin and
dihydrostreptomycin on the fetus are independent of the critical
periods of embryogenesis. Ototoxicity can occur throughout the
gestation period (Snider et al., 1980), as well as in adults (see
effects in humans, section 2.3.1 below). In children of streptomycin-
and dihydrostreptomycin-treated mothers, as well as in adults,
high-tone hearing is primarily affected first, which is outside of the
range of normal speech frequencies (Donald & Sellars, 1981).
The results of a literature review of pregnancy outcomes in women
receiving streptomycin or dihydrostreptomycin for tuberculosis is
presented by Snider et al., 1980. Of a total of 203 women, 206
pregnancies were followed to term. Seventy-two women received
streptomycin or dihydrostreptomycin during the first 4 months of
pregnancy, 73 women received one or the other after the fourth month,
and the timing was unknown for 61 women. The dose of streptomycin or
dihydrostreptomycin administered in these cases, where stated, was
between 1 g to 2 g daily or twice weekly, with total doses ranging
from 2 g to 202 g. Several other drugs were administered concomitantly
for tuberculosis, i.e. 88 women also received isoniazid, 1 received
rifampicin, 1 received ethambutol, 83 received p-amino-salicylic acid,
and for 59 women the other drug was not known. There were 2
spontaneous abortions, no premature births and no stillbirths, and 170
normal term infants were delivered. Abnormalities were observed in 35
infants (a rate of 169 per 1000, roughly 1 in 6, is reported by the
authors). The majority of these consisted of vestibular dysfunction
and varying degrees of hearing loss. Hearing loss occurred in the
high-tone range first, i.e. before the range of normal speech
frequencies was affected. No other abnormalities were reported (Snider
et al., 1980).
2.2.6 Special studies on genotoxicity
Streptomycin and dihydrostreptomycin bind to and alter the
configuration of the 30S subunit of ribosomes, thus inhibiting protein
synthesis and causing misreading of the genetic code. RNA and DNA
synthesis are unaffected (Goldberg, 1965; Davies et al., 1964).
The results of genotoxicity assays with dihydrostreptomycin are
summarized in Table 3.
Table 3. Results of genotoxicity assays on dihydrostreptomycin
Test system Test object Concentration Results Reference
In vitro
Cytogenetics Human lymphocytes 4.7-13.7 mg/ml Negative Obe, 1970
2.2.7 Special studies on immune responses
The incidence of allergic reactions in humans to systemically
administered aminoglycosides is reported to be very low (Pratt &
Fekaty, 1986).
2.2.8 Special studies on ototoxicity
2.2.8.1 Cats
The ototoxicity of streptomycin and dihydrostreptomycin was
investigated in cats after they had recovered from surgical
destruction of one ear. Seven cats were treated with streptomycin at
doses and treatment periods ranging from 200 mg/kg bw/day for 9.5 days
to 25 mg/kg bw/day for 84 days. Six cats were treated with
dihydrostreptomycin at doses and treatment periods ranging from 300
mg/kg bw/day for 21 days to 100 mg/kg bw/day for 60 days. After the
last dose, animals were kept treatment-free for 1 year then necropsied
for histopathological examination of the inner ear and the brain stem
nuclei.
Clinical signs of ototoxicity were similar in both groups, which
included permanent high frequency hearing loss, loss of
post-rotational nystagmus, and ataxia. Weight loss was also noted as
a treatment-related effect in both groups. With dihydrostreptomycin
treatment, the hearing loss was delayed and occurred several weeks to
several months after treatment.
In the inner ear, loss of hair cells in the cochlea, and damage
to the sensorimotor epithelium and hair loss in the cristae of the
vestibular canals were observed. The cristae appeared to be more
susceptable to toxic effects than the maculae of the saccule and
utricle.
In the brain stem, no lesions were found in the vestibular
nuclei. The vestibular portion of the VIIIth nerve was normal,
despite the fact that the sensorimotor epithelium and supporting cells
of the vestibular apparatus had been destroyed (surgically on one
side, and due to streptomycin and dihydrostreptomycin treatment on the
other side).
Effects observed in the brain stem included degenerative changes
in the ventral and dorsal cochlear nuclei, occurring primarily in
those parts corresponding to the ear which had been surgically
destroyed. In 2 animals treated with streptomycin, these lesions were
observed on the side corresponding to the ear which had not been
destroyed surgically. In these 2 animals, degeneration of the spiral
ganglion was also observed.
The authors described these degenerative changes as being typical
of trans-synaptic atrophy. The nuclei were smaller, containing smaller
nerve cells arranged more compactly, and changes were observed in the
myeloarchitecture. The cochlear branch of the VIIIth nerve appeared
shrunken with only a few myelinated fibres. There were no lesions in
the cerebellum or any other part of the brain stem.
The authors concluded that the lesions produced by both
streptomycin and dihydrostreptomycin were limited to the vestibular
end-organ of the inner ear in cats (McGee & Olszewski, 1962).
Dihydrostreptomycin was administered subcutaneously to groups of
2 cats at a dose of 800 mg/kg bw/day for 15 days or 200 mg/kg bw/day
for 120 days. Moderate to severe ataxia was observed from days 8 and
10 in the 800 mg/kg bw/day group, and from days 28 and 78 in the 200
mg/kg bw/day group. Animals were necropsied at the end of the
treatment period and the inner ear examined. Scattered degeneration of
the hair cells was observed in the cristae of the horizontal
semicircular canals, and was more severe in the high-dose group. The
cochlea of dihydrostreptomycin-treated cats was comparable to controls
as judged by electrophysiological studies of voltage changes at the
round window in response to tones of varying frequencies. The authors
reported that streptomycin produced more severe vestibular and
cochlear changes in a previous study than those produced by
dihydrostreptomycin; however, the doses of streptomycin used were not
stated. The authors also reported that cochlea of the cat appears to
be more sensitive to streptomycin than dihydrostreptomycin, whereas
the opposite is true in humans (Hawkins & Lurie, 1953).
2.2.9 Special studies on microbiological effects
2.2.9.1 Hamsters
Groups of 6 hamsters were fed a diet containing 0 or 10 mg/kg
dihydrostreptomycin. After 47 days, oxytetracycline (10 mg/kg) was
added to the diet and a suspension of E. coli (106 organisms/ml)
susceptible to both drugs was added to the drinking-water for two
weeks. Faecal samples were collected throughout the study and analyzed
for lactose-fermenting enteric organisms resistant to either
dihydrostreptomycin or oxytetracycline. No dihydrostreptomycin- or
oxytetracycline-resistant organisms were detected in the faeces at any
time (Rollins et al., 1975).
2.2.9.2 Dogs
Groups of 5 beagle dogs with an average weight of 15 kg were fed
a diet containing 0, 2, or 10 mg dihydrostreptomycin per kg of feed
(equivalent to 50 or 250 µg/kg bw/day) for 35 days. In both treatment
groups there was a shift in the faecal flora from predominantly
dihydrostreptomycin-susceptible lactose fermenting coliforms to a
resistant population after 15 days, which was significant (p < 0.01)
in both groups. This persisted throughout the 28-day post-treatment
phase of the study. A definitive response was not seen in the control
group. The authors concluded that the NOEL for development of drug
resistance in enteric bacteria was less than 2 mg/ kg of diet,
equivalent to 50 µg/kg bw/day (Gaines et al., 1978).
2.2.9.3 Humans
Healthy human volunteers were treated with 0.75 mg of
dihydrostreptomycin administered orally in a hamburger patty, 4 days
per week, for 7 weeks. Faecal samples were examined weekly for the
presence of coliforms bearing R-factor mediated resistance to
dihydrostreptomycin. The presence of resistant coliforms fluctuated
from week to week in about 30% of untreated controls. Fluctuations
were also observed in treated subjects. Four of 25 treated subjects
and 6/29 controls never excreted resistant coliforms; however, when
resistant coliforms were acquired, they tended to persist longer and
to multiply to greater numbers in the presence of dihydrostreptomycin
than in controls (Snyder et al., 1972).
2.2.9.4 Dairy starter cultures
Five strains each of various bacterial species were tested for
their sensitivity to dihydrostreptomycin by measuring zones of
inhibition of bacterial growth around discs impregnated with 2 or 10
µg/disc. The bacteria used were strains of Streptococcus (S.
lactis, S. cremoris, S. diacetilactis, S. thermophilus, S. durans, S.
faecalis) Lactobacillus bulgaricus, Brevibacterium linens,
Leuconostoc dextranicum, Staphylococcus (S. aureus, S. epidermidis),
and Micrococcus varians. All were susceptible except all
strains of Streptococcus faecalis and 3/5 strains of Streptococcus
durans (Reinbold & Reddy, 1974).
2.2.9.5 Minimum inhibitory concentrations in vitro
The minimum inhibitory concentration (MIC) of dihydrostreptomycin
sulfate was determined in vitro for bacteria isolated from the
intestines or faeces of healthy human adults. Over 100 isolates were
tested which represented 17 species and covered the 10 most common
genera of human intestinal microbes. The methods and controls used
were those proposed by the National Council for Clinical Laboratory
Standards (NCCLS) describing MIC assays for anaerobic bacteria.
E. coli was additionally assayed under aerobic conditions. The agar
dilution method was used, with Wilkins Chalgren agar or BHI agar
supplemented with 5% rabbit's blood, and incubations were for 48 hours
at 37 ± 2 °C. Dihydrostreptomycin was tested at serial double
dilutions from 128 µg/ml to 2 µg/ml. At each concentration, bacterial
cells were tested at two densities, 1 x 105 cells per spot, which is
recommended by NCCLS for clinical isolates, and 1 x 107 cells per
spot, which is considered to be more representative of the bacterial
concentration within the intestinal ecosystem. The results of this
study are summarized in Table 4.
Bifidobacterium spp. were found to be the most sensitive. Data
available for 5 strains of Bifidobacterium adolescentis gave an
MIC50 value of 32 µg/ml and a MIC range of 16-64 µg/ml, and data on
5 strains of Bifidobacterium longum gave an MIC50 value of 16 µg/ml
and a MIC range of 8-32 µg/ml.
The MIC50 value for dihydrostreptomycin in most of the other
bacterial species tested (17 bacterial species, with 5-11 strains
tested per species) was higher than 32 µg/ml, with the highest MIC50
values being more than 128 µg/ml.
An MIC50 value of 32 µg/ml was therefore established as the
concentration without effect on the human gut flora (Carman, 1994).
Table 4. MIC values for bacterial isolates from human intestinal material
(All values represent mcg/ml)
Species 1 x 107 cells / spot 1 x 105 cells / spot
n = no. of strains MIC50 MIC90 Range MIC50 MIC90 Range
E. coli 16 64 8-64 16 32 8-64
(aerobic) n=11
E. coli 64 128 32->128 32 64 16-128
(anaerobic) n=11
Bacteroides vulgatus >128 >128 128-128 >128 >128 64->128
n=5
Bacteroides uniformis >128 >128 >128 >128 >128 >128
n=5
Bifidobacterium 32 64 16-64 32 32 8-32
adolescentis
n=5
Bifidobacterium 16 32 8-32 16 16 8-32
longum n=5
Lactobacillus >128 >128 64->128 128 >128 32->128
acidophilus n=10
Fusobacterium >128 >128 128->128 >128 >128 128->128
russi n=5
Fusobacterium >128 >128 128->128 >128 >128 64->128
prauznitii n=5
Peptostreptococcus >128 >128 64->128 >128 >128 64->128
DZ n=5
Peptostreptococcus >128 >128 128->128 >128 >128 128->128
productus 1 n=5
Ruminococcus 64 64 64 64 64 32-64
gnavus n=5
Ruminococcus 64 64 64-128 64 64 64
bromii n=5
Table 4 (contd)
Species 1 x 107 cells / spot 1 x 105 cells / spot
n = no. of strains MIC50 MIC90 Range MIC50 MIC90 Range
Eubacterium >128 >128 128->128 >128 >128 64->128
aerofaciens n=5
Eubacterium >128 >128 >128 >128 >128 128->128
rectale n=5
Coprococcus 64 64 64-128 32 64 32-64
eutactus n=5
Coprococcus 64 64 32-64 32 64 32-64
comes n=5
Gemmiger 64 128 64->128 64 128 32->128
formicilis n=10
2.3 Observations In humans
2.3.1 Ototoxicity
The aminoglycosides are all potentially toxic to the inner ear at
therapeutic doses. Streptomycin-induced ototoxicity primarily affects
the vestibular system before auditory function is affected, whereas
dihydrostreptomycin primarily affects the cochlea before vestibular
function is affected. With both streptomycin and dihydrostreptomycin
hearing loss occurs in the high tone range first, i.e. before the
range of frequencies associated with normal speech is affected
(Martindale, 1993; Davies, 1991; Shambaugh et al., 1959; Hawkins &
Lurie, 1953; Pratt & Fekaty, 1986).
The primary toxic effect of both streptomycin and
dihydrostreptomycin is on the peripheral sensory portions of the inner
ear rather than on the eighth cranial nerve itself, which results in
progressive destruction of the hair cells of the Organ of Corti from
the basal region (responsive to high-frequency sounds) to the apex of
the cochlea (responsive to low-frequency sounds) as dosage and
duration of treatment are increased (Davies, 1991).
Dihydrostreptomycin causes delayed ototoxicity in humans
manifested as a sensorineural hearing loss which may involve any or
all frequencies. Hearing loss may occur from 1 to 6 months after drug
treatment, it is permanent, and it is not related to the size of the
dose (McGee & Olszewski, 1962; Shambaugh et al., 1959).
Aminoglycosides, including streptomycin and dihydrostreptomycin,
accumulate in the perilymph of the inner ear (Davies, 1991). A large
proportion of both drugs are excreted unchanged by the kidneys (Pratt
& Fekaty, 1986), and the risk of ototoxicity is therefore increased
when renal function is compromised (Erlansen & Lundgren, 1964).
Patients presenting with ototoxic side effects after treatment
with streptomycin, dihydrostreptomycin or kanamycin, for various
clinical conditions, were studied in a retrospective study. The route
of administration was not stated, although it was probably
intramuscular injection.
Two patients receiving a 50:50 mixture of streptomycin and
dihydrostreptomycin at doses of 0.5 or 1.0 mg/kg bw/day of each drug
(total dose 5 or 14.5 g of each drug) reported vertigo at the end of
the course of treatment. Four patients receiving dihydro-streptomycin
at a dose of 1 g per day (equivalent to 14 to 20 mg/kg bw/day, total
dose 6 to 36 g) reported tinnitus or impaired hearing (as assessed by
tone audiometry) between 2 weeks and 3 months after the course of
treatment. None of the patients in this group reported vertigo. Three
of these patients had impairment of renal function which may have
increased blood levels of dihydrostreptomycin and hence increased the
risk of ototoxicity. It was not stated whether the renal impairment
was pre-existing or caused by dihydrostreptomycin treatment (Erlanson
& Lundgren, 1964).
Dihydrostreptomycin has been reported to be more likely to cause
partial or complete hearing loss than streptomycin and was therefore
not recommended for use in humans (Martindale, 1993).
2.3.2 Renal toxicity
Nephrotoxicity due to aminoglycosides usually presents in humans
as an acute tubular necrosis manifested as proteinuria, cylinduria and
inability to concentrate the urine. This is followed by a reduction in
glomerular filtration rate with a rise in serum creatinine and blood
urea nitrogen. Aminoglycosides bind to the luminal surface of the
proximal tubules, are internalized by pinocytosis and fuse with
lysosomes. It is postulated that they become sequestered in lysosomes
where they disrupt phospholipid metabolism (prominant myeloid bodies
have been observed in renal tubular cells exposed to gentamicin), and
renal cell death occurs consequent to changes in lysosomal
biochemistry (Pratt & Fekaty, 1986).
2.3.3 Neuromuscular blockade
Aminoglycosides can produce a non-depolarizing type of
neuromuscular blockade due to reduced acetylcholine release from motor
nerve endings and reduced sensitivity of the post-junctional endplate;
this effect is completely reversed by administration of calcium (Pratt
& Fekaty, 1986).
2.3.4 Allergic reactions
The incidence of allergic reactions to systemically administered
aminoglycosides is reported to be very low. The incidence of allergic
reactions to dihydrostreptomycin specifically was not reported (Pratt
& Fekaty 1986).
2.3.5 Other effects
Aminoglycosides have been reported to cause neutropenia,
agranulocytosis, and aplastic anaemia on rare occasions. Transient
elevation of hepatic enzymes occurs occasionally with
amino-glycosides. The incidence of specific effects associated with
dihydrostreptomycin were not reported (Pratt & Fekaty, 1986).
5. REFERENCES
ANDERSON, D.G. & JEWELL, M. (1945). The absorption, excretion and
toxicity of streptomycin in man. New Engl. J. Med., 233: 485-491.
BACHARACH, A.L., CLARK, B.J., McCULLOCH, M., & TOMICH, E.G. (1959).
Comparative toxicity studies on ten antibiotics in current use.
J. Pharm. & Pharmacol., 11: 737-741.
BEEK, B., GÖBEL, D., OBE, G., & RADENBACH K.L. (1974). Prospective
controlled clinical trial of antitubercular agents in triple
combinations for mutagenicity in leukocyte cultures (short report).
Prax. Pneumol., 28: 970.
BERG, K. (1951). The toxic effect of streptomycin on the vestibular
and cochlear apparatus: an experimental study on cats. Acta Otolaryn
(Stoch), suppl. 97: 1-77.
BLOBEL, H., & BURCH, C.W. (1960). Diffusion of dihydrostreptomycin and
chlortetracycline into milk of dairy cows following parenteral
administration. J. Amer. Vet. Med. Assoc., 137 698-700.
BOUCHER, D & DELOST, P. (1964). Developpement post-natal des
descendants issus de meres traités par la streptomycine au cours de la
gestation chez la souris. C.R. Soc, Biol. (Paris), 158: 2065-2069.
BRITISH PHARMACEUTICAL CODEX (1968). The Pharmaceutical Press, London.
BROOKS, C., & ROLPH, T.P. (1989a). The effect of streptopen injection
on the health of cattle. Unpublished report No. AnH89/R/65 from
Pitman-Moore Ltd., Uxbridge, Middlesex, England. Submitted to WHO by
Pitman-Moore, Inc., Mundelein, IL, USA.
BROOKS, C., & ROLPH, T.P. (1989b). The effect of streptopen injection
on the health of sheep. Unpublished report No. AnH89/R/66 from Pitman-
Moore Ltd., Uxbridge, Middlesex, England. Submitted to WHO by Pitman-
Moore, Inc., Mundelein, IL, USA.
BROOKS, C., EASTWOOD, B., & ROLPH, T.P. (1989). The effect of
streptopen injection on the health of pigs. Unpublished report No.
AnH89/R/75 from Pitman-Moore Ltd., Uxbridge, Middlesex, England.
Submitted to WHO by Pitman-Moore, Inc., Mundelein, IL, USA.
BYWATER, R.J. (1982). Aminoglycoside antibiotics. In: Brander, G.C.,
Pugh, D.M. & Bywater, R.J. (eds.), Veterinary Applied Pharmacology and
Therapeutics, 4th edition, Balliere Tindall, London, pp. 387-393.
CARMAN, R.J. (1994). Dihydrostreptomycin MIC determinations for human
gut flora. Unpublished report from TechLab Inc., VPI Research Park,
Blacksburg, Virginia 24060, USA. Submitted to WHO by Norbrook
Laboratories Ltd., Newry, Northern Ireland.
CHRISTENSEN, E., HERTZ, H., RISKAER, N. & VRA-JENSEN, G. (1951).
Histological investigations in chronic streptomycin poisoning in
guinea-pigs. Ann. Otol., 60: 343-349.
CLARK, C.H. (1977). Toxicity of aminoglycoside antibiotics. Modern
Veterinary Practice, Part 7, 58: 594-598.
DAS, B.C., & SHARMA, T. (1983). Reduced frequency of baseline sister
chromatid exchanges in lymphocytes grown in antibiotics- and serum-
excluded culture medium. Hum Gen., 64: 249-253.
DAVIES, D.M. (1991). Textbook of adverse drug reactions. Fourth
edition, Oxford University Press, London, p. 51.
DAVIES, J., GILBERT, W., & GORINI, L. (1964). Streptomycin suppression
and the code. Proc. Nat. Acad. Sci., 51: 883-890.
DESALVA, S.J., EVANS, R.A., & MARCUSSEN, H.W. (1969). Lethal effects
of antibiotics in hamsters. Toxicol. Appl. Pharmacol., 14: 510-514.
DOLLERY, C. (1991). Therapeutic Drugs, C. Dollery (ed.), Churchill
Livingston, London, pp. 100-103.
DONALD, P.R. & SELLARS, S.L. (1981). Streptomycin ototoxicity in the
unborn child. S. Afr. Med. J., 60: 316-318.
EDISON, A.O., KUNA, S., CUCHIE, F.T. & HANSON, J.T. (1951). Relative
absorption of salts of streptomycin and dihydrosreptomycin after oral
administration. Antibiotics & Chemotherapy, 1: 49-53.
ELIAS, W.F. & DURSO, J. (1945). Blood, urine and faecal levels of
streptomycin in the treatment of human infections of E. Typhosa.
Science, 101: 589-591.
ERICSON-STRANDVIK, B. & GYLLENSTEN L. (1963). The central nervous
system of fetal mice after administration of streptomycin. Acta
Pathol. Microbiol. Scand., 59: 292-300.
ERLANSON, P., & LUNDGREN, A. (1964). Ototoxic side effects following
treatment with streptomycin, dihydrostreptomycin and kanamycin. Acta
Medica Scandinavica, 176: fasc. 2.
GAINES, S.A., ROLLINS, L.D., SILVER, R.P, & WASHINGTON, M. (1978).
Effects of low concentrations of dihydrostreptomycin on drug
resistance in enteric bacteria. Antimicrobial agents and
chemotherapy, 14: 252-256.
GOLDBERG, I.H. (1965). Mode of action of antibiotics. II. Drugs
affecting nucleic acid and protein synthesis. Am. J. Med., 39: 722-
752.
GRAHAM, B.E., VANDER BROOK, N.J. & KUIZENGA, M.H. (1946). Preliminary
studies on the absorption and excretion of streptomycin in dogs.
Science, 103: 364-365.
GRAY, J.E. & PURMALIS A. (1958). The acute toxicity of procaine
penicillin G and of dihydrostreptomycin sulfate in the pigeon and the
chicken. Avian Disease, 2: 187-196.
HAMMOND P.B. (1953). Dihydrostreptomycin dose-serum level relationship
in cattle. J. Amer. Vet. Med. Assoc., 122: 203-206.
HAWKINS, J.E. & LURIE, M.H. (1953). The ototoxicty of
dihydrostreptomycin and neomycin in the cat. Ann. Otol., 62: 1128-
1148.
HUBER, W.G. (1966). Streptomycin. In: Veterinary Pharmacology and
Therapeutics, Leo Meyer Jones (ed), 3rd edition, Iowa State College
Press, pp. 519-530.
HUEBNER, R.A., GLASSMAN, J.M., HUDYMA, G.M. & SEIFTER, J. (1956). The
toxic dose of dihydrostreptomycin in fowl. Cornell Vet., 46: 219-
212.
JAJU, M., JAJU, M., & AHUJA, Y.R. (1983). Cytogenetic effects of
chemotherapy with three combinations of anti-tubercular drugs
involving isoniazid, thiacetazone, para-amino-salicylic acid and
streptomycin on human lymphocytes: chromosome aberrations, sister
chromatids exchanges and mitotic index. Hum. Gen., 64: 42-49.
KERN, G. (1962). Zur Frage der Intrauterine Streptomycin Schadigung.
Schweiz. Med. Wochenschr., 92: 77-79.
KODAMA, F., FUKUSHIMA, F., & UMEDA, M. (1980). Chromosome aberrations
induced by clinical medicines. J. Tox. Sci., 5: 141-150.
MARSHALL, E.K. (1948). The absorption, distribution and excretion of
streptomycin. J. Pharmacol. Exper. Therapeut., 92: 43-48.
MARTINDALE, (1993). The extra pharmacopoeia. Reynolds, J.E.F. (ed.),
30th Edition, Pharmaceutical Press, pp. 159-160.
MARYNOWSKI, A., & SIANOZECKA, E. (1972). Comparison of the incidence
of congenital malformations in neonates from healthy mothers and from
patients treated for tuberculosis. Ginekol. Pol., 43: 713-715.
McGEE, T.M., & OLSZEWSKI, J. (1962). Streptomycin sulphate and
dihydrostreptomycin toxicity. Arch. Otolaryngol., 75: 295-311.
MOLITOR, H., GRAESSLE, O.E., KUNA, S., MUSHETT, C.W., SILBER, R.H.
(1946). Some toxicological and pharmacological properties of
streptomycin. J. Pharm. Exp. Ther., 86: 151-173.
NAKAMOTO, Y., OTANI, H., & TANAKA, O. (1985). Effects of
aminoglycosides administered to pregnant mice on postnatal development
of inner ear in their offspring. Teratology, 32: 34B.
NEU, R., ASPILLAGA, M.J., & GARDNER, L.I. (1965). Effects of
antibiotics on chromosomes of cultured human leucocytes. Nature
(London), 205: 171-172.
NOMURA, T., KIMURA, S., KANZAKI, T., ET AL. (1984). Induction of
tumors and malformations in mice after prenatal treatment with some
antibiotic drugs. Med. J. Osaka Univ., 35: 13-17.
OBE, G. (1970). The effect of streptomycin and dihydrostreptomycin on
human chromosomes in vitro. Molec. Gen. Genetics, 107: 361-365.
PRATT, W.B., & FEKATY, R. (1986). Bactericidal inhibitors of protein
synthesis, the aminoglycosides. In: The antimicrobial drugs, Chapter
7, Oxford University Press, Oxford, pp. 153-183.
REINBOLD, G.W., & REDDY, M.S. (1974). Sensitivity or resistance (of)
dairy starter and associated micro-organisms to selected antibiotics.
J. Milk Food Technol., 37: pp. 517-521.
RISKAER, N., CHRISTENSEN, E. & HERTZ, H. (1952). The toxic effects of
streptomycin and dihydrostreptomycin in pregnncy, illustrated
experimentally. Acta Tuber. Pneumol. Scand., 27: 211-216.
ROBINSON, C.G. & CAMBON, K.G. (1964). Hearing loss in infants of
tuberculous mothers treated with streptomycin during pregnancy.
N. Engl. J. Med., 271: 949-951.
ROLLINS, L.D., GAINES, S.A., POCURULL, D.W., & MERCER, H.D. (1975).
Animal model for determining the no-effect level of an antimicrobial
drug on drug resistance in the lactose-fermenting enteric flora.
Antimicrobial Agents and Chemotherapy, 7: 661-665.
RUDD, A.P., & SILLEY, P. (1987a). Antibiotic concentrations in cattle
serum following a single intramuscular injection of Streptopen
injection. Unpublished report No. An.H.87/R/22 from Pitman-Moore Ltd.,
Uxbridge, Middlesex, England. Submitted to WHO by Pitman-Moore, Inc.,
Mundelein, IL, USA.
RUDD, A.P., & SILLEY, P. (1987b). Antibiotic concentrations in sheep
serum following a single intramuscular injection of Streptopen
injection. Unpublished report No. An.H.87/R/27 from Pitman-Moore Ltd.,
Uxbridge, Middlesex, England. Submitted to WHO by Pitman-Moore, Inc.,
Mundelein, IL, USA.
RUDD, A.P., & SILLEY, P. (1987c). Antibiotic concentrations in dog
serum following a single intramuscular injection of Streptopen
injection. Unpublished report No. An.H.87/R/34 from Pitman-Moore Ltd.,
Uxbridge, Middlesex, England. Submitted to WHO by Pitman-Moore, Inc.,
Mundelein, IL, USA.
RUDD, A.P., & SILLEY, P. (1987d). Antibiotic concentrations in cat
serum following a single intramuscular injection of Streptopen
injection. Unpublished report No. An.H.87/R/42 from Pitman-Moore Ltd.,
Uxbridge, Middlesex, England. Submitted to WHO by Pitman-Moore, Inc.,
Mundelein, IL, USA.
SHAMBAUGH, G.E., DERLACKI, E.L., HARRISON, W.H., HOUSE, H., HOUSE, W.,
HILDYARD, V., SCHUKNECHT, H., & SHEA, J.J. (1959). Dihydrostreptomycin
deafness. JAMA, 170: 1657-1660.
SNIDER, D.E., LAYDE, P.M., JOHNSON, M.W. & LYLE, M.A. (1980).
Treatment of tuberculosis during pregnancy. Am. Rev. Resp. Dis.,
122: 65-79.
SNYDER, M. J., AL-IBRAHIM, M., & HORNICK, R. B. (1972). The effect of
oral DHS on resistance development in the intestinal microflora of
man. Unpublished report from the Division of Infectious Diseases,
Department of Medicine, University of Maryland School of Medicine.
Submitted to WHO by FDA.
STALHEIM, O.H.V. (1970). Absorption and excretion of tritiated
dihydrostreptomycin in cattle and swine. American Journal of
Veterinary Research, 31: 497-499.
STEBBINS, R.B., GRAESSLE, O.E., & ROBINSON H.J. (1945). Studies on the
absorption and excretion of streptomycin in animals. Proc. Soc. Exp.
Biol. Med., 60: 68-72.
STEVENSON, L.D., ALVORD, E.C., & CORRELL, J. W. (1947). Degeneration
and necrosis of neurones in eighth cranial nuclei caused by
streptomycin. Proc. Soc. Exp. Biol. Med., 65: 86-88.
TISDEL, M., & HARRIS, D.L. (1976). Dihydrostreptomycin: 90-day
toxicity study in guinea pigs. Unpublished report, Warf Study Code T-
615 from Warf Institute, Inc., Madison, Wisconsin, USA, on behalf of
Animal Health Institute. Submitted to WHO by FDA.
TISDEL, M., HARRIS, D.L., HAARS, R., & NEES, P.O. (1976).
Dihydrostreptomycin: 90-day toxicity study in cats. Unpublished
report, Warf Study Code T-614 from Warf Institute, Inc., Madison,
Wisconsin, USA, on behalf of Animal Health Institute. Submitted to WHO
by FDA.
TSANG, Y.C., & CHIN, T.C. (1963). Neurotoxicity of streptomycin.
Scientia Sinica, 12: 1019-1040.
VARPELA, E., HIETALAHTI, J., & ARO, M.J.T. (1969). Streptomycin and
dihydrostreptomycin medication during pregnancy and their effect on
the child's inner ear. Scand. J. Resp. Dis., 50: 101-109.
WARKANY, J. (1979). Antituberculous drugs. Teratology, 20: 133-138.
WAZETER, F. X. (1970a). Dihydrostreptomycin: Ninety-day toxicity study
in cats. Unpublished report from International Research and
Development Corporation on behalf of Animal Health Institute.
Submitted to WHO by FDA.
WAZETER, F. X. (1970b). Dihydrostreptomycin: Two-year oral toxicity
study in rats (six month interim report). Unpublished report from
International Research and Development Corporation on behalf of Animal
Health Institute. Submitted to WHO by FDA.
WAZETER, F. X. (1970c). Dihydrostreptomycin: Rabbit teratogenic study.
Unpublished report from International Research and Development
Corporation on behalf of Animal Health Institute. Submitted to WHO by
FDA.
WAZETER, F. X. (1971). Dihydrostreptomycin: Two-year oral toxicity
study in rats (18 month interim report). Unpublished report from
International Research and Development Corporation on behalf of Animal
Health Institute. Submitted to WHO by FDA.
WAZETER, F. X., & GOLDENTHAL, E.I. (1972). Dihydrostreptomycin: Two-
year oral toxicity study in rats. Unpublished report from
International Research and Development Corporation on behalf of Animal
Health Institute. Submitted to WHO by FDA.
WIGHTMAN, S.R., MANN, P.C., & WAGNER, J.E. (1980). Dihydrostreptomycin
toxicity in the Mongolian gerbil, Meriones unguiculatus. Laboratory
Animal Science, 30: 71-75.
Both dihydrostreptomycin and streptomycin are used for treatment
of bacterial infections in food-producing animals.
Dihydrostreptomycin is formed by reduction of streptomycin. As
a result, pharmacokinetic properties, toxicological profiles, and
spectrum of antimicrobial and biological activity of the two compounds
are similar. Therefore, data on the two compounds were considered
together for the purpose of establishing a single ADI. The Committee
noted that the two compounds are generally considered together in the
published literature and in the report of the twelfth meeting of the
Committee. Complete toxicological monographs were prepared for each
compound and are provided in their entirety below.
2. BIOLOGICAL DATA
2.1 Biochemical aspects
2.1.1 Absorption, distribution and excretion
2.1.1.1 Rats
The sulfate and calcium chloride complex salts of streptomycin,
and the sulfate and hydrochloride salts of dihydrostreptomycin, were
administered orally in solution to groups of 5 rats at a single dose
of 7.5 g of antibiotic base per kg bw. Heart blood was withdrawn at
0.5, 1, 2, 3, and 4 hours, and assayed microbiologically using
Staphylococcus aureus. Peak blood levels of all four compounds were
measured at 1-2 hours. Streptomycin calcium chloride complex and
dihydrostreptomycin hydrochloride were better absorbed (peak blood
levels of 3200 to 4300 µg/ml, respectively) compared to the two
sulfate salts of each compound (peak blood levels of 200-300 µg/ml).
The elimination half-lives and AUCs were not calculated for this study
(Edison et al., 1951).
2.1.1.2 Cats
Nine female cats aged 4 to 6 months and weighing approximately 2
to 3 kg were given single intramuscular injections of 10 mg/kg bw each
of penicillin G and dihydrostreptomycin. Serum levels of each drug
were assayed by microbiological agar diffusion methods up to 32 hours
after injection. Dihydrostreptomycin was assayed using Bacillus
pumilis, and penicillin was assayed using either Bacillus subtilis
or Bacillus stearothermophilus. One cat had detectable penicillin
levels in the pre-treatment sample (0.04 µg/ml). Another cat died
within two minutes of the six-hour blood sample, which was taken by
heart puncture. Death was considered to be caused by the blood
sampling method, and therefore was not treatment-related.
Peak plasma levels of approximately 25 µg/ml were reached at
approximately 1 hour. The plasma elimination half-life was
approximately 1 hour, and the AUC was 61.4 ± 15.1 µg/ml/hour.
Dihydrostreptomycin was below the limit of detection (0.6 µg/ml) in
all animals by 24 hours after injection (Rudd & Silley, 1987d).
2.1.1.3 Dogs
Ten dogs (six females, four males, aged 1.5 to 4 years and
weighing approximately 11 to 22 kg) were given single intramuscular
injections of 10 mg/kg bw each of penicillin G and
dihydrostreptomycin. Serum levels of each drug were assayed by
microbiological agar diffusion methods up to 72 hours after injection.
Dihydrostreptomycin was assayed using Bacillus pumilis, and
penicillin was assayed using either Bacillus subtilis or Bacillus
stearothermophilus.
Peak plasma levels of approximately 41 µg/ml were reached at
approximately 1 hour. The plasma elimination half-life was
approximately 1 hour, and the AUC was 74.1 ± 8.50 µg/ml/hour.
Dihydrostreptomycin was below the limit of detection (0.6 µg/ml) in
all animals by 8 hours after injection (Rudd & Silley, 1987c).
2.1.1.4 Sheep
Ten female sheep aged 15 to 18 months and weighing approximately
60 to 90 kg were given single intramuscular injections of 10 mg/kg bw
each of penicillin G and dihydrostreptomycin. Serum levels of each
drug were assayed by microbiological agar diffusion methods up to 72
hours after injection. Dihydrostreptomycin was assayed using Bacillus
pumilis, and penicillin was assayed using either Bacillus subtilis
or Bacillus stearothermophilus.
Peak plasma levels of approximately 45 µg/ml were reached at
approximately 1 hour. The plasma elimination half-life was
approximately 2 hours, and the AUC was 151.5 ± 35.9 µg/ml/hour.
Dihydrostreptomycin was below the limit of detection (0.3 µg/ml) in
all animals by 24 hours after injection (Rudd & Silley, 1987b).
2.1.1.5 Cattle
Ten cattle (one male, nine females, weighing approximately 200
to 450 kg) were given single intramuscular injections of 10 mg/kg bw
each of penicillin G and dihydrostreptomycin. Serum levels of each
drug were assayed by microbiological agar diffusion methods up to 72
hours after injection. Dihydrostreptomycin was assayed using Bacillus
pumilis, and penicillin was assayed using either Bacillus subtilis
or Bacillus stearothermophilus.
Peak plasma levels of approximately 44 µg/ml were reached at
approximately 1 hour. The plasma elimination half-life was
approximately 5 hours, and the AUC was 207.2 ± 33.8 µg/ml/hour.
Dihydrostreptomycin was below the limit of detection (0.3 µg/ml) in
all animals by 48 hours after injection (Rudd & Silley, 1987a).
Two young Holstein-Friesian steers weighing approximately 300 kg
each were injected intramuscularly with uniformly tritiated
dihydrostreptomycin (specific activity 262 mCi/mmol) plus carrier drug
at a single dose of 25 mg/kg bw, given as three separate injections
into the scapular region. Plasma, urine, saliva and lachrymal
secretions were sampled up to 5 days after the injection. The maximal
concentrations in plasma and urine were 78 and 1875 µg/ml,
respectively, and were achieved at 3-4 hours after injection. Low drug
concentrations (1.7 µg/ml) were still detectable in urine at 96 hours
after injection. No radioactivity was detected in saliva or lachrymal
secretions. The apparent volume of distribution was 23%,
corresponding to the extra-cellular fluid. The absorption and
excretion rates were similar when assayed microbiologically with
Staphylococcus aureus (Stalheim, 1970).
Dihydrostreptomycin was administered intramuscularly to 21
heifers and 6 dairy cows at 5 and 7.5 mg/lb bw (11 and 16.5 mg/kg bw),
respectively. Peak blood levels were reached at 1-2 hours after
injection and averaged approximately 45 µg/ml (with a range of 8.5-
100 µg/ml) for the 11 mg/kg bw dose, and 65.0 µg/ml (with a range of
40-122 µg/ml) for the 16.5 mg/kg bw dose. Dihydrostreptomycin was
assayed in the milk of 7 cows which had been injected with 11 mg/kg
bw. The drug was detected in 4 cows only, at concentrations ranging
from trace levels to 6.25 µg/ml, at 4 to 18 hours after injection. The
limit of detection of the assay was not stated for either blood or
milk (Hammond, 1953).
After intramuscular administration of 0.5 g dihydrostreptomycin
per 100 lb (11.1 mg/kg bw) to 26 dairy cows, drug concentrations were
detectable in the milk from 11 animals. At 36 hours milk levels were
at the limit of detection of 0.04 µg/ml for 8 cows. At 48 hours the
drug was undetectable in all animals. When administered at 1 to 2
g per 100 lb bw (22 to 44 mg/kg bw) peak levels of 0.07 to 0.12 µg/ml
were reached in milk at 24 hours, but were below the limit of
detection at 48 hours (Blobel & Burch, 1960).
2.1.1.6 Pigs
Three cross-bred barrows weighing approximately 100 kg each were
injected intramuscularly with uniformly tritiated dihydrostreptomycin
(specific activity 262 mCi/mmol) plus carrier drug at a single dose of
25 mg/kg bw/day, given as three separate injections. Plasma and urine
were sampled up to 5 days after the injection. The maximal
concentrations in plasma and urine were approximately 90 and 7100
µg/ml, respectively, and were achieved 1-2 hours after injection. Low
drug concentrations (approximately 3 µg/ml) were still detectable in
urine at 86 hours after injection. The apparent volume of distribution
was 21%, corresponding to the extracellular fluid. The absorption and
excretion rates were similar when assayed microbiologically with
Staphylococcus aureus (Stalheim, 1970).
The results of the foregoing studies are summarized in Table 1.
2.1.1.7 Humans
As a class, aminoglycoside antibiotics cross membranes very
poorly and only about 1% of an oral dose is absorbed, even when there
is intestinal inflammation or ulceration (Pratt & Fekaty, 1986).
Dollery (1991) reported that after oral administration of
streptomycin, 60%-100% of the drug can be recovered unchanged from the
faeces.
Table 1. Pharmacokinetics parameters for dihydrostreptomycin after intramuscular administration to various species
(Values represent ± standard deviation or range)
Species Dose (i.m.) Cmax (plasma) Tmax hours AUC mcg/ Cmax urine t´ hours Vd Reference
(mg/kg bw) (µg/ml) (ml/hour) (µg/ml)
Cats 10 25.1 ± 8.6 1.2 ± 0.4 61.4 ± 15.1 - 1.4 ± 0.1 - Rudd & Silley, 1987d
Dogs 10 41.2 ± 8.07 0.8 ± 0.26 74.1 ± 8.50 - 1.0 ± 0.17 - Rudd & Silley, 1987c
Sheep 10 44.8 ± 14.3 0.8 ± 0.3 151.5 ± 35.9 - 2.3 ± 0.3 - Rudd & Silley, 1987b
Cattle 10 44.3 ± 15.2 1.1 ± 0.4 207.2 ± 33.8 - 4.9 ± 0.5 - Rudd & Silley, 1987a
Cattle 11 44.7 (8.5-100) 1 - 2 - - - - Hammond, 1953
Cattle 16.5 65.0 (40.0-122) 1 - 2 - - - - Hammond, 1953
Cattle 25 78 3 - 4 - 1875 - 23% Stalheim, 1970
Pigs 25 87 1 - 2 - 7120 - 21% Stalheim, 1970
The aminoglycosides are reported to have a volume of distribution
of 25% of lean body mass in adults, corresponding to the extracellular
fluid volume. The volume of distribution in neonates may average 60%
of body weight. The volume of distribution in obese individuals is
less than in those with normal body weight. The volume of distribution
also varies with edema, which tends to reduce serum concentrations,
and dehydration which increases serum concentrations. The presence of
fever reduces serum concentrations by up to 40%, due to increased
renal blood flow and glomerular filtration.
Aminoglycosides accumulate in the kidney relative to plasma
levels, and detectable concentrations of aminoglycosides persist in
urine for several weeks, suggesting binding of the drug to kidney.
Accumulation also occurs in the perilymph of the inner ear, where the
elimination half-life is much longer than in serum (10-12 hours in
perilymph compared to 2 hours in serum).
Aminoglycoside levels in interstitial fluid approximate serum
levels. In bile, 25-50% of serum levels are obtained in the absence of
biliary obstruction. In sputum and bronchial secretions 25-67% of
serum levels may be achieved; in pericardial, pleural and ascitic
fluids approximately 50% of serum levels are obtained; and synovial
fluid may contain 50-100% of serum levels. Penetration into the eye,
cerebrospinal fluid and ventricular fluid is very poor. Placental
transfer occurs and fetal serum concentrations range from 20-40% of
maternal serum levels (Pratt & Fekaty, 1986).
Approximately 20% of a parenteral dose of streptomycin cannot be
accounted for in urine, but no metabolites have yet been identified.
Approximately 1% is excreted in bile (Dollery, 1991).
The excretion rate after parenteral administration of
amino-glycosides is dependent on renal function and is linearly
related to the creatinine clearance rate. The elimination half-life in
adults is 2 hours, but 5-6 hours in neonates due to their lower
glomerular filtration rate (Pratt & Fekaty, 1986).
2.1.2 Biotransformation
The aminoglycosides are reported not to be metabolized in humans
and are excreted in their active forms by glomerular filtration (Pratt
& Fekaty, 1986).
2.1.3 Effects on enzymes and other biochemical parameters
No information available
2.2 Toxicological studies
2.2.1 Acute toxicity studies
2.2.1.1 Mice
The oral LD50 of different dihydrostreptomycin salts was compared
in male Carworth CF1 mice weighing 20 g on average.
Dihydrostreptomycin hydrochloride gave an LD50 of 12 500 mg/kg bw,
whereas the sulfate salt gave an LD50 of greater than 30 000 mg/kg bw
(Edison et al., 1951).
2.2.1.2 Chickens
The LD50 for dihydrostreptomycin sulfate administered
intramuscularly to groups of fifty 1, 2, 3, or 4 week-old chicks was
743, 1090, 1738, and 1868 mg/kg bw, respectively. Clinical signs of
toxicity in all birds were depression, drooping wings, closed eyes,
muscular weakness and slowed respiration (Huebner et al., 1956).
Dihydrostreptomycin sulfate was administered intramuscularly to
groups of 3 white Leghorn chickens weighing 600 g, at doses of 800 to
2500 mg/kg bw. Clinical signs of toxicity included ataxia,
prostration, gasping, and coma. The LD50 was 2167 mg/kg bw (Gray &
Purmalis, 1958).
2.2.1.3 Pigeons
Dihydrostreptomycin sulfate was administered intramuscularly at
doses of 400 to 1000 mg/kg bw to groups of 5 racing pigeons weighing
an average of 360 g. Clinical signs of toxicity included emesis,
somnolence, ataxia, depression, and coma. The LD50 was determined as
715 mg/kg bw (Gray & Purmalis, 1958).
2.2.1.4 Gerbils
A group of 10 gerbils (5/sex), 7-10 weeks of age and weighing
55-65 g were given single intramuscular injections of 50 mg
dihydrostreptomycin sulfate (equivalent to 769-909 mg/kg bw).
Ascending flaccid paralysis was observed in 10/10 animals at 2 to 5
minutes after injection, and 8/10 animals died within 4 to 25 minutes
after injection. The 2 surviving animals gradually regained muscle
control and awareness with apparently complete recovery at 65 and 120
minutes post-injection, respectively (Wightman et al., 1980).
The results of acute toxicity studies on dihydrostreptomycin are
summarized in Table 2.
Table 2. Acute toxicity of dihydrostreptomycin
Species Number Route LD50 mg/kg bw Reference
(age/weight) (salt)
Mice - oral >30 000 Edison et al., 1951
(20g) (sulfate)
12 500
(hydrochloride)
Chickens 50/group i.m. 743 - 1868 Huebner et al., 1956
(1-4 weeks) (sulfate)
Chickens 3/group i.m. 2167 Gray & Purmalis,
(600g) (sulfate) 1958
Pigeons 5/group i.m. 715 Gray & Purmalis,
(360g) (sulfate) 1958
Gerbil 10 i.m. < 769 Wightman et al., 1980
(7-10 weeks,
55-65g)
2.2.2 Short-term toxicity studies
2.2.2.1 Guinea-pigs
Three groups of 30 young adult guinea-pigs (15/sex/group) were
treated for 90 days with either 40 mg dihydrostreptomycin/kg bw/day in
distilled water by gavage, an equal volume of distilled water alone by
gavage (negative control), or 200 mg kanamycin/kg bw/day, s.c.
(positive control).
The kanamycin-treated animals exhibited spastic twitching
immediately after dosing, injection site reactions and some animals
became ataxic. Body-weight gain was depressed in the kanamycin group,
but was comparable to controls in the dihydrostreptomycin group.
Auditory function was assessed using the pinna twitch reflex
(Preyer reflex) in response to a whistle. Hearing loss was observed in
all the animals in the kanamycin group after week 6, and in two
negative control animals after weeks 7 to 9, which were later found to
be suffering from an inner ear infection. No hearing loss was observed
in the dihydrostreptomycin treated animals.
A large number of animals died during the study (7 negative
controls, 6 positive controls, and 6 treated with
dihydrostreptomycin). These were necropsied, as were all surviving
animals at the end of the study. All tissues with observed gross
lesions, plus the organ of Corti from all animals, were examined
histologically.
Of the animals treated by gavage, several animals died of a
ruptured oesophagus (3 negative controls and 3 in the
dihydrostreptomycin group). Almost all of the remaining animals dying
on test had lesions of the lungs due to pneumonia.
The authors reported that because the organs of Corti were
inadequately preserved they showed signs of degeneration,
histologically. However, the architecture of the cell layers and the
hair cells were still discernible. The positive control animals
(kanamycin group) demonstrated either no hair cells at any level of
the cochlea, or very few and damaged hair cells. The majority of
dihydrostreptomycin-treated animals had hair cells with largely normal
architecture, although hair cell damage was noted as being more severe
in males than females treated with dihydrostreptomycin (Tisdel &
Harris, 1976).
2.2.2.2 Cats
Dihydrostreptomycin was administered orally in a food vehicle
(liver cat food) to 3 groups of 10 cats (5/sex/group) weighing between
1.5 and 4.6 kg, for 90 days at doses of 1, 5 or 10 mg/kg bw/day. Ten
cats of each sex were used as controls.
One male cat in the mid-dose group died during the ninth week of
treatment. A watery red urethral discharge and a distended bladder
were observed in this animal the day prior to death, and pathological
examination revealed acute cystitis with concomitant peritonitis. All
other cats survived the 90 days of treatment and no compound-related
effects were observed on body-weight gain, food consumption,
haematology, blood chemistry, urinalysis, gross pathology or
histopathology (only liver and kidneys of controls and 10 mg/kg/day-
treated cats were examined) (Wazeter, 1970a).
Vestibular function was assessed in 10 cats (5/sex) treated daily
with oral doses of 40 mg dihydrostreptomycin/kg bw/day for 90 days.
Streptomycin sulfate was used as the positive control (200 mg/kg
bw/day, s.c.). Animals in the negative control group were
administered water by gavage.
Three cats died, one in each of the negative control, positive
control, and dihydrostreptomycin groups, due to urinary obstruction
which was considered unrelated to treatment.
For the dihydrostreptomycin group, no treatment-related effects
were observed on body weight, haematology, blood chemistry,
ophthalmoscopic examination, bone marrow smears, or gross pathology.
Vestibular function remained normal throughout the treatment period
based on results of righting reflex tests in which animals were
dropped from an inverted position two feet above a cushioned mat. The
NOEL was 40 mg/kg bw/day dihydrostreptomycin in this study. The
results with streptomycin are described in section 2.2.2.5 of the
monograph on streptomycin (Tisdel et al., 1976).
2.2.2.3 Sheep
A target animal safety study was conducted with
dihydro-streptomycin in 3 groups of 4 sheep (2/sex/group) aged 13 to
16 months and weighing approximately 45 kg to 70 kg. Animals were
treated with daily intramuscular injections of 10 mg procaine
penicillin G plus 10 mg dihydrostreptomycin/kg bw/day for 5
consecutive days (the recommended therapeutic treatment regime), the
second group received 30 mg of each drug/kg bw/day for 5 days, and the
third group received 10 mg of each drug/kg bw/day for 15 days. A
treatment-free control group was not included, although pre-treatment
parameters were measured in each animal.
Behaviour was normal and there were no clinical signs of
neuromuscular blockade. No localized injection site reactions were
observed. Pathological changes observed in skeletal muscle and liver
at post-mortem examination were largely due to parasitic infestations.
Slight congestion/consolidation was observed in the lungs at necropsy,
which was not examined further. There was no evidence of ototoxicity
based on results of a crude hearing test and normal histology of the
VIIIth cranial nerve. There was no pathological evidence of
nephrotoxicity at post-mortem examination. Urinalyses were not
performed.
Some haematological and biochemical parameters were altered
during and after treatment. Differences reached statistical
significance in some groups compared with pre-treatment values,
whereas other parameters were altered then subsequently recovered to
pre-treatment values. The haematological changes included a reduction
in haemoglobin, red cells, haematocrit and mean cell volume.
Biochemical changes included a decrease in sodium, phosphorus,
creatinine, and bilirubin, and an increase in chloride. The only
consistent dose-related trends were decreased sodium and increased
chloride levels during prolonged treatment (15-day group), and a lower
haematocrit in all treatment groups. These changes, although
statistically significant were small and were considered by the
authors not to be clinically relevant (Brooks & Rolph, 1989b).
2.2.2.4 Pigs
A target animal safety study was conducted with
dihydrostreptomycin in 3 groups of 4 pigs (2/sex/group in groups 2 and
3, 1 female and 3 males in group 1) approximately 8 weeks of age and
weighing between 23 and 29 kg. Animals were treated with daily i.m.
injections of 10 mg procaine penicillin G plus 10 mg
dihydrostreptomycin/kg initial bw/day for 5 consecutive days (the
recommended therapeutic treatment regime, group 1), the second group
received 30 mg of each drug/kg initial bw/day for 5 days (group 2),
and the third group received 10 mg of each drug/kg initial bw/day for
15 days (group 3). An untreated control group was not included,
although pre-treatment parameters were measured in all animals.
Body weights increased rapidly in all groups (in group 3 body
weights had increased by 50% after 15 days). Therefore the dose
administered on a body-weight basis was reduced with time,
particularly in group 3. A crude hearing test revealed no auditory
impairment, and behaviour was normal, except for 2 animals in group 3
that showed symptoms that were attributed to stress (vomiting,
inactivity, haematemesis and slight cyanosis of ears and legs) on days
1 and 15, respectively.
Changes were observed compared with pretreatment values in
haematology and serum chemistry values (reduced haemoglobin, red cells
and haematocrit, reduced neutrophils, increased mean corpuscular
haemoglobin, decreased creatinine, and increased calcium), some of
which reached statistical significance. However, there were no obvious
drug-related or time-related trends, and although statistically
significant, the changes were small and were considered by the authors
not to be clinically relevant.
The VIIIth cranial nerve was histologically normal in all but one
animal in group 1 in which focal chronic inflammation was observed.
Focal interstitial nephritis was observed in one pig in group 1 and
two pigs in group 2. These effects were not considered by the authors
to be treatment-related. No local injection site reactions were
observed (Brooks et al., 1989).
2.2.2.5 Cattle
A target animal safety study was conducted with
dihydrostreptomycin in 3 groups of 4 cattle (2/sex/group),
approximately 6 months of age and weighing between 100 and 170 kg.
Animals were treated with daily i.m. injections of 10 mg procaine
penicillin G plus 10 mg dihydrostreptomycin/kg bw/day for 5
consecutive days (the recommended therapeutic treatment regime), the
second group received 30 mg of each drug/kg bw/day for 5 days, and the
third group received 10 mg of each drug/kg bw/day for 15 days. An
untreated control group was not included, although pre-treatment
parameters were measured in each animal.
No consistent treatment-related effects on haematological or
biochemical parameters were observed. Behaviour was normal and there
were no clinical signs of neuromuscular blockade. The few injection
site reactions that were observed were minor in nature. The only
pathological changes present in tissues and organs at post-mortem
examination were in the lungs, which were attributed to respiratory
tract infection. There was no evidence of ototoxicity based on results
of a crude hearing test and normal histology of the VIIIth cranial
nerve. There was no histological evidence of nephrotoxicity at
post-mortem examination. Urinalyses were not performed (Brooks &
Rolph, 1989a).
2.2.3 Long-term toxicity/carcinogenicity studies
2.2.3.1 Rats
Dihydrostreptomycin was administered in the diet to Charles River
CD rats, (35/sex/group), to achieve dosages of approximately 1, 5, or
10 mg/kg bw/day for up to 2 years (dietary concentrations were
adjusted weekly to compensate for changes in food consumption and body
weight). Two control groups were included in the study. Five
rat/sex/group were scheduled for interim kills at 6 and 12 months. The
remaining 25 animals/sex/group were administered dihydro-streptomycin
for 2 years. Interim study reports were submitted at 6 and 18 months,
and a final report at 2 years.
In the 6-month interim report, it was reported that 2 rats died
in the low-dose group during the first week of treatment (cause of
death unknown), and were replaced. One male control rat died after its
6-month blood sample was taken. There were no treatment-related
effects observed on food consumption, haematology or urinalysis
(analyses from 5 rats/ sex/group at 3 and 6 months), hearing or
vestibular function (measured in all rats at 3 and 6 months). Serum
chemistry was not evaluated in this study. Body weights were slightly
decreased in males in all treatment groups compared with controls,
which reached statistical significance for all groups; however, no
clear dose-response relationship was established. One male rat in the
5 mg/kg bw/day group had a grossly abnormal posture from the seventh
treatment onwards, and was found to have severe bilateral suppurative
otitis media when necropsied at 6 months. One to two rats in all
treated groups, but no controls, were also reported to have this
condition at the 6 month necropsy when 5 animals per sex/group were
killed. No other treatment-related effects were noted on gross
pathology or histopathology. Histological examination of the auditory
system or associated nerves was not performed (Wazeter, 1970b).
In the 18-month interim report, the body weights of male rats in
the high-dose group were significantly reduced when compared to
control group 1 but not control group 2. Body weights in all other
male treatment groups were comparable to controls. No
treatment-related effects were observed on food consumption,
haematology, or urinalysis. No effects were reported on hearing or
vestibular function as defined by the tests used. One female rat in
the high-dose group had an abnormal posture and occasional slowed
righting reflex from week 73 onwards, and two males in the mid-dose
group had "impaired use of the hindquarters" from week 64 onwards, one
of which subsequently died in week 69. Mortality rates were similar
for all treatment and control groups at 78 weeks, ranging from 0 to 4
deaths per group of 25 animals. None of the deaths were considered by
the author to be treatment-related. Causes of death were reported as
due primarily to spontaneous neoplasias (usually of the pituitary or
mammary glands) and infectious processes; however, no gross pathology
or histopathology data were provided with the report (Wazeter, 1971).
In the two-year report, 12 to 17 out of 25 rats/sex in treated
groups had survived up to two years. No treatment-related effects were
observed on survival, food consumption, urinalysis, haematology, or
hearing. Body-weight gain was reduced in males in the high-dose group
compared to control group 2, but not control group 1. Body weights
were comparable to controls in all other groups. Vestibular function
was impaired in both control and treated groups (inability to remain
on a bar or abnormal gait was observed in 5 control rats, 2 rats each
in the low- and mid-dose groups, and 3 rats in the high-dose group, no
sex differences were observed). On necropsy, 2 rats in the high-dose
group had gross lesions of the middle ear (purulent otitis media). All
other gross pathological changes and histopathological changes
(examined in controls and high-dose group only) occurred with similar
frequency in all rats examined at two years. Neoplasms were observed
with comparable frequency in both treatment and control groups and
were similar to the historical control incidence for this facility.
Although this study did not meet current standards regarding the
number of animals started on the two-year phase of the study
(25/sex/group), the Committee concluded that survival of more than 50%
of all treated animals in the 2-year phase of the study (24/50, 33/50,
and 29/50 in the low-, mid-, and high-dose groups, respectively),
represented an adequate test of the carcinogenic potential of the
compound. The NOEL was 5 mg/kg bw/day based on decreased body-weight
gain in males at the high dose (Wazeter & Goldenthal, 1972).
2.2.4 Reproductive toxicity studies
No information available
2.2.5 Special studies on embryotoxicity/teratogenicity
2.2.5.1 Guinea-pigs
Streptomycin and dihydrostreptomycin were administered by daily
i.m. injection to groups of 2 to 4 pregnant guinea-pigs at doses of
10, 25, 50, 100 or 200 mg/kg bw/day. The duration of the treatment
period was not stated. A dose of 100-200 mg/kg bw/day of both drugs
caused abortion or death within 8-10 days. All fetusus were macerated,
indicating that death occurred prior to abortion or death of dams. At
doses of 25-50 mg/kg bw/day, some animals aborted, some survived, and
some stillbirths were observed. A dose of 10 mg/kg bw/day for 24 days
caused no abortions. The surviving F1 animals were clinically normal
with respect to vestibular and auditory function, and the CNS was
normal on histological examination. The placentae from streptomycin-
or dihydrostreptomycin-treated animals showed marked hyperaemia,
haemorrhage, and endometrial necrosis 24 hours after a single
intramuscular dose of 100 mg/kg bw. These changes progressed with
further treatment. Serum concentrations of dihydrostreptomycin and
streptomycin measured in the fetus were 2-4% of those in the dams
(Riskaer et al., 1952).
2.2.5.2 Rabbits
Groups of 31, 23, and 26 pregnant female Dutch rabbits, weighing
approximately 2 to 4 kg, were treated by oral intubation with 0, 5, or
10 mg dihydrostreptomycin/kg bw/day, respectively, from days 6 to 18
of gestation. The vehicle control group received 0.5% aqueous
methylcellulose.
One rabbit in the 5 mg/kg bw/day group was found dead on
gestation day 10. Four control rabbits and 1 in the 10 mg/kg bw/day
treatment group aborted, all after gestation day 14. No
treatment-related effects were observed on maternal behaviour,
appearance, or body-weight gain. On day 30, all animals were killed
for pathological examination. There were no treatment-related effects
on the pregnancy rate, number of corpora lutea, number of viable
fetuses, percentage of abnormal fetuses, litter size, mean fetal body
weight, or 24-hour survival rate. The number of abortions and
resorptions/empty implantation sites were higher in controls compared
to treated groups. Presence of a 13th rib was a frequently noted fetal
abnormality; however the incidence was similar in all groups. One
control fetus was acephalic with a ventral hernia, and one fetus in
the 5 mg/kg bw/day group had agenesis of skin and soft tissue over the
left lateral nasal and buccal area, and absent hind claws. All of
these findings were considered by the authors as unrelated to
treatment.
Because no maternal toxicity was observed, the Committee
concluded that the dose levels may not have been high enough to fully
exclude teratogenic potential (Wazeter, 1970c).
2.2.5.3 Humans
Auditory toxicity has been reported in children whose mothers
were treated with streptomycin and dihydrostreptomycin during
pregnancy. However, details of the dose administered and the timing
in relation to the pregnancy are often not stated (Davies, 1991;
Robinson & Cambon, 1964; Snider et al., 1980; Varpela et al.,
1969; Warkany, 1979).
Organogenesis of the inner ear occurs at week 7 of pregnancy, and
cochlear development continues up to mid-term (Varpela et al.,
1969). It is the only organ in the body to reach full adult size and
complete differentiation by midterm (Robinson & Cambon, 1964).
However, unlike teratogens, the toxic effects of streptomycin and
dihydrostreptomycin on the fetus are independent of the critical
periods of embryogenesis. Ototoxicity can occur throughout the
gestation period (Snider et al., 1980), as well as in adults (see
effects in humans, section 2.3.1 below). In children of streptomycin-
and dihydrostreptomycin-treated mothers, as well as in adults,
high-tone hearing is primarily affected first, which is outside of the
range of normal speech frequencies (Donald & Sellars, 1981).
The results of a literature review of pregnancy outcomes in women
receiving streptomycin or dihydrostreptomycin for tuberculosis is
presented by Snider et al., 1980. Of a total of 203 women, 206
pregnancies were followed to term. Seventy-two women received
streptomycin or dihydrostreptomycin during the first 4 months of
pregnancy, 73 women received one or the other after the fourth month,
and the timing was unknown for 61 women. The dose of streptomycin or
dihydrostreptomycin administered in these cases, where stated, was
between 1 g to 2 g daily or twice weekly, with total doses ranging
from 2 g to 202 g. Several other drugs were administered concomitantly
for tuberculosis, i.e. 88 women also received isoniazid, 1 received
rifampicin, 1 received ethambutol, 83 received p-amino-salicylic acid,
and for 59 women the other drug was not known. There were 2
spontaneous abortions, no premature births and no stillbirths, and 170
normal term infants were delivered. Abnormalities were observed in 35
infants (a rate of 169 per 1000, roughly 1 in 6, is reported by the
authors). The majority of these consisted of vestibular dysfunction
and varying degrees of hearing loss. Hearing loss occurred in the
high-tone range first, i.e. before the range of normal speech
frequencies was affected. No other abnormalities were reported (Snider
et al., 1980).
2.2.6 Special studies on genotoxicity
Streptomycin and dihydrostreptomycin bind to and alter the
configuration of the 30S subunit of ribosomes, thus inhibiting protein
synthesis and causing misreading of the genetic code. RNA and DNA
synthesis are unaffected (Goldberg, 1965; Davies et al., 1964).
The results of genotoxicity assays with dihydrostreptomycin are
summarized in Table 3.
Table 3. Results of genotoxicity assays on dihydrostreptomycin
Test system Test object Concentration Results Reference
In vitro
Cytogenetics Human lymphocytes 4.7-13.7 mg/ml Negative Obe, 1970
2.2.7 Special studies on immune responses
The incidence of allergic reactions in humans to systemically
administered aminoglycosides is reported to be very low (Pratt &
Fekaty, 1986).
2.2.8 Special studies on ototoxicity
2.2.8.1 Cats
The ototoxicity of streptomycin and dihydrostreptomycin was
investigated in cats after they had recovered from surgical
destruction of one ear. Seven cats were treated with streptomycin at
doses and treatment periods ranging from 200 mg/kg bw/day for 9.5 days
to 25 mg/kg bw/day for 84 days. Six cats were treated with
dihydrostreptomycin at doses and treatment periods ranging from 300
mg/kg bw/day for 21 days to 100 mg/kg bw/day for 60 days. After the
last dose, animals were kept treatment-free for 1 year then necropsied
for histopathological examination of the inner ear and the brain stem
nuclei.
Clinical signs of ototoxicity were similar in both groups, which
included permanent high frequency hearing loss, loss of
post-rotational nystagmus, and ataxia. Weight loss was also noted as
a treatment-related effect in both groups. With dihydrostreptomycin
treatment, the hearing loss was delayed and occurred several weeks to
several months after treatment.
In the inner ear, loss of hair cells in the cochlea, and damage
to the sensorimotor epithelium and hair loss in the cristae of the
vestibular canals were observed. The cristae appeared to be more
susceptable to toxic effects than the maculae of the saccule and
utricle.
In the brain stem, no lesions were found in the vestibular
nuclei. The vestibular portion of the VIIIth nerve was normal,
despite the fact that the sensorimotor epithelium and supporting cells
of the vestibular apparatus had been destroyed (surgically on one
side, and due to streptomycin and dihydrostreptomycin treatment on the
other side).
Effects observed in the brain stem included degenerative changes
in the ventral and dorsal cochlear nuclei, occurring primarily in
those parts corresponding to the ear which had been surgically
destroyed. In 2 animals treated with streptomycin, these lesions were
observed on the side corresponding to the ear which had not been
destroyed surgically. In these 2 animals, degeneration of the spiral
ganglion was also observed.
The authors described these degenerative changes as being typical
of trans-synaptic atrophy. The nuclei were smaller, containing smaller
nerve cells arranged more compactly, and changes were observed in the
myeloarchitecture. The cochlear branch of the VIIIth nerve appeared
shrunken with only a few myelinated fibres. There were no lesions in
the cerebellum or any other part of the brain stem.
The authors concluded that the lesions produced by both
streptomycin and dihydrostreptomycin were limited to the vestibular
end-organ of the inner ear in cats (McGee & Olszewski, 1962).
Dihydrostreptomycin was administered subcutaneously to groups of
2 cats at a dose of 800 mg/kg bw/day for 15 days or 200 mg/kg bw/day
for 120 days. Moderate to severe ataxia was observed from days 8 and
10 in the 800 mg/kg bw/day group, and from days 28 and 78 in the 200
mg/kg bw/day group. Animals were necropsied at the end of the
treatment period and the inner ear examined. Scattered degeneration of
the hair cells was observed in the cristae of the horizontal
semicircular canals, and was more severe in the high-dose group. The
cochlea of dihydrostreptomycin-treated cats was comparable to controls
as judged by electrophysiological studies of voltage changes at the
round window in response to tones of varying frequencies. The authors
reported that streptomycin produced more severe vestibular and
cochlear changes in a previous study than those produced by
dihydrostreptomycin; however, the doses of streptomycin used were not
stated. The authors also reported that cochlea of the cat appears to
be more sensitive to streptomycin than dihydrostreptomycin, whereas
the opposite is true in humans (Hawkins & Lurie, 1953).
2.2.9 Special studies on microbiological effects
2.2.9.1 Hamsters
Groups of 6 hamsters were fed a diet containing 0 or 10 mg/kg
dihydrostreptomycin. After 47 days, oxytetracycline (10 mg/kg) was
added to the diet and a suspension of E. coli (106 organisms/ml)
susceptible to both drugs was added to the drinking-water for two
weeks. Faecal samples were collected throughout the study and analyzed
for lactose-fermenting enteric organisms resistant to either
dihydrostreptomycin or oxytetracycline. No dihydrostreptomycin- or
oxytetracycline-resistant organisms were detected in the faeces at any
time (Rollins et al., 1975).
2.2.9.2 Dogs
Groups of 5 beagle dogs with an average weight of 15 kg were fed
a diet containing 0, 2, or 10 mg dihydrostreptomycin per kg of feed
(equivalent to 50 or 250 µg/kg bw/day) for 35 days. In both treatment
groups there was a shift in the faecal flora from predominantly
dihydrostreptomycin-susceptible lactose fermenting coliforms to a
resistant population after 15 days, which was significant (p < 0.01)
in both groups. This persisted throughout the 28-day post-treatment
phase of the study. A definitive response was not seen in the control
group. The authors concluded that the NOEL for development of drug
resistance in enteric bacteria was less than 2 mg/ kg of diet,
equivalent to 50 µg/kg bw/day (Gaines et al., 1978).
2.2.9.3 Humans
Healthy human volunteers were treated with 0.75 mg of
dihydrostreptomycin administered orally in a hamburger patty, 4 days
per week, for 7 weeks. Faecal samples were examined weekly for the
presence of coliforms bearing R-factor mediated resistance to
dihydrostreptomycin. The presence of resistant coliforms fluctuated
from week to week in about 30% of untreated controls. Fluctuations
were also observed in treated subjects. Four of 25 treated subjects
and 6/29 controls never excreted resistant coliforms; however, when
resistant coliforms were acquired, they tended to persist longer and
to multiply to greater numbers in the presence of dihydrostreptomycin
than in controls (Snyder et al., 1972).
2.2.9.4 Dairy starter cultures
Five strains each of various bacterial species were tested for
their sensitivity to dihydrostreptomycin by measuring zones of
inhibition of bacterial growth around discs impregnated with 2 or 10
µg/disc. The bacteria used were strains of Streptococcus (S.
lactis, S. cremoris, S. diacetilactis, S. thermophilus, S. durans, S.
faecalis) Lactobacillus bulgaricus, Brevibacterium linens,
Leuconostoc dextranicum, Staphylococcus (S. aureus, S. epidermidis),
and Micrococcus varians. All were susceptible except all
strains of Streptococcus faecalis and 3/5 strains of Streptococcus
durans (Reinbold & Reddy, 1974).
2.2.9.5 Minimum inhibitory concentrations in vitro
The minimum inhibitory concentration (MIC) of dihydrostreptomycin
sulfate was determined in vitro for bacteria isolated from the
intestines or faeces of healthy human adults. Over 100 isolates were
tested which represented 17 species and covered the 10 most common
genera of human intestinal microbes. The methods and controls used
were those proposed by the National Council for Clinical Laboratory
Standards (NCCLS) describing MIC assays for anaerobic bacteria.
E. coli was additionally assayed under aerobic conditions. The agar
dilution method was used, with Wilkins Chalgren agar or BHI agar
supplemented with 5% rabbit's blood, and incubations were for 48 hours
at 37 ± 2 °C. Dihydrostreptomycin was tested at serial double
dilutions from 128 µg/ml to 2 µg/ml. At each concentration, bacterial
cells were tested at two densities, 1 x 105 cells per spot, which is
recommended by NCCLS for clinical isolates, and 1 x 107 cells per
spot, which is considered to be more representative of the bacterial
concentration within the intestinal ecosystem. The results of this
study are summarized in Table 4.
Bifidobacterium spp. were found to be the most sensitive. Data
available for 5 strains of Bifidobacterium adolescentis gave an
MIC50 value of 32 µg/ml and a MIC range of 16-64 µg/ml, and data on
5 strains of Bifidobacterium longum gave an MIC50 value of 16 µg/ml
and a MIC range of 8-32 µg/ml.
The MIC50 value for dihydrostreptomycin in most of the other
bacterial species tested (17 bacterial species, with 5-11 strains
tested per species) was higher than 32 µg/ml, with the highest MIC50
values being more than 128 µg/ml.
An MIC50 value of 32 µg/ml was therefore established as the
concentration without effect on the human gut flora (Carman, 1994).
Table 4. MIC values for bacterial isolates from human intestinal material
(All values represent mcg/ml)
Species 1 x 107 cells / spot 1 x 105 cells / spot
n = no. of strains MIC50 MIC90 Range MIC50 MIC90 Range
E. coli 16 64 8-64 16 32 8-64
(aerobic) n=11
E. coli 64 128 32->128 32 64 16-128
(anaerobic) n=11
Bacteroides vulgatus >128 >128 128-128 >128 >128 64->128
n=5
Bacteroides uniformis >128 >128 >128 >128 >128 >128
n=5
Bifidobacterium 32 64 16-64 32 32 8-32
adolescentis
n=5
Bifidobacterium 16 32 8-32 16 16 8-32
longum n=5
Lactobacillus >128 >128 64->128 128 >128 32->128
acidophilus n=10
Fusobacterium >128 >128 128->128 >128 >128 128->128
russi n=5
Fusobacterium >128 >128 128->128 >128 >128 64->128
prauznitii n=5
Peptostreptococcus >128 >128 64->128 >128 >128 64->128
DZ n=5
Peptostreptococcus >128 >128 128->128 >128 >128 128->128
productus 1 n=5
Ruminococcus 64 64 64 64 64 32-64
gnavus n=5
Ruminococcus 64 64 64-128 64 64 64
bromii n=5
Table 4 (contd)
Species 1 x 107 cells / spot 1 x 105 cells / spot
n = no. of strains MIC50 MIC90 Range MIC50 MIC90 Range
Eubacterium >128 >128 128->128 >128 >128 64->128
aerofaciens n=5
Eubacterium >128 >128 >128 >128 >128 128->128
rectale n=5
Coprococcus 64 64 64-128 32 64 32-64
eutactus n=5
Coprococcus 64 64 32-64 32 64 32-64
comes n=5
Gemmiger 64 128 64->128 64 128 32->128
formicilis n=10
2.3 Observations In humans
2.3.1 Ototoxicity
The aminoglycosides are all potentially toxic to the inner ear at
therapeutic doses. Streptomycin-induced ototoxicity primarily affects
the vestibular system before auditory function is affected, whereas
dihydrostreptomycin primarily affects the cochlea before vestibular
function is affected. With both streptomycin and dihydrostreptomycin
hearing loss occurs in the high tone range first, i.e. before the
range of frequencies associated with normal speech is affected
(Martindale, 1993; Davies, 1991; Shambaugh et al., 1959; Hawkins &
Lurie, 1953; Pratt & Fekaty, 1986).
The primary toxic effect of both streptomycin and
dihydrostreptomycin is on the peripheral sensory portions of the inner
ear rather than on the eighth cranial nerve itself, which results in
progressive destruction of the hair cells of the Organ of Corti from
the basal region (responsive to high-frequency sounds) to the apex of
the cochlea (responsive to low-frequency sounds) as dosage and
duration of treatment are increased (Davies, 1991).
Dihydrostreptomycin causes delayed ototoxicity in humans
manifested as a sensorineural hearing loss which may involve any or
all frequencies. Hearing loss may occur from 1 to 6 months after drug
treatment, it is permanent, and it is not related to the size of the
dose (McGee & Olszewski, 1962; Shambaugh et al., 1959).
Aminoglycosides, including streptomycin and dihydrostreptomycin,
accumulate in the perilymph of the inner ear (Davies, 1991). A large
proportion of both drugs are excreted unchanged by the kidneys (Pratt
& Fekaty, 1986), and the risk of ototoxicity is therefore increased
when renal function is compromised (Erlansen & Lundgren, 1964).
Patients presenting with ototoxic side effects after treatment
with streptomycin, dihydrostreptomycin or kanamycin, for various
clinical conditions, were studied in a retrospective study. The route
of administration was not stated, although it was probably
intramuscular injection.
Two patients receiving a 50:50 mixture of streptomycin and
dihydrostreptomycin at doses of 0.5 or 1.0 mg/kg bw/day of each drug
(total dose 5 or 14.5 g of each drug) reported vertigo at the end of
the course of treatment. Four patients receiving dihydro-streptomycin
at a dose of 1 g per day (equivalent to 14 to 20 mg/kg bw/day, total
dose 6 to 36 g) reported tinnitus or impaired hearing (as assessed by
tone audiometry) between 2 weeks and 3 months after the course of
treatment. None of the patients in this group reported vertigo. Three
of these patients had impairment of renal function which may have
increased blood levels of dihydrostreptomycin and hence increased the
risk of ototoxicity. It was not stated whether the renal impairment
was pre-existing or caused by dihydrostreptomycin treatment (Erlanson
& Lundgren, 1964).
Dihydrostreptomycin has been reported to be more likely to cause
partial or complete hearing loss than streptomycin and was therefore
not recommended for use in humans (Martindale, 1993).
2.3.2 Renal toxicity
Nephrotoxicity due to aminoglycosides usually presents in humans
as an acute tubular necrosis manifested as proteinuria, cylinduria and
inability to concentrate the urine. This is followed by a reduction in
glomerular filtration rate with a rise in serum creatinine and blood
urea nitrogen. Aminoglycosides bind to the luminal surface of the
proximal tubules, are internalized by pinocytosis and fuse with
lysosomes. It is postulated that they become sequestered in lysosomes
where they disrupt phospholipid metabolism (prominant myeloid bodies
have been observed in renal tubular cells exposed to gentamicin), and
renal cell death occurs consequent to changes in lysosomal
biochemistry (Pratt & Fekaty, 1986).
2.3.3 Neuromuscular blockade
Aminoglycosides can produce a non-depolarizing type of
neuromuscular blockade due to reduced acetylcholine release from motor
nerve endings and reduced sensitivity of the post-junctional endplate;
this effect is completely reversed by administration of calcium (Pratt
& Fekaty, 1986).
2.3.4 Allergic reactions
The incidence of allergic reactions to systemically administered
aminoglycosides is reported to be very low. The incidence of allergic
reactions to dihydrostreptomycin specifically was not reported (Pratt
& Fekaty 1986).
2.3.5 Other effects
Aminoglycosides have been reported to cause neutropenia,
agranulocytosis, and aplastic anaemia on rare occasions. Transient
elevation of hepatic enzymes occurs occasionally with
amino-glycosides. The incidence of specific effects associated with
dihydrostreptomycin were not reported (Pratt & Fekaty, 1986).
5. REFERENCES
ANDERSON, D.G. & JEWELL, M. (1945). The absorption, excretion and
toxicity of streptomycin in man. New Engl. J. Med., 233: 485-491.
BACHARACH, A.L., CLARK, B.J., McCULLOCH, M., & TOMICH, E.G. (1959).
Comparative toxicity studies on ten antibiotics in current use.
J. Pharm. & Pharmacol., 11: 737-741.
BEEK, B., GÖBEL, D., OBE, G., & RADENBACH K.L. (1974). Prospective
controlled clinical trial of antitubercular agents in triple
combinations for mutagenicity in leukocyte cultures (short report).
Prax. Pneumol., 28: 970.
BERG, K. (1951). The toxic effect of streptomycin on the vestibular
and cochlear apparatus: an experimental study on cats. Acta Otolaryn
(Stoch), suppl. 97: 1-77.
BLOBEL, H., & BURCH, C.W. (1960). Diffusion of dihydrostreptomycin and
chlortetracycline into milk of dairy cows following parenteral
administration. J. Amer. Vet. Med. Assoc., 137 698-700.
BOUCHER, D & DELOST, P. (1964). Developpement post-natal des
descendants issus de meres traités par la streptomycine au cours de la
gestation chez la souris. C.R. Soc, Biol. (Paris), 158: 2065-2069.
BRITISH PHARMACEUTICAL CODEX (1968). The Pharmaceutical Press, London.
BROOKS, C., & ROLPH, T.P. (1989a). The effect of streptopen injection
on the health of cattle. Unpublished report No. AnH89/R/65 from
Pitman-Moore Ltd., Uxbridge, Middlesex, England. Submitted to WHO by
Pitman-Moore, Inc., Mundelein, IL, USA.
BROOKS, C., & ROLPH, T.P. (1989b). The effect of streptopen injection
on the health of sheep. Unpublished report No. AnH89/R/66 from Pitman-
Moore Ltd., Uxbridge, Middlesex, England. Submitted to WHO by Pitman-
Moore, Inc., Mundelein, IL, USA.
BROOKS, C., EASTWOOD, B., & ROLPH, T.P. (1989). The effect of
streptopen injection on the health of pigs. Unpublished report No.
AnH89/R/75 from Pitman-Moore Ltd., Uxbridge, Middlesex, England.
Submitted to WHO by Pitman-Moore, Inc., Mundelein, IL, USA.
BYWATER, R.J. (1982). Aminoglycoside antibiotics. In: Brander, G.C.,
Pugh, D.M. & Bywater, R.J. (eds.), Veterinary Applied Pharmacology and
Therapeutics, 4th edition, Balliere Tindall, London, pp. 387-393.
CARMAN, R.J. (1994). Dihydrostreptomycin MIC determinations for human
gut flora. Unpublished report from TechLab Inc., VPI Research Park,
Blacksburg, Virginia 24060, USA. Submitted to WHO by Norbrook
Laboratories Ltd., Newry, Northern Ireland.
CHRISTENSEN, E., HERTZ, H., RISKAER, N. & VRA-JENSEN, G. (1951).
Histological investigations in chronic streptomycin poisoning in
guinea-pigs. Ann. Otol., 60: 343-349.
CLARK, C.H. (1977). Toxicity of aminoglycoside antibiotics. Modern
Veterinary Practice, Part 7, 58: 594-598.
DAS, B.C., & SHARMA, T. (1983). Reduced frequency of baseline sister
chromatid exchanges in lymphocytes grown in antibiotics- and serum-
excluded culture medium. Hum Gen., 64: 249-253.
DAVIES, D.M. (1991). Textbook of adverse drug reactions. Fourth
edition, Oxford University Press, London, p. 51.
DAVIES, J., GILBERT, W., & GORINI, L. (1964). Streptomycin suppression
and the code. Proc. Nat. Acad. Sci., 51: 883-890.
DESALVA, S.J., EVANS, R.A., & MARCUSSEN, H.W. (1969). Lethal effects
of antibiotics in hamsters. Toxicol. Appl. Pharmacol., 14: 510-514.
DOLLERY, C. (1991). Therapeutic Drugs, C. Dollery (ed.), Churchill
Livingston, London, pp. 100-103.
DONALD, P.R. & SELLARS, S.L. (1981). Streptomycin ototoxicity in the
unborn child. S. Afr. Med. J., 60: 316-318.
EDISON, A.O., KUNA, S., CUCHIE, F.T. & HANSON, J.T. (1951). Relative
absorption of salts of streptomycin and dihydrosreptomycin after oral
administration. Antibiotics & Chemotherapy, 1: 49-53.
ELIAS, W.F. & DURSO, J. (1945). Blood, urine and faecal levels of
streptomycin in the treatment of human infections of E. Typhosa.
Science, 101: 589-591.
ERICSON-STRANDVIK, B. & GYLLENSTEN L. (1963). The central nervous
system of fetal mice after administration of streptomycin. Acta
Pathol. Microbiol. Scand., 59: 292-300.
ERLANSON, P., & LUNDGREN, A. (1964). Ototoxic side effects following
treatment with streptomycin, dihydrostreptomycin and kanamycin. Acta
Medica Scandinavica, 176: fasc. 2.
GAINES, S.A., ROLLINS, L.D., SILVER, R.P, & WASHINGTON, M. (1978).
Effects of low concentrations of dihydrostreptomycin on drug
resistance in enteric bacteria. Antimicrobial agents and
chemotherapy, 14: 252-256.
GOLDBERG, I.H. (1965). Mode of action of antibiotics. II. Drugs
affecting nucleic acid and protein synthesis. Am. J. Med., 39: 722-
752.
GRAHAM, B.E., VANDER BROOK, N.J. & KUIZENGA, M.H. (1946). Preliminary
studies on the absorption and excretion of streptomycin in dogs.
Science, 103: 364-365.
GRAY, J.E. & PURMALIS A. (1958). The acute toxicity of procaine
penicillin G and of dihydrostreptomycin sulfate in the pigeon and the
chicken. Avian Disease, 2: 187-196.
HAMMOND P.B. (1953). Dihydrostreptomycin dose-serum level relationship
in cattle. J. Amer. Vet. Med. Assoc., 122: 203-206.
HAWKINS, J.E. & LURIE, M.H. (1953). The ototoxicty of
dihydrostreptomycin and neomycin in the cat. Ann. Otol., 62: 1128-
1148.
HUBER, W.G. (1966). Streptomycin. In: Veterinary Pharmacology and
Therapeutics, Leo Meyer Jones (ed), 3rd edition, Iowa State College
Press, pp. 519-530.
HUEBNER, R.A., GLASSMAN, J.M., HUDYMA, G.M. & SEIFTER, J. (1956). The
toxic dose of dihydrostreptomycin in fowl. Cornell Vet., 46: 219-
212.
JAJU, M., JAJU, M., & AHUJA, Y.R. (1983). Cytogenetic effects of
chemotherapy with three combinations of anti-tubercular drugs
involving isoniazid, thiacetazone, para-amino-salicylic acid and
streptomycin on human lymphocytes: chromosome aberrations, sister
chromatids exchanges and mitotic index. Hum. Gen., 64: 42-49.
KERN, G. (1962). Zur Frage der Intrauterine Streptomycin Schadigung.
Schweiz. Med. Wochenschr., 92: 77-79.
KODAMA, F., FUKUSHIMA, F., & UMEDA, M. (1980). Chromosome aberrations
induced by clinical medicines. J. Tox. Sci., 5: 141-150.
MARSHALL, E.K. (1948). The absorption, distribution and excretion of
streptomycin. J. Pharmacol. Exper. Therapeut., 92: 43-48.
MARTINDALE, (1993). The extra pharmacopoeia. Reynolds, J.E.F. (ed.),
30th Edition, Pharmaceutical Press, pp. 159-160.
MARYNOWSKI, A., & SIANOZECKA, E. (1972). Comparison of the incidence
of congenital malformations in neonates from healthy mothers and from
patients treated for tuberculosis. Ginekol. Pol., 43: 713-715.
McGEE, T.M., & OLSZEWSKI, J. (1962). Streptomycin sulphate and
dihydrostreptomycin toxicity. Arch. Otolaryngol., 75: 295-311.
MOLITOR, H., GRAESSLE, O.E., KUNA, S., MUSHETT, C.W., SILBER, R.H.
(1946). Some toxicological and pharmacological properties of
streptomycin. J. Pharm. Exp. Ther., 86: 151-173.
NAKAMOTO, Y., OTANI, H., & TANAKA, O. (1985). Effects of
aminoglycosides administered to pregnant mice on postnatal development
of inner ear in their offspring. Teratology, 32: 34B.
NEU, R., ASPILLAGA, M.J., & GARDNER, L.I. (1965). Effects of
antibiotics on chromosomes of cultured human leucocytes. Nature
(London), 205: 171-172.
NOMURA, T., KIMURA, S., KANZAKI, T., ET AL. (1984). Induction of
tumors and malformations in mice after prenatal treatment with some
antibiotic drugs. Med. J. Osaka Univ., 35: 13-17.
OBE, G. (1970). The effect of streptomycin and dihydrostreptomycin on
human chromosomes in vitro. Molec. Gen. Genetics, 107: 361-365.
PRATT, W.B., & FEKATY, R. (1986). Bactericidal inhibitors of protein
synthesis, the aminoglycosides. In: The antimicrobial drugs, Chapter
7, Oxford University Press, Oxford, pp. 153-183.
REINBOLD, G.W., & REDDY, M.S. (1974). Sensitivity or resistance (of)
dairy starter and associated micro-organisms to selected antibiotics.
J. Milk Food Technol., 37: pp. 517-521.
RISKAER, N., CHRISTENSEN, E. & HERTZ, H. (1952). The toxic effects of
streptomycin and dihydrostreptomycin in pregnncy, illustrated
experimentally. Acta Tuber. Pneumol. Scand., 27: 211-216.
ROBINSON, C.G. & CAMBON, K.G. (1964). Hearing loss in infants of
tuberculous mothers treated with streptomycin during pregnancy.
N. Engl. J. Med., 271: 949-951.
ROLLINS, L.D., GAINES, S.A., POCURULL, D.W., & MERCER, H.D. (1975).
Animal model for determining the no-effect level of an antimicrobial
drug on drug resistance in the lactose-fermenting enteric flora.
Antimicrobial Agents and Chemotherapy, 7: 661-665.
RUDD, A.P., & SILLEY, P. (1987a). Antibiotic concentrations in cattle
serum following a single intramuscular injection of Streptopen
injection. Unpublished report No. An.H.87/R/22 from Pitman-Moore Ltd.,
Uxbridge, Middlesex, England. Submitted to WHO by Pitman-Moore, Inc.,
Mundelein, IL, USA.
RUDD, A.P., & SILLEY, P. (1987b). Antibiotic concentrations in sheep
serum following a single intramuscular injection of Streptopen
injection. Unpublished report No. An.H.87/R/27 from Pitman-Moore Ltd.,
Uxbridge, Middlesex, England. Submitted to WHO by Pitman-Moore, Inc.,
Mundelein, IL, USA.
RUDD, A.P., & SILLEY, P. (1987c). Antibiotic concentrations in dog
serum following a single intramuscular injection of Streptopen
injection. Unpublished report No. An.H.87/R/34 from Pitman-Moore Ltd.,
Uxbridge, Middlesex, England. Submitted to WHO by Pitman-Moore, Inc.,
Mundelein, IL, USA.
RUDD, A.P., & SILLEY, P. (1987d). Antibiotic concentrations in cat
serum following a single intramuscular injection of Streptopen
injection. Unpublished report No. An.H.87/R/42 from Pitman-Moore Ltd.,
Uxbridge, Middlesex, England. Submitted to WHO by Pitman-Moore, Inc.,
Mundelein, IL, USA.
SHAMBAUGH, G.E., DERLACKI, E.L., HARRISON, W.H., HOUSE, H., HOUSE, W.,
HILDYARD, V., SCHUKNECHT, H., & SHEA, J.J. (1959). Dihydrostreptomycin
deafness. JAMA, 170: 1657-1660.
SNIDER, D.E., LAYDE, P.M., JOHNSON, M.W. & LYLE, M.A. (1980).
Treatment of tuberculosis during pregnancy. Am. Rev. Resp. Dis.,
122: 65-79.
SNYDER, M. J., AL-IBRAHIM, M., & HORNICK, R. B. (1972). The effect of
oral DHS on resistance development in the intestinal microflora of
man. Unpublished report from the Division of Infectious Diseases,
Department of Medicine, University of Maryland School of Medicine.
Submitted to WHO by FDA.
STALHEIM, O.H.V. (1970). Absorption and excretion of tritiated
dihydrostreptomycin in cattle and swine. American Journal of
Veterinary Research, 31: 497-499.
STEBBINS, R.B., GRAESSLE, O.E., & ROBINSON H.J. (1945). Studies on the
absorption and excretion of streptomycin in animals. Proc. Soc. Exp.
Biol. Med., 60: 68-72.
STEVENSON, L.D., ALVORD, E.C., & CORRELL, J. W. (1947). Degeneration
and necrosis of neurones in eighth cranial nuclei caused by
streptomycin. Proc. Soc. Exp. Biol. Med., 65: 86-88.
TISDEL, M., & HARRIS, D.L. (1976). Dihydrostreptomycin: 90-day
toxicity study in guinea pigs. Unpublished report, Warf Study Code T-
615 from Warf Institute, Inc., Madison, Wisconsin, USA, on behalf of
Animal Health Institute. Submitted to WHO by FDA.
TISDEL, M., HARRIS, D.L., HAARS, R., & NEES, P.O. (1976).
Dihydrostreptomycin: 90-day toxicity study in cats. Unpublished
report, Warf Study Code T-614 from Warf Institute, Inc., Madison,
Wisconsin, USA, on behalf of Animal Health Institute. Submitted to WHO
by FDA.
TSANG, Y.C., & CHIN, T.C. (1963). Neurotoxicity of streptomycin.
Scientia Sinica, 12: 1019-1040.
VARPELA, E., HIETALAHTI, J., & ARO, M.J.T. (1969). Streptomycin and
dihydrostreptomycin medication during pregnancy and their effect on
the child's inner ear. Scand. J. Resp. Dis., 50: 101-109.
WARKANY, J. (1979). Antituberculous drugs. Teratology, 20: 133-138.
WAZETER, F. X. (1970a). Dihydrostreptomycin: Ninety-day toxicity study
in cats. Unpublished report from International Research and
Development Corporation on behalf of Animal Health Institute.
Submitted to WHO by FDA.
WAZETER, F. X. (1970b). Dihydrostreptomycin: Two-year oral toxicity
study in rats (six month interim report). Unpublished report from
International Research and Development Corporation on behalf of Animal
Health Institute. Submitted to WHO by FDA.
WAZETER, F. X. (1970c). Dihydrostreptomycin: Rabbit teratogenic study.
Unpublished report from International Research and Development
Corporation on behalf of Animal Health Institute. Submitted to WHO by
FDA.
WAZETER, F. X. (1971). Dihydrostreptomycin: Two-year oral toxicity
study in rats (18 month interim report). Unpublished report from
International Research and Development Corporation on behalf of Animal
Health Institute. Submitted to WHO by FDA.
WAZETER, F. X., & GOLDENTHAL, E.I. (1972). Dihydrostreptomycin: Two-
year oral toxicity study in rats. Unpublished report from
International Research and Development Corporation on behalf of Animal
Health Institute. Submitted to WHO by FDA.
WIGHTMAN, S.R., MANN, P.C., & WAGNER, J.E. (1980). Dihydrostreptomycin
toxicity in the Mongolian gerbil, Meriones unguiculatus. Laboratory
Animal Science, 30: 71-75.
